Back to Journals » Neuropsychiatric Disease and Treatment » Volume 16
Psychometric Analysis of the Perceived Stress Scale Among Healthy University Students
Authors Anwer S , Manzar MD , Alghadir AH, Salahuddin M, Abdul Hameed U
Received 19 June 2020
Accepted for publication 31 August 2020
Published 19 October 2020 Volume 2020:16 Pages 2389—2396
DOI https://doi.org/10.2147/NDT.S268582
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Yuping Ning
Shahnawaz Anwer,1,2 Md Dilshad Manzar,3 Ahmad H Alghadir,1 Mohammed Salahuddin,4 Unaise Abdul Hameed5
1Rehabilitation Research Chair, College of Applied Medical Sciences, King Saud University, Riyadh, Saudi Arabia; 2Department of Building and Real Estate, Hong Kong Polytechnic University, Kowloon, Hong Kong Special Administrative Region; 3Department of Nursing, College of Applied Medical Sciences, Majmaah University, Al Majmaah 11952, Saudi Arabia; 4Pharmacology Division, Department of BioMolecular Sciences, University of Mississippi, Oxford, MS, USA; 5Department of Physiotherapy, Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia
Correspondence: Shahnawaz Anwer
Rehabilitation Research Chair, College of Applied Medical Sciences, King Saud University, Riyadh 1433, Saudi Arabia
Email [email protected]
Background: There is a gradual increase in the prevalence of stress during professional courses. Previous studies reported a high incidence of stress among university students. The psychometric properties of the perceived stress scale-10 (PSS-10) have been established in different populations. The current study aimed to assess psychometric properties of the PSS-10 in Saudi university students.
Methods: Healthy university students (n= 192) participated in this cross-sectional study. All the participants were explained about the aim and procedures of the study. Participants were requested to complete the English version of the PSS, the generalized anxiety disorder-7 (GAD-7), the sleep hygiene index (SHI), and demographic details.
Results: The range of the PSS-10 total score was 0– 35; 1% reported minimum score of 0, but none reported maximum score of 40. Therefore, there was no issue of ceiling or floor effect in the PSS-10 total score. Positive and significant correlations of the PSS total and the PSS Factor-1 (distress perception) with the GAD-7 total score, SHI item-8 and SHI item-13 score support its convergent validity. Negative or no correlation of the PSS Factor-2 score (coping perception) with the GAD-7 total score, SHI item-8 and SHI item-13 scores demonstrate its divergent validity. The internal homogeneity test indicated moderate to strong positive correlations (r=0.60– 0.82) between the PSS Factors and the items loading on them. The internal consistency test showed a good agreement for the PSS Factor-1 and the PSS Factor-2 scores (Cronbach’s alpha 0.78 and 0.71, respectively), suggesting an acceptable level of consistency. Factor analysis favored a 2-Factor model of the PSS in the Saudi students.
Conclusion: The current study supported the use of the PSS-10 to assess the perceived stress among Saudi university students.
Keywords: PSS, stress, university students, validity, reliability
Introduction
Psychological stress results from an imbalance between the external environmental demands and an individual’s perception of meeting them. Studies have suggested that mental stress is often associated with depression, anxiety, and physical conditions including cancer and cardiovascular diseases.1–4 People often experience stress if they realize that their assets are inadequate to handle a situation.5
There is a gradual rise in the prevalence of stress during professional courses.6,7 Previous studies reported a high incidence of stress among university students,8,9 resulting in an increased tendency of the suicidal act.10,11 Emotional stress and other related disorders significantly affect the academic performance as well as professional practice.12,13 Students who perceive medical stress can present with mental distress and further health problems.14,15
University students irrespective of courses often meet various sources of stress for instance lifestyle changes, variable environment, interpersonal relationships, and academic burdens, all of which result in a significant psychological impairment. High risk of perceived stress is present among residents in Saudi Arabia.16 Moreover, medical students in the Arab countries have frequent problems of stress, depression and anxiety.17 Besides, medical students demonstrated a high level of stress in Saudi university.18
The perceived stress scale-10 (PSS-10) is a commonly used scale to assess stress.19 The PSS evaluate the degree to which external demands appear to be higher than individual’s perceived capability to handle the situation.19 The original PSS-10 was considered as a single construct due to the irrelevant distinction between the two different dimensions.20 However, a confirmatory factor analysis (CFA) by Golden-Kreutz suggested that the PSS-10 had predominantly two-dimensional structure.21 Besides, Andreou et al22 indicated that the two-dimensional model of the PSS-10 and the PSS-14 appears to be a better fit. Furthermore, a principal component analysis (PCA) approved the presence of two dimensions of the PSS-10.21
It is widely accepted that gender influences stress and females reported higher levels of daily stressors as compared to males.22,23 McDonough and Walters24 reported approximately 23% higher distress scores in the females than males. Similarly, another study also reported higher stress levels in females as compared to males.25 A recent study also found significantly increased levels of anxiety, depression, and frustration in female than male university students.26 Since the influence of gender on stress is well known, the current study includes only male participant to minimize gender’s effect.
The psychometric properties of the PSS-10 have been established in different populations.27–30 Several past studies have examined the validity of PSS-10 to assess perceived stress among university students.31–37 For example, a previous study examined confirmatory factor analysis (CFA) of PSS-10 and they found the 2-factor model is most suitable to assess perceived stress among the Ethiopian university students.31 Similarly, another study evaluated the principal components factor analysis of PSS-10 and they reported an adequate reliability and validity of PSS-10 to measure perceived stress among Turkish university students.32 Additionally, Lu et al34 conducted construct validity analysis of PSS-10 and they reported that the 2-factor model of the principal component analysis indicated positive (Factor 1) and negative (Factor 2) perception of stress among Chinese university students. Although many studies have been published on the psychometric properties of PSS-10 among university students in different countries, no previous study evaluated the psychometric properties of the PSS-10 in the Saudi population. Therefore, the current study aimed to assess the psychometric properties of the PSS-10 in Saudi university students.
Methods
Participants and Study Design
Healthy university students participated in this cross-sectional study. This study failed to include any female participants because the study was conducted in the male campuses. All the participants were explained about the aim and procedures of the study. Participants were excluded if they had a history of stress-related disorders. Participants were requested to complete the English version of the PSS, the generalized anxiety disorder-7 (GAD-7), the sleep hygiene index (SHI), and demographic details. The participants were requested to provide a written informed consent. The study was approved by the institutional Ethical committee, Rehabilitation Research chair, King Saud University, Saudi Arabia. All the procedures were followed the Declaration of Helsinki.
Measures
PSS-10
The PSS is a 10-item questionnaire designed to evaluate the self-reported amount of stress in the participants by assessing thoughts and feelings in the previous month. Each question is scored from 0 (never) to 5 (very often) with a total possible score range of 0 to 40. A higher score indicates a high level of stress.19
GAD-7
The GAD-7 scale is a 7-item questionnaire designed to assess the self-reported level of anxiety in the participants in the last two weeks. Each question is scored from 0 (not at all) to 3 (nearly every day) with a total score in the range of 0 to 21. The items were constructed to assess symptoms of anxiety as per the Diagnostic and Statistical Manual of Mental Disorders-IV-TR.27 The GAD-7 scale has been found to have psychometric validity in Saudi university students.38
SHI
The SHI is a 13-item questionnaire designed to assess participants' sleep hygiene behaviour. Items in the questionnaire are dichotomous and scored 0 (no) or 1 (yes). The SHI total score (range of 0 to 13) is obtained by adding together all the item scores. A higher SHI total score signifies poor sleep hygiene. In addition, two items of the SHI (item-8 and item 13) also assess stress and worry at bedtime. Therefore, both of these items were used to assess the convergent validity of the PSS.28 The SHI with dichotomous scoring pattern has been validated in Saudi university students.39
Statistical Analysis
SPSS 16.0 for Windows (SPSS Inc., Chicago, USA) along with add on module-AMOS (Analysis of Moment Structures) was used for the statistical analysis. Descriptive statistics including mean, percentage, frequency, skewness and kurtosis index were employed for demographics and item analysis. The Cronbach’s alpha test was used to assess the internal consistency of the scale. The Spearman correlation test was used to evaluate the internal homogeneity and the convergent validity. Sample size adequacy and the sample suitability for the factor analysis of the PSS scores were evaluated using the anti-image matrix, Determinant, Bartlett’s test of Sphericity, Inter-item Correlation, Communality, and Kaiser-Meyer-Olkin Test of Sampling Adequacy (KMO). The Confirmatory factor analysis (CFA) was conducted using Maximum likelihood extraction. CFA tested two models, i.e. 1-Factor model, and 2-Factor correlated model (found valid in previous studies).29,31 Multiple indices from various classes of fit measurements were also employed.30 According to standard practice, model fit was evaluated using the adjusted goodness of fit index (AGFI), chi-square statistics, Akaike information criterion (AIC), goodness of fit index (GFI), comparative fit index (CFI), parsimony normed fit index (PNFI), Tucker–Lewis index (TLI), root-mean-square error of approximation (RMSEA), and root-mean-square residual (RMR).
Results
Participants’ Characteristics
Table 1 details the participant’s characteristics. The average scores for the PSS-10, the GAD-7 and the SHI were 16.16, 5.27, and 6.70, respectively. Most of the participants (79%) were involved in the light physical activity.
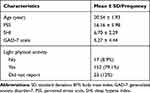 |
Table 1 Participant Characteristics of Saudi University Students |
Item Analysis and Internal Consistency
Item analysis for the PSS-10 is presented in Table 2. Item analysis indicated that data did not have issues of skewness or kurtosis. Floor and ceiling effects were calculated if more than 15% of the participants reported the lowest or the highest score, respectively.31,32 The range of the PSS-10 total score was 0–35; 1% reported minimum score of 0 but none reported the maximum score of 40. Therefore, there was no issue of the ceiling or the floor effect in the PSS-10 total score.
 |
Table 2 Descriptive Statistics of the Perceived Stress Scale-10 (PSS-10) in Saudi University Students |
Convergent and Divergent Validity
Table 3 presents the convergent and the divergent validity. Positive and significant correlations of the PSS total and the PSS Factor-1 scores (distress perception) with the GAD-7 total score, SHI item-8 and SHI item-13 scores confirm the convergent validity. Negative or no correlation of the PSS Factor-2 score (coping perception) with the GAD-7 total score, SHI item-8 and SHI item-13 scores demonstrate the divergent validity of the PSS in this population of Saudi male students. This is because the PSS Factor-2 score does not assess stress, but it measures the coping strategy to stress.
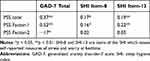 |
Table 3 Convergent and Divergent Validity: Correlation of the Perceived Stress Scale-10 (PSS-10) with Related Measures in Saudi University Students |
Homogeneity Test
The internal homogeneity test indicated moderate to strong positive correlations (r=0.60–0.82) between the PSS Factors and the items loading on them (Table 4). The internal consistency test indicated a good agreement for the Factor-1 and the Factor-2 of the PSS scale (Cronbach’s alpha 0.78 and 0.71, respectively), suggesting an acceptable level of consistency (Table 4).
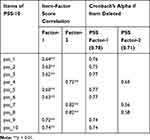 |
Table 4 Internal Consistency and Rotated Factor Matrix of the 2-Factor Model of the Perceived Stress Scale-10 (PSS-10) in Saudi University Students |
Sample Size Adequacy
Table 5 illustrates measures of sample size adequacy and the sample suitability for factor analysis of the PSS-10 scores. The anti-image (>0.5) and the Kaiser-Meyer-Olkin Test of Sampling Adequacy (KMO) (>0.5) suggests that the sample size is adequate.33 The Bartlett’s test (<.001) signifies that the original matrix is not an identity matrix and therefore, there is no issue of singularity in the measured variables-the PSS item scores.33 The determinant score (>.01) indicates that there was no problem of multicollinearity in the PSS item scores.33
 |
Table 5 Measures of Sample Size Adequacy and Sample Suitability for Factor Analysis of the Perceived Stress Scale-10 (PSS-10) Scores in Saudi University Students |
Factor Analysis
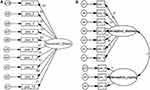
Table 6 shows that the 2-Factor model (Figure 1) had the best fit with lowest values for AIC, χ2 and χ2/df, and optimal values for AIC, PNFI, CFI, TLI, and RMSEA.
 |
Table 6 Fit Statistics of the Perceived Stress Scale-10 (PSS-10) in Saudi University Students |
Discussion
The current study found the evidence for the psychometric validation of the PSS-10 in Saudi university students. There were no floor and ceiling effects for the PSS total scores indicating that even at the highest or the lowest scores of the PSS total score, the variance of the measures is not numerous.32 This supports the construct validity as well the content validity of the PSS in Saudi university students as a self-rated measure of stress. In a previous study, Wu and Amtmann did not find any major floor and/or ceiling effects in patients with Multiple Sclerosis.40
Stress disorders are commonly associated with anxiety41 and impaired sleep,42 whereas sleep impairment may be due to bedtime stress and worries.43 Therefore, the correlation between the PSS and the measures of anxiety, i.e. the GAD-7 scale27 and bedtime stress and worries as assessed by items of the SHI28 were used to confirm the convergent validity of the PSS. The results of the current study indicated that the correlation between the PSS total and the PSS Factor-1 scores with the GAD-7 total, SHI item-8 and SHI item-13 scores confirm the convergent validity of the PSS in Saudi university students. Past studies have also confirmed the convergent validity of PSS-10 in various populations by evaluating its associations with measures of anxiety.44–46 The studies assessed the convergent validity of the PSS by evaluating its associations with the measures of anxiety. Perera et al46 used the Spielberger Trait Anxiety Inventory in community-dwelling adults to establish the convergent validity of the PSS. Similarly, the Hospital Anxiety and Depression Scale was used to assess convergent validity of the PSS in patients with the systemic lupus erythematosus,47 while the GAD-7 was employed in community-dwelling adults.48 Maroufizadeh et al49 reported a moderate association between the PSS-10 and anxiety sub-item of the Depression Anxiety Stress-21 scale in adults with asthma.49
The Cronbach’s alpha value for the two factors in the current study found an acceptable consistency with little higher values for the Factor-1, which is a measure of distress. However, in a systematic review, Lee50 reported higher values, i.e. 0.74 to 0.91 in diverse populations. The internal homogeneity as demonstrated by the moderate to strong correlations between the PSS factors and their respective items, further validate the PSS-10 in this population of Saudi university students. Possibly no previous study had reported the internal homogeneity, as most of the earlier studies had depended on the evaluation of the internal consistency using the Cronbach’s alpha.
The 2-Factor model indicated the best fit. Similarly, previous studies have also supported the 2-factor model of PSS-10.31,50,51 Moreover, Nielsen et al52 also indicated better statistical fit for a two-dimensional model than a one-dimensional model of the PSS-10 among Danish nationals. Another study reported acceptable statistical fit for a two-dimensional PSS-10 among Greeks.22 Furthermore, Golden-Kreutz21 reported a “poor fit” for the one-dimensional model, although the statistics for the two-dimensional model suggested “close fit”. In contrast, some studies supported the 1-factor47,48,53 model, while some favored a bi-factor50,51 model of PSS-10. Future studies involving multi-center designs with socio-culturally distinct populations are recommended to assess inconsistencies in the factorial validity.
The current study had potential limitations. First, the result of the present study is only limited to male students. Second, the current study did not assess the concurrent validity. Therefore, future studies using the diagnostic clinical interview to determine the concurrent validity of the PSS-10 in Saudi students are warranted. Third, the current study used the original English version of questionnaire; however, the participants were not the native speakers that might result poor understanding of verbal descriptors and thus affect the validity of responses. Therefore, future studies may be conducted using an Arabic translated version of the questionnaire to validate these results.
Conclusion
The current study reports adequate item analysis, internal consistency, convergent and divergent validity, and factorial validity that supports the use of PSS-10 to assess the perceived stress among Saudi university students. Further research is recommended to determine the diagnostic validity of PSS-10 for measuring perceived stress in these population.
Acknowledgments
The authors are grateful to the Deanship of Scientific Research, King Saud University for funding through Vice Deanship of Scientific Research Chairs. The authors extend their appreciation to the Deanship of Scientific Research at Majmaah University for funding this work under Project Number No (RGP-2019-40).
Funding
This project was funded by the Deanship of Scientific Research, King Saud University through Vice Deanship of Scientific Research Chairs and the Deanship of Scientific Research at Majmaah University (Project Number No: RGP-2019-40). The funding body played no role in study design, the writing of the manuscript or the decision to submit the manuscript for publication.
Disclosure
The authors report no conflicts of interest for this work.
References
1. Bomhof-Roordink H, Seldenrijk A, van Hout HP, van Marwijk HW, Diamant M, Penninx BW. Associations between life stress and subclinical cardiovascular disease are partly mediated by depressive and anxiety symptoms. J Psychosom Res. 2015;78(4):332–339. doi:10.1016/j.jpsychores.2015.02.009
2. Payne JK. State of the science: stress, inflammation, and cancer. Oncol Nurs Forum. 2014;41(5):533–540.
3. Salleh MR. Life event, stress and illness. Malays J Med Sci. 2008;15(4):9–18.
4. Schneiderman N, Ironson G, Siegel SD. Stress and health: psychological, behavioral, and biological determinants. Annu Rev Clin Psychol. 2005;1:607–628. doi:10.1146/annurev.clinpsy.1.102803.144141
5. Folkman S. Stress: appraisal and Coping. In: Gellman MD, Turner JR, editors. Encyclopedia of Behavioral Medicine. New York: Springer New York; 2013:1913–1915.
6. Aktekin M, Karaman T, Senol YY, Erdem S, Erengin H, Akaydin M. Anxiety, depression and stressful life events among medical students: a prospective study in Antalya, Turkey. Med Educ. 2001;35:12–17. doi:10.1046/j.1365-2923.2001.00726.x
7. Guthrie EA, Black D, Bagalkote H, Shaw C, Campbell M, Creed F. Psychological stress and burnout in medical students: a five-year prospective longitudinal study. J R Soc Med. 1998;91:237–243. doi:10.1177/014107689809100502
8. Dahlin M, Joneborg N, Runeson B. Stress and depression among medical students: a cross sectional study. Med Educ. 2005;39:594–604. doi:10.1111/j.1365-2929.2005.02176.x
9. Zocolillo M, Murphy GE, Wetzel RD. Depression among medical students. J Affect Disord. 1986;11:91–96. doi:10.1016/0165-0327(86)90065-0
10. Malathi A, Damodaran A. Stress due to exams in medical students role of yoga. Indian J Physiol Pharmacol. 1999;43:218–224.
11. Bramness JA, Fixdal TC, Vaglum P. Effect of medical school stress on the mental health of medical students in early and late clinical curriculum. Acta Psychiatr Scand. 1991;84:340–345. doi:10.1111/j.1600-0447.1991.tb03157.x
12. Tyssen R, Vaghum P, Grønvold NT, Ekeberg O. Suicide ideation among medical students and youth physicians: a nationwide and prospective of prevalence and predictors. J Affect Disord. 2001;64:69–79. doi:10.1016/S0165-0327(00)00205-6
13. Tyssen R, Hem E, Vaghum P, Grønvold NT, Ekeberg Ø. The process of suicidal planning among medical doctors: predictors in a longitudinal Norwegian sample. J Affect Disord. 2004;80:191–198. doi:10.1016/S0165-0327(03)00091-0
14. Vitaliano PP, Russo J, Carr JE, Heerwagen JH. Medical school pressures and their relationship to anxiety. J Nerve Ment Dis. 1984;172:730–736. doi:10.1097/00005053-198412000-00006
15. Tyssen R, Vaglum P, Gronvold NT, Ekeberg O. Factors in medical school that predict postgraduate mental health problems in need of treatment. A nationwide and longitudinal study. Med Educ. 2001;35:110–120. doi:10.1046/j.1365-2923.2001.00770.x
16. Alosaimi FD, Kazim SN, Almufleh AS, Aladwani BS, Alsubaie AS. Prevalence of stress and its determinants among residents in Saudi Arabia. Saudi Med J. 2015;36(5):605–612. doi:10.15537/smj.2015.5.10814
17. El-Gilany AH, Amr M, Hammad S. Perceived stress among male medical students in Egypt and Saudi Arabia: effect of sociodemographic factors. Ann Saudi Med. 2008;28(6):442–448.
18. Abdel Rahman AG, Al Hashim BN, Al Hiji NK, Al-Abbad Z. Stress among medical Saudi students at College of Medicine, King Faisal University. J Prev Med Hyg. 2013;54(4):195–199.
19. Cohen S, Kamarck T, Mermelstein R. A global measure of perceived stress. J Health Soc Behav. 1983;24(4):385–396.
20. Cohen S, Tyrrell DA, Smith AP. Negative life events, perceived stress, negative affect, and susceptibility to the common cold. J Pers Soc Psychol. 1993;64(1):131–140. doi:10.1037/0022-3514.64.1.131
21. Golden-Kreutz DM, Browne MW, Frierson GM, Andersen BL. Assessing stress in cancer patients: a second-order factor analysis model for the perceived stress scale. Assessment. 2004;11(3):216–223. doi:10.1177/1073191104267398
22. Andreou E, Alexopoulos EC, Lionis C, et al. Perceived stress scale: reliability and validity study in Greece. Int J Environ Res Public Health. 2011;8(8):3287–3298. doi:10.3390/ijerph8083287
23. Tamres LK, Janicki D, Helgeson VS. Sex differences in coping behavior: a meta-analytic review and an examination of relative coping. Pers Soc Psychol Rev. 2002;6(1):2–30. doi:10.1207/S15327957PSPR0601_1
24. McDonough P, Walters V. Gender and health: reassessing patterns and explanations. Soc Sci Med. 2001;52(4):547–559. doi:10.1016/S0277-9536(00)00159-3
25. Matud MP. Gender differences in stress and coping styles. Pers Individ Dif. 2004;37(7):1401–1415. doi:10.1016/j.paid.2004.01.010
26. Calvarese M. The effect of gender on stress factors: an exploratory study among university students. Soc Sci. 2015;4(4):1177–1184. doi:10.3390/socsci4041177
27. Hogan JM, Carlson JG, Dua J. Stressors and stress reactions among university personnel. Int J Stress Manag. 2002;9(4):289–310. doi:10.1023/A:1019982316327
28. Khalili R, SiratiNir M, Ebadi A, Tavallai A, Habibi M. Validity and reliability of the Cohen 10-item perceived stress scale in patients with chronic headache: Persian version. Asian J Psychiatr. 2017;26:136–140. doi:10.1016/j.ajp.2017.01.010
29. Klein EM, Brähler E, Dreier M, et al. The German version of the perceived stress scale - psychometric characteristics in a representative German community sample. BMC Psychiatr. 2016;16:159.
30. Nordin M, Nordin S. Psychometric evaluation and normative data of the Swedish version of the 10‐item perceived stress scale. Scand J Psychol. 2013;54(6):502–507. doi:10.1111/sjop.12071
31. Manzar MD, BaHammam AS, Hameed UA, et al. Dimensionality of the Pittsburgh sleep quality index: a systematic review. Health Qual Life Outcomes. 2018;16(1):89. doi:10.1186/s12955-018-0915-x
32. Manzar MD, Salahuddin M, Peter S, et al. Psychometric properties of the perceived stress scale in Ethiopian university students. BMC Public Health. 2019;19(1):41. doi:10.1186/s12889-018-6310-z
33. Örücü MÇ, Demir A. Psychometric evaluation of perceived stress scale for Turkish university students. Stress Health. 2009;25(1):103–109. doi:10.1002/smi.1218
34. Lu W, Bian Q, Wang W, Wu X, Wang Z, Zhao M. Chinese version of the perceived stress scale-10: a psychometric study in Chinese university students. PLoS One. 2017;12(12):e0189543. doi:10.1371/journal.pone.0189543
35. Denovan A, Dagnall N, Dhingra K, Grogan S. Evaluating the perceived stress scale among UK university students: implications for stress measurement and management. Stud High Educ. 2019;44(1):120–133. doi:10.1080/03075079.2017.1340445
36. Roberti JW, Harrington LN, Storch EA. Further psychometric support for the 10‐item version of the perceived stress scale. J Coll Couns. 2006;9(2):135–147. doi:10.1002/j.2161-1882.2006.tb00100.x
37. Smith KJ, Rosenberg DL, Timothy Haight G. An assessment of the psychometric properties of the perceived stress scale‐10 (PSS 10) with business and accounting students. Account Perspect. 2014;13(1):29–59. doi:10.1111/1911-3838.12023
38. Alghadir A, Manzar MD, Anwer S, Albougami A, Salahuddin M. Psychometric properties of the generalized anxiety disorder scale among Saudi University male students. Neuropsychiatr Dis Treat. 2020;16:1427–1432. doi:10.2147/NDT.S246526
39. Anwer S, Alghadir A, Manzar MD, Noohu MM, Salahuddin M, Li H. Psychometric analysis of the sleep hygiene index and correlation with stress and anxiety among Saudi University students. Nat Sci Sleep. 2019;11:325. doi:10.2147/NSS.S222440
40. Wu SM, Amtmann D. Psychometric evaluation of the perceived stress scale in multiple sclerosis. ISRN Rehabil. 2013;2013.
41. Bergdahl J, Bergdahl M. Perceived stress in adults: prevalence and association of depression, anxiety and medication in a Swedish population. Stress Health. 2002;18(5):235–241. doi:10.1002/smi.946
42. Lemma S, Gelaye B, Berhane Y, Worku A, Williams MA. Sleep quality and its psychological correlates among university students in Ethiopia: a cross-sectional study. BMC Psychiatr. 2012;12(1):237. doi:10.1186/1471-244X-12-237
43. Åkerstedt T, Kecklund G, Axelsson J. Impaired sleep after bedtime stress and worries. Biol Psychol. 2007;76(3):170–173. doi:10.1016/j.biopsycho.2007.07.010
44. Baik SH, Fox RS, Mills SD, et al. Reliability and validity of the perceived stress scale-10 in Hispanic Americans with English or Spanish language preference. J Health Psychol. 2017;1359105316684938.
45. Mills SD, Azizoddin D, Racaza GZ, Wallace DJ, Weisman MH, Nicassio PM. The psychometric properties of the perceived stress scale-10 among patients with systemic lupus erythematosus. Lupus. 2017;26(11):1218–1223. doi:10.1177/0961203317701844
46. Perera MJ, Brintz CE, Birnbaum-Weitzman O, et al. Factor structure of the perceived stress scale-10 (PSS) across English and Spanish language responders in the HCHS/SOL Sociocultural Ancillary Study. Psychol Assess. 2017;29(3):320–328. doi:10.1037/pas0000336
47. Michaelides MP, Christodoulou A, Kkeli N, Karekla M, Panayiotou G. Structure factorielle de l’échelle de stress perçu et implications pour la cotation. Revue Europeenne de Psychologie Appliquee. 2016;66:309–316. doi:10.1016/j.erap.2016.07.002
48. Mastin DF, Bryson J, Corwyn R. Assessment of sleep hygiene using the sleep hygiene index. J Behav Med. 2006;29(3):223–227. doi:10.1007/s10865-006-9047-6
49. Maroufizadeh S, Zareiyan A, Sigari N. Reliability and validity of Persian version of perceived stress scale (PSS-10) in adults with asthma. Arch Iran Med. 2014;17(5):361–365.
50. Lee EH. Review of the psychometric evidence of the perceived stress scale. Asian Nurs Res (Korean Soc Nurs Sci). 2012;6(4):121–127.
51. Salahuddin M, Maru TT, Kumalo A, et al. Validation of the Pittsburgh sleep quality index in community dwelling Ethiopian adults. Health Qual Life Outcomes. 2017;15:58. doi:10.1186/s12955-017-0637-5
52. Nielsen MG, Ørnbøl E, Vestergaard M, et al. The construct validity of the perceived stress scale. J Psychosom Res. 2016;84:22–30. doi:10.1016/j.jpsychores.2016.03.009
53. Lim CR, Harris K, Dawson J, et al. Floor and ceiling effects in the OHS: an analysis of the NHS PROMs data set. BMJ Open. 2015;5:e007765. doi:10.1136/bmjopen-2015-007765
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.