Back to Journals » OncoTargets and Therapy » Volume 7
Prognostic significance of the combined expression of neutral endopeptidase and dipeptidyl peptidase IV in intrahepatic cholangiocarcinoma patients after surgery resection
Authors Zhu J, Guo X, Qiu B, Li Z, Xia N, Yang Y, Liu P
Received 10 November 2013
Accepted for publication 18 December 2013
Published 17 February 2014 Volume 2014:7 Pages 297—304
DOI https://doi.org/10.2147/OTT.S57355
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Jianyong Zhu,1,* XiaoDong Guo,2,* Baoan Qiu,1 Zhiyan Li,2 Nianxin Xia,1 Yingxiang Yang,1 Peng Liu1
1Department of Hepatobiliary Surgery, Navy General Hospital, PLA, Beijing, People's Republic of China; 2302 Hospital of PLA, Beijing, People's Republic of China
*These authors contributed equally to this work
Aim: The aim of this study was to investigate the relationship between the expression of neutral endopeptidase (NEP) and dipeptidyl peptidase IV (DPP IV) proteins, and the clinical significance of the two proteins in patients with intrahepatic cholangiocarcinomas (IHCC).
Methods: Expression patterns and subcellular localizations of NEP and DPP IV proteins in 186 primary IHCC and 60 noncancerous liver tissue specimens were detected by immunohistochemistry.
Results: Both the expression of NEP and DPP IV proteins in IHCC tissues were significantly higher than those in noncancerous liver tissues (both P<0.001). Of 186 patients with IHCC, 128 (68.82%) highly expressed both NEP and DPP IV proteins. In addition, the coexpression of NEP and DPP IV proteins was significantly associated with advanced tumor stage (P=0.009), positive lymph node metastasis (P=0.016) and distant metastasis (P=0.013), and the presence of recurrence (P=0.027). Moreover, Kaplan–Meier analysis showed that IHCC patients with high NEP expression, high DPP IV expression, and combined overexpression of NEP and DPP IV proteins all had poorer overall survival and early recurrence after surgery. Furthermore, Cox analysis suggested that NEP expression, DPP IV expression, and combined expression of NEP and DPP IV proteins were all independent prognostic markers for overall survival and recurrence-free survival in patients with IHCC.
Conclusion: Our data suggest, for the first time, that both the expression of NEP and DPP IV proteins may be upregulated in human IHCC tissues and the combined expression of NEP and DPP IV proteins may play important roles in progression and prognosis of patients with IHCC.
Keywords: clinicopathological characteristics, tumor progression, prognosis
Introduction
Cholangiocarcinomas are relatively rare malignancies that arise from the malignant transformation of bile duct epithelium anywhere along the biliary tree from the small bile ducts and bile ductules to the large bile ducts at the hilum of the liver or outside the liver.1 Cholangiocarcinomas include intrahepatic cholangiocarcinomas (IHCC) and extrahepatic cholangiocarcinomas. IHCC accounts for 5% of primary malignant liver tumors and is one of the most malignant solid tumors found in the digestive organs.2 It is characterized by strong invasiveness and early metastasis.3 Although the surgical resection provides the opportunity for long-term survival, the clinical outcome of patients with IHCC is very poor, with a 5-year survival rate ranging from 25% to 35% because lymph nodal/distant metastasis or micrometastasis are present early in patients, limiting the surgery option.4 Since recent studies have demonstrated that complex molecular and cellular events may be implicated in carcinogenesis and prognosis of IHCC, it is very important to investigate the molecular mechanisms and to identify the efficient diagnostic and prognostic markers of IHCC.
Neutral endopeptidase (NEP) is a zinc-dependent, cell surface metallopeptidase that is involved in the cleavage and inactivation of certain peptide hormones and is important for signal transduction, including transduction of enkephalins, bombesin, and substrate P.5,6 Under nonpathological conditions, NEP is widely distributed in the epithelial cells of the kidney, liver, stomach, intestine, breast, lung, and prostate gland.7 Under pathological conditions, NEP has been demonstrated to play a crucial role in migration, survival, and apoptosis of various cancer cells.8 NEPs’ diagnostic and prognostic values were originally discovered in acute lymphoblastic leukemia with elaboration of rabbit antisera against leukemic cells.9 Subsequently, accumulating studies have indicated that NEP is not specific to hematopoietic malignancies, but is also abnormally expressed by several solid tumors such as nephroblastoma, neuroblastoma, melanoma, renal carcinoma, lung cancer, gastric cancer, liver cancer, pancreatic cancer, breast cancer, endometrial stromal sarcoma, prostate cancer, and bladder cancer.10–18 It also can distinguish primary hepatocellular carcinoma from secondary liver metastases originating from other organs.19 However, the NEP functions in IHCC are still unknown.
Dipeptidyl peptidase IV (DPP IV) is a transmembrane serine protease that is a multifunctional membrane-bound glycoprotein containing a short cytoplasmic domain comprising of six amino acids, a transmembrane region, and an extracellular domain with DPP IV activity, capable of cleaving NH2-terminal dipeptides from polypeptides with either L-proline or L-alanine at the penultimate position.20 Under nonpathological conditions, DPP IV is widely expressed in many tissues including placenta, kidney, lung, liver, skeletal muscle, heart, brain, and pancreas.21 Functionally, it acts as a serine protease, receptor, costimulatory protein, adhesion molecule, and mediator of apoptosis.22 Accumulating evidence has demonstrated the involvement of DPP IV in a variety of cancer-derived cell lines and tissues. The upregulated DPP IV expression is associated with the aggressiveness of T and B lymphomas, leukemias, thyroid follicular cancer, papillary carcinomas, astrocytic tumors, and gastrointestinal stromal tumor.23–27 DPP IV acts either as a tumor suppressor or a tumor promoter by suppressing or promoting tumor metastasis and tumor growth. However, the roles of DPP IV in IHCC are still unknown.
As mentioned above, both NEP and DPP IV function as regulatory proteins in cancer progression and development by modulating the effects of biologically active peptides. Their roles in tumorigenesis and development of IHCC are an emerging issue with potential clinical implications. Therefore, the aim of the current study was to investigate both the relationship between the expression of NEP and DPP IV proteins, and the clinical significance of the two proteins in patients with IHCC.
Materials and methods
Patients and tissue samples
The study was approved by the Research Ethics Committee of Navy General Hospital and 302nd Hospital of PLA, Beijing, People’s Republic of China. Informed consent was obtained from all patients. All specimens were handled and made anonymous according to the ethical and legal standards.
One hundred and eighty-six formalin-fixed and paraffin-embedded IHCC tissues and 60 noncancerous liver tissues obtained from 186 consecutive patients who underwent primary hepatectomy due to IHCC in the Navy General Hospital and 302nd Hospital of PLA, Beijing, People’s Republic of China, from December 2000 to January 2006 were retrieved for immunohistochemistry analysis. Noncancerous liver tissues were used as control tissues. The study population consisted of patients with IHCC as confirmed by pathological analysis. Tumor staging was determined according to the sixth edition of the tumor–node–metastasis classification of the International Union against Cancer.28 None of the patients recruited in this study had chemotherapy or radiotherapy before the surgery. Patients were excluded from this cohort with the following exclusion criteria: uncontrolled infection; previously received any anticancer therapy; pregnancy and lactation; prior malignancy; impaired heart, lung, liver, or kidney function; and/or previous malignant disease. The background of primary liver diseases of the 186 patients with IHCC in this study was in all cases liver cirrhosis. The clinicopathological features of 186 patients with IHCC are summarized in Table 1.
All 186 IHCC patients received follow-up until death from disease, or until the latest clinical therapy at the end of this study. Overall survival was defined as the interval between the dates of surgery and death. Recurrence-free survival was defined as the interval between the dates of surgery and recurrence; if recurrence was not diagnosed, patients were censored on the date of death or the last follow-up. Deaths from other causes were treated as censored cases. The patients’ follow-up time ranged from 0.8–132.2 months, and the median survival at the last follow-up was 21.8 months. The median follow-up period was 22.6 months. All patients were observed until March 2012. Postoperative surveillance included routine clinical and laboratory examinations every 3rd month, computed tomography scans of the abdomen, and radiographs of the chest every 3rd month. After 5 years, the examination interval was extended to 12 months.
Immunohistochemistry analysis
The expression of NEP and DPP IV proteins was detected in IHCC and noncancerous liver specimens from 186 patients with IHCC by immunohistochemistry analysis. Surgical specimens were fixed in 10% formalin, embedded in paraffin, and sectioned at a 4 μm thickness. Staining was done using avidin-biotin complex with a microprobe manual stainer (Thermo Fisher Scientific, Waltham, MA, USA). The slide to which a paraffin section was attached went through deparaffinization and hydration, and was then treated with a solution of peroxidase-blocking reagent (Agilent Technologies, Santa Clara, CA, USA) to exhaust endogenous peroxidase activity. The sections were processed with antigen retrieval by being boiled in citrate buffer (pH 6.0) for 20 minutes and then cooled for an additional 20 minutes at room temperature. Subsequently, the slides were incubated overnight with the primary antibodies against anti-NEP mouse monoclonal antibody (#sc-46656; Santa Cruz Biotechnology, Inc., Dallas, TX, USA) or anti-DPP IV goat polyclonal antibody (#AF1180, R&D Systems, Minneapolis, MN, USA) at 4°C. Secondary antibodies (mouse anti-goat IgG-B [#sc-2489] and goat anti-mouse IgG-B [#sc-2039]; Santa Cruz Biotechnology, Inc) for the detection of primary antibodies were attached to biotin and reacted for 10 minutes and then washed with buffer solution and reacted with horseradish peroxidase for 10 minutes. Being washed again, peroxidase activity was visualized with 3,3’-diaminobenzidine (DAB) as a chromogen. All sections were rinsed and counterstained lightly with Harris’s hematoxylin. The negative controls were processed in a similar manner with phosphate-buffered saline (PBS) instead of primary antibody. The positive expressions of NEP and DPP IV proteins confirmed by western blotting were used as positive controls for immunostaining.
Following a hematoxylin counterstaining, immunostaining was scored by two independent experienced pathologists who were blinded to the clinicopathological parameters and clinical outcomes of the patients. The scores of the two pathologists were compared and any discrepant scores were trained through re-examining the stainings by both pathologists to achieve a consensus score. The number of positive-staining cells showing immunoreactivity in cytoplasm and membrane for both NEP and DPP IV in ten representative microscopic fields was counted and the percentage of positive cells was calculated. The percentage scoring of immunoreactive tumor cells was as follows: 0 (0%); 1 (1%–10%); 2 (11%–50%); and 3 (>50%). The staining intensity was visually scored and stratified as follows: 0 (negative); 1 (weak); 2 (moderate); and 3 (strong). A final immunoreactivity score (IRS) was obtained for each case by multiplying the percentage score and the intensity score. Therefore, tumors with an IRS exceeding median of total IRSs for NEP or DPP IV were deemed to be high expressions of NEP or DPP IV; all other scores were considered to be low expressions of NEP or DPP IV.
Statistical analysis
The software of SPSS version 13.0 for Windows (IBM Corporation, Armonk, NY, USA) and SAS 9.1 (SAS Institute Inc, Cary, NC, USA) were used for statistical analysis. The chi-squared test was used to show differences in categorical variables. Correlations between NEP and DPP IV expression were calculated using Spearman’s correlation. Patient survival and the differences in patient survival were determined by the Kaplan–Meier method and the log-rank test, respectively. A Cox regression analysis (proportional hazard model) was performed for the multivariate analyses of prognostic factors. Differences were considered statistically significant when P was less than 0.05.
Results
Expression and localization of NEP and DPP IV in human IHCC tissues
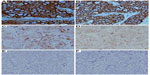
Immunohistochemistry assay was performed to detect the expression patterns and subcellular localizations of NEP and DPP IV proteins in 186 primary IHCC and 60 noncancerous liver tissue specimens. As shown in Figure 1, both NEP and DPP IV positive immunostainings were localized in the cytoplasm and membrane of tumor cells in IHCC tissues, which was consistent with the previous studies of other cancers.17,27 The expression of both NEP and DPP IV proteins were significantly higher in IHCC tissues than those in noncancerous liver tissues (IRS for NEP: 5.66±0.38 versus 2.02±0.11, P<0.001; IRS for DPP IV: 6.18±0.41 versus 2.06±0.15, P<0.001). Of 186 patients with IHCC, 128 (68.82%) had high expression of both NEP and DPP IV, 26 (13.98%) had low expression of both NEP and DPP IV, 20 (10.75%) had NEP-high and DPP IV-low expression, and 12 (6.45%) had NEP-low and DPP IV-high expression. According to the Spearman’s correlation analysis, a significant correlation was found between NEP expression and DPP IV expression in IHCC tissues (r=0.86, P<0.001).
Correlation of NEP and DPP IV expression with the clinicopathologic characteristics of human IHCC tissues
Next, we analyzed the correlations of NEP and DPP IV expression and combined expression of NEP/DPP IV with various clinicopathologic parameters of IHCC tissues. As shown in Table 1, aberrant NEP and DPP IV expression were both observed more frequently in IHCC tissues with advanced tumor stage than in those with early tumor stage (both P=0.01). In addition, the expression of NEP protein was significantly higher in the IHCC tissues with positive lymph node (P=0.006) and distant metastases (P=0.008) than in those with negative lymph-node and distant metastases. Moreover, the abnormal DPP IV expression was significantly associated with IHCC tissues with the presence of recurrence (P=0.012). Furthermore, the coexpression of NEP and DPP IV proteins was significantly associated with advanced tumor stage (P=0.009), positive lymph node (P=0.016) and distant metastases (P=0.013), and the presence of recurrence (P=0.027).
Prognostic implications of NEP and DPP IV expression in patients with IHCCs
The associations of NEP and DPP IV expression with overall survival and recurrence-free survival of patients with IHCCs were analyzed by the Kaplan–Meier method and the log-rank test. As shown in Figure 2, there was a trend that 5-year overall survival in the group with high NEP expression was significantly poorer than that in the group with low NEP expression (P<0.001, log-rank test; Figure 2A). Similarly, a significant relationship was also found between NEP expression and 5-year recurrence-free survival (P<0.001, log-rank test; Figure 2B). Regarding DPP IV, the overall survival (P<0.001; Figure 2C) and the recurrence-free survival (P<0.001; Figure 2D) of IHCC patients with high DPP IV expression were both significantly shorter than those with low DPP IV expression. More interestingly, the association between coexpression of NEP/DPP IV and the survival rates were tested by the method of Kaplan–Meier. The chi-square value by log rank (Mantel–Cox) indicated a significant difference among different groups with regard to the conjoined expression status of NEP/DPP IV (Figure 2E and F). The results by pairwise comparison showed that the statistically significant difference of overall survival and recurrence-free survival existed between NEP-high/DPP IV-high patients and any of the other three groups (both P<0.001). In all four groups, NEP-high/DPP IV-high patients had the poorest prognosis.
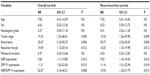
Furthermore, in a multivariate Cox model including patients’ age, sex, histological grade, tumor stage, lymph node and distant metastasis status, recurrence status, resection margin status, perineural invasion status, NEP expression, DPP IV expression, and combined NEP/DPP IV expression, we found that tumor stage (both P=0.009), recurrence status (both P=0.006), resection margin status (both P=0.012), NEP expression (P=0.012 and 0.016, respectively), DPP IV expression (P=0.015 and 0.018, respectively) and combined expression of NEP and DPP IV proteins (P=0.008 and 0.01, respectively) were all independent prognostic markers for overall survival and recurrence-free survival in patients with IHCC (Table 2).
Discussion
It is extremely important to identify efficient markers for early detection, treatment, prediction of disease progression, and prevention of IHCC. In the current study, we confirmed that the overexpression of NEP and DPP IV proteins both mainly occurred in the cytoplasm and cell membrane of tumor cells in IHCC tissues relative to noncancerous liver tissues. Both the increased expression of NEP and DPP IV proteins were significantly associated with aggressive clinicopathological features of IHCC. We observed the coexpression of NEP and DPP IV proteins to be associated with tumor stage, tumor metastasis, and patients’ prognosis. Taken together, our results suggest for the first time that the coexpression of NEP and DPP IV proteins may be a useful diagnostic and prognostic marker in IHCC patients.
A previous study has demonstrated that several proteinases are implicated in tumorigenesis, tumor growth, and dissemination of various human cancers.29 Most efforts have been directed towards the understanding of the role of matrix metalloproteinases. However, the role of other proteinases such as peptidases in tumor progression has not been fully elucidated. Both NEP and DPP IV are glycopeptidases and have been broadly related to pivotal roles in cancer pathophysiology.5,20 Functionally, the two proteins act as regulatory proteins in cancer progression and development by modulating the effects of biologically active peptides. Notably, NEP function in cancer varies by tissue type. For example, NEP promotes proliferation of gastric cancer cell lines16 but suppresses lung and pancreas cancer cell lines.13,17 In line with these opposing effects, the prognostic significance of NEP expression may vary between different tumor types. For example, NEP expression is a favorable prognostic factor in hepatocellular carcinoma19 and diffuse large B cell lymphoma,9 whereas it predicts poor outcome in prostate cancer, renal carcinoma, breast cancer, and endocrine pancreas cancer.10,11,17 According to our data in the current study, NEP expression was dramatically upregulated in IHCC tissues compared with noncancerous liver tissues. In addition, the increased expression of NEP protein was significantly associated with advanced tumor progression and unfavorable prognosis in patients with IHCC suggesting that NEP protein may function as a tumor promoter in IHCC. Regarding DPP IV, it also has pro-oncogenic and anti-oncogenic activities in different human cancers. For example, the enhanced DPP IV activity has been found in lung squamous cell carcinoma as compared with that in normal lung tissue;23 the upregulated DPP IV expression has been demonstrated to be associated with the aggressiveness of T and B lymphomas and leukemias, thyroid follicular cancer, papillary carcinomas, astrocytic tumors, and gastrointestinal stromal tumor.24,25 Contrarily, the decreased expression of DPP IV has been observed in prostatic, colorectal, hematological, and renal tumors.26,27,30 An inverse correlation between DPP IV expression and the grade of tumor has also been observed in endometrial cancers.31 We found here that the upregulation of DPP IV protein may be significantly associated with aggressive clinicopathological features and unfavorable clinical outcome of patients with IHCC, suggesting that DPP IV may have a pro-oncogenic activity in IHCC.
As mentioned above, our data showed the positive correlation between NEP and DPP IV expression in IHCC tissues, which prompted us to investigate the clinical significance of the combined expression of NEP and DPP IV proteins. More interestingly, simultaneous upregulation of NEP and DPP IV was significantly associated with the aggressiveness of IHCCs. Significant difference of prognosis was also found among four different statuses of NEP/DPP IV coexpression. The patients with NEP-low/DPP IV-low had the best outcome, while those with NEP-high/DPP IV-high had the worst. Multivariate analysis revealed that the NEP/DPP IV coexpression profiles were independent prognostic indicators for IHCCs. The advantages of NEP/DPP IV coexpression to individual NEP or DPP IV in predicting the outcome of IHCCs has been shown in our result.
In conclusion, our data from the current study suggest for the first time that both the expression of NEP and DPP IV proteins may be upregulated in human IHCC tissues, and the combined expression of NEP and DPP IV proteins may play important roles in progression and prognosis of patients with IHCC. Given the synergistic effect on overall as well as recurrence-free survival of resected IHCC by the combined expression of NEP and DPP-IV proteins, a mechanistic link between the two biomarkers is worth investigating. Clinical implications on how these findings may improve patient selection for surgery should also be considered.
Disclosure
The authors report no conflicts of interest in this work.
References
Tian F, Li D, Chen J, et al. Aberrant expression of GATA binding protein 6 correlates with poor prognosis and promotes metastasis in cholangiocarcinoma. Eur J Cancer. 2013;49:1771–1780. | |
Huang Q, Liu L, Liu CH, et al. Expression of Smad7 in cholangiocarcinoma: prognostic significance and implications for tumor metastasis. Asian Pac J Cancer Prev. 2012;13:5161–5165. | |
Sempoux C, Jibara G, Ward SC, et al. Intrahepatic cholangiocarcinoma: new insights in pathology. Semin Liver Dis. 2011;31:49–60. | |
Gu FM, Gao Q, Shi GM, et al. Intratumoral IL-17+ cells and neutrophils show strong prognostic significance in intrahepatic cholangiocarcinoma. Ann Surg Oncol. 2012;19:2506–2514. | |
Maguer-Satta V, Besançon R, Bachelard-Cascales E. Concise review: neutral endopeptidase (CD10): a multifaceted environment actor in stem cells, physiological mechanisms, and cancer. Stem Cells. 2011;29:389–396. | |
Carl-McGrath S, Lendeckel U, Ebert M, Röcken C. Ectopeptidases in tumour biology: a review. Histol Histopathol. 2006;21:1339–1353. | |
Sato Y, Itoh F, Hinoda Y, et al. Expression of CD10/neutral endopeptidase in normal and malignant tissues of the human stomach and colon. J Gastroenterol. 1996;31:12–17. | |
Sumitomo M, Shen R, Nanus DM. Involvement of neutral endopeptidase in neoplastic progression. Biochim Biophys Acta. 2005;1751:52–59. | |
Ishimaru F, Potter NS, Shipp MA. Phorbol ester-mediated regulation of CD10/neutral endopeptidase transcripts in acute lymphoblastic leukemias. Exp Hematol. 1996;24:43–48. | |
Iwaya K, Ogawa H, Izumi M, Kuroda M, Mukai K. Stromal expression of CD10 in invasive breast carcinoma: a new predictor of clinical outcome. Virchows Arch. 2002;440:589–593. | |
Voutsadakis IA, Vlachostergios PJ, Daliani DD, et al. CD10 is inversely associated with nuclear factor-kappa B and predicts biochemical recurrence after radical prostatectomy. Urol Int. 2012;88:158–164. | |
Murali R, Delprado W. CD10 immunohistochemical staining in urothelial neoplasms. Am J Clin Pathol. 2005;124:371–379. | |
Gürel D, Kargi A, Karaman I, Onen A, Unlü M. CD10 expression in epithelial and stromal cells of non-small cell lung carcinoma (NSCLC): a clinic and pathologic correlation. Pathol Oncol Res. 2012;18:153–160. | |
Terauchi M, Kajiyama H, Shibata K, Ino K, Mizutani S, Kikkawa F. Anti-progressive effect of neutral endopeptidase 24.11 (NEP/CD10) on cervical carcinoma in vitro and in vivo. Oncology. 2005;69:52–62. | |
Chu P, Arber DA. Paraffin-section detection of CD10 in 505 nonhematopoietic neoplasms. Frequent expression in renal cell carcinoma and endometrial stromal sarcoma. Am J Clin Pathol. 2000;113:374–382. | |
Khor TS, Alfaro EE, Ooi EM, et al. Divergent expression of MUC5AC, MUC6, MUC2, CD10, and CDX-2 in dysplasia and intramucosal adenocarcinomas with intestinal and foveolar morphology: is this evidence of distinct gastric and intestinal pathways to carcinogenesis in Barrett Esophagus? Am J Surg Pathol. 2012;36:331–342. | |
Erhuma M, Köbel M, Mustafa T, et al. Expression of neutral endopeptidase (NEP/CD10) on pancreatic tumor cell lines, pancreatitis and pancreatic tumor tissues. Int J Cancer. 2007;120:2393–2400. | |
Del Rio P, Crafa P, Papadia C, et al. Is CD10 a reliable marker of invasive colorectal cancer? Ann Ital Chir. 2011;82:279–282. | |
Uematsu F, Takahashi M, Yoshida M, Igarashi M, Nakae D. Methylation of neutral endopeptidase 24.11 promoter in rat hepatocellular carcinoma. Cancer Sci. 2006;97:611–617. | |
Yu DM, Yao TW, Chowdhury S, et al. The dipeptidyl peptidase IV family in cancer and cell biology. FEBS J. 2010;277:1126–1144. | |
Kotacková L, Baláziová E, Sedo A. Expression pattern of dipeptidyl peptidase IV activity and/or structure homologues in cancer. Folia Biol (Praha). 2009;55:77–84. | |
McGuinness C, Wesley UV. Dipeptidyl peptidase IV (DPPIV), a candidate tumor suppressor gene in melanomas is silenced by promoter methylation. Front Biosci. 2008;13:2435–2443. | |
Elble RC, Pauli BU. Lu-ECAM-1 and DPP IV in lung metastasis. Curr Top Microbiol Immunol. 1996;213:107–122. | |
Sulda ML, Abbott CA, Macardle PJ, Hall RK, Kuss BJ. Expression and prognostic assessment of dipeptidyl peptidase IV and related enzymes in B-cell chronic lymphocytic leukemia. Cancer Biol Ther. 2010;10:180–189. | |
Stulc T, Sedo A. Inhibition of multifunctional dipeptidyl peptidase-IV: is there a risk of oncological and immunological adverse effects? Diabetes Res Clin Pract. 2010;88:125–131. | |
Sun YX, Pedersen EA, Shiozawa Y, et al. CD26/dipeptidyl peptidase IV regulates prostate cancer metastasis by degrading SDF-1/CXCL12. Clin Exp Metastasis. 2008;25:765–776. | |
Cordero OJ, Imbernon M, Chiara LD, et al. Potential of soluble CD26 as a serum marker for colorectal cancer detection. World J Clin Oncol. 2011;2:245–261. | |
Nozaki Y, Yamamoto M, Ikai I, et al. Reconsideration of the lymph node metastasis pattern (N factor) from intrahepatic cholangiocarcinoma using the International Union Against Cancer TNM staging system for primary liver carcinoma. Cancer. 1998;83(9):1923–1929. | |
Herszényi L, Lakatos G, Hritz I, Varga MZ, Cierny G, Tulassay Z. The role of inflammation and proteinases in tumor progression. Dig Dis. 2012;30:249–254. | |
Varona A, Blanco L, Perez I, et al. Expression and activity profiles of DPP IV/CD26 and NEP/CD10 glycoproteins in the human renal cancer are tumor-type dependent. BMC Cancer. 2010;10:193. | |
Kajiyama H, Kikkawa F, Ino K, Shibata K, Mizutani S. Expression of CD26/dipeptidyl peptidase IV in endometrial adenocarcinoma and its negative correlation with tumor grade. Adv Exp Med Biol. 2003;524:245–248. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.