Back to Journals » Risk Management and Healthcare Policy » Volume 13
Prevention and Treatment Strategies for the Cardiology Department of a Non-COVID-19 Designated Hospital in the Post-Epidemic Period
Authors Fan Q, Chen X, Lin Y, Wang Z
Received 8 May 2020
Accepted for publication 8 July 2020
Published 31 July 2020 Volume 2020:13 Pages 979—987
DOI https://doi.org/10.2147/RMHP.S261533
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Professor Marco Carotenuto
Qian Fan, Xin Chen, Yan Lin, Zhiquan Wang
Department of Cardiology, Zhongnan Hospital of Wuhan University, Wuhan University, Wuhan, People’s Republic of China
Correspondence: Zhiquan Wang
Department of Cardiology, Zhongnan Hospital of Wuhan University, No. 169 Donghu Road, Wuchang District, Wuhan 430071, Hubei, People’s Republic of China
Email [email protected]
Background: Coronavirus infection disease 2019 (COVID-19) occurred in Wuhan in December 2019. With the spread of the virus, the global epidemic situation has become extremely serious, especially in the United States, Spain and Italy. Due to a series of control measures, the epidemic situation in Wuhan has been alleviated to a certain extent, and this region has entered into a post-epidemic period. The treatment of some acute and worsened cardiovascular diseases has become more complex because of epidemic prevention measures.
Patients and Methods: We examined cardiovascular patients in the emergency department, as well as outpatient clinics and inpatient units in the Zhongnan Hospital of Wuhan University, from March 20th to April 17th, 2020, as the study subjects, and we performed standard medical activities according to the principles of border treatment and border protection. Additionally, we aimed to minimize the adverse effects of the epidemic on the therapy that was administered to cardiology patients.
Results: Due to this standard and feasible strategy, the cardiology department admitted a total of 97 patients, with 36 patients being discharged. No patients have been observed to become infected with SARS-CoV-2 in the cardiology department. In addition, we have no outpatient, caregivers or medical staff infected.
Conclusion: Our study aimed to provide prevention and treatment strategies for the rapid and effective medical recovery of patients in non-COVID-19 designated hospitals in high-risk areas after remission, as well as in low- and medium-risk areas.
Keywords: post-epidemic period, non-COVID-19 designated hospitals, strategy
Introduction
Coronavirus infection disease 2019 (COVID-19), which is caused by severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2), was first reported in Wuhan in December 2019. Patients with COVID-19 are the main source of infection, but asymptomatic latent infections can also be contagious. The primary manner in which COVID-19 appears to spread is via person-to-person contact via air droplets or skin contact.1 With the spread of the virus occurring in different regions and countries, the global epidemic situation has rapidly deteriorated. On March 11th, the World Health Organization (WHO) announced that the COVID-19 outbreak had acquired pandemic characteristics and had become a public health event that seriously threatened human health. As of April 17th, 2020, COVID-19 has been transmitted through more than 200 countries and regions, with nearly 2.2 million people being infected and more than 140,000 having died. At present, according to the statistics of epidemic reports, the top three countries (in regard to the number of confirmed cases) are the United States, Spain and Italy, with the number of cases in New York state, Madrid and Lombardy accounting for 33.3%, 27.6% and 37.3% of the total cases in these countries, respectively. There have been similarities between the current epidemic situation in these areas and the severity of cases in Wuhan in China at the time of its epidemic situation, and the epidemic incidence curve from these areas has been demonstrated to overlap with that of Wuhan.2 Due to the strict screening, centralized treatment and community control measures that have been adopted by the government, the number of new cases per day in Wuhan has decreased from the initial number of thousands of cases to 0 case, and the effective reproduction number (Rt) has decreased from the peak value of 3.82 to less than 0.3, which is evidence that the epidemic situation was effectively alleviated.3 However, with the gradual return of nearly 50,000 COVID-19 infected patients to the communities and hospitals, as well as the emergence of a small group of new asymptomatic cases and potential foreign importers, current medical activities still face tremendous challenges. For example, cardiovascular disease, as the most common disease affecting the population, is an urgent and critical issue in most patients. Previous studies have demonstrated that patients with a history of cardiovascular disease can exhibit increased risks of COVID-19 severity and death.4,5 In the early stages of the epidemic, due to the greater risk of nosocomial infection, most patients were worried about being infected, thus making them fearful of going to the hospital.6 As the epidemic situation improved and the population entered into the post-epidemic period, patients gradually returned to the hospital. Therefore, the performance of normal cardiovascular diagnosis and treatment procedures in the post-epidemic stage, while simultaneously ensuring aggressive treatment for the patient, provisions of medical protection, the timely identification of patients who may possibly have COVID-19 and effective isolation, is very necessary.
Hence, we examined cardiovascular patients in the emergency department, as well as patients in outpatient clinics and inpatient units of the Zhongnan Hospital of Wuhan University, from March 20th to April 17th, 2020, in this study. The objective of this study was to analyse the incidences of COVID-19 infections after strict standard procedures were implemented for patients and to explore the strategies of treatment and protection in the post-epidemic period. These analyses will provide guidance for some countries in gradually performing medical activities, especially for patients with cardiovascular disease in high-risk areas after the peak outbreak, at the same time, the analyses may provide strategies for some countries to quickly initiate the treatment of non-COVID-19 patients in medium-risk and low-risk areas that have sustained long periods of the epidemic.
Patient Data Statistics
As a designated hospital for the treatment of COVID-19 in the early stages, the Zhongnan Hospital of Wuhan University opened its emergency room on March 20th, 2020, after a thorough disinfection. The emergency room patients mainly included local and referred patients. A total of 2316 patients were treated in the emergency department, including 1697 patients with medical emergencies and 619 patients with surgical emergencies, and 63 patients were admitted to the cardiology ward. Prior to the opening of the outpatient department of cardiology, the source of the visits and the inpatients was only via the emergency department. Due to the gradual improvement of the epidemic situation in Wuhan, the number of newly confirmed cases was documented at 0 for 1 week, and no confirmed patient was identified in the emergency department. The specialist outpatient of cardiology department was opened on March 27th. By April 17th, a total of 1350 cases had been treated, including 34 hospitalized patients.
Based on the previously described two sources of inpatients, a total of 97 patients were admitted to our department, including 23 patients with acute heart failure, 30 patients with acute coronary syndrome, 12 patients with arrhythmia and 32 patients with other diseases. All of the patients were transferred to the buffer ward. After statistical analysis of the data, it was demonstrated that 0 patients were positive for COVID-19 via nucleic acid testing by the use of reverse transcription-polymerase chain reaction. It was also demonstrated that 2 patients were positive for the IgG antibody against SARS-CoV-2, and 1 patient was weakly positive for the IgM antibody against SARS-CoV-2. Two IgG-positive patients were out-of-hospital infection cases and have currently recovered. A 56-year-old male patient with rheumatic heart disease was observed to be weakly IgM positive, and he did not demonstrate symptoms of cough, sputum, fever or other discomforts. At the time of the emergency admissions, relevant examinations had been performed to exclude the diagnosis of COVID-19, but the IgM antibody was detected as being weakly positive, the nucleic acid testing was negative and the pulmonary CT showed right upper lobe, ground glass opacities in the buffer ward during the hospitalization on April 1st. Subsequently, the IgM antibody was again tested, and the result was negative on April 2nd. Therefore, COVID-19 consultants in the hospital were invited to assist in the final exclusion determination, and they considered that the patient’s condition may have been related to the disturbance caused by his rheumatic immune heart disease.
Management Strategies and Recommendations for Outpatient, Emergency and Inpatient Cases in Cardiology
Outpatient Management Mode of Cardiology
- Online appointment: by following the official account of the hospital, the patient entered the outpatient appointment platform. The interface indicated whether the body temperature was greater than 37.3°C, whether the patient had been exposed to suspected or confirmed personnel within 14 days and whether the patient had been diagnosed with COVID-19, as well as other related aspects of their medical history. If none of these conditions were observed, then the patient was able to go to the next step and select the doctor and time period for the doctor visit.
- Treatment process: after signing the epidemic notification and commitment contract, the patient entered the outpatient building and went to the cardiology clinic for treatment. The escorting personnel of the patient were not allowed to enter the outpatient clinic. If the patient needed to be accompanied by a family member, then the family member was also required to have their temperature measured, and they were also inquired about their medical and contact history. See Figure 1 of the outpatient department of cardiology for more details.
- From the time of the establishment of the clinic, the specialists in the cardiology outpatient area adopted second-level protection measures (See Supplementary Table S1 for details). One week after the opening of the clinic, a retrospective analysis of the hospital outpatient data demonstrated that, out of approximately 6000 patients, there were no confirmed or suspected cases. The protection level of the cardiology clinic doctors was adjusted to the one-level on April 10th.
 |
Figure 1 Flow chart of the outpatient department of cardiology. |
Admission Procedures for Cardiovascular Patients
From the time of the opening of the clinic on March 20th, patients from emergency or outpatient sources were required to strictly adhere to the four items of COVID-19 (blood routine examination, pulmonary CT imaging, IgG+IgM antibody testing and nucleic acid testing) before entering the cardiology ward. After the exclusion of SARS-CoV-2 infection, the patients could then be admitted to the department of cardiology. All of the patients were transferred to the buffer room of the department of cardiology for 1–2 days, and the use of nucleic acid testing was performed again. If no abnormalities were detected, then the patients could be transferred to the general ward. If there was an abnormality detected upon re-examination, then the patient was transferred to the cardiology isolation ward, and the diagnosis was quickly and clearly performed; any confirmed cases were transferred to the designated hospital as soon as possible. In addition, family members were not allowed to accompany the patient in the ward. If the patient truly needed to be accompanied by family members (due to cases of paralysis and unconsciousness), then only one family member was authorized to accompany the patient. The family members remaining in the ward were required to truthfully disclose their health status and to complete the COVID-19 four-item procedure in the emergency or outpatient clinics. Normal people can only stay after signing an informed consent. At the same time, in order to avoid cross-infections, other individuals are not permitted to visit.
From March 20th to March 27th, the patients who were admitted only passed through the emergency route (See Figure 2 for details). With the opening of the outpatient department of cardiology on March 27, the admissions of patients originated from the emergency and outpatient departments (See Figure 3 for details).
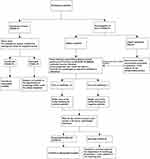 |
Figure 2 Flow chart of emergency admission in the department of cardiology. |
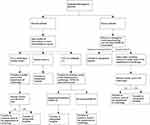 |
Figure 3 Flow chart of the emergency and outpatient departments of cardiology. |
Ward Management of Cardiology Department
The buffer ward of the cardiology department was initially established in the buffer building of the hospital, and the ward was adjusted to the specialty setting of the cardiology ward after 1 week.
The hospital buffer building setting requirements were comprised of multiple aspects. First, the building was divided into a positive area and a negative area. The positive area accepted patients with abnormal pulmonary CT or antibody results from the emergency screening procedure. The negative area accepted patients with normal, routine blood tests, as well as normal CT and antibody tests, during the emergency screening procedure. Additionally, patients were isolated in a single room, and the treatment strategy adopted the dual management mode of cardiologists and buffer doctors. In the ward, the medical staff enacted second-level protection, and patients were given ordinary-level protection. After the confirmation of the second nucleic acid negative result, the patient could then be transferred to the common ward of the cardiology department to continue their treatment.
The cardiology department setting requirements consisted of the following factors. First, the department was divided into a common ward, a buffer ward and an isolation ward. The isolation ward was located in a relatively independent position at the blind end of the ward. Additionally, there was a substantial partition between the common ward and the buffer ward. A special room for the application and removal of protective equipment was also set up in the ward. The medical staff and patients in the common ward implemented ordinary-level protection. In the early stages of the buffer ward, the medical staff were given second-level protection, and the patients were provided with ordinary-level protection. Through the analysis of previously collected data, it was observed that, from the time of the opening of the department on March 20th, no suspected or confirmed cases were detected in the cardiology ward. On April 10th, the level of medical protection in the buffer ward was adjusted from second-level to one-level. The specific details of the ward setting are shown in Figure 4.
 |
Figure 4 Setting diagram of the cardiology ward. |
Medical Staff
Before returning to work, all of the medical staff were arranged to conduct the measurements of the four items of the COVID-19 protocol. In the case of ensuring medical care and safety, the scheduling pattern was changed. The medical staff in the common ward and in the buffer/isolation ward were separated, in order to avoid cross-infection in the ward. Situations of close contact (such as communication) between the medical staff and the patients or their families in the buffer ward were performed in a special area.
Non-Invasive Tests in the Department of Cardiology
Non-invasive tests were integral to the decision-making process in the cardiology department, with such tests including electrocardiograms, echocardiograms and stress testing, among other procedures. Before the performance of these operations, we would enact strict disinfection procedures before the use of the instruments. Furthermore, we would perform another round of disinfection after the use of instruments, in order to avoid cross-infection.
Interventional Patient Management in the Department of Cardiology
The department of cardiology had two catheterization rooms. One room was located in the contaminated area on the same floor as the emergency department, and the other room was located in the cleaning area of the internal medicine admission building.
- The patient was admitted to the hospital in a state of emergency and required an immediate operation, due to the emergency situation. If COVID-19 screening was not performed or if the screening results were not returned to the staff, then the medical staff adopted second-level protection, and the patient was administered first-level protection. The operation would then be performed in the catheter room in the contaminated area. The patient was transferred to the hospital buffer zone (the hospital buffer building) or to the buffer/isolation ward in the department of cardiology, based on the screening results and the patient’s condition.
- Hospital emergency operation:
- In the buffer or isolation ward of the cardiology department, patients with COVID-19 imaging features from the pulmonary CT or patients with positive serum IgG/IgM antibody results required immediate operations, due to the emergency situation, and they received their operations in the catheter room of the contaminated area. The medical staff adopted second-level protection, and the patient was administered first-level protection. The patient was transferred to the hospital buffer zone (the hospital buffer building) or to the buffer/isolation ward in the department of cardiology.
- The nucleic acid testing, pulmonary CT and IgG/IgM antibody results were negative, and the second nucleic acid test had not yet been performed (or the test result had not yet been returned to the patient). Due to the emergency situation, an immediate operation was required to be conducted in the catheter room of the non-contaminated area. The medical staff and the patient both adopted one-level protection measures. The patient was returned to the same ward area after the operation was completed.
- Patients who received emergency operations in the common ward underwent the procedures in the catheter room in the cleaning area. The medical staff and the patient both adopted one-level protection measures. The patient was returned to the same ward area after the operation was completed.
Discussion
In the post-epidemic period of COVID-19, the treatment of some acute and worsened cardiovascular diseases has become more complex because of epidemic prevention. It was particularly important to standardize the procedures of emergency and outpatient treatment, to set up the buffer area of the ward, to select the catheter room and to adjust the treatment strategy and protection level. The cardiology department of the Zhongnan Hospital of Wuhan University performed standard medical treatments according to the principle of border treatment and border protection. For example, if patients underwent emergency or selective operations, then appropriate treatment options and catheterization rooms were selected according to a rigorous operation evaluation process, and postoperative patients were also transported to the appropriate ward, thus avoiding cross-infection.7
Due to this standard and feasible strategy, from March 20th, 2020 to April 17th, 2020, the cardiology department admitted a total of 97 patients, with 36 patients being discharged. The operation was performed as follows: 5 cases (including 4 PCI cases and 1 permanent pacemaker case) were reported in the contaminated area because of emergency situations, 29 cases were reported in the selective cleaning area, no cases of emergency operations were reported in the buffer/isolation ward and no cases of emergency operations were reported in the common ward. At present, no patients, caregivers or medical staff have been observed to become infected with SARS-CoV-2 in the cardiology department, thus indicating that the project was successful in screening cases, avoiding cross-infection, ensuring the timely and effective treatment of patients and minimizing adverse effects on the diagnosis and treatment of cardiovascular diseases. In contrast, the lack of standard nosocomial infection prevention measures may result in the occurrence of serious events. For example, an 87-year-old male patient was reported by the Health Commission of Heilongjiang Province during hospitalization as having not undergone rigorous screening and management protocols on April 12th, thus resulting in the infection of seven patients and accompanying staff, as well as the infection of seven medical staff in the same ward.
The patients in the post-epidemic stages are very different from the patients of the peak period of the epidemic. In the early stages of the recovery of medical activities, a buffer building can be set up to assess the infection status and/or severity of SARS-CoV-2. The buffer building could allow for the avoidance of the gathering of patients in the emergency department, as well as the prevention of the transmission of the pathogen in different buildings (caused by suspected or confirmed cases) and the preservation of manpower and material resources. With the monitoring and information feedback that are occurring during the epidemic situation, a specialized buffer ward can gradually be created. Although this ward continued to allow for the protection of patients, it favoured the effective and timely professional treatment of cardiovascular patients, especially patients with acute and critical illnesses. In addition, with the lack of suspected and confirmed cases, the second-level protection measures of medical care can be adjusted to the one-level, which can achieve the protective effects without the use of excessive protection measures, in order to avoid unnecessary waste during the post-epidemic period.
However, there were some limitations in our study. First, due to the limited study time and the limited number of patients, the research data need to be further expanded upon and investigated in the future. Second, as an experience sharing, the strategies of therapy and protection during the post-epidemic period may be adjusted, with the understanding of the pathogenesis of the disease and the development of vaccines.
Conclusion
In the post-epidemic period, effective procedures were formulated to minimize the impacts of the epidemic on the therapies for cardiology patients, according to the outpatient and inpatient departments of the Zhongnan Hospital of Wuhan University. These procedures can be adopted for the rapid and effective medical recovery of non-COVID-19 designated hospitals in high-risk areas after remission, as well as in low- and medium-risk areas.
Author Contributions
All authors contributed to data analysis, drafting or revising the article, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Bai Y, Yao L, Wei T, et al. Presumed asymptomatic carrier transmission of COVID-19. JAMA. 2020;323(14):1406. doi:10.1001/jama.2020.2565
2. Remuzzi A, Remuzzi G. COVID-19 and Italy: what next? Lancet. 2020;395(10231):1225–1228. doi:10.1016/S0140-6736(20)30627-9
3. Pan A, Liu L, Wang C, et al. Association of Public Health interventions with the epidemiology of the COVID-19 outbreak in Wuhan, China. JAMA. 2020;323(19):1915. doi:10.1001/jama.2020.6130
4. Aggarwal G, Cheruiyot I, Aggarwal S, et al. Association of Cardiovascular Disease With Coronavirus Disease 2019 (COVID-19) Severity: A Meta-Analysis. Curr Probl Cardiol. 2020;45(8):100617. doi:10.1016/j.cpcardiol.2020.100617
5. Aggarwal G, Lippi G, Michael HB. Cerebrovascular disease is associated with an increased disease severity in patients with Coronavirus Disease 2019 (COVID-19): A pooled analysis of published literature. Int J Stroke. 2020;15(4):385–389. doi:10.1177/1747493020921664
6. Wang D, Hu B, Hu C, et al. Clinical characteristics of 138 hospitalized patients with 2019 Novel Coronavirus-infected pneumonia in Wuhan, China. JAMA. 2020;323(11):1061. doi:10.1001/jama.2020.1585
7. Zhang L, Fan Y, Lu Z. Experiences and lesson strategies for cardiology from the COVID-19 outbreak in Wuhan, China, by ‘on the scene’ cardiologists. Eur Heart J. 2020;41(19):1788–1790. doi:10.1093/eurheartj/ehaa266
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
