Back to Journals » Nutrition and Dietary Supplements » Volume 12
Prevalence of Vitamin D Deficiency Among Iranian Pregnant Women
Authors Sepandi M , Esmailzadeh S, Hosseini MS, Hashemi SR, Abbaszadeh S , Alimohamadi Y , Taghdir M
Received 12 May 2020
Accepted for publication 30 June 2020
Published 24 July 2020 Volume 2020:12 Pages 97—102
DOI https://doi.org/10.2147/NDS.S261229
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Chandrika J Piyathilake
Mojtaba Sepandi,1 Simindokht Esmailzadeh,2 Mahboobeh Sadat Hosseini,1 Seyedeh Razieh Hashemi,3 Sepideh Abbaszadeh,1 Yousef Alimohamadi,4,5 Maryam Taghdir1,2
1Health Research Center, Life Style Institute, Baqiyatallah University of Medical Sciences, Tehran, Iran; 2Department of Nutrition and Food Hygiene, Faculty of Health, Baqiyatallah University of Medical Sciences, Tehran, Iran; 3Trauma Research Center, Baqiyatallah University of Medical Sciences, Tehran, Iran; 4Pars Advanced and Minimally Invasive Medical Manners Research Center, Pars Hospital, Iran University of Medical Sciences, Tehran, Iran; 5Department of Epidemiology & Biostatistics, School of Public Health, Tehran University of Medical Sciences, Tehran, Iran
Correspondence: Maryam Taghdir
Health Research Center, Life Style Institute, Baqiyatallah University of Medical Sciences, Tehran, Iran
Email [email protected]
Background: Vitamin D deficiency (VDD) is a common concern. A high prevalence of VDD has been reported among pregnant women in different countries. The aim of this study was to assess the prevalence of VDD in the first trimester of pregnancy.
Methods: This cross-sectional study was conducted on 267 pregnant women (before 14 weeks of gestation). The level of 25-hydroxyvitamin D (25(OH)D) was measured. Demographic data (age, educational level, season of blood sampling, and vitamin D supplementation intake) were collected using a questionnaire.
Results: Based on the results of the study, 205 out of 267 subjects (76.8%) had deficient vitamin D levels (< 20 ng/mL), 39 (14.6%) had insufficient levels (20– 29 ng/mL), and 23 (8.6%) had sufficient levels (≥ 30 ng/mL). In addition, 133 women (49.8%) had severe VDD. VDD was more prevalent in autumn/winter than in spring/summer (P=0.03). The prevalence of VDD was higher among the younger age group than in the older group (P=0.04). In multivariate analysis, the only variable that was significantly associated with low vitamin D status was taking supplements. Those who were not receiving vitamin D supplements had higher odds of VDD status (adjusted odds ratio=77.3, 95% CI 23.9– 249.6).
Conclusion: VDD is a public health problem in the first trimester of pregnancy. Greater awareness among healthcare providers and the community is required for prevention and appropriate treatment.
Keywords: pregnancy, vitamin D deficiency, vitamin D insufficiency
Introduction
Vitamin D deficiency (VDD) is a worldwide public health issue,1 which increases the risk of serious diseases, including cancers, cardiovascular diseases, and autoimmune diseases such as type 1 diabetes.2 A high prevalence of VDD has been reported among pregnant women and neonates in different countries.3,4 The prevalence of VDD in pregnant women varies from 18% to 84%.4 The prevalence of VDD is high in the Middle Eastern countries, such as Iran, Saudi Arabia, and the United Arab Emirates, owing to low exposure to the sun because of cultural factors.2,5
The prevalence rates of severe, moderate, and mild VDD among the Iranian adult population have been reported as 26.7%, 23.9%, and 19.6%, respectively.6 According to the results of a previous study in Iran, about 75.1% of women and 72.1% of men were suffering from VDD.6
VDD can lead to osteomalacia in pregnancy. Other consequences of VDD in pregnancy include an increased risk of gestational diabetes mellitus, preeclampsia, intrauterine growth retardation, and low birth weight.7,8 The present investigation has been conducted to study the prevalence of VDD among pregnant women (before 14 weeks of gestation).
Materials and Methods
Study Design and Sample Size
This cross-sectional study was conducted in Tehran, Iran, on 267 pregnant women (before 14 weeks of gestation) who visited the Gynaecology and Obstetrics Clinic of Baqiyatallah Hospital for a routine check-up from March 21, 2014 to March 20, 2015. The study size was calculated using the following formula:
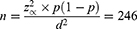
where, α=0.05, d=0.05, and the prevalence of VDD (p)=0.8.9
Eligibility Criteria, Variables, and Sampling Method
The eligibility criteria were pregnant women before 14 weeks of gestation and availability of related data. All of the study participants were residing in Tehran (36°21′N). The study sample was determined by a systematic random sampling method from all qualifying pregnant women. Demographic data (age, educational level, season of blood sampling, and vitamin D supplementation intake) were collected using a questionnaire, and body mass index (BMI) was calculated from weight in kg divided by height in m2. Volumes of about 5 mL of the fasting blood samples from all study subjects were collected and serum was separated via centrifugation (Sigma 4-16KHS) at 3500 rpm for 10 minutes. The serum level of 25-hydroxyvitamin D (25(OH)D) was measured using the chemiluminescent immunoassay (CLIA) method (Liaison® 25-OH Vitamin D CLIA kit; DiaSorin, Stillwater, MN, USA); the kit’s expected range was 3–150 ng/mL, which is based on an interassay precision that approximated 20% CV (functional sensitivity). A serum vitamin D level <20 ng/mL indicates VDD, 20–29 ng/mL indicates suboptimal status, and 30–50 ng/mL indicates an optimal level of 25(OH)D for maximal effect on parathyroid hormone.8,10
Statistical Analysis
The Kolmogorov–Smirnov test was used to evaluate the normality of data distribution. Factors related to VDD were identified through univariate and multivariate logistic regression analysis after adjusting for age (18–29 and 30–39 years), educational level (≤12 and >12 years), BMI (underweight <18.5 kg/m2, normal 18.5–24.9 kg/m2, overweight 25–29.9 kg/m2, and obese ≥30 kg/m2), season of blood sampling (spring/summer and autumn/winter), and vitamin D supplementation intake (yes or no). Age and BMI were considered as continuous variables in logistic regression analysis. The differences were considered significant at P-values of less than 0.05. Statistical analysis was conducted using SPSS software (version 16) (SPSS, Chicago, IL, USA).
Ethical Considerations
This study was approved by the ethics committee of Baqiyatallah University of Medical Sciences (Code: 5904). All subjects provided the study with voluntary informed consent prior to participation. Those who were not willing to participate in the study were not included (two women).
Results
During the study, 267 pregnant women, aged 18–39 years, were investigated. The mean age was 28.5±5.0 years. The median of serum 25(OH)D concentrations of all participants was 10 ng/mL (interquartile range [IQR]=5.4–18.6 ng/mL) and the highest reading recorded among subjects was 71.8 ng/mL.
The baseline characteristics of participants are shown in Table 1. The overall prevalence of VDD and vitamin D insufficiency was 76.7% and 14.6%, respectively. Among them, 140 women (52.4%) had severe VDD (25(OH)D <10 ng/mL). As shown in Table 2, in autumn/winter, VDD was prevalent among 82.3% of the pregnant women and in spring/summer VDD was prevalent among 71.5% of the pregnant women (P=0.03). Almost 15% of participants took vitamin D as a nutrient supplement. The median level of 25(OH)D in the age group 30–39 years was higher than in the age group 18–29 years (13.4 vs 8 ng/mL, P=0.0001). The prevalence of VDD was higher among the younger age group (P=0.04). The median (IQR) level of 25(OH)D was 10 (5.2–17.6)ng/mL in participants with a high level of education (>12 years) and 9.1 (6.1–18.9) ng/mL in those with a low level (≤12 years). Educated women (with a college degree) had a lower prevalence of VDD than those with lower educational levels (75.4% vs 77.9%, P=0.6).
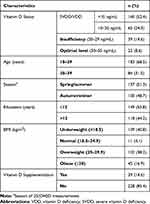 |
Table 1 Baseline Characteristics of 267 Iranian Pregnant Women |
 |
Table 2 Maternal Characteristics and Vitamin D Status of 267 Iranian Pregnant Women |
The median (IQR) levels of 25(OH)D in spring/summer and autumn/winter were 12.1 (5.8–20.7) ng/mL and 8.3 (5.2–16.1) ng/mL, respectively (P=0.07). Many of the participants were overweight (38.2%) or obese (16.9%). Overweight and obese women had a lower prevalence of VDD (74.5% and 71.1%, respectively) compared to those with normal body weight (82.6%).
Only 14.6% of participants reported a history of vitamin D supplementation. About 16.1% of women with lower educational level and 12.7% of women with higher educational level had a history of supplementation (P=0.43). Twelve percent of the younger age group and 20.2% of the older age group had received vitamin D supplements (P=0.07). The relative frequency of taking vitamin D supplements among underweight, normal weight, overweight, and obese pregnant women was 14.7%, 18.2%, 12.7%, and 17.8%, respectively (P=0.8). The frequency of taking vitamin D supplements was 7.5% in spring/summer and 11.5% in autumn/winter (P=0.16) (data not shown in the tables).
In multivariate analysis, the only variable significantly related to low vitamin D status was taking supplements. Compared to pregnant women receiving vitamin D supplements, those who were not receiving vitamin D supplements had higher odds of VDD status (adjusted odds ratio [OR]=77.3, 95% CI 23.9–249.6) (Table 3).
 |
Table 3 Crude and Adjusted Odds Ratio for Vitamin D Deficiency in 267 Iranian Pregnant Women |
Discussion
Our findings, which are consistent with previous studies, showed a high prevalence of VDD (76.8%) among Iranian pregnant women. VDD has previously been reported in Iranian pregnant women at prevalences of 78%,11 70.4%,12 and 69.2%.13 The high prevalence of VDD in women has also been observed in other countries. In New Zealand, the Netherlands, and Canada, respectively, 61%, 60%, and 46% of pregnant women were vitamin D deficient.14–16
Vitamin D status is typically influenced by factors such as latitude, season of the year, time of day, and air pollution.17 Tehran ranks among the most populated cities in the world and this makes its inhabitants susceptible to VDD. Increased accommodation in apartments because of the increased population of the city and air pollution are among the factors limiting exposure to the sun in Tehran. Tehran is a sunny city, but with limited direct exposure to the sun.
Some studies have reported a higher prevalence of VDD among elderly people,18 whereas, in the present study, as in another study conducted in Tehran,19 the prevalence of VDD was higher among the younger age group. This may be due to lifestyle modifications among younger people. Younger people favor living in apartments and using electronic devices such as mobile phones and tablets, so they take less physical activity in the open air. Moreover, to prevent skin disorders, many young women like to apply anti-solar creams to their face. VDD among adolescents has been reported at higher rates in polluted areas than in non-polluted areas.20 In 2017, Feizabad et al conducted a population-based study on 325 students in Tehran in the winter and reported that more than half of the students (52.9%) suffered from VDD (25(OH)D <20 ng/mL). VDD was more than twice as prevalent in girls (74.4%) as in boys and VDD was more prevalent in polluted areas than in non-polluted areas.20 According to cultural aspects, in Iran and other Muslim countries, women wear a scarf and long-sleeved clothes. The prevalence of VDD was 50% among pregnant Saudi women, in an area highly exposed to the sun.21 It should be noted the assessment of vitamin D status is important not only in pregnant women, but also in adolescents and young people.
In this study, the median serum 25(OH)D concentration of all participants was 10 ng/mL. In a study in Norway on five main immigrant groups, including Iranians, the median serum 25(OH)D level was 10.8 ng/mL in Iranian women.22
The median level of of vitamin D was higher in summer than in winter, showing that season, as an environmental factor, is capable of affecting the VDD. In the present study, the prevalence of VDD was significantly higher in autumn/winter than in spring/summer. These results are similar to those of preceding studies in China, Iran, and Greece.23–25 Kull et al argued that the mean serum 25(OH)D concentration in winter was meaningfully lower than in summer among the general population of Estonia.26
Our results, similarly to a previous study in Iran,27 indicated no substantial relationship between vitamin D status and the level of education. But, in contrast to our results, Atiq et al reported a significantly higher level of 25(OH)D in uneducated mothers in Pakistan,28 and another study in Norway, on five immigrant groups in Oslo, reported a positive relationship between education and vitamin D level in women born in Turkey and Iran.29 Educated women may be consuming vitamin D-fortified food or be more exposed to sunlight. Factors such as style of clothing, air pollution, insufficient vitamin D intake, and lack of routine enrichment of foods with vitamin D in Iran could account for the results of our study.19,23
The results of the present study, in line with other studies,30,31 showed that severe VDD was more prevalent among overweight and obese than in normal weight pregnant women. Therefore, it is more important to assess the vitamin D status in obese or overweight pregnant women.
According to the results of this study, after adjusting for other variables, taking vitamin D supplements was the only variable that was significantly related to vitamin D status. Vitamin D was taken by 14.6% of participants as a nutrient supplement. Compared to pregnant women taking vitamin D supplements, those not receiving vitamin D supplements had higher odds of VDD status (adjusted OR=77.3, 95% CI 23.9–249.6). This wide confidence interval may be due to the low number of pregnant women taking supplements. Vitamin D supplementation in pregnant women could be the most effective way to obtain adequate vitamin D. Unfortunately, however, vitamin D supplementation is not part of most of the ordinary pregnancy care programs in Iran and physicians have not reached a consensus in terms of the consumption of specific vitamin D supplementation. This disagreement is to some extent due to insufficient data on vitamin D status, vitamin D supplementation, and their links with pregnancy-related results to develop recommendations in Iran. Although the potential impact of VDD during pregnancy on maternal health has been much discussed recently, a contributing link between VDD during pregnancy and opposing pregnancy-related results should be determined using Hill’s criteria.32
Because the most important source of vitamin D is sunlight, 10–15 minutes of sun exposure two to three times a week is highly recommended to absorb a suitable amount of vitamin D for women of childbearing age. Also, eating fortified foods that contain vitamin D is helpful to prevent VDD.
Since the hospital in which the study was conducted is one of the largest referral hospitals in Tehran, the results of this study could be generalized to the urban population. Our study also has several limitations that should be addressed in future investigations. These include ignoring the dietary vitamin D intake measurement, extent of exposure to sunlight, and other likely risk factors for VDD.
Conclusions
According to our results, VDD is a significant public health problem in the first trimester of pregnancy. The investigation of vitamin D nutritional status in pregnant women and increased awareness among healthcare providers could help to prevent the adverse effects of VDD as well as assist in choosing good treatments.
Acknowledgements
We acknowledge the personnel of Gynecology & Obstetrics Clinic of Baqiyatallah Hospital for their assistance. The authors would like to thank the Clinical Research Development Unit of Baqiyatallah Hospital for the guidance and advice.
Abbreviations
VDD, vitamin D deficiency; IQR, interquartile range.
Ethics/Copyright
This study was approved by the ethics committee of Baqiyatallah University of Medical Sciences (Code: 5904). All subjects provided the study with voluntary informed consent prior to participation. Those who were not willing to participate in the study were excluded.
Author Contributions
All authors made a significant contribution to the work reported, whether in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Holick MF. High prevalence of vitamin D inadequacy and implications for health.
2. Dawson-Hughes B, Heaney RP, Holick MF, Lips P, Meunier PJ, Vieth R. Estimates of Optimal Vitamin D Status. Springer; 2005.
3. Saraf R, Morton SM, Camargo CA
4. Hajizadeh S, Shary JR, Reed SG, Wagner CL. The prevalence of hypovitaminosis D and its risk factors in pregnant women and their newborns in the Middle East: a systematic review. Int J Reprod Biomed. 2019;17(10):685.
5. Kovacs CS. Calcium and bone metabolism in pregnancy and lactation. J Clin Endocrinol Metab. 2001;86(6):2344–2348. doi:10.1210/jcem.86.6.7575
6. Mirhashemi S, Kalantar Motamedi M, Mirhashemi A, Taghipour H, Danial Z. Vitamin D deficiency in Iran. Int J Med Rev. 2017;4(3):64–65. doi:10.29252/ijmr-040301
7. Fiscaletti M, Stewart P, Munns C. The importance of vitamin D in maternal and child health: a global perspective. Public Health Rev. 2017;38(1):1–17. doi:10.1186/s40985-017-0066-3
8. Dawodu A, Akinbi H. Vitamin D nutrition in pregnancy: current opinion. Int J Womens Health. 2013;5:333. doi:10.2147/IJWH.S34032
9. Kazemi A, Sharifi F, Jafari N, Mousavinasab N. High prevalence of vitamin D deficiency among pregnant women and their newborns in an Iranian population. J Womens Health. 2009;18(6):835–839. doi:10.1089/jwh.2008.0954
10. Munns CF, Mairead Kiely NS, Specker BL, et al. Global consensus recommendations on prevention and management of nutritional rickets. J Clin Endocrinol Metab. 2016;101(2):394–415. doi:10.1210/jc.2015-2175
11. Azar Pirdehghan MV, Dehghan R, Zare F. High prevalence of vitamin D deficiency and adverse pregnancy outcomes in yazd, a Central Province of Iran. J Reprod Infertil. 2016;17(1):34.
12. Amouzegar A, Azizi F, Ashrafivand S, et al.Prevalence of calcium and vitamin D deficiency and their association with feto-maternal outcomes in a sample of Iranian pregnant women. Hum Antibodies. 2020;(Preprint):1–6. doi:10.3233/HAB-200415
13. Mirbolouk F, Pakseresht S, Asgharnia M, Farjadmand BM, Kazemnezhad E. Study of vitamin D status in pregnant women in north of Iran. Int J Womens Health Reprod Sci. 2016;4(4):176–180. doi:10.15296/ijwhr.2016.39
14. Judkins A, Eagleton C. Vitamin D deficiency in pregnant New Zealand women. N Z Med J. 2005;119(1241):U2144–U2144.
15. van der Meer IM, Karamali NS, Boeke AJP, et al. High prevalence of vitamin D deficiency in pregnant non-western women in The Hague, Netherlands. Am J Clin Nutr. 2006;84(2):350–353. doi:10.1093/ajcn/84.2.350
16. Ward LM. Vitamin D deficiency in the 21st century: a persistent problem among Canadian infants and mothers. Can Med Assoc J. 2005;172(6):769–770. doi:10.1503/cmaj.050177
17. Christakos S, Ajibade DV, Dhawan P, Fechner AJ, Mady LJ, Vitamin D. Metabolism. Rheum Dis Clin North Am. 2012;38(1):1–11. doi:10.1016/j.rdc.2012.03.003
18. Kinyamu HK, Gallagher JC, Balhorn KE, Petranick KM, Rafferty KA. Serum vitamin D metabolites and calcium absorption in normal young and elderly free-living women and in women living in nursing homes. Am J Clin Nutr. 1997;65(3):790–797. doi:10.1093/ajcn/65.3.790
19. Hashemipour S, Larijani B, Adibi H, et al. Vitamin D deficiency and causative factors in the population of Tehran. BMC Public Health. 2004;4(1):38. doi:10.1186/1471-2458-4-38
20. Feizabad E, Hossein-nezhad A, Maghbooli Z, Ramezani M, Hashemian R, Moattari S. Impact of air pollution on vitamin D deficiency and bone health in adolescents. Arch Osteoporos. 2017;12(1):34. doi:10.1007/s11657-017-0323-6
21. Al-Faris NA. High prevalence of vitamin D deficiency among pregnant Saudi women. Nutrients. 2016;8(2):77. doi:10.3390/nu8020077
22. Holvik K, Meyer H, Haug E, Brunvand L. Prevalence and predictors of vitamin D deficiency in five immigrant groups living in Oslo, Norway: the Oslo immigrant health study. Eur J Clin Nutr. 2005;59(1):57–63. doi:10.1038/sj.ejcn.1602033
23. Hovsepian S, Amini M, Aminorroaya A, Amini P, Iraj B. Prevalence of vitamin D deficiency among adult population of Isfahan City, Iran. J Health Popul Nutr. 2011;29(2):149. doi:10.3329/jhpn.v29i2.7857
24. Jiang L, Xu J, Pan S, Xie E, Hu Z, Shen H. High prevalence of hypovitaminosis D among pregnant women in southeast China. Acta Paediatr. 2012;101(4):e192–e194. doi:10.1111/j.1651-2227.2011.02557.x
25. Nicolaidou P, Hatzistamatiou Z, Papadopoulou A, et al. Low vitamin D status in mother-newborn pairs in Greece. Calcif Tissue Int. 2006;78(6):337–342. doi:10.1007/s00223-006-0007-5
26. Kull M, Kallikorm R, Tamm A, Lember M. Seasonal variance of 25-(OH) vitamin D in the general population of Estonia, a Northern European country. BMC Public Health. 2009;9(1):22. doi:10.1186/1471-2458-9-22
27. Salek M, Hashemipour M, Aminorroaya A, et al. Vitamin D deficiency among pregnant women and their newborns in Isfahan, Iran. Exp Clin Endocrinol Diabetes. 2008;116(6):352. doi:10.1055/s-2008-1042403
28. Atiq M, Suria A, Nizami S, Ahmed I. Maternal vitamin-D deficiency in Pakistan. Acta Obstet Gynecol Scand. 1998;77(10):970–973. doi:10.1080/j.1600-0412.1998.771004.x
29. Chapuy M-C, Preziosi P, Maamer M, et al. Prevalence of vitamin D insufficiency in an adult normal population. Osteoporos Int. 1997;7(5):439–443. doi:10.1007/s001980050030
30. Contreras-Manzano A, Villalpando S, Robledo-Pérez R. Vitamin D status by sociodemographic factors and body mass index in Mexican women at reproductive age. Salud Publica Mex. 2017;59(5, sep–oct):518–525. doi:10.21149/8080
31. Renzaho AM, Halliday JA, Nowson C. Vitamin D, obesity, and obesity-related chronic disease among ethnic minorities: a systematic review. Nutrition. 2011;27(9):868–879. doi:10.1016/j.nut.2010.12.014
32. Hill AB. The environment and disease: association or causation? Proc R Soc Med. 1965;58(5):295. doi:10.1177/003591576505800503
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
