Back to Journals » Clinical Interventions in Aging » Volume 12
Perspectives of older people living in long-term care facilities and of their family members toward advance care planning discussions: a systematic review and thematic synthesis
Authors Mignani V , Ingravallo F , Mariani E, Chattat R
Received 29 November 2016
Accepted for publication 24 December 2016
Published 3 March 2017 Volume 2017:12 Pages 475—484
DOI https://doi.org/10.2147/CIA.S128937
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Richard Walker
Veronica Mignani,1 Francesca Ingravallo,1 Elena Mariani,2 Rabih Chattat2
1Department of Medical and Surgical Sciences, University of Bologna, Via Irnerio, Bologna, Italy; 2Department of Psychology, University of Bologna, Viale Berti Pichat, Bologna, Italy
Objective: We aimed to search and synthesize qualitative studies exploring the perspectives of older people living in long-term care facilities and of their family members about advance care planning (ACP) discussions.
Methods: The enhancing transparency in reporting the synthesis of qualitative research (ENTREQ) framework was used to guide the review and report its results. PubMed, CINAHL, and PsycINFO were searched for studies published between January 2000 and November 2015. All included studies were assessed for comprehensiveness of reporting, and a thematic synthesis of their results was performed.
Results: The nine included studies differed in terms of qualitative method used, comprehensiveness of reporting, and geographical origin. The thematic synthesis led to the identification of four main themes: 1) plans already made; 2) end-of-life care and decision-making; 3) opinions and attitudes toward ACP; and 4) how, when, about what, and with whom to do ACP.
Conclusion: Despite their willingness to be involved in a shared decision-making process, older residents and their families still have little experience with ACP.
Practical implications: In view of implementing ACP for elders living in long-term care facilities, it would be important to rethink ACP and also to incorporate their nonmedical preferences, according to their own priorities.
Keywords: advance care planning, frail elderly, caregivers, residential facilities, qualitative research
Introduction
Advance care planning (ACP) is defined as an interactive process between a person/family and clinicians that helps to determine the course of a person’s care and appoints a proxy to make decisions in the event of a loss of capacity.1 This process may lead to the formal documentation of preferences through advance directives (including living wills and lasting power of attorney), according to domestic laws. ACP is already supported by legislation and endorsed by professional bodies in Australia, USA,2 and in several European countries, although considerable disparities exist in legislation among European Union member states.3
ACP is increasingly recognized as an:
[…] opportunity to help patients and their families to prepare, in their own terms, for the changes wrought by serious progressive illness and work with them to plan nursing, social and medical care so that it better fits their needs, hopes and aspirations.4
Consistent with this perspective, a recent review found that complex ACP interventions might actually increase both the frequency of out-of-hospital care and compliance with patients’ end-of-life (EOL) wishes and satisfaction with care.5
ACP is particularly relevant in the context of long-term care facilities for older people (including nursing homes and care homes), which are increasingly the place where older people are dying. Results from a randomized controlled trial showed that ACP may improve EOL care of older people and reduce stress, anxiety, and depression of family members.2 On the other hand, a recent review study showed that nursing home staff often failed to recognize actual residents’ EOL preferences.6 In addition, family members, who may be asked to act as surrogate decision-makers, often failed to predict patient’s treatment preferences.7 Lack of ACP discussion may therefore result in inconsistencies between residents’ wishes and the care they receive at EOL.
ACP interventions (ie, Let Me Decide, Let Me Talk, Physician Orders for Life-Sustaining Treatment, Making Advance Care Planning a Priority, Respecting Choices program; advance directive discussions; and self-developed interventions) have been tested in long-term care facilities for older people,5 but an effective and recognized guide to performing ACP in these settings is still lacking. Better understanding the perspectives of both residents and family members may help researchers and health care providers in developing and implementing ACP interventions according to a person-centered approach. In fact, perspectives of elders and their families on ACP may diverge from those of health care professionals and from academic assumptions about ACP.8,9 A qualitative approach enables researchers to investigate individuals’ perspectives, and undertaking a thematic synthesis of qualitative data is a way to fully explore these perspectives,10 providing “a range and depth of meanings, experiences, and perspectives across health-care contexts”.11
This study aimed to systematically search and synthesize qualitative studies exploring the perspectives of older people living in long-term care facilities and of their family members about ACP discussions. This review may be useful in order to identify key issues and areas that need further research. The research questions were the following:
- What are the opinions and attitudes of older people living in long-term care facilities and their family members about ACP discussions?
- Are older people and their family members willing to have ACP discussions?
- When, how, and with whom would older people and their family members like to talk about ACP?
- Which aspects of ACP are important to older people and their family members?
Methods
The ENTREQ (enhancing transparency in reporting the synthesis of qualitative research) framework11 was used to guide this review and report its results.
Search strategy
We searched PubMed, CINAHL, and PsycINFO for studies published between January 2000 and November 2015. Box 1 presents the search strategies used. The reference lists of all included studies were checked to identify further studies of interest.
  | Box 1 Search strategies |
Study selection
Qualitative studies investigating the opinions or attitudes of older people living in long-term care facilities and of their family members about ACP were included.
The following inclusion and exclusion criteria were used:
Inclusion criteria:
- Studies with a study population including older people (age >65 years) living in long-term care facilities (including nursing homes and care homes) and/or their family members.
- Qualitative studies or mixed method studies including a qualitative component.
- Studies whose main aim included exploring participants’ opinions and attitudes about ACP discussions.
- Studies published in English.
Exclusion criteria:
- Studies with a study population including only people younger than 65 years old.
- Studies with a study population including only people living at home or hospitalized.
- Studies addressing only the completion of advance directives (including living wills and lasting power of attorney) but not ACP discussions.
- Studies published in book chapters, dissertations, and abstracts.
- Studies not published in English.
Two of the review authors (FI and VM) independently screened titles and abstracts to identify potentially relevant articles. Two reviewers (FI and VM) obtained and scrutinized the full texts of the selected articles. Any disagreements were resolved by a third reviewer (RC).
Comprehensiveness of reporting
Universally accepted tools for critically appraising qualitative research are still lacking. Therefore, in line with Tong et al,12 we preferred to assess the comprehensiveness of each study’s reporting in order to “provide contextual details to allow readers to assess the trustworthiness and transferability of the study findings to their particular setting”.
We used the consolidated criteria for reporting qualitative research (COREQ), a 32-item checklist designed to promote comprehensive reporting of qualitative studies.13 The COREQ is organized in three domains. The first domain (8 items) concerns research and reflexivity and, more specifically, the personal characteristics of those who carried out the interviews and their relationship with the participants. The second domain (15 items) concerns the study design and its components: theoretical framework, participant selection, setting, and data collection. The third domain (9 items) concerns analysis and findings, specifically data analysis and reporting.
Two of the reviewers (EM and VM) independently assessed each study according to the COREQ. Any disagreement was resolved by a third reviewer (FI). No study was excluded on the basis of this assessment.
Data extraction
The main characteristics of the included studies were extracted independently by two reviewers (FI and VM). For each study, the following were extracted: authors, year of publication, country, stated aims, qualitative methodology adopted, setting, and participants.
Thematic synthesis
A thematic synthesis was performed by two of the reviewers (FI and VM) according to Thomas and Harden14 in three stages: free line-by-line coding of the primary studies’ results; organization of these “free codes” into related areas to develop “descriptive” themes; and development of “analytical” themes. As suggested by Thomas and Harden,14 if a study directly addressed a research question, “going beyond” the contents of the original study may not have been necessary in order to produce a satisfactory synthesis.
Results
Included studies
The database searches returned 729 articles after any duplicates were removed. After screening titles/abstracts, 64 articles were examined in-depth, ultimately leading to the identification of 9 eligible articles15–23 for the systematic review (Figure 1).
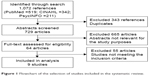  | Figure 1 Flowchart of the selection of studies included in the systematic review. |
The main characteristics of the studies selected for the review are reported in Table 1. The articles that were included in the review were published between 2008 and 2015 and carried out in Australia (1 article),17 Belgium (2 articles),19,21 Norway (2 articles),22,23 UK (2 articles),18,20 and USA (2 articles).15,16 Seven studies used semi-structured interviews,15,18–23 which were associated with focus groups in two cases,22,23 while one study consisted only of focus groups.16 Additionally, one study used semi-structured interviews in the context of a case study.17 Five of the included studies were performed in long-term care facilities,17,18,20,22,23 while the remaining four15,16,19,21 recruited participants from other settings as well (ie, community center, acute geriatric ward, medical oncology ward, palliative care unit, and home services for older people). In two studies,17,20 a complex ACP intervention was carried out. Of the included studies, two addressed the older people perspectives;16,19 three addressed the family members’ perspectives;15,18,21 and four addressed both perspectives.17,20,22,23 Overall, the included studies involved 135 elders and 133 family members or friends. Regarding the elders’ age range, three studies referred to “older people” without reporting their age range,17,18,20 while two studies also included people younger than 65 years old.15,16
Comprehensiveness of reporting
The comprehensiveness of reporting (Table 2) varied across the studies, with the number of reported details ranging between 11 and 32 of the 32 items required by the COREQ. Five out of nine studies provided details on at least 20 of the 32 items. All nine studies included respondents’ quotations in their results; seven of them also included an interview guide.
  | Table 2 Consolidated criteria for reporting qualitative research (COREQ) items reported by the nine articles included in the review |
Thematic synthesis
The thematic synthesis led to the identification of four main themes: 1) plans already made; 2) EOL care and decision-making; 3) opinions and attitudes toward ACP; and 4) how, when, about what, and with whom to carry out ACP.
Plans already made
Several studies found that older residents had primarily planned the practical issues related to their death (ie, funeral and financial issues).15,16,19,23 Making arrangements for the period following their death was also frequent among elders who did not want to talk about their preferences for EOL care,19 showing that they were generally well prepared for their death but not necessarily for the dying process.16
Most elders had never talked about their preferences for EOL care with their family or residential staff.16,22,23 Some of the residents remarked that communication was limited due to discomfort among their family, friends, and providers;16 or due to their own introverted personalities;23 or due to the staff’s lack of time.22 However, even if they had not discussed or documented them, some elders assumed that their EOL care preferences were known.16,22,23 In one study, numerous relatives said that they had a clear sense of their loved one’s preferences for life-prolonging treatment even if they had not talked with their loved one about these issues.23
A few residents had discussed their wishes for EOL care (including details regarding the place of care) with both their family members and/or physician.15,19,22 The documentation of preferences through an advance directive was often encouraged by family members,19 lawyers or financial planners,15,16 and, less frequently, by health care professionals.15 In one study, some residents reported concerns that their documented EOL care preferences would not be followed for some reason.17 Overall, even though EOL care and ACP are regulated by law in Belgium,19 many elders and family members still lacked accurate knowledge about ACP and advance directives.19,21 In one study from the USA,15 the majority of family members of older residents with advanced stages of dementia reported that their loved ones had some form of written advance directive; while in another US study,20 only 20% of elders reported having had prior conversations about ACP, and only 15% reported having had a prior conversation with their primary care provider.
EOL care and decision-making
Many studies highlighted that the attitudes of older residents toward decision-making varied. Many residents trusted the staff or their family members to make decisions on their behalf and in their best interest19,20,22,23 and felt comfortable just being informed.22 Other elders wanted to participate in the decision-making process and leave the final decisions to the staff.23 Very few elders wanted to be responsible for ACP and make their own decisions.23 A few elders believed that they were not entitled to do ACP or did not have the ability to do so even though they were not cognitively impaired,19 or they believed that medical decisions had to be made by the physician.22 On the other hand, when they were offered the opportunity to express their thoughts, many residents with dementia/cognitive impairment were able to consistently express their preferences.19
Several studies reported that family members’ attitudes toward EOL care decision-making also varied and that they were influenced by both their trust in health care providers and family dynamics.21 Most family members preferred shared decision-making with the staff,22,23 while others found it acceptable for the staff to make the decisions as long as the family members were informed.23 Some relatives appeared to be used to taking over decision-making and organizing most of the residents’ matters,22 while others felt burdened by decision-making,21,22 especially when they did not know the residents’ wishes.22
Opinions and attitudes toward ACP
Both elders and family members had generally positive opinions about ACP.15–20,23 In the two studies in which a complex ACP intervention was performed,17,20 both residents and relatives expressed satisfaction with the process: ACP conversations provided an opportunity for residents to express themselves and for family members to hear what their loved ones desired.17,20 In a study by Jeong et al,17 both residents and family members “felt strongly that ‘the essence of being’ – who the resident was and how s/he has lived life – was enhanced through the ACP process, becoming one of the important factors justifying participation in ACP”.
The majority of older residents were willing and comfortable talking about EOL care.16,19,20 However, some elders were reluctant to talk about EOL situations and preferences for care18,19 or did not want to make care plans, even in cases where their family members had a positive opinion about the benefits of ACP.21 Other elders did not see the necessity of such discussions 22,23 or were not concerned about their future, stating that they took life “day by day”.20,22 Some studies found that the attitudes of elders toward ACP were mainly prompted and/or influenced by the following: the need to “put their affairs in order”;15 medical, living situation, or financial issue of a friends or a family member;15 previous experiences with death and dying of a loved one;19 and the wish to relieve family members from the burden of care, including decision-making.16,19 In the study by Piers et al,19 elders also reported the following motivations for proceeding with ACP: limited trust that family members would respect their wishes; lack of surrogate decision-makers; wish to exert control over their EOL; and avoidance of specific situations inducing fear (eg, underwent surgery). On the other hand, some elders and family members reported that they did not proceed with ACP due to trust that physicians would respect the patient’s wishes or would do the “right thing” related to the patient’s EOL care.19,21
According to family members, the main barriers to ACP were dementia/lack of cognitive capacity,15,18 reluctance of some residents to discuss EOL issues,18 resident’s personality,15 and avoidance of the discussion altogether.15,21 In fact, while ACP could be experienced as a form of release for some family members,17,22 for others initiating conversations could be uncomfortable or burdensome for several reasons.17,21–23 Some family members reported experiencing ambivalence since they considered the decision-making process to be representative of either “letting go” or “letting (their loved one) suffer”.17 Other family members wanted to spare their loved one from dealing with this emotional issue or feared that their loved one would react with blame, believing that the family members were waiting for him/her to die.21 Interestingly, the fear of future feelings of regret may have been both a barrier and a facilitator to family involvement in ACP.21 Family members of residents with dementia reported that barriers to ACP included the following: not recognizing the importance of ACP until their relative’s cognitive impairment prevented them from having the discussion; never having considered the need to have ACP conversations; and the residents’ denial of their dementia diagnosis.15
How, when, about what, and with whom to do ACP
Some elders and family members believed that ACP would be initiated gradually15,18 and sensitively18 in the context of routine care.16 They also believed that ACP would require more time and attentiveness from health care professionals than was typical during a visit.16 Many elders and family members stressed that ACP discussions should take place at “the right time”, but opinions about “the right time” varied. Some stated that discussions should start early (ie, before the onset of serious health problems or cognitive impairment)16,18 or “as soon as possible”,23 while others wanted to postpone these types of conversations until the patient’s health deteriorated.23 Regarding ACP conversations in long-term care facilities, some family members believed that it should take place early,18 while others believed that it would be somewhat overwhelming to have those conversations so soon after admission20 since it would be emotionally difficult.23
Health care professionals who knew the elder well were considered the ideal group of people to initiate ACP,16,22 and family members would appreciate if the staff took the initiative23 and organize regular meetings.22 However, only a few studies cited physicians, nurses, and social workers as effective ACP initiators or facilitators.15,16
Regarding wishes for EOL care, residents stressed the importance of both quality of life20 and a natural death, meaning that they did not wish for their lives to be prolonged for no reason.22,23 Elders also mentioned their wishes for relief from pain and suffering through pain medications,19,22,23 dying with dignity, and not being alone when the time came.22 When asked to choose between different treatment options, older residents were mainly interested in subsequent functional status.22 In one study, EOL care preferences were reported to be mostly influenced by the participants’ experiences with death and dying and by their personal fears.19 Relatives agreed with residents about the importance of pain relief in EOL care.22
Discussion
This study aimed to review and synthesize qualitative findings about perspectives of older residents living in long-term care facilities and of their family members about ACP discussions. One of the study’s main findings was the paucity of studies specifically involving these populations. It is likely that we failed to identify some relevant studies despite conducting a systematic search in the databases and a manual screening of the studies’ reference lists. Another limitation of the review stems from the population involved in the included studies, which was often mixed (ie, elders/families in long-term care facilities and elders/families from other care settings). In addition, the included studies were heterogeneous with regard to the qualitative method used, the comprehensiveness of reporting, and the geographical origin. Regarding the latter, seven out of nine studies were carried out in countries in which ACP is supported by legislation (ie, Australia, Belgium, UK, and USA); in particular, the US legislation requires all individuals admitted to a care home are offered ACP.24 The remaining two studies were performed in Norway, where ACP is not standard and occurs infrequently in nursing homes.22,23 Finally, since the review results were based on the researchers’ interpretation of the included studies,10 there may be bias related to the reviewers’ background. We trust that this potential bias has been mitigated by the multidisciplinary nature of the research group, which encompassed nursing, bioethics, and psychogeriatric experts.
All these factors prevent any generalizability and limit the transferability of the review findings to the global population of older people living in long-term care settings. On the other hand, the review was conducted according to the ENTREQ framework; to our knowledge, it is the first of its kind to attempt to systematically review existing evidence in order to answer to the research questions. The studies included in the review were published in the last 8 years, outlining the increasing interest in the review topic. Additionally, the studies’ heterogeneity might strengthen the relevance of findings that were consistently reported across the studies, which may have important practical implications.
First, the majority of the studies found that most older residents had already planned some practical and specific aspects unrelated to their future care. On the other hand, both residents and family members had scarce or incomplete knowledge about ACP and advance directives, even in countries in which ACP is well recognized by law. We did not know whether some residents were not offered ACP or they refused the opportunity to discuss it. Of course, any preference to not be involved in ACP needed to be respected4 in light of the fact that one of the ACP prerequisites is the voluntary nature of participating in the process.25 However, beyond the lack of involvement in any ACP conversations, we found a concerning lack of communication between elders and both relatives and health care professionals about the elders’ wishes, which may result in a lack of alignment between residents’ actual wishes and the care provided to them.26
On the other hand, a finding consistent across the studies was that older people living in long-term care facilities had generally positive attitudes toward ACP, and they were less concerned about talking about death and dying than expected. This result was in line with findings from a previous review showing that most elders appreciated discussions about EOL care, while a minority did not welcome them.27 In fact, as discussed by Fried et al,28 elders were in different stages of readiness to participate in ACP, and they experienced highly varied barriers, as well as facilitators, to ACP. In particular, we found that residents’ attitudes toward ACP might have been diversely influenced by their trust in family members and clinicians and previous life experiences. This latter factor, as part of a person’s personality and biography, made his/her preferences unique and personal, which justified the need of elders and their families to discuss ACP with health care professionals who know them very well. In fact, both residents and family members stressed that such a complex process required time, continuity, and stable relationships. Therefore, it is important that health care professionals assess the elder’s readiness to participate in ACP and adapt their approach to the person,29,30 focusing on the individual’s decision-making process in order to provide the best individualized care possible.31 It is worth noting the finding that when properly approached, many residents with cognitive impairments were able to express their preferences consistently. This finding was consistent with other studies32,33 and highlighted the need to not exclude these residents a priori from ACP.
Additionally, residents’ relatives had generally positive attitudes toward ACP and expressed satisfaction with the process. This result was in line with those of a randomized controlled trial involving inpatient elders, which found that ACP significantly reduced symptoms of posttraumatic stress, anxiety, and depression in family members, preparing them for the death of a loved one.2 However, some relatives may have found it difficult or burdensome to initiate ACP conversations but appreciated their value as a guide in order to fulfill the wishes of their loved ones. These findings, highlighting family ambivalence toward ACP conversations, may provide a new perspective on the results from several studies that identified relatives’ unwillingness to have ACP discussions as one of the main barriers to ACP.27
In addition, studies included in this review showed consistently that even if family members’ positions about decision-making varied widely, most of them preferred to take part in shared decision-making. Shared decision-making gave them an opportunity to be guided and advised by health care professionals and thereby feel relieved from the burden of decision-making. On the other hand, this review disclosed that this need for advice and guidance on EOL issues is often unmet. In fact, health care professionals were cited as effective ACP initiators or facilitators in only a few cases. The lack of professionals’ drive toward ACP conversations has been consistently reported by elders in other studies.9,29,34,35
Interestingly, most residents believed it was important to plan for practical issues not related to treatment and care, and they seemed uninterested in having control over their lives or making decisions about medical treatments, citing what they believed to be important outcomes (ie, pain relief, natural death, and preserved quality of life and dignity at EOL). Along with previous data showing that elders focused on outcomes instead of treatments when making important decisions about their future health,36,37 this finding suggests that it would be relevant to focus on these aspects in ACP discussions with older residents. In fact, beyond the request for pain relief, this review found scarce insight into what medical options residents and family members considered important to include in ACP, and wide variability was found regarding the “right time” for ACP. These findings confirm the need for further studies and guidance regarding the timing and style of introducing ACP to patients and their families,38 with the consideration that choosing the right moment and appropriate wording to engage patients in ACP may have a profound impact on the value and effects of ACP.4
Conclusion
Despite their willingness to be involved in a shared decision-making process regarding EOL care, older residents of long-term care settings across the globe and their family members still know and have little experience with ACP. Further, methodologically rigorous studies specifically addressing older people living in long-term care facilities in different cultural contexts are needed in order to explore and understand their perspectives and authentically provide person-centered EOL care.
Practical implications
This review suggests that barriers to ACP for older people living in long-term care facilities are more related to health care professionals’ willingness to initiate ACP conversations than to patients’ and family members’ willingness to be involved in such a process. In fact, the results of this review proposed that residents and their families rely on health care professionals’ expertise and judgment and desire their involvement in EOL care decision-making. This finding was consistent with previous studies and highlighted the urgent need to enhance health care professionals’ knowledge, skills, and comfort in ACP conversations. Health care professionals who know an elder well were considered the ideal group of people to initiate ACP,2,6,9,29 and most elders and their families expect health care providers to initiate and anticipate their needs concerning EOL issues.6
In addition, the findings of this review indicated that elders and their families desired a personalized approach by health care professionals, within a relationship based on trust, respect, and sensitivity. Regarding the “right time” to perform ACP, further studies are needed in order to develop appropriate guidance on approaching both residents and their family members.
Finally, this review showed that, at least for the current generation of older people living in long-term care settings, planning for nonmedical issues was very important, suggesting the need to rethink ACP for this population and also to incorporate nonmedical preferences.
Acknowledgment
This research was made possible with funding from Fondazione del Monte di Bologna e Ravenna.
Disclosure
The authors report no conflicts of interest in this work.
References
U.S. Department of Health and Human Services, Assistant Secretary for Planning and Evaluation, Office of Disability, Aging and Long-Term Care Policy. Advance directives and advance care planning: report to congress, 2008. Available from: https://aspe.hhs.gov/pdf-report/advance-directives-and-advance-care-planning-report-congress. Accessed September 12, 2016. | ||
Detering KM, Hancock AD, Reade MC, Silvester W. The impact of advance care planning on end of life care in elderly patients: randomised controlled trial. BMJ. 2010;23;340:c1345. | ||
Committee of Ministers of the Council of Europe. Recommendation CM/Rec (2009)11 of the Committee of Ministers to member states on principles concerning continuing powers of attorney and advance directives for incapacity, 2009. Available from: https://www.coe.int/t/dghl/standardsetting/cdcj/CDCJ%20Recommendations/CM_Rec(2009)11E_Principles%20on%20powers%20of%20attorney.pdf. Accessed September 12, 2016. | ||
Rietjens J, Korfage I, van der Heide A. Advance care planning: not a panacea. Palliat Med. 2016;30(5):421–422. | ||
Brinkman-Stoppelenburg A, Rietjens JA, van der Heide A. The effects of advance care planning on end-of-life care: a systematic review. Palliat Med. 2014;28(8):1000–1025. | ||
Fosse A, Schaufel MA, Ruths S, Malterud K. End-of-life expectations and experiences among nursing home patients and their relatives – a synthesis of qualitative studies. Patient Educ Couns. 2014;97(1):3–9. | ||
Shalowitz DI, Garrett-Mayer E, Wendler D. The accuracy of surrogate decision makers: a systematic review. Arch Intern Med. 2006;13;166(5):493–497. | ||
Singer PA, Martin DK, Lavery JV, Thiel EC, Kelner M, Mendelssohn DC. Reconceptualizing advance care planning from the patient’s perspective. Arch Intern Med. 1998;158:879–884. | ||
Seymour J, Gott M, Bellamy G, Ahmedzai SH, Clark D. Planning for the end of life: the views of older people about advance care statements. Soc Sci Med. 2004;59(1):57–68. | ||
Woodman C, Baillie J, Sivell S. The preferences and perspectives of family caregivers towards place of care for their relatives at the end-of-life. A systematic review and thematic synthesis of the qualitative evidence. BMJ Support Palliat Care. 2015;6(4):418–429. | ||
Tong A, Flemming K, McInnes E, Oliver S, Craig J. Enhancing transparency in reporting the synthesis of qualitative research: ENTREQ. BMC Med Res Methodol. 2012;27;12:181. | ||
Tong A, Morton R, Howard K, Oliver S, Craig J. Adolescent experiences following organ transplantation: a systematic review of qualitative studies. J Pediatr. 2009;155(4):542–549. | ||
Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care. 2007;19(6):349–357. | ||
Thomas J, Harden A. Methods for the thematic synthesis of qualitative research in systematic reviews. BMC Med Res Methodol. 2008;10;8:45. | ||
Hirschman KB, Kapo JM, Karlawish JH. Identifying the factors that facilitate or hinder advance planning by persons with dementia. Alzheimer Dis Assoc Disord. 2008;22(3):293–298. | ||
Malcomson H, Bisbee S. Perspectives of healthy elders on advance care planning. J Am Acad Nurse Pract. 2009;21(1):18–23. | ||
Jeong SY, Higgins I, McMillan M. Experiences with advance care planning: older people and family members’ perspective. Int J Older People Nurs. 2011;6(3):176–186. | ||
Stewart F, Goddard C, Schiff R, Hall S. Advanced care planning in care homes for older people: a qualitative study of the views of care staff and families. Age Ageing. 2011;40(3):330–335. | ||
Piers RD, van Eechoud IJ, Van Camp S, et al. Advance care planning in terminally ill and frail older persons. Patient Educ Couns. 2013;90(3):323–329. | ||
Stone L, Kinley J, Hockley J. Advance care planning in care homes: the experience of staff, residents, and family members. Int J Palliat Nurs. 2013;19(11):550–557. | ||
van Eechoud IJ, Piers RD, Van Camp S, et al. Perspectives of family members on planning end-of-life care for terminally ill and frail older people. J Pain Symptom Manage. 2014;47(5):876–886. | ||
Bollig G, Gjengedal E, Rosland JH. They know!-do they? A qualitative study of residents and relatives views on advance care planning, end-of-life care, and decision-making in nursing homes. Palliat Med. 2016;30(5):456–470. | ||
Gjerberg E, Lillemoen L, Førde R, Pedersen R. End-of-life care communications and shared decision-making in Norwegian nursing homes – experiences and perspectives of patients and relatives. BMC Geriatr. 2015;15:103. | ||
Royal College of Physicians, National Council for Palliative Care, British Society of Rehabilitation Medicine, British Geriatrics Society, Alzheimer’s Society, Royal College of Nursing, Royal College of Psychiatrists, Help the Aged, Royal College of General Practitioners. Advance care planning. Concise Guidance to Good Practice series, No 12. London: RCP, 2009. | ||
Mullick A, Martin J, Sallnow L. An introduction to advance care planning in practice. BMJ. 2013;347:f6064. | ||
Morrison RS, Chichin E, Carter J, Burack O, Lantz M, Meier DE. The effect of a social work intervention to enhance advance care planning documentation in the nursing home. J Am Geriatr Soc. 2005;53(2):290–294. | ||
Sharp T, Moran E, Kuhn I, Barclay S. Do the elderly have a voice? Advance care planning discussions with frail and older individuals: a systematic literature review and narrative synthesis. Br J Gen Pract. 2013;63(615):e657–e668. | ||
Fried TR, van Doorn C, O’Leary JR, Tinetti ME, Drickamer MA. Older person’s preferences for home vs hospital care in the treatment of acute illness. Arch Intern Med. 2000;160(10):1501–1506. | ||
Simon J, Porterfield P, Bouchal SR, Heyland D. ‘Not yet’ and ‘Just ask’: barriers and facilitators to advance care planning – a qualitative descriptive study of the perspectives of seriously ill, older patients and their families. BMJ Support Palliat Care. 2015;5(1):54–62. | ||
Walczak A, Butow PN, Davidson PM, et al. Patient perspectives regarding communication about prognosis and end-of-life issues: how can it be optimised? Patient Educ Couns. 2013;90(3):307–314. | ||
Lambert HC, McColl MA, Gilbert J, Wong J, Murray G, Shortt SE. Factors affecting long-term-care residents’ decision-making processes as they formulate advance directives. Gerontologist. 2005;45(5):626–633. | ||
Whitlatch CJ. Assessing the personal preferences of persons with dementia. In: Lichtenberg PA, editor. Handbook of Assessment in Clinical Gerontology. London: Academic Press; 2010:557–578. | ||
Goodman C, Amador S, Elmore N, Machen I, Mathie E. Preferences and priorities for ongoing and end-of-life care: a qualitative study of older people with dementia resident in care homes. Int J Nurs Stud. 2013;50(12):1639–1647. | ||
Ott BB. Views of African American nursing home residents about living wills. Geriatr Nurs. 2008;29(2):117–1124. | ||
Samsi K, Manthorpe J. ‘I live for today’: a qualitative study investigating older people’s attitudes to advance planning. Health Soc Care Community. 2011;19(1):52–59. | ||
Rosenfeld KE, Wenger NS, Kagawa-Singer M. End-of-life decision making: a qualitative study of elderly individuals. J Gen Intern Med. 2000;15(9):620–625. | ||
McMahan RD, Knight SJ, Fried TR, Sudore RL. Advance care planning beyond advance directives: perspectives from patients and surrogates. J Pain Symptom Manage. 2013;46(3):355–365. | ||
Murray L, Butow PN, White K, Kiernan MC, D’Abrew N, Herz H. Advance care planning in motor neuron disease: a qualitative study of caregiver perspectives. Palliat Med. 2016;30(5):471–478. |
 © 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

