Back to Journals » Vascular Health and Risk Management » Volume 13
Prognostic indices among hypertensive heart failure patients in Nigeria: the roles of 24-hour Holter electrocardiography and 6-minute walk test
Authors Mene-Afejuku TO , Balogun MO , Akintomide AO, Adebayo RA
Received 12 October 2016
Accepted for publication 13 January 2017
Published 27 February 2017 Volume 2017:13 Pages 71—79
DOI https://doi.org/10.2147/VHRM.S124477
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Amudha Kadirvelu
Tuoyo O Mene-Afejuku,1,2 Michael O Balogun,2 Anthony O Akintomide,2 Rasaaq A Adebayo2
1Department of Medicine, Metropolitan Hospital Center, New York, NY, USA; 2Cardiology Unit, Department of Medicine, Obafemi Awolowo University Teaching Hospitals Complex, Ile-Ife, Osun State, Nigeria
Background: Hypertensive heart failure (HHF) is associated with a poor prognosis. There is paucity of data in Nigeria on prognosis among HHF patients elucidating the role of 24-hour Holter electrocardiogram (ECG) in concert with other risk factors.
Objective: The aim of this study was to determine the prognostic utility of 24-hour Holter ECG, the 6-minute walk test (6-MWT), echocardiography, clinical and laboratory parameters among HHF patients.
Methods: A total of 113 HHF patients were recruited and followed up for 6 months. Thirteen of these patients were lost to follow-up, and as a result only 100 HHF patients were analyzed. All the patients underwent baseline laboratory tests, echocardiography, 24-hour Holter ECG and the 6-MWT. HHF patients were analyzed as “mortality vs alive” and as “events vs no-events” based on the outcome at the end of 6 months. Events was defined as HHF patients who were rehospitalized for heart failure (HF), had prolonged hospital stay or died. No-events group was defined as HHF patients who did not meet the criteria for the events group.
Results: HHF patients in the mortality group (n = 7) had significantly higher serum urea (5.71 ± 2.07 mmol/L vs 3.93 ± 1.45 mmol/L, p = 0.003) than that in those alive. After logistic regression, high serum urea conferred increased mortality risk (p = 0.035). Significant premature ventricular complexes (PVCs) on 24-hour Holter ECG following logistic regression were also significantly higher (p = 0.015) in the mortality group than in the “alive” group (n = 93) at the end of the 6-month follow-up period. The 6-minute walk distance (6-MWD) was least among the HHF patients who died (167.26 m ± 85.24 m). However, following logistic regression, the 6-MWT was not significant (p = 0.777) for predicting adverse outcomes among HHF patients. Patients in the events group (n = 41) had significantly higher New York Heart Association (NYHA) class (p = 0.001), Holter-detected ventricular tachycardia (VT; p = 0.009), Holter-detected atrial fibrillation (AF; p = 0.028) and PVCs (p = 0.017) following logistic regression than those in the no-events group (n = 59).
Conclusion: High NYHA class, elevated serum urea, Holter ECG-detected AF and ventricular arrhythmias are predictive of a poor outcome among HHF patients. The 6-MWT was not a useful prognostic index in this study.
Keywords: hypertensive heart failure, ventricular tachycardia, Holter electrocardiography, prognosis
Introduction
Heart failure (HF) is an increasingly costly and deadly manifestation of a series of cardiac diseases and constitutes a major public health problem worldwide.1,2 Despite current state-of-the-art treatment of HF, mortality rate remains high, and ~50–60% of HF patients will die within 5 years of diagnosis.1 The prognosis worsens with advancement of HF, and the mortality rate is as high as 50% per year in severe cases.3 HF is also associated with increased morbidity as it is characterized by frequent hospital admissions and prolonged hospital stay.4 Hypertensive HF (HHF) patients have clinical characteristics similar to those of other patients with HF with the caveat that symptoms of diastolic dysfunction and elevated left ventricular filling pressures may be present earlier on as compared to other causes of HF.2 HHF is the commonest form of HF in Nigeria,5 and has been found to be laden with several poor prognostic indices. As a result, overall 1-year survival of HHF patients is ~71% contingent on the absence of poor prognostic markers.6
Holter-based electrocardiogram (ECG) parameters with special emphasis on risk markers such as heart rate variability (HRV) and arrhythmias have been useful in predicting mortality.7 It is widely accepted that structural changes in the myocardium are better identified by means of imaging techniques. Therefore, combining the electrocardiographic alterations with echocardiographic parameters among patients with HF may provide the complex insight into the interplay between factors contributing to mortality.1
In addition, the 6-minute walk test (6-MWT) has been proposed to have prognostic utility in HF patients.8–11 A reduced 6-minute walk distance (6-MWD) of <300 m among HF patients has also been proposed to be associated with poor prognosis.11
While there are studies on prognostic indices among HHF patients, there is scarcity of data evaluating the usefulness of 24-hour Holter ECG and the 6-MWT in conjunction with other factors in Nigeria.6–11 Therefore, we prospectively recruited HHF patients with the aim of having a broader look at various prognostic indices, including but not limited to the following: echocardiographic parameters, 24-hour Holter ECG, 6-MWT and laboratory parameters among others.
The information garnered from this study will be useful in risk stratification of HHF patients and may also be pivotal in formulating management strategies for high-risk patients as some of these risk factors may be modifiable.
Methods
This is a prospective cohort study in which 113 HHF patients were recruited consecutively over a 1-year period. Thirteen of these patients were lost to follow-up. Approval of the Ethics and Research Committee of Obafemi Awolowo University Teaching Hospitals Complex, Nigeria, was obtained before the commencement of the study, and written informed consent was obtained from each of the study participants.
Inclusion criteria
Subjects aged 18 years and older.
Subjects with a clinical diagnosis of HF and who satisfied the recommendations of the European Society of Cardiology12 for the diagnosis of heart failure.
Subjects with systemic hypertension defined as average of three blood pressure measurements ≥140/90 mmHg, or if the subject was already on antihypertensive therapy.13
Exclusion criteria
Subjects admitted with suspected heart failure who did not meet the diagnostic clinical criteria for the diagnosis of HF or systemic hypertension.
Subjects with heart failure from any other etiology other than systemic hypertension.
Subjects who died within 48 hours of admission before full clinical evaluation was performed.
Subjects unable to walk without assistance from another person (not including mobility aids) or if unable to walk because of noncardiac limitations, for example, osteoarthritis.
The patients were interviewed and examined in detail. HF was defined according to the recommendations of the European Society of Cardiology.12 HHF in this study was used to describe patients with HF secondary to systemic hypertension. The 12-lead resting ECG of the patients was obtained with the aid of a 3-channel electrocardiograph (Cardiofax YD-907D). All the 12-lead ECGs were read by the cardiologist, and left ventricular hypertrophy (LVH) was determined using the Sokolow–Lyon voltage criteria.14 Other abnormalities on the ECG were also defined based on standard criteria.14,15
HHF patients also carried out the 6-MWT at admission according to standard guidelines16 excluding those in New York Heart Association (NYHA) class IV who had the test deferred until their functional class had improved. The distance covered in a single test was recorded as the farthest distance covered at the end of 6 minutes irrespective of frequency of stops or inability to complete the 6-minute walk time frame.16
Echocardiography was performed using a standard Vivid 7 Dimension ultrasound imaging system with the 5S transthoracic-phased array sector probe for adults with a frequency of 2.2 to 5.0 MHz using the transducer manufactured by General Electric (GE) Medical Systems. All the HHF patients underwent 2-dimensional [2D]-derived M mode Doppler (pulsed wave, continuous wave, color flow) and tissue Doppler transthoracic echocardiography with simultaneous ECG recordings. Measurements were in accordance with the recommendations of the American Society of Echocardiography.17
The left ventricular ejection fraction (LVEF) was calculated from echocardiographic machine-derived volumes computed based on the Teichholz equations. The average of three consecutive measurements was recorded as the LVEF. The formula is:
LVEF: 100(LVEDV - LVESV)/LVEDV
where LVEDV is the left ventricular end diastolic volume and LVESV is the left ventricular end systolic volume.
The LV end systolic and diastolic volumes were derived using the Teichholz formula18:
EDV: (7 × LVEDD3) ÷ (2.4 + LVEDD)
ESV: (7 × LVESD3) ÷ (2.4 + LVESD)
where LVEDD is the left ventricular end diastolic diameter and LVESD is the left ventricular end systolic diameter.
The Tei index was calculated using the following formula based on echocardiographic-derived parameters:19
IVCT + IVRT)/LVET
where IVCT is the isovolumic contraction time (interval between mitral valve closure and aortic valve opening). IVRT is the isovolumic relaxation time (interval between aortic valve closure and mitral valve opening) and LVET is the left ventricular ejection time (interval from opening to closure of aortic valve).
The 24-hour Holter monitoring was also carried out at admission using Schiller type (MT-101) Holter ECG machine, and baseline recordings were recorded.20 The following 24-hour Holter ECG parameters were recorded from all participants: heart rate, heart rate variability (HRV), arrhythmias (premature atrial complexes, atrial fibrillation [AF], premature ventricular complexes [PVCs] and ventricular tachycardia [VT]) and peak ectopy rate. The HRV was recorded in four time domains, but only the SDNN (standard deviation of all normal to normal sinus RR intervals over 24 hours) was analyzed as it is the best known, best validated and earliest HRV parameter utilized to prognosticate HF patients.1
Baseline clinical and biochemical parameters such as body mass index (BMI), packed cell volume, electrolytes, urea and creatinine were estimated. The glomerular filtration rate (GFR) was estimated using the Cockcroft–Gault equation.21 HHF patients had a chest X-ray posterior–anterior view just before admission.
The length of hospital stay of patients was recorded, and subjects were followed up for 6 months via monthly clinic visits. Time from discharge to readmission was noted for patients who were readmitted within the 6-month follow-up period. The time from first seeing the patient to death for those that died was also recorded within the 6-month follow-up period. Phone calls were made to patients or their next of kin to confirm default of clinic attendance or mortality, respectively.
The HHF patients were analyzed as “mortality vs alive” and as “events vs no-events” based on the outcome at the end of 6 months. Events was defined as HHF patients who were rehospitalized for HF, had prolonged hospital stay or died. No-events was defined as HHF patients who did not meet the criteria for the events group. For the purpose of this study, prolonged hospital stay was defined as hospital stay >8 days based on findings by Wright et al,4 who stated that a median hospital length of stay >6 days among HF patients was associated with multiple adverse features. As a result, to account for peculiarities unique to our environment in terms of social issues and patient characteristics, we chose >8 days as the definition of prolonged hospital stay.
In this study, HHF patients were defined as having had poor prognosis if they had an event based on the definitions above during the 6-month follow-up period.
It is important to note that all the patients in this study had guideline-directed medical therapy22 including but not limited to the following medications: diuretics, angiotensin converting enzyme (ACE) inhibitors, angiotensin receptor blockers (ARBs), β-blockers as well as aldosterone receptor antagonist. The effect of therapy was not analyzed, as the focus of the study was to uncover nontherapy-related factors that confer poor prognosis among HHF patients.
Statistics
The data analysis was carried out using IBM SPSS software version 20.0 (IBM Corporation, Armonk, NY, USA). Descriptive statistics were computed for continuous variables while frequency tables were generated for categorical variables. The continuous variables were expressed as mean ± standard deviation while categorical data were expressed as percentages. Differences between two continuous variables were determined using the independent Student’s t-test. The differences between categorical data were determined using the Chi-squared (χ2) test. The Cox proportional-hazard regression model was used to evaluate the association of variables with mortality or morbidity. Cox regression survival curves were used to estimate the survival rates for HHF patients. The level of significance was p ≤ 0.05 and confidence interval of 95%.
Results
A total of 113 patients were recruited for this study, of whom 13 were lost to follow-up. Of the 100 HHF patients eventually analyzed, the mortality group comprised of seven patients. The events group was made up of 41 patients, and the no-events group was composed of 59 patients. Five of the deaths among the HHF patients were intrahospital deaths probably secondary to pump failure from progressively worsening disease with a median of 17 days from the date of admission. The other two deaths occurred at ~4 months and 5 months, following discharge.
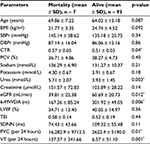
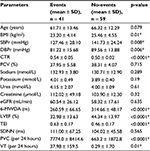
Table 1 shows that the cardiothoracic ratio (CTR) measured on chest X-ray was significantly higher among the patients in the mortality group as compared to those alive (0.57 ± 0.05 vs 0.51 ± 0.03; p = 0.04). Also, patients in the mortality group had poorer renal function indices than those alive evidenced by higher serum urea and lower estimated GFR (eGFR) (5.71 ± 2.07 mmol/L vs 3.93 ± 1.45 mmol/L; p = 0.003 and 39.81 ± 22.38 mL/min vs 60.69 ± 20.73 mL/min; p = 0.012), respectively.
Patients in the mortality group (n = 7) covered a lower distance during the 6-MWT at admission as compared to the 6-MWD on admission of those alive after 6 months of follow-up (167.26 ± 85.24 m vs 301.92 ± 49.05 m; p = 0.006).
Based on the results of 24-hour Holter ECG monitoring, patients in the mortality group had more PVCs and counts of nonsustained VT than those alive (16,282.9 ± 9712.5 per day vs 2622.4 ± 5190.0 per day; p = 0.01 and 137.57 ± 341.66 per day vs 6.57 ± 51.10 per day; p = 0.001), respectively. The heart rate variability as measured by standard deviation of all normal sinus RR intervals over 24 hours (SDNN) was not different between the groups (p = 0.11).
All the patients who died had NYHA III or IV at admission as compared to 46.2% of those alive (p = 0.012). There were also significantly higher proportions of right bundle branch block (p = 0.024) on ECGs of patients in the mortality group as compared to those alive. However, there was no significant difference in the proportions of LVH by voltage criteria (p = 0.439) and left bundle branch block (p = 0.361) on the ECGs of HHF patients alive and those who died. A significantly higher proportion of patients in the mortality group (71.4%) had AF on 24-hour Holter ECG monitoring as opposed to 21.5% of those alive (p = 0.01).
Table 2 shows that patients in the events group had significantly lower BMI, systolic and diastolic blood pressures than those in the no events group (23.20 ± 4.14 kg/m2 vs 25.46 ± 4.55 kg/m2; p = 0.013, 127.46 ± 28.10 mmHg vs 141.73 ± 24.24 mmHg; p = 0.008 and 81.22 ± 15.68 mmHg vs 89.56 ± 13.88 mmHg; p = 0.006), respectively.
The packed cell volume (p = 0.715), serum sodium (p = 0.289), urea (p = 0.61) and creatinine (p = 0.32) were not significantly different between the events group and the no-events group. HHF patients in the events group had significantly lower ejection fraction and 6-MWD than those in the no events group (32.98 ± 13.63% vs 44.34 ± 13.97%; p ≤ 0.0001 and 260.59 ± 66.65 m vs 314.66 ± 48.17 m; p ≤ 0.0001), respectively.
The myocardial performance index (Tei index) was more impaired among HHF patients in the events group than those in the no events group (p ≤ 0.0001). They also had significantly higher counts of PVCs and VT on 24-hour Holter ECG monitoring than those in the no events group (p ≤ 0.0001 and p = 0.01), respectively.
Significant proportions of HHF patients in the events group had significantly higher NYHA class (III or IV) at admission as compared to the no events group (p ≤ 0.0001).
There were, however, no significant differences in the proportions of LVH by voltage criteria (p = 0.494) and right bundle branch block (p = 0.301) on the ECGs of the events group in comparison to those in the no events group. However, a significantly higher proportion of patients in the events group (43.9%) had AF on 24-hour Holter ECG monitoring as opposed to 11.9% in the no events group (p ≤ 0.0001).
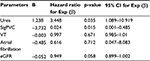
The parameters that were found to achieve statistical significance were entered into the regression analysis. Elevated serum urea (p = 0.035) was predictive of all-cause mortality among HHF patients as displayed in Table 3. In addition, low counts of PVCs on 24-hour Holter ECG monitoring had lower risk of death (Exp [b] = 0.024, p = 0.015).
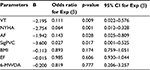
As depicted in Table 4, higher NYHA class III or IV (p = 0.001), presence of AF (p = 0.028), VT (p = 0.009) and PVCs (p = 0.017) all recorded on 24-hour Holter ECG monitoring were predictive of adverse events among HHF patients.
Figure 1 depicts the Cox regression survival plot for HHF patients based on the presence of significant PVCs on 24-hour Holter ECG, which was defined as the presence of PVCs >10% of the total QRS complexes recorded on 24-hour Holter ECG. Eighteen HHF patients had significant PVCs on Holter ECG recording while the remaining 82 did not meet the criterion for significant PVCs. The plot shows that HHF patients with significant PVCs on 24-hour Holter ECG had significantly lower cumulative survival rates than those without significant PVCs (-2 log statistics, p ≤ 0.0001).
Figure 2 depicts the Cox regression survival plot for HHF patients based on the presence or absence of elevated serum urea. Elevated serum urea was defined as serum urea >7.1 mmol/L. The plot in Figure 2 shows that HHF patients with elevated serum urea had significantly reduced cumulative survival rates (-2 log statistics, p ≤ 0.0001) than those with relatively normal serum urea levels.
  | Figure 2 Cox regression survival plot for HHF patients based on the presence of elevated or normal serum urea level. Abbreviation: HHF, hypertensive heart failure. |
Discussion
This study aims to identify the factors that confer poor prognosis among patients with HHF. At the end of the study, renal dysfunction evidenced by elevated serum urea and the presence of significant PVCs on 24-hour Holter ECG were the most potent factors in predicting mortality among patients with HHF. The predictors of adverse events as defined in this study were high NYHA class on admission, 24-hour Holter recorded VT, AF and significant PVCs.
Renal insufficiency is a common accompaniment of HF and also confers increased mortality risk.23–27 Patients with heart failure and a low cardiac output usually have reduced renal blood flow and associated elevated serum urea. Elevated serum urea in this study seemed to be a better predictor of all-cause mortality than eGFR as an index of renal dysfunction, which is similar to the findings of Heywood et al25 and Gotsman et al.26 Following regression analysis, elevated serum urea increased the risk of dying (Exp [β] = 3.448; p = 0.035). Patients who died had a significantly lower eGFR than survivors but eGFR was not found to be a useful predictor of mortality following regression analysis. This may indicate that even though eGFR is useful in assessing the severity of renal dysfunction, its prognostic utility in HF may be of little value.25,26
Serum urea may therefore have a different mechanism in conferring increased mortality risk as compared to eGFR. This may be in relation to the unique role of urea as a neurohormonal biomarker in the setting of HF, which may stem from the intricate physiology of urea reabsorption.25–27 Reabsorption of urea is “concentration dependent” and as such, angiotensin II known to be elevated in HF can enhance absorption of the sodium and water in the proximal tubules and lead to an increase in the concentration of the filtered urea in the proximal tubules.27,28 This in turn can cause significant passive reabsorption of the urea down a concentration gradient. Second, increased reabsorption of the water in the proximal nephron reduces fluid delivery distally, resulting in slow tubular flow in the collecting duct, and increased flow-dependent reabsorption of the urea in this segment.27,28 Urea is also reabsorbed in the distal nephron dependent on the level of antidiuresis. Therefore, higher levels of arginine vasopressin (AVP) as seen in HF induce extensive absorption of urea.27,28 The terminal part of the inner medullary collecting duct possesses a high level of urea permeability that is dramatically increased in the presence of AVP, a process stated to be transporter mediated.27,28 AVP, glucocorticoids and mineralocorticoids have also been shown to regulate the urea transporters in the kidney.27,28
Elevated serum urea parallels increase in the humoral components of neurohormonal activation in HF such as angiotensin, norepinephrine and AVP, which are not routinely measured clinically largely because of huge cost considerations.27,28
Therefore, serum urea may serve as an index of neurohumoral activation and may be useful in risk-stratifying patients for more aggressive therapy to possibly reduce the risk of a poor outcome among HHF patients.
Higher NYHA class (III or IV) was strongly predictive of poor prognosis among HHF patients. Following regression analysis, it remained a strong predictor for an adverse event (p = 0.001) among HHF patients. This is in consonance with several studies (Karaye and Sani,3 Pocock et al,29 Ahmed et al30 as well as Bouvy et al31).
Ventricular arrhythmias are frequent findings in HF and may serve as predictors of sudden death in these patients.32 The presence of significant PVCs on 24-hour Holter ECG recording was found to be significant for increased mortality as well as an overall cause of adverse events in HHF patients following regression analysis in this study (p = 0.015 and p = 0.017, respectively). The survival plot in Figure 1 above, clearly displays the effect of significant PVCs on the chances of survival.
It has been noted that a higher frequency of PVCs is associated with a decrease in LVEF, an increase in incidence of heart failure and in turn increased mortality.33
Therefore, therapies that can reduce or prevent multiple PVCs may improve outcomes among HF patients.
The presence of VT on subsequent Holter monitoring was predictive of a poor outcome in this study (p = 0.009 following logistic regression). All the patients who died in this study had short runs VT on Holter monitoring. Six of the seven patients had nonsustained VT and one of the patients who died had sustained VT. This is similar to the findings of Doval et al,34 where the presence of nonsustained VT and couplets of PVCs on Holter monitoring had predictive value for sudden cardiac death. Casaleggio et al35 also had comparable findings as the presence of nonsustained VT and high peak ectopy rates were validated as predictors of increased risk of sudden death even after Cox proportional hazards regression analysis was carried out.
AF on 24-hour Holter ECG conferred increased risk of mortality and/or morbidity in this study. The prognostic significance of AF may stem from worsening diastolic dysfunction due to a shorter diastolic filling time, secondary to rapid ventricular heart rates.36 The loss of effective atrial contraction also impacts negatively especially in patients with underlying diastolic dysfunction, such as HHF patients.37
A close examination of the findings in this study would reveal that most of the electrocardiographic abnormalities that conferred poor prognosis among the study population were 24-hour Holter ECG-derived parameters rather than the 12-lead ECG parameters. Although, ECG abnormalities were prevalent among HHF patients, most of them were nonspecific and added little to the risk stratification of these patients. This may stem from the ability of the 24-hour Holter ECG monitor to detect underlying arrhythmias that may be easily missed with the 12-lead ECG as it is just like a snap shot of the electrical activities of the heart over a few seconds.
The results are similar to the findings of the study on the prognostic significance of ECG abnormalities for mortality risk in acute heart failure: insight from the Sub-Saharan Africa survey of Heart Failure (THESUS-HF) where ECG abnormalities were not too useful in prognosticating heart failure patients.37
Therefore, even though continuous ambulatory Holter monitoring is not considered as a basic diagnostic tool in diagnosis of HF, it may still have a role in risk stratification of patients. This is useful, because the abnormalities in the electrocardiographic parameters may add more information in full prognostic assessment of HF patients1 as has been demonstrated in this study.
A reduced 6-MWD has been proposed to be predictive of adverse events in HF patients.16,38 Most of these studies on further analysis have not been able to substantiate this claim. However, Ingle et al9 suggested that reduced 6-MWD in conjunction with left ventricular dysfunction was predictive of mortality. However, the 6-MWD was of poor prognostic utility in patients with mild left ventricular dysfunction.
The findings in this study are in tandem with most studies indicating that there is poor association between reduced 6-MWD and poor prognosis in HF. In spite of the finding that HHF patients who died had significantly lower mean 6-MWD of 167.26 m (p < 0.0001) than those alive, it was still not predictive of mortality. Therefore, 6-MWD is not predictive of a poor outcome in HHF patients and may only serve the purpose of assessing exercise tolerance and the patient’s adaptability to coping with functional impairment associated with HHF.
Conclusion
The 24-hour Holter ECG is a very important adjunctive tool in assessing HHF patients as it can detect poor prognostic indicators such as VT, significant counts of PVCs and AF. Elevated serum urea and high functional NYHA class were indices for poor prognosis among patients with HHF. Therefore, early detection and treatment of these abnormalities may be useful in reducing morbidity and mortality among HHF patients.
Limitations
A longer period of follow-up of the HHF patients might have uncovered some more prognostic utility of some of the parameters in this study. In addition, the use of cardiopulmonary exercise testing might have provided more information on the role of exercise as a prognostic tool among HHF patients.
Disclosure
The authors report no conflicts of interest in this work.
References
Cygankiewicz I, Zaręba W, De Luna AB. Prognostic value of Holter monitoring in congestive heart failure. Cardiol J. 2008;15(4):313–323. | ||
Bloomfield GS, Barasa FA, Doll JA, Velazquez EJ. Heart failure in Sub-Saharan Africa. Curr Cardiol Rev. 2013;9(2):157–173. | ||
Karaye KM, Sani MU. Factors associated with poor prognosis among patients admitted with heart failure in a Nigerian tertiary medical centre: a cross-sectional study. BMC Cardiovasc Disord. 2008;8:16. | ||
Wright SP, Verouhis D, Gamble G, Swedberg K, Sharpe N, Doughty RN. Factors influencing the length of hospital stay of patients with heart failure. Eur J Heart Fail. 2003;5(2):201–209. | ||
Dokainish H, Teo K, Zhu J, et al. Heart failure in Africa, Asia, the Middle East and South America: the INTER-CHF study. Int J Cardiol. 2016;204:133–141. | ||
Isezuo AS, Omotoso AB, Araoye MA, Carr J, Corrah T. Determinants of prognosis among black Africans with hypertensive heart failure. Afr J Med Med Sci. 2003;32(2):143–149. | ||
Karim N, Hasan JA, Ali SS. Heart rate variability – a review. J Basic Appl Sci. 2011;7(1):71–77. | ||
Boxer RS, Kleppinger A, Ahmad A, Annis K, Hager D, Kenny AM. The 6-minute walk is associated with frailty and predicts mortality in older adults with heart failure. Congest Heart Fail. 2010;16(5):208–213. | ||
Ingle L, Rigby AS, Carroll S, et al. Prognostic value of the 6 min walk test and self-perceived symptom severity in older patients with chronic heart failure. Eur Heart J. 2007;28(5):560–568. | ||
Adedoyin RA, Adeyanju SA, Balogun MO, et al. Assessment of exercise capacity in African patients with chronic heart failure using six minutes walk test. Int J Gen Med. 2010;8(3):109–113. | ||
Faggiano P, Aloia AD, Gualeni A, Brentana L, Cas LD. The six minute walking test in chronic heart failure: indications, interpretation and limitations from a review of the literature. Eur J Heart Fail. 2004;6(6):687–691. | ||
McMurray JJ, Adamopoulos S, Anker SD. The task force for the diagnosis and treatment of acute and chronic heart failure 2012 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association (HFA) of the ESC. Eur Heart J. 2012;33(14):1787–1847. | ||
Ojji D, Stewart S, Ajayi S, Manmak M, Sliwa K. A predominance of hypertensive heart failure in Abuja Heart Study cohort of urban Nigerians: a prospective clinical registry of 1515 de novo cases. Eur J Heart Fail. 2013;15(8):835–842. | ||
Narayanan K, Reinier K, Teodorescu C, et al. Electrocardiographic versus echocardiographic left ventricular hypertrophy and sudden Cardiac arrest in the community. Heart Rhythm. 2014;11(6):1040–1046. | ||
AHA/ACC/HRS Scientific Statement. Guidelines for the standardization and interpretation of the electrocardiogram. Am Coll Cardiol. 2007;49:1128–1135. | ||
ATS Committee on Proficiency Standards for Clinical Pulmonary Function Laboratories. ATS statement: guidelines for the six-minute walk test. Am J Respir Crit Care Med. 2002;166(1):111–117. | ||
Lang RM, Bierig M, Devereux RB, et al. Recommendations for chamber quantification: a report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr. 2005;18(12):1440–1463. | ||
Arora G, Morss AM, Piazza G, et al. Differences in left ventricular ejection fraction using teichholz formula and volumetric methods by CMR: implications for patient stratification and selection of therapy. J Cardiovasc Med Reson. 2010;12(Suppl 1):202. | ||
Akintunde AA. The clinical value of the Tei index among Nigerians with hypertensive heart failure: correlation with other conventional indices. Cardiovasc J Afr. 2012;23(1):40–43. | ||
Crawford MH, Bernstein SJ, Deedwania PC, et al. ACC/AHA Guidelines for Ambulatory Electrocardiography. A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Revise the Guidelines for Ambulatory Electrocardiography). Developed in collaboration with the North American Society for Pacing and Electrophysiology. J Am Coll Cardiol. 1999;34(3):912–948. | ||
Botev R, Mallie JP, Couchoud C, et al. Estimating glomerular filtration rate: cockcroft-gault and modification of diet in renal disease formulas compared to renal inulin clearance. Clin J Am Soc Nephrol. 2009;4(5):899–906. | ||
Yancy CW, Jessup M, Bozkurt B. 2013 ACCF/AHA Guideline for the Management of Heart Failure: executive summary. A Report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. JACC. 2013;62(16):1495–1539. | ||
Oyedeji AT, Balogun MO, Akintomide AA, et al. The significance of mild renal dysfunction in chronic heart failure. West Afr J Med. 2011;30(6):442–446. | ||
Hillege HL, Nitsch D, Pfeffer MA, et al. Renal function as a predictor of outcome in a broad spectrum of patients with heart failure. Circulation. 2006;113(5):671–678. | ||
Heywood JT, Fonarow GC, Costanzo MR, et al; ADHERE Scientific Advisory Committee and Investigators. High prevalence of renal dysfunction and its impact on outcome in 118,465 patients hospitalized with acute decompensated heart failure: a report from the ADHERE database. J Card Fail. 2007;13:422–430. | ||
Gotsman I, Zwas D, Planer D, Admon D, Lotan C, Keren A. The significance of serum urea and renal function in patients with heart failure. Medicine (Baltimore). 2010;89(4):197–203. | ||
Kazory A. Emergence of blood urea nitrogen as a biomarker of neurohormonal activation in heart failure. Am J Cardiol. 2010;106(5):694–700. | ||
Schrier RW. Blood urea nitrogen and serum creatinine: not married in heart failure. Circ Heart Fail. 2008;1(1):2–5. | ||
Pocock SJ, Wang D, Pfeffer MA, et al. Predictors of mortality and morbidity in patients with chronic heart failure. Eur Heart J. 2006;27(1):65–75. | ||
Ahmed A, Aronow WS, Fleg JL. Higher New York Heart Association Classes and increased mortality and hospitalization in heart failure patients with preserved left ventricular function. Am Heart J. 2006;15(2):444–450. | ||
Bouvy ML, Heerdink ER, Leufkens HGM, Hoes AW. Predicting mortality in patients with heart failure: a pragmatic approach. Heart. 2003;89(6):605–609. | ||
Ajayi OE, Ajayi AA. Valvular regurgitations may increase risk of arrhythmias in Nigerians with hypertensive heart failure. J Cardiovasc Med (Hagerstown). 2013;14(6):453–460. | ||
Dukes JW, Dewland TA, Vittinghoff E, et al. Ventricular ectopy as a predictor of heart failure and death. J Am Coll Cardiol. 2015;66(2):101–109. | ||
Doval HC, Nul DR, Grancelli HO, et al. Nonsustained ventricular tachycardia in severe heart failure: independent marker of increased mortality due to sudden death. Circulation. 1996;94(12):3198–3203. | ||
Casaleggio A, Maestri R, La Rovere MT, Rossi P, Pinna GD. Prediction of sudden death in heart failure patients: a novel perspective from the assessment of the peak ectopy rate. Eurospace. 2007;9(6):385–390. | ||
Anter E, Jessup M, Callans DJ. Atrial fibrillation and heart failure: treatment considerations for a dual epidemic. Circulation. 2009;119(18):2516–2525. | ||
Dzudie A, Milo O, Edwards C, et al. Prognostic significance of ECG abnormalities for mortality risk in acute heart failure: insight from the Sub-Saharan Africa Survey of Heart Failure (THESUSHF). J Card Fail. 2014;20(1):45–52. | ||
Zielinska D, Bellwon J, Rynkiewicz A, Elkady MA. Prognostic value of the six-minute walk test in heart failure patients undergoing cardiac surgery: literature review. Rehabil Res Pract. 2013;2013:965494. |
 © 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.