Back to Journals » International Journal of Women's Health » Volume 10
Intrapartum ultrasound: viewpoint of midwives and parturient women and reproducibility
Authors Van Adrichem A , Faes E, Kinget K , Jacquemyn Y
Received 2 November 2017
Accepted for publication 15 March 2018
Published 6 June 2018 Volume 2018:10 Pages 251—256
DOI https://doi.org/10.2147/IJWH.S155865
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Elie Al-Chaer
Adrielle Van Adrichem,1 Ellen Faes,1 Kristof Kinget,2 Yves Jacquemyn1
1Antwerp University Hospital UZA, Antwerp University UA – ASTARC, Edegem, Belgium; 2KLINA Hospital, Brasschaat, Belgium
Introduction: Vaginal examination (VE) is known to be subjective in interpretation and is considered uncomfortable by many women. Intrapartum ultrasound aims to be more objective and less invasive. The purpose of this study was to evaluate the acceptability of introducing intrapartum ultrasound to both midwives and parturients. Furthermore, we wanted to evaluate the reproducibility of different measurements when introduced de novo among operators without prior ultrasound experience.
Subjects and methods: This study determined intra- and interobserver variability of intrapartum ultrasound in nulliparous women in labor. Ultrasound examinations were performed independently by a midwife and a gynecologist. The symphysis–head distance (SHD) and the angle of progression (AOP) were measured by translabial ultrasound. Structured questionnaires were given to midwives and parturients. Intraclass correlation coefficient (ICC) and limits of agreement (LA) were calculated to evaluate variability.
Results: A total of 33 patients were included; of whom, 28 filled in the questionnaire. A total of 19 midwives working on a delivery ward were asked to respond to the questionnaire, and 13 returned the forms. Midwives clearly continued to prefer VE over ultrasound, the majority evaluated translabial ultrasound as easy to use, but some declared to be unable to use it. The majority of patients, 71%, preferred ultrasound over VE. Reproducibility of intrapartum translabial ultrasound was good; ICC for interobserver variability was 0.603 (p=0.001) for SHD, and ICC for intraobserver variability was 0.844 (p<0.001) and 0.914 (p<0.001) for SHD and AOP, respectively.
Conclusion: Patients prefer ultrasound over VE; midwives tend to stick to trusted VE. Reproducibility of intrapartum ultrasound in non-experienced operators is good.
Keywords: intrapartum, ultrasound, labor
Introduction
For centuries, progression of labor has been evaluated by vaginal examination (VE), describing dilation, effacement, consistency and position of the cervix and descent of the fetal head. Interobserver variability of VE is large, and it is a traditional but unreliable method.1–4 Furthermore, the vaginal examination can be experienced as intimidating and uncomfortable by a woman in labor. In recent years, intrapartum ultrasound has become increasingly popular. During labor, ultrasound can be performed by transabdominal, translabial and transperineal way. Measurements for dilation, effacement, position and descent of the fetal head have been developed.2,3,5,6 Ultrasound during labor has been proven to be able to predict labor outcomes in primiparous women with prolonged first stage of labor.7 Moreover, intrapartum ultrasound evaluation is superior to VE in terms of identifying the correct fetal head position.4 The symphysis–head distance (SHD) and the angle of progression (AOP) have been the most studied measurements by transperineal ultrasound.7–10
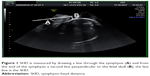
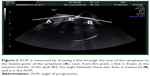
The SHD is the distance between the under border of the symphysis to the fetal skull measured perpendicular to the axis of the symphysis (Figure 1). This distance has been shown to be predictive for the outcome of labor,8 its measurement has been described as reproducible and a negative correlation exists with the AOP.6 The AOP is the angle between the axis of the symphysis and the line drawn from the under border of the symphysis tangential to the fetal skull (Figure 2). This angle is considered a reproducible indicator to evaluate fetal descent during labor.9,11
Studies that have compared ultrasound and VE have repeatedly demonstrated ultrasound to be more accurate; patients experience ultrasound as less invasive and less painful.1,2,4
In some countries, ultrasound during pregnancy and labor is performed by midwives; in Belgium, ultrasound is not part of midwife competencies. The aim of this study was to examine the acceptability of parturients and the viewpoint of the midwife when introducing intrapartum ultrasound. Furthermore, we evaluated the intra- and interobserver variability of intrapartum sonographic measurements performed by midwives without ultrasound experience.
Subjects and methods
Women and midwives were recruited from an academic (Antwerp University Hospital, Universitair Ziekenhuis Antwerpen) and a nonacademic (Klinieken Noord Antwerpen Hospital) maternity department. The study was approved by the ethics committee of both institutions. Written informed consent was obtained from women during labor and from midwives performing the ultrasound.
End points are inter- and intra-observer variability and acceptability by parturients and midwives. A convenience sample was used. Women included were nulliparous in spontaneous labor, with a singleton term pregnancy and cephalic presentation.
Ultrasound was performed with the machine as available on the delivery ward, Voluson P6, with convex 4C-RS transducer (GE Medical Systems, Zipf, Austria) in UZA and Aloka Prosound Alpha 6 and with convex UST-9115-5 transducer (Hitachi Ltd., Tokyo, Japan) in KLINA.
Measurements were standardized and performed by translabial way. All midwives who took part in the study received a 1-hour training consisting of a slideshow presentation and one supervised measurement. Engagement of the head differed between parturients between Hodge 2 and 3. Urinary bladder was emptied before measurement. Ultrasound gel was placed on the transducer that was then covered by a glove; gel was put on the glove. The patient was put in a semi-recumbent position with legs flexed. The transducer was placed in a midsagittal plane, and the fetal skull and maternal symphysis were visualized.
To evaluate the interobserver variability, two operators performed measurements independently, and they had no access to the measurement of the other. To estimate the intraobserver variability, one operator performed three repetitive measurements.
Symphysis–head distance (SHD) was performed as described by Youssef et al8 The distance from the under border of the symphysis to the fetal skull was measured perpendicular to the length axis of the symphysis (Figure 1). The AOP was defined as the angle between the length axis of the symphysis and a line from the inferior border of the symphysis tangential to the fetal skull (Figure 2).
Acceptability of ultrasound examination for women in labor was tested by presenting statements to the patients, at least 2 hours after delivery. For each statement, the possible answers were as follows: strongly agree, agree, neutral, disagree and strongly disagree, resulting in a 5-point Likert score. For each ultrasound, a written informed consent was signed. Patients who entered neutral for VE did not remember if an explicit informed consent was asked, but they did not feel forced to undergo the examination in any way.
Statements were subdivided into categories, concerning VE (12 statements, eg, I experienced the vaginal examination as being painful), translabial ultrasound (14 statements, eg, I experienced this ultrasound as painful) and the conditions under which the examination was performed (five statements, eg, during ultrasound examination, I prefer my partner to be in the same room). The questionnaire was based on similar studies on vaginal ultrasound.12,13 In addition, a Visual Analog Score for pain during the examination was performed. Pain scores were evaluated at rest (between uterine contractions) and were compared with the pain scores of previous VE (with or without epidural anesthesia).
A similar questionnaire was developed for the midwives including 18 statements on ultrasound technique (eg, the technique was easy to learn for me) and 11 statements concerning vaginal examination versus translabial ultrasound (eg, vaginal examination provides more clear results than ultrasound). The questionnaire was based on a similar example.14
SPSS 24.0 (IBM Corporation, Armonk, NY, USA) was used for statistical analysis. Interobserver and intraobserver variability was examined using intraclass correlation coefficient (ICC; two-way mixed absolute agreement single measures). ICC>0.70 is considered good correlation; ICC<0.3 is reported as low correlation and ICC between 0.5 and 0.7 are scored as moderate correlation.15 To visualize results, Bland–Altman plots and limits of agreement (LA) have been used.
To analyze acceptability, the 5-point Likert scale was coded in three groups: agree, neutral, not agree. Fisher’s exact test was performed with p<0.05 accepted as significant. Wilcoxon signed-rank test was used for the comparison of Visual Analog Score results between groups.
Results
A total of 19 midwives received the training for intrapartum ultrasound, of these 11 midwives actually performed the examinations and filled in the questionnaire. Table 1 presents characteristics of this population. From the 33 included women, three were excluded because ultrasound imaging was not performed according to the protocol. It was possible to measure AOP in every patient, and SHD was not measured in four patients because the fetal head did not yet reach to the under border of the symphysis.
  | Table 1 Characteristics of study population |
Questionnaires were given to 33 women in labor, the questionnaires were always given after the ultrasound examinations and 28 women returned the questionnaire. All 19 midwives who received the training also received the questionnaire for midwives, and 13 returned the questionnaire.
Table 2 presents the ICCs for interobserver variability, and Figures 3 and 4 illustrate Bland–Altman plots for interobserver variability. Table 3 presents ICCs for intraobserver variability.
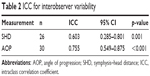  | Table 2 ICC for interobserver variability |
  | Figure 3 Bland–Altman plot for interobserver variability between two observers for SHD. |
  | Figure 4 Bland–Altman plot for interobserver variability for AOP. |
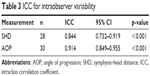  | Table 3 ICC for intraobserver variability |
A total of 20 of the 28 patients (71.4%) preferred intrapartum ultrasound over VE; the other eight patients (28.6%) had no preference. Table 4 presents the results of the different statements concerning women in labor.
  | Table 4 Answers by women in labor on statements concerning VE and translabial ultrasound |
Table 5 presents the answers to the statements that were given to the midwives who have been performing ultrasound for this study. The majority of midwives considered ultrasound as easy to use (63.7%) with an advantage for the patient. As to be expected, midwives who have been in practice for several years felt more at ease with VE as compared with intrapartum ultrasound after minimal training.
  | Table 5 Answers to statements on VE and translabial ultrasound by midwives |
Discussion
Concerning interobserver variability after minimal training in intrapartum ultrasound as in this study, moderate agreement between measurements was reached for SHD. For AOP, a good agreement between different observers could be reached. The results that have been published in previous studies were conflicting and mainly obtained with observers who had previous ultrasound experience. The study by Duckelmann et al9 presented an ICC of 0.72, comparable to our results. In the same study, it was examined whether a difference in previous ultrasound experience influenced variability. Observers with more experience demonstrated larger ICC and a smaller confidence interval, and this was confirmed in other studies.16 In addition, the presence of uterine contractions can influence differences in the ICC.8,17
Intraobserver variability in our study is good for both SHD and AOP, and the results are comparable to those from other studies.16
When preparing this study, it became clear that midwives in the Belgian context of not receiving any formal ultrasound training during training are not very motivated to introduce intrapartum ultrasound in their practice. Although the majority of midwives declare not to be able to perform intrapartum ultrasound autonomously and correctly (72.7%); at the same moment, they considered the technique easy to use and perform. Almost all midwives have experienced learning intrapartum ultrasound as an agreeable expansion of their activities. Midwives do find ultrasound an advantage for the patients but not for themselves. This discrepancy and the lack of personal advantage can hinder the introduction of intrapartum ultrasound in clinical practice.
Women in labor seem to prefer the noninvasive translabial intrapartum ultrasound over VE; the difference in pain between both types of examination is remarkable resulting in a significantly different visual analog pain score. To the best of our knowledge, this is the first study that compares women’s experiences of digital VE with translabial ultrasound; all previous studies have compared VE with transvaginal ultrasound.12
A major bias of this study is that the technique that midwives have been using for several years in daily work, and feel very much at ease with, is compared with something they have learned very recently and in a very short time. To introduce intrapartum ultrasound in daily midwifery practice, one needs more than a short training. Eventual advantages for women in labor have to be put against getting used to new technical skills.
Conclusion
This small study demonstrates acceptable intra- and interobserver variability for both SHD and AOP. Women in labor seem to prefer translabial ultrasound over VE; more: intensive training of midwives will allow for eventual introduction of intrapartum ultrasound in clinical practice. Intrapartum ultrasound for the evaluation of labor progress could be a supplementary tool for active management and may reduce the use of unnecessary VE during labor and improves obstetric and neonatal outcomes. This study can be considered as a preliminary study; a larger prospective study is needed to verify our results.
Disclosure
The authors report no conflicts of interest in this work.
References
Benediktsdottir S, Eggebo TM, Salvesen KA. Agreement between transperineal ultrasound measurements and digital examinations of cervical dilatation during labor. BMC Pregnancy Childbirth. 2015;15:273. | ||
Hassan WA, Eggebo TM, Ferguson M, Lees C. Simple two-dimensional ultrasound technique to assess intrapartum cervical dilatation: a pilot study. Ultrasound Obstet Gynecol. 2013;41(4):413–418. | ||
Debska M, Kretowicz P, Debski R. Intrapartum sonography – eccentricity or necessity? J Ultrason. 2015;15(61):125–136. | ||
Akmal S, Kametas N, Tsoi E, Hargreaves C, Nicolaides KH. Comparison of transvaginal digital examination with intrapartum sonography to determine fetal head position before instrumental delivery. Ultrasound Obstet Gynecol. 2003;21(5):437–440. | ||
Malvasi A, Giacci F, Gustapane S, Sparic R, Barbera A, Tinelli A. Intrapartum sonographic signs: new diagnostic tools in malposition and malrotation. J Matern Fetal Neonatal Med. 2016;29(15):2408–2413. | ||
Erlik U, Wolman I. Intrapartum sonographic assessment of labor. J Obstet Gynaecol India. 2013;63(5):297–300. | ||
Torkildsen EA, Salvesen KA, Eggebo TM. Prediction of delivery mode with transperineal ultrasound in women with prolonged first stage of labor. Ultrasound Obstet Gynecol. 2011;37(6):702–708. | ||
Youssef A, Maroni E, Ragusa A, et al. Fetal head-symphysis distance: a simple and reliable ultrasound index of fetal head station in labor. Ultrasound Obstet Gynecol. 2013;41(4):419–424. | ||
Duckelmann AM, Bamberg C, Michaelis SA, et al. Measurement of fetal head descent using the ‘angle of progression’ on transperineal ultrasound imaging is reliable regardless of fetal head station or ultrasound expertise. Ultrasound Obstet Gynecol. 2010;35(2):216–222. | ||
Chan YT, Ng VK, Yung WK, Lo TK, Leung WC, Lau WL. Relationship between intrapartum transperineal ultrasound measurement of angle of progression and head-perineum distance with correlation to conventional clinical parameters of labor progress and time to delivery. J Matern Fetal Neonatal Med. 2015;28(12):1476–1481. | ||
Levy R, Zaks S, Ben-Arie A, et al. Can angle of progression in pregnant women before onset of labor predict mode of delivery? Ultrasound Obstet Gynecol. 2012;40(3):332–337. | ||
Bennett CC, Richards DS. Patient acceptance of endovaginal ultrasound. Ultrasound Obstet Gynecol. 2000;15(1):52–55. | ||
Lewin D, Fearon B, Hemmings V, Johnson G. Women’s experiences of vaginal examinations in labour. Midwifery. 2005;21(3):267–277. | ||
de Veer AJE, Francke AL. Ervaringen van Verpleegkundigen en Verzorgenden met Nieuwe Technologieën in de Zorg [Experiences of nurses with new technologies]. Utrecht: NIVEL; 2009. Dutch. | ||
Alessi J, Verhagen A. Evidence Based Diagnostiek van het Bewegingsapparaat [Evidence based diagnosis of the musculoskeletal system]. Springer, Berlin; 2014:178. Dutch. | ||
Molina FS, Terra R, Carrillo MP, Puertas A, Nicolaides KH. What is the most reliable ultrasound parameter for assessment of fetal head descent? Ultrasound Obstet Gynecol. 2010;36(4):493–499. | ||
Ghi T, Maroni E, Youssef A, et al. Sonographic pattern of fetal head descent: relationship with duration of active second stage of labor and occiput position at delivery. Ultrasound Obstet Gynecol. 2014;44(1):82–89. |
 © 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.