Back to Journals » International Medical Case Reports Journal » Volume 14
Successful Expectant Management of the Anomalous Fetus with Sirenomelia in Twin Pregnancy: A Case Report and Literature Review
Received 4 January 2021
Accepted for publication 26 March 2021
Published 9 April 2021 Volume 2021:14 Pages 229—232
DOI https://doi.org/10.2147/IMCRJ.S300318
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Ronald Prineas
Temesgen Tilahun,1 Dawit Desta2
1Department of Obstetrics & Gynecology, Institute of Health Sciences, Wollega University, Nekemte, Ethiopia; 2Department of Emergency Surgery, Gynecology, and Obstetrics, Arjo Hospital, Arjo, Ethiopia
Correspondence: Temesgen Tilahun
Department of Obstetrics & Gynecology, Institute of Health Sciences, Wollega University, P.O Box: 395, Nekemte Oromia Ethiopia, Central, Addis Ababa, Nekemte, Ethiopia
Tel +251912057186
Email [email protected]
Background: Sirenomelia is a rare congenital defect. Its management during pregnancy and after delivery is becoming a controversial issue because of its complex nature and management outcome. The possibility of expectant management in the sirenomelia twin drove us to write this case report.
Case Presentation: We report a case of successful expectant management in twin sirenomelia which was diagnosed in the second trimester. Prenatal counseling of the couple by a multi-disciplinary team regarding the diagnosis, treatment, and prognosis of the sirenomelia twin was done. The mother gave birth, at term, to one normal and one sirenomelia neonate by cesarean section.
Conclusion: Expectant management of sirenomelia one in twin pregnancy is advisable in a resource-limited setting.
Keywords: sirenomelia, twin pregnancy, expectant management
Introduction
Sirenomelia, which is also known as mermaid syndrome, is a multisystem congenital anomaly characterized by a partial or complete fusion of the lower limbs into a single lower limb, giving the appearance of a mermaid’s tail.1–3 It is associated with the gastrointestinal tract (anorectal, esophageal), genitourinary tract (renal, genitalia, lower urinary tract), cardiovascular system, respiratory tract, musculoskeletal system, and central nervous system anomalies.2,3
Sirenomelia is a very rare congenital malformation with an incidence of 0.98–4.2 per 100, 000 live births.3–5 Its incidence of twin pregnancy is extremely low. However, compared with a singleton pregnancy and dizygotic twins, the incidence of sirenomelia in the monozygotic twin is more than 100-fold.2 Therefore, the diagnosis and management of sirenomelia in twin pregnancy is a worthy matter to be discussed. The exact etiology of sirenomelia is unclear.4 Different works of literature associate it with extreme maternal age,3 maternal diabetes, prenatal exposure to retinoic acid, cadmium, cyclophosphamide,4 cocaine, landfills water, or lamotrigine.6. Here we present successful expectant management of sirenomelia one in twin pregnancy which was diagnosed in the second trimester.
Case Presentation
This is a 20-year-old woman from Western Ethiopia who was married to a non-consanguineous –24–year–old man. She is a farmer and of low socioeconomic status. She is a primigravida mother who does not remember her last normal menstrual period but claims to be amenorrheic for the last 09 months. She presented to Arjo primary hospital with the complaint of labor pain of 3 hours. There was no passage of liquor. She had no self or family history of chronic medical problems like hypertension, diabetes Mellitus, or bronchial asthma. She had no history of smoking, chewing khat, alcohol, or other drug abuse. Folic acid supplementation was not given for the mother during and/or before the pregnancy. She has no history of exposure to hazardous chemicals. There was no history of twinning or congenital anomaly in the family. She had four visits of prenatal care follow up at Arjo primary hospital. During the prenatal care visit, physical examination, and essential laboratory tests including blood group, blood glucose, hemoglobin, urinalysis, and serology for human immunodeficiency virus (HIV), hepatitis and syphilis were done. The laboratory results showed hemoglobin = 13g/dl, blood sugar= 106mg/dl, hepatitis B surface antigen (HBsAg) = negative, Venereal Disease Research Laboratory Test (VDRL) = nonreactive, HIV rapid test = negative and A negative blood group.
Second-trimester ultrasound examination, done at 3rd antenatal care visit, revealed diamniotic twin intrauterine pregnancy (one sirenomelia twin). The first twin was in cephalic presentation with an average gestational age of 27 weeks while the second twin was in breech presentation with an average gestational age of 26 weeks. There was only one leg bone in the second twin fetus. There was oligohydramnios in 2nd twin fetus. Placenta was fundal and a dividing membrane was seen.
The 4th antenatal care visit was done one month after the 3rd visit. It showed the normal fetus in good condition but oligohydramnios in anomalous sirenomelia twin. The couple was counseled by the multidisciplinary team regarding diagnosis, treatment, prognosis, and possible complications of sirenomelia. Finally, expectant management was decided and the mother was appointed to come after 4 weeks. Unfortunately, she came to the hospital in labor.
Clinical examination during this time showed that she is in labor pain. Her vital signs were blood pressure= 100/60 mmHg Pulse rate=86 beats per minute, respirator rate=22 breaths per minute, and temperature=36.2°c. The conjunctiva was pink. Abdominal examination showed term-sized gravid uterus, multiple fetal poles felt, fetal heart best heart at two places (143 and 130 beats per minute), 3 contractions in ten minutes each staying 30 to 40 seconds. On pelvic examination cervix was 6cm dilated, 100%effaced, vertex presentation, the station at −1, membrane intact, and adequate pelvis. Intrapartum ultrasound examination showed the first twin is a cephalic presentation and the second twin in breech presentation. Both fetuses were alive. With the impression of an active phase of labor and twin pregnancy, she was admitted to the labor ward. After 4 hours, she was reevaluated and the cervix was still 6cm. Thus, with the final diagnosis of the arrest of cervical dilatation cesarean section was done under spinal anesthesia to effect delivery of first twin male alive neonate weighing 2500gms with APGAR scores of 8 and 9 at 1st and 5th minute respectively, second twin sirenomelic neonate weighing 1800gms with APGAR scores of 7 and 9 at 1st and 5th minute respectively. The single placenta was delivered by cord traction. It is a monochorionic diamniotic placenta. There were no identified gross placental and umbilical cord pathologies. Detailed physical examination of the second twin showed the absence of external genital organs, fused leg bones (both femur and tibia), short neck (Figure 1), and imperforate anus. This is a rudimentary limb, fused leg bones, no mobility, and on foot. Though the prognosis is poor, there was an attempt to refer the newborn to a better setting but the families refused the medical advice. The newborn was active and feeding well for the first two days of delivery. On the third day, it got sick and passed away.
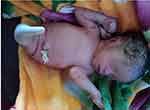 |
Figure 1 Anomalous fetus with sirenomelia in twin delivery at Arjo Primary Hospital, 2020, Western Ethiopia. |
On the fourth operative day, the mother had a smooth postoperative course and her first neonate was normal. They were discharged with advice about postpartum care follow-up.
Discussion
Sirenomelia is a severe congenital malformation involving multiple organ systems.1–3,7–9 The fusion of the lower extremities, called symelia, is the pathognomonic finding in sirenomelia.9,10 The visceral anomalies occur uniformly and significantly affect survival.9,10 Gross examinations of our case showed completely fused lower limbs, absence of external genitalia, and imperforated anus. But we did not have an abdominal ultrasound examination and x-ray of the sirenomelia neonate to comment on visceral anomaly and detail skeletal defect.
The etiology and pathogenesis of sirenomelia remain unknown.1,10 However, there are two proposed hypotheses. These are the defective blastogenesis hypothesis and the vascular steal hypothesis.9 Experimental analysis in mice shows genetic origin in sirenomelia.9 But in humans, sirenomelia is still considered sporadic.1 In our case, there is no risk factor and chronic medical condition detected. But the mother was not supplemented with folic acid during and before pregnancy.
Though sirenomelia is a very rare condition,1 its incidence in twin pregnancies is more common when compared to singleton pregnancies.2 There are approximately 300 cases reported in the literature, 15% of which are associated with twinning, most often monozygotic.7,11 In twin pregnancies, in addition to the above-mentioned mechanisms, mechanical defects resulting from lateral compression by amniotic folds can end up in sirenomelia.3 Therefore, the diagnosis and management of sirenomelia in twin pregnancy need attention.
Early diagnosis of sirenomelia is very crucial for timely prenatal counseling and decision of its management. High-resolution or color Doppler ultrasound during prenatal care can safely make the diagnosis of sirenomelia.12 During the first trimester, the amniotic fluid volume is usually normal, unrelated to fetal urine production. In the second and third trimesters, oligo-hydramnios from renal agenesis is a common finding in sirenomelia.13 This makes ultrasound examination difficult. Therefore, it advisable if to have an ultrasound examination in the late first and early second trimester.1 In our case, the diagnosis was made in the late second trimester.
In the presence of oligohydramnios and after 20 weeks of pregnancy, fetal Magnetic Resonance Imaging (MRI) is the preferred option. It demonstrates various anomalies in greater detail than a fetal sonogram.12
Sirenomelia is a fatal malformation.1 About 50% of cases are stillborn because of bilateral renal agenesis and associated visceral anomalies.11 Therefore, early diagnosis and decision are important. In singleton pregnancies, the decision to terminate or continue the pregnancy depends on factors like the extent of visceral anomalies, family-related issues, and the presence of a multidisciplinary medical team.10,14,15 The prognosis worsens especially in association with VACTERL and VACTERL-H syndrome.16 In a twin pregnancy, expectant management is possible as far as there is no unique complication of twin pregnancies and other obstetric problems necessitating termination of pregnancy.13 In a better setting and when the diagnosis is made in early pregnancy, voluntary selective termination of sirenomelia one in twin pregnancy may be advised.2 Our case was diagnosed in the late 2nd trimester of pregnancy. After having appropriate prenatal counseling, expectant management was decided. Prenatal care was successful. The mother delivered by cesarean section at term.
Sirenomelia neonates usually die within a few days of delivery because of associated anomalies and poor medical care.1,2,10 In our case, the neonate died on the 3rd day of delivery. However, because of advanced medical care and multidisciplinary approach, sirenomelia is no longer considered a lethal condition.14 Survival depends on visceral associated anomalies, particularly kidneys, rather than sirenomelia itself.10 So far, there are six cases of sirenomelia that survived by multidisciplinary treatment.14,17 In our case, though an effort was made to refer the neonate to a better setting, it was not possible. The family ignored the neonate due to cultural and religious reasons. Thus, it did not have any imaging, genetic testing, or a post mortem examination.
Abbreviations
HIV, human immunodeficiency virus; HBsAg, hepatitis B surface antigen; MRI, magnetic resonance imaging; VDRL, Venereal Disease Research Laboratory Test.
Data Sharing Statement
The datasets used during the current study are available from the corresponding author on reasonable request.
Ethics Approval and Consent to Participate
The Ethics Committee of Wollega University has approved the publication of this case.
Consent for Publication
Written informed consent was obtained from the couple for publication of this case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Acknowledgment
We thank the couple for allowing the publication of this case report.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis, and interpretation, or in all these areas; took part in drafting, revising, or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Disclosure
The authors report no competing interests in this work.
References
1. Kavunga EK, Bunduki GK, Mumbere M, Masumbuko CK. Sirenomelia associated with an anterior abdominal wall defect: a case report. J Med Case Rep. 2019;13(1):213. doi:10.1186/s13256-019-2162-0
2. Xu T, Wang X, Luo H, Yu H. Sirenomelia in twin pregnancy: a case report and literature review. Medicine. 2018;97(51):e13672. doi:10.1097/MD.0000000000013672
3. Orioli IM, Amar E, Arteaga-Vazquez J, et al. Sirenomelia: an epidemiologic study in a large dataset from the International Clearinghouse of Birth Defects Surveillance and Research, and literature review. Am J Med Genet. 2011;157C(4):358–373. doi:10.1002/ajmg.c.30324
4. Tonni G, Grisolia G. Sirenomelia: a review on embryogenic environmental theories, novel three-dimensional ultrasound imaging and first-trimester diagnosis in a case of mosaic 69,XXX/46,XX fetus. Arch Gynecol Obstet. 2013;288(1):3–11. doi:10.1007/s00404-013-2847-3
5. Reddy KR, Srinivas S, Kumar S, Reddy S, Prasad H, Irfan GM. Sirenomelia: a rare presentation. J Neonatal Surg. 2012;1(1):7.
6. Saldarriaga W, Salcedo-Arellano MJ, Ramirez-Cheyne J. Sirenomelia: two cases in Cali, Colombia. BMJ Case Rep. 2015;2015. doi:10.1136/bcr-2014-207543
7. Nokeaingtong K, Kaewchai S, Visrutaratna P. Sirenomelia type VI (sympus apus) in one of the dizygotic twins at Chiang Mai University Hospital. BMJ Case Rep. 2015;2015:bcr2014208501. doi:10.1136/bcr-2014-208501
8. Meisheri IV, Waigankar VS, Patel MP, et al. Sirenomelia: the mermaid syndrome. Pediatr Surg Int. 1996;11(8):580–581. doi:10.1007/BF00626073
9. Garrido-Allepuz C, Gonza´lez-Lamun˜o D, Ros MA. Sirenomelia Phenotype in Bmp7;Shh compound mutants: a novel experimental model for studies of caudal body malformations. PLoS One. 2012;7(9):e44962. doi:10.1371/journal.pone.0044962
10. Duhamel B. From the mermaid to anal imperforation: the syndrome of caudal regression. Arch Dis Child. 1961;36(186):152–155. doi:10.1136/adc.36.186.152
11. Sharma N, Kumar N, Jhobta A, Bhoil R. Sirenomelia, the Fetal ‘Mermaid’: ultrasound and Magnetic Resonance Features. Explor Res Hypothesis Med. 2017;2(3):68–71. doi:10.14218/ERHM.2016.00026
12. Tönnies P, Watermann D, Gellén J
13. Kurt RK, Atcı N, Ozturk İ. 11th congress of the mediterranean association for ultrasound in obstetrics and gynecology. Perinatal J. 2014;SE01–SE62. doi:10.2399/prn.14.SE001058
14. Messineo A, Innocenti M, Gelli R. Multidisciplinary surgical approach to a surviving infant with sirenomelia. Pediatrics. 2006;118(1):e220.
15. Hoque J, Tingi E, Sinha S, Bamigboye V. An unusual case of Sirenomelia Sympus Dipus (Mermaid Syndrome). Obstet Gynecol Rep. 2017;1(1):1–2. doi:10.15761/OGR.1000106
16. Kitova TT, Uchikova EH, Uchikov PA, Kitov BD. Sirenomelia associated with VACTERL and VACTERL-H syndrome. Int J Morphol. 2020;38(3):793–798. doi:10.4067/S0717-95022020000300793
17. Stanton MP, Penington EC, Hutson JM. A surviving infant with sirenomelia (Mermaid syndrome) is associated with an absent bladder. J Pediatr Surg. 2003;38(8):1266–1268. doi:10.1016/s0022-3468(03)00286-0
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
