Back to Journals » OncoTargets and Therapy » Volume 9
Patterns of failure and survival in patients with nasopharyngeal carcinoma treated with intensity-modulated radiation therapy in Saudi Arabia
Authors Maklad AM, Bayoumi Y, Senosy Hassan MA, Elawadi AA, AlHussain H, Elyamany A , Aldhahri SF, Al-Qahtani KH, AlQahtani M, Tunio MA
Received 31 August 2015
Accepted for publication 29 April 2016
Published 25 October 2016 Volume 2016:9 Pages 6561—6567
DOI https://doi.org/10.2147/OTT.S95457
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Min Li
Ahmed Marzouk Maklad,1,2 Yasser Bayoumi,2,3 Mohamed Abdalazez Senosy Hassan,2,4 AbuSaleh A Elawadi,5,6 Hussain AlHussain,2 Ashraf Elyamany,7,8 Saleh F Aldhahri,9 Khalid Hussain Al-Qahtani,10 Mubarak AlQahtani,11 Mutahir A Tunio12
1Clinical Oncology, Sohag University, Sohag, Egypt; 2Radiation Oncology, Comprehensive Cancer Center, King Fahad Medical City, Riyadh, Saudi Arabia; 3Radiation Oncology, NCI, Cairo University, Cairo, 4Radiation Oncology, Minia Oncology Center, Minia, 5Clinical Oncology and Nuclear Medicine, Faculty of Medicine, Mansoura University, Mansoura, Egypt; 6Medical Physics, Comprehensive Cancer Center, King Fahad Medical City, Riyadh, Saudi Arabia; 7Medical Oncology, SECI-Assiut University, Assiut, Egypt; 8Medical Oncology, Comprehensive Cancer Center, King Fahad Medical City, 9Department of Otolaryngology, Head and Neck Surgery, King Saud University, 10Department of Otolaryngology-Head and Neck Surgery, College of Medicine, King Saud University, 11Department of ENT, King Fahad Medical City, 12Radiation Oncology, King Fahad Medical City, Riyadh, Saudi Arabia
Background: We aimed to investigate the patterns of failure (locoregional and distant metastasis), associated factors, and treatment outcomes in nasopharyngeal carcinoma patients treated with intensity-modulated radiation therapy (IMRT) combined with chemotherapy.
Patients and methods: From April 2006 to December 2011, 68 nasopharyngeal carcinoma patients were treated with IMRT and chemotherapy at our hospital. Median radiation doses delivered to gross tumor volume and positive neck nodes were 66–70 Gy, 63 Gy to clinical target volume, and 50.4–56 Gy to clinically negative neck. The clinical toxicities, patterns of failures, locoregional control, distant metastasis control, disease-free survival, and overall survival were observed.
Results: The median follow-up time was 52.2 months (range: 11–87 months). Epstein–Barr virus infection was positive in 63.2% of patients. Overall disease failure developed in 21 patients, of whom 85.8% belonged to stage III/IV disease. Among these, there were seven locoregional recurrences, three regional recurrences with distant metastases, and eleven distant metastases. The median interval from the date of diagnosis to failure was 26.5 months (range: 16–50 months). Six of ten (60%) locoregional recurrences were treated with reirradiation ± concurrent chemotherapy. The 5-year locoregional control, distant metastasis control, disease-free survival, and overall survival rates of whole cohort were 81.1%, 74.3%, 60.1%, and 73.4%, respectively. Cox regression analyses revealed that neoadjuvant chemotherapy, age, and Epstein–Barr virus were independent predictors for disease-free survival.
Conclusion: Neoadjuvant chemotherapy followed by IMRT with or without chemotherapy improves the long-term survival of Saudi patients with nasopharyngeal carcinoma. Distant metastasis was the main pattern of treatment failure. Neoadjuvant chemotherapy, age, and Epstein–Barr virus status before IMRT were important independent prognostic factors.
Keywords: nasopharyngeal carcinoma, treatment outcomes, patterns of failures, prognostic factors
Introduction
Radiation therapy, especially intensity-modulated radiation therapy (IMRT) with or without concurrent chemotherapy, is the standard of care for primary nasopharyngeal carcinoma (NPC), resulting in excellent local control and overall survival (OS) rates.1–5 However, local or locoregional recurrences followed by distant metastasis still represent major failure pattern, especially in patients with advanced stages.6,7
Treatment for local or locoregional recurrences is challenging; various treatment options for local or locoregional recurrences have been suggested, including surgery, systemic chemotherapy, and reirradiation with various techniques. Surgery is the feasible option for nodal recurrences in patients treated primarily with IMRT and concurrent chemotherapy.8 Systemic chemotherapy is the treatment of choice in metastatic NPC patients, but it is considered as a palliative option for patients with local or locoregional recurrences.9 Reirradiation in the form of brachytherapy, stereotactic radiosurgery/radiation therapy, and IMRT has been used to treat local or locoregional recurrences with acceptable toxicity and progression-free survival.10–12
Previously, we reported our experience of IMRT with simultaneous modulated accelerated boost technique and concurrent chemotherapy in Saudi patients with NPC.13 Herein, we report long-term follow-up of these patients, especially focusing on the pattern of failures (local, locoregional, and distant), after IMRT and concurrent chemotherapy, prognostic factors and outcomes of reirradiation, and systemic chemotherapy in Saudi patients with recurrent, metastatic NPC.
Patients and methods
Study population
After the approval from the King Fahad Medical City (KFMC) Ethical Committee, this retrospective study was conducted with 68 consecutive patients with histologically proven, nonmetastatic NPC, with Karnofsky performance status ≥70% and who were treated at our institute between April 2006 and December 2011. All patients provided written informed consent. All cases were evaluated through detailed history and physical examination; hematological, renal, and hepatic function tests; Epstein–Barr virus on histological specimens; and rigid nasendoscopy, magnetic resonance imaging (MRI), and computed tomography (CT) imaging of head and neck to evaluate local tumor; CT chest and abdomen, positron emission tomography imaging, and bone scan were also done to detect any distant metastasis. Additional dental and audiological assessments prior to the IMRT were also carried out.
Treatment
Radiation therapy
CT simulation was done for all patients in the supine position with thermoplastic masks for immobilization. Data were acquired with and without contrast (according to renal function tests) using 3 mm slices for planning purpose. Pre-chemotherapy MRI and CT imaging were registered with CT simulation data to delineate the tumor. The gross tumor volume (GTV) included primary (GTV-T) and nodal disease (GTV-N). High-risk clinical tumor volume (CTV-1) included GTV plus 0.5–1.0 cm margins. CTV-2 as designed for potentially involved regions included the nasopharyngeal cavity (limited only to the posterior part of nasal cavity), maxillary sinus (limited to 5 mm anterior to the posterior nasal aperture and maxillary mucosa), pterygopalatine fossa, posterior ethmoid sinus, parapharyngeal space, skull base, anterior third of clivus and cervical vertebra, inferior sphenoid sinus and cavernous sinus, and the retropharyngeal area from the base of the skull to the cranial edge of the second cervical vertebra. The CTV of the neck nodal regions included levels II, III, IV, and V, which were outlined as per Radiation Therapy Oncology Group CTV delineation guidelines for head and neck malignancies. The planning target volume was created with an additional 4 mm margin around CTV. Organs at risk including the brainstem, spinal cord, parotid glands, optic nerves, chiasm, lens, eyeballs, larynx, esophagus, temporomandibular joints, mandible, and cochlea were also contoured. Eclipse™ (Varian Medical Systems, Inc., Palo Alto, CA, USA) was used for IMRT planning. IMRT (step-and-shoot technique) was delivered by using a simultaneous-integrated boost (SIB) technique. IMRT was delivered by using an SIB technique. All patients were treated on Varian Linear Accelerator Series 2100C/D (Varian Medical Systems, Inc.), Clinac DHX (Dual High Energy) upgraded to Trilogy system. Patients’ treatment plans were verified according to the criteria, distance-to-agreement (DTA) 3 mm, and dose difference 3%, using portal dosimetry and PTW 2D-ARRAY seven29 and OCTAVIUS system. The radiation dose delivered was 70 Gy in 35 fractions (2.0 Gy/d) to gross tumor (pre-chemotherapy volume), 63 Gy in 35 fractions (1.8 Gy/d) to high-risk volume, and 56 Gy in 35 fractions (1.6 Gy/d) to low-risk volume. For local or locoregional recurrent cases, reirradiation was given by SRS 25–30 Gy/five fractions or IMRT 50–60 Gy/25–30 fractions according to volume of recurrence and surrounding critical structures.
Chemotherapy
Neoadjuvant chemotherapy was given to 56 patients, which mainly consisted of two to three cycles. Regimens used were cisplatin/docetaxel in 30 patients, cisplatin/epirubicin in 16 patients, and cisplatin/5-flourouracil in ten patients, 3-week interval prior to the initiation of IMRT. Sixty-four patients (91.2%) received concurrent chemoradiation. Concurrent chemotherapy alone was given to eight patients either weekly cisplatin 40 mg/m2 (40 patients) or 3-weekly cisplatin 100 mg/m2 (24 patients).
Follow-up
The duration of follow-up was calculated from the date of diagnosis to either the date of death or the date of the last follow-up. All patients were evaluated at least once every 3 months during the first 2 years and every 6 months thereafter until death. Each follow-up included a complete history, physical examination, and rigid nasendoscopy. CT/MRI scans of the head and neck were performed at 2–3 months posttreatment and afterward as needed. Acute toxicity profile during treatment and first 3 months was assessed by Common Toxicity Criteria Version 3.0 (US Department of Health and Human Services, NIH, NCI, USA), and late toxicities were scored according to the Radiation Therapy Oncology Group radiation morbidity scoring criteria at each follow-up.
Statistical analysis
Primary end points were patterns of failure and OS. Secondary points were locoregional control, distant metastasis control, and disease-free survival (DFS). Locoregional recurrence was defined as the time from diagnosis to reappearance of locoregional failure in irradiated field (nasopharynx or nodes). Distant metastasis control was defined as the time from diagnosis to occurrence of systemic failure. DFS was defined as the time from diagnosis to locoregional failure, distant failure, or death resulting from any cause, whichever occurred first. All survival curves were calculated by using the Kaplan–Meier method, and the difference in survival curves was compared by using the log-rank test. Different categorical variables were compared with the χ2 test. The level of significance was set at P<0.05, and P-values were based on two-sided tests. Multivariate analysis using the Cox proportional hazard model was performed to define various potential prognostic factors.
Results
Patient characteristics
Majority of the NPC patients had locally advanced NPC, stage IV (47.1%) and stage III (38.2%), and majority of cohort had undifferentiated histopathology (75%). Patients’ characteristics are shown in Table 1.
Patterns of failure
Median follow-up duration was 52.2 months (range: 11–87 months). No significant neurological or other late toxicities were documented during the follow-up period. The overall failure rate was 30.8% (21 patients) (Table 1). Ten patients (14.7%) had locoregional recurrences; among these, three locoregional recurrences occurred with combined distant metastasis. Among all locoregional recurrences, there were six local and four nodal recurrences (Figure 1). Initial time to locoregional recurrence was 36.5 months (range: 36.5–63 months). Four patients recurred locally only (two of them were treated by reirradiation after endoscopic resection and one patient presented with extensive local recurrence, which involves base of skull and upper cervical vertebrae with pending fracture, he was unfit for surgical fixation, difficult to manipulate, and did not receive reirradiation, and the fourth one refused treatment). Three patients recurred locoregionally, two of them treated by reirradiation and the third treated by neck dissection plus reirradiation. Eleven/68 patients (16.2%) developed distant metastasis; among them three patients developed local recurrence and was salvaged with reirradiation followed by systemic chemotherapy. Two patients developed local and nodal recurrences and distant metastasis simultaneously (one of them was treated with systemic chemotherapy, while the other patient was unfit and died due to disease progression). Further, five metastatic patients were treated by systemic chemotherapy; three patients were unfit for chemotherapy, two refused treatment, and one patient had only solitary liver metastases treated by surgery alone. Reirradiation was well tolerated; acute grades 3 and 4 mucositis were observed in two of seven patients (28.6%); however, no significant late toxicities were observed. Nodal recurrences were salvaged by neck dissection.
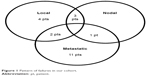  | Figure 1 Pattern of failures in our cohort. |
Eleven patients (16.2%) developed distant metastases (lung, five patients; liver, two; and multiple sites, four). Initial time to distant metastasis was 16 months (range: 16–54 months). All patients with distant metastases were salvaged with systemic chemotherapy as monotherapy (paclitaxal, 5-floururacil [PF], three patients; taxotere (doectaxal) and cisplatin [TP], two patients). Systemic chemotherapy was poorly tolerated with acute grade 3–4 toxicities; neutropenia (three patients) and anemia (one patient); however, no chemotherapy-related late toxicity was observed.
A total of 16 cancer-related deaths were observed; among these, four patients with locoregional recurrences, ten patients with distant metastasis, and two patients with combined locoregional recurrences and distant metastasis died due to disease progression. The 5-year locoregional control, distant metastasis control, DFS, and OS rates of whole cohort were 81.1%, 74.3%, 60.1%, and 73.4%, respectively (Figure 2A–D).
The 4-year and 5-year OS rates for locoregional recurrent NPC were 71.4% and 42.9%, respectively (Figure 3). Median survival in rT2, rT3, and rT4 was 63 months, 25 months, and 14 months, respectively (P=0.001). Median survival in rN1 and rN2 were 40 months and 19 months, respectively (P=0.01). For metastatic NPC, the 2-year and 5-year-OS rates were 45.5% and 10%, respectively.
  | Figure 3 Kaplan–Meier curves showing overall survival rates according to pattern of failures. |
Cox regression analysis of prognostic factors in DFS rates showed that age >40 years, male sex, stages T and N, and neoadjuvant chemotherapy were associated with DFS (Table 2).
Discussion
In the present retrospective review, the distant metastasis was the most common pattern of failure in Saudi patients with NPC treated with IMRT with SIB technique and concurrent chemotherapy that is in agreement with international data.7–9,14 rT4 (especially with intracranial extension via the foramen lacerum and foramen ovale) was the predominant manifestation of locoregional recurrence, which is also in agreement with international data.15 Recurrence with intracranial extension was found to have poor DFS and OS rates even after IMRT as also seen in our study.16 Most of the locoregional recurrences in our study were observed in patients with male sex, advanced-stage disease, positive Epstein–Barr virus status, and in patients without chemotherapy, where efforts were done to lessen the doses to spare critical neurologic structures (optic nerve/chiasm or temporal lobe). Similar findings have been reported by a Chinese study by Kong et al.17
In our cohort, majority of patients with locoregional recurrences were treated with reirradiation via reduced-volume IMRT and stereotactic radiation therapy (SRT) with acute grade 3–4 mucositis of 28.6% without any late side effects (temporal lobe necrosis or mucosal necrosis). High incidence of acute grade 3–4 toxicities can be attributed to high volume of local recurrences and planning target volume in our cohort as compared to reported data. However, high incidence of acute grade 3–4 mucositis in reirradiation in NPC patients is not surprising, as Qiu et al reported 70.3% acute grade 3–4 toxicities,18 and Han et al reported 35.7% acute grade 3–4 toxicities in recurrent NPC patients treated with reirradiation.19
The 5-year DFS and OS rates of NPC patients, especially with locoregional and distant failures in our cohort, were found in agreement with international data.15,18,19 In recurrent NPC cases, rT stage and rN stage were found important prognostic factors for OS in our study cohort. Age was found to be an important independent prognostic factor in this study, which is also in agreement with reported literature.20 Bulky recurrent disease (>100 cm3) or in close proximity to critical neurological structures were treated with systemic chemotherapy alone in our cohort. Worse OS rates in our patients with metastatic disease are also in agreement with international data.21
Strengths of this study were 1) long follow-up duration, 2) accurate evaluation of extent of recurrent disease by MRI, and 3) better selection of patients for reirradiation via IMRT and SRT to minimize late toxicity. Limitations of our study were 1) retrospective data, 2) comparatively a small sample size of Saudi patients, and 3) dosimetric analysis of locoregional recurrent cases.
Conclusion
Distant metastasis is the most common pattern of failure after IMRT with SIB technique with or without neoadjuvant and concurrent chemotherapy in Saudi patients with NPC. Early detection of local and locoregional recurrences is important as reirradiation with IMRT or SRT with or without chemotherapy is still feasible option with acceptable toxicity. However, efforts shall be made for proper patient selection. The volume of initial primary disease and initial T and N stages are important prognostic factors for predicting DFS. Systemic chemotherapy remains the standard treatment option for patients with bulky recurrent and metastatic NPC. However, our results need to be further tested and validated in large prospective trials.
Disclosure
The authors report no conflicts of interest in this work.
References
Roeder F, Zwicker F, Saleh-Ebrahimi L, et al. Intensity modulated or fractionated stereotactic reirradiation in patients with recurrent nasopharyngeal cancer. Radiat Oncol. 2011;6:22. | ||
Chua DT, Sham JS, Kwong DL, Au GK. Treatment outcome after radiotherapy alone for patients with stage I–II nasopharyngeal carcinoma. Cancer. 2003;98(1):74–80. | ||
Xiao WW, Han F, Lu TX, Chen CY, Huang Y, Zhao C. Treatment outcomes after radiotherapy alone for patients with early-stage nasopharyngeal carcinoma. Int J Radiat Oncol Biol Phys. 2009;74(4):1070–1076. | ||
Al-Sarraf M, Leblanc M, Giri PG, et al. Chemoradiotherapy versus radiotherapy in patients with advanced nasopharyngeal cancer: phase III randomized intergroup study 0099. J Clin Oncol. 1998;16(4): 1310–1317. | ||
Chen Y, Liu MZ, Liang SB, et al. Preliminary results of a prospective randomized trial comparing concurrent chemoradiotherapy plus adjuvant chemotherapy with radiotherapy alone in patients with locoregionally advanced nasopharyngeal carcinoma in endemic regions of China. Int J Radiat Oncol Biol Phys. 2008;71(5):1356–1364. | ||
Baujat B, Audry H, Bourhis J, et al; MAC-NPC Collaborative Group. Chemotherapy in locally advanced nasopharyngeal carcinoma: an individual patient data meta-analysis of eight randomized trials and 1753 patients. Int J Radiat Oncol Biol Phys. 2006;64(1):47–56. | ||
Perri F, Dell’Oca I, Muto P, et al. Optimal management of a patient with recurrent nasopharyngeal carcinoma. World J Clin Cases. 2014;2(7):297–300. | ||
Xu T, Tang J, Gu M, Liu L, Wei W, Yang H. Recurrent nasopharyngeal carcinoma: a clinical dilemma and challenge. Curr Oncol. 2013;20(5):e406–e419. | ||
Zheng W, Xu YJ, Qiu SF, et al. Analysis on clinical characteristics and influencing factors of patients with locoregionally advanced nasopharyngeal carcinoma. Asian Pac J Cancer Prev. 2015;16(10):4393–4399. | ||
Law SC, Lam WK, Ng MF, Au SK, Mak WT, Lau WH. Reirradiation of nasopharyngeal carcinoma with intracavitary mould brachytherapy: an effective means of local salvage. Int J Radiat Oncol Biol Phys. 2002;54(4):1095–1113. | ||
Chua DT, Sham JS, Kwong PW, Hung KN, Leung LH. Linear accelerator-based stereotactic radiosurgery for limited, locally persistent, and recurrent nasopharyngeal carcinoma: efficacy and complications. Int J Radiat Oncol Biol Phys. 2003;56(1):177–183. | ||
Hsiung CY, Yorke ED, Chui CS, et al. Intensity-modulated radiotherapy versus conventional three-dimensional conformal radiotherapy for boost or salvage treatment of nasopharyngeal carcinoma. Int J Radiat Oncol Biol Phys. 2002;53(3):638–647. | ||
Fareed MM, AlAmro AS, Bayoumi Y, et al. Intensity-modulated radiotherapy with simultaneous modulated accelerated boost technique and chemotherapy in patients with nasopharyngeal carcinoma. BMC Cancer. 2013;13:318. | ||
Lu TX, Mai WY, Teh BS, et al. Initial experience using intensity-modulated radiotherapy for recurrent nasopharyngeal carcinoma. Int J Radiat Oncol Biol Phys. 2004;58(3):682–687. | ||
Tian YM, Xiao WW, Bai L, et al. Impact of primary tumor volume and location on the prognosis of patients with locally recurrent nasopharyngeal carcinoma. Chin J Cancer. 2015;34(6):247–253. | ||
Chen HY, Ma XM, Ye M, Hou YL, Xie HY, Bai YR. Effectiveness and toxicities of intensity-modulated radiotherapy for patients with locally recurrent nasopharyngeal carcinoma. PLoS One. 2013;8(9):e73918. | ||
Kong F, Ying H, Du C, et al. Patterns of local-regional failure after primary intensity modulated radiotherapy for nasopharyngeal carcinoma. Radiat Oncol. 2014;9:60. | ||
Qiu S, Lin S, Tham IW, Pan J, Lu J, Lu JJ. Intensity-modulated radiation therapy in the salvage of locally recurrent nasopharyngeal carcinoma. Int J Radiat Oncol Biol Phys. 2012;83(2):676–683. | ||
Han F, Zhao C, Huang SM, et al. Long-term outcomes and prognostic factors of re-irradiation for locally recurrent nasopharyngeal carcinoma using intensity-modulated radiotherapy. Clin Oncol (R Coll Radiol). 2012;24(8):569–576. | ||
Hwang JM, Fu KK, Phillips TL. Results and prognostic factors in the retreatment of locally recurrent nasopharyngeal carcinoma. Int J Radiat Oncol Biol Phys. 1998;41(5):1099–1111. | ||
Hsieh CH, Hsu CL, Wang CH, et al. Cisplatin, tegafur-uracil and leucovorin plus mitomycin C: an acceptably effective and toxic regimen for patients with recurrent or metastatic nasopharyngeal carcinoma. Biomed J. 2013;36(5):229–236. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.



