Back to Journals » International Journal of Chronic Obstructive Pulmonary Disease » Volume 15
Serum IL-8 and VEGFA are Two Promising Diagnostic Biomarkers of Asthma-COPD Overlap Syndrome
Authors Ding Q, Sun S, Zhang Y, Tang P, Lv C , Ma H, Yu Y, Xu S, Deng Z
Received 4 October 2019
Accepted for publication 1 February 2020
Published 13 February 2020 Volume 2020:15 Pages 357—365
DOI https://doi.org/10.2147/COPD.S233461
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Chunxue Bai
Qunli Ding,1 Shifang Sun,1 Yun Zhang,1 Pan Tang,1 Chengna Lv,1 Hongying Ma,1 Yiming Yu,1 Suling Xu,2 Zaichun Deng1
1Department of Pulmonary and Critical Care Medicine, The Affiliated Hospital of Medical School of Ningbo University, Ningbo, People’s Republic of China; 2Department of Dermatology, The Affiliated Hospital of Medical School of Ningbo University, Ningbo, People’s Republic of China
Correspondence: Zaichun Deng
Department of Pulmonary and Critical Care Medicine, The Affiliated Hospital of Medical School of Ningbo University, No. 247, Renmin Road, Jiangbei District, Ningbo, Zhejiang Province, People’s Republic of China
Tel/Fax +86 57487035780
Email [email protected]
Background: Asthma-COPD overlap (ACO; previously referred to as asthma-COPD overlap syndrome) is characterized by persistent airflow limitation consistent with COPD, together with several distinguishing features of asthma. Asthma-COPD overlap syndrome is a condition of mixing symptoms of asthma and COPD, because of its complexity, it is difficult to find effective diagnostic markers in clinic.
Purpose: Our aims were to detect the expression of serum cytokines in patients with asthma, explore the diagnostic potential of differential serum cytokines in ACOS.
Patients and Methods: Ninety asthmatic patients were divided into ACOS group and non-ACOS group according to the major and minor criteria of ACOS, 15 kinds of cytokines including IL-3, IL-4, IL-8, IL-9, IL-13, IL-17A, VEGFA, VEGFC, VEGFD, bFGF, Fit-1 PIGF, Tie-2 were detected by MSD, and IL-27 and TGF-beta were determined by ELISA assay.
Results: The serum levels of IL-9, VEGFA and PIGF in patients with ACOS were significantly higher than those in non-ACOS group (P< 0.05, respectively), while the level of IL-8 and IL-17A in subjects with ACOS was lower than that in the non-ACOS group (P< 0.05, respectively). We analyzed the correlation between several difference factors and FEV1/FVC% in the ACOS group, found VEGFA was negatively correlated with FEV1/FVC%, while IL-8 and IL-17A were positively correlated with FEV1/FVC%. Finally, three correlation factors were analyzed by ROC curve for the occurrence of ACOS.
Conclusion: The results suggested that IL-8 was highly sensitive and VEGFA was highly specificity, both of which could be used as biomarkers for the diagnosis of ACOS.
Keywords: asthma, ACOS, biomarker, IL-8, VEGF-A
Introduction
Asthma and COPD are chronic inflammatory respiratory disease characterized by inflammation and excess mucus production. Many studies have confirmed that they have different inflammatory response, generally speaking, asthma is an eosinophil-dominant inflammation driven by TH2 cytokines,1 while COPD is a neutrophil- and macrophage-dominant inflammatory process driven by TH1 cytokines.2 Clinically, a part of smokers with severe asthma associated with long-term airway obstruction, which is characterized by airway remodeling and increased neutrophil counts. These asthmatic patients who also manifest the symptoms of COPD are diagnosed with asthma-COPD overlap syndrome (ACOS).3,4 Meanwhile, patients with COPD with good obstruction reversibility, whereas increased eosinophil counts, can also be classified as ACOS.5 Most ACOS patients are elderly and manifest the symptoms of both asthma and COPD.6 The literatures suggest that ACOS is associated with more rapid decline in lung function, more frequent exacerbations, worsening quality of life and higher mortality rates compared with asthma or COPD.7 It is important to distinguish ACOS from asthma or COPD. In fact, the clinical phenotypes and mechanism of ACOS are still in a vague state. Although several diagnostic criteria, such as the modified Spanish criteria8 and American Thoracic Society Roundtable criteria, have been established for ACOS, its exact definition has not been established.9 Currently, the main criteria for an asthmatic patient to be diagnosed with ACOS are as follows: (a) persistence over time of airflow obstruction (FEV1/FVC<0.7 or <LLN) and (b) exposure to noxious particles or gases, with ≥10 pack-years for smokers.10 However, there are no effective methods to distinguish ACOS and “pure” asthma or COPD yet.
Although the concept of ACOS has been around for a long time, the question of whether ACOS is simply the additive result of asthma and COPD, or whether multiple environmental factors contribute to the progression of a single asthma/COPD patient to another disease has not been well answered. According to the Dutch hypothesis,11 single asthmatic/COPD patients with airway obstruction will progress to ACOS as a result of the combined mechanisms of action of exogenous and endogenous factors, including genes, gender, age, allergens, smoking, air pollution, infection and inflammation, response to treatment and clinical course.12 However, considering that ACOS is associated with inflammatory processes, it is significantly important to study the roles of inflammatory cytokine levels in the development of this disease. In this study, the expression of various inflammatory factors, VEGF family members and other related factors in the serum of patients with ACOS were analyzed by MSD detection to investigate the biological mechanisms of these different factors in establishing the diagnosis of ACOS.
Patients and Methods
Subjects
Ninetyasthmatic subjects and 40 normal controls were recruited through the Department of Respiration, The Affiliated Hospital of Medical School of Ningbo University. All patients provided written informed consent for their samples to be used in related approved studies, and this study was approved by the local ethics committee (Institutional Review Board approval number: KY20170309). All of the patients had a clear history of asthmatic symptoms. Patients with asthma met the definition of the Global Initiative for Asthma.13 Based on Cataldo et al14 summarized the classification of ACOS patients in asthma patients, and we divided asthmatic patients into ACOS group and non-ACOS group. The classification method included major criteria and minor criteria. The major criteria of ACOS in an asthmatic patient were as follows: (1) exposure to noxious gases, with ≥10 pack-years for smokers. (2) airflow obstruction for over time (FEV1/FVC<0.7 or <lower limit of normal). Meanwhile, the minor criteria of ACOS in an asthma patient: (1) no response on acute bronchodilator test; (2) reduced lung diffusion capacity; (3) age>40 years; (4) emphysema present on chest CT scan; (5) little variability obstruction. An asthmatic patient who met the two major criteria and at least one minor criterion was classified as ACOS group. Specifically, ACOS was diagnosed if patients with asthma were older than 40 years old, had post-bronchodilator forced FEV1/FVC <0.7, and fulfilled at least one of the following criteria, including more than 10 pack-years’ smoking history, less than 80% of diffusing capacity of the lung for carbon monoxide (DLCO)/alveolar volume, and presence of low attenuation area or emphysema on high resolution computed tomography (HRCT). Normal control subjects were healthy lifelong volunteers who had no history of lung disease. Healthy controls were also age and gender matched with the patients.
Analysis of Cytokines
All of serum was separated from the anticoagulant blood by centrifugation (1500rpm, 10 mins) at 4°C. A Meso Scale Discovery system (Meso Scale Diagnostics, Rockville, MD) was used to measure concentrations of interleukin(IL)-4,-5-8,-9,-13,-17A (base catalog number K15067L-1 for human assay, sensitivity of <0.6 pg/mL), and Flt-1(VEGFR-1, sensitivity of <0.6 pg/mL), placental growth factor (PIGF, sensitivity of <0.6 pg/mL), TEK receptor tyrosine kinase (Tie-2, sensitivity of <0.6 pg/mL), vascular endothelial growth factor-A, -C, -D (VEGF-A, -C, -D, sensitivity of <0.6 pg/mL, respectively), fibroblast growth factor 2 (bFGF) (Cat numbers: K15190G-1 for human assay, sensitivity of <0.6 pg/mL), transforming growth factor beta 1 (TGF-beta1), IL-27 were determined by ELISA assay (Cat numbers: SEA385HU, SEA123HU 96T, respectively, Sensitivity of <0.6 pg/mL).
Ethical Statement
The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was approved by The Affiliated Hospital of Medical School of Ningbo University Ethics Committee. This study was conducted in accordance with the Declaration of Helsinki, and all subjects provided written informed consent for inclusion in the study.
Statistical Analysis
Data were analyzed with the aid of commercially available statistical packages (SPSS Statistics software, version 19.0, GraphPad Prism6). Enumeration data were expressed as percentage, whereas measurement data were expressed as mean ± standard error of mean(SEM) or median with quartile range. Between-group ANOVA (Kruskal–Wallis) was followed by the Mann–Whitney U-test with Bonferroni correction. Correlation coefficients were obtained by the Spearman rank-order method with correction for tied values. A receiver operating characteristic (ROC) curves were allowed for sensitivity and specificity analysis obtained by SPSS 19.0. For all tests, P<0.05 was considered significant.
Results
Clinical Data
A total of 90 patients were enrolled in this study. According to the diagnostic criteria, 69 patients had asthma (non-ACOS) and 21 patients had ACOS. The clinical characteristics of the subjects are shown in Table 1. Patient with ACOS had significantly more tobacco smoking pack-years than patients with non-ACOS. The frequency of cough, dyspnea and wheezing between ACOS and non-ACOS was statistically insignificant, while the frequency of phlegm was significantly higher in the ACOS than that in the non-ACOS group. The total serum immunoglobulin E(IgE) was higher in the ACOS group than that in the non-ACOS group. We detected the VEGFA expression in the serum and found that the mean of VEGFA expression in asthmatic subjects (758.2pg/mL±72.31) was significantly higher than that in the control group (42.21pg/mL±7.781) (P<0.0001). The median prebronchodilator FEV1 (percent predicted) of asthmatic patients (Median 77.25%, range 52.36–103.2%) was lower than that in the control group (Median 105.5%, range 79.8–110.3%) (P<0.05). However, FEV1/FVC ratio in both groups had no significant difference. Based on the ACOS classification requirements, we divided asthmatic subjects into ACOS group and non-ACOS group. In ACOS group, all of the patients had smoking history, and the median FEV1% and FEV1/FVC in the ACOS group (52.36%, range 45.34–68.23%; 0.651, range 0.63–0.78) were significantly lower than those in the non-ACOS group (87.43%, range 64.33–100.01%; 0.822, range 0.69–0.89) (P<0.05) and control group (Median 105.5%, range 79.8–110.3%; 0.823, range 0.71–0.98) (P<0.05), respectively. The concentration of VEGFA in asthmatic group was significantly higher than that in the control group (P<0.0001), and the FEV1/FVC% of all subjects in the ACOS group were lower than 70% compared with the other groups, P<0.001 (Table 1).
 |
Table 1 The General Biochemical Indicators Compared Among Control Group, ACOS Group and Non-ACOS |
Cytokines in Serum of ACOS Patients
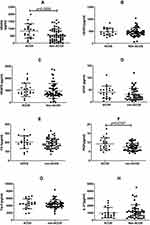
We tested seven types of cytokines in serum of asthmatic patients, including IL-4, IL-5, IL-8, IL-9, IL-13, IL-17A and IL-27. As the results, IL-8 in the serum of ACOS group was lower than that in the non-ACOS group (128.8pg/mL±22.26 versus1028pg/mL±286) (P=0.0439). The concentration of IL-9 in the serum of ACOS group (Mean±SEM: 1.97pg/mL±0.247) was significantly higher than that in the non-ACOS group (Mean±SEM:1.252pg/mL±0.1033) (P=0.0023). Meanwhile, the mean of concentration of IL-17A in the non-ACOS group was 11.88pg/mL, which was higher than that in the ACOS group (Mean±SEM:4.96pg/mL±0.957) (P=0.0227) (Figure 1).
Angiogenesis Related Factors of VEGFA and PIGF Were Increased in Serum of ACOS Patients
We choice VEGFA, VEGFC, VEGFD, bFGF, Flt-1, PIGF and Tie-2, which were related with angiogenesis, to detect the concentration of those in serum between ACOS group and non-ACOS group. The result displayed the concentration of VEGFA and PIGF in the ACOS group were significantly higher than those in the non-ACOS group (Mean±SEMVEGFA of non-ACOS group: 561.3pg/mL±58.25 vs Mean±SEMVEGFA ofACOS group: 844.4pg/mL±114.8) (P=0.0205), (Mean±SEMPIGF of non-ACOS group: 7.438pg/ml±0.309 vs. Mean±SEMPIGF of ACOS group: 9.226pg/mL±0.755) (P=0.0107), respectively (Figure 2).
Relationships Between Concentrations of Serum VEGFA, Cytokines IL-8 and IL-17A and FEV1/FVC%
The serum concentrations of VEGFA in the ACOS subjects were correlated inversely with lung function (FEV1/FVC1%)(all ACOS patients: VEGFA r=−0.343, P=0.017) (Figure 3A), however, the concentration of cytokines IL-17A and IL-8 in the ACOS group was positively correlated with FEV1/FVC% (IL-17A r=0.304, P=0.036; IL-8 r=0.44, P=0.002) (Figure 3B and C).
Serum IL-8 and VEGFA May Be the AOCS Biomarkers
The sensitivity and specificity of serum IL-8 and VEGFA as biomarkers were analyzed using the ROC curve to confirm their ability to discriminate ACOS from non-ACOS in total asthma (Figure 4A). The ROC curve demonstrated by IL-8 obtained an area under the curve of 0.676, with a cutoff value of 167.5 to discriminate ACOS from non-ACOS. Additionally, VEGFA obtained an area under the curve of 0.649, with a cutoff value of 909.85 (Figure 4B). IL-8 had a sensitivity of 80% and a specificity of 58.5%, while VEGFA had a sensitivity of 60% and a specificity of 80.8%.
 |
Figure 4 ROC curve for discriminating ACOS from non-ACOS using IL-8 (A) and VEGFA (B). Abbreviations: ROC, receiver operating characteristic; VEGFA, vascular endothelial growth factor-A. |
Discussion
Our study showed the difference between ACOS and asthma. ACOS and asthmatic patients had similar demographic profiles; however, the frequency of phlegm in the ACOS group was significantly higher than that in the non-ACOS group. Similarly, asthma and COPD medications were more frequently administered in ACOS patients than in non-ACOS patients, but based on the results, there were no statistically significant differences between the two groups. Long-acting muscarinic antagonist was more frequently administered in ACOS patients than in non-ACOS patients, and the inhaled corticosteroid/long-acting beta-2 agonist (ICS/LABA) inhaler was more frequently used by asthmatic patients than by ACOS patients. Our results revealed significantly higher levels of total IgE in ACOS patients compared with asthmatic patients, which was considered an unexpected finding considering the differences in the treatment drugs. This finding is consistent with the results of Chen et al.15 Another study showed significantly higher concentrations of total IgE in asthma compared with ACOS.16
Compared with single asthma or single COPD, ACOS is more complex and includes the symptoms of both asthma and COPD. Different diseases require different conditions to develop ACOS. For an asthmatic patient with a long history of smoking or long-term exposure to air pollution,17,18 combined with pulmonary CT scan revealing emphysema and low ventilation volume,19 the diagnosis of ACOS is established. However, for a COPD patient, COPD may progress to ACOS if airway hyperresponsiveness20,21 or airway remodeling and airway inflammation22,23 are observed. Therefore, the definition of ACOS is still unclear in clinical practice.
IL-8 is an effective neutrophil chemoattractant and activator that is released from macrophages, neutrophils, bronchial smooth muscle cells, and epithelial cells (Mio, 1997 #272). When inflammatory occurs, neutrophils are able to enforce their own recruitment by the production of IL-8.24 The concentration of sputum IL-8 was increased in an established COPD, and IL-8 was associated with lung function in COPD patients. A previous study found that non-Th2-related cytokines such as IL-8 were higher in ACOS compared with asthma.25 Meanwhile, Chalmers et al (2001) found that smoking history in asthmatic patients had a positive correlation with IL-8, and a negative correlation between FEV1 and sputum IL-8 was observed.26 In our study, we found that the serum concentration of IL-8 was decreased in the ACOS group, and a positive correlation between serum IL-8 and FEV1/FVC was observed. A recent study showed that neither IL-8 nor IL-5/IL-8 produced sufficient sensitivity and specificity to accurately identify the various diagnostic categories of asthma, COPD, and ACOS. The area under the ROC curve was <0.7 in every case. However, in this study, we found that serum IL-8 had high sensitivity (80%) in the ROC curve. Although the serum level of IL-8 in the ACOS group was lower than that in the non-ACOS group, which was not consistent with the hypothesis, the level of IL-8 was positively correlated with FEV1/FVC, which was consistent with the results of several experiments. The reason for this result had not been studied in depth, which may be related to the small sample size and more ACOS patients in this study had been treated with ICS/LABA inhaler.
VEGF is a glycosylated peptide factor that belongs to the platelet-derived growth factor family. VEGF family members include VEGF-A, VEGF-B, VEGF-C, VEGF-E, and PIGF.27 VEGF is generally expressed in tissues rich in blood vessels, such as the trachea of the lung tissue.28 Meanwhile, VEGF can be produced by inflammatory cells including neutrophils, lymphocytes, monocytes, and eosinophils. It is well known that VEGF plays an important role in airway remodeling, and several studies have shown that VEGF expression is significantly increased in the serum of asthmatic and/or COPD patients.29 However, based on the result of our study, a negative correlation between serum VEGF-A and FEV1/FVC was observed, which might be possibly related to emphysema observed in ACOS in asthmatic patients. It had been clearly reported that the concentration of VEGFA and its receptor VEGFR2 significantly decreased in emphysema. Moreover, increased serum VEGFA had a high specificity (80.8%) in the ACOS group.
In this study, serum IL-8 and VEGFA levels in ACOS patients showed high specificity and sensitivity, but considering the wide expression of IL-8 and VEGF-A in most tissues, it is necessary to identify more specific diagnostic biomarkers of ACOS in the follow-up studies.
Conclusion
Considering that serum IL-8 has high sensitivity and VEGF-A has high specificity, both of them could be used as diagnostic biomarkers of ACOS.
Abbreviations
ACOS, asthma-chronic obstructive pulmonary disease overlap syndrome; VEGF-A, -C, -D, vascular endothelial growth factor-A, vascular endothelial growth factor-C, vascular endothelial growth factor-D; bFGF, fibroblast growth factor 2; Flt-1, VEGFR-1; PIGF, placental growth factor; Tie-2, TEK receptor tyrosine kinase.
Data Sharing
Since no additional data were available in our study, please contact the corresponding author for the analysis dataset.
Acknowledgments
This work was supported by a grant from the Natural Science Foundation of Zhejiang (No.LY15H010004, QL Ding) and a grant from the Natural Science Foundation of Ningbo (No.2014A610279, QL Ding). Moreover, there were no competing interests in this case.
Author Contributions
All authors contributed to data analysis, drafting or revising the article, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Disclosure
The authors have no conflicts of interest to declare.
References
1. Fabbri LM, Romagnoli M, Corbetta L, et al. Differences in airway inflammation in patients with fixed airflow obstruction due to asthma or chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2003;167:418–424. doi:10.1164/rccm.200203-183OC
2. O’Donnell R, Breen D, Wilson S, Djukanovic R. Inflammatory cells in the airways in COPD. Thorax. 2006;61(5):448–454. doi:10.1136/thx.2004.024463
3. Alshabanat A, Zafari Z, Albanyan O, et al. Asthma and COPD Overlap Syndrome (ACOS): a systematic review and meta analysis. PLoS One. 2015;10(9):e0136065. doi:10.1371/journal.pone.0136065
4. Bellanti JA, Settipane RA. For the patient. The asthma-COPD overlap syndrome (ACOS): is it asthma? Is it COPD? Or is it both? Allergy Asthma Proc. 2015;36(1):87. doi:10.2500/aap.2015.36.3815
5. Bell MC, Busse WW. Is it asthma or is it COPD: the overlap syndrome. J Allergy Clin Immunol Pract. 2015;3(4):641–642. doi:10.1016/j.jaip.2014.11.003
6. Postma DS, Rabe KF. The asthma-COPD overlap syndrome. N Engl J Med. 2015;373(13):1241–1249. doi:10.1056/NEJMra1411863
7. Vaz Fragoso CA, Murphy TE, Agogo GO, Allore HG, McAvay GJ. Asthma-COPD overlap syndrome in the US: a prospective population-based analysis of patient-reported outcomes and health care utilization.nt. J Chron Obstruct Pulmon Dis. 2017;12(3):517–527. doi:10.2147/COPD.S121223
8. Cosio BG, Soriano JB, López-Campos JL, et al. Defining the asthma-COPD overlap syndrome in a COPD cohort. Chest. 2016;149:45–52. doi:10.1378/chest.15-1055
9. Sin DD, Miravitlles M, Mannino DM, et al. What is asthma-COPD overlap syndrome? Towards a consensus definition from a round table discussion. Eur Respir J. 2016;48:664–673. doi:10.1183/13993003.00436-2016
10. Leung JM, Sin DD. Asthma-COPD overlap syndrome: pathogenesis, clinical features, and therapeutic targets. BMJ. 2017;358:j3772. doi:10.1136/bmj.j3772
11. Sluiter HJ, Koeter GH, de Monchy JG, et al. The Dutch hypothesis (chronic non-specific lung disease) revisited. Eur Respir J. 1991;4(4):479–489.
12. Jin J, Liu X, Sun Y. The prevalence of increased serum IgE and Aspergillus sensitization in patients with COPD and their association with symptoms and lung function. Respir Res. 2014;15:130. doi:10.1186/s12931-014-0130-1
13. Oline appendix of global strategy for asthma management and prevention; 2018. Available from: http://ginasthma.org.
14. Cataldo D, Corhay JL, Derom E, et al. A Belgian survey on the diagnosis of asthma-COPD overlap syndrome. Int J Chron Obstruct Pulmon Dis. 2017;12:601–613. doi:10.2147/COPD.S124459
15. Chen FJ, Lin GP, Huang XY, et al. Evaluation of the characteristics of asthma in severe and extremely severe COPD. Int J Chron Obstruct Pulmon Dis. 2019;14(3):2663–2671. doi:10.2147/COPD.S225258
16. Cheng WC, Wu BR, Liao WC, et al. Clinical predictors of the effectiveness of tiotropium in adults with symptomatic asthma: a real-life study. J Thorac Dis. 2018;10(6):3661–3669. doi:10.21037/jtd.2018.05.139
17. Bowatte G, Lodge CJ, Lowe AJ, et al. Do variants in GSTs modify the association between traffic air pollution and asthma in adolescence? Int J Mol Sci. 2016;17(4):485. doi:10.3390/ijms17040485
18. Nadeau K, McDonald-Hyman C, Noth EM, et al. Ambient air pollution impairs regulatory T-cell function in asthma. J Allergy Clin Immunol. 2010;126(4):845–852. doi:10.1016/j.jaci.2010.08.008
19. Gelb AF, Yamamoto A, Mauad T, et al. Unsuspected mild emphysema in nonsmoking patients with chronic asthma with persistent airway obstruction. J Allergy Clin Immunol. 2014;133(1):263–265. doi:10.1016/j.jaci.2013.09.045
20. Hogg JC, Chu F, Utokaparch S, et al. The nature of small-airway obstruction in chronic obstructive pulmonary disease. N Engl J Med. 2004;350(26):2645–2653. doi:10.1056/NEJMoa032158
21. Cockcroft DW, Wenzel S. Airway hyperresponsiveness and chronic obstructive pulmonary disease outcomes. J Allergy Clin Immunol. 2016;138:1580–1581. doi:10.1016/j.jaci.2016.06.039
22. Hodge G, Nairn J, Holmes M, et al. Increased intracellular T helper 1 proinflammatory cytokine production in peripheral blood, bronchoalveolar lavage and intraepithelial T cells of COPD subjects. Clin Exp Immunol. 2007;150(1):22–29. doi:10.1111/j.1365-2249.2007.03451.x
23. Singh D, Kolsum U, Brightling CE, et al. Eosinophilic inflammation in COPD: prevalence and clinical characteristics. Eur Respir J. 2014;44(6):1697–1700. doi:10.1183/09031936.00162414
24. John M, Au BT, Jose PJ, et al. Expression and release of interleukin-8 by human airway smooth muscle cells: inhibition by Th-2 cytokines and corticosteroids. Am J Respir Cell Mol Biol. 1998;18(1):84–90. doi:10.1165/ajrcmb.18.1.2813
25. De Llano LP, Cosío BG, Iglesias A, et al. Mixed Th2 and non-Th2 inflammatory pattern in the asthma-COPD overlap: a network approach. Int J Chron Obstruct Pulmon Dis. 2018;13(12):591–601. doi:10.2147/COPD.S153694
26. Chalmers GW, MacLeod KJ, Thomson L, et al. Smoking and airway inflammation in patients with mild asthma. Chest. 2001;120(6):1917–1922. doi:10.1378/chest.120.6.1917
27. Zhao X, Yu FQ, Huang XJ, et al. Azithromycin influences airway remodeling in asthma via the PI3K/Akt/MTOR/HIF-1alpha/VEGF pathway. J Biol Regul Homeost Agents. 2018;32(5):1079–1088.
28. Lu HY, Zhao GL, Fu MF. Polymorphisms in the vascular endothelial growth factor (VEGF) gene associated with asthma. Genet Mol Res. 2016;15(2). doi:10.4238/gmr.15027880
29. Zha W, Su M, Huang M, et al. Administration of pigment epithelium-derived factor inhibits airway inflammation and remodeling in chronic OVA-induced mice via VEGF suppression. Allergy Asthma Immunol Res. 2016;8(2):161–169. doi:10.4168/aair.2016.8.2.161
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.