Back to Journals » Journal of Asthma and Allergy » Volume 11
Prevalence of allergic sensitization, hay fever, eczema, and asthma in a longitudinal birth cohort
Authors Owens L, Laing IA, Zhang G , Turner S , Le Souëf PN
Received 9 April 2018
Accepted for publication 4 May 2018
Published 13 August 2018 Volume 2018:11 Pages 173—180
DOI https://doi.org/10.2147/JAA.S170285
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Luis Garcia-Marcos
Louisa Owens,1,2 Ingrid A Laing,3,4 Guicheng Zhang,5,6 Stephen Turner,7 Peter N Le Souëf1
1School of Medicine, University of Western Australia, Perth, WA, Australia; 2School of Women’s and Children’s Health, University of New South Wales, Sydney, NSW, Australia; 3Telethon Kids Institute, Perth, WA, Australia; 4School of Biomedical Sciences, University of Western Australia, Perth, WA, Australia; 5School of Public Health, Curtin University, Perth, WA, Australia; 6Centre for Genetic Origins of Health and Disease, University of Western Australia, Perth, WA, Australia; 7School of Medical Sciences, University of Aberdeen, Aberdeen, Scotland, UK
Purpose: The aim of this study was to longitudinally assess the prevalence of allergic sensitization, asthma, eczema and hay fever from infancy to adulthood in a single cohort.
Participants and methods: This prospective study is based on a longitudinal birth cohort of 253 participants, with respiratory and immunological assessments at 1, 6, 11, 18 and 24 years of age. Subjects were recruited from an urban maternity hospital. Retention rates varied from 45% to 72% at follow-up assessments. Asthma diagnosis was based on physician diagnosis of asthma and symptoms/medications in the previous 12 months. Allergic sensitization was defined by the positive skin prick test. Hay fever and eczema were based on a questionnaire.
Results: The prevalence of allergic sensitization rose from 19% (n=33) at 1 year of age to 71% (n=77) at 24 years of age. The rate of asthma halved from 25% at 6 years of age to 12%–15% between 11 and 24 years of age, but the prevalence of allergic sensitization among those with asthma doubled from 50% at 6 years of age to 100% at 24 years of age. Hay fever rates rose throughout childhood from 7% at 6 years of age to 44% at 24 years of age, while the prevalence of eczema reduced from 25% at 6 years of age to 16% at 24 years of age. Parental atopy doubled the odds of asthma in their offspring by 24 years of age (odds ratio [OR]= 2.63, 95% CI 1.1–6.2, p=0.029). In all, 74% of those with asthma at 24 years of age also reported hay fever. The relationship between eczema and asthma was only significant up to 11 years of age, and the relationship between hay fever and asthma was stronger in adolescence and early adulthood than in early childhood.
Conclusion: Patterns of atopic disorders vary throughout childhood. Although the prevalence of allergic sensitization and hay fever rose throughout childhood and the prevalence of asthma reduced, the strength of their relationship with asthma increased with age.
Keywords: allergy, rhinitis, childhood, adolescence
Plain language summary
What was known before this study?
Asthma is linked to conditions such as allergies, eczema and hay fever and prevalence rates are very high in Australia.
Why did we do this study?
We measureed allergy responses in a group of people every 5-6 years, from infancy to early adulthood to seehow the rates of asthma, allergy, eczema and hay fever change with age, and how the diagnoses of asthma, allergy, hay fever and eczema relate to or predict each other.
What did we find?
• A higher proportion had asthma and eczema during early childhood (up to 6 years of age) than when older (from 11 to 24 years).
• Hayfever and allergies were more common in early adulthood than early childhood
• Eczema was closely linked to asthma in early childhood, but not in late teens.
• The link between hay fever and asthma was weaker during early childhood than during adolescence.
• Having a parent with asthma or allergy doubled the risk of their child having asthma.
What does this mean?
Allergies and hay fever are very common among adolescents with
asthma. Eczema should not be used as a predictor for
asthma in older children.
Introduction
Atopy, a genetic susceptibility to developing allergic disorders, is commonly associated with asthma in children. The prevalence of atopy is higher among children with asthma at 40%–77% compared with 21%–64% of children without asthma.1 Other atopic disorders such as eczema and allergic rhinitis are also common comorbidities for children with asthma, referred to as “allergic multimorbidity”.2,3 In unsupervised cluster analysis, performed to characterize sub-phenotype groups of asthma, atopy is more common in all asthma clusters than in non-asthmatics. Yet, it is not a defining feature of any group, as there are those with and without atopy in all clusters.4
Individuals who are atopic have a tendency to develop IgE sensitization to environmental triggers (allergens). These can include house dust mites, pollens, moulds or foods. Measurement of these hyper-IgE reactions is used to assess for atopy. Allergic sensitization in childhood is a predictive factor for the development of asthma later on. This link is strongest for those who develop allergic sensitization within the first few years of life.5,6 However, a recent study from our group showed that early onset sensitization was predictive of asthma only up to 6 years of age, and there was no significant link with asthma from 11 to 24 years of age.7
Given the prevalence of atopy in asthma, as well as the predictive strength of early sensitization for a subsequent diagnosis of asthma, allergic sensitization has been hypothesized to play a causal role in the development of asthma, possibly with allergen-induced airway inflammation interacting with the airway microbiome and viral respiratory infections to create a chronic asthmatic phenotype.6,8 However, comparison of the prevalence rates of allergic sensitization and asthma in population groups suggests that they do not closely correlate with each other, whether looking at worldwide populations or even between states in Australia, as would be expected if the relationship was causal.1,9,10 Areas with the highest rates of allergic sensitization do not have the highest rates of asthma. When the prevalence rates of sensitization and asthma throughout childhood are assessed, allergic sensitization appears to increase through infancy, school age, adolescence and early adulthood, whereas asthma prevalence peaks before 10 years of age and again in adulthood with a trough in between these periods.11–14 Therefore, our aims were to assess the longitudinal prevalence of asthma, allergic sensitization and related conditions of eczema and hay fever from infancy to early adulthood in a single cohort using data from the Perth Infant Asthma Follow-up (PIAF) study and to assess the trending of each disorder in relation to each other.
Participants and methods
The PIAF study involves a longitudinal birth cohort of 253 infants recruited between 1987 and 1989 from a general antenatal clinic in Perth, Western Australia. Recruitment has been described previously.15 Families were not selected based on risk factors for atopy or asthma. However, there was a higher prevalence of parental allergic rhinitis and eczema, but not asthma, among those who enrolled compared with those who declined. Infants were excluded if they had <37 weeks of gestation at birth or if they had a respiratory illness prior to their first assessment at 1 month. Comprehensive respiratory and immunological assessments were carried out at 1, 6 and 12 months in those aged 6, 11, 18 and 24 years. Each assessment included a questionnaire and skin prick testing, with total and specific IgE testing added from 18 years onward.
Skin prick testing to five allergens was carried out at each of the infant assessments up to 1 year (rye grass pollen, cow’s milk, egg white, Dermatophagoides pteronyssinus and Dermatophagoides farinae).16 A further six allergens were added from 6 years onward (mixed grass, cat pellet, dog dander, cockroach, Alternaria tenuis and Aspergillus fumigatus). A wheal with a diameter of at least 3 × 3 mm greater than the negative control was considered as positive.
Specific IgE testing to house dust mite, cat and a mixed grass consisting of Bermuda, rye, Timothy, meadow (Kentucky blue), Johnson and Bahia grasses was performed using ImmunoCAP in those aged 18 and 24 years. A standard cutoff value of 0.35 iU/mL was used. Allergic sensitization was defined by at least one positive allergen on the skin prick test or any specific IgE of >0.35 iU/mL, as specified in the results. Only skin prick testing was used in the longitudinal prevalence data of allergic sensitization, given that it had been measured at all assessments.
“Current asthma” was defined by a physician diagnosis of asthma with symptoms or medications within the previous 12 months. Questions relating to allergies included do you have hay fever? (yes/no), have you ever been diagnosed with eczema? (yes/no) and do you still have eczema? (yes/no).
Each assessment was authorized by the ethics committee of Western Australia Child and Adolescent Health Service Research. Written informed consent was obtained for each assessment from either the parent (if the participant was <18 years of age at the time of assessment) or the subject themselves (if the participant was >18 years of age), as approved by the ethics committee of Western Australia Child and Adolescent Health Service Research (HREC 2054EP).
Statistics
Differences in prevalence rates between groups were compared using Pearson’s chi-square test for categorical variables and Student’s t-test for continuous variables. Contemporaneous prevalence rates for asthma, eczema, allergic sensitization and hay fever were based only on those seen at the assessment.
The predictive strength of factors for a diagnosis of asthma at each assessment was measured using logistic regression, and odds ratios (ORs) were reported. Spearman’s correlation was used to assess the link between current asthma and allergic sensitization at 24 years of age. Only those with data recorded for both parents were included in the analysis of parental history. The correlation between skin prick test results and specific IgE tests was assessed using Pearson’s correlation coefficient and chi-square test.
A two-sided p value of <0.05 was used to define statistical significance. Statistical analyses were performed using IBM SPSS Statistics for Windows, version 20.0 (released 2011; IBM Corporation, Armonk, NY, USA).
Results
Population demographics
Follow-up rates at each assessment varied from 45% to 72%, with 77 subjects (30%) seen in all four assessments at 6, 11, 18 and 24 years. Characteristics and demographics of those seen at each assessment have been published previously.7 The proportion of subjects with atopic sensitization by 1 year of age was significantly higher in the group seen at 24 years (25%) than the whole cohort (19%).
Prevalence of atopy and asthma
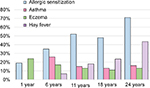
The prevalence of allergic sensitization, based on the skin prick test, rose from 19% (n=33) by 1 year of age to 71% (n=77) at 24 years of age (Figure 1). The prevalence of hay fever also increased rapidly throughout childhood, rising from 7% (n=8) at 6 years of age to 44% (n=64) at 24 years of age. The prevalence of current asthma peaked at 6 years of age at 25% (n=32), followed by a steady rate of 11%–15% between 11 and 24 years of age. Eczema prevalence halved between 1 and 11 years of age. There was no significant sex difference in the prevalence of asthma, allergic sensitization, hay fever or eczema at any assessment.
Specific IgE testing correlated strongly with skin prick testing, with a coefficient of 0.63 (p<0.001) at 18 years of age and 0.7 at 24 years of age (p<0.001). A positive specific IgE test had a 97% sensitivity and 66% specificity at 18 years of age and 88% sensitivity and 75% specificity at 24 years of age for the positive skin prick test.
Family history and asthma
Of the 242 subjects with data collected from both parents, 31% (n=75) had a parent with asthma, which doubled the risk of asthma by 24 years of age in their offspring (OR=2.35, 95% CI 1.1–5, p=0.027). Two-thirds of the subjects (66%, n=160) had a parent with eczema, asthma or allergic rhinitis, which was associated with a similar increased risk of asthma by 24 years (OR=2.63, 95% CI 1.1–6.2, p=0.029).
Prevalence of allergic sensitization and multimorbidity in asthma
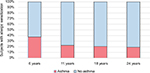
Only 50% of those with asthma had a positive skin prick test at 6 years of age, but this doubled to 100% by 24 years. The prevalence of hay fever among those with asthma rose from 14% at 6 years of age to 74% by 24 years (Figure 2). The prevalence of eczema among children with asthma halved between 6 and 24 years of age. Less than one-quarter of those with asthma had both eczema and hay fever at any assessment. All of those with asthma plus eczema at 24 years of age also had hay fever. Approximately 20% of those with allergic sensitization had asthma at each assessment between 11 and 24 years of age (Figure 3).
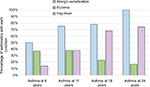  | Figure 2 Percentage of subjects with asthma and other atopic traits at each assessment. |
The predictive strength of allergic sensitization, eczema and hay fever for asthma also varied with age (Table 1). At 6 years of age, allergic sensitization was associated with an increased risk of asthma, with a trend toward statistical significance (OR=2.3, p=0.056). At 24 years of age, as all of those with asthma also had allergic sensitization, an OR could not be calculated; however, the correlation was significant (spearman’s rho 0.258, p=0.008). At 6 years of age, eczema was strongly associated with asthma (OR=4.8, p=0.002), while hay fever was not significantly associated with asthma (OR=3.7, p=0.081). Eczema was no longer predictive of asthma at 18 or 24 years of age, while hay fever was significantly associated with asthma from 11 to 24 years of age.
Prevalence of house dust mite and grass sensitization
House dust mite and mixed grass were the two most common allergens on skin prick testing at each assessment. House dust mite sensitization was slightly more prevalent at each assessment, and 40%–60% of those with house dust mite sensitization at each assessment were also sensitized to mixed grass (Figure 4).
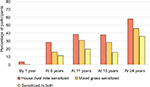  | Figure 4 Percentage of participants sensitized to mixed grass and house dust mite at each assessment. Note: Sensitization was measured by the skin prick test, wheal ≥3×3 mm. |
Discussion
Asthma, eczema and hay fever have been described as “the atopic triad”.17 We have shown in a longitudinal birth cohort with data to early adulthood that the prevalence of allergic sensitization rapidly increases throughout childhood into early adulthood. However, the associated atopic disorders do not all share the same trajectory, with only hay fever following a similar increase in prevalence into adulthood. This has important implications not only in understanding the natural history of atopy and atopic diseases but also for economic planning and disease prevention strategies.
Australia has one of the highest rates of atopy worldwide with rates continuing to rise, and atopic disorders are accompanied by a significant burden on both patients and their health systems.18–20 Atopy is associated with inherited factors and environmental exposures; therefore, collecting up-to-date local epidemiological information is necessary. In a recent longitudinal Danish study, the rate of allergic sensitization in early adulthood was 31% at 26 years of age, less than half the rate in our Australian cohort, demonstrating the importance of collecting local data.21 Both our cohort and the Danish cohort reported a similar rapid increase in the prevalence of allergic rhinitis throughout childhood; however, the trends in asthma were not concordant. In the Danish cohort, asthma rates increased between 5 and 10 years of age up to a peak of 10%, whereas in our cohort, there was an asthma prevalence of 26% at 6 years of age, followed by a reduction in later childhood. This early peak in asthma prevalence within our cohort is unlikely to be explained simply by the high rates of asthma in Australia, as by 11 years of age, asthma rates were very similar between the two cohorts but may be related to differing predominant asthma phenotypes in the two countries.
This longitudinal analysis also highlights some important features of the relationships between different atopic disorders. There has been a long running debate regarding the role of atopy in asthma and whether this is causative or not.22 Viral respiratory infections and sensitization to aeroallergens within the first few years of life appear to have a synergistic effect on both the risk of asthma developing during childhood and the degree of airway inflammation during acute exacerbations.6,8,23,24 Many studies have looked at the efficacy of early allergen avoidance in the primary prevention of asthma with mixed results.25 In our study, although there was a strong association between asthma and allergic sensitization throughout childhood and into adulthood, the prevalence of positive skin prick tests rose from 35% at 6 years of age to 71% at 24 years of age, while the prevalence of asthma dropped over the same time period. This inverse relationship is supported by previous cross-sectional studies that demonstrated that rates of allergic sensitization and asthma do not correlate.9,10 This supports the theory that only early sensitization, within the first few years of life, could have a strong causative role in asthma development.
All of those with asthma at 24 years of age had a positive skin prick test compared with only 50% of those with asthma at 6 years of age. This may be reflective of the general increase in atopy prevalence, as the prevalence of asthma among those with allergic sensitization remained stable at 20% from 11 to 24 years of age; however, asthma was strongly correlated with allergic sensitization at 24 years of age, suggesting a genuine relationship between the two.
In preschool children, eczema is one of only two major factors on the Asthma Predictive Index that helps to predict which young children with recurrent wheeze will develop asthma.26 Clinicians have been using this predictive tool for several decades when counseling parents about the risk of their child developing asthma.27 Children with eczema have also been chosen in asthma prevention studies due to their increased risk of developing asthma.28 However in our study, eczema was only associated with asthma up to 11 years of age; therefore, the absence of eczema should not be used as a clinical tool to distinguish asthma from other causes of respiratory symptoms in older children and adolescents.
We have demonstrated that a positive skin prick test has a much stronger relationship with asthma than eczema and indeed may make the diagnosis of asthma unlikely in older adolescents if negative. Previous studies have shown that multi-sensitivity is a stronger predictive tool for asthma than sensitivity to single allergens and in the UK MAAS study, several classes of atopy were identified and only early onset sensitization to multiple allergens was associated with an increased risk of asthma.29,30 Hay fever also has a strong relationship with asthma during adolescence in our cohort and may be useful as part of a clinical diagnostic tool, particularly in the absence of skin prick testing.
There is a long-standing belief in the developmental progression of allergic disorders from eczema in infancy to asthma in childhood and then allergic rhinitis in adolescence, with a resolution of the eczema over this period (the atopic march).31,32 This theory was recently disputed by a large study in the UK looking at the prevalence of eczema, asthma and hay fever in two pediatric longitudinal cohorts.33 Belgrave et al identified a number of atopic disease trajectories and demonstrated that the temporal relationships between atopic disorders are a lot more complex than previously believed. Less than 10% of their cohort followed the classical atopic march path. Unfortunately, our cohort was too small to assess the frequency of the atopic trajectories described in the UK study, but we did show that among those with asthma at 6 years of age, eczema was the most common allergic comorbidity and by 18 years, hay fever was the most common comorbidity.
Skin prick testing is often used in cohort studies as a wide range of allergens can be tested easily and cost-effectively; however, in practice, many allergy clinics use specific IgE. Unfortunately, the two methods do not correlate well in young children.34 We used both methods at 18 and 24 years of age and found that specific IgE testing had a very good sensitivity with moderate specificity for skin prick testing, likely related to the utilization of a much smaller allergen panel.
The prevalence of allergic sensitization at 24 years of age was higher than we expected for an unselected cohort at 71%; however, it was not dissimilar to the rate of 65% seen in the Dunedin birth cohort at 21 years of age.13 The increase in prevalence of atopy across childhood, which we observed, was likely due to a combination of factors. First, there has been an increase in atopy worldwide over the past few decades, and second, there is a documented increase in atopy during childhood and adolescence.12,13,35 In addition, two-thirds of the families enrolled in this study had at least one parent with a history of atopy and those participants with early sensitization were less likely to withdraw from the 24-year follow-up. This may reflect some selection bias among those recruited and retained for long-term follow-up due to their increased interest in the study. Perth is the most isolated capital city in the world, and many young adults move interstate for travel, work or college, meaning they are unable to attend follow-up assessments. This likely contributed to our poor retention rates at some assessments.
One of the limitations of this study is that the definition of asthma was based on physician’s diagnosis. This did not take the complexity of different asthma phenotypes and their underlying pathophysiology into account.36 The pathogenesis of asthma is still not clearly understood with abnormal epithelium, immature innate immune responses, genetics, abnormal lung development and the environment, all implicated.37–39 Interestingly, some of the gene mutations linking asthma, eczema and hay fever are not related to immune responses but rather the integrity of the epithelium.40–41
Conclusion
This collection of serial data at crucial developmental periods during childhood and adolescence allows for a comprehensive analysis of atopy trends in the first 3 decades of life. The longitudinal study of allergic sensitization, hay fever, eczema and asthma prevalence in an urban environment highlights that although rates of allergic sensitization and hay fever increase throughout childhood and into early adulthood and rates of asthma reduce, their relationship with asthma strengthens. Universal assumptions should not be made about the relationships between atopic disorders as they may be age dependent.
Acknowledgments
We would like to thank all the previous contributors to the PIAF study including David Mullane, Desmond Cox, Kimberley Franks, Lou Landau, Jack Goldblatt, Sally Young, Siew-Kim Khoo, Neil Gibson, Veena Judge, Lyle Palmer, Paul O’Keefe, Jackie Arnott, Steve Stick and Peter Rye. This study was funded by NHMRC research grant APP1031635, Princess Margaret Hospital Foundation Seeding grant 9383; University of Western Australia PhD scholarship and Asthma Foundation of Western Australia PhD top-up scholarship. The sponsors had no role in the design of this study or writing of this manuscript.
Disclosure
The authors have no conflicts of interest to disclose in relation to this work.
References
Pearce N, Pekkanen J, Beasley R. How much asthma is really attributable to atopy? Thorax. 1999;54(3):268–272. | ||
Pinart M, Benet M, Annesi-Maesano I, et al. Comorbidity of eczema, rhinitis, and asthma in IgE-sensitised and non-IgE-sensitised children in MeDALL: a population-based cohort study. Lancet Respir Med. 2014;2(2):131–140. | ||
Gough H, Grabenhenrich L, Reich A, et al; MAS Study Group. Allergic multimorbidity of asthma, rhinitis, and eczema over 20 years in the German birth cohort MAS. Pediatr Allergy Immunol. 2015;26(5):431–437. | ||
Moore WC, Meyers DA, Wenzel SE, et al; National Heart, Lung, and Blood Institute’s Severe Asthma Research Program. Identification of asthma phenotypes using cluster analysis in the Severe Asthma Research Program. Am J Respir Crit Care Med. 2010;181(4):315–323. | ||
Illi S, von Mutius E, Lau S, et al; Multicentre Allergy Study (MAS) Group. Perennial allergen sensitisation early in life and chronic asthma in children: a birth cohort study. Lancet. 2006;368(9537):763–770. | ||
Kusel MM, de Klerk NH, Kebadze T, et al. Early-life respiratory viral infections, atopic sensitization, and risk of subsequent development of persistent asthma. J Allergy Clin Immunol. 2007;119(5):1105–1110. | ||
Owens L, Laing I, Zhang G, et al. Early sensitization is associated with reduced lung function from birth into adulthood. J Allergy Clin Immunol. 2016;137(5):1605–1607.e2. | ||
Jackson DJ, Evans MD, Gangnon RE, et al. Evidence for a causal relationship between allergic sensitization and rhinovirus wheezing in early life. Am J Respir Crit Care Med. 2012;185(3):281–285. | ||
Peat JK, Toelle BG, Gray EJ, et al. Prevalence and severity of childhood asthma and allergic sensitisation in seven climatic regions of New South Wales. Med J Aust. 1995;163(1):22–26. | ||
Ronchetti R, Jesenak M, Rennerova Z, Barreto M, Ronchetti F, Villa MP. Relationship between atopic asthma and the population prevalence rates for asthma or atopy in children: atopic and nonatopic asthma in epidemiology. Allergy Asthma Proc. 2009;30(1):55–63. | ||
Tariq SM, Matthews SM, Hakim EA, Stevens M, Arshad SH, Hide DW. The prevalence of and risk factors for atopy in early childhood: a whole population birth cohort study. J Allergy Clin Immunol. 1998;101(5):587–593. | ||
Tai A, Tran H, Roberts M, Clarke N, Wilson J, Robertson CF. Trends in eczema, rhinitis, and rye grass sensitization in a longitudinal asthma cohort. Ann Allergy Asthma Immunol. 2014;112(5):437–440. | ||
Sears MR, Greene JM, Willan AR, et al. Long-term relation between breastfeeding and development of atopy and asthma in children and young adults: a longitudinal study. Lancet. 2002;360(9337):901–907. | ||
De Marco R, Locatelli F, Cerveri I, et al; Italian Study on Asthma in Young Adults Study Group. Incidence and remission of asthma: a retrospective study on the natural history of asthma in Italy. J Allergy Clin Immunol. 2002;110(2):228–235. | ||
Young S, Le Souëf PN, Geelhoed GC, Stick SM, Turner KJ, Landau LI. The influence of a family history of asthma and parental smoking on airway responsiveness in early infancy. N Engl J Med. 1991;324(17):1168–1173. | ||
Pepys J. Skin tests for immediate, type I, allergic reactions. Proc R Soc Med. 1972;65(3):271–272. | ||
Oettgen HC, Geha RS. IgE in asthma and atopy: cellular and molecular connections. J Clin Invest. 1999;104(7):829–835. | ||
Robertson CF, Roberts MF, Kappers JH. Asthma prevalence in Melbourne schoolchildren: have we reached the peak? Med J Aust. 2004;180(6):273–276. | ||
Beasley R. Worldwide variation in prevalence of symptoms of asthma, allergic rhinoconjunctivitis, and atopic eczema: ISAAC. Lancet. 1998;351(9111):1225–1232. | ||
O’Connell EJ. The burden of atopy and asthma in children. Allergy. 2004;59(suppl 78):7–11. | ||
Nissen SP, Kjaer HF, Høst A, Nielsen J, Halken S. The natural course of sensitization and allergic diseases from childhood to adulthood. Pediatr Allergy Immunol. 2013;24(6):549–555. | ||
Peat JK, Tovey E, Toelle BG, et al. House dust mite allergens. A major risk factor for childhood asthma in Australia. Am J Respir Crit Care Med. 1996;153(1):141–146. | ||
Gern JE. Mechanisms of virus-induced asthma. J Pediatr. 2003;142(2 suppl):S9–S13; discussion S13–S14. | ||
Murray CS, Poletti G, Kebadze T, et al. Study of modifiable risk factors for asthma exacerbations: virus infection and allergen exposure increase the risk of asthma hospital admissions in children. Thorax. 2006;61(5):376–382. | ||
van Schayck OC, Maas T, Kaper J, Knottnerus AJ, Sheikh A. Is there any role for allergen avoidance in the primary prevention of childhood asthma? J Allergy ClinImmunol. 2007;119(6):1323–1328. | ||
Castro-Rodríguez JA, Holberg CJ, Wright AL, Martinez FD. A clinical index to define risk of asthma in young children with recurrent wheezing. Am J Respir Crit Care Med. 2000;162(4 pt 1):1403–1406. | ||
Huffaker MF, Phipatanakul W. Utility of the Asthma Predictive Index in predicting childhood asthma and identifying disease-modifying interventions. Ann Allergy Asthma Immunol. 2014;112(3):188–190. | ||
Wahn PU. Allergic factors associated with the development of asthma and the influence of cetirizine in a double-blind, randomised, placebo-controlled trial: first results of ETA®. Pediatr Allergy Immunol. 1998;9(3):116–124. | ||
Kaleyias J, Papaioannou D, Manoussakis M, Syrigou E, Tapratzi P, Saxoni-Papageorgiou P. Skin-prick test findings in atopic asthmatic children: a follow-up study from childhood to puberty. Pediatr Allergy Immunol. 2002;13(5):368–374. | ||
Simpson A, Tan VY, Winn J, et al. Beyond atopy: multiple patterns of sensitization in relation to asthma in a birth cohort study. Am J Respir Crit Care Med. 2010;181(11):1200–1206. | ||
Dharmage SC, Lowe AJ, Matheson MC, Burgess JA, Allen KJ, Abramson MJ. Atopic dermatitis and the atopic march revisited. Allergy. 2014;69(1):17–27. | ||
Wahn U, Bergmann R, Kulig M, Forster J, Bauer CP. The natural course of sensitisation and atopic disease in infancy and childhood. Pediatr Allergy Immunol. 1997;8(10 suppl):16–20. | ||
Belgrave DC, Granell R, Simpson A, et al. Developmental profiles of eczema, wheeze, and rhinitis: two population-based birth cohort studies. PLoS Med. 2014;11(10):e1001748. | ||
Schoos AM, Chawes BL, Følsgaard NV, Samandari N, Bønnelykke K, Bisgaard H. Disagreement between skin prick test and specific IgE in young children. Allergy. 2015;70(1):41–48. | ||
Asher MI, Montefort S, Bjorksten B, et al; ISAAC Phase Three Study Group. Worldwide time trends in the prevalence of symptoms of asthma, allergic rhinoconjunctivitis, and eczema in childhood: ISAAC Phases One and Three repeat multicountry cross-sectional surveys. Lancet. 2006;368(9537):733–743. | ||
Pavord ID, Beasley R, Agusti A, et al. After asthma: redefining airways diseases. Lancet. 2018;391(10118):350–400. | ||
Holgate ST, Arshad HS, Roberts GC, et al. A new look at the pathogenesis of asthma. Clin Sci. 2010;118(7):439–450. | ||
Owens L, Laing IA, Zhang G, Le Souëf PN. Infant lung function predicts asthma persistence and remission in young adults. Respirology. 2017;22(2):289–294. | ||
Burke H, Leonardi-Bee J, Hashim A, et al. Prenatal and passive smoke exposure and incidence of asthma and wheeze: systematic review and meta-analysis. Pediatrics. 2012;129(4):735–744. | ||
Palmer CN, Irvine AD, Terron-Kwiatkowski A, et al. Common loss-of-function variants of the epidermal barrier protein filaggrin are a major predisposing factor for atopic dermatitis. Nat Genet. 2006;38(4):441–446. | ||
Weidinger S, O’Sullivan M, Illig T, et al. Filaggrin mutations, atopic eczema, hay fever, and asthma in children. J Allergy Clin Immunol. 2008;121(5):1203–1209.e1. |
 © 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.