Back to Journals » Clinical Ophthalmology » Volume 15
Long-Term Outcome After Silicone Oil Removal in Eyes with Myopic Retinal Detachment Associated with Macular Hole
Authors Ghoraba HH, Leila M , Shebl M , Abdelhafez MA, Abdelfattah HM
Received 22 December 2020
Accepted for publication 29 January 2021
Published 8 March 2021 Volume 2021:15 Pages 1003—1011
DOI https://doi.org/10.2147/OPTH.S298565
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Scott Fraser
Hammouda Hamdy Ghoraba,1,2 Mahmoud Leila,3 Mohamed Shebl,4 Mohamed Ahmed Abdelhafez,4 Haithem Maamoun Abdelfattah4,5
1Ophthalmology Department, Faculty of Medicine, Tanta University, Tanta, Egypt; 2Magrabi Eye Hospital, Tanta, Egypt; 3Retina Department, Research Institute of Ophthalmology, Giza, Egypt; 4Vitreoretinal Consultant, Magrabi Eye Hospital, Tanta, Egypt; 5Vitreoretinal Associate Consultant, Benha Teaching Hospital, Benha, Egypt
Correspondence: Mahmoud Leila
Retina Department, Research Institute of Ophthalmology, Giza, Egypt
Tel +201286644025
Email [email protected]
Purpose: To assess the efficacy of pars plana vitrectomy (PPV) and silicone oil tamponade for management of myopic retinal detachment associated with macular hole (MRDMH) and to assess the anatomical and functional outcomes of this technique and its long-term validity after silicone oil removal.
Methods: Retrospective interventional non-comparative case series including consecutive patients who had PPV and silicone oil tamponade for MRDMH. All patients had an axial length ≥ 26 mm. Main outcome measures were retinal re-attachment and macular hole closure after silicone oil removal, improvement of best-corrected visual acuity (BCVA), and complications secondary to surgery. Chi square/Fisher’s exact test was used to analyze categorical variables, while One-way ANOVA/Kruskal–Wallis test was used to compare variables across the closure type and complications. Correlations between numerical variables were tested using Spearman correlation. Kaplan–Meier method was used to estimate the event-free survival. P value is significant at 0.05.
Results: The study included 26 eyes of 26 patients. Retinal re-attachment rate after primary and secondary surgeries was 88.4% and 100%, respectively. W-type macular hole closure occurred in 58% of eyes. Vision improved in 58% of eyes. Mean final BCVA was 0.05 decimal units, p = 0.004. Cataract and glaucoma developed in 42% and 15% of eyes, respectively. Initial BCVA, axial length and duration of silicone oil tamponade did not correlate significantly with either the type of macular hole closure or the final BCVA.
Conclusion: PPV and silicone oil tamponade technique promotes successful anatomical and functional outcome in MRDMH. Long-term success is maintained after silicone oil removal. High incidence of silicone oil-induced complications mandate its removal from eyes with successful retinal re-attachment.
Keywords: retinal detachment in high myopia, myopic macular hole, retinal detachment secondary to myopic macular hole, PPV for myopic retinal detachment associated with macular hole
Introduction
Surgical management of myopic retinal detachment associated with macular hole (MRDMH) is an existing dilemma. Gonvers and Machemer in 1982 introduced pars plana vitrectomy (PPV) and partial gas-fluid exchange for management of MRDMH.1 However, several studies using this technique reported variable success rates with considerable discrepancy among authors regarding the validity of the technique to achieve retinal re-attachment and macular hole closure. A plausible explanation is that the technique of Gonvers and Machemer focused on relieving the anteroposterior traction force in the posterior pole rather than addressing the multifactorial etiology of MRDMH, particularly in the subgroup of patients with posterior staphyloma and extensive chorioretinal atrophy. The subsequent inability of the inelastic retina to conform to the concavity of the staphyloma and poor adhesion between the neurosensory retina and the underlying atrophic retinal pigment epithelium (RPE) and choroid were major causes of failure.2–5 Hence, several alternative techniques were introduced for MRDMH, though with no consensus to date among retina surgeons on one optimal surgical approach.6–12 Some authors advocated that a longer term tamponade provided by silicone oil could improve the surgical outcome of MRDMH patients for several reasons. Firstly, silicone oil provides the desired tamponade effect while averting centrifugal overstretch of the inelastic retina around the hole. Overstretch is produced by forcible backward displacement of the retina by the gas bubble with possible enlargement of the hole or compromise of the centripetal movement of photoreceptors to close the hole, subsequently resulting in higher incidence of open macular hole or even iatrogenic enlargement of the hole. Secondly, silicone oil tamponade provides protracted tamponade duration that would increase the odds of retinal re-attachment in the presence of underlying atrophic RPE and choroid by providing a scaffold to stimulate glial proliferation across the hole and allowing time latitude for absorption of sub-retinal fluid. Finally, silicone oil defers prone positioning of the patient that would be otherwise required for a long period of time and entails non-compliance of the patient.2,7,9,13–17 Nevertheless, the issue of using silicone oil mandated defining the appropriate time for its removal to avoid a recurrence of retinal detachment and to avoid silicone-oil induced complications particularly secondary glaucoma. To date, the timing of silicone oil removal is still debated.18–20 In the present study we used PPV and silicone oil tamponade for management of MRDMH and focused on exploring the anatomical and functional outcomes of this technique and its long-term validity after silicone oil removal.
Patients and Methods
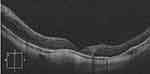
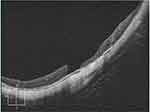
This is a retrospective interventional non-comparative consecutive case series. The study included patients with MRDMH operated on between 2011 and 2015 in a tertiary retina center; Magrabi eye hospital, Tanta, Egypt. The study exclusively recruited patients with high myopia whose axial length measured ≥26 mm and had associated retinal detachment secondary to the macular hole. Exclusion criteria included patients presenting with retinal detachment attributed to pathologies other than high myopia as rhegmatogenous retinal detachment with peripheral breaks, trauma, tractional diabetic disease, or congenital disease as optic pit maculopathy. In addition, the study excluded patients with recurrent retinal detachment after previous scleral buckle surgery or PPV, patients presenting with proliferative vitreoretinopathy grade C, patients with macular disease that would compromise the final best-corrected visual acuity (BCVA) as myopic choroidal neovascular membrane, recruited patients who did not present for silicone oil removal after initial surgery, patients who did not complete at least 3 years of follow-up after silicone oil removal, and patients with dense media opacity, including cataracts, that precluded adequate pre-operative assessment of the macular hole or the retinal periphery. All recruited patients received detailed ophthalmological examination that included slit-lamp anterior segment examination, intra-ocular pressure (IOP) measurement using applanation tonometry, slit-lamp biomicroscopy to determine the presence of a macular hole and associated features of high myopia including posterior staphyloma and chorioretinal atrophic patches, and indirect ophthalmoscopy with 360-degree scleral indentation to exclude the presence of peripheral retinal breaks. We measured BCVA using decimal units and assigned an equivalent of 0.01 and 0.001 decimal units for patients with visual acuity of counting fingers (CF) or hand movement (HM), respectively. BCVA values were later converted to the logarithm of the minimum angle of resolution (logMAR) units for the purpose of statistical analysis. Whenever possible, the presence of a macular hole was confirmed using spectral-domain optical coherence tomography (SD-OCT) imaging (Cirrus HD-OCT 4000; Carl Zeiss Meditech, Inc., Dublin, California, USA). We measured axial length for all patients using optical biometry (Zeiss IOL Master 500; Carl Zeiss Meditech, Inc., Jena, Germany). Main outcome measures were retinal re-attachment and macular hole closure after silicone oil removal, improvement of BCVA, and complications secondary to surgery.
Surgical Technique
A single surgeon (HG) performed all surgical procedures described herein. All patients underwent 23-g PPV. The surgical technique consisted of core vitrectomy, triamcinolone-assisted dissection of posterior hyaloid, and shaving of the vitreous base. Internal limiting membrane (ILM) peel was attempted in all patients assisted by triamcinolone acetonide, however, peel was either not possible or incomplete in most of the cases due to extreme thinning of the retina and difficult visualization due to poor contrast caused by diffuse chorioretinal atrophy. The surgeon performed fluid-air exchange while aspirating sub-retinal fluid through the macular hole using hand-held soft tip cannula mounted on a flute needle under low-infusion pressure. That was followed by injection of silicone oil 5000 cSt; centistokes. Post-operatively, patients had to maintain a face-down position for 10 days. Silicone oil was removed in all patients. The minimum follow-up period prior to silicone oil removal was 5 months. Silicone oil was extracted using a 3-port technique. After removal of the bulk of silicone oil, the surgeon performed multiple fluid lavage of the vitreous cavity through the infusion-extraction ports using the negative suction of the extraction syringe. At the end of the procedure the retinal periphery was inspected to rule out retinal breaks. The post-operative follow-up visits were scheduled at 1 day, 1 week, 1 month, and 3-monthly thereafter. Follow-up examination consisted of assessment of BCVA, IOP, retinal re-attachment and OCT examination for assessment of macular hole closure. U-type macular hole was defined as a closed macular hole with restoration of normal foveal contour. V-type macular hole was defined as a closed macular hole with steep foveal contour. W-type macular hole closure was defined as flattened hole edges against the RPE with no sub-retinal fluid, though with persistent full-thickness defect of the neurosensory retina (open-flat macular hole). Patients who developed recurrent retinal detachment after silicone oil removal underwent repeat surgery with removal of residual epiretinal membranes if any, fluid-air exchange with aspiration of the sub-retinal fluid through the hole and injection of 5000 cSt silicone oil. All patients who underwent repeat surgery completed a minimum of 5-month follow-up period prior to silicone oil removal.
Statistical Analysis
Descriptive analysis was conducted for the patients’ characteristics using: frequencies and percentages for categorical variables; means and standard deviations for normally distributed quantitative variables; and medians, minimums and maximums for non-normal data. Chi square/Fisher’s exact test was used to analyze categorical variables, while One-way ANOVA/Kruskal–Wallis test was used to compare variables across the closure type and complications. Correlations between numerical variables were tested using Spearman correlation. Kaplan–Meier method was used to estimate the event-free survival where it is defined as the duration of follow up or time to recurrence in the cases with events. Analysis was done at significance level of 0.05.
Results
Baseline Characteristics of Study Participants
The study included 26 eyes of 26 patients. Female gender constituted 73% (19 patients) of the study sample. Mean age was 59.5 years (range 29–76 years; SD 11). Mean axial length was 30 mm (range 26–36; SD 2.5). Mean baseline visual acuity was 0.01 decimal units (2 logMAR); range 0.001–0.05; SD 0.01). At baseline, 11 patients (42%) had clear crystalline lens, 11 patients (42%) were pseudophakic, and 4 patients (15%) were aphakic. Mean duration of silicone oil tamponade was 16 months (range 5–30; SD 6.3). Mean follow-up period after silicone oil removal was 63 months (range 37–108; SD 15) (Table 1).
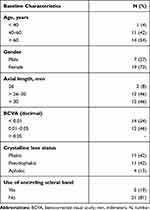 |
Table 1 Baseline Characteristics of Study Participants |
Anatomical Outcome
Primary retinal re-attachment was achieved in 23 eyes (88.4%). Recurrence of retinal detachment occurred in 3 eyes (11.5%) after 16, 26, and 13 months of silicone oil removal, respectively. Recurrence occurred due to re-opening of previously closed macular hole. One eye with U-type closure, another eye with V-type closure, and a third eye with W-type closure. After re-operation, all 3 eyes achieved retinal re-attachment. Final retinal re-attachment rate after silicone oil removal was 100% (Figure 1). W-type macular hole closure occurred in 15 eyes (58%), U-type macular hole closure occurred in 9 eyes (35%), and V-type macular hole closure occurred in 2 eyes (8%) (Figure 2–4). Eleven patients (42%) developed cataracts and eventually required phacoemulsification surgery. Four patients (15%) developed glaucoma that was unresponsive to maximum medical therapy and eventually required filtering surgery.
Functional Outcome
At the end of the follow-up period, BCVA deteriorated in 2 patients (8%), remained stable in 9 patients (35%) and improved in 15 patients (58%). Mean final BCVA was 0.05 decimal units (1.3 logMAR), range 0.001–0.2; SD 0.06. The difference between mean initial and final BCVA was statistically significant, p = 0.004 (Table 2).
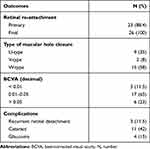 |
Table 2 Anatomical and Functional Post-Operative Outcomes |
Statistical Correlation of Studied Variables
Anatomical Outcome
Statistical analysis revealed that initial BCVA, axial length and duration of silicone oil tamponade did not correlate significantly with the type of macular hole closure, p = 0.7, 0.1 and 0.9, respectively.
Functional Outcome
Statistical analysis revealed that initial BCVA, axial length and duration of silicone oil tamponade did not correlate significantly with final BCVA, p = 0.4, 0.4 and 0.1, respectively.
Discussion
The present study explored the rationale that the durability of silicone oil tamponade would promote successful re-attachment of the retina, closure of the macular hole, and long-term successful outcome after silicone oil removal. These outcomes would be otherwise difficult to achieve due to the inherent weak adhesion between the retina and the choroid in MRDMH patients.2–5 Using this technique we achieved retinal re-attachment and macular hole closure in 88.4% of patients after a single surgery, and in all patients after a second surgery. Our recurrence rate due to re-opening of the macular hole was 11.5% over a mean follow-up period of 5 years after removal of silicone oil. It is worthy of note that 61.5% of our patients had a follow-up period of more than 5 years and 1 patient had a follow-up period of 9 years. Our functional outcome in terms of improvement of BCVA was less notable. Final BCVA improved in 58% of our patients. Though the improvement of vision was statistically significant, the majority of our patients remained within the HM and CF ranges; while only 6 patients (23%) achieved final BCVA ≥ 0.1. Our less favorable visual outcome could be attributed to the W-type closure of the macular hole, which occurred in 58% of patients. In addition, 61.5% of our patients had axial length ≥30 mm with entailed extensive chorioretinal degeneration in the posterior pole. To our knowledge, the follow-up period after removal of silicone oil reported herein, is the longest reported in literature compared to other authors who used a similar technique for management of MRDMH (Table 3). In comparison to our findings, Nishimura et al15 reported 92% retinal re-attachment rate and 55% macular hole closure rate. They reported mean follow-up period of 44.5 months inclusive of 23.3 months mean duration of silicone oil filling. The authors did not comment on the type of macular hole closure. Scholda et al13 reported 100% retinal re-attachment rate. The authors reported a mean follow-up period of 31.6 months inclusive of 155 days mean duration of silicone oil filling. The authors did not comment on the type of macular hole closure. Hong et al9 reported 76.2% and 100% retinal re-attachment rates after primary and repeat surgeries, respectively. Macular hole closure rate was 61.9% after primary surgery and 76.2% after repeat surgery. They reported a mean follow-up period of 24 months inclusive of 8.95 months mean duration of silicone oil filling. The authors did not comment on the type of macular hole closure. Ghoraba et al20 reported retinal re-attachment and macular hole closure in 88.7% of eyes. They had 23 months mean follow-up period after silicone oil removal. All their recurrent cases had flat-open macular hole configuration. Meng et al17 reported retinal re-attachment and macular hole closure in 86% of eyes. After repeat surgery, retinal re-attachment rate improved to 95% but the macular hole closure rate remained the same. The authors reported a mean follow-up period of 22.2 months inclusive of 3–12 months duration of silicone oil filling. Nadal et al12 reported an 85.1% retinal re-attachment rate. The authors reported anatomical macular hole closure and open macular hole configuration in 60.9% and 39.1%, respectively, of those patients who had retinal re-attachment. Overall macular hole closure rate was 51.9%. Mean follow-up period was 12 months inclusive of 119 days mean duration of silicone oil filling. Cheung et al14 reported 83% retinal re-attachment rate and macular hole closure rate after initial surgery and 92% rates after repeat surgery. They reported a mean follow-up period of 12.1 months inclusive of 3–4 months duration of silicone oil filling. The authors did not comment on the type of macular hole closure. Kumar et al21 reported 100% retinal re-attachment rate and macular hole closure rate. They reported a median follow-up period of 8 months inclusive of at least 3 months duration of silicone oil filling. The authors did not comment on the type of macular hole closure. Qian et al18 had a series of 51 eyes for which they performed PPV and silicone oil injection. Forty-one eyes (80.4%) had successful retinal re-attachment. After silicone oil removal, 33 (80.5%) of 41 eyes remained re-attached. Macular hole closure rate was 48.8%. Follow-up duration was at least 6 months inclusive of 4.6 months mean duration of silicone oil filling. The authors did not comment on the type of macular hole closure. Mancino et al22 reported a 54% rate of retinal re-attachment and macular hole closure after initial surgery. Mean follow-up duration was 1 year inclusive of 3 months duration of silicone oil filling. The authors did not comment on the type of macular hole closure. Our results support the rationale of using silicone oil for long-term tamponade in the management of MRDMH to achieve primary retinal re-attachment and to maintain long-term success after silicone oil removal. We acknowledge the long-term complications associated with the use of silicone oil, namely cataract formation and secondary glaucoma. In fact, all phakic patients included in our study required phacoemulsification surgery and 15% of all patients required filtering surgery. However, the risk of irreversible vision loss posed by the nature of the disease provided a plausible argument that these complications were not prohibitive when weighed against the overall initial and long-term anatomical and functional successful outcomes. Limitations of the present study included a small sample size, retrospective design and a lack of concurrent comparison with other modalities for management of MRDMH. These factors limited the statistical power of the study to reveal significant correlations between studied variables. Hence, crucial questions were left unanswered including optimum duration of silicone oil tamponade before removal and correlation between axial length and silicone oil tamponade and anatomical and functional outcomes.
 |
Table 3 Review of Studies on PPV and Silicone Oil Injection for High Myopic Retinal Detachment Associated with Macular Hole |
Conclusion
PPV and silicone oil tamponade technique is effective in promoting successful anatomical and functional outcome in patients with MRDMH. Long-term success is maintained after silicone oil removal. High incidence of silicone oil-induced complications mandate its removal from eyes with successful retinal re-attachment.
Data Sharing Statement
The data collected from history-taking and clinical examination of patients recruited in the current study are confidential. Access to these data is restricted by the Magrabi Eye Hospital in accordance with patients’ data protection policy. These data are available for researchers who meet the criteria for access to confidential data through contacting the medical director, Professor Hammouda Ghoraba, via email at: [email protected].
Statement of Ethics
- The study was approved by the institution review board of Magrabi Eye Hospital, Tanta, Egypt.
- The study adhered strictly to the tenets of the Declaration of Helsinki of 1975 and the revision of 2013.
- The study required that all participants received thorough explanation of the surgical maneuvers entailed, possible outcome and expected complications and signed an informed consent prior to enrollment. The consent included a statement that authorized the authors to publish patients’ data for research purposes in an anonymous manner that does not allow identification of the patient.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Gonvers M, Machemer R. A new approach to treating retinal detachment with macular hole. Am J Ophthalmol. 1982;94:468–472. doi:10.1016/0002-9394(82)90240-9
2. Ichibe M, Yoshizawa T, Murakami K, et al. Surgical management of retinal detachment associated with myopic macular hole: anatomical and functional status of the macula. Am J Ophthalmol. 2003;136:277–284. doi:10.1016/S0002-9394(03)00186-7
3. Panozzo G, Mercanti A. Optical coherence tomography findings in myopic traction maculopathy. Arch Ophthalmol. 2004;122:1455–1460. doi:10.1001/archopht.122.10.1455
4. Shimada N, Tanaka Y, Tokoro T, Ohno-Matsui K. Natural course of myopic traction maculopathy and factors associated with progression or resolution. Am J Ophthalmol. 2013;156:948–957. doi:10.1016/j.ajo.2013.06.031
5. Gaucher D, Haouchine B, Tadayoni R, et al. Long-term follow-up of high myopic foveoschisis: natural course and surgical outcome. Am J Ophthalmol. 2007;143:455–462. doi:10.1016/j.ajo.2006.10.053
6. Ripandelli G, Coppé AM, Fedeli R, Parisi V, D’Amico DJ, Stirpe M. Evaluation of primary surgical procedures for retinal detachment with macular hole in highly myopic eyes. A randomized comparison of vitrectomy versus posterior episcleral buckling surgery. Ophthalmology. 2001;108:2258–2265. doi:10.1016/S0161-6420(01)00861-2
7. Ghoraba HH, Mansour HO, El Gouhary SM. Effect of 360° episcleral band as adjunctive to pars plana vitrectomy and silicone oil tamponade in the management of myopic macular hole retinal detachment. Retina. 2014;34:670–678. doi:10.1097/IAE.0b013e3182a487ea
8. Mete M, Alfano A, Guerriero M, et al. Inverted internal limiting membrane flap technique versus complete internal limiting membrane removal in myopic macular hole surgery. A comparative study. Retina. 2017;37:1923–1930. doi:10.1097/IAE.0000000000001446
9. Hong N, Huang B, Tong J. Primary silicone oil tamponade and internal limiting membrane peeling for retinal detachment due to macular hole in highly myopic eyes with chorioretinal atrophy. BMC Ophthalmol. 2015;15:165–172. doi:10.1186/s12886-015-0154-4
10. Ando F, Ohba N, Touura K, Hirose H. Anatomical and visual outcomes after episcleral macular buckling compared with those after pars plana vitrectomy for retinal detachment caused by macular hole in highly myopic eyes. Retina. 2007;27:37–44. doi:10.1097/01.iae.0000256660.48993.9e
11. Ma J, Li H, Ding X, Tanumiharjo S, Lu L. Effectiveness of combined macular buckle under direct vision and vitrectomy with ILM peeling in refractory macular hole retinal detachment with extreme high axial myopia: a 24-month comparative study. Br J Ophthalmol. 2017;101:1386–1394. doi:10.1136/bjophthalmol-2016-310123
12. Nadal J, Verdaguer P, Canut MI. Treatment of retinal detachment secondary to macular hole in high myopia. Vitrectomy with dissection of the inner limiting membrane to the edge of the staphyloma and long-term tamponade. Retina. 2012;32:1525–1530. doi:10.1097/IAE.0b013e3182411cb8
13. Scholda C, Wirtitsch M, Biowski R, Stur M. Primary silicone oil tamponade without retinopexy in highly myopic eyes with central macular hole detachments. Retina. 2005;25:141–146. doi:10.1097/00006982-200502000-00004
14. Cheung BTO, Lai TYY, Yuen CYF, Lai WWK, Tsang CW, Lam DSC. Results of high-density silicone oil as a tamponade agent in macular hole retinal detachment in patients with high myopia. Br J Ophthalmol. 2007;91:719–721. doi:10.1136/bjo.2006.111526
15. Nishimura A, Kimura M, Saito Y, Sugiyama K. Efficacy of primary silicone oil tamponade for the treatment of retinal detachment caused by macular hole in high myopia. Am J Ophthalmol. 2011;151:148–155. doi:10.1016/j.ajo.2010.07.023
16. Xie A, Lei J. Pars plana vitrectomy and silicone oil tamponade as a primary treatment for retinal detachment caused by macular holes in highly myopic eyes: a risk-factor analysis. Curr Eye Res. 2013;38(1):108–113. doi:10.3109/02713683.2012.722742
17. Meng L, Wei W, Li Y, Han X, Shi X, Yang M. Treatment of retinal detachment secondary to macular hole in highly myopic eyes. Pars plana vitrectomy with internal limiting membrane peel and silicone oil tamponade. Retina. 2014;34:470–476. doi:10.1097/IAE.0b013e31829d004b
18. Qian J, Jiang YR. Anatomic evaluation of macular holes with silicone oil tamponades in highly myopic eyes using optical coherence tomography. Eur J Ophthalmol. 2010;20(5):938–944. doi:10.1177/112067211002000520
19. Ortisi E, Avitabile T, Bonfiglio V. Surgical management of retinal detachment because of macular hole in highly myopic eyes. Retina. 2012;32:1704–1718. doi:10.1097/IAE.0b013e31826b671c
20. Ghoraba HH, Elgouhary MS, Mansour HO. Silicone oil reinjection without macular buckling for treatment of recurrent myopic macular hole retinal detachment after silicone oil removal. J Ophthalmol. 2014;2014:1–5. doi:10.1155/2014/434272
21. Kumar A, Tinwala S, Gogia V, Sinha S. Clinical presentation and surgical outcomes in primary myopic macular hole retinal detachment. Eur J Ophthalmol. 2012;22(3):450–455. doi:10.5301/ejo.5000012
22. Mancino R, Ciuffoletti E, Martucci A, et al. Anatomical and functional results of macular hole retinal detachment surgery in patients with high myopia and posterior staphyloma treated with perfluoropropane gas or silicone oil. Retina. 2013;33:586–592. doi:10.1097/IAE.0b013e3182670fd7
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.