Back to Journals » Diabetes, Metabolic Syndrome and Obesity » Volume 14
Prevalence of Metabolic Syndrome and Factors Associated With It Among Adults of West Gojjam: A Community-Based Cross-Sectional Study
Authors Walle B, Reba K, Debela Y, Tadele K, Biadglegne F, Gutema H
Received 31 December 2020
Accepted for publication 10 February 2021
Published 26 February 2021 Volume 2021:14 Pages 875—883
DOI https://doi.org/10.2147/DMSO.S295451
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Juei-Tang Cheng
Bizuayehu Walle,1 Kidist Reba,2 Yamrot Debela,3 Kassahun Tadele,4 Fantahun Biadglegne,5 Hordofa Gutema3
1Department of Physiology, College of Medicine and Health Sciences, Bahir Dar University, Bahir-Dar, Ethiopia; 2Department of Adult Health Nursing, School of Health Science, College of Medicine and Health Sciences, Bahir Dar University, Bahir-Dar, Ethiopia; 3Department of Health Education and Behavioural Sciences, School of Public Health, College of Medicine and Health Sciences, Bahir-Dar University, Bahir-Dar, Ethiopia; 4Department of Pathology, School of Medicine, College of Medicine and Health Sciences, Bahir-Dar University, Bahir-Dar, Ethiopia; 5Department of Medical Laboratory Sciences, School of Medicine, College of Medicine and Health Sciences, Bahir-Dar University, Bahir-Dar, Ethiopia
Correspondence: Hordofa Gutema Tel +251911791775
Email [email protected]
Background: Metabolic syndrome is a cluster of risk factors for cardiovascular diseases, indicating great clinical attention. However, much less attention has been given to metabolic syndrome in the study area.
Objective: The objective of this study is to determine the prevalence of metabolic syndrome and its associated factors in the adult population of West Gojjam zone, Ethiopia.
Methods: A community-based cross-sectional study was conducted in West Gojjam from September 15 to October 20, 2018. A total of 627 participants were randomly selected. The data were collected using the WHO STEP-wise approach for non-communicable diseases by contextualizing the instrument based on the study questions. The collected data were entered into and analyzed in SPSS version 20. Binary logistic regression was used to identify predictors of the dependent variable. The odds ratio was used to measure the strength of association between variables. For all statistical significance tests, the cut-off value set was p < 0.05 with CI of 95%.
Results: In the studied region, high prevalence of metabolic syndrome at 17.3% is documented. In the final model, age (adjusted odds ratio [AOR] = 1.02, CI: 1.01– 1. 05), occupation (AOR = 2.97, CI: 1.25– 7.04), a moderate or high level of physical activity (AOR = 0.28, CI: 0.14– 0.56 and AOR = 0.42, CI: 0.18– 0.97) and type of oil used for cooking (AOR = 2.62, CI: 1.87– 7.86) are significantly associated with metabolic syndrome.
Conclusion: The prevalence of metabolic syndrome in this study is high, and it is determined by age, occupation, physical activity and type of oil used for cooking. Designing an intervention which focuses on promoting a healthy lifestyle like physical activity and using oils which are liquid at room temperature to prevent the risk of major non-communicable diseases is needed.
Keywords: metabolic syndrome, community-based study, associated factor, West Gojjam
Introduction
Metabolic syndrome (MetS) is a cluster of risk factors for cardiovascular diseases (CVD) that is getting more clinical attention. It comprises multiple risk factors (abdominal obesity, dyslipidemia, hypertension, and insulin resistance with or without glucose intolerance, pro-inflammatory and pro-thrombotic states) that can occur in different combinations.1 People with MetS are twice as likely to die from, and thrice as likely to have, a heart attack or stroke compared to people without it. These people will also have fivefold greater risk of developing type 2 diabetes mellitus.2
The criteria used for the diagnosis of metabolic syndrome include abdominal obesity (waist circumference, >102 cm in men and >88 cm in women), elevated triglycerides (≥1.69 mmoL/L (≥150 mg/dL)), low high-density lipoprotein (HDL) cholesterol (<1.04 mmoL/L (<40 mg/dL) in men and <1.29 mmoL/L (<50 mg/dL) in women), hypertension (≥130/85 mmHg) or use of antihypertensive medication, elevated fasting blood glucose (≥6.1 mmoL/L (≥110 mg/dL)) or use of anti-diabetic medication and other risk factors, but the individual diagnosis of the metabolic syndrome is made when three or more of the risk factors are present.3 More recently, the International Diabetes Foundation (IDF) has suggested redefinition of the metabolic syndrome by using adapted waist circumferences for different ethnic groups.4
The detection, prevention and treatment of MetS should become a very important approach for the decrement of the cardiovascular disease burden in the world.5 According to the IDF, this cluster of factors is driving the twin global epidemics of type 2 diabetes and cardiovascular diseases. With current trends, the premature deaths and disabilities resulting from these conditions will cripple the health budgets of many nations, both developed and developing.4
Several decades ago, the burden of diseases among African populations was from infectious diseases and cardiovascular disorders were then seen as rare among these populations. However, these nations are witnessing epidemiological transition which has placed them on a double burden of disease. This implies that while infections and infestations are still a major health burden in these countries, non-communicable diseases have also become a problem.6,7 Limited available evidence suggests an increasing prevalence of MetS among populations in sub-Saharan African countries over the past decade6,8,9 and this indicates an increasing risk for developing MetS from time to time in this population. This warrants the need for having appropriate indicators to detect the problems as early as possible.
Although studies were conducted in Ethiopia focusing on MetS, only one study was conducted at community level10 while most of them were conducted at facility level by focusing on patients with specific types of diseases.9,11–16 The current study is conducted at community level among adults in West Gojjam zone of Amhara region, Ethiopia to address the existing evidence gap with regard to MetS in the community.
Methods and Materials
Study Setting and Population
The study was conducted in West Gojjam of Amhara regional state, Ethiopia from September 15 to October 20, 2018. The estimated total population of West Gojjam Zone is 2.4 million and there are five hospitals (1 teaching and 4 district) and around 108 health centers. The study was conducted among individuals who are ≥18 years old after excluding those who are unable to communicate due to mental illness.
Study design: a community-based cross-sectional study design was employed.
Sampling Procedure and Sample Size Estimation
The sample size was calculated using the single population proportion formula assuming 17.9% prevalence of MetS,9 95% confidence interval (CI) and 3% margin of error. Based on this, the sample size for this study is 627.
Out of 15 districts in the zone, 4 were randomly selected. Likewise, from each district again 4 kebeles (smallest administrative area) were selected. After proportional allocation of sample size for each of the selected kebeles, households were selected using a systematic random sampling technique and a lottery method was used to select individual participants from the household.
Data Collection Procedures
The data were collected using an interviewer-administered questionnaire which is adapted from the WHO STEPS Instrument17 for socio-demographic, behavioral, physical and biomedical measurements. Physical anthropometric measurement, blood pressure measurement, and blood sample collection and measurement were carried out by trained nurses and laboratory technicians.
Blood Pressure and Anthropometric Measurements
Blood pressure was measured using a digital measuring device. Measurements were taken after participants had been sitting for at least 5 minutes. For the reliability of measurement, it was measured twice with a 2-minute interval and the average of the two readings was recorded as the final blood pressure of the participant. Participants were weighed in kilograms in light clothing and bare feet. Height was measured using a measuring tape; participants stood in erect posture without shoes, and the measurement was recorded to the nearest 0.5 cm. Waist circumference in centimeters was measured at the midpoint between the lowermost rib and the iliac crest of the hip bone.
Laboratory Measurements
The necessary biochemical measurements were collected using the SD LipidoCare® Analyzer. Fresh capillary whole blood from the fingertip was collected using a 35-µL capillary tube in the morning after 12 hours of overnight fasting and used for testing glucose and lipid (triacylglycerol, total cholesterol, HDL-cholesterol and LDL-cholesterol) based on the recommendation of the manufacturer.
Data Quality Control
Two-day training was given for data collectors to familiarize them with the data collection tool and each variable in the questionnaire and anthropometric measurements. The English version of the questionnaire was translated into Amharic and back to English for checking language consistency. A pre-test was conducted on 5% of the sample size in another nearby zone and modification was made based on its findings. Weighing scales were checked and calibrated against a zero reading after every individual measurement. Qualified medical laboratory professionals were recruited for laboratory investigation. The laboratory personnel can also be oriented by one of the investigators who have the qualification and experience in related laboratory measurements. Furthermore, during laboratory analysis, standard operating procedure was followed, and control samples were run.
Data Management and Statistical Analysis
The data were checked for completeness, coded and entered in EPI data 3.1, and exported to SPSS 20 for analysis. Descriptive analysis was explored using frequency and percentage for categorical variables. Continuous variables were expressed as mean ± SD. Normality was checked for continuous variables and transformation was made for data that are not normally distributed. Bivariate and multivariate logistic regression analysis was used to evaluate the differences in the distribution of categorical variables for study groups. P value < 0.2 was used as a cut-off to include variables for the multivariate binary logistic regression model. The result of the OR was used for interpretation of the strength of prediction of the independent variables to the outcome. For all statistical significance tests, the cut-off value set was p<0.05 with CI of 95%.
Results
Making a response rate of 94.7%, a total of 594 respondents participated in this study.
Participants' Socio-Demographic Characteristics
The mean age of the participants was 32.7 (SD ± 5.7). Three hundred and eight (51.9%) of them were male and around two-thirds (65%) of them were married. The majority (97.5%) of the participants were Amhara in ethnicity. Two hundred and fifty (42.1%) of the participants have completed college and above. Regarding the occupation, more than one-third (37.1%) of the participants are engaged in their own job. The mean monthly income of the participants is 3532.6 (SD ± 121) Birr (Table 1).
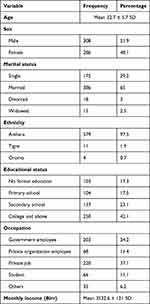 |
Table 1 Socio-Demographic Characteristics of Adult People of West Gojjam Zone, Amhara Region, Ethiopia |
Behavioral Characteristics and Dietary Practice
The majority (96.8%) of the study participants are currently non-smokers. About two-thirds (6.5.7%) of them ever drank alcohol, and of these, a large number (93.1%) of them consumed alcohol in the last one month. One hundred and forty-seven (40.9%) of the participants are engaged in a low level of physical activity. More than half (60%) of them use vegetable oils which are solid at room temperature to prepare food. Three hundred and thirty-nine (57.1%) of them consume fruit for 1–3 days in a typical week. Three hundred and forty (57.2%) of them consume vegetables for 1–3 days in a typical week (Table 2).
 |
Table 2 Behavioral Characteristics and Dietary Practice of Adult People of West Gojjam Zone, Amhara Region, Ethiopia |
Clinical Features, Anthropometric Measures and Biochemical Values
The prevalence of metabolic syndrome is 17.3%. Very few (0.3%) of the participants are currently taking anti-diabetic medication. Only seven (1.2%) of the study participants are taking anti-hypertensive medication. Around two-thirds of them are in the normal range of BMI measure. For 163 (27.4%) of the participants, the systolic blood pressure measure is ≥130 mmHg, and diastolic blood pressure measure is ≥85 mmHg for 114 (19.2%) of the participants. For one-fifth (20.5%) of men participants, the value of HDL cholesterol is <35 mg/dL, and for 53 (18.5%) of women participants, the value of HDL cholesterol is <39 mg/dL. Three hundred and forty-two (57.6%) of them have a value of <150 mg/dL for triglyceride. Regarding fasting blood sugar, 456 (76.8%) of them have lower blood sugar (Table 3).
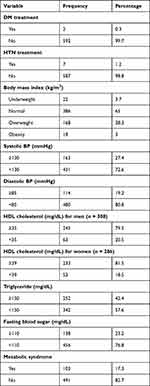 |
Table 3 Anthropometric Measures, Clinical Features and Biochemical Values of Adult People of West Gojjam Zone, Amhara Region, Ethiopia |
Factors Associated with Metabolic Syndrome
Age, sex, occupational status, ever drink alcohol, level of physical activity, type of oil used for cooking, fruit consumption and vegetable consumption were included in multiple logistic regression for having P value <0.2. In multiple logistic regression, only age, occupation, level of physical activity and type of oil used for cooking were significantly associated with metabolic syndrome at P value <0.05.
Age is found to have positive significant association with metabolic syndrome (AOR = 1.02, CI: 1.01–1.05). Participants who are working in a private company are 2.97 times more likely to develop metabolic syndrome as compared with those who are government employees (AOR = 2.97, CI: 1.25–7.04). Those who are engaged in a moderate and high level of physical activity are 28% and 42% less likely to develop metabolic syndrome as compared to their counterparts (AOR = 0.28, CI: 0.14–0.56 and AOR = 0.42, CI: 0.18–0.97 respectively). Participants who prepare food using butter are 2.62 times more likely to develop metabolic syndrome as compared with those who use vegetable oils which are liquid at room temperature (AOR = 2.62, CI: 1.87–7.86) (Table 4).
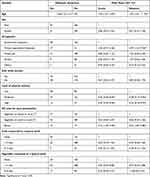 |
Table 4 Factors Associated with Metabolic Syndrome Among Adult People of West Gojjam Zone, Amhara Region, Ethiopia |
Discussion
The prevalence of metabolic syndrome is found at 17.3% with 95% CI (14.3–20.5). This finding is comparable to the studies conducted in Addis Ababa (17.9%), Ghana (15%) and Nigeria (18%).9,18,19 However, it is low as compared with other studies conducted in different parts of the country. A prevalence study conducted on MetS in northwest Ethiopia reported 66.7% and 45.3% for patients with type 2 diabetes mellitus and 40.7% for hypertensive patients.13–15 A study conducted among hypertensive patients in southern Ethiopia also revealed a 48.7% prevalence of MetS.16 The difference in the study setting and population might be the reason for the discrepancy. Those studies have used a facility as the study setting and their population was people with specific health problems, while the current study is conducted at community level on the general population. The prevalence of MetS in our study is higher as it is compared with studies which are conducted in southwest Ethiopia (9.6%) and in Cameroon (5.9% and 7.9%) for women and men respectively.8,10 Using different MetS measurement criteria in the study of southwest Ethiopia and failing to measure HDL-c concentration in the study from Cameroon might be the main reasons for the discrepancy with these studies.
Age of the study participants has a positive significant association with MetS. As age increases by one year, the occurrence of MetS will increase by 2%, which is also supported by other studies. In a study conducted in Nigeria, as age increased the chance of developing MetS significantly increased.20 Other studies also demonstrated that the risk of MetS increased as age increased.16,21 A study conducted in the southern part of Ethiopia also revealed that participants who were found in the age group of 18 and 28 years were reported at 68% less likely to develop MetS as compared with those whose age was greater than or equal to 40 years. Being in the age range of 47–57 and above 57 years was 8 and 21 times more likely to experience MetS as compared with those who are found in the age range between 25 and 35 years.13
Occupational status was also found to be a significant predictor of MetS. Working in a private company increases the risk of MetS by 2.97 times more than working in a government company. This indicates that private company employees are more engaged in a sedentary lifestyle as they are working in an office most of their working time and other studies' findings also showed a significant association between occupation and MetS. The finding of a study conducted in Gondar, Ethiopia has also shown that self-employed individuals are more likely to develop MetS compared to those who are government employees.15 Retiring from work was also found to increase the risk of developing MetS.16
Physical activity is another very important variable significantly associated with MetS. Being engaged in a moderate and high level of physical activity decreases the occurrence of MetS by 28% and 42% as compared to a lower level of physical activity. Supporting this finding, other studies showed that doing moderate and vigorous intensity of physical activity decreases the occurrence of MetS.22,23 Individuals who engage in physical activity were 53% less likely to develop MetS as compared with those who did not engage in physical activity.24 A study in Cameroon also reported that regular physical activity was significantly associated with lower development of MetS.25 A study conducted among working adults in Addis Ababa, Ethiopia reported that men who engaged in higher physical activity decreased the occurrence of MetS by 44% as compared to those engaged in a low level of physical activity.11 Another study conducted in southwest Ethiopia reported that being physically inactive increases the chance of developing MetS by 2.61 times.10
The type of oil used for cooking is also found to be a factor which is significantly associated with MetS. Using butter for food preparation increases the chance of developing MetS by 2.62 times as compared with those who use vegetable oil which is liquid at room temperature. Similar to the current study, the finding of a study conducted in north Ethiopia showed significant association between the type of oil used for cooking food and MetS. It is obvious that butter is an animal product which is rich in saturated fatty acid and risk for chronic diseases,26 while oils which are liquid at room temperature are known to be monosaturated fatty acids and have lower risk of chronic diseases.27
The major limitation of this study is the utilization of a cross-sectional study design, and it fails to establish a temporal relationship between MetS and its associated factors. Additionally, only the WHO definition of MetS was used to assess its prevalence and different figures of this prevalence could have been identified.
Conclusion
In the study site, a high prevalence of MetS is observed. Age, occupation, physical activity and type of oil used for cooking were significantly associated with MetS. Therefore, there is a need for designing an intervention which focuses on promoting a healthy lifestyle like physical activity and using oils which are liquid at room temperature for cooking to prevent the risk of major noncommunicable diseases. Furthermore, longitudinal studies should be conducted to address predictors of MetS at community level.
Abbreviations
AOR, adjusted odds ratio; BMI, body mass index; CVD, cardiovascular diseases; CI, confidence interval; HDL, high-density lipoprotein; IDF, International Diabetes Foundation; OR, odds ratio; SPSS, Statistical Package for Social Sciences; WHO, World Health Organization.
Data Sharing Statement
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
Ethical Approval and Consent
The protocol of the study was reviewed and approved by the Ethical clearance committee of Bahir Dar University. Permission was also obtained from Amhara regional and bureau and West Gojjam zone health department to conduct this study. Participants’ written informed consent was sought before they are recruited to participate in the study. Names and other personal information which can violate the confidentiality of the respondents were not taken. The data obtained in due course were confidentially stored. Those participants diagnosed to have MetS or its components were given health education and enrolled to chronic care in the health facilities. This study was conducted in accordance with the Declaration of Helsinki.
Acknowledgments
We thank Bahir Dar University for funding this study. We are also grateful to the study participants for their time and cooperation.
Author Contributions
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article and revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published; and agree to be accountable for all aspects of the work.
Funding
Bahir Dar University is the funding organization for collection, entry, analysis and interpretation of this research data.
Disclosure
The authors declare that they have no conflicts of interest for this work.
References
1. Grundy SM, Brewer B
2. Zimmet P, Alberti G, Rios MS. A new IDF worldwide definition of the metabolic syndrome: the rationale and the results. Rev Esp Cardiol. 2005;58(12):1371–1375. doi:10.1016/S0300-8932(05)74065-3
3. Alberti KG, Zimmet PZ. Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med J Br Diabet Assoc. 1998;15(7):539–553. doi:10.1002/(SICI)1096-9136(199807)15:7<539::AID-DIA668>3.0.CO;2-S
4. Alberti G, Zimmet P, Shaw J. The metabolic syndrome - a new worldwide definition. Lancet. 2005;366:9491. doi:10.1016/S0140-6736(05)67402-8
5. Eckel RH, Grundy SM, Zimmet PZ. The metabolic syndrome. Lancet. 2005;365:9468. doi:10.1016/S0140-6736(05)66378-7
6. Okafor CI. The metabolic syndrome in Africa: current trends. Indian J Endocrinol Metab. 2012;16(1):56–66. doi:10.4103/2230-8210.91191
7. Mbanya JCN, Motala AA, Assah FK. Diabetes in sub-Saharan Africa. Lancet. 2010;375(9733):2254–2265. doi:10.1016/S0140-6736(10)60550-8
8. Fezeu L, Balkau B, Kengne A-P, Sobngwi E, Mbanya J-C. Metabolic syndrome in a sub-Saharan African setting: central obesity may be the key determinant. Atherosclerosis. 2007;193(1):70. doi:10.1016/j.atherosclerosis.2006.08.037
9. Tran A, Gelaye B, Girma B, et al. Prevalence of metabolic syndrome among working adults in Ethiopia. Int J Hypertens. 2011;2011:1–8. doi:10.4061/2011/193719
10. Kerie S, Menberu M, Geneto M. Metabolic syndrome among residents of Mizan-Aman town, South West Ethiopia, 2017: a cross sectional study. PLoS One. 2019;14(1):e0210969.
11. Workalemahu T, Gelaye B, Berhane Y, Williams MA. Physical activity and metabolic syndrome among Ethiopian adults. Am J Hypertens. 2013;26(4):535–540. doi:10.1093/ajh/hps079
12. Birhane T, Yami A, Alemseged F, et al. Prevalence of lipodystrophy and metabolic syndrome among HIV positive individuals on highly active anti-retroviral treatment in Jimma, South West Ethiopia. Pan Afr Med J. 2012;13:43.
13. Biadgo B, Melak T, Ambachew S, et al. The prevalence of metabolic syndrome and its components among Type 2 diabetes mellitus patients at a tertiary Hospital, Northwest Ethiopia. Ethiop J Health Sci. 2018;28(5).
14. Tachebele B, Abebe M, Addis Z, Mesfin N. Metabolic syndrome among hypertensive patients at University of Gondar Hospital, North West Ethiopia: a cross sectional study. BMC Cardiovasc Disord. 2014;14:14. doi:10.1186/1471-2261-14-177
15. Birarra MK, Gelayee DA. Metabolic syndrome among type 2 diabetic patients in Ethiopia: a cross-sectional study. BMC Cardiovasc Disord. 2018;18(1):149. doi:10.1186/s12872-018-0880-7
16. Tadewos A, Egeno T, Amsalu A. Risk factors of metabolic syndrome among hypertensive patients at Hawassa University Comprehensive Specialized Hospital, Southern Ethiopia. BMC Cardiovasc Disord. 2017;17(1):218. doi:10.1186/s12872-017-0648-5
17. WHO. NCDs The STEPS instrument and support materials [Internet]. WHO. Available from: http://www.who.int/ncds/surveillance/steps/instrument/en/.
18. Gyakobo M, Amoah AG, Martey-Marbell DA, Snow RC Prevalence of the metabolic syndrome in a rural population in Ghana; 2012. Available from: http://ugspace.ug.edu.gh/handle/123456789/4202.
19. Ulasi II, Ijoma CK, Onodugo OD. A community-based study of hypertension and cardio-metabolic syndrome in semi-urban and rural communities in Nigeria. BMC Health Serv Res. 2010;10(1):71. doi:10.1186/1472-6963-10-71
20. Osuji CU, Omejua EG. Prevalence and characteristics of the metabolic syndrome among newly diagnosed hypertensive patients. Indian J Endocrinol Metab. 2012;16(Suppl1):S104–9. doi:10.4103/2230-8210.94256
21. Kawamoto R, Ohtsuka N, Ninomiya D, Nakamura S, Inoue A. Aging and metabolic syndrome effect on carotid atherosclerosis assessed by ultrasonography. Geriatr Gerontol Int. 2007;7(3):221–228. doi:10.1111/j.1447-0594.2007.00409.x
22. Yu S, Guo X, Yang H, Zheng L, S`un Y. Metabolic syndrome in hypertensive adults from rural Northeast China: an update. BMC Public Health. 2015;15(1):247. doi:10.1186/s12889-015-1587-7
23. Huang J-H, Li R-H, Huang S-L, et al. Relationships between different types of physical activity and metabolic syndrome among Taiwanese workers. Sci Rep. 2017;7.
24. Katzmarzyk PT, Herman KM. The role of physical activity and fitness in the prevention and treatment of metabolic syndrome. Curr Cardiovasc Risk Rep. 2007;1(3):228–236. doi:10.1007/s12170-007-0037-1
25. Assah FK, Ekelund U, Brage S, Mbanya JC, Wareham NJ. Urbanization, physical activity, and metabolic health in Sub-Saharan Africa. Diab Care. 2011;34(2):491–496. doi:10.2337/dc10-0990
26. Mayo Clinic, University of California, Los Angeles, Dole Food Company, editors. Encyclopedia of Foods: A Guide to Healthy Nutrition. San Diego, Calif: Academic Press; 2002 516.
27. Chowdhury K, Banu LA, Khan S, Latif A. Studies on the fatty acid composition of edible oil. Bangladesh J Sci Ind Res. 1970;42(3):311–316. doi:10.3329/bjsir.v42i3.669
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
