Back to Journals » Pediatric Health, Medicine and Therapeutics » Volume 10
Prevalence and associated factors of perinatal asphyxia among newborns in Dilla University referral hospital, Southern Ethiopia– 2017
Authors Alemu A, Melaku G , Abera GB , Damte A
Received 28 November 2018
Accepted for publication 16 May 2019
Published 24 July 2019 Volume 2019:10 Pages 69—74
DOI https://doi.org/10.2147/PHMT.S196265
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Roosy Aulakh
Abebe Alemu,1 Getnet Melaku,1 Gerezgiher Buruh Abera,2 Ashenafi Damte2
1Department of Midwifery, College of Health Science and Medicine, Dilla University, Dilla, Ethiopia; 2Department of Nursing, College of Health Sciences, Mekelle University, Mekelle, Tigray, Ethiopia
Background: Globally, perinatal asphyxia is a significant contributing factor for neonatal morbidity and mortality. Thus, this study was aimed to assess the prevalence and associated factors with perinatal asphyxia among newborns in Dilla University referral hospital.
Methods: A cross-sectional study was conducted among newborns in Dilla University referral hospital, Ethiopia from February to April 2017. Systematic random sampling techniques were used to enroll a total of 262 study subjects. Multivariate logistic regression analysis was used to identify factors associated with the perinatal asphyxia among newborns.
Result: Of the newborns, 32.8% had perinatal asphyxia, and factors associated significantly were anemia during pregnancy (adjusted OR=2.99, 95%CI: 1.07–8.35), chronic hypertension (adjusted OR=4.89, 95%CI: 1.16–20.72), meconium-stained amniotic fluid (adjusted OR=3.59, 95%CI: 1.74–7.42), and low birth weight newborns (adjusted OR=3.31, 95%CI: 1.308–8.37).
Conclusion: Maternal anemia during pregnancy, chronic hypertension, meconium stained amniotic fluid, and low birth weight were significantly associated with perinatal asphyxia. Therefore, early screening and appropriate intervention during pregnancy, and intrapartum might reduce perinatal asphyxia among newborns.
Keywords: perinatal asphyxia, newborn, Dilla, Ethiopia
Background
Globally, perinatal asphyxia has significantly contributed to neonatal morbidity and mortality. Perinatal asphyxia is defined as the inability of the newborn to initiate and sustain adequate respiration after delivery.1,2 In developing countries neonatal mortality rate constitutes 42% of under-5 deaths.3,4 According to a World Health Organization report, perinatal asphyxia is the third leading cause of under-5 child deaths (11%) following preterm birth (17%) and pneumonia (15%).5,6
In developing countries, neonatal deaths accounted for 52% of all under-5 child mortality in South Asia, 53% in Latin America and Caribbean, and 34% in sub-Saharan Africa due to preventable causes including perinatal asphyxia.7,8
In Ethiopia, perinatal asphyxia is one of the leading causes of neonatal mortality, constituting 34%.8 A study revealed that perinatal asphyxia can lead to physical, mental and social incapability in newborns due to severe hypoxic-ischemic organ damage.9
Studies showed that mother’s age less than 20 years, mother's illiteracy, multiple pregnancy, and gestational age were the determinants of perinatal asphyxia.10,11 Perinatal asphyxia was associated with maternal anemia during pregnancy, pregnancy-induced hypertension, antepartum hemorrhage, antenatal care visits less than 3 and lack of ultrasound checkup.12,13
The literature revealed that neonatal and intrapartum-related factors like breech presentation, mode of delivery, meconium-stained amniotic fluid (MSAF), prolonged rupture of membrane, prolonged labor, activity, pulse, grimace, appearance and respiration (APGAR) score<7, birth weight, and prematurity of the newborn were found to be significant factors for birth asphyxia.12,13
According to the Ethiopian demographic health survey 2016, the reduction in neonatal mortality was comparatively low. The international community agreed to reduce neonatal mortality to at least as low as 12 deaths per 1,000 live births by 2030.12–14
In most developing countries, a small number of data are available on risk factors associated with perinatal asphyxia. There is a lack of evidence showing that maternal and neonatal factors play an important role in the occurrence of birth asphyxia.15–21
However, perinatal asphyxia has a high contribution to neonatal morbidity and mortality. There are insufficient studies conducted on perinatal asphyxia in the study area. Therefore, this study was aimed to assess the prevalence and associated factors with identifying determinants of perinatal asphyxia among newborns at Dilla University referral hospital, Southern Ethiopia, 2017.
Materials and methods
Study design and period
This cross-sectional study was conducted from February to April 2017 in Dilla University referral hospital, southern Ethiopia.
Sampling procedure
A total of 262 postnatal mothers who have live newborns were enrolled using a systematic random sampling technique.
Inclusion and exclusion criteria
All live newborns during the data collection period were included in the study, but newborns with congenital anomalies were excluded.
Data collection and quality assurance
An interviewer-administered structured questionnaire was used to obtain information on socio-demographic characteristics and obstetric history and related risk factors. To assure data quality, training was given for data collectors, the questionnaires were checked for completeness before data entry by the principal investigator.
Data processing and analysis
Data were analyzed using SPSS version 22 software (IBM Corporation, Armonk, NY, USA). A binary logistic regression was done to examine association of dependent and independent variables, and variables with p-value <0.2 were entered into multivariate logistic regression analysis. The variables with p-value <0.05 in the multivariate analysis were significantly associated with the outcome variable.
Operational definition
Perinatal asphyxia is the inability of a newborn to initiate and sustain respiration, by scoring an APGAR score less than 7 persistently for more than 5 min after delivery.
Study variables
The dependent variable of this study was perinatal asphyxia, and independent variables were categorized maternal socio-demographic and obstetric characteristics.
Ethical consideration
Ethical clearance was obtained from the College of Health Sciences, Mekelle University. The permission was found from Dilla University referral hospital medical director office. An informed written consent was obtained from all mothers of the newborns that were included for the study.
Results
Maternal socio-demographic and obstetric characteristics
From total (N=262), 256 study participants responded to a questionnaire (response rate was 97.7%). More than three quarters of the study subjects were literate and 106 (41.4%) of them were housewives. Two hundred and twenty-nine (89.5%) of mothers had a singleton pregnancy, and 144 (56.3%) of them were multiparous (Table 1).
 |
Table 1 Socio-demographic and obstetric history of mothers of newborns at Dilla University referral hospital, Southern Ethiopia 2017 (n=256) |
Neonatal characteristics
In the study, 129 (50.4%) women who participated delivered female neonates and 45 (17.6%) of newborns were low birth weight. Based on gestation age 66 (25.8%) of neonates were delivered at preterm; 157 (61.3%) born at term and 33 (12.9%) at post-term (Table 2).
 |
Table 2 Characteristics of neonates who were born in Dilla University referral hospital, Southern Ethiopia, 2017 (n=256) |
Magnitude of perinatal asphyxia
The number of neonates assessed as perinatal asphyxia immediately after delivery was 84 (32.8%) and 172 (67.2%) neonates delivered were assessed as non-asphyxiated (Figure 1).
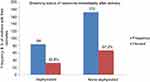 |
Figure 1 Breathing status of neonates immediately after delivery who were born at Dilla University referral hospital Southern Ethiopia, 2017 [n=256]. |
Factors associated with perinatal asphyxia
Multivariate logistic regressions analysis showed that anemia during pregnancy, chronic hypertension, meconium-stained amniotic fluid, and low birth weight were significantly associated factors with neonatal asphyxia among newborns.
Neonates delivered from mothers who had anemia during pregnancy were 3 times more likely to be asphyxiated as compared to neonates from mothers who were non-anemic during pregnancy (adjusted OR=2.992, 95%CI: 1.073–8.35) and neonates from mothers who had chronic hypertension were about 5 times more likely to be asphyxiated compared to those newborns from mothers who encountered no hypertension (adjusted OR=4.9, 95%CI: 1.16–20.7).
Neonates who were delivered with meconium-stained amniotic fluid were 3.5 times more likely to have perinatal asphyxia as compared to those neonates delivered with clear amniotic fluid (adjusted OR=3.5, 95%CI: 1.739, 7.4), and low birth weight newborns were 3 times more likely to develop perinatal asphyxia compared to normal weight newborns (adjusted OR=3.309, 95% CI: 1.308, 8.368) (Table 3).
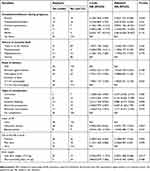 |
Table 3 Associated factors with perinatal asphyxia among newborns at Dilla University referral hospital, southern Ethiopia, 2017 (n=256) |
Discussion
The prevalence of perinatal asphyxia among newborns was 32.8%. This finding is higher than those of other studies conducted in India (6.6%), Nigeria (21.1%), Cameroon (8.5%), and also at hospitals in Jimma (11.1%), and Addis Ababa (16.2%) in Ethiopia, respectively.6,12,14,21 This finding inconsistency may be due to the difference in the study population, study area and time.
In this study, perinatal asphyxia was significantly associated with maternal anemia during pregnancy, maternal chronic hypertension, meconium-stained amniotic fluid and low birth weight of newborns.
In this study, anemia during pregnancy was found to be significantly associated with perinatal asphyxia. This is consistent with other study findings in rural districts of Pakistan and India.18,20 Anemia during pregnancy might affect fetal development and complicate the birth. Thus, having antenatal follow up during pregnancy may prevent anemia.
In this study, maternal history of chronic hypertension was found to be significantly associated with perinatal asphyxia. Neonates from mothers with chronic hypertension were found to be asphyxiated compared to newborns from mothers who encountered no disease during pregnancy. This finding is in line with other studies that reported chronic hypertension was found to be a risk factor for perinatal asphyxia in Ethiopia, Cameroon, and India.14,20,22 This might be maternal hypertension directly affect the fetal wellbeing in the uterus, which directly contributes to neonatal asphyxia at birth.
This study showed that meconium-stained amniotic fluid was a significantly associated factor with perinatal asphyxia. Newborns who were delivered with meconium-stained amniotic fluid were found to be asphyxiated when compared to those neonates delivered with clear amniotic fluid. This finding is in agreement with other studies that have found the meconium-stained amniotic fluid was a risk factor for perinatal asphyxia.13,23 This is because when amniotic fluid is stained due to different factors, there is a risk of fetal distress which might lead the newborn to be asphyxiated at birth.
Low birth weight was found to be a significant factor for perinatal asphyxia in this study. This finding is in corroboration with previous study findings in Ethiopia, Tanzania, and Indonesia, but it is inconsistent with a study conducted in Nigeria.9,11,12,18,22,23 This finding discrepancy might be due to the difference in the socio-economic status of the study population and the study time.
The limitation of this study was there was selection bias because only neonates delivered at the hospital were included. It is known that many mothers gave birth at home with risk; those neonates were not incorporated in this study. Thus, it may not represent the whole rural area.
Conclusion
Of the newborns, 32.8% had perinatal asphyxia, and factors significantly associated were anemia during pregnancy, chronic hypertension, meconium-stained amniotic fluid, and low birth weight. Therefore, early screening during pregnancy and providing health care is mandatory in order to reduce perinatal asphyxia among newborns.
Abbreviation list
ANC, Antenatal care; DURH, Dilla University Referral Hospital; EDHS, Ethiopian Demographic and Health Survey; LBW, low birth weight; MCH, maternal and child health; MSAF, meconium-stained amniotic fluid; NICU, neonatal intensive care unit; NMR, neonatal mortality rate; PMR, perinatal mortality rate; PROM, prolonged rupture of membranes; SDG, sustainable development goals; SNNPR, South Nations Nationalities Peoples; UNICEF, United Nation Children’s Fund.
Acknowledgments
We would like to thank all our study participants for their patience and for participating in this research.
Author contributions
All authors contributed toward data analysis, drafting and revising the paper, gave final approval of the version to be published, and agree to be accountable for all aspects of the work
Disclosure
The authors report no conflicts of interest in this work.
References
1. Lawn JE, Cousens S, Zupan J. Lancet neonatal survival steering team 4 million neonatal deaths: When? Where? Why? Lancet. 2005;365:891–900. doi:10.1016/S0140-6736(05)71048-5
2. World health organization, Global Health Organization (GHO) Data. Available from: http://www.who.int/whoghod/whoghodt/.
3. WHO; Word Health Statistics: Part II Global health indicators 2015. Available form: http://www.who.int/whosis/whostat/EN_WHS2011_Full.pdf. Accessed November 20, 2016.
4. FMOH, UNICEF. Countdown to a healthier Ethiopia: building on successes to accelerate newborn survival; 2015. Available from: (www.ephi.gov.et). Accessed November 20, 2016.
5. WHO. Word health statistics: part I global health indicators; 2015. Available from: (http://www.who.int/whosis/whostat/EN_WHS2011_Full.pdf).
6. WHO. Global health observatory data repository world health organization; 2015. Available from: http://apps.who.int/ghodata/.
7. Liu et al. Distribution of causes of neonatal and under-five deaths, CHERG/WHO/UNICEF. Lancet. 2014;388:3027–3035.
8. United Nations Children’s Fund, World Health Organization, World Bank and United Nations. Levels & Trends in Child Mortality Report 2015. New York (NY), Geneva and Washington (DC). Available from: http://www.unicef.org/publications/flesSept_15.pdf.
9. Olga G., Yeghiazaryan K, Cebioglu M et al. Birth asphyxia as the major complication in newbornsa: moving towards improved individual outcomes by prediction, targeted prevention and tailored medical care. EPMA J. 2011;2:197–210. doi:10.1007/s13167-011-0087-9
10. Bilkisu G. Prevalence and Risk Factors for Perinatal Asphyxia as Seen at a Specialist Hospital in Gusau, Nigeria. 2016. IP: 8.37.232.140.
11. Foumane P, Nkomom G, Mboudou ET et al. Risk factors of clinical birth asphyxia and subsequent newborn death following nuchal cord in a low-resource setting. Open J Obstet Gynecol. 2013;3(642):647.
12. Central Statistical Agency (CSA) [Ethiopia] and ICF. 2016. Ethiopia Demographic and Health Survey 2016. Addis Ababa, Ethiopia, and Rockville, Maryland, USA: CSA and ICF.
13. Fdre M Health Sector Transformation Plan (HSTP) 2015/16-2019/20 (2008-2012 EFY) Draft_V2. Oct2015.
14. WHO Global Health Observatory (GHO) data. Under-five mortality; 2016. Available from: http://www.who.int/gho/child_health/mortality/mortality_under_five_text/en/. Accessed December 28, 2016.
15. Farhana T, Rizvi A, Ariff S, Soofi S, Bhutta ZA. Risk factors associated with birth asphyxia in rural district matiari, pakistan: a case control study. Int J Clin Med. 2014;5:1430–1441. doi:10.4236/ijcm.2014.521181
16. Lee ACC, Darmstadt GL, Mullany LC. Risk Factors for Birth Asphyxia Mortality in a Community-Based Setting in Southern Nepal. MPH Baltimore: Capstone Johns Hopkins School of Public Health; 2007.
17. Bahubali G., et al. Antenatal and intrapartum risk factors for perinatal asphyxia: A case control study. India Curr Pediatr Res. 2013;17(2):119–122. .
18. Getachew B, Yifru B. perinatal mortality and associated risk factors: a case control study. Ethiop J Health Sci. 2012;22(3).
19. Bekana K, Abebaw G, Hardeep RS, Sisay Y. Prevalence and associated factors of neonatal mortality in North Gondar Zone, Northwest Ethiopia. Ethiop J Health Dev. 2012;26(2):66–71.
20. Gurmesa T, Mesganaw F, Alemayehu W. Determinants and causes of neonatal mortality in Jimma Zone, Southwest Ethiopia: a multilevel analysis of prospective follow up study. Plos one. 2014;9(9):e107184.
21. Berhan Y, Berhan A. Perinatal mortality trends in Ethiopia. Ethiop J Health Sci. 2014. doi:10.4314/ejhs.v24i1.4S
22. Martono T. Risk factors for birth asphyxia: folia Medica Indonesiana. 2011;47(4):211–214.
23. S B SS, Nair CC, G N M, Srinivasa S, Manjunath MN. Clinical profile and outcome of perinatal asphyxia in a tertiary care centre. Curr Pediatr Res. 2015;19(1 & 2):9–12.
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
