Back to Journals » Psychology Research and Behavior Management » Volume 14
Sleep Quality and the Depression-Anxiety-Stress State of Frontline Nurses Who Perform Nucleic Acid Sample Collection During COVID-19: A Cross-Sectional Study
Authors Chen X, Liu P , Lei GF, Tong L, Wang H, Zhang XQ
Received 16 September 2021
Accepted for publication 16 November 2021
Published 26 November 2021 Volume 2021:14 Pages 1889—1900
DOI https://doi.org/10.2147/PRBM.S338495
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Professor Mei-Chun Cheung
Xiang Chen,* Ping Liu,* Guang-Feng Lei, Li Tong, Hui Wang, Xue-Qing Zhang
Department of Nursing, The First People’s Hospital of Changde City, Changde, 415000, Hunan Province, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Xue-Qing Zhang
Department of Nursing, The First People’s Hospital of Changde City, 818 Renmin Road, Changde, 415000, Hunan Province, People’s Republic of China
Email [email protected]
Objective: To explore the sleep quality and depression-anxiety-stress state of frontline nurses in high-risk areas who conduct nucleic acid sampling testing for COVID-19 to provide a basis for formulating intervention programs in crisis management.
Methods: From August 22 to 30, 2021, a convenient sampling method was used in Zhangjiajie City, Hunan Province, China. A total of 248 frontline nurses who performed nucleic acid sample collection were selected. The following tests were used: the general information questionnaire, Pittsburgh Sleep Quality Questionnaire (PSQI), and Depression–Anxiety Stress Scale (DASS-21).
Results: A total of 236 nurses completed the survey; 88.14% (n = 208) were women, the average age was 33.02± 6.81, the PSQI score was 15 (13– 17), and 231 (97.88%) nurses had sleep disorders during the period in Zhangjiajie, 219 nurses (81.36%) had anxiety, 135 nurses (45.76%) had depression, and 112 nurses (42.59%) felt stressed. Spearman correlation analysis was used to associate the PSQI with the DASS-21. The results showed that the use of hypnotic drugs was negatively correlated with DASS-21 (P< 0.05), while the rest were positively correlated. The results of the multivariate analysis of sleep disorders showed that depression, anxiety, and stress were related to sleep quality (P< 0.05), and there was no statistical difference in the other variables.
Conclusion: During the COVID-19 pandemic, the sleep quality and depression-anxiety-stress state of the frontline nurses performing nucleic acid testing were adversely affected. Sleep disturbance is a serious problem among nurses testing for the delta strain during the pandemic. Anxiety, stress, and depression are associated with sleep disorders. It is necessary to take corresponding measures and conduct crisis management interventions to improve sleep quality and mental health adjustment during public health emergencies.
Keywords: COVID-19, perform nucleic acid sample collection, sleep quality, depression-anxiety-stress
Introduction
Since December 2019, a pneumonia epidemic caused by a new type of coronavirus discovered in Wuhan, China,1 spread across the country and the world. The World Health Organization (WHO) declared it a global pandemic and a public health emergency on January 30, 2020. This global pandemic has been ongoing for nearly 20 months. The delta is a mutated strain of COVID-19. It was first discovered in India in October 2020.2 It was named “delta” by the WHO in May 2021 and has gradually become the dominant strain across the world,3 affecting at least 120 countries and regions. This strain has the characteristics of fast transmission, strong infectivity, high pathogenicity, short incubation period, and a high viral load. Moreover, patients may have typical symptoms or asymptomatic infections, even after vaccination.2 They are advised to go to the hospital for nucleic acid screening immediately, during the early stages of exposure. The local clustered epidemic caused by imported delta strains spread to many provinces, The epidemics in Nanjing, Jiangsu, Zhangjiajie, Hunan, and other places have attracted worldwide attention,4 and prevention and control situation in many places has become difficult.5 The Hunan Provincial Government sent 1435 medical health workers, including doctors, nurses, and laboratory technicians, to support Zhangjiajie. On August 26, 2021, Zhangjiajie City launched a total of 1872 nucleic acid sampling locations (including fixed and mobile), and 7.85 million people of Zhangjiajie underwent nucleic acid testing. In this testing location, the sampling workload was large, the sampling site conditions were simple and crude, the weather was hot, the isolation suits were not breathable, the working time was uncertain, the understanding of new strains was insufficient, and the risk of infection was present. All these factors may produce high work stress, and physical and mental stress symptoms in the nurses sampled, affecting their sleep quality and mental state.
During this pandemic, the medical workers have faced tremendous physical and psychological stress. Sleep is vital for the regulation of psychological and physical processes, and the lack of sleep or sleep disorders may interact with psychological and physical disorders. A systematic review report on sleep quality during COVID-19 included 86 studies from around the world with 34 conducted by medical personnel,6,7 showing that front-line medical staff’s sleep quality was significantly lower than in non-medical personnel. Another systematic review of medical staff dealing with COVID-19 indicated that the prevalence rates of anxiety, depression, and stress among medical staff were 67.55%, 55.89%, and 62.99,8 respectively. The prevalence of sleep disorders among nurses was approximately 34.8% (95% confidence interval, 24.8 to 46.4%).9 Studies in Italy, Mexico, the United States, Switzerland, India,10 and China have shown that medical staff, especially nurses, who directly participate in frontline care of COVID-19 patients, have varying degrees of sleep and mental disorders. Italian researchers11–13 have found that compared with other medical staff, COVID-19 frontline medical staff had significantly higher levels of stress, burnout, secondary trauma, anxiety, and depression; COVID-19 frontline medical staff in Mexico14 are at risk of occupational exposure (62.5%). In India,15 frontline medical staff often suffer from anxiety, depression, burnout, insomnia, and stress-related diseases, which may be mediated by individual psychological vulnerability. In China,16 COVID-19 has increased negative emotions significantly in frontline medical staff and their overall sleep quality is poor. Some even have more serious sleep disorders than untreated patients with COVID-19 pneumonia.17 Maintaining the medical staff’s mental health is key to controlling infectious diseases. Therefore, it is important to assess the sleep quality and mental status of frontline medical staff dealing with COVID-19, especially nurses. Domestic research on COVID-19 has mainly focused on pathogenic research and epidemic spread. Regarding disease prevention and control, investigation, diagnosis, and treatment, there are few articles on the sleep quality and mental state of frontline medical staff, specifically on the nurses who go to the hardest-hit areas for nucleic acid collection. This study evaluated the sleep quality of this special population, along with their mental status, to explore the formulation of crisis management intervention measures to accurately and effectively respond to public health emergencies.
Materials and Methods
Research Design and Research Participants
A cross-sectional study was conducted using a convenience sampling method through an online (WeChat) survey of 248 frontline nurses who went to Zhangjiajie to conduct nucleic acid sampling. The inclusion criteria were as follows: 1) nurses who went to Zhangjiajie for nucleic acid sampling during the pandemic; 2) nurses who were willing to participate and able to accurately fill in the questionnaire. The exclusion criteria were: 1) completion time <3 min; 2) questionnaires with incorrect common-sense answers; and 3) questionnaires with the same answer for 80% of the items. This study was approved by the ethics committee of the Changde First People’s Hospital. They were sent to the Zhangjiajie nucleic acid sampling team from August 22 to 30, 2021. A total of 248 people were sent questionnaires, of which 236 responded (95.64%).
The Measurement Questionnaire
The questionnaire included general information, sleep quality, and depression-anxiety-stress scale.
General Information
This included three parts: the general sociodemographic information of nurses performing nucleic acid sampling, their sources of stress, and training and social support. Sociodemographic characteristics included gender, age, education level, marital status, fertility status, working years, professional title, family support status, and whether the respondents was the only child. The sources of the stress questionnaire included eight items that caused worry: insufficient supply of protective materials, occupational exposure, insufficient personal knowledge or ability regarding COVID-19, delta strains spreading more easily, that delta strains will require longer treatment and recovery, the likelihood of contracting serious illnesses, the cooperation of local residents, and not adapting to sleep, eating, and other lifestyle habits. Each entry had four options, which were as follows: not worried, slightly worried, moderately worried, and significantly worried. The Cronbach’s α coefficient of the source of stress questionnaire was 0.76, and the confirmatory factor analysis of Comparative Fit IndexCFI was 0.88. Training and support for nucleic acid sampling nurses mainly included seven items, including training and testing related to COVID-19, putting on and taking off isolation gowns, and nucleic acid sampling.
Pittsburgh Sleep Quality Index (PSQI)
This scale was compiled by Buysse et al in 198918 and translated into Chinese19 to evaluate the the most recent sleep quality. It comprises 19 self-assessment items, with nine self-assessment and five other assessment items. When scoring, only the score of the former was calculated. The self-assessment items consisted of seven factors, each was calculated from 0 to 3 points; “0” indicating no difficulty, “1” mild difficulty, “2” moderate difficulty, and “3” severe difficulty. The cumulative score of each factor comprised the total PSQI score. This ranged from 0 to 21. A score ≥8 indicated a sleep disorder. The higher the score, the worse the quality of sleep. The internal consistency of Cronbach’s alpha for the Chinese version of the PSQI was 0.713.20 In this study, the Cronbach’s α coefficient of the PSQI was 0.71, and the confirmatory factor analysis of Comparative Fit IndexCFI was 0.78.
The Depression Anxiety Stress Scale, DASS
The scale was compiled by Lovibond21 and others. It is a self-rating scale used to measure the severity of negative mood symptoms. The original scale has 42 items. After localization and streamlining,22 there were 21 items, including three subscales, to examine the individual experience of negative emotions, such as depression, anxiety, and stress. According to the scoring guidelines for this scale the sum of seven items from each subscale multiplied by 2 was the subscale score which ranged from 0 to 42 points. The higher the score, the more serious the depression, anxiety, or stress. According to the score, the symptoms were divided into five levels: normal, mild, moderate, severe, and extremely severe. The depression scale ≤9 was classified as normal, l0–l3 was mild, 14–20 was moderate, 21–27 was severe, and ≥28 was extremely severe. Regarding the anxiety scale, ≤7 was normal, 8–9 was mild, 10–14 was moderate, 15–19 was severe, and ≥20 was extremely severe. On the stress scale, ≤14 was classified as normal, 15–18 was classified as mild, 19–25 as moderate, 26–33 as severe, and ≥34 was considered extremely severe. Studies in China and abroad have tested the reliability and validity of the scale. The internal consistency coefficients of the three subscales were 0.77, 0.79, and 0.76; the Cronbach’s α value of the scale was greater than 0.90.22 In this research, the Cronbach’s α coefficient and the CFI of the Depression–Anxiety Stress Scale (DASS-21) were 0.72 and 0.90.
Data Collection
We used the convenience sampling method. The web-questionnaires were sent to the research team, who shared them with the nucleic acid collection teams from various hospitals in Zhangjiajie. The following quality control methods were used: 1) Before the survey, the research team selected 10 nurses from the frontline fever clinics to fill in the questionnaire and discover possible problems; 2) Three random common-sense questions unrelated to the survey were inserted to eliminate invalid questionnaires; 3) Missing answers were prompted. Otherwise, the questionnaire could not be submitted.
Statistical Analysis
All statistical analyses were performed using SPSS 20.0 software and jamovi v1.8.1.23 Quantitative data were expressed as mean ± standard deviation, and categorical data as numbers (%). Spearman correlation analysis was used to analyze the relationship between PSQI and DASS-21 regarding depression, anxiety, and negative stress emotions. Univariate and multivariate analyses were used to explore the factors related to the occurrence of sleep disorders. All analyses were performed using a two-sided test at P<0.05.
Results
Demographic Characteristics of the Nurse Assistants Performing Nucleic Acid Tests
A total of 1435 medical staff supported testing in Zhangjiajie from July to August 2021. However, the precise number of doctors, nurses, and laboratory technicians has not been determined. This study aimed to investigate the sleep quality and mental state of frontline nurses performing nucleic acid testing during COVID-19 in Zhangjiajie. A total of 248 individuals answered the survey, of which four people were excluded due to incomplete responses, three were eliminated as they could not complete the web-questionnaires in less than 3 minutes, and 80% of the answers were identical. Two people who did not follow the instructions—two physicians, and one a laboratory technician—were excluded. The final sample size was 236, and the response rate was 95.16%. The majority (88.14%, n = 208) were female, whereas 11.86% (n = 28) were male, with a mean age of 33.02 ± 6.81 years old. Most of them were in the 31 to 40 age group—109 (46.19%). A total of 161 (68.22%) nurses assisting in Zhangjiajie were married, 181 (76.69%) had a bachelor’s degree, and 51.27% had one child. The largest number of professional titles was intermediate (nurse-in-charge)—117 (49.58%). The sociodemographic characteristics of the nurses are presented in Table 1.
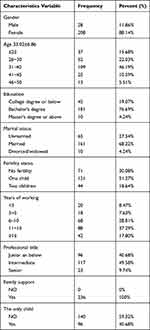 |
Table 1 Demographic of Nurse Performing Nucleic Acid Test (N = 236) |
Sources of Stress in Nurses Performing Nucleic Acid Tests
We evaluated stress in nurses performing nucleic acid testing and found several sources. The first was the delta strain of COVID-19 requiring longer treatment and recovery and the possibility of a more severe illness (83.9%), greater transmissibility and faster replication of the delta strain (82.2%), occupational exposures (82.2%), and personal knowledge or lack of ability to deal with the delta strain of COVID-19 (80.3%). Most nurses performing nucleic acid testing in Zhangjiajie did not worry about insufficient supplies of protective materials (193, 81.78%). More than half of the nurses did not worry about the cooperation of local residents (57.2%), and a small number of nurses worried about not adapting their sleeping, eating, and other lifestyle habits (37.29%), as shown in Table 2.
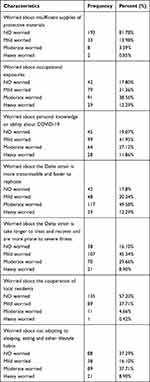 |
Table 2 The Sources of Stress in Nurse Performing Nucleic Acid Test (N = 236) |
Training and Social Support
The research showed that all nurses using medical coverage (100%) and performing nucleic acid testing (100%), accepted the training and examination related to COVID-19 (100%). They knew the symptoms, signs, diagnosis, treatment, disinfection, isolation, transmission, and precautionary measures. All nurses performing nucleic acid testing in Zhangjiajie had been fully vaccinated against COVID-19 (100%) and had passed the strict training and examination on COVID-19. During the assistance period, 99.15% of nurses received humanistic care from the local government, and 95.34% received psychological support. However, only 63.56% received support for sleep disorders during the assistance period (Table 3).
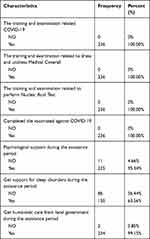 |
Table 3 The Training and Support in Nurse Performing Nucleic Acid Test (N = 236) |
The Total Score and Subscales of PSQI Score
According to the questionnaire, the total score of the PSQI was 15 (13–17), and 231 (97.88%) nurses had sleep disorders during the assistance period. The PSQI subscale scores are presented in Table 4.
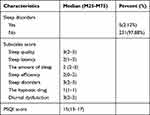 |
Table 4 The Total Score and Subscales of PSQI Score in Nurse Performing Nucleic Acid Test (N = 236) |
The Psychological Negative Emotion Grade of DASS-21
The scores on the DASS-21 for depression, anxiety, and stress were 10.18±4.00, 11.67±4.49, and 13.32±5.59, respectively. Among the nurses, 219 had anxiety and negative emotions, accounting for 81.36%; 135 (45.76%) had depression and negative emotions, and 112 (36.20%) felt stress and negative emotions (Table 5).
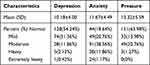 |
Table 5 The Psychological Negative Emotion of DASS-21 in Nurse Performing Nucleic Acid Test (N = 236) |
Correlation Analysis Between Sleep Quality and Negative Emotions
The Spearman correlation analysis associated the PSQI with the DASS-21 score on depression, anxiety, and stress. The results showed that sleep quality, sleep latency, sleep duration, sleep efficiency, sleep disorders, diurnal dysfunction with anxiety, stress, and depression were positively correlated (P < 0.05). Hypnotic drug use was correlated with negative emotional anxiety, feeling stress, and depression (P < 0.05) (Table 6).
 |
Table 6 The Correlation Analysis Between Sleep Quality with Psychological Negative Emotion in Nurse Performing Nucleic Acid Test (N = 236) |
Univariate and Multivariate Analysis of Factors in Sleep Disorder
Demographic characteristics included gender, age, education, marital status, years of work, professional title, sources of stress, training and social support, and negative emotion grade of anxiety, depression, and stress. Univariate analysis showed worry about insufficient supplies of protective materials, occupational exposures, personal knowledge or ability regarding COVID-19, that the delta strain is more transmissible and faster to replicate, that the delta strain requires longer treatment and recovery, the cooperation of local residents, not adapting to sleeping, eating, and other lifestyle habits. Support for sleep disorders during the assistance period, provision of humanistic care from the local government during the assistance period, depression, anxiety, and stress may be risk factors for sleep disorders that influence sleep quality (P<0.05). Multivariate analysis showed that depression, anxiety, and stress were the three factors associated with sleep quality (P<0.05). However, no statistical differences were observed between the other variables (Table 7).
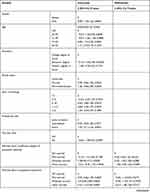 |  |  |
Table 7 The Univariate and Multivariate Analysis on Factors for Sleep Disorder Among Nurse Performing Nucleic Acid Test (N = 236) |
Discussion
Since COVID-19 was first identified in Wuhan, China at the end of December 2019, the delta strain has become a major endemic strain in most parts of the world. In China, the first confirmed delta strain cases were in Nanjing, and in Zhangjiajie, Hunan Province, a world-famous tourist city. The situation in Zhangjiajie is severe; the Hunan government sent 1435 medical staff, including doctors, nurses, and laboratory technicians to support Zhangjiajie. A study17 showed that sleep disturbance is prevalent among medical staff during the COVID-19 outbreak, especially in high-risk staff who directly contact patients, as well as nurses, doctors, and administrative personnel. A meta-analysis9 included 93 cross-sectional studies of 93,112 nurses and reported pooled prevalence estimates for anxiety, stress, depression, and sleep disorders during COVID-19. This is because nurses are in close proximity to the patients. They have a high risk of infection from patients, even the asymptomatic cases, and this may lead to problems such as sleep disturbance, stress, anxiety, and depression.24 However, there are a few reports on nurses performing nucleic acid testing for psychological stress and sleep quality, especially because the delta strain is more transmissible and faster to replicate, the infection takes longer to treat and recover, and is more likely to be a severe illness.
The results showed that among the nurses performing nucleic acid testing in Zhangjiajie who participated in the investigation, 88.14% were female and 11.86% were male. In China, the nursing profession continues to be female-dominated, and the percentage of men remains lower. In 2019, the data showed 4.09 million people registered as nurses in China, of which male nurses accounted for only 2.3%.25 Regarding education level, most nurses performing nucleic acid testing had a bachelor’s degree (76.69%) and 68.22% were married. The largest number of professional titles was intermediate (nurse-in-charge). The current study shows that all of the nurses taking the initiative to fight against COVID-19 had family support for assisting in Zhangjiajie. Chinese healthcare providers have a strong sense of responsibility and mission, and show a spirit of dedication to overcome this epidemic.26 The nurses’ PSQI score was 15 (range 13–17). We found that 97.88% of the 236 nurses performing nucleic acid testing had sleep disturbances and their sleep quality was worse than that in other studies,27–37 in which the prevalence rate of sleep disturbance ranged from 12% to 87%. An analysis from Poland38 using multiple comparisons showed that the greatest intensity of insomnia was statistically significant in subjects who had contact with patients with COVID-19 or knew about it, which was significantly higher than in subjects who did not have contact (H (2) =17.48; p < 0.001). This could be because of the different investigated sources. For instance, nurses performing nucleic acid testing need to be on duty for 24 hours, and when they conduct nucleic acid testing in Zhangjiajie, they are faced with an extremely contagious disease in an unfamiliar environment. Some are worried about not adapting to their new sleeping, eating, and other lifestyle habits (37.29%). Another reason is the special epidemic situation—83.9% of nurses were worried about the delta strain taking longer to treat and recover and much more prone to severe illness, and 82.2% about occupational exposure to the delta strain because it is more transmissible and faster to replicate. Of the nurses, 80.3% were worried about their knowledge or ability to deal with the delta strain of COVID-19.
Existing research has shown that psychological problems in health workers during COVID-19 are higher than in past epidemics.39 The results indicated that the scores on the DASS-21 for depression, anxiety, and stress were 10.18±4.00, 11.67±4.49, and 13.32±5.59, respectively. A total of 219 nurses experienced stress and negative emotions. The results were different from that of a study in Qatar,40 which showed that most nurses had normal or mild symptoms severity of depression (96%), anxiety (86%), and stress (98%). These findings were consistent with previous findings in Wuhan, China, which is the first pandemic center for COVID-19. High levels of anger, stress, anxiety, and depression due to excessive work stress, direct exposure to COVID-19, and the possibility of infection.35 Some studies41,42 reported psychological problems because health workers were not immune to COVID-19, and failure to have the necessary care equipment caused a feeling of “lack of proper support.” This is inconsistent with our findings. Most nurses (193, 81.78%) performing nucleic acid testing in Zhangjiajie did not worry about insufficient supplies of protective materials, because the government organized adequate training and provided the necessary care equipment, and all of them were vaccinated against COVID-19. All nurses were originally trained and examined for COVID-19, used protective clothing, and performed nucleic acid testing.
The Spearman correlation analysis showed that sleep quality, latency, duration, efficiency, and disorders, diurnal dysfunction with anxiety, feelings of stress, and depression were positively correlated. The use of hypnotic drugs was correlated with negative emotional anxiety, stress, and depression. Multivariate analysis also showed that depression, anxiety, and feelings of stress were the three factors associated with sleep quality. No statistically significant differences were observed between the other variables. Similar to another investigation in China, including 512 medical staff fighting COVID-19, those who had close and direct contact with infected patients exhibited higher anxiety scores than those who did not.43 This is also consistent with many studies of COVID-19 showing that frontline health workers with anxiety and depression were more likely to develop sleep disturbance.44 In this study, we found that depression, anxiety, and stress negative emotions were the major reasons for sleep disruption. The current study showed that during the assistance period, 99.15% of nurses received humanistic care from the local government, and 95.34% of nurses received psychological support, although the government had made every endeavor to provide a good environment and ensure support for nurses to reduce depression, anxiety, and stress. However, the final intervention effect was not assessed, and 97.88% had sleep disorders, and only 63.56% received support during the assistance period. A study showed that progressive muscle relaxation training could reduce negative emotions and improve sleep quality.45 Similar to the findings, training, psychological support, humanistic care, sufficient protective equipment, and establishing a mental health team could reduce anxiety and depression levels and improve sleep quality.46 Therefore, the results show that we need not only multiple measures to improve sleep quality, but also to evaluate the intervention effect of nurses who perform nucleic acid tests.
Limitations
There are several limitations to this study. First, the precise number of physicians, nurses, and laboratory technicians has not been counted by the authority of the Zhangjiajie government, so the sample size cannot be calculated. Second, the total number of potential subjects was 1435, but only 275 individuals answered the survey, and four people were physicians and laboratory technicians, so the study could not compare the sleep disorders of nurses with those of other medical staff. Third, we did not conduct face-to-face interviews; only an online survey was used for safety and feasibility.
Conclusions
Sleep disturbance is a serious problem among nurses performing nucleic acid tests during the delta strain COVID-19 epidemic, especially among assistant nurses. Anxiety, stress, and depression are associated with sleep disorders, and multiple interventions should be implemented to improve sleep quality.
Ethics Statement
This was an online study, when open the web questionnaire, the preliminary remarks cleared the purpose, informed consent guidelines of the investigation, and if the participants carried out an investigation, standing for the participants provided informed consent, if the participants disapproval, they will not answer the web questionnaire. Ethical approval was issued by the Ethics Committee of The First People’s Hospital of Changde (2021-238-01), and the study was conducted according to the Helsinki Declaration of 1975, as revised in 2000.
Acknowledgments
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published; and agree to be accountable for all aspects of the work.
Funding
This research was supported by the Changde Science and Technology Bureau for Emergency Special Project of COVID-19 in Changde City, Hunan Province (2020SK003). If necessary, the data can be opened to the public.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Fauci AS, Lane HC, Redfield RR. Covid-19–Navigating the uncharted. New Engl J Med. 2020;382(13):1268–1269. doi:10.1056/NEJMe2002387
2. Lopez BJ, Andrews N, Gower C, et al. Effectiveness of Covid-19 vaccines against the B.1.617.2 (delta) variant. N Engl J Med. 2021;385(7):585–594. doi:10.1056/NEJMoa2108891
3. Planas D, Veyer D, Baidaliuk A, et al. Reduced sensitivity of SARS-CoV-2 variant Delta to antibody neutralization. Nature. 2021;596(7871):276–280. doi:10.1038/s41586-021-03777-9
4. Li XN, Huang Y, Wang W, et al. Effectiveness of inactivated SARS-CoV-2 vaccines against the Delta variant infection in Guangzhou: a test-negative case-control real-world study. Emerg Microbes Infect. 2021;10(1):1751–1759. doi:10.1080/22221751.2021.1969291
5. Li Q, Zhan X, Wang J, et al. Considerations and guidance to control the rebound in COVID-19 cases. Biosci Trends. 2021;15(5):341–344. doi:10.5582/bst.2021.01361
6. Yue L, Zhao R, Xiao Q, et al. The effect of mental health on sleep quality of front-line medical staff during the COVID-19 outbreak in China: a cross-sectional study. PLoS One. 2021;16(6):e253753. doi:10.1371/journal.pone.0253753
7. Lin YN, Liu ZR, Li SQ, et al. Burden of sleep disturbance during COVID-19 pandemic: a systematic review. Nature Sci Sleep. 2021;13:933–966. doi:10.2147/NSS.S312037
8. Vizheh M, Qorbani M, Arzaghi SM, et al. The mental health of healthcare workers in the COVID-19 pandemic: a systematic review. J DiabetMetabolDisord. 2020;19(2):1967–1978.
9. Salari N, Khazaie H, Hosseinian-Far A, et al. The prevalence of sleep disturbances among physicians and nurses facing the COVID-19 patients: a systematic review and meta-analysis. Globaliz Health. 2020;16(1):1–4.
10. Al-Dossary R, Alamri M, Albaqawi H, et al. Awareness, attitudes, prevention, and perceptions of COVID-19 outbreak among nurses in Saudi Arabia. Intern J Environ Res Pub Health. 2020;17(21):8269. doi:10.3390/ijerph17218269
11. Simonetti V, Durante A, Ambrosca R, et al. Anxiety, sleep disorders and self‐efficacy among nurses during COVID-19 pandemic: a large cross-sectional study. J Clin Nurs. 2021;30(9–10):1360–1371. doi:10.1111/jocn.15685
12. Magnavita N, Tripepi G, Di Prinzio RR. Symptoms in health care workers during the COVID-19 epidemic: a cross-sectional survey. Intern J Environ Res Public Health. 2020;17(14):5218. doi:10.3390/ijerph17145218
13. Trumello C, Bramanti SM, Ballarotto G, et al. Psychological adjustment of healthcare workers in Italy during the COVID-19 pandemic: differences in stress, anxiety, depression, burnout, secondary trauma, and compassion satisfaction between frontline and non-frontline professionals. Intern J Environ Res Public Health. 2020;17(22):8358. doi:10.3390/ijerph17228358
14. Hernández-Díaz Y, Genis-Mendoza AD, Fresán A, et al. Knowledge, emotions and stressors in front-line healthcare workers during the COVID-19 outbreak in Mexico. Intern J Environ Res Public Health. 2021;18(11):5622. doi:10.3390/ijerph18115622
15. Gupta S, Sahoo S. Pandemic and mental health of the front-line healthcare workers: a review and implications in the Indian context amidst COVID-19. Gen Psychiatry. 2020;33(5):e100284. doi:10.1136/gpsych-2020-100284
16. Mo Y, Deng L, Zhang L, et al. Work stress among Chinese nurses to support Wuhan in fighting against COVID-19 epidemic. J NursManag. 2020;28(5):1002–1009.
17. Jiang F, Xiao Y, Dong H, et al. Sleep quality in medical staffs during the outbreak of coronavirus disease 2019 in China: a web-based cross-sectional study. Front Psychiatry. 2021;12. doi:10.3389/fpsyt.2021.630330
18. Buysse DJ, Reynolds CR, Monk TH, et al. The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res. 1989;28(2):193–213. doi:10.1016/0165-1781(89)90047-4
19. Zhang C, Zhang H, Zhao M, et al. Reliability, validity, and factor structure of Pittsburgh Sleep Quality Index in community-based centenarians. Front Psychiatry. 2020;11:573530. doi:10.3389/fpsyt.2020.573530
20. Yan DQ, Huang YX, Chen X, et al. Application of the Chinese version of the Pittsburgh Sleep Quality Index in people living with HIV: preliminary reliability and validity. Front Psychiatry. 2021;12:676022. doi:10.3389/fpsyt.2021.676022
21. Lovibond PF, Lovibond SH. The structure of negative emotional states: comparison of the Depression Anxiety Stress Scales (DASS) with the beck depression and anxiety inventories. Behav Res Ther. 1995;33(3):335–343. doi:10.1016/0005-7967(94)00075-U
22. Jiang LC, Yan YJ, Jin ZS, et al. The depression anxiety stress scale-21 in Chinese hospital workers: reliability, latent structure, and measurement invariance across genders. Front Psychol. 2020;11:247. doi:10.3389/fpsyg.2020.00247
23. R Core Team. R: a Language and environment for statistical computing. (Version 4.0) [Computer software]; 2021. Available from: https://cran.r-project.org. (R packages retrieved from MRAN snapshot 2021-04-01).
24. Chong MY, Wang WC, Hsieh WC, et al. Psychological impact of severe acute respiratory syndrome on health workers in a tertiary hospital. Br J Psychiatry. 2004;185:127–133. doi:10.1192/bjp.185.2.127
25. Chen Y, Zhang Y, Jin R. Professional identity of male nursing students in 3-year colleges and junior male nurses in China. Am J Mens Health. 2020;14(4):1819214471. doi:10.1177/1557988320936583
26. Liu YE, Zhai ZC, Han YH, et al. Experiences of front-line nurses combating coronavirus disease-2019 in China: a qualitative analysis. Public Health Nurs. 2020;37(5):757–763. doi:10.1111/phn.12768
27. Rossi R, Socci V, Pacitti F, et al. Mental health outcomes among frontline and second-line health care workers during the coronavirus disease 2019 (COVID-19) pandemic in Italy. JAMA Network Open. 2020;3(5):e2010185. doi:10.1001/jamanetworkopen.2020.10185
28. Jahrami H, BaHammam AS, AlGahtani H, et al. The examination of sleep quality for frontline healthcare workers during the outbreak of COVID-19. Sleep Breath. 2021;25(1):503–511. doi:10.1007/s11325-020-02135-9
29. Lai J, Ma S, Wang Y, et al. Factors associated with mental health outcomes among health care workers exposed to coronavirus disease 2019. JAMA Network Open. 2020;3(3):e203976. doi:10.1001/jamanetworkopen.2020.3976
30. Zhan Y, Liu Y, Liu H, et al. Factors associated with insomnia among Chinese front-line nurses fighting against COVID-19 in Wuhan: a cross-sectional survey. J NursManag. 2020;28(7):1525–1535.
31. Pan X, Xiao Y, Ren D, et al. Prevalence of mental health problems and associated risk factors among military healthcare workers in specialized COVID-19 hospitals in Wuhan, China: a cross-sectional survey. Asia Pac Psychiatry;2020. e12427. doi:10.1111/appy.12427
32. Wang S, Xie L, Xu Y, et al. Sleep disturbances among medical workers during the outbreak of COVID-2019. Occup Med. 2020;70(5):364–369. doi:10.1093/occmed/kqaa074
33. Tu ZH, He JW, Zhou N. Sleep quality and mood symptoms in conscripted frontline nurse in Wuhan, China during COVID-19 outbreak: a cross-sectional study. Medicine. 2020;99(26):e20769. doi:10.1097/MD.0000000000020769
34. Que J, Shi L, Deng J, et al. Psychological impact of the COVID-19 pandemic on healthcare workers: a cross-sectional study in China. Gen Psychiatry. 2020;33(3):e100259. doi:10.1136/gpsych-2020-100259
35. Zhang C, Yang L, Liu S, et al. Survey of insomnia and related social psychological factors among medical staff involved in the 2019 novel coronavirus disease outbreak. Front Psychiatry. 2020;11:306.
36. Zhang WR, Wang K, Yin L, et al. Mental health and psychosocial problems of medical health workers during the COVID-19 epidemic in China. PsychotherPsychosom. 2020;89(4):242–250.
37. Zhou Y, Yang Y, Shi T, et al. Prevalence and demographic correlates of poor sleep quality among frontline health professionals in Liaoning Province, China during the COVID-19 outbreak. Front Psychiatry. 2020;11:520. doi:10.3389/fpsyt.2020.00520
38. Krupa S, Filip D, Mędrzycka-Dąbrowska W, et al. Sleep disorders among nurses and other health care workers in Poland during the COVID-19 pandemic. Appl Nurs Res. 2021;59:151412. doi:10.1016/j.apnr.2021.151412
39. Dong ZQ, Ma J, Hao YN, et al. The social psychological impact of the COVID-19 pandemic on medical staff in China: a cross-sectional study. Eur Psychiatry. 2020;63(1):e65. doi:10.1192/j.eurpsy.2020.59
40. Nashwan AJ, Villar RC, Al-Qudimat AR, et al. Quality of life, sleep quality, depression, anxiety, stress, eating habits, and social bounds in nurses during the coronavirus disease 2019 pandemic in Qatar (The PROTECTOR Study): a Cross-Sectional, Comparative Study. J Pers Med. 2021;11(9):918. doi:10.3390/jpm11090918
41. Spoorthy MS, Pratapa SK, Mahant S. Mental health problems faced by healthcare workers due to the COVID-19 pandemic-A review. Asian J Psychiatr. 2020;51:102119. doi:10.1016/j.ajp.2020.102119
42. Salari N, Mohammadi M, Vaisi-Raygani A, et al. The prevalence of severe depression in Iranian older adults: a meta-analysis and meta-regression. BMC Geriatr. 2020;20(1):39. doi:10.1186/s12877-020-1444-0
43. Liu CY, Yang YZ, Zhang XM, et al. The prevalence and influencing factors in anxiety in medical workers fighting COVID-19 in China: a cross-sectional survey. Epidemiol Infect. 2020;148:e98. doi:10.1017/S0950268820001107
44. Li Q, Chen J, Xu G, et al. The psychological health status of healthcare workers during the COVID-19 outbreak: a cross-sectional survey study in Guangdong, China. Front Public Health. 2020;8:562885. doi:10.3389/fpubh.2020.562885
45. Liu K, Chen Y, Wu D, et al. Effects of progressive muscle relaxation on anxiety and sleep quality in patients with COVID-19. Complement Ther Clin Pract. 2020;39:101132. doi:10.1016/j.ctcp.2020.101132
46. Chung J. Social support, social strain, sleep quality, and actigraphic sleep characteristics: evidence from a national survey of US adults. Sleep Health. 2017;3(1):22–27. doi:10.1016/j.sleh.2016.10.003
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
