Back to Journals » International Journal of General Medicine » Volume 13
Psychometric Evaluation of Persian Version of Nurses’ Intention to Care Scale (P-NICS) for Patients with COVID-19
Authors Rahmatpour P , Sharif Nia H , Sivarajan Froelicher E, Kaveh O, Pahlevan Sharif S , Taghipour B
Received 18 May 2020
Accepted for publication 27 July 2020
Published 18 August 2020 Volume 2020:13 Pages 515—522
DOI https://doi.org/10.2147/IJGM.S260579
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Pardis Rahmatpour,1 Hamid Sharif Nia,2 Erika Sivarajan Froelicher,3 Omolhoda Kaveh,4 Saeed Pahlevan Sharif,5 Behzad Taghipour6
1School of Nursing and Midwifery, Iran University of Medical Sciences, Tehran, Iran; 2School of Nursing and Midwifery Amol, Mazandaran University of Medical Sciences, Sari, Iran; 3School of Medicine, University of California San Francisco, San Francisco, CA, USA; 4School of Nursing and Midwifery Sari, Mazandaran University of Medical Sciences, Sari, Iran; 5Taylor’s Business School, Taylor’s University Lakeside Campus, Subang Jaya, Malaysia; 6 Amol Imam Khomeini Hospital, Mazandaran University of Medical Science, Sari, Iran
Correspondence: Hamid Sharif Nia Tel +989118951036
Email [email protected]
Background: Given the high incidence of coronavirus and the shortage of nurses in Iranian hospitals, nurses’ intention to care for patients with COVID-19 is important. The aim of this study is to evaluate the reliability and validity of the Persian version of the nurses’ intention to care scale (NICS) by Iranian nurses who care for patients with COVID-19 in hospitals.
Methods: A cross-sectional study was conducted on nurses (n= 400) at public and private Mazandaran hospitals. An online questionnaire was used that consisted of two parts: demographic variables and NICS. The scale was translated into Persian first and then validated using both construct and content validity.
Results: The findings from an exploratory factor analysis yielded six factors that explained 53.12% of the total variance of the NICS. The confirmatory factor analysis demonstrated that the model had a good fit and the inter-item correlation values of the factors indicated good internal consistency.
Conclusion: The Persian version of NICS in Iranian nurses had six factors. The results of our study add insight for nurse administrators and educators to further develop strategies to increase nurses’ intention by improving positive attitudes and reducing their negative beliefs.
Keywords: COVID-19, intention, nursing care, reliability, theory of planned behavior, validity
Introduction
Most countries in the world are fighting a disease called COVID-19. It began in Wuhan city, located in the Hubei Province of China. COVID-19 has flu-like symptoms, including fever, dry cough, myalgia, and dyspnea1 based on a WHO report, it infects people of all ages. However, older people and those with underlying medical conditions such as cardiovascular disease, diabetes, chronic respiratory disease, and cancer are at especially high risk of developing severe pulmonary conditions requiring prolonged treatment on ventilators.2 The virus was identified as genus beta-coronavirus, placing it alongside other Severe Acute Respiratory Syndrome (SARS) and Middle East Respiratory Syndrome (MERS), but compared with SARS and MERS, COVID-19 has spread more rapidly and the mortality rates are higher.3
Iran is one of the countries with a very high incidence of coronavirus so that according to the World Health Organization (WHO) to date 7 July 2020, 243,051 total confirmed cases and 11,731 total deaths were reported.4 Under these stressful medical and social conditions, health care providers face many challenges: a sudden rise in workload, high risk of infection for themselves and their families, and especially because of inadequate protective equipment. Among health care providers, nurses have a great responsibility for patients with COVID-19 and are at the front lines in the fight to COVID-19 among other members of the healthcare system.5 They are under extreme stress and experience psychological conflict between their duties as nurses and their concern for their own safety. Nurses have direct and prolonged contact with these patients, and any lack of personal protective equipment (PPE) and inefficient crisis management will affect them in providing care. During the SARS outbreak, health care workers were at highest risk of infection; however in Taiwan, 42.7% of nurses reported having positive intentions to provide care to patients with SARS.6 Despite the shortage of facilities and difficulties in caring for these patients, uncomfortable conditions such as the use of face masks and protective clothes, they continued to care and did not quit their jobs.7 Nursing patients with COVID-19 is affected by external factors (facilities, crisis management, incentives, and organizational support) as well as internal factors (motivation, spirituality, humanitarian actions).8–10 Indeed, one way to retain existing nurses in the hospital is attention to their needs such as providing sufficient and adequate PPE, and providing up-to-date continuing education for nurses may help to reinforce nurses’ self-efficacy in caring for such patients.6
The term intention is defined as purposeful and prompt action. In the nursing literature, “intention” implies providing holistic nursing care with love.11 This concept also incorporates the Theory of Planned Behavior (TPB), where intention is defined in terms of trying to perform a given behavior rather than in relation to actual performance”. Intentions are assumed to be motivational factors that influence the behavior and consist of attitudes toward the behavior, subjective norms, and perceived behavior control.12 Many studies have used these theories to examine nurses’ intentions with respect to specific practices, and several scales have been designed to measure this concept.
To the best of our knowledge, there are no studies about nurses’ intention to care for patients with COVID-19 and the literature regarding nursing intention to care focuses on intention to care for patients with SARS,6 H1N1 influenza,13 a high-risk pathogen that infected patients.14 Most of them use similar scale to measure nurses’ intention that was developed by Yoo et al (2005) in the prediction of nurses intention for caring patients with SARS, where the authors identified the following six factors; positive behavioral beliefs, negative behavioral beliefs, positive social norms, negative social norms, positive control beliefs and negative control beliefs.15
A reliable and valid scale would help to explore how these factors influence the nurses’ intention to care for patients with a COVID-19 diagnosis. Given, that most Iranian hospitals are facing a shortage of nurses;16 in this situation nurses’ intention to care for patients with COVID-19 is critically important to the healthcare system. Because of the similarity of SARS to COVID-19 disease, the questionnaire by Yoo et al (2005) was used in this study. The aim of this study is to evaluate the reliability and validity of a Persian version of the Nurses’ Intention to Care Scale (P-NICS) in Iranian nurses who care for patients with COVID-19 in hospitals.
Materials and Methods
This is a cross-sectional study was conducted among Iranian nurses in hospitals affiliated by Mazandaran University of Medical Sciences in March 2020.
Sample Size
The minimum sample size for factor analysis was estimated using “a rule of thumb approach” in which 400 subjects were considered adequate.17 Given the scale has 40 items this would provide 10 subjects per item.
Setting and Procedure
Mazandaran province is an Iranian province located along the southern coast of the Caspian Sea. According to the high prevalence of coronavirus in Mazandaran Province, all public and private hospitals admitted patients with symptoms of COVID-19. Given the infectiousness of this virus, to avoid nosocomial transmission of COVID-19, an online data collection with convenience sampling method was performed for this study. The questionnaire itself took approximately 10 min to complete. The P-NICS created via Google Forms and its URL link was sent to nurses through a social networking application such as Telegram channel or WhatsApp. Thus, all nurses who work in hospitals could be included in this sample. Data were extracted in the Excel file from Google Forms and prepared for analysis.
Measurements
The questionnaire consists of two parts. First, the demographic information included: age, gender, marital status, years of work experience, and education (bachelor or master degree). Also, one question asks nurses about their attitude toward caring for patients with COVID-19; the response options consist of a seven-point Likert scale, ranging from 1 (Strongly did not want to) to 7 (strongly will). The second part was Yoo et al nurses’ intention scale based on Ajzen’s TPB.12 The questionnaire was developed in four phases, the beliefs of 43 nurses, content validity, face validity and construct validity.15 In this study, the nurses’ beliefs of Yoo et al study was used; it consisted of three domains: (1) behavioral beliefs (14 items), (2) subjective norms beliefs (8 items) and (3) control beliefs (18 items) using a seven-point Likert scale, ranging from 1 (strongly disagree) to 7 (strongly agree).
Analysis Methods
Content Validity
Content Validity Ratio (CVR) and Content Validity Index (CVI) for the P-NICS items were calculated by ten faculty members with expertise in psychiatric nursing. When the number of experts is 10, the minimum acceptable CVR based on Lawshe is equal to 0.62.18
Construct Validity
Construct validity of P-NICS was evaluated through the Maximum Likelihood Exploratory Factor Analysis (EFA) with Promax rotation on the first set of 200 responses for EFA. The Kaiser–Meyer–Olkin test and Bartlett’s test of sphericity were used to check the appropriateness of the study sample and the model. The number of factors was determined based on Horn’s parallel analysis.19
The presence of an item in a latent factor was determined based on a factor loading of almost 0.33, which was estimated using the following formula: CV = 5.152÷ √ (n – 2), where CV was the number of extractable factors and n was the sample size. Next, the items with communalities less than 0.2 were excluded from EFA.20 Also according to the three indicator rule having factorability, at least three items must exist for each factor.21 For assessment of the structural factors, confirmatory factor analysis (CFA) was conducted using the maximum-likelihood method and the most common goodness of fit indices. The model fitness indicators were accepted according to Root Mean Square of Error of Approximation (RMSEA< 0.08), Comparative Fit Index (CFI> 0.9), Parsimonious Comparative Fit Index (PCFI> 0.5), Parsimonious Normed Fit Index (PNFI > 0.5), Incremental Fit Index (IFI > 0.9) and CMIN/DF (< 3).22
Convergent and Discriminant Validity
The convergent and discriminant validity of P-NICS were estimated using Fornell and Larcker’s approach and through Average Variance Extracted (AVE), Maximum Shared Squared Variance (MSV) Composite reliability (CR). An AVE of more than 0.5 reflects suitable convergent validity and an AVE greater than MSV confirm discriminant validity.23
Reliability Assessment
Internal consistency of P-NICS was assessed by the Cronbach’s alpha (α), McDonald’s omega (Ω), Average Inter-Item Correlation (AIC) Coefficient’s, CR (which replaces Cronbach’s alpha coefficient in structural equation modeling)24 and Maximal Reliability H (the value of > 0.7 was considered good).22 Also, AIC 0.2 to 0.4 was considered as a good internal consistency.25
Multivariate Normality and Outliers
Univariate distributions were examined for outliers, skewness, and kurtosis. Multivariate distributions were evaluated for normality and multivariate outliers. Multivariate normality can be evaluated through the use of the Mardia’s coefficient of multivariate kurtosis. One indication of deviation from normal distribution was a Mardia’s coefficient > 5. Multivariate outliers were evaluated through the evaluation of a Mahalanobis distance. Items with a Mahalanobis distance of p<0.001 were considered to be multivariate outliers.26,27
All of the statistical procedures were analyzed by SPSS-AMOS24, JASP 0.13.1.0, and the SPSS R-Menu 2.0.
Ethical Consideration
The following information was included in the informed consent: the introduction of the questionnaire; the study aims, number of items, The average completion time of the questionnaire, the researcher’s affiliation and email address for queries, ethical code of study conduct, the voluntary nature of participation and using anonymous responses in research by the research team to protect confidentiality. The questionnaire items are not viewed by the participant until they agree to participate and click on the “next button.” Also, the completion of the survey by the participants is considered informed consent. The questionnaire items are not viewed by participant until they agree to participate and click on “next button”. The protocol of this study was approved by the Mazandaran University of Medical Sciences Research Ethics Committee (IR.MAZUMS.REC.1399.7298).
Results
The mean and standard deviation for the age of 400 nurses and years worked as a nurse were 33.6 (±7.9) and 10.12 (±8.2) years respectively. Other demographic characteristics of nurses are shown in Table 1. Also, 20.5% of nurses responded strongly that they would provide nursing care to patients with a COVID-19 diagnosis.
 |
Table 1 Demographic Characteristics of Participants (n=400) |
In MLEFA, KMO test value was 0.84 and Bartlett’s test value was 3588.89 (P < 0.001). MLEFA revealed a six-factor structure for P-NICS. The eigenvalues and percent of variances of these six factors are shown in Table 2. These six factors explained 53.12% of the total variance of the P-NICS in Iranian nurses who cared for patients with COVID-19.
 |
Table 2 Exploratory Factors Extracted from 40 Items of P-NICS (n=200) |
Given that CFA findings, all goodness of fit indices confirmed the model fit (χ2 = 688.76; n = 250; df= 418, P < 0.001; CMIN/DF = 1.64, PCFI = 0.82; PNFI = 0.73; RMSEA = 0.06 (CI 90%: 0.05, 0.06); IFI = 0.92, and CFI = 0.91 (Figure 1).
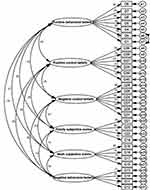 |
Figure 1 Model of confirmation factor analysis of P-NICS. |
The Cronbach’s alpha, McDonald’s omega, CR, and maximal reliability of six extracted factors of the P-NICS were excellent (0.8<). Also, the AIC values of factors were good. Regarding convergent and discriminant validity, the AVE of factors was more than MSV and shows that six factors have good convergent and discriminant validity. Composite reliability, convergent and discriminant validity and internal consistency indices of the P-NICS are given in Table 3.
 |
Table 3 Composite Reliability, Convergent and Discriminant Validity, and Internal Consistency Indices of the P-NICS (n=200) |
Discussion
The results of the present study support a six-factor structure of P-NICS where 31 items explained 53.12% of the total variance of the nurses’ intention to care in the Iranian context. This is the first valid and reliable scale about nurses’ intention to care for patients with COVID-19. In the Yoo et al study, with PCA six factors explained 68.2% of the total variance.15 Considering that scales with higher variance are more desirable in explaining the concept, it should be noted that EFA focuses on the shared variance of the variables; whereas PCA focuses on the total variation among the variables; thus, the percentage of extracted variance of PCA will be greater than EFA.28
The internal consistency of items of the P-NICS was good, and the high level of Cronbach’s alpha signifies the internal consistency suitability of the scale and the correlation between the items. Also, the CR of the scale was evaluated with CFA and demonstrated acceptable reliability of the P-NICS. One of the advantages of measuring CR is that this estimate is not affected by the number of scale items and obtained structure and is dependent on the actual factor loading of each item of the latent variables.29 The CR value of this scale was calculated in this study for the first time.
Based on EFA results the P-NICS consists of six factors namely positive behavioral beliefs (PBB), positive control beliefs (PCB), negative control beliefs (NCB), family subjective norms (FSN), work subjective norms (WSN) and negative behavioral beliefs (NBB).
In this study, the first factor is PBB which addressed positive beliefs in the outcomes of caring for patients with COVID-19. Iranian nurses reported that increasing self-efficacy, gaining new knowledge, and “to be a good role model” are positive beliefs that Lee et al identified as behavioral beliefs that bring about attitudes toward the behavior.30 Indeed, nurses had a positive attitude towards caring for patients and an increased desire to care and be providing nursing care involved for these patients.
The second factor of PCB is control beliefs that are the beliefs that nurses have about how easy or difficult it will be to care for patients. Iranian nurses reported that professional responsibilities, prevention from further infection, and empathy for patients with COVID-19 are positive control beliefs that affect nurses’ intentions. “Perceived control belief” was the most significant variable among predictor variables in nurses’ intention to care for patients with emerging infectious diseases in Lee et al study.30
The third factor was the NCB. It related to the negative beliefs of nurses about caring for patients with COVID-19. Because of the dangerous nature of the COVID-19 disease, items such as fear of infection and death or contagious disease are negative beliefs that decrease nurses’ intention to care. Ko et al stated that although nurses have a commitment to providing the best care for patients with this life-threatening illness; however, they have concerns about staying away from their homes, fearing that they might spread the disease to their families and friends during the SARS epidemic.6
In this study, two factors of FSN and WSN are about subjective norms of TPB that are reflective of a nurse’s beliefs about the expectations of significant others regarding the performance of particular behaviors. In the FSN factor, the nurses demonstrated that their family and friends supported them in caring for patients with COVID-19. Nurses distinguished the two factors of FSN and WSN, and they reported the hospital colleague’s role in their caring intention as another factor (WSN). Sun Young et al (2015) assessed the nurses’ intentions to care for patients with New Influenza-H1N1. Among the predictors, subjective norm had the greatest effect on the intention to care. The nurses with higher subjective norms and more positive perceived behavioral control reported higher intentions.13 However, in the study by Lee et al (2020) that investigated factors that influence nurses’ intention to care for patients with emerging infectious diseases, subjective norms did not explain nurses intentions.30
The last factor is NBB, and it referred to negative beliefs on the outcomes of caring for patients with COVID-19. Nurses demonstrated that some items like “not having enough vacation or extra bonus,” and “being isolated” were negative attitudes toward caring for patients with COVID-19. Ko et al stated that nurses’ intention to care was predicted by their attitudes and reinforcement of nurses’ positive attitudes could be achieved through verbal expression of approval and support from nursing administrators, or substantial rewards such as special compensation payments could be used to encourage and acknowledge nurses for their efforts.6
In general, Iranian nurses like nurses in other countries, face difficulties such as infection control, patient acute illness, and increased nursing workload in caring for COVID-19 patients.7 A valid and reliable scale helps to assess nurses’ viewpoints and accurately measure their intention to identify the effective factors.
Limitation
The subjects were recruited from one province in Iran; therefore the generalizability of the study may be a limitation. Since P-NICS explores 53.12% of the total variance, further studies with qualitative methods may be needed to explore nurses’ intention to care for patients with COVID-19. Although there were advantages to using an online questionnaire in the COVID-19 outbreak; we should point out that selection bias, lack of physical interaction, inability to verify an individual’s status, or the veracity of their responses were limitation of this online survey.
Conclusions
The findings of this study highlight that the P-NICS in Iranian nurses have 31 items and six factors which explain more than half of the variance of the concept. The P-NICS has good reliability, internal consistency, and constructs validity to identify nurses’ intention to care for patients with COVID-19. Nurses have close contact with patients with COVID-19 and therefore the identification of predictors of nurses’ intentions can be very useful to hospitals managers and policymakers. Improving self-efficacy, knowledge of nurses is helpful during the COVID-19 pandemic. During this COVID-19 pandemic, nurses need support. The results of our study add insight for nurse administrators and educators to further develop strategies to increase nurses’ intention by encouraging positive attitudes, taking all necessary steps to ensure that nurses and their families have the necessary PPE to be safe. Also, the motivated nurses need to have their negative beliefs reduced, and providing sufficient PPE, managing job overload and financial aid are all beneficial.
Acknowledgment
We thank all the participants who took part in the study.
Funding
There is no funding to report.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Wang W, Tang J, Wei F. Updated understanding of the outbreak of 2019 novel coronavirus (2019‐nCoV) in Wuhan, China. J Med Virol. 2020.
2. World Health Organization. Coronavirus disease 2019 ( COVID-19). Situation Rep. 2020;51.
3. Peeri NC, Shrestha N, Rahman MS, et al. The SARS, MERS and novel coronavirus (COVID-19) epidemics, the newest and biggest global health threats: what lessons have we learned? Int J Epidemiol. 2020. doi:10.1093/ije/dyaa033
4. World Health Organization. Coronavirus disease 2019 (COVID-19): situation report 74; 2020. Available from: https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200403-sitrep-74-covid-19-mp.pdf?sfvrsn=4e043d03_4.
5. Huang L, Rong Liu H. Emotional responses and coping strategies of nurses and nursing college students during COVID-19 outbreak. medRxiv. 2020.
6. Ko N-Y, Feng M-C, Chiu D-Y, Wu M-H, Feng J-Y, Pan S-M. Applying theory of planned behavior to predict nurses’ intention and volunteering to care for SARS patients in southern Taiwan. Kaohsiung J Med Sci. 2004;20(8):389–398. doi:10.1016/S1607-551X(09)70175-5
7. Danielis M, Mattiussi E. The care of patients through the lens of the fundamentals into times of the COVID-19 outbreak. Intensive Critical Care Nursing. 2020;102883. doi:10.1016/j.iccn.2020.102883
8. Griffeth RW, Hom PW, Gaertner S. A meta-analysis of antecedents and correlates of employee turnover: update, moderator tests, and research implications for the next millennium. J Manage. 2000;26(3):463–488. doi:10.1177/014920630002600305
9. Mayo E. The human problems of an industrial civilization. Routledge. 2004.
10. Dai Y, Hu G, Xiong H, Qiu H, Yuan X. Psychological impact of the coronavirus disease 2019 (COVID-19) outbreak on healthcare workers in China. medRxiv. 2020.
11. Sofhauser C. Intention in nursing practice. Nurs Sci Q. 2016;29(1):31–34. doi:10.1177/0894318415614629
12. Ajzen I. The theory of planned behavior. Organ Behav Hum Decis Process. 1991;50(2):179–211. doi:10.1016/0749-5978(91)90020-T
13. Sun Young J, Hyo Sun P, Hee-Jung W, Mijung K. Intentions to care for new influenza A (H 1 N 1) patients and influencing factors: an application of theory of planned behavior. J Korean Acad Society Home Health Care Nursing. 2015;22(1):78–87.
14. Kim HJ, Choi YH. Factors influencing clinical nurses’ nursing intention for high risk pathogen infected patient. J Korean Clin Nursing Res. 2016;22(3):327–335.
15. Yoo HR, Kwon BE, Jang YS, Youn HK. Validity and reliability of an instrument for predictive nursing intention for SARS patient care. J Korean Acad Nurs. 2005;35(6):1063–1071. doi:10.4040/jkan.2005.35.6.1063
16. Shamsi A, Peyravi H. Nursing shortage, a different challenge in Iran: A systematic review. Med J Islamic Republic Iran. 2020;34(1):54–62.
17. World Health Organization; 2020. Available from: https://www.who.int/docs/default-source/coronaviruse/clinical-management-of-novel-cov.pdf.
18. Lawshe CH. A quantitative approach to content validity 1. Pers Psychol. 1975;28(4):563–575. doi:10.1111/j.1744-6570.1975.tb01393.x
19. Ö Ç, Koçak D. Using Horn’s parallel analysis method in exploratory factor analysis for determining the number of factors. Edu Sci. 2016;16(2):537–551.
20. Hahs-Vaughn DL. Applied multivariate statistical concepts. Taylor Francis. 2016.
21. Plichta SB, Kelvin EA. Munro’s statistical methods for health care research. Wolters Kluwer Health/Lippincott Williams Wilkins. 2012.
22. Pahlevan Sharif S, Sharif Nia H. Factor Analysis and Structural Equation Modeling with SPSS and AMOS.
23. Fornell C, Larcker DF. Evaluating structural equation models with unobservable variables and measurement error. J Marketing Res. 1981;18(1):39–50. doi:10.1177/002224378101800104
24. Sharif Nia H, Shafipour V, Allen K-A, Heidari MR, Yazdani-Charati J, Zareiyan A. A second-order confirmatory factor analysis of the moral distress scale-revised for nurses. Nurs Ethics. 2019;26(4):1199–1210. doi:10.1177/0969733017742962
25. Briggs SR, Cheek JM. The role of factor analysis in the development and evaluation of personality scales. J Pers. 1986;54(1):106–148. doi:10.1111/j.1467-6494.1986.tb00391.x
26. Byrne BM. Structural equation modeling with AMOS: basic concepts, applications, and programming, third edition. Taylor Francis. 2016.
27. Wong H. Handbook of partial least squares: concepts, methods and applications: springer handbooks of computational statistics series. Springer Sci Business Media; 2010:2010.
28. Park HS, Dailey R, Lemus D. The use of exploratory factor analysis and principal components analysis in communication research. Hum Commun Res. 2002;28(4):562–577. doi:10.1111/j.1468-2958.2002.tb00824.x
29. Vinzi VE, Chin WW, Henseler J, Wang H. Handbook of Partial Least Squares. 201. Springer; 2010.
30. Lee J, Kang S J. Factors influencing nurses’ intention to care for patients with emerging infectious diseases: application of the theory of planned behavior. Nurs Health Sci. 2020;22:82–90. doi:10.1111/nhs.12652
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
