Back to Journals » International Journal of Women's Health » Volume 10
Misoprostol for the prevention of postpartum hemorrhage during home births in rural Lao PDR: establishing a pilot program for community distribution
Authors Durham J , Phengsavanh A, Sychareun V, Hose I , Vongxay V , Xaysomphou D, Rickart K
Received 2 September 2017
Accepted for publication 25 February 2018
Published 9 May 2018 Volume 2018:10 Pages 215—227
DOI https://doi.org/10.2147/IJWH.S150695
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Elie Al-Chaer
Jo Durham,1 Alongkone Phengsavanh,2 Vanphanom Sychareun,2 Isaac Hose,1 Viengnakhone Vongxay,2 Douangphachanh Xaysomphou,2 Keith Rickart3
1Faculty of Medicine, School of Public Health, University of Queensland, Brisbane, Queensland, Australia; 2Faculty of Post-Graduate Studies, University of Health Sciences, Vientiane, Lao PDR; 3Communicable Diseases Branch, Department of Health, Brisbane, Queensland, Australia
Purpose: The purpose of this study was to gather the necessary data to support the design and implementation of a pilot program for women who are unable to deliver in a healthcare facility in the Lao People’s Democratic Republic (PDR), by using community distribution of misoprostol to prevent postpartum hemorrhage (PPH). The study builds on an earlier research that demonstrated both support and need for community-based distribution of misoprostol in Lao PDR.
Methods: This qualitative study identified acceptability of misoprostol and healthcare system needs at varying levels to effectively distribute misoprostol to women with limited access to facility-based birthing. Interviews (n=25) were undertaken with stakeholders at the central, provincial, and district levels and with community members in five rural communities in Oudomxay, a province with high rates of maternal mortality. Focus group discussions (n=5) were undertaken in each community.
Results: Respondents agreed that PPH was the major cause of preventable maternal mortality with community distribution of misoprostol an acceptable and feasible interim preventative solution. Strong leadership, training, and community mobilization were identified as critical success factors. While several participants preferred midwives to distribute misoprostol, given the limited availability of midwives, there was a general agreement that village health workers or other lower level workers could safely administer misoprostol. Many key stakeholders, including women themselves, considered that these community-level staff may be able to provide misoprostol to women for self-administration, as long as appropriate education on its use was included. The collected data also helped identify appropriate educational messages and key indicators for monitoring and evaluation for a pilot program.
Conclusion: The findings strengthen the case for a pilot program of community distribution of misoprostol to prevent PPH in remote communities where women have limited access to a health facility and highlight the key areas of consideration in developing such a program.
Keywords: community distribution, misoprostol, postpartum hemorrhage, prevention, Lao PDR
Introduction
More than 303,000 women are estimated to have died globally during, and following, pregnancy and childbirth in 2015.1 Most of these deaths are preventable1,2 and are a result of women in remote rural areas in particular, having limited access to basic essential obstetrical care.1,3 Globally, postpartum hemorrhage (PPH) is the single leading direct cause of maternal mortality4,5 and is also associated with severe morbidity.6 Due to the high prevalence of anemia among pregnant women in low-resource settings, the outcome of PPH is often worsened, resulting in detrimental health outcomes from relatively moderate loss of blood.7 Despite the high number of deaths due to PPH, it is largely preventable with active management of the third stage of labor (AMTSL).8 Components of AMTSL include administration of an oxytocic immediately following birth (usually oxytocin), placental delivery by controlled cord traction, and uterine massage.8 As many maternal deaths from PPH occur in women without identifiable risk factors, all women should have access to AMTSL, including the use of an oxytocic.1 Oxytocin however, requires skilled administration by injection, access to cold-chain storage, and medical disposables, making it unfeasible in many low-resource settings.9–11 In low-resource settings where access to oxytocin is not possible, misoprostol provides a low-cost, heat-stable oxytocic that can be taken orally, providing a practical alternative for preventing PPH.12 Available studies also show that with adequate information, education, and support, misoprostol can be safely administered by community health workers, or self-administered.12–16
Notwithstanding its potential life-saving properties, the community distribution of misoprostol has been controversial. Much of the controversy relates to the potential use of misoprostol as an abortive agent, as well as possible uterine rupture that can result from inappropriate administration during the third trimester of pregnancy.17 However, there is no evidence that inappropriate use of misoprostol for abortion is a major problem.3,14,16,18 Studies in Tanzania, Ethiopia, Nigeria, and Papua New Guinea, for example, have shown that misoprostol can be successfully distributed at the community level and administered by women themselves or non-medical providers following basic training and support.3,14,16,18 Based on the quality and depth of evidence, both the World Health Organization (WHO) and the International Federation of Gynecology and Obstetrics (FIGO) guidelines for the prevention of PPH now include a recommendation for misoprostol (600 μg orally) administered during the third stage of labor by community health workers in contexts where women are unable to access facility-based birthing.10,19,20
The Lao People’s Democratic Republic (PDR) is a lower middle-income country in South-East Asia with high maternal mortality estimated at 197 deaths per 100,000 live births (80% uncertainty interval 136–307). The largest contributor to maternal death is PPH,21–27 and there are stark disparities in access to maternal healthcare.23 The proportion of urban women assisted by a health professional during birth (80%), for example, is more than double that of rural women (31%), with ~69% of women in rural areas delivering at home assisted by relatives or on their own.23 Reasons for low uptake of facility-based birthing in rural communities relate to distance and cost of reaching health facilities; poor attitudes of health staff; poor quality of care and care practices in clinics including a lack of privacy and the presence of male staff; the desire to deliver at home with family support; the economic need to work until the onset of labor; and the wish to follow traditional practices.28 Improving maternal mortality is a priority for the Lao government, and in this context, the prophylactic use of misoprostol during home deliveries potentially provides an interim solution to prevent PPH, until all pregnant women have access to basic essential obstetric care.
Misoprostol is currently on the essential medicines list (EML) and approved to prevent and treat PPH by a trained midwife at the central, provincial, and district hospitals, as well as in health centers. The recently released National Strategy and Action Plan for Integrated Services on Reproductive, Maternal, Newborn and Child Health 2016–202529 also includes the prophylactic use of misoprostol to prevent PPH during home deliveries, without the presence of a skilled birth attendant. As with any health intervention, community distribution of misoprostol for the prevention of PPH is complex,7 mainly due to the required timing of distribution and ensuring correct use.7 Given this, the purpose of this study was to gather the necessary data to design and implement a pilot program supporting community distribution of misoprostol to prevent PPH in cases where women are unable to deliver in a healthcare facility. The study builds on earlier research in Lao PDR30 which demonstrated both support and need for community-based distribution of misoprostol and is part of a larger program of research by the authors on the use of misoprostol in the Lao PDR.
Research methods
Study design
This qualitative study aimed to collect information that would be used to inform the design of community-based distribution of misoprostol to prevent PPH in expectant mothers. Interviews (n=25) were undertaken with key stakeholders at the central, provincial, and district levels. In addition, five focus group discussions (FGDs) were undertaken in five rural communities in Oudomxay province.
Study setting
The healthcare system in Lao PDR is primarily public, especially in rural areas where the intervention will take place. The healthcare delivery system has four administrative levels: central (Ministry of Health [MoH]), provincial (provincial health offices), district (district health offices), and village health centers (souksalas) in key catchment areas. Health services are stratified through the central (tertiary) hospitals based in the national capital of Vientiane, provincial (secondary) hospitals based in provincial capitals, and district (first referral level) hospitals based in each district capital (Figure 1). At the primary healthcare level, there is a network of health workers, which includes the staff in district hospitals or souksalas, village health workers (VHWs), who are a relatively new cadre of government employees having completed a 6-month basic training program, and lay people from the community, who are village health volunteers (VHVs).31 At the district and souksala level, training of health staff is often rudimentary with few facilities having midwives or skilled birth attendants. Basic essential obstetric care is only available at the district level, limiting access for remote rural communities. Each community has a VHV, and in some communities, there is a VHW.
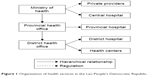  | Figure 1 Organization of health services in the Lao People’s Democratic Republic. |
The province of Oudomxay, in the northwest of the country, was selected as the location for this pilot program. Oudomxay is ethnically diverse with a mountainous topography, meaning that many villages have limited access to basic infrastructure healthcare. It has the second lowest national rate of births attended by a skilled birth attendant23 and has high rates of under-nutrition. Rural families in the study setting live a semi-subsistence lifestyle. Men and women are engaged in farm work for long hours each day, with most of the food grown for home consumption and supplemented by hunting. Houses are simple, mainly made of wooden walls with a dirt or wooden floor and thatched roof, with no latrines or piped water. As in all Lao villages, a village head (Nai Ban) provides leadership and undertakes administrative duties supported by key village personnel, such as a representative from the Lao Women’s Union or the Lao Youth Union.
Sample
The study used a purposive sampling design32,33 with key informants (N=25) identified based on local knowledge and snowball sampling to identify participants with a knowledge of the topic and the context.34 In-country reports were also retrieved from an Internet search to identify information-rich participants. Informants included MoH staff at central and provincial levels (n=5), district level (n=4), hospital staff (central/provincial/district) (n=2), international nongovernmental organization staff (n=2), multilateral organization staff (n=2), an international expert (n=1), souksala staff (n=2), and VHV/VHW/village heads (n=7). In total, 10 participants worked in Vientiane and 15 were working in Oudomxay at the province, district, and village levels.
Five villages were selected using criterion sampling33 for the FGDs based on: 1) known cases of PPH, 2) travel time from provincial capital (2–4 hours), 3) distance to district health service (>4 km), and 4) population (50–150 people). One FGD was conducted in each sample village making five FGDs in total. The sampling also aimed to ensure ethnic diversity between villages. These villages were within four districts of Oudomxay (Xay, La, Namo, and Nga districts). Upon arrival in each sample village, available and appropriate participants were nominated by the Nai Ban, VHV, or VHW according to inclusion criteria.33 The inclusion criteria were: 1) women aged 18–40 years, 2) women with children aged <5 years, and 3) husbands, mothers, and mothers-in-law of these women, if culturally appropriate. The interview format was decided in consultation with key village informants (village heads, VHVs, and VHWs) and included 1) women only, 2) combination of women and mothers or mothers-in-law, or 3) combination of women, mothers or mothers-in-law, and husbands. Focus groups consisted of 5–9 participants each. To promote participation and culture appropriateness, women were invited to bring children to each FGD.
Data collection
Key informant interviews (n=25) were conducted in either English or Laotian using a semi-structured interview guide. FGDs (n=5) at the village level were undertaken in Laotian or the local ethnic language. A topic guide was used with open and semi-structured questions,11,35 allowing relevant areas to be explored, while providing opportunities for participants to raise pertinent issues.36,37
Two medical doctors (VV and DX) from the Lao University of Health Sciences (UHS) trained in public health research and translation, assisted with interviews conducted in Laotian. In FGDs where participants preferred to use their own language, a local interpreter identified within the village or from the district health office assisted with translation. On these occasions, questions asked in English were simultaneously translated into Lao and then into the local language. In this process, it is possible that there were some translation errors or loss of nuance and original meaning. Nevertheless, it was felt that the benefits of interviewing participants who do not speak Lao outweighed the risks of not representing ethnic minorities, especially given it is women from these populations who are most likely to give birth at home without access to healthcare.23 Interviews and FGDs were recorded (with informed consent) by using an audio-recorder, with summary notes taken. These field notes were crosschecked with audio-recordings with ambiguous portions back-translated.
Refreshments were provided during FGDs, and at the end of each FGD, a small gift of soap, adhesive bandages, and antiseptic cream was given to acknowledge the potential loss of productivity for participants after the conclusion of each FGD. Participants were not informed of the gift prior to the interview, and the gift was not considered sufficient to be coercive.
Data analysis
The interview transcripts in English were read multiple times by three of the researchers (JD, KR, and IH) to identify codes. The data were then coded jointly by JD and KR and grouped into key themes, by using both inductive and deductive approaches34 guided by the “Prevention of Postpartum Haemorrhage at Home Birth” program implementation guide.35 Throughout the analytical process, there was movement back and forth between the entire data set and the coded extracts, with interpretations checked by the research team.
Ethics
Ethical approval for this study was granted by the School of Public Health University of Queensland Ethical Review Committee (approval # IH101015) and the National Ethics Committee for Health Research, MoH of Lao PDR (approval # 004). Individual participants provided written informed consent. At the village level, where participants were illiterate, participant information sheets were read to participants in the preferred language. This allowed for and encouraged discussion in order to ensure understanding. Hard copies were provided to participants who requested them. Oral consent was provided and recorded in the presence of a witness. Where participants could sign their name, written consent was obtained. Sometimes however, where the participant was unable to write their name they provided verbal consent or a local person assisted participants when necessary to write their names. Given known levels of literacy in the remote, rural villages verbal consent was approved by the National Ethics Committee for Health Research, Ministry of Health of Lao PDR and the School of Public Health University of Queensland Ethical Review Committee. All data was de-identified, and it was stressed that participation was voluntary and that participants could withdraw at any time and decline to answer any of the questions.
For key informant interviews (central to district levels), written consent was obtained, and participants’ organizations and positions were recorded during data collection and subsequently coded and de-identified. The participants were, however, given the option of remaining identifiable, or being contacted in the future to check interpretations of the findings. Given the small sample size, during the consent process, participants were made aware of the small risk of deductive identification.38
Results
Accessing facility-based birthing and managing PPH
Almost all respondents agreed that facility-based birthing was increasing across the country including within Oudomxay, due to improved infrastructure, better levels of education, and Lao PDR’s free maternal and child healthcare policy, which provides better access to antenatal care (ANC), facility-based delivery, and postpartum care. Nevertheless, respondents recognized that in remote rural areas such as those in Oudomxay, women continued to experience multiple barriers in accessing facility-based birthing, rarely had birth preparedness plans and a major cause of preventable maternal mortality in the province was PPH. Echoing a sentiment expressed by many, one district health staff member succinctly summarized some of the barriers experienced by women:
There are many barriers [to accessing a healthcare facility], the first one is about their low family income. The second is the transportation. If they don’t have a car, they would have to walk for a few hours to get to the health facility. The third one is that we don’t have the specific delivery room for them, so they are shy when they come to deliver at the health facility. And the last one is that after delivery, it might take a few days for the women to recover, and when they want to go back home, it also takes a few hours. That’s why they don’t want to deliver at the health facility. [KII_12_district]
In FGDs, women described postpartum bleeding as a normal, cleansing process, which if inhibited could result in adverse health effects to the mother. However, they described heavy, ongoing bleeding that did not decrease over time as dangerous. While unable to identify the amount of blood that was dangerous, participants recounted symptoms such as feeling dizzy, fainting, collapsing, or losing consciousness. Initial management for these symptoms included drinking water or herbal teas, uterine massage, and other traditional practices to manage PPH, with presentation at a hospital usually being the last resort.
Acceptability of community-based distribution of misoprostol
All healthcare professionals interviewed recognized that community distribution of misoprostol could provide an interim solution to reduce PPH until access to facility-based birthing is improved. In FGDs, women said they would be happy to take tablets after birth if recommended by the district health staff, providing it did not stop “good” (normal) postpartum bleeding. The women also felt that short-term minor side effects would be acceptable as long as they were aware of them in advance.
A few healthcare professionals expressed concerns over the use of misoprostol in the case of twins, noting that incorrect use would affect community confidence:
If we use it without knowing that there is a second baby in the mother’s tummy, mother’s uterus, it can cause … If they take the misoprostol right after the first baby is delivered, it can also lead to death of the second baby for twin cases … . It can lead to the death of newborns by wrongly introducing misoprostol in the wrong time. Then, it’s a problem. Then, the mothers in the community will get traumatized by this experience. [KII_04_central]
Some healthcare professionals were concerned about the use of misoprostol as an abortifacient. However, most felt that this was not a major concern, given increased access to family planning. Furthermore, they were also aware that women were able to access a Chinese brand of misoprostol via local pharmacies, as one person explained:
And you know, because there’s very poor pharmaceutical controls, there’s also a LOT [interviewee emphasis] of self-administered medical abortion going on, in Vientiane. I can’t speak for other provinces, it’s well known, and everybody knows it happens, people know it goes down. People call it the Chinese medicine, people call it misoprostol. Pharmacists will tell you no I don’t stock it, because people do naughty things with it. Like that’s a really common statement. And I mean you can’t ignore that issue, I don’t think, you can’t pretend like that’s not happening. But I think with appropriate rollout measures, that shouldn’t be used as a reason to avoid distribution, just speaking personally. Because that’s happening anyways, people are accessing miso anyways, so saying that there’s a potential for misuse as a reason not to distribute it, seems to me a hollow answer, given the fact that people are already accessing it, and it’s not like that’s going to change. You know, government control of pharmaceuticals is not going to somehow improve suddenly. So why would you NOT distribute a potentially beneficial initiative, because of a potential misuse, when that potential misuse already exists in the community. [KII_2_central]
Overall, however, stakeholders expressed strong support for misoprostol to prevent PPH at home-births. The potential for misoprostol to save lives was a priority, as the following interview excerpts from key stakeholders help to illustrate:
They have already discussed in a meeting that for women in remote areas if they come to the souksala or the district for ANC late in pregnancy then they could be given miso with an explanation of how to use it and take it with them. We can try to advise them to have birth at the health facility and we implement the free delivery in Lao but if they can’t, we can give misoprostol. [KII_03_central]
And after delivery, every woman must take misoprostol immediately. Because most of the women in the rural area already have anemia, a mild bleeding may cause serious problem. [KII_06_province]
… the most important is to help them to have a safe delivery no matter where they deliver. [KII_12_district]
Some stakeholders, especially from international organizations, felt that establishing in-country evidence via a pilot program would help increase acceptability.
We need really a comprehensive discussion and debate among partners and the government. Also, it would be good to have some evidence. If we have some good programs where misoprostol has been safely used and then gain research for maternal and newborn health then it can be used for the debate. [KII_04_central]
A further important point raised was the need for a pilot program to have the potential for scaling up a national program.
… the activity components should be easy to scale up. For instance, think about it. After the pilot project if it shows good results and it should really be shared with partners [of the MoH], so the government, can see if it is possible to scale up or not. If it stays only in one community or two communities it’s not very meaningful. We should always think [from the start] about the possibility of scaling up later on. For this, we should really think about the cost. Also, we should think about getting very solid data that is convincing for everyone. [KII_04_central]
Supply and procurement
All key informants felt that high-level government endorsement supported by the promulgation of a decree would be key to securing a sustainable misoprostol supply. Key informants identified integrating misoprostol into the mother and childcare package, sourcing the drug through existing channels and making it available at the community level via the district health hospital as the most sustainable supply and procurement mechanism. However, several informants observed that donor funding is often critical for the MoH channels to function effectively even with drugs on the EML. Almost all stakeholders felt that based on experience, revolving drug funds would be ineffective as a means of a sustainable supply of misoprostol.
Preferred administration methods of misoprostol
For healthcare professionals, providing women access to misoprostol in late pregnancy during ANC visits was the ideal scenario. However, most felt given that the majority of women in rural and remote locations present only once at ANC, instead of the recommended four visits, and usually during early pregnancy, this approach would achieve low coverage. For most respondents, the next preferred distribution option were community midwives based in souksalas. A lesser number of midwives, however, especially in the areas most in need, was identified as a limitation. The least preferred option was misoprostol distribution by non-midwives or lower level staff in the community, however, as one person noted “you have lots of women there who will never meet a healthcare provider” [KII_14_central].
Given a community-based distribution model, there was a general agreement that VHWs would be preferable to VHVs to distribute misoprostol, given their higher level of education and practical training in provincial hospitals. However, it was recognized that the low coverage of VHWs at the village level would be a limiting factor in the effectiveness of only using this group of healthcare workers.
Although some respondents, including some women, were reluctant to endorse self-administration of misoprostol, most recognized that VHWs (or skilled birth attendants) may not always be available at the time of birth, and as such, advanced distribution of misoprostol in late pregnancy by community level staff, for self-administration may be appropriate. Given lower levels of education in remote areas, participants highlighted the importance of pictorial information on misoprostol and its usage:
We have to show them the picture and the video of the real situation showing how the misoprostol can prevent the postpartum hemorrhage, and the scenario demonstration is a good idea to encourage their understanding about misoprostol. And we have to show them the mechanism of the drug on contracting the uterus. [KII_06_province]
There was consensus that provision of misoprostol in private pharmacies for women to self-administer would be inappropriate and potentially unsafe, as one person explained:
The danger would be if women could just go and buy it and not really know what to do. The pharmacists are not always trained either. That’s the thing, they could just be a villager themselves, then they are just selling it to other villages really without any appropriate training. That’s a bit of a danger. [KII_13_province]
Gender and the administration of misoprostol
There was an agreement among all stakeholders, including community members, that women and others likely to be present at the birth should receive education on the correct usage of the drug and its possible side effects. It was also recognized that as key opinion leaders, the village head and the village Lao Women’s Union representative would play an important role in supporting community-based misoprostol distribution by promoting an understanding of the purpose and usage of misoprostol. All key informants felt community distribution of misoprostol should include the promotion of facility-based birthing in line with MoH policy.
A limitation identified with VHWs and VHVs distributing misoprostol was that often in rural areas, men occupy these roles due to their higher levels of Laotian language as compared to women. Also in some ethnic communities, cultural norms preclude a man being present during delivery. For women in these communities, the Lao Women’s Union representative (who can generally speak Lao), especially if misoprostol were to be provided immediately after delivery, may be a preferred provider. As one health worker at the district level explained:
I think the best distributor could be the Lao women union because in some village, the health volunteers are male, so they are not good at working for mother and child health. So, I think the Lao women union is better. [KII_12_district]
Respondents at the district level also felt it was easier for women to “open their hearts” to other women and discuss intimate personal matters such as birthing, especially where the other woman had experienced childbirth herself. Another issue identified with some VHWs and VHVs was that they are usually selected based on their education level. Lao Women’s Union representatives on the other hand, are usually multiparous senior village women and trusted by expectant mothers in matters related to pregnancy and child rearing. One person from the district also noted that women tend to trust women from their own ethno-linguistic group more than health staff from other ethno-linguistic groups.
In some ethnic groups, they won’t listen to health center staff because they are in different ethnic group. That’s why, I need the health volunteer and the Lao women union in that village give them the health education. [KII_11_district]
However, there was a recognition of capacity constraints for village Lao Women’s Union representatives who are often responsible for work in multiple sectors, as one informant explained:
… women’s union is one woman in a village – she has a life, she has other things to do. The nutrition strategy says she’ll be the nutrition unit of the village, the health strategy says she’ll become the family planning unit of the village, like you know it’s just ridiculous. If you looked at every different ministry and every different strategy how many times the women’s union was going to do something – you’d see that she basically has like a 20 hour a day job – being the volunteer for the education sector, the transport sector, the education … information system, monitoring, and evaluation. [KII_02_central]
Most stakeholders felt that misoprostol should be stored at souksalas (with VHWs sourcing supplies from these facilities as needed based on the number of pregnant women in the village). Healthcare professionals highlighted the need for appropriate packaging and labeling of misoprostol with a very specific indication for PPH prevention using pictorial images to differentiate it from a Chinese brand of misoprostol available in private pharmacies as an abortifacient. All participants felt that providing the drug late in pregnancy was preferable. In the FGDs, women were concerned that otherwise they would forget how to take it, or their children might inadvertently take it, given the lack of safe storage in traditional housing.
None of the women in this study reported having birth preparedness plans and some of the key informants suggested that misoprostol distribution should accompany the development of these plans, including promotion of facility-based birthing. Some stakeholders also suggested that community distribution of misoprostol should include the provision of safe birthing kits and other key messages related to newborn care:
There should be a lot of other things that should be included so things like, clean cord care, and leaving the baby on the mother and early breastfeeding, early initiation of breastfeeding, skin to skin, putting the baby skin to skin on the mother, which would help the mother’s risk of hemorrhage, as well as the baby’s … rate of survival ... So, facility birth should be a goal, but given the fact that facility birth is not accessible for everyone at this time, or preferred for very good reasons, then harm reduction mentality would be – let’s get clean birth kits out, let’s get access to miso in the community. [KII_02_central]
Training needs
Informants identified training and clinical guidelines as essential in any pilot program of community-based distribution of misoprostol. One person also mentioned that including WHO recommendations to administer misoprostol only after excluding the existence of a second baby as important to be included in national guidelines, training curriculum, and community messages. This should include guidelines for ANC staff to ask whether there is a family history of multiple births and training misoprostol administrators to palpate for a second twin prior to administering misoprostol. For longer-term sustainability following the pilot program, informants suggested for misoprostol training to be included in the existing training for mother and childcare package. This would also help integrate training into current mechanisms whereby training cascades down from the higher levels to the souksala and village level, including monitoring and refresher training.
Training VHVs in the appropriate use and distribution of misoprostol was a concern for some key informants due to low literacy levels, the unpaid nature of these positions, often low motivation, and lack of longevity, as illustrated in the excerpt below:
I was the trainer, myself. Half of the villages were illiterate. Every message, it should be like a pictorial or a verbal explanation. Also, another challenge is that they are taking rotations, because nobody wants to become a village health volunteer, because it doesn’t give any incentive for them, either financial or non-financial. After three years, they change so that there are new people who are coming to become a village health volunteer. We should do the refreshing training for those staff. [KII_04_central]
The need for health staff to be trained in data collection methods for monitoring and evaluation as well as how to deliver information appropriately to women was also seen as critical in promoting the acceptance and uptake of misoprostol.
When we distribute misoprostol to women, we need to train the health staff in the health center especially the head of the health center to train [pregnant women] about how to use and how to monitor [misoprostol] because the health staff can communicate with pregnant women in the community, … if we train the health staff in the community so they understand how to use misoprostol they can explain to the women in the community who feel uncomfortable about coming to meet the doctor in town. [KII_07_province]
Education messages for women, their families, and influential people in the village such as village heads and the Lao Women’s Union representative were identified as:
- the benefit of taking misoprostol;
- possible side effects;
- correct dose and administration; and
- promotion of facility-based birthing, postnatal care, and infant vaccination.
Participants identified the information delivery mechanisms at the community level as:
- information sessions in each target community, with both men and women, by district level health staff;
- ongoing promotion of safe birthing practices, including misoprostol, by the village head and Lao Women’s Union representative at village meetings;
- pictorial representation of health promotion materials on safe birthing practices displayed within the village; and
- VHWs/VHVs counseling pregnant women and their families about safe birthing practices.
Community interviews identified that women often drink herbal tea after childbirth, and some informants noted the need to include messages about safe tea consumption, as some herbal teas may have possible uterotonic properties. A comprehensive list of key safe birthing messages identified are included in Box 1.
  | Box 1 Key messages to accompany misoprostol distribution |
Central level technical advisory group and key partners
All healthcare professionals interviewed stated that a directive and policy from MoH that would support community distribution of misoprostol for the prevention of PPH could be interpreted as contrary to the strong policy focus on increasing facility-based deliveries, as one person explained:
It is a good idea to distribute misoprostol to prevent PPH. But I think that this activity might not be aligned with the government policy because, now, we try to encourage women to come to deliver at the hospital, but if we give them the drug [misoprostol], they might not come because they might think that taking the drug is enough for them to deliver safely [rather than come to hospital]. It’s just my opinion. Anyway, I realize that misoprostol distribution is very effective for prevent PPH as many countries have already implemented community distribution. So, if the government has a policy to implement misoprostol distribution at the community level, we will follow the policy because I know that it can reduce the risk of PPH. [KII_6_province]
Endorsement and technical support from key international players such as the WHO was considered crucial in gaining higher-level political support. The Lao Association of Obstetrics and Gynecology was seen as having a critical role in advocating for the implementation of community-based distribution of misoprostol and supporting the implementation at the provincial and district levels. Key informants at the central level suggested that the existing Maternal and Child Health (MCH) Technical Working Group (TWG) provided a good forum for technical advice and oversight of implementation of the pilot program and any subsequent scaling up of a broader program. Informants also suggested establishing a Technical Advisory Group under the TWG. Commonly mentioned potential participants of a Technical Advisory Group included relevant staff from the UHS, members of the Lao Association of Obstetrics and Gynecology, staff from the Centre for Maternal and Child Health, the WHO, and United Nations Population Fund. The Department of Training and Resource along with the Lao Association of Obstetrics and Gynecology and prominent obstetricians/gynecologists from the central maternity hospital were also identified as useful resources for developing a training curriculum.
Implementation, monitoring, and evaluation
Key informants agreed that a pilot program should be implemented by the MoH through the MCH centers (central to provincial) with advice from the Lao Association of Obstetrics and Gynecology and the Technical Advisory Group. External program funders, technical support partners, and the UHS were identified as possible partners in monitoring and evaluating the pilot program. Box 2 summarizes the potential indicators that have been identified. At the district and community levels, key informants agreed that monitoring should be integrated into existing MCH monitoring processes and forms, as one person suggested:
  | Box 2 Potential indicators for monitoring community distribution of misoprostol |
Every woman who gets pregnant gets a book, right, every woman who gets pregnant gets registered a book, so you could see that they could put a sticker on the front that says ‘miso given out on this day, returned, used’ you know and somebody, you know, and there’s a mark and somebody files that away with a sticker number 5071 [for example]. [KII_06_provincial]
Based on this research, Table 1 summarizes some of the enablers and barriers to implementing community-based distribution of misoprostol for the prevention of PPH in Lao PDR. Strong government support and recognition that community distribution of misoprostol provides an interim measure to reduce maternal mortality from PPH are critical to its success. Some of the potential barriers including weak health information systems, medical supply chain mechanisms, and low levels of health worker education are some of the reasons why women do not have adequate access to safe, facility birthing.
Discussion
Despite substantial improvements in access to facility-based birthing in Lao PDR, women in remote and rural areas continue to give birth at home without a skilled birth attendant. This relates to well-documented access barriers including transport, distance, and the timing of when women go into labor39 which have been observed in similar settings.14 While women continue to give birth unsupervised, whether through choice or circumstance, they are at risk of maternal mortality or morbidity due to PPH, particularly if they do not have access to oxytocics as a part of the AMTSL. In other settings where women do not have access to skilled birth attendants, misoprostol, a proven uterotonic drug that can be distributed and administered by unskilled providers, has been used as an effective interim solution to prevent PPH.3,13,16,40,41 A community-based, double-blind, randomized controlled trial of misoprostol for PPH prevention in home births in Gambia, for example, found the drug to be safe and effective.42 A placebo-controlled trial undertaken in rural areas in India (N=1,620, n=812 received oral misoprostol, n=808 placebo, after delivery) showed that misoprostol reduced acute PPH by nearly 50% compared with placebo and was associated with a significant reduction in acute severe postpartum hemorrhage of 80%.43 Similarly, a double-blind, randomized controlled trial of misoprostol for PPH prevention in home births in Pakistan, found that the drug was safe and effective in reducing PPH.44 Other studies have found community distribution of misoprostol by trained lay people for the prevention of PPH to be safe and effective, acceptable to women and their families.12–14,16,18,35
Based on the evidence, FIGO have recently updated their guidelines to include the option of secondary prevention at the community level as a targeted and cost-effective approach.45 In secondary prevention of PPH, a regimen of 800 μg sublingual misoprostol is administered to women with higher-than-average bleeding (~350 mL or more).45,46 To be effective, however, this approach requires community-level healthcare providers to identify appropriate recipients of misoprostol, a task that may not be possible in remote villages of Lao PDR due to the difficulty in accurately assessing postpartum blood loss.46
The findings of this study suggest that community-based distribution of misoprostol during late pregnancy to prevent PPH by trained VHWs, where available, would be feasible and appropriate. This is provided that women, their families, and the community receive adequate information and education by people they trust. Trusted and credible sources of information were district health and souksala staff, VHWs, village heads, and representatives from the Lao Women’s Union. In areas where VHWs are not available or appropriate, other suitable cadres might include VHVs, or women themselves may self-administer after receiving appropriate education. While some informants expressed concerns about the ability of VHWs and other village-level staff to distribute and administer misoprostol, and the ability of women and families to understand and follow instructions on its use, studies in Tanzania,16 Ethiopia,3 Papua New Guinea,14 and other low-resource setting countries have shown that misoprostol can be effectively distributed at the community level and administered by lay people following an unsupervised birth.34,42,44,47–49 These studies have usually included training and education about birth preparedness, the importance of supervised births, recognizing danger signs, including PPH, and correct usage and common side effects.14,35,42,43,48–50
While concerns were also raised relating to the potential misuse of misoprostol as an abortifacient, a viable solution of appropriate packaging and branding was identified. Furthermore, several participants noted that misoprostol, sometimes with mifepristone, is readily available under a different name through private pharmacies for use in medical abortion. A number of study participants also suggested the inclusion of clean birthing kits with misoprostol for home births. This approach has been used effectively in similar remote, low-resource environments such as Papua New Guinea.14 The development of clinical guidelines and training including consistent engagement with provincial, district, and community health structures, as well as key community opinion leaders and women themselves was seen as crucial. One person had concerns that in the case of twins, misoprostol may be inadvertently given before the birth of the second child – a concern that has been raised in the literature13 and WHO guidelines advising to administer misoprostol only after excluding the existence of a second baby.10 ANC staff asking whether there is a family history of multiple births should be included in any national guidelines.
As in an earlier study in Lao PDR,30 a minority of stakeholders cited concerns that access to misoprostol would detract from the drive to increase facility-based birthing.12,14,50,51 Other studies conducted in similar environments to Lao PDR have shown that the provision of well-developed health promotion messaging to expectant mothers and their families on the use of misoprostol, with inclusion of the importance of facility birthing where possible, can actually increase the number of supervised deliveries.12,15,50–55 Furthermore, the strong political commitment to reducing maternal mortality and the recognition that providing all women with access to basic and emergency obstetric care as a long-term endeavor provides an enabling environment for the introduction of community-based distribution of misoprostol to prevent PPH. This is further evidenced by the release of the National Strategy and Action Plan for Integrated Services on Reproductive, Maternal, Newborn and Child Health 2016–202556 after the present study was conducted, which includes the prophylactic use of misoprostol for PPH during home deliveries in the absence of a skilled birth attendant. The study provides the necessary information to develop and evaluate a pilot program of community-based distribution of misoprostol for PPH prevention.
Limitations
A study limitation was that purposive sampling of the villages and the sample size means that the data are not representative of the Lao PDR as a whole or of all remote areas in Lao PDR where misoprostol could prevent PPH. The study included, however, 25 key informants likely to be involved in decisions related to the community distribution of misoprostol for the prevention of PPH. The use of interpreters may have influenced data collection, especially in non-Lao-speaking villages where a third interpreter who was a local speaker was required. Crosschecking and back-translation of audio recordings, with the interpreter(s) where possible, helped ensure the quality of the translation. Furthermore, despite the limitations, the results of this study align with those of other studies in similar environments and provide important information in designing a pilot intervention to distribute misoprostol, as a prophylaxis to prevent PPH, to expectant mothers, who are unable to access healthcare.
Conclusion
This study lends further support to the findings of a previous stakeholder analysis and provides valuable lessons to inform the design of a pilot program in Oudomxay, Lao PDR. The study suggests that the community distribution of misoprostol for the prevention of PPH is acceptable to community members and key stakeholders and feasible in remote areas in Lao PDR. It also suggests that the potential risks pertaining to the safe and effective use of community-based distribution of misoprostol for home births are manageable, especially when compared to the risks for women who, for various reasons, are unable to access facility-based birthing. This, however, is not to sidestep the importance of addressing the socioeconomic determinants preventing women from receiving appropriate perinatal care. Furthermore, while oxytocin remains the gold standard for PPH, misoprostol has rigorous evidence to support its use to prevent PPH in remote settings where both oxytocin and timely transfer to higher-level care are not available. As such, this study provides the impetus to develop national policies and programs for the community distribution of misoprostol to prevent PPH and reduce maternal mortality in Lao PDR.
Disclosure
The authors report no conflicts of interest in this work.
References
WHO. Essential Obstetric Care: Fact Sheet No 245. Geneva, Switzerland: WHO Press; 2015. | ||
Alkema L, Chou D, Hogan D, et al. Global, regional, and national levels and trends in maternal mortality between 1990 and 2015, with scenario-based projections to 2030: a systematic analysis by the UN Maternal Mortality Estimation Inter-Agency Group. Lancet. 2016;387(10017):462–474. | ||
Prata N, Gessessew A, Abraha AK, Holston M, Potts M. Prevention of postpartum hemorrhage: options for home births in rural Ethiopia. Afr J Reprod Health. 2009;13(2):87–95. | ||
Rajan PV, Wing DA. Postpartum hemorrhage: evidence-based medical interventions for prevention and treatment. Clin Obstet Gynecol. 2010;53(1):165–181. | ||
Say L, Chou D, Gemmill A, et al. Global causes of maternal death: a WHO systematic analysis. Lancet Glob Health. 2014;2(6):e323–e333. | ||
Amaral E, Souza J, Surita E, et al. A population-based surveillance study on severe acute maternal mortality (near-miss) and adverse perinatal outcomes in Campinas, Brazil: the Vogomoma Project. BMC Pregnancy Childbirth. 2011;11:9. | ||
Oladapo OT, Fawole B, Blum J, Abalos E. Advance misoprostol distribution for preventing and treating postpartum haemorrhage. Cochrane Database Syst Rev. 2012;2:CD009336. | ||
Begley CM, Gyte GM, Devane D, McGuire W, Weeks A. Active versus expectant management for women in the third stage of labour. Cochrane Datatbase Syst Rev. 2011;11:CD007412. | ||
Rasheed R, Alam AA, Younus S, Raza F. Oral versus vaginal misoprostol for labour induction. J Pak Med Assoc. 2007;57(8):404–407. | ||
WHO. WHO Recommendations for the Prevention of Postpartum Haemorrhage. Geneva, Switzerland: WHO Press; 2012. | ||
Grenier L, Smith J, Currie S, Suhowatsky S. Advance distribution of misoprostol for self-administration: Expanding coverage for the prevention of postpartum hemorrhage. Program implementation guide. Revised, November 2013. Available from: https://www.mchip.net/sites/default/files/Miso%20Expansion%20Guide.pdf. Accessed May 2017. | ||
Smith JM, Gubin R, Holston MM, Fullerton J, Prata N. Misoprostol for postpartum hemorrhage prevention at home birth: an integrative review of global implementation experience to date. BMC Pregnancy Childbirth. 2013;13(1):44. | ||
Alfirevic Z, Blum J, Walraven G, Weeks A, Winikoff B. Prevention of postpartum hemorrhage with misoprostol. Int J Gynecol Obstet. 2007;99(Suppl 2):S198–S201. | ||
Vallely LM, Homiehombo P, Walep E, et al. Feasibility and acceptability of clean birth kits containing misoprostol for self-administration to prevent postpartum hemorrhage in rural Papua New Guinea. Int J Gynecol Obstet. 2016;133(3):301–306. | ||
Prata N, Passano P, Bell S, Rowen T, Potts M. New hope: community-based misoprostol use to prevent postpartum haemorrhage. Health Policy Plan. 2013;28(4):339–346. | ||
Prata N, Mbaruku G, Campbell M, Potts M, Vahidnia F. Controlling postpartum hemorrhage after home births in Tanzania. Int J Gynecol Obstet. 2005;90(1):51–55. | ||
Oladapo OT. Misoprostol for preventing and treating postpartum hemorrhage in the community: a closer look at the evidence. Int J Gynecol Obstet. 2012;119(2):105–110. | ||
Prata N, Ejembi C, Fraser A, Shittu O, Minkler M. Community mobilization to reduce postpartum hemorrhage in home births in northern Nigeria. Soc Sci Med. 2012;74(8):1288–1296. | ||
Lalonde A. Prevention and treatment of postpartum hemorrhage in low-resource settings – FIGO Safe Motherhood and Newborn Health (SMNH) Committee. Int J Gynecol Obstet. 2012;117(2):108–118. | ||
International Federation of Gynecology and Obstetrics. International Federation of Gynecology and Obstetrics. Prevention of Post-Partum Haemorrhage with Misoprostol: FIGO Guideline in brief; 2012. Available from: http://www.figo.org/sites/default/files/uploads/project-publications/Miso/PPH%20prevention/Prevention%20of%20PPH%20with%20Misoprostol_In%20Brief_2012_English.pdf. Accessed August 12, 2017. | ||
Eckermann L. Finding a “safe” place on the risk continuum: a case study of pregnancy and birthing in Lao PDR. Health Sociol Rev. 2006;15(4):374–386. | ||
Eckermann L, Scopaz A, Clarke M. Quality of life for pregnant and recent parity women in Lao PDR. In: Eckermann L, editor. Gender, Lifespan and Quality of Life. New York: Springer; 2014:115–133. | ||
MoH LM, MoES. Lao Social Indicator Survey (LSIS). Vientiane, Lao PDR: Lao PDR Ministry of Health, Lao Statistics Bureau, UNFPA, UNICEF; 2012. Available from: https://dhsprogram.com/pubs/pdf/FR268/FR268.pdf. Accessed March 28, 2018. | ||
Ye Y, Yoshida Y, Sakamoto Junichi J. Factors affecting the utilization of antenatal care services among women in Kham district, Xiengkhouang province, Lao PDR. Nagoya J Med Sci. 2010;72(1–2):23–33. | ||
WHO. Trends in Maternal Mortality: 1990 to 2015 – Estimates by WHO, UNICEF, UNFPA, World Bank Group and the United Nations Population Division. Geneva, Switzerland: WHO – Department of Reproductive Health and Research; 2015. | ||
UNFPA. The State of World Population 2016. 2016. Available from: https://www.unfpa.org/sites/default/files/sowp/downloads/The_State_of_World_Population_2016_-_English.pdf. Accessed March 28, 2018. | ||
World Health Organisation. Maternal health. Available from: http://www.wpro.who.int/laos/topics/maternal_health/en/. Accessed June 22, 2017. | ||
Sychareun V, Hansana V, Somphet V, Xayavong S, Phengsavanh A, Popenoe R. Reasons rural Laotians choose home deliveries over delivery at health facilities: a qualitative study. BMC Pregnancy Childbirth. 2012;12:86. | ||
Ministry of Health. National Strategy and Action Plan for Integrated Services on Reproductive, Maternal, Newborn and Child Health 2016–2025 Vientiane, Lao PDR 2016. Available from: http://www.laoshealth.org/assets/national-rmnch-strategy-2016-2025.pdf. | ||
Durham J, Warner M, Phengsavanh A, Sychareun V, Vongxay V, Rickart K. Stakeholder analysis of community distribution of misoprostol in Lao PDR: a qualitative study. PLoS One. 2016;11(9):e0162154. | ||
WHO, Ministry of Health. Health Service Delivery Profile: Lao PDR 2012. Lao PDR: WHO, Ministry of Health; 2012. | ||
Liamputtong P. The science of words and the science of numbers: research methods as foundations for evidence-based practice in health. In: Research Methods in Health: Foundations for Evidence-Based Practice. Melbourne: Oxford University Press 2010:3–26. | ||
Padgett DK. Qualitative and Mixed Methods in Public Health. Thousand Oaks: Sage Publications; 2012. | ||
Pope C, Mays N. Qualitative Research in Health Care. Malden, MA: Wiley; 2006. | ||
Sanghvi H, Zulkarnain M, Chanpong G. Prevention of Postpartum Hemorrhage at Home Birth: A Program Implementation Guide. Baltimore: Jhpiego; 2009. | ||
Creswell JW. Research Design: Qualitative, Quantitative, and Mixed Methods Approaches. Thousand Oaks: Sage Publications; 2013. | ||
Bowling A. Research Methods in Health: Investigating Health and Health Services. Maidenhead, Berkshire: Open University Press: McGraw-Hill Education (UK); 2014. | ||
Sieber JE. Witnesses to research wrongdoing. J Empir Res Hum Res Ethics. 2012;7(5):3–14. | ||
Sychareun V, Hansana V, Somphet V, Xayavong S, Phengsavanh A, Popenoe R. Reasons rural Laotians choose home deliveries over delivery at health facilities: a qualitative study. BMC Pregnancy Childbirth. 2012;12(1):86. | ||
Prata N, Bell S, Karasek D, Vahidnia F, Hamza S, Holston M. Inability to predict postpartum hemorrhage: insights from Egyptian intervention data. BMC Pregnancy Childbirth. 2011;11:97. | ||
Cardoso P, Nielsen BB, Hvidman L, Nielsen J, Aaby P. Effect of sublingual misoprostol on severe postpartum haemorrhage in a primary health centre in Guinea-Bissau: randomised double blind clinical trial. BMJ. 2005;331(7519):723. | ||
Walraven G, Blum J, Dampha Y, et al. Misoprostol in the management of the third stage of labour in the home delivery setting in rural Gambia: a randomised controlled trial. BJOG. 2005;112(9):1277–1283. | ||
Derman RJ, Kodkany BS, Goudar SS, et al. Oral misoprostol in preventing postpartum haemorrhage in resource-poor communities: a randomised controlled trial. Lancet. 2006;368(9543):1248–1253. | ||
Mobeen N, Durocher J, Zuberi N, et al. Administration of misoprostol by trained traditional birth attendants to prevent postpartum haemorrhage in homebirths in Pakistan: a randomised placebo-controlled trial. BJOG. 2011;118(3):353–361. | ||
Morris JL, Winikoff B, Dabash R, et al. FIGO’s updated recommendations for misoprostol used alone in gynecology and obstetrics. Int J Gynecol Obstet. 2017;138(3):363–366. | ||
Raghavan S, Geller S, Miller S, et al. Misoprostol for primary versus secondary prevention of postpartum haemorrhage: a cluster-randomised non-inferiority community trial. BJOG. 2016;123(1):120–127. | ||
Sanghvi H, Ansari N, Prata NJV, Gibson H, Ehsan AT, Smith JM. Prevention of postpartum hemorrhage at home birth in Afghanistan. Int J Gynecol Obstet. 2010;108(3):276–281. | ||
Mir AM, Wajid A, Gull S. Helping rural women in Pakistan to prevent postpartum hemorrhage: a quasi experimental study. BMC Pregnancy Childbirth. 2012;12:120. | ||
Smith JM, Dimiti A, Dwivedi V, et al. Advance distribution of misoprostol for the prevention of postpartum hemorrhage in South Sudan. Int J Gynecol Obstet. 2014;127(2):183–188. | ||
Rajbhandari S, Hodgins S, Sanghvi H, et al. Expanding uterotonic protection following childbirth through community-based distribution of misoprostol: operations research study in Nepal. Int J Gynecol Obstet. 2010;108(3):282–288. | ||
Sanghvi H, Ansari N, Prata NJ, Gibson H, Ehsan AT, Smith JM. Prevention of postpartum hemorrhage at home birth in Afghanistan. Int J Gynecol Obstet. 2010;108(3):276–281. | ||
Spangler S, Gobezayehu A, Getachew T, Sibley L. Interpretation of national policy regarding community-based use of misoprostol for postpartum hemorrhage prevention in Ethiopia: a tale of two regions. J Midwifery Womens Health. 2014;59(Suppl 1):S83–S90. | ||
Starrs A, Winikoff B. Misoprostol for postpartum hemorrhage: moving from evidence to practice. Int J Gynecol Obstet. 2012;116(1):1–3. | ||
VSI, BixbyCenter. Prevention of Postpartum Hemorrhage in Five Rural Zambian Districts. Bixby Center for Population Health Sustainability Ministry of Health; 2010. Available from: http://bixby.berkeley.edu/wp-content/uploads/2015/03/MOH_VSI-Zambia-Pilot-Evaluation-Report-2010-12-FINAL-LETTER.pdf. Accessed February 2, 2018. | ||
VSI, BixbyCenter. Introduction of Misoprostol for Prevention of Postpartum Hemorrhage at the Community Level in Kenya VSI, Bixby Center for Population Health; 2011. Available from: http://bixby.berkeley.edu/wp-content/uploads/2015/03/Kenya-KOGS-VSI-Miso-PPH-Report-2011-03F.pdf. Accessed February 2, 2018. | ||
Ministry of Health. National Strategy and Action Plan for Integrated Services on Reproductive, Maternal, Newborn and Child Health 2016–2025, Lao PDR. Vientiane, Lao PDR: Ministry of Health; 2016. |
 © 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

