Back to Journals » International Journal of General Medicine » Volume 7
Reasons for encounter and diagnoses of new outpatients at a small community hospital in Japan: an observational study
Authors Takeshima T, Kumada M, Mise J, Ishikawa Y, Yoshizawa H, Nakamura T, Okayama M, Kajii E
Received 13 February 2014
Accepted for publication 16 March 2014
Published 5 June 2014 Volume 2014:7 Pages 259—269
DOI https://doi.org/10.2147/IJGM.S62384
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Taro Takeshima,1,2 Maki Kumada,3,4 Junichi Mise,5 Yoshinori Ishikawa,6 Hiromichi Yoshizawa,4 Takashi Nakamura,3,4 Masanobu Okayama,1 Eiji Kajii1
1Division of Community and Family Medicine, Center for Community Medicine, Jichi Medical University, Shimotsuke, Japan; 2Department of Healthcare Epidemiology, School of Public Health in the Graduate School of Medicine, Kyoto University, Kyoto, Japan; 3Division of The Project for Integration of Community Health, Center for Community Medicine, Jichi Medical University, Shimotsuke, Japan; 4Department of General Internal Medicine, Chikusei City Hospital, Chikusei, Japan; 5Division of Human Resources Development for Community Medicine, Center for Community Medicine, Jichi Medical University, Shimotsuke, Japan; 6Department of Surgery, Chikusei City Hospital, Chikusei, Japan
Purpose: Although many new patients are seen at small hospitals, there are few reports of new health problems from such hospitals in Japan. Therefore, we investigated the reasons for encounter (RFE) and diagnoses of new outpatients in a small hospital to provide educational resources for teaching general practice methods.
Methods: This observational study was conducted at the Department of General Internal Medicine in a small community hospital between May 6, 2010 and March 11, 2011. We classified RFEs and diagnoses according to component 1, “Symptoms/Complaints”, and component 7, “Diagnosis/Diseases”, of the International Classification of Primary Care, 2nd edition (ICPC-2). We also evaluated the differences between RFEs observed and common symptoms from the guidelines Model Core Curriculum for Medical Students and Goals of Clinical Clerkship.
Results: We analyzed the data of 1,515 outpatients. There were 2,252 RFEs (1.49 per encounter) and 170 ICPC-2 codes. The top 30 RFE codes accounted for 80% of all RFEs and the top 55 codes accounted for 90%. There were 1,727 diagnoses and 196 ICPC-2 codes. The top 50 diagnosis codes accounted for 80% of all diagnoses, and the top 90 codes accounted for 90%. Of the 2,252 RFEs, 1,408 (62.5%) included at least one of the 36 symptoms listed in the Model Core Curriculum and 1,443 (64.1%) included at least one of the 35 symptoms in the Goals of Clinical Clerkship. On the other hand, “A91 Abnormal result investigation”, “R21 Throat symptom/complaint”, and “R07 Sneezing/nasal congestion”, which were among the top 10 RFEs, were not included in these two guidelines.
Conclusion: We identified the common RFEs and diagnoses at a small hospital in Japan and revealed the inconsistencies between the RFEs observed and common symptoms listed in the guidelines. Our findings can be useful in improving the general practice medical education curricula.
Keywords: general practice, primary care, medical education, International Classification of Primary Care
Introduction
Primary care practice contributes to lower mortality.1 One of the important roles of primary care practice is the early management of new health problems.2 In addition, the registration of primary care-based morbidity is essential for the surveillance of disease, clinical research, and general practice teaching and curricula.3 Analysis of the reasons for encounter (RFE) and diagnoses of new outpatients contribute to the educational resources regarding general practice for medical students and residents.4–6
The World Organization of Family Doctors (WONCA) created the International Classification of Primary Care (ICPC) in 1987, and the second edition (ICPC-2) was published in 1998. The ICPC is widely used in general practice for the classification of three important elements of the health care encounter: RFEs, diagnoses or problems, and processes of care. The ICPC is based on a simple biaxial structure: 17 chapters detailing body systems, each with an alphabetical identifier (A, B, D, F, H, K, L, N, P, R, S, T, U, W, X, Y, Z), comprise the first axis, and seven components with rubrics bearing two-digit numeric codes comprise the second axis.7,8 Several studies have examined RFEs and diagnoses in general practice settings worldwide (the Netherlands, Malta, Serbia, Denmark, South Korea, South Africa, Tunisia, Poland, People’s Republic of China, and Japan) using the ICPC standard titles.5,9–15 The ICPC-2 has been used to identify the prevalence of diseases among outpatients with RFEs of tiredness, dyspnea, nausea/vomiting, pruritus, medically unexplained symptoms, and psychological problems16–21 and in the development of a competence-based curriculum of general practice in Germany.22
The importance of general practice has only recently been recognized in Japan. The Ministry of Education, Culture, Sports, Science and Technology (MEXT) proposed a model for an integrated medical education curriculum, the Model Core Curriculum for Medical Students, in 2001. This model includes 36 common symptoms, the identification of which is necessary for medical training. The Model Core Curriculum was revised in 2007 to include a clinical training program in clinics and community hospitals,23 and the Ministry of Health, Labour and Welfare established the Clinical Clerkship system in 2004. In this system, residents are required to spend at least 1 month in practice at community medical institutes within the first 2 years of the clerkship. The 35 common symptoms that comprise the Goals of Clinical Clerkship were also identified as this time, and all medical residents must submit 20 detailed case reports selected from these 35 symptoms.4,24
Because the universal health insurance system in Japan guarantees free access, patients in Japan are able to visit any medical institution, even if they have a family doctor who provides personal, comprehensive, and continuing care for the individual in the context of the family and the community. Therefore, most medical institutions treat new outpatients, regardless of the size of the medical institution (clinics, small hospitals, large hospitals, and university hospitals), although some large tertiary hospitals charge an additional fee to patients without a referral from a primary or secondary medical institution.25–27 The number of small community hospitals (less than 200 beds) account for approximately 70% of all hospitals in Japan;28 thus, the RFE data from these hospitals could be extremely useful for studies regarding prevalence of diseases and medical school curriculum design.
The frequency of RFEs and diagnoses differs according to the location and size of the medical institution.4,29–34 Yamada et al reported the RFEs and clinical diagnoses of 4,495 patients at five rural clinics in Japan.29 Three studies, to our knowledge, have reported the RFEs of outpatients who visited the general internal medicine (GIM) departments of university hospitals.31–33 Okamoto and Kubota4 reported the common symptoms of outpatients who visited the GIM departments of large community hospitals in Japan. One study looked at RFEs at a small community hospital, but the data were supplied by one physician; therefore, general practice trends found in that hospital could not be examined.35 Because of this dearth of information about small hospitals in Japan, it would be relevant to examine the RFEs and diagnoses of patients who visited these small hospitals and assess the applicability of the guidelines for medical students and residents.
Our purpose was to evaluate the RFEs and diagnoses of outpatients with new health problems who visited a small hospital and, through this evaluation, provided useful data that will contribute to the improvement of the general practice guidelines for medical students and residents.
Materials and methods
Study design
An observational design was used.
Patients
We consecutively enrolled new outpatients who went to the General Internal Medicine Department of Chikusei City Hospital, Chikusei City, Japan during daytime between May 6, 2010 and March 11, 2011. “New patients” were defined as individuals who had a new health problem or who had not visited the hospital with the same health problem within 3 months.
Setting
Chikusei City Hospital is the sole government hospital of Chikusei City and was established in 1972. Chikusei City is located in the north Kanto area and has a population of 108,527, according to the National Population Census36 (October 2010). There are five small- and medium-sized private hospitals (between 109 and 220 beds) and 64 clinics in Chikusei City. A tertiary emergency medical facility, Jichi Medical University Hospital (located nearby in Shimotsuke city, Japan) – which has critical care units, 1,100 beds, and a variety of specialists – is located 30 minutes away by ambulance from Chikusei City Hospital. Chikusei City Hospital has 90 beds, and the annual bed occupancy rate was 63.1% in 2010. The hospital also has several departments, including GIM, surgery, orthopedics, and dermatology, and medical equipment, including rapid blood and urine test systems, electrocardiogram, X-ray machine, ultrasonography unit, endoscopy unit, computerized tomography (CT), and magnetic resonance imaging. In 2010, an average of 243 patients visited this hospital per day; approximately 34 were visiting the hospital for the first time in 3 months, and approximately eleven visited this hospital before visiting another hospital or clinic. All patients with new problems related to internal medicine were first examined in the GIM department. The GIM department takes about five medical students from Jichi Medical University (Shimotsuke city, Japan) per year in Clinical Clerkships.
Measurements
We recorded the RFE, clinical diagnosis, date of visit, age, and sex of all new patients. RFEs and diagnoses were classified according to component 1, “Symptoms/Complaints”, or component 7, “Diagnosis/Diseases”, of the ICPC-27 by two of the authors (TT and MK) independently. One author (JM), who is a member of the ICPC committee of the Japan Primary Care Association and who translated the ICPC-2 from English to Japanese, provided the final classification code if the two investigators chose different codes or were in doubt. We chose component 7, “Diagnosis/Diseases”, as the RFE when a patient complained of a disease itself, such as “R74: Upper respiratory infection acute”. We adopted the RFEs as the diagnosis when we could not define the diagnoses. We calculated the frequency of RFEs, clinical diagnoses, and the proportion of the observed symptoms contained in the Model Core Curriculum for Medical Students and Goals of Clinical Clerkship.
Data analysis
Data are presented as means ± standard deviations and percentage of population. All analyses were performed using Stata software (v 11.0; StataCorp LP, College Station, TX, USA).
Ethics
This study was approved by the bioethics committee of Jichi Medical University.
Results
We examined 1,557 new visits and excluded the visits with RFEs of vaccination (37 cases), health check-up (three cases), and requests for documentation of long-term care insurance (2 cases). The final number of participants analyzed was 1,515. Their mean age was 52.9±19.9 years (range 16–96), and 804 (53.1%) were men. Referrals from other institutions accounted for 131 encounters (8.7%), and there were nine (0.6%) referrals from other departments of Chikusei City Hospital. Four of the authors examined the new patients: TT examined 549 (36.2%); MK examined 514 (33.9%); TN examined 350 (23.0%); and HY examined 102 (6.7%). We followed the medical records of 362 patients, whose diagnoses were not fixed at the first examination or for whom further testing was required, for 3 months; at the end of that time, TT and MK assigned the final diagnosis.
There were 2,252 RFEs (1.49 per encounter) from the 1,515 cases; 2,243 RFEs were classified into 170 ICPC-2 codes (interrater agreement =98.1%). There were 1,727 diagnoses from the 1,515 cases; 1,722 diagnoses were classified into 196 ICPC-2 codes (interrater agreement =97.6%). The distribution of RFEs and diagnoses according to the 17 chapters of the ICPC-2, which are based on body systems plus additional chapters for psychological and social problems, are shown in Figure 1. The three chapters most frequently observed in the RFEs were “R: Respiratory”, 615 cases (27.3%); “A: General and unspecified”, 547 cases (24.3%); and “D: Digestive”, 406 cases (18.0%). The most observed chapters of diagnoses were “R: Respiratory”, 548 cases (31.7%); “D: Digestive”, 381 cases (22.1%); and “K: Circulatory”, 144 cases (8.3%). In contrast, “F: Eye”, “H: Ear”, “W: Pregnancy, childbearing, family planning”, “X: Female genital system including breast”, “Y: Male genital system”, and “Z: Social problems” were quite rare in both RFEs and diagnoses.
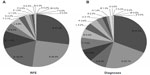  | Figure 1 The frequencies of reasons for encounter (A) and diagnoses (B), according to components 1 (symptoms/complaints) and 7 (diagnosis/diseases) in the International Classification of Primary Care, 2nd edition,7 of new outpatients who visited the General Internal Medicine Department of Chikusei City Hospital, Chikusei City, Japan. |
The top 30 RFE codes accounted for about 80% of all RFEs, and the top 55 RFE codes accounted for about 90% of all RFEs (Figure 2). Table 1 shows the distribution of the titles of the top 30 RFE codes. The three most frequently observed titles of RFEs were “R05 Cough”, 245 (10.9%); “A03 Fever”, 215 (9.5%); and “A91 Abnormal result investigation”, 182 (8.1%). The details of “A91 Abnormal result investigation” are shown in Table 2. The three most frequently observed abnormal results in investigations were “Elevated triglyceride or low-density lipoprotein cholesterol in blood test”, 46 (17.0%); “Abnormality in chest X-ray”, 42 (15.5%); and “Abnormality in upper gastrointestinal series”, 42 (15.5%).
  | Table 2 Abnormal conditions found in the screening tests |
The top 50 diagnosis codes accounted for about 80% of all diagnoses, and the top 90 diagnosis codes accounted for 90% of all diagnoses (Figure 3). The distribution of 50 diagnoses (80.3% of all diagnoses) is shown in Table 3. The three most frequently observed diagnoses were “R74 Upper respiratory infection acute”, 288 (16.7%); “D73 Gastroenteritis presumed infection”, 101 (5.8%); and “D87 Stomach function disorder”, 78 (4.5%).
Twenty-four symptoms listed in the Model Core Curriculum and 25 symptoms listed in the Goals of Clinical Clerkship were commonly observed and included in the RFEs. The Model Core Curriculum category “Urinary problems” is separated into the categories of “Oliguria/anuria/frequent urination” and “Urinary retention/incontinence” in the Goals of Clinical Clerkship. Of the 36 symptoms listed in the Model Core Curriculum, 32 appeared at least once in 1,408 RFEs (62.5%) of the 2,252 RFEs observed at the GIM department (Table 4). However, “Shock”, “Hemorrhagic diathesis”, “Pleural effusion”, and “Menstruation problems” in the Model Core Curriculum were not included in any RFEs observed in this setting. All the 35 symptoms in the Goals of Clinical Clerkship appeared at least once in 1,443 (64.1%) of all 2,252 RFEs (Table 4). On the other hand, “A91 Abnormal result investigation”, “R21 Throat symptom/complaint”, or “R07 Sneezing/nasal congestion”, which placed in the top ten RFEs in this study, were not included in either the Curriculum or the Goals.
Discussion
This study is the first investigation of the distribution of RFEs and diagnoses for all new patients examined in a GIM department in a small hospital in Japan. In addition, we examined the frequencies of common symptoms detailed in the Model Core Curriculum for Medical Students and the Goals of Clinical Clerkship in the observed RFEs.
Of the 17 chapters of the ICPC-2, which cover body systems and social and psychological problems, the following were common to the observed RFEs and diagnoses: “A: General and unspecified”, “D: Digestive”, “K: Circulatory”, “N: Neurological”, and “R: Respiratory”. All of these fall into the field of internal medicine, as would be expected in an investigation in a GIM department. However, the proportion of “L: Musculoskeletal” (seventh most frequent) and “S: Skin (tenth most frequent) in RFEs and diagnoses in Chikusei City Hospital were extremely low compared to the previous data from 10,570 diagnoses observed at five clinics in a rural area of Japan between April 1, 1997 and March 31, 1998 by Yamada et al.29 In that study, “L: Musculoskeletal” was the second and “S: Skin” the third most frequently observed diagnosis. Although both rural and urban Japanese citizens can visit a hospital easily under the free access system in Japan, the difference in the results of these two studies may be accounted for by the choices available to patients in Chikusei City, including choosing a specialist, such as a dermatologist or orthopedist, or visiting another hospital or medical institution, compared to the limited number of medical institutions in rural areas.
The RFE codes from the ICPC-2 in this study were very similar to the results of previous studies. “R05 Cough”, “A03 Fever”, “N01 Headache”, “D06 Abdominal pain localized”, and “A04 Weakness/general tiredness” were among the top ten most common RFEs in three previous studies.4,29,33 The first-place ranking of “R05 Cough” and the second-place ranking of “A03 Fever” in this study are the same as found by Yamada et al.29 Full knowledge of these symptoms is a high priority for medical students and residents.
We also examined “A91 Abnormal result investigation”, which was the third most frequently observed symptom on the RFEs. It is unclear whether “A91 Abnormal result investigation” is common in RFEs worldwide.37 In Japan, only one study, whose authors worked in the GIM department of a small hospital, reported A91 as the most common RFE,35 while reviews of RFEs in clinics and large hospitals did not find “A91 Abnormal result investigation” to be common.4,29,30,32 We found that “A91 Abnormal result investigation” was a common reason for visiting primary care physicians in a small hospital in Japan. This result could be related to the health care system of Japan. The Occupational Health Acts of 1972 and Community Health Acts of 1982 mandated the provision of programs for primary and secondary prevention, including chronic diseases such as hypertension and diabetes, and screening for gastric and lung cancer.25 Under the free access system, patients may choose any medical institution for a variety of reasons, such as the specialists or test equipment available. The management of “Abnormality in chest X-ray” and “Abnormality in upper gastrointestinal series” requires further examination, such as the interpretation of a chest CT image or scheduling of an upper gastrointestinal endoscope procedure. In Japan, patients are more willing to trust and visit medical institutes with gastrointestinal test equipment for their primary medical care.38 Three of the four physicians (TT, MK, and TN) who practice in the General Internal Medicine Department in Chikusei City Hospital have both chest and gastrointestinal skills and experience. Thus, it is possible that patients who visit Chikusei City Hospital expect diagnosis and treatment as early as possible because the hospital possesses high-tech equipment (eg, CT scanner, endoscopy).
Diagnoses in this study are also similar to data from previous studies of large clinics. “R74 Upper respiratory infection acute”, “D73 Gastroenteritis presumed infection”, “D87 Stomach function disorder”, “R78 Acute bronchitis/bronchiolitis”, and “A97 No disease” are listed among the top ten diagnoses in the report by Yamada et al.29 Acute diseases such as R74, D73, and R78 should have high priority in medical student and resident GIM curricula. In our data, “K86 Hypertension uncomplicated”, “T93 Lipid disorder”, and “T90 Diabetes non-insulin dependent” were also listed in the top ten. These diagnoses are mostly the result of the “A91 Abnormal result investigation” RFE code. In previous studies, these are also listed as high-prevalence diseases.29,34 It is important for physicians in clinics and small hospitals to understand the nature and treatment of these chronic diseases.
Notably, 32 of the 36 common symptoms listed in the Model Core Curriculum revised in 200723 (but all 35 common symptoms listed in the Goals of Clinical Clerkship24) were found in the 2,252 RFEs observed in this study. This indicates that serving the outpatients of GIM departments in small hospitals is suitable for the Clinical Clerkship of General Practice. On the other hand, the 36 common symptoms in the Model Core Curriculum and the 35 common symptoms of the Goals of Clinical Clerkship were 62.5% and 64.0%, respectively, of all RFEs observed in the General Internal Medicine Department of Chikusei City Hospital. Okamoto and Kubota4 reported that the 35 common symptoms accounted for 56.7% of the RFEs of 4,558 patients examined in the GIM department of a large hospital (801 beds). Thus, the common symptoms listed in the Curriculum and Goals only partially represent the RFEs observed in actual practice in small and large hospitals. Furthermore, neither the Curriculum nor the Goals contain “A91 Abnormal result investigation”, “R21 Throat symptom/complaint”, or “R07 Sneezing/nasal congestion”, which all placed in the top ten RFEs in this study. These RFEs should be included in the curricula and goals for medical students and residents.
Okamoto and Kobota4 reported that “B02 Lymph glands enlarged” (listed in the Model Core Curriculum and the Goals of Clinical Clerkship) was observed in 33 RFEs (0.9% of all RFEs) at a large hospital. This proportion of B02 is higher than observed in our data, where “B02 Lymph glands enlarged” was observed in only three patients (0.1%). We presume that small hospitals may not see as many B02 patients due to fewer referrals from outside institutions. Another unseen symptom in our study, menstruation problems, may be related to the paucity of primary physicians in Japan who take obstetric or gynecology patients. The importance of the skills of obstetrics and gynecology necessary for general practitioners in Japan needs to be discussed. The categories occurring with a low frequency in this study were convulsion (listed in the Model Core Curriculum and the Goals of Clinical Clerkship), shock and dehydration (Model Core Curriculum), and hearing problems (Goals of Clinical Clerkship), all of which could be treated in an emergency room.39 Red eye (Goals of Clinical Clerkship) was observed in 72 outpatients (0.5%) who visited clinics in a rural area.29 Therefore, medical students and residents should experience treating primary care outpatients in a variety of settings, such as clinics, small hospitals, large hospitals, and emergency rooms in rural and urban regions in Japan, to be exposed to a variety of the common symptoms listed in these two guidelines.
The numbers of RFEs (170) and diagnoses (191) observed in this study are too numerous for medical students and residents to learn. Fortunately, the top 30 codes accounted for 80% of all RFEs and the top 55 codes accounted for 90% of all RFEs. Furthermore, the top 50 codes accounted for 80% of all diagnoses and the top 90 codes accounted for 90% of all diagnoses. Therefore, medical students and residents should focus on studying the management of these very common RFEs and diagnoses. Hereafter, we should pay attention not only to the frequency of RFEs and diagnoses, but also to differential diagnosis difficulties associated with one symptom and the critical nature of the disease when we discuss the necessary training for medical students and residents in general practice.
This study has two strengths. First, we included all new outpatients for almost 1 year – from May 6, 2010 to March 11, 2011. The frequency of RFEs and diagnoses might vary by season in Japan; therefore, our data has less selection bias due to seasonal differences. Second, we made a great effort to decrease misclassification ICPC-2 codes by using two investigators.
This study has two limitations. First, diagnostic accuracy in this study was not based on strict diagnostic criteria using laboratory tests. More objective methods, such as using test results, were not used in all diagnoses; however, the physicians in the General Internal Medicine Department of Chikusei City Hospital had more than 5 years of clinical practice experience in assessing patient history and conducting physical examinations. The medical history and physical examination of patients leads to the correct diagnosis in 88% of cases, while test findings lead to the correct diagnosis in the remaining 12% of cases.40 Therefore, we believe inaccuracies in diagnoses do not affect the interpretation of the results. Second, we analyzed the data from only one small urban community hospital. Therefore, our findings may not be representative of all small hospitals in Japan. Nonetheless, we consider Chikusei City Hospital to be a typical community hospital because it has the same three major departments (internal medicine, surgery, and orthopedics) as found in most small hospitals in Japan.28 Therefore, we believe that the findings in this study are not particularly biased. However, it is important to analyze more cases using data from a variety of hospitals and clinics in different settings to confirm our results.
Conclusion
We identified the common RFEs and diagnoses of new outpatients at one small urban community hospital in Japan. We found that “A91 Abnormal result investigation” was a common RFE, making it important to include in the education of medical students and residents. We also revealed inconsistencies in RFEs between observed and common symptoms listed in the guides for medical students and residents in Japan. These findings can be used to revise the medical educational curriculum for students and residents. Further studies should address RFEs, diagnoses, and the curricular guides in more types of health facilities and different regions.
Acknowledgment
This study was supported by JSPS KAKENHI Grant Number 23790577.
Author contributions
TT contributed to the conception and design of the study; the acquisition of data; the analysis and interpretation of data; and the writing and revision of the manuscript. MK contributed to the conception and design of the study; the acquisition and interpretation of data; and the revision of the manuscript. JM and YI contributed to the conception and design of the study; the analysis and interpretation of the data; and the revision of the manuscript. HY and TN contributed to the acquisition and interpretation of the data; and the revision of the manuscript. MO contributed to the conception and design of the study; and the revision of the manuscript. EK contributed to the conception and design of the study; and the writing and revision of the manuscript. All authors approved the final version of the manuscript.
Disclosure
The authors report no conflicts of interest in this work.
References
Jerant A, Fenton JJ, Franks P. Primary care attributes and mortality: a national person-level study. Ann Fam Med. 2012;10(1):34–41. | |
Starfield B, Shi L, Macinko J. Contribution of primary care to health systems and health. Milbank Q. 2005;83(3):457–502. | |
Lionis C, Stoffers HE, Hummers-Pradier E, Griffiths F, Rotar-Pavlic D, Rethans JJ. Setting priorities and identifying barriers for general practice research in Europe. Results from an EGPRW meeting. Fam Pract. 2004;21(5):587–593. | |
Okamoto T, Kubota N. Common clinical problems in general medicine outpatients: target analysis of residency training. Japanese Journal of Primary Care. 2007;30:197–204. Japanese. | |
Gataa R, Ajmi TN, Bougmiza I, Mtiraoui A. Morbidity patterns in general practice settings of the province of Sousse, Tunisia. Pan Afr Med J. 2009;3:11. | |
Lee KW, Lee JK, Ma HK, Kim JW, Yoon CH. Analysis of clinical contents in a family practice clinic of rural area according to the ICPC method. J Korean Acad Fam Med. 1998;19:374–382. | |
WONCA International Classification Committee (WICC). ICPC-2: International Classification of Primary Care. 2nd ed. Oxford: Oxford Medical Publications; 1998. | |
Soler JK, Okkes I, Wood M, Lamberts H. The coming of age of ICPC: celebrating the 21st birthday of the International Classification of Primary Care. Fam Pract. 2008;25(4):312–317. | |
Soler JK, Okkes I, Oskam S, et al; Transition Project. An international comparative family medicine study of the Transition Project data from The Netherlands, Malta and Serbia. Is family medicine an international discipline? Comparing incidence and prevalence rates of reasons for encounter and diagnostic titles of episodes of care across populations. Fam Pract. 2012;29(3):283–298. | |
Moth G, Olesen F, Vedsted P. Reasons for encounter and disease patterns in Danish primary care: changes over 16 years. Scand J Prim Health Care. 2012;30(2):70–75. | |
Kim BS, Kim SH, Choi HR, Won CW. Trends of the new outpatients in a university-based family practice. Korean J Fam Med. 2011;32(5):285–291. | |
Brueton V, Yogeswaran P, Chandia J, et al. Primary care morbidity in Eastern Cape Province. S Afr Med J. 2010;100(5):309–312. | |
Okkes IM, Polderman GO, Fryer GE, et al. The role of family practice in different health care systems: a comparison of reasons for encounter, diagnoses, and interventions in primary care populations in The Netherlands, Japan, Poland, and the United States. J Fam Pract. 2002;51(1):72–73. | |
Okkes IM, Oskam SK, Lamberts H. The probability of specific diagnoses for patients presenting with common symptoms to Dutch family physicians. J Fam Pract. 2002;51(1):31–36. | |
Wun Y, Lu X, Liang W, Dickinson J. The work by the developing primary care team in China: a survey in two cities. Fam Pract. 2000;17(1):10–15. | |
Kenter EG, Okkes IM, Oskam SK, Lamberts H. Tiredness in Dutch family practice. Data on patients complaining of and/or diagnosed with “tiredness”. Fam Pract. 2003;20(4):434–440. | |
Frese T, Sobeck C, Herrmann K, Sandholzer H. Dyspnea as the reason for encounter in general practice. J Clin Med Res. 2011;3(5):239–246. | |
Frese T, Klauss S, Herrmann K, Sandholzer H. Nausea and vomiting as the reasons for encounter in general practice. J Clin Med Res. 2011;3(1):23–29. | |
Frese T, Herrmann K, Sandholzer H. Pruritus as reason for encounter in general practice. J Clin Med Res. 2011;3(5):223–229. | |
Soler JK, Okkes I. Reasons for encounter and symptom diagnoses: a superior description of patients’ problems in contrast to medically unexplained symptoms (MUS). Fam Pract. 2012;29(3):272–282. | |
Rosendal M, Vedsted P, Christensen KS, Moth G. Psychological and social problems in primary care patients – general practitioners’ assessment and classification. Scand J Prim Health Care. 2013;31(1):43–49. | |
Steinhaeuser J, Chenot JF, Roos M, Ledig T, Joos S. Competence-based curriculum development for general practice in Germany: a stepwise peer-based approach instead of reinventing the wheel. BMC Res Notes. 2013;6:314. | |
[Model Core Curriculum in Medical Education, the guideline for the educational programme] [webpage on the Internet]. Tokyo: Ministry of Education, Culture, Sports, Science and Technology; 2007. Available from: http://www.mext.go.jp/b_menu/shingi/chousa/koutou/033-1/toushin/1304433.htm. Accessed February 10, 2014. Japanese. | |
[Goals of Clinical Clerkship] [webpage on the Internet]. Tokyo: Ministry of Health, Labour and Welfare; 2004. Available from: http://www.mhlw.go.jp/topics/bukyoku/isei/rinsyo/keii/030818/030818b.html. Accessed April 25, 2014. Japanese. | |
Ikeda N, Saito E, Kondo N, et al. What has made the population of Japan healthy? Lancet. 2011;378(9796):1094–1105. | |
Okayama M. Overview of community health care. In: Kajii E, editor. White Paper of Community Health Care. 3rd ed. Jichi: Jichi Medical University; 2012:3–20. Japanese. | |
Fukui T, Rahman M, Takahashi O, et al. The ecology of medical care in Japan. Japan Med Assoc J. 2005;48:163–167. | |
[Medical facilities survey] [webpage on the Internet]. Tokyo: Ministry of Health, Labour and Welfare; 2010. Available from: http://www.mhlw.go.jp/toukei/list/79-1.html. Accessed February 10, 2014. Japanese. | |
Yamada T, Yoshimura M, Nago N, et al. What are common diseases and common health problems? The use of ICPC in the community-based project. Japanese Journal of Primary Care. 2000;23:80–89. Japanese. | |
Waza K, Imai K, Oonishi Y, Mise J, Igarashi M. A study on the reasons for encounter at the university hospital’s affiliated community-oriented primary care clinic by using the ICPC. Japanese Journal of Primary Care. 1998;21:182–190. Japanese. | |
Kanda T, Kuwabara A, Kobayashi I, Fujita KI, Nakajima H, Tamura JI. Application of international classification of primary care to patient record in general medicine of Gunma University Hospital. Kitakanto Med J. 2000;50(3):215–219. Japanese. | |
Imanaka S, Onishi H, Oda Y, et al. [An analysis of chief complaints of elderly patients by modified-international classification of primary care: a case of high-functional hospital]. The Journal of Japanese Society of General Medicine. 1999;4:1–8. Japanese. | |
Yamashiro S. Department of general medicine in university hospital in Japan. The Journal of Japanese Society of General Medicine. 2005;10:61–67. Japanese. | |
Tanaka K, Nomaguchi S, Matsumura S, Fukuhara S. Ranking the frequency of patient illness at primary care clinics. Japanese Journal of Primary Care. 2007;30(4):344–351. Japanese. | |
Ando S, Igarashi M. Chief complaints and their diagnoses in ambulatory medicine: classification of chief complaints and reasons for encounter by ICPC. Japanese Journal of Primary Care. 1996;19:291–297. Japanese. | |
National Population Census [webpage on the Internet]. Tokyo: Ministry of Internal Affairs and Communications; 2010. Available from: http://www.stat.go.jp/data/kokusei/2010/index2.htm. Accessed April 25, 2014. Japanese. | |
Duckitt R, Palsson R, Bosanska L, Dagna L, Durusu TM, Vardi M; CDIME group. Common diagnoses in internal medicine in Europe 2009: a pan-European, multi-centre survey. Eur J Intern Med. 2010;21(5):449–452. | |
Sekine S, Komatsu K, Matsushima D, et al. Factors affecting people’s preferences of visiting a kakaritsukei (home-doctor). General Medicine. 2010;11(2):71–77. | |
Malmström T, Huuskonen O, Torkki P, Malmström R. Structured classification for ED presenting complaints – from free text field-based approach to ICPC-2 ED application. Scand J Trauma Resusc Emerg Med. 2012;20:76. | |
Peterson MC, Holbrook JH, Von Hales D, Smith NL, Staker LV. Contributions of the history, physical examination, and laboratory investigation in making medical diagnoses. West J Med. 1992; 156(2):163–165. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.





