Back to Journals » Clinical Ophthalmology » Volume 14
Outcomes of Small Incision Lenticule Extraction with Dual-Incisions in Myopic Patients
Authors Abdelwahab S , Hamed A , Elshahat A, Rashad S, Elfauyomi M
Received 8 July 2020
Accepted for publication 20 August 2020
Published 7 October 2020 Volume 2020:14 Pages 3067—3074
DOI https://doi.org/10.2147/OPTH.S270032
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Video abstract of "Refractive Small incision Lenticule Extraction with Dual-Incision" [ID 270032].
Views: 349
Shereef Abdelwahab,1 Abdelmonem Hamed,1 Ahmed Elshahat,1 Soliman Rashad,2 Maha Elfauyomi1
1Benha University, Benha, Egypt; 2Suez Canal University, Ismailia, Egypt
Correspondence: Abdelmonem Hamed Tel +20 1221640288
Email [email protected]
Purpose: To assess the stability, safety, predictability, and efficacy of small incision lenticule extraction (SMILE) with dual-incisions in myopic patients.
Setting: Ebsar Eye center, Benha, Qalyopia, Egypt.
Design: Single-center, retrospective, COHORT study.
Patients and Methods: The study was conducted as a retrospective non-comparative analysis of the records of 105 eyes of 53 patients treated by the SMILE with a dual-incisions technique for a mean spherical myopic error of − 5.05 ± 1.93 D (range: − 1.38 to − 9.0 D) with or without astigmatism and the mean astigmatism of − 0.90 ± 0.83 D. The mean LogMAR corrected distance visual acuity (CDVA) was − 0.04 ± 0.07.
Results: One month after surgery, the mean refractive error was − 0.03 ± 0.56 D (range: 0.88 to − 1.50 D), and the mean postoperative astigmatism was 0.20 ± 0.31 D. The mean LogMAR UDVA was 0.07 ± 0.18 in the last follow-up visit, 12 months after surgery. At the end of the follow-up period, approximately 91.43% of patients had unchanged CDVA or gained one or more lines, 8.57% lost one line of CDVA, and 0.0% lost 2 lines.
Conclusion: SMILE with dual-incisions is effective and safe, with a stable and predictable outcome for correction of myopia and myopic astigmatism.
Keywords: SMILE, ReLEX, SMILE technique, kerato-refractive, LASER vision correction, small incision lenticule extraction
Introduction
Small-incision lenticule extraction (SMILE) is a bladeless and flapless technique for laser vision correction of myopia and myopic astigmatism, which has lately become intended by the refractive surgeons and strongly wished for patients as well. In this technique, a corneal stromal lenticule is created using a VisuMax® femtosecond laser (Carl Zeiss Meditec, Jena, Germany) and removed through a single corneal incision.1,2
By avoiding the creation of a corneal flap, SMILE eliminates the possibility of flap-related complications such as flap displacement, striae, and dislocation. Also, it is all-in-one femtosecond laser refractive surgery and finally, it is a micro-incision and minimally invasion surgery.2,3 This explains higher surgeon confidence with the safety, efficacy, and predictability of SMILE and higher patient satisfaction postoperatively.4,5
Epithelial ingrowth within the corneal cap-stromal interface has been reported in 0.5% of eyes undergoing SMILE,5 and pocket inflammatory infiltrates in 0.3%.6 Some surgeons prefer to irrigate the pocket at the end of SMILE, especially when SMILE is combined with corneal collagen cross-linkage.7 Because performing dual incisions which facilitate the irrigation of the SMILE pocket in most of the above-mentioned situations, we decided to analyse the safety and efficacy of SMILE performed using dual vertical incisions.
Patients and Methods
Study Design
This is a single-center, retrospective, COHORT study of consecutive patients. Analysis of the records of 53 myopic patients treated by SMILE between February and May 2019 by one experienced LASIK surgeons (SMA) using the VisuMax femtosecond laser at the Ebsar Eye Center, Egypt. A full and thorough ophthalmologic examination was carried out prior to surgery including the assessment of manifest and cycloplegic refraction, uncorrected distance visual acuity (UDVA), best-corrected distance visual acuity (CDVA), intraocular pressure, pupil size, corneal tomography (Pentacam Oculus), as well as anterior segment and fundus evaluation. During each postoperative follow-up visit the patients were assessed for CDVA and UDVA by using the ETDRS visual acuity chart and expressed in LogMAR visual acuity, refraction, and corneal tomography. The study protocol had followed and was adhered to the tenets and principles of the Declaration of Helsinki and was approved by Benha Faculty of Medicine Research Ethics Committee that it meets national and international guidelines for research on humans. Informed consent and permission to use their data for analysis and publication were obtained from each patient prior to surgery as part of our routine preoperative protocol.
Inclusion Criteria Were
Spherical equivalent up to −10 D, age of 21y or older, stable refraction for at least 1y, soft contact lens discontinued for 1 week and rigid gas permeable lens discontinued for 3 weeks prior to the procedure, the minimum corneal thickness of 500 μm at the thinnest location, a residual stromal bed of at least 250. Only patients who have completed one year of follow-up were included in this study. Patients who missed the follow-up visits for at least 12 months were not included in the statistical analysis.
Exclusion Criteria Included
Proof of residual or active ocular diseases such as herpetic keratitis, uveitis, glaucoma, visually significant cataract, retinal diseases such as retinal dystrophies or diabetic retinopathy, corneal diseases like dystrophy or keratoconus, history of ocular trauma or surgery, severe dry eyes, use of systemic medications like (eg, Corticosteroids or antimetabolites), autoimmune diseases, or females who were pregnant or nursing.
Refractive Small Incision Lenticule Extraction Procedure
Data from 53 consecutive subjects who were seeking SMILE for myopia and myopic astigmatism in Ebsar eye center, Benha, Egypt, in the period between 1st of February and 31st May 2019 was studied. All SMILE surgeries were performed by one experienced refractive surgeon (SMA). Each subject underwent manifest and cycloplegic refraction, uncorrected and best-corrected distant visual acuity (UDVA and BDVA), slit-lamp biomicroscopy, and corneal topography (Pentacam, Oculus).
Surgical Technique
After the application of topical anesthesia, standard sterile draping, and insertion of the speculum, the patient’s eye was centered and docked with small size curved interface cone.
Once proper centration was achieved, the surgeon switched-on the automatic suction. The femtosecond laser platform (VisuMax®; Carl Zeiss Meditec, Jena, Germany) was used to create the lenticule and incision of all cases. The femtosecond laser produces ultrashort pulses of light at a repetition rate of 500 kHz with a typical pulse energy of 125 nJ, which are focused at a precise depth in the corneal tissue. A plasma state evolves with an optical breakdown, and a small gas bubble is formed from the vaporization of tissue. A series of bubbles are created in a spiral manner, with a typical spot and track distance of 3 mm for the lamellar cuts and 2 mm for the vertical side cuts resulting in cleavage of tissue planes. At the beginning the femtosecond laser cuts the posterior surface of the lenticule, which is followed by the side cut of the lenticule, then the anterior surface of the lenticule is created. Finally, two side-cut incisions are created instead of one; a primary entry incision of 3.0 mm centered at 120◦, and a secondary draining incision (3.0 mm) centered at 270◦ to be positioned at the most dependant site with the gravity for better evacuation of the pocket (Figure 1) (Dr. Abdelmonem Hamed technique whereas the second incision has a location at 270◦ which is different than other second incision proposed for SMILE by other authors who created the second incision opposite to the first one at 300◦).
 |
Figure 1 SMILE with dual-incisions. |
After releasing the suction, the patient was moved toward the observation position under the VisuMax® integrated surgical microscope. The refractive small incision lenticule extraction (ReSMILE) push-up technique8,9 was then used to facilitate recognition of the edge of the lenticule inside the pocket through the coaxial illumination of the VisuMax® femtosecond laser machine microscope, the lenticule was then dissected and removed through the primary SMILE corneal wound. The SMILE procedure had the following parameters: 100 mm cap thickness, 7.5 mm anterior-plane (cap) cut diameter, and 6.5 mm optical zone of the lenticule. The target postoperative sphere was Plano.
Postoperative Evaluation
Patients have been instructed to instil tobramycin and dexamethasone (Tobradex; Alcon Laboratories, Inc., Fort Worth, TX) and ofloxacin (Exocin; Allergan Ltd., Marlow, United Kingdom) four times daily for the first week, which is our standard protocol for broadspectrum prophylaxis. Patients were reviewed at 1 day and 1, 3, 6, and 12 months postoperatively. Refraction was obtained at the 1-month postoperative visit. All subsequent follow-up visits included measurements uncorrected distance visual acuity (UDVA), manifest refraction, and corrected distance visual acuity (CDVA), as well as slit-lamp examination, and Pentacam corneal tomography.
Statistical Analysis
Outcome analysis was performed according to the Standard Graphs for Reporting Refractive Surgery.10 The outcomes were analysed. Data from the 12-month visit were used for analysis. Student’s paired t-test was used to calculate the statistical significance.
Microsoft Excel master sheet 2010 (Microsoft Corporation, Redmond, WA) was used for data entry and statistical analysis. A P-value of less than 0.05 was defined as statistically significant.
Results
Table 1 shows the demographic data for the study population. Figure 2 shows the standard graphs for reporting the outcomes of refractive surgeries. Any case with intraoperative complications was excluded from this study. We had only one eye of postoperative epithelial ingrowth (noticed in 3rd month follow up) that had been scraped and washed out of the pocket through the second side cut incision located at 270 degrees.
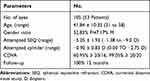 |
Table 1 Preoperative Demographic and Refractive Characteristics of the Included Patients |
Refraction
Preoperative mean spherical equivalent was −5.05 ± 1.93 D (Range: - 1.38 D to - 9.0 D; Table 1). Postoperative (at 12 month) mean spherical equivalent was −0.33 ± 0.40 D (range: −1.5 D to 0.88 D).
Refractive Efficacy
At 12 months postoperatively, 105 eyes (100%) achieved a UCVA of 20/25, and 100 eyes (95%) had achieved a UCVA of 20/20, and 71 eyes (68%) had achieved 20/16 (Figure 2A: which shows cumulative percentages of eyes in which target refraction was zero attaining specified levels of uncorrected distance visual acuity (UDVA) 12 months after SMILE). While Figure 2B shows the difference between postoperative UDVA and preoperative corrected distance visual acuity CDVA, it shows 80.0% of eyes achieved UCDV within 1 line of CDVA, and 97.8% of eyes achieved UCDV within 2 lines of CDVA.
Safety
On 12 months postoperatively, 26 eyes (24.76%) showed a gain of 1 line CDVA, 3 eyes (2.86%) showed a gain of 2 lines CDVA, 67 eyes (63.81%) showed no change in CDVA, while 9 eyes (8.57%) showed a loss of 1 line of CDVA at 12 months postoperatively (Figure 2C: which shows the percentage of eyes (y-axis) in which there was a gain/loss of a specified number of LogMAR of corrected distance visual acuity (CDVA) lines 12 months after SMILE).
Predictability
A scatter plot of the attempted correction versus the achieved correction (manifest spherical equivalent) at 12 months after SMILE is shown in Figure 2D and E. 95% of eyes were within 1.0 D of the attempted correction, and 77% of eyes were within 0.5 D of the attempted correction.
Stability
Figure 2F; shows the Long-term stability of SMILE in myopic patients between three and 12 months. Only 8.57% had a change greater than 0.5 D. However, the spherical equivalent had insignificant change from −0.34 ± 0.46 D at 3rd month to −0.33 ± 0.40 D at 12th month (P-value: 0.62).
Astigmatism Analysis
Figure 2G shows refractive astigmatism at 12 postoperatively were 89.52% of eyes were ≤0.5 diopters of astigmatism, while 100% of eyes were ≤1.0 diopters of astigmatism. Figure 2H show the higher R2 value which equals 88 on the attempted versus the achieved spherical equivalent scatter plot, this suggests that the SMILE with 2 side-cut incisions led to a predictable outcome. Figure 2I show the vector analysis results at 12 months postoperatively, the arithmetic mean was 1.5 ± 12.4, however, the absolute mean was 7.3 ± 11.8. The percentage of refractive astigmatism angle error < −15° was 6.7%, however, the percentage of refractive astigmatism angle error ˃ −15° was 7.6%. The mean of the target induced astigmatism (TIA) was −0.90 ± 0.83, and the surgical induced astigmatism (SIA) was 0.99 ± 78.
Discussion
With the increasing popularity of SMILE as a refractive choice for subjects with myopia and myopic astigmatism, there is an increased need to irrigate the stromal pocket either during or after the operation in the follow-up period. One such situation is in cases with epithelial ingrowth. Among the reported complications of SMILE is epithelial ingrowth10,11 which may require surgical removal. In the past, we resorted to converting the SMILE cap into a flap using a new suction cone and a conversion license, to be able to effectively scrape off the recurrent epithelial ingrowth and wash out the epithelial cells. Yet recently, we started creating two incisions for all of our SMILE cases, one primary entry incision centered between 9 and 12 o’clock at 120◦, and a 2nd draining incision at 270◦. This secondary incision has allowed us to effectively irrigate the stromal pocket to wash away the epithelial cells by inserting the irrigation cannula through the main incision and forcing fluid through the pocket and out of the draining incision which is located at the most dependent site with the gravity for better evacuation of fluidics. The same concept applies when we irrigate the stromal pocket in cases with severe inflammatory infiltrate or bleeding inside the pocket, or when we instil Riboflavin into the pocket in cases undergoing combined SMILE with corneal collagen cross-linkage. The advantage is the conversion of the stromal pocket from a closed dead space where fluid struggles to circulate through therefore trapping epithelial cells, inflammatory cells, blood, or Riboflavin in cases of SMILE XTRA, to an open space where fluid can flow unidirectional washing away unwanted content from the stromal pocket with ease.
Previous major studies in a large number of patients undergoing SMILE are summarized in Table 2.1,4,6,12–16 Our findings were comparable with, or slightly better than those in previous studies in terms of safety and efficacy.
 |
Table 2 Previous Studies on Refractive Outcomes in a Cohort of Patients Undergoing SMILE |
Interpreting the results of this study, there was a stability that supports the results of other studies that reported similar 6- and 12-month visual outcomes reflecting refractive stability17 which means the second SMILE incision had no adverse effect on the refractive outcomes of this research study.
In the light of our research results, we believe that adding a second side cut incision at 270 degrees will act as a second hand for the refractive surgeons facilitating management in a plethora of situations, ranging from epithelial ingrowth, inflammatory infiltrate and combined SMILE with corneal collagen cross-linkage (SMILE XTRA).18,19 Therefore, we recommend adopting the double-incisions SMILE technique as an effective, potentially beneficial alternative to single-incision surgery. We believe that adding the second incision to standard SMILE will reduce the need to convert the cap into a flap. This should save the cost of a new cone and the conversion license. Also, we do recommend creating a special and fine instrument for epithelial ingrowth removal to be used with double SMILE surgery in the future. However, more detailed research studies are required to evaluate the dual-incisions SMILE technique and to get out its advantages and disadvantages to light, especially the effect of the second incision on the eye dryness after dual-incisions SMILE, and its refractive outcomes as well.
Disclosure
The authors did not receive any financial support from any public or private sources. The authors have no financial or proprietary interest in a product, method, or material described herein. The authors report no conflicts of interest for this work.
References
1. Sekundo W, Kunert KS, Blum M. Small incision corneal refractive surgery using the small incision lenticule extraction (SMILE) procedure for the correction of myopia and myopic astigmatism: results of a 6 month prospective study. Br J Ophthalmol. 2011;95(3):335–339.
2. Shah R, Shah S, Sengupta S. Results of small incision lenticule extraction: all-in-one femtosecond laser refractive surgery. J Cataract Refract Surg. 2011;37(1):127–137.
3. Wang Y, Wu Z, Tang X, et al. Two-millimeter micro-incision lenticule extraction surgery with minimal invasion: a preliminary clinical report. Zhonghua Yan Ke Za Zhi. 2014;50(9):671–680.
4. Vestergaard A, Ivarsen AR, Asp S, Hjortdal JØ. Small-incision lenticule extraction for moderate to high myopia: predictability, safety, and patient satisfaction. J Cataract Refract Surg. 2012;38(11):2003–2010.
5. Moshirfar M, McCaughey MV, Reinstein DZ, Shah R, Santiago-Caban L, Fenzl CR. Small incision lenticule extraction. J Cataract Refract Surg. 2015;41(3):652–665.
6. Ivarsen A, Asp S, Hjortdal J. Safety and complications of more than 1500 small-incision lenticule extraction procedures. Ophthalmology. 2014;121:822–828.
7. Graue-Hernandez EO, Pagano GL, Garcia-de la Rosa G, et al. Combined small-incision lenticule extraction and intrastromal corneal collagen crosslinking to treat mild keratoconus: long-term follow-up. J Cataract Refract Surg. 2015;41(11):2524–2532.
8. Hamed A, Fekry A. Refractive small incision lenticule extraction: push-up and pushdown techniques. J Cataract Refract Surg. 2016;42:1713–1715.
9. Hamed AM, Abdelwahab SM, Soliman TT. Intraoperative complications of refractive small incision lenticule extraction in the early learning curve. Clin Ophthalmol. 2018;12:665–668.
10. Reinstein DZ, Archer TJ, Randleman JB. JRS standard for reporting astigmatism outcomes of refractive surgery. J Refract Surg. 2014;30:654–659.
11. Wang Y, Ma J, Zhang J, et al. Incidence and management of intraoperative complications during small-incision lenticule extraction in 3004 cases. J Cataract Refract Surg. 2017;43(6):796–802.
12. Hjortdal JØ, Vestergaard AH, Ivarsen A, Ragunathan S, Asp S. Predictors for the outcome of small-incision lenticule extraction for Myopia. J Refract Surg. 2012;28:865–871.
13. Reinstein DZ, Carp GI, Archer TJ, Gobbe M. Outcomes of small incision lenticule extraction (SMILE) in low myopia. J Refract Surg. 2014;30:812–818.
14. Pedersen IB, Ivarsen A, Hjortdal J. Tree-year results of small incision lenticule extraction for high myopia: refractive outcomes and aberrations. J Refract Surg. 2015;31:719–724.
15. Hansen RS, Lyhne N, Grauslund J, Vestergaard AH. Small-incision lenticule extraction (SMILE): outcomes of 722 eyes treated for myopia and myopic astigmatism. Graefes Arch Clin Exp Ophthalmol. 2016;254:399–405.
16. Elmassry A, Ibrahim O, Osman I, et al. Long-term refractive outcome of small incision lenticule extraction in very high myopia. Cornea. 2020;39(6):669–673.
17. Sekundo W, Gertnere J, Bertelmann T, et al. One-year refractive results, contrast sensitivity, high-order aberrations and complications after myopic small-incision lenticule extraction (ReLEx SMILE). Graefes Arch Clin Exp Ophthalmol. 2014;252:837–843.
18. Osman IM, Helaly HA, Abou Shousha M, AbouSamra A, Ahmed I. Corneal safety and stability in cases of small incision lenticule extraction with collagen cross-linking (SMILE Xtra). J Ophthalmol. 2019;2019:1–10.
19. Ganesh S, Brar S. Clinical outcomes of small incision lenticule extraction with accelerated cross-linking (ReLEx SMILE Xtra) in patients with thin corneas and borderline topography. J Ophthalmol. 2015;2015:263412.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

