Back to Journals » Clinical Pharmacology: Advances and Applications » Volume 13
Penetration of Flurbiprofen from a Locally Applied Sore Throat Lozenge and Spray into Cadaveric Human Pharynx Tissue: A Novel ex vivo Model and Microautoradiography Method
Authors Turner R, Wevrett SR, Edmunds S , Brown MB, Kulasekaran A, Adegoke O, Farrah J
Received 29 September 2020
Accepted for publication 1 December 2020
Published 19 January 2021 Volume 2021:13 Pages 13—20
DOI https://doi.org/10.2147/CPAA.S284433
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Arthur E. Frankel
Rob Turner,1 Sean Robert Wevrett,1 Suzanne Edmunds,1 Marc Brown,1 Anuradha Kulasekaran,2 Oluwajoba Adegoke,2 John Farrah2
1MedPharm Ltd, Guildford, UK; 2Reckitt Benckiser Healthcare International Ltd., Slough, Berkshire, UK
Correspondence: Oluwajoba Adegoke
Reckitt Benckiser Healthcare International Ltd, Slough, Berkshire, UK
Tel +44 1482 582134
Email [email protected]
Objective: Flurbiprofen 8.75 mg lozenge and spray are used for symptomatic relief of sore throat, with a rapid onset of analgesia suggesting a localized mechanism of action. Building on previous studies, this investigation aimed to use microautoradiography to visualize the depth penetration of radiolabeled flurbiprofen into human pharynx tissue using an ex vivo model. Quantification of flurbiprofen in the tissue was performed to provide a quantitative representation of flurbiprofen distribution through the tissue.
Methods: Cadaveric human pharynx tissue was mounted between the donor and receiver compartments of a Franz diffusion cell. After that 8.75 mg spray and dissolved lozenge formulations, containing radiolabeled flurbiprofen, were added to the donor compartment of a Franz diffusion cell. After incubation for one hour, the pharynx tissue was removed, processed, and sectioned both horizontally and vertically. The sections were placed within an imaging cassette to determine the penetration of radiolabeled flurbiprofen visually, before being solubilized to quantify the amount of flurbiprofen present in each section.
Results: In the horizontally sectioned samples, flurbiprofen was present in the top layers of all replicates and decreased in intensity throughout the tissue. Of the applied dose, 48.0– 99.9% of flurbiprofen was detected in the top one-third of the pharynx tissue, closest to the dosing site, and 0– 14.8% of flurbiprofen was detected within the deepest third of pharynx tissue, furthest from the dosing site. In the vertically sectioned tissue samples, radiolabeled flurbiprofen was found at a high intensity at the dosing site and reduced in intensity throughout the thickness of the tissue. Lateral penetration of flurbiprofen was also seen in tissue dosed with the spray.
Conclusion: Our findings demonstrate that lozenge and spray formulations of flurbiprofen can penetrate throughout the layers of cadaveric human pharynx tissue in an ex vivo model, as visualized by microautoradiography.
Keywords: flurbiprofen, Franz diffusion cell, microautoradiography, pharynx
Introduction
Acute upper respiratory tract infections (URTIs) are a common cause for presentation to primary care services1 and the majority of the population will experience a URTI annually.2
A common symptom of URTIs is sore throat (pharyngitis),2 resulting in pain and discomfort in the pharynx due to local inflammation.3,4 Most cases of sore throat caused by infection are viral in origin, with only a small proportion resulting from a bacterial infection.5,6 Pharyngitis may also be attributable to a number of other causes, including medication or concomitant illness, snoring, vocal straining or tracheal intubation, chemical irritation, and environmental factors.7 Pharyngitis resulting from URTIs is typically a self-limiting condition and most commonly resolves within 7 days.5 However, the pain, swelling, and discomfort caused by the condition are unpleasant symptoms and can have a negative impact on the quality of life.8,9 In viral pharyngitis, antibiotics are ineffective,10–12 yet where used, they may contribute towards antibiotic resistance.13,14 Thus, symptomatic relief of pain from inflammation within the pharynx is the main objective of most treatments for pharyngitis.13
Locally acting non-steroidal anti-inflammatory drugs (NSAIDs), including flurbiprofen, have been demonstrated as very effective treatments for sore throat.15,16 A potential additional benefit of formulations that are applied directly to the mucous membranes of the throat (such as lozenges, gargles, and throat sprays) is that they are known to deliver drugs locally to alleviate symptoms of pharyngitis, such as sore throat, difficulty swallowing, and swollen throat, more rapidly than systemic oral analgesia.13,16–20 The rapid relief of symptoms is via an anti-inflammatory mechanism resulting in analgesic action.15 This effect is considered to be due to the local absorption which has been previously demonstrated through the buccal mucosa and ex vivo cadaveric human pharynx tissue.21–24
This research builds on a previous study, which involved the development of a method to quantify permeation and penetration of flurbiprofen through the human pharynx tissue in an ex vivo model using a Franz diffusion cell method,25 followed by quantification of the permeation and penetration of flurbiprofen in the human pharynx tissue,23,24 and development of a model to replicate absorption from lozenge and throat spray using a Franz diffusion cell.
The distribution of flurbiprofen within pharyngeal tissue, and the mechanism of local relief via lateral movement of flurbiprofen through the pharynx, are not yet fully understood. The aim of this study was to quantify and visualize the depth of flurbiprofen penetration, delivered via 8.75 mg lozenge and throat spray formulations, within human pharyngeal tissue using microautoradiography.
Materials and Methods
This investigation was conducted by MedPharm Ltd. (Guildford, UK) in accordance with the International Conference on Harmonisation (ICH) Pharmaceutical Quality System Q10, 2008.26
Test Formulations
The test formulations manufactured and supplied by Reckitt Benckiser were Strefen flurbiprofen 8.75 mg honey and lemon lozenge (manufactured in Nottingham, UK; also known as Strepsils Intensive, Strepfen Intensive, Strepsils Max Pro, Strefen Intensive, Benactiv Gola, Dobendan Direkt, and Graneodin F), and Benactivdol Gola flurbiprofen 8.75 mg/dose throat spray (manufactured in Bangplee, Thailand; also known as Strepsils Intensive, Strepfen Intensive, Benactiv Gola, and Dobendan Direkt).
Franz Cell Model and Radiolabeling
To analyze the penetration of flurbiprofen into human pharyngeal tissue, radiolabeled flurbiprofen was added to both the 8.75 mg lozenge and throat spray formulations. The radiolabeled flurbiprofen was produced by American Radiolabeled Chemicals, Inc. The target concentration of flurbiprofen in the dissolved lozenge sample was determined in a previous experiment to be 1.17 mg/mL. A Franz diffusion cell model27 was used to mimic the physiological conditions of in situ human pharynx tissue.
Ethically sourced cadaveric human pharynx tissue (consisting of the epithelial layer, basement membrane, and lamina propria) was supplied by Ethical Tissue (Research Ethics Committee reference 220367) and mounted between the donor and receiver compartments of a Franz diffusion cell (Figure 1) with an average surface area of 0.07 cm2. Radiolabeled flurbiprofen with a specific activity of 20 μCi/mL, in throat spray and lozenge formulations, was applied to the human pharynx tissue in solution form. The specific activity of 20 µCi/mL was selected based on a preliminary experiment that showed it produced notable variation in the intensity of the signal observed throughout the tissue.
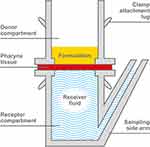 |
Figure 1 Schematic representation of the Franz cell. |
The quantities of flurbiprofen applied represented the anticipated amount that could come into contact with the pharynx tissue based on posology, format, and tissue surface area.28,29 The total amount of flurbiprofen applied was 195.4 μg and 17.6 μg for the spray and lozenge formulations, respectively. The volume of the spray formulation applied was calculated to replicate three spray actuations (one dose); however, due to the safety concerns surrounding the inclusion of radiolabeled flurbiprofen in the spray formulation for this study, the solution was applied using a pipette rather than from the spray bottle. A dosage volume of 12 μL of radiolabeled flurbiprofen throat spray was used to account for the relative size of the sections of pharyngeal tissue (0.07 cm2) compared to the average size of the pharynx in vivo. The lozenge solution was designed to represent the typical dose delivered from an 8.75 mg lozenge, relative to the size of the pharyngeal tissue used and the average rate of saliva production. A solution of lozenge was dissolved in phosphate-buffered saline with a flurbiprofen (radiolabeled and unlabeled) concentration of 1.17 mg/mL and a specific activity of 20 μCi/mL was made up; 15 μL of the solution was used.
Following application, the Franz diffusion cells were incubated for 1 hour at 37°C in a water bath. This incubation time was selected as representative of in vivo conditions, based on a study demonstrating that spray and lozenge formulations provide a prolonged delivery of up to 2 hours.30
Pharynx Tissue Processing and Imaging and Quantification of Radiolabeled Flurbiprofen
The pharynx tissue was removed from the Franz cell, then placed in the required orientation for cutting. One of the initial six lozenge samples was discarded due to Franz cell leakage during the incubation period and this replicate was not included in the final analysis. Thus, only five samples were analysed for the lozenge. Tissue samples were then covered with optimal cutting temperature embedding compound, flash frozen, and stored at −70°C prior to sectioning. Samples were covered with additional optimal cutting temperature embedding compound at room temperature and sectioned vertically and horizontally in 30 μm sections (Figure 2A and B).
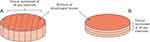 |
Figure 2 Sectioning of the human pharynx tissue vertically (A) and sectioning of the human pharynx tissue horizontally (B). |
Each section of pharynx tissue containing radiolabeled flurbiprofen was placed inside an imaging cassette and exposed to a freshly conditioned phosphor screen. The horizontal and vertical sections were exposed for 2 hours and 1 hour per replicate, respectively, then scanned using a TyphoonTM imager. Based on a preliminary feasibility study using a higher concentration of radiolabeled flurbiprofen (200 μCi/mL), the first sample of pharynx tissue of the horizontal sections was assessed at exposure times of 2, 3, and 4 hours. Based on this, 2 hours was selected as the optimal exposure duration and was used subsequently. For the vertical sections, the first sample of pharynx tissue was assessed at an exposure time of 1 hour. As the images produced showed sufficient intensity of the radiolabeled flurbiprofen, no further exposure times were tested.
For each sample, the recovery of flurbiprofen as a proportion of the amount applied was calculated, based on the amount of flurbiprofen detected in each section, and the total flurbiprofen applied to the tissue (6 replicates for the spray formulation; 5 replicates for the lozenge formulation).
Results
Horizontally Sectioned Tissue
Radiolabeled flurbiprofen was detected in the top one-third layer of pharyngeal tissue for all replicates. The radiolabeled flurbiprofen was at the highest intensity at the surface and reduced in intensity throughout the thickness of the tissue (Figure 3). The percentage of applied radiolabeled flurbiprofen absorbed in the top one-third of the tissue varied from 87.7–98.7% for the lozenge formulation and 48.0–99.9% for the spray formulation (Figure 3).
The percentage of applied radiolabeled flurbiprofen absorbed in the deepest third of tissue varied from 0.0–2.0% for the lozenge formulation and from 0.0–14.8% for the spray formulation. The thickness of pharynx tissue samples, total amount of flurbiprofen applied and total amount of flurbiprofen detected within the tissue are presented in Table 1 for each replicate. The percentage of the applied dose recovered from the tissue for both flurbiprofen lozenge and spray is displayed in Figure 4. The percentage of applied flurbiprofen recovered within the tissue was relatively low (9.0–49.2%) as full mass balance was not performed; therefore, the residual flurbiprofen present in the receiver fluid and on the Franz cell apparatus was not quantified.
 |
Table 1 Tissue Thickness and Percentage of Applied Dose of Flurbiprofen Recovered within Pharynx Tissue |
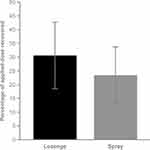 |
Figure 4 Mean percentage of applied dose of radiolabeled flurbiprofen recovered from the pharynx tissue. Error bars represent standard deviation. |
Vertically Sectioned Tissue
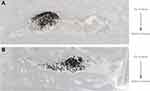
The sections showing the highest intensity of radioactivity were selected and manually overlaid with images of the tissue sections to show the distribution of radioactivity within the tissue (Figure 5A and B). Radiolabeled flurbiprofen was found at the highest intensity at the dosing site and reduced in intensity throughout the tissue (Figure 5A and B). For tissue dosed with the spray, lateral penetration was also observed, while no lateral diffusion was observed in tissue dosed with the lozenge solution (Figure 5A and B).
Discussion
This study reaffirmed the findings of our previous study, which demonstrated that flurbiprofen from a throat spray solution and a dosing solution prepared from a lozenge formulation is capable of penetrating the pharynx tissue,24 while allowing visualization of radiolabeled flurbiprofen penetration across all layers of the pharynx tissue. Radiolabeled flurbiprofen was detected in the deepest sections of the human cadaveric pharynx tissue. In the samples of pharynx tissue that were vertically sectioned, microautoradiography showed the highest intensity of radiolabeled flurbiprofen at the site of dosing, with the intensity reducing throughout the more distal tissue.
It is not currently plausible to investigate the penetration of flurbiprofen into human pharynx tissue in vivo and, as such, alternative methods of investigation must be used. The Franz diffusion cell method has been used previously to mimic physiological and anatomical conditions to allow the study of diffusion through various tissues,31,32 including human pharynx tissue.23,25 This ex vivo model was developed to mimic the clinical scenario as closely as possible,25 using full-thickness cadaveric pharynx tissue, which provides a close match to the physiological and anatomical conditions of the human pharynx. Synthetic and animal models have been used as substitutes for human tissues in previous studies,31–33 and although these are accessible models, they do not accurately reflect the clinical environment. The model used does have limitations in this respect: the lack of a blood supply to the tissue may alter the penetration and diffusion of flurbiprofen through the tissues; the absence of a mucosal barrier may influence the dynamics of drug penetration into the tissues, and the fact that there was no active inflammatory process means that the clinical setting was not entirely reproduced. Additionally, due to the use of radiolabeled flurbiprofen, the spray dose was applied to the tissue samples using a pipette rather than the spray bottle. This method of application differs from real-world administration of the spray and may have influenced the results observed. Our data should therefore only be considered with these limitations in mind.
In the present study, lateral diffusion of radiolabeled flurbiprofen within pharynx tissue was not observed in the vertically sectioned tissue following dosing with lozenge solution. Evidence of lateral diffusion has been suggested previously in unpublished experiments performed within our laboratory. Further investigation is required to explore the reasons for this disparity, with possible reasons including inter-donor variability or uneven diffusion through the pharynx tissues that was not captured by the present experimental protocol.
As described above, and notable in Figure 3, there was a high degree of variability in penetration observed between replicates. In fact, several replicates contained very little, or no, detectable radiolabeled flurbiprofen within the deepest sections of tissue. The reasons for this discrepancy also require further investigation. The pharynx tissue samples were of variable thickness which may have had some influence on the penetration; however, there was not a clear relationship between thickness of the pharynx tissue sample and depth of penetration of flurbiprofen. Inter-donor variability may have had an influence with respect to replicate 6 from the flurbiprofen 8.75 mg spray dose experiment: 99.9% of the detected radiolabeled flurbiprofen was within the most superficial third of tissue, the lowest penetration level for the spray formulation; notably, replicate 6 was from a different donor to the other spray replicates, which were all from the same donor. All the lozenge solution replicates were from one donor.
Our model involved incubation of flurbiprofen for one hour post-application to human pharynx tissue in the donor compartment of the Franz cell. While this was designed to reflect exposure in an in vivo system, this is longer than an application of flurbiprofen would usually be expected to remain in contact with pharynx tissue in a clinical setting. Although clinical studies have demonstrated flurbiprofen is detectable in the mouth and oropharyngeal region at 2 hours post-dose in vivo,30 the concentration of the dose exposed to the pharynx over time follows a different relationship compared to the relatively constant delivery in the Franz cell.
Conclusions
As with our previous study,23,25 our findings confirm that flurbiprofen in both 8.75 mg spray and lozenge formulations is able to penetrate human pharynx tissue in an ex vivo model. The use of microautoradiography provided a visual representation of the distribution of flurbiprofen in cadaveric human pharynx tissue. This is important in understanding how flurbiprofen is distributed throughout the pharyngeal tissue following topical application. Although a higher percentage of radiolabeled flurbiprofen remained in the top third of the pharynx tissue, its detection in the lower third of the tissue (furthest from the dosing site) confirms that it can penetrate the deepest layers of the tissue. The evidence that flurbiprofen is available locally through the layers of pharyngeal tissue is worthy of further research, as gaining greater understanding will allow elucidation of the mechanisms involved in rapid pain relief following topical delivery.
Abbreviations
ICH, International Conference on Harmonisation; NSAID, non-steroidal anti-inflammatory drug; URTI, upper respiratory tract infection.
Data Sharing Statement
All data relating to this investigation are reported within the manuscript.
Ethical Approval
Human pharynx tissue was ethically sourced from cadavers by a pathologist (Ethical Tissue, University of Bradford, UK: Research Ethics Committee reference 220367).
Acknowledgments
Medical writing assistance was provided by Elements Communications Ltd., Westerham, UK, and was funded by Reckitt Benckiser Healthcare Ltd., UK.
Author Contributions
All authors contributed to data analysis, drafting or revising the article, have agreed on the journal to which the article will be submitted, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Funding
This work was supported by Reckitt Benckiser Healthcare Ltd, UK.
Disclosure
Rob Turner, Sean Robert Wevrett, Suzanne Edmunds, and Marc Brown are employees of MedPharm Ltd. Anuradha Kulasekaran, Oluwajoba Adegoke, and John Farrah are employees of Reckitt Benckiser Healthcare International Ltd. Reckitt Benckiser were the commercial sponsor for the work detailed in this publication, during the conduct of the study, and are the commercial sponsor for multiple projects at MedPharm, outside the submitted work. MedPharm is a CRO with expertise in topical drug delivery-designed studies and interpreted reports. Medical writing assistance was provided by Elements Communications Ltd. The authors report no other potential conflicts of interest for this work.
References
1. Francis NA, Butler CC, Hood K, Simpson S, Wood F, Nuttall J. Effect of using an interactive booklet about childhood respiratory tract infections in primary care consultations on reconsulting and antibiotic prescribing: a cluster randomised controlled trial. BMJ. 2009;339:b2885. doi:10.1136/bmj.b2885
2. Kenealy T, Arroll B. Antibiotics for the common cold and acute purulent rhinitis. Cochrane Database Syst Rev. 2013;Cd000247. doi:10.1002/14651858.CD000247.pub3
3. Schachtel BP, Fillingim JM, Beiter DJ, Lane AC, Schwartz LA. Subjective and objective features of sore throat. Arch Intern Med. 1984;144:497–500. doi:10.1001/archinte.1984.00350150081026
4. Eccles R. Mechanisms of symptoms of the common cold and influenza. Br J Hosp Med (Lond). 2007;68:71–75. doi:10.12968/hmed.2007.68.2.22824
5. Worrall GJ. Acute sore throat. Can Fam Physician. 2007;53:1961–1962.
6. Ebell MH, Smith MA, Barry HC, Ives K, Carey M. The rational clinical examination. Does this patient have strep throat? JAMA. 2000;284:2912–2918. doi:10.1001/jama.284.22.2912
7. Renner B, Mueller CA, Shephard A. Environmental and non-infectious factors in the aetiology of pharyngitis (sore throat). Inflamm Res. 2012;61:1041–1052. doi:10.1007/s00011-012-0540-9
8. Schachtel B, Shephard A, Schachtel E, Lorton MB, Shea T, Aspley S. Qualities of sore throat index (QuaSTI): measuring descriptors of sore throat in a randomized, placebo-controlled trial. Pain Manag. 2018;8:85–94. doi:10.2217/pmt-2017-0041
9. Addey D, Shephard A. Incidence, causes, severity and treatment of throat discomfort: a four-region online questionnaire survey. BMC Ear Nose Throat Disord. 2012;12:9. doi:10.1186/1472-6815-12-9
10. Pelucchi C, Grigoryan L, Galeone C, et al. Guideline for the management of acute sore throat. Clin Microbiol Infect. 2012;18(Suppl 1):1–28. doi:10.1111/j.1469-0691.2012.03766.x
11. Spinks A, Glasziou PP, Del Mar CB. Antibiotics for sore throat. Cochrane Database Syst Rev. 2013:Cd000023.
12. Hildreth CJ, Burke AE, Glass RM. JAMA patient page. Inappropriate use of antibiotics. JAMA. 2009;302:816. doi:10.1001/jama.302.7.816
13. Oxford JS, Leuwer M. Acute sore throat revisited: clinical and experimental evidence for the efficacy of over-the-counter AMC/DCBA throat lozenges. Int J Clin Pract. 2011;65:524–530. doi:10.1111/j.1742-1241.2011.02644.x
14. Zaman SB, Hussain MA, Nye R, Mehta V, Mamun KT, Hossain N. A review on antibiotic resistance: alarm bells are ringing. Cureus. 2017;9:e1403.
15. Burova N, Bychkova V, Shephard A. Improvements in throat function and qualities of sore throat from locally applied flurbiprofen 8.75 mg in spray or lozenge format: findings from a randomized trial of patients with upper respiratory tract infection in the Russian Federation. J Pain Res. 2018;11:1045–1055. doi:10.2147/JPR.S149331
16. Schachtel B, Aspley S, Shephard A, et al. Onset of action of a lozenge containing flurbiprofen 8.75 mg: a randomized, double-blind, placebo-controlled trial with a new method for measuring onset of analgesic activity. Pain. 2014;155:422–428. doi:10.1016/j.pain.2013.11.001
17. de Looze F, Russo M, Bloch M, Montgomery B, Shephard A, DeVito R. Meaningful relief with flurbiprofen 8.75 mg spray in patients with sore throat due to upper respiratory tract infection. Pain Manag. 2018;8:79–83. doi:10.2217/pmt-2017-0100
18. de Looze F, Russo M, Bloch M, et al. Efficacy of flurbiprofen 8.75 mg spray in patients with sore throat due to an upper respiratory tract infection: A randomised controlled trial. Eur J Gen Pract. 2016;22:111–118. doi:10.3109/13814788.2016.1145650
19. Schachtel B, Aspley S, Shephard A, Schachtel E, Lorton MB, Shea T. Onset of analgesia by a topically administered flurbiprofen lozenge: a randomised controlled trial using the double stopwatch method. Br J Pain. 2018;12:208–216. doi:10.1177/2049463718756152
20. Schachtel BP, Cleves GS, Konerman JP, Brown AT, Markham AO. A placebo-controlled model to assay the onset of action of nonprescription-strength analgesic drugs. Clin Pharmacol Ther. 1994;55:464–470. doi:10.1038/clpt.1994.56
21. Barsuhn CL, Olanoff LS, Gleason DD, Adkins EL, Ho NF. Human buccal absorption of flurbiprofen. Clin Pharmacol Ther. 1988;44:225–231. doi:10.1038/clpt.1988.141
22. Gonzalez-Younes I, Wagner JG, Gaines DA, Ferry JJ, Hageman JM. Absorption of flurbiprofen through human buccal mucosa. J Pharm Sci. 1991;80:820–823. doi:10.1002/jps.2600800903
23. Turner R, Wevrett S, Edmunds S, Brown M, Atkinson R, Shea T. Determination of the permeation and penetration of flurbiprofen from a locally acting sore throat lozenge and spray into human pharynx tissue using a novel ex vivo model and a validated analytical method. Naunyn Schmiedeberg Arch Pharmacol. 2018;391:1–93.
24. Turner R, Wevrett SR, Edmunds S, et al. Determination of the permeation and penetration of flurbiprofen into cadaveric human pharynx tissue. Clin Pharmacol. 2020;12:13–20. doi:10.2147/CPAA.S234227
25. Turner R, Wevrett SR, Edmunds S, Brown M, Atkinson R, Shea T. Validation of an analytical method to quantify the permeation and penetration of flurbiprofen into human pharynx tissue. Biomed Chromatogr. 2019;33:e4499. doi:10.1002/bmc.4499
26. International Conference on Harmonisation of Technical Requirements for Registration of Pharmaceuticals for Human Use. ICH Harmonised Tripartite Guideline. Pharmaceutical Quality System Q10. Available from: https://database.ich.org/sites/default/files/Q10_Guideline.pdf.
27. Franz TJ. Percutaneous absorption on the relevance of in vitro data. J Invest Dermatol. 1975;64:190–195. doi:10.1111/1523-1747.ep12533356
28. Walsh JH, Leigh MS, Paduch A, et al. Evaluation of pharyngeal shape and size using anatomical optical coherence tomography in individuals with and without obstructive sleep apnoea. J Sleep Res. 2008;17:230–238. doi:10.1111/j.1365-2869.2008.00647.x
29. Peres JC, Rouquette JL, Miocevic O, Warner MC, Slowey PD, Shirtcliff EA. New techniques for augmenting saliva collection: bacon rules and lozenge drools. Clin Ther. 2015;37:515–522. doi:10.1016/j.clinthera.2015.02.015
30. Limb M, Connor A, Pickford M, et al. Scintigraphy can be used to compare delivery of sore throat formulations. Int J Clin Pract. 2009;63:606–612. doi:10.1111/j.1742-1241.2008.01984.x
31. Takeuchi H, Mano Y, Terasaka S, et al. Usefulness of rat skin as a substitute for human skin in the in vitro skin permeation study. Exp Anim. 2011;60:373–384. doi:10.1538/expanim.60.373
32. Ayoub R, Muraza G, Imran M, et al. Formulation and permeation kinetic studies of flurbiprofen gel. Trop J Pharm Res. 2015;14:195–203. doi:10.4314/tjpr.v14i2.2
33. Hussain A, Khan GM, Jan SU, et al. Effect of olive oil on transdermal penetration of flurbiprofen from topical gel as enhancer. Pak J Pharm Sci. 2012;25:365–369.
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.