Back to Journals » Risk Management and Healthcare Policy » Volume 14
Impact of COVID-19 Pandemic on Healthcare Professionals and Oral Care Operational Services: A Systemic Review
Authors Bordea IR, Candrea S, Sălăgean T, Pop ID, Lucaciu O, Ilea A , Manole M, Băbțan AM , Sirbu A, Hanna R
Received 29 September 2020
Accepted for publication 3 December 2020
Published 4 February 2021 Volume 2021:14 Pages 453—463
DOI https://doi.org/10.2147/RMHP.S284557
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Marco Carotenuto
Ioana Roxana Bordea,1,* Sebastian Candrea,2,* Tudor Sălăgean,3 Ioana Delia Pop,3 Ondine Lucaciu,1 Aranka Ilea,1 Marius Manole,4 Anida-Maria Băbțan,1 Adina Sirbu,1 Reem Hanna5,6
1Department of Oral Rehabilitation, “Iuliu Hațieganu” University of Medicine and Pharmacy Cluj-Napoca, Cluj-Napoca, Romania; 2Department of Pedodontics, County Hospital Cluj-Napoca, Cluj-Napoca, Romania; 3Department of Land Measurements and Exact Sciences, University of Agricultural Sciences and Veterinary Medicine Cluj-Napoca, Cluj-Napoca, Romania; 4Department of Dental Propaedeutics and Esthetics, Iuliu Hatieganu University of Medicine and Pharmacy, Cluj Napoca, Romania; 5Department of Surgical Sciences and Integrated Diagnostics, Laser Therapy Centre, University of Genoa, Genoa, Italy; 6Department of Oral Surgery, Dental Institute, King’s College Hospital NHS Foundation Trust, Denmark Hill, London, UK
*These authors contributed equally to this work
Correspondence: Tudor Sălăgean Tel +40744707371
Email [email protected]
Abstract: The unprecedented climate of the COVID-19 pandemic has some restrictions on oral care operational services, which heavily impacted the delivery of aerosol generating procedures (AGPs). This led the health authorities to set up guidelines and policies that should be followed to minimize the virus spread and ensure safe and effective dental care delivery. This systemic review aimed to evaluate the current guidelines and strategies in providing safe dental services and ensuring efficacy of the current universal personal preventive and protective measures, as well the impact that this outbreak might have on practicing the dental profession in full scope. The review focus questions were as follows: are the current guidelines and measures in literature mitigated enough to ensure safe and effective oral care delivery to patients during the COVID-19 pandemic? Is it possible to highlight the essential and fundamental cross-infection control measures and policies? Twenty articles were chosen out of 180,248 after the inclusion and exclusion criteria were applied in the period between January 1st and August 1st 2020. Our results highlighted effective safety measures that can be implanted in protecting healthcare professionals and patients and ensuring optimal dental care delivery in a safe and healthy environment, taking into consideration the risk assessment and management of AGPs. In conclusion, informative updated standardized policies and protocols are required when more knowledge on the virus behavior keeps evolving. Moreover, there is a need for evidence-based protective measures to be modified on a regular basis to be followed, until a safe vaccine is produced.
Keywords: COVID-19, risk assessment, cross-infection control, diagnostic tests, dental care emergency guidelines, disinfectants, public health, aerosol generating procedures, airborne, healthcare personnel protection
Highlights
1. Risk assessment and preventive measures in minimizing SARS-CoV-2 virus transmission are essential to protect professional healthcare workers and patients.
2. Justifiable measures to ensure effective and safe oral care delivery during the COVID-19 pandemic should be employed and revised as the knowledge on virus transmission is evolving.
3. Urgent need to conduct research studies to identify strategies of minimizing virus transmission in a dental practice setting and establish a framework and effective method to detect the virus in saliva.
4. Utilization of various treatment modalities such as laser-assisted therapy to minimize aerosol exposure during dental procedures.
Introduction
A wave of acute pneumonia emerged in Wuhan City of China in December 2019. It was confirmed that the emergence of this respiratory disease is from a novel coronavirus (SARS-CoV-2). On March 12th 2020, the World Health Organization (WHO) declared the outbreak of this virus a “global pandemic”.1 Coronaviruses (CoV) belong to a large family of viruses (Coronaviridae), which are mRNA in structure with glycoprotein cover and a spike protein on the surface.2
Coronavirus disease 2019 (COVID-19, nCoV-2019) is a novel recognized disease governed by a zoonotic virus which mutates, allowing human pathogenicity with a high predilection to the upper respiratory tract (URT).1 There are four phenotypes of coronavirus strains (α-CoV, β-CoV, γ-CoV, and δ-CoV) in which most of them can cause illness in vertebrates. Despite the current evidence suggesting that γ-CoV and δ-CoV can be found in birds, they can also infect mammals, including humans. These strains mainly affect the URT, gastrointestinal tract (GIT) and central nervous system (CNS).3,4 On the other hand, the novel 2019 coronavirus (SARS-CoV-2) is part of the β-CoV family, as are SARS-CoV (severe acute respiratory syndrome coronavirus) and MERS-CoV (Middle East respiratory syndrome coronavirus), which have claimed human fatalities reported from 2001–2003 and 2012–2014 respectively.5,6
The literature has stated that approximately 70% of the new pathogens that affect humans originated from animals and also are RNA viruses, due to their high mutation rate and potential genetic changes.7 The latter is related to a genetic recombination in positive-sense RNA viruses and a reassortment in RNA viruses with segmented genomes. Among these viruses with high impact on human life are as follows: SARS-CoV, influenza virus and human immunodeficiency virus (HIV).7 SARS-CoV-2 has a typical coronavirus structure with a “spike protein” (S protein) on the membrane envelope and also expresses other proteins such as polyproteins, nucleoproteins and membrane proteins.8,9 The S protein has the ability to connect at the receptor level in the host body to facilitate viral access to specific cells, which can encounter a variety of amino acids. However, SARS-CoV-2 specifically targets angiotensin converting enzyme 2 (ACE2) where it connects. On this note, ACE2 plays a big role in facilitating this connection, otherwise this type of virus is disabled.8 This concept is sustained by the fact that the serum derived from ACE2-Ig antibody that is provided by treated SARS-Cov patients can inhibit the SARS-Cov-2 infection. The epithelial cells of the oral cavity, URT and salivary ducts are very rich in ACE2, thus making them very susceptible to SARS-Cov-2 infection.8
The resemblance between the receptor-binding domain (RBD) of S protein in SARS-Cov-2 and SARS-Cov is more than 76%, whereas the genomic characteristic of SARS-Cov-2 has four amino acids at the fusing point of the S1 and S2 subunits of the S protein. At this site, the furin or other proteases can produce a cleavage between S1 and S2.10
Virus Transmission Routes and Diagnostic Tools
The transmission routes and effective diagnostic tests of COVID-19 are constantly receiving great attention from healthcare workers and scientists. The potential modes of transmission of nCoV-2019 [Coronavirus Disease 2019 [COVID-19)] can be either by direct contact, as a result of a cough or a sneeze with droplets [(Flügge’s droplets), greater than 5 μm in diameter] produced by an infected individual at close proximity (less than 1 m)11, or indirect contact when the patient becomes in contact with infected surfaces and then touches the mouth, nose or eye where the virus is ultimately transmitted through these gates to reach the URT.12,13 Asymptomatic patients who are either in the incubation period or in the recovery phase are considered an uncertain threat in spreading the virus.8,14 In this context, it has been estimated that the virus incubation period is between 5 and 6 days, but the evidence is currently adopting the 14 days policy for medical observation and quarantine of the exposed subjects.15 On this note, the clinical presentations of COVID-19 patients range from asymptomatic to severely symptomatic, in which fever and dry cough are considered mild and where dyspnea is associated is considered moderate to severe. Additionally, atypical symptoms have been reported such as fatigue, muscle pain, confusion, headache, sore throat, diarrhea and vomiting.16
Currently, the universal approaches to COVID-19 containment and prevention or reduction of the risks of transmission are as follows: control the source of infection, employ cross-infection control measures, build up capacity to provide an early diagnostic test to detect the virus, isolate the suspected subject and provide healthcare for the affected patients.17 In this context, all dental healthcare professionals strive to provide high-quality dental care under the current unprecedented challenges. However, due to the virus contagiosity and close proximity of oral healthcare providers to the patients during aerosol generating procedure (AGP) delivery, a structured framework and guidelines for operational dental care provision are required to manage the patients safely and equally to protect the dental healthcare workers. Unfortunately, the current information in the literature on this matter is scarce mainly due to a very short time span between the unprecedented virus outbreaks and the time when it was declared epidemic, because knowledge on this new virus is regularly revolving and ultimately the fact that this virus has shown its growth is exponential not linear. The present systemic review aimed to evaluate the current guidelines and strategies in providing dental care safely and review the efficacy of current universal personal protective measures.
Materials and Methods
The search strategy was performed on PubMed and Google Scholar databases, according to the Preferred Reporting Items of Systematic Reviews and Meta-analysis (PRISMA),18 using the following key words: COVID-19; risk assessment; cross-infection control; diagnostic tests; dental care emergency guidelines; disinfectants; public health; aerosol generating procedures; airborne; healthcare personnel protection.
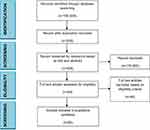
Initially, a total of 15,000 articles were extracted from PubMed and 165,000 papers identified in Google Scholar. The inclusion criteria were based on full text articles published in the English language between January 1st and August 1st 2020, whereas the exclusion criteria were related to MERS-CoV or SARS-CoV, as well as papers published in other languages (not English). Additionally, articles that have been breveted and mentioned on the Google Scholar database were excluded. After the inclusion criteria were applied, 8 papers from the PubMed database and 61 papers from Google Scholar database were included in this systematic review. These 69 articles were subjected to further rigorous analysis, in which only those papers on novel coronavirus and its impact on dentistry were considered. After a thorough and extensive analysis, 20 papers (2 in PubMed, 15 in Google Scholar, and 3 in both PubMed and Google Scholar) were included in this investigation. PRISMA selection criteria identified the source of the selected articles (Figure 1). Two authors performed this formal screening independently (IRB and SC). Any disagreement or discrepancy over the eligibility of particular studies was resolved through discussion with a third author (OL).
The Focused Question
Are the current guidelines and measures in literature mitigated enough to ensure safe and effective oral care delivery to patients during the COVID-19 pandemic? Furthermore, is it possible to highlight the essential and fundamental cross-infection control measures and policies?
Results and Discussions
General dental practitioners (GDPs) and other healthcare professionals in any dental practice setup are subjected to a possibility of contracting the SARS-CoV-2 virus during close contact with suspected/infected patients while performing AGPs, if full personal protective equipment (PPE) is not utilized.19 The AGPs produce airborne particles which are known to increase the potential of contracting the virus. This presents unique challenges among healthcare professionals. A report by Azarpazhooh et al encouraged the use of a high-resolution videoscope during endodontic treatment, whilst the use of goggles or face shields when using a dental operating microscope (DOM) and loupes is less comfortable.20 The overall clinical environment during this unprecedented time can be considered a hazard during the patient’s journey seeking dental care. Inappropriate handling and disposing of the clinical and non-clinical waste are considered another source of virus transmission. It is important also to note that the air of the dental clinic room is a potential route of virus transmission if a proper ventilation protocol is not implemented. Therefore, the dental practice needs to set up and implement robust cross-infection control policies and strategic operating guidelines.19
Dental Procedures and Dental Care Service Delivery versus Framework and Guidelines for Cross-Infection Control
The American Dental Association (ADA) during the national alert status has decreed that only emergency dental care should be delivered via telephone consultation with or without the need for an appropriate medication prescription based on the dentist’s clinical judgment.21 Non-steroidal anti-inflammatory drugs (NSAIDs), paracetamol and opioids are used in dentistry to alleviate pain. It is important to note that the majority of opioids can enhance the viral pathogenesis by modulating the immune responses,22 but the current evidence is very weak.23 The ADA has suggested that the emergency dental procedures should be performed as minimally invasive as possible. Thus, bleeding, severe infections and trauma should be treated in dental units, according to ADA recommendations.20 Llisted below are the dental conditions that are considered either as an emergency or a non-emergency according to the ADA:
Emergency Dental Conditions20
1. Pulpal inflammation, resulting in pain.
2. Inflammation of tissue surrounding an impacted third molar (pericoronitis).
3. Postoperative osteitis or dry socket dressing changes.
4. Localized pain associated with swelling as a result of localized abscess or localized infection.
5. Pain or soft tissue trauma, as a result of a broken tooth.
6.Dental traumatology related to an avulsed/luxated tooth.
7. Loss of temporary restoration, as a result of soft tissue trauma or a broken tooth.
Non-Emergency Dental Conditions20,21
1. Initial or regular oral examinations and follow-up appointments with or without routine radiographs.
2. Regular hygienist appointment (scaling and root planning) and other preventive therapies.
3. Orthodontic treatments other than those to address acute issues (eg, pain, infection, trauma).
4. Elective tooth removal procedures.
5. Restorative treatments related to asymptomatic carious teeth or crown preparation.
6. Aesthetic dental treatments.
Nonetheless, any other dental treatments that require a face-face approach without generating aerosol should be managed as minimally invasive as possible (Figure 2). These measures are placed to support the emergency departments and designated hot hub centers by triaging patients and reducing the workloads.21
 |
Figure 2 Patient screening and triage process. Notes: Data from Peng et al.8 The red arrow indicates that the suspected patient should be referred to emergency units for treatment. |
A report by Peng et al8 suggested basic patients’ selection criteria, representing a set of questions, which are correlated to the patient’s body temperature (Appendix 1). These questions were formulated to address whether patients have come in contact with the virus, which must be based on displayed symptoms and travel history to epicenters. In this context, Figure 3 shows the relationship between the body temperature and patient’s triage accordingly, taking into consideration the screening questions in Appendix 1.8 This patients’ selection criteria questionnaire concept is based on fever displayed symptoms. This was supported by Ather et al confirming that the contents of this questionnaire reveal important facts such as patient contacts with confirmed SARS-CoV-2 individuals or recent travel to the virus epicenter or presented with respiratory symptoms like SARS-CoV-2, taking into consideration a body temperature exceeding 38 °C.24 Ultimately, this provides the dentist with a vital platform for decision-making on whether to treat the patient, noting the urgency of the treatment. Alharbi et al and co-workers have established guidelines based on grouping the patients, rendering the patients’ status (symptoms at presentation) and the need for treatment, reflecting on the risks and benefits. This strategic approach would assist in triaging the patients and providing dental care accordingly.25
 |
Figure 3 Modified patient triage process which is based on body temperature and screening questions (Appendix 1). Notes: Adapted from Peng X, Xu X, Li Y et al Transmission routes of 2019-nCoV and controls in dental practice. Int J Oral Sci. 2020;12:9, 10.1038/s41368-020-0075-9. Creative Commons Attribution 4.0 International License; http://creativecommons.org/licenses/by/4.0/8. |
During the COVID-19 pandemic, whenever there is a risk of airborne transmission due to AGPs, PPE gear including filtering face-piece [FFP3 (class 3)] respirators is mandatory and strategic cross-infection control protocols should be implemented.26 According to Peng et al,8 the hand-wash hygiene framework is based on “two times before and three times after“. The hand hygiene guideline is as follows: prior to and after patient’s examination and treatment, after contact with all of the contaminated surfaces or equipment or body fluids (blood, saliva, secretions, excreta) or skin wound.8 A report suggested that patients of unknown virus status (asymptomatic) are required to wear face-masks and gloves during the entire dental visit.27 Nonetheless, two reports suggested any confirmed COVID-19 cases should not be treated in a general dental practice setup and, therefore, should be referred either to the hospital or designated specialized centers for COVID-19, which are fully equipped with PPE. The dental treatments must be performed in negative-pressure rooms or airborne infection isolation rooms and these cases should be reported to the infectious diseases control department.8,24
Beside the use of PPE to minimize the generated aerosols during the dental procedures, a high-volume evacuator (HVE) and a high-efficiency particulate arrestor (HEPA) filter can be utilized to ensure the air is well-filtered. The HVE filter is a suction device that can eradicate the air particles at a rate up to 2.83 m3 per minute, if it is held at a proper distance of approximately 6–15 mm from the aerosol-generating area. However, the HEPA filter is an air filtration device that can remove 99.97% of the particles measured at 0.3 μm in diameter but it is more expensive than the HVE filter.28 Moreover, Peng et al have reported the importance of anti-retraction hand-piece usage to reduce the volume of the aerosols generated during the dental procedures. This type of dental hand-piece can significantly reduce the backflow of oral bacteria, hepatitis B virus, as well as other viruses into the hand-piece’s tubes and subsequently in the dental unit system, compared to the standard hand-piece without anti-retraction function. In line with the guidelines during the period of the nCoV-2019 epidemic, the standard hand-piece should only be utilized in designated specialized centers.8
A study by Sabino-Silva et al has shown that salivary biomarkers are considered as a simple diagnostic tool to detect SARS-CoV-2 virus. Additionally, it reported the following gates for the virus transmission when it is in the saliva: lower and upper respiratory tracts, crevicular fluid where the blood can access the mouth and the major and minor salivary glands. Based on the production of SARS-CoV-specific secretory immunoglobulin A (sIgA) in the saliva, a salivary diagnostic test to detect COVID-19 status via specific virus antibodies can be considered.29 Another study by Chen et al focused on SARS-CoV-2 detection in the saliva where the results were only observed at advanced stage of the disease. This has highlighted a red flag not only in terms of precaution and cross-infection control measures but also in terms of the prognosis rate assessment.30 It is important to note that saliva is an important bio-fluid in which its constant quantitative and qualitative properties reflect multiple conditions and disorders. A non-invasive harvest protocol can be evolved due to the role of salivary biomarkers.31
Regarding imaging prescription if mandatory, an extra-oral radiograph is more preferable than intra-oral such as an orthopantomogram or cone beam computer tomography if justified to minimize the gag and cough reflexes. However, if intraoral imaging is required then the sensor should be double shielded in order to prevent cross-infection.24 In this regard, several studies have shown that the use of antiseptic mouth rinse prior to any dental treatment or intra-oral examination, as a regular protocol for each patient, is vital to reduce the bacterial colonies and SARS-CoV-2 viral load in the saliva. The disinfected solution should contain oxidative agents such as 1% HP or 0.2% PI.8,32,33 On this note, Herrera et al have suggested that the viral load in the saliva can be reduced with the following types of mouth-rinses: N-hexadecyl pyridinium chloride, cetylpyridinium chloride (CPC), chlorhexidine, essential oil, beta-cyclodextrin and citrox.34 Within this context, a combination of these solutions may enhance the efficacy of the antiviral effect. Thus, the combination of cyclodextrins and citrox as an oral mouthwash solution prior to dental treatment can add benefits toward viral eradication.35 At present, there is no trial study that has proven the efficacy against SARS-CoV-2 yet. It is noteworthy that there are two registered clinical trials (NCT04341688, NCT04409873)36,37, which are in non-recruiting status, aiming to assess the efficacy of these solutions and others to reduce the SARS-CoV-2 viral load.
The results of the in vitro study by To et al have confirmed via viral culture analysis that SARS-CoV-2 viruses are present in the saliva.38 Notably, most of the dental procedures can generate aerosols where saliva is the most abundant contaminator for the dental practitioner.38 Moreover, the use of rubber dam isolation should be a standard practice when high-speed hand-pieces are used, in order to minimize the exposure to the generated aerosols, especially during inlays, onlays or full coverage crown preparations. It is noteworthy that hand scalers can be utilized in periodontal interventions (scaling and root planning, periodontal abscess) instead of ultrasonic machines to minimize the exposure to the aerosols. In addition, PPE and careful surface disinfection must be the core standard of practice.39,40 Implementing a high standard of cross-infection control protocols, taking into consideration the potential risks to patients and healthcare professional personals, is mandatory.41
It is important to note that pediatric patients have the advantages of a wider range of non-aerosol generating procedures, which are commonly used, due to their minimally invasive nature, helping to establish a good patient–clinician rapport, regardless of the pandemic context. The following are these included treatment modalities: atraumatic restorative treatment, sealing carious lesions using fissure sealants, silver diamine fluoride to stop the evolution of the carious process, selective caries removal, the Hall technique for decayed teeth and laser use for various performed treatments.42–44 It is important to highlight the benefits of utilizing laser-assisted therapy for adult patients as well, due to its advantages in producing less aerosols, eliminating tooth vibration, minimal to less local anesthetic administration and providing analgesic effects.45
It is significant to emphasize tooth brushing with fluoridated toothpaste for all patients, including children, to prevent tooth decay.46 A report by Addy highlighted the importance of oral hygiene by stating that the majority of toothpastes, if not all of them, contain detergents/surfactants with significant antimicrobial properties, which are similar to those in the detergents of many hand-washing formulations recommended against coronavirus.46
Additionally, all appliances in the patients’ waiting areas should be frequently cleaned and disinfected. In this context, a report by Dominiak et al32 highlighted the efficiency of the following various disinfectants in eliminating SARS-CoV-2 virus: ethyl alcohol-base (78%) (EA), sodium hypochlorite (0.21%) (SH), povidone-iodine solution (0.23%) (PI) and hydrogen peroxide (>0.5%). Thus, EA and SH solutions are less effective at a reduced concentration under 71% and 0.01% respectively, and chlorhexidine digluconate at 0.02%. The action time that is needed to disinfect and inactivate the virus ranges from 30 seconds to 10 minutes.29,30,32 Interestingly, another article concluded that surface disincentive solutions such as 0.1% of SH and 62–71% of ethanol can significantly reduce the potential coronaviruses within 1 minute after exposure,47 whereas the SARS-CoV-2 virus remains viable for a relatively longer period of time on different surfaces compared to SARS-CoV-1 viability. A study by Holohan and Ghebreyesus has measured the virus viability in the aerosols as well as on metal, plastic and cardboard surfaces. The study results revealed that SARS-CoV-2 viability could be detected up to 3 days on stainless steel and plastic, up to 3 hours in aerosols, up to 4 hours on copper and up to 24 hours on cardboard.48 In this context, another study by Kampf et al has evaluated the persistence of coronaviruses on different surfaces and the potency of various disinfectants on these viruses. The results have shown that these viruses can remain active at a temperature around 20 °C on inanimate surfaces (wood and glass) for up to 4 days, up to 5 days on paper and plastic and up to 2 days on steel. Interestingly, the viability of these viruses on surgical gloves and aluminum decreases after 8 hours.47
It is essential to use surgery air disinfection via a nebulizer to pulverize the fine particles of disinfectant in the air.38 On this note, it has been well documented that an interval of several hours between patients’ appointments is required to allow good ventilation of surgery air. Additionally, an airflow pattern combined with a minimal of three air changes per hour is adequate for a dental unit. Moreover, an ultraviolet germicidal irradiation may be installed; however, its use is yet to be confirmed in dental clinics.38 Oxygen–ozone therapy has been proposed due to its strong oxidative potential on proteins and amino acids, as another solution to purify the air in dental practices.32
On all the above-mentioned notes, extra high-volume suction usage besides the regular suction can dramatically reduce the volume of the aerosols up to 70%.49,50 Meng et al suggested the use of chemo-mechanical caries removal, as a non-aerosol production method in restorative dentistry.14 Moreover, use of a resorbable suture after tooth extraction is encouraged, as a preventive measure to avoid the patient’s second visit to the practice.14 Ultimately, these measures are aimed to minimize virus exposure.
In terms of clinical and non-clinical waste guidelines, a study by Peng et al8 highlighted the importance of disposing of the clinical waste, which is classified as infectious or non-infectious, in a proper manner following the cross-infection control guidelines. The double-layer yellow-colored medical waste package with a “gooseneck” ligation should be used in order to prevent any virus transition while handling or disposing of any infectious waste.8 From a risk assessment standpoint, Yang et al proposed a disinfection protocol based on dividing the dental practice into various areas, according to the contagious risk assessment of the clinical environments.51 The area where only staff are allowed is considered of fewer viruses charged than the non-restricted area. Following this proposal, the dental clinic can be divided into three sections accordingly, which are as follows: a low risk area where patients are not allowed, a medium risk area only accessible to healthy and stable patients and a high risk area where the risk of infection is greater (operating theatres, isolated high dependency units or intensive care units). The proposed type and frequency of the detergent usage to disinfect the above-mentioned areas are as follows: water and detergent-based solution once or twice a day for a low risk environment, chlorine-based agent (500 mg/l chlorine) disinfectant for 10 and 30 minutes once or twice a day for a medium risk zone and the same agent more than twice a day for a high risk area.51
The nCoV-2019 pandemic is an unprecedented situation in which healthcare workers across the globe are facing tremendous pressure in delivering services. This is due to lockdown regulations, restricted travels and scientific community gathering as well as the authorities’ restrictions on general dental practice services, which ultimately had a great impact on patient’s care specifically and on the continuous professional development in general. All the above-mentioned restrictions and limited dental care delivery are aimed to prevent the spread of the virus. Therefore, at this difficult time, scientific documents have been shown to be one of the most important methods to update and share scientific knowledge.52
As this pandemic outbreak has fundamentally reformed the dental care services at a general dental practice setup, new policies and guidelines have been implemented and continued to be updated, in order to comply with cross-infection control and to ensure safety of the dental healthcare professionals and patients. On this note, the health and safety framework and dental procedure protocols are required to be structured by the health authorities and published periodically to assist dentists and healthcare workers in providing dental care services effectively and safely. In this context, two studies conducted in 2020 have shown the potential deadly risk among dental professionals due to lack of PPE and health and safety information.53,54 One study reported that Jordanian dentists were aware of COVID-19 symptoms, mode of transmission and infection control measures in dental clinics; however they had limited knowledge and understanding of the extra precaution measures needed to protect patients and dental staff.53 While the second paper highlighted the impact of shortage of or a lack of access to PPE on healthcare workers’ mortality. The results of the study revealed that 4% of the deceased physicians were dentists.54
The authors of this systematic review are anticipating the guidelines and protocols for oral care operational delivery services would change periodically, depending on the COVID-19 pandemic status in each country.
Conclusions
During this unprecedented time of the COVID-19 pandemic, this systemic review has concluded that safety is surely of supreme importance and may have an impact on dentists and other dental healthcare workers, in terms of practicing their profession on full scope as well as financial implications. It also highlights the current health and safety guidelines and dental care services framework to ensure patient safety, as well as utilization of minimally invasive treatment modalities such as laser-assisted therapy to minimize aerosol exposure.
Moreover, these guidelines are evolving and updated on a regular basis. The current evidence related to dental care management is based on observational data. However, there is a lack of potentially designed interventions to form the basis for evidence-based recommendations. Within the limitations of this review, due to the current constraint data, it is imperative that clinicians should understand the dynamic of this pandemic where safety measures are crucial and evidence-based preventive measures are a necessity. Moreover, informative and updated standardized policies and structured protocols are required when the knowledge on the virus behavior keeps evolving. These strategic frameworks need to be modified and published periodically until a safe vaccine is produced. There is no proven safe effective direct therapy for coronavirus disease. Nonetheless, the current ongoing randomized clinical trials globally are investigating a safe therapy with high efficacy but no scientific evidence is provided regarding the majority of the recommendations.
Acknowledgments
The publication was supported by funds from the National Research Development Projects to finance excellence (PFE)-37/2018-2020 granted by the Romanian Ministry of Research and Innovation.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work. All authors have read and agreed to the published version of the manuscript.
Disclosure
The authors declare no conflict of interest.
References
1. WHO Coronavirus Disease (COVID-19) Dashboard Available from: https://covid19.who.int.
2. Valencia DN. Brief Review on COVID-19: the 2020 Pandemic Caused by SARS-CoV-2. Cureus. 2020;12. doi:10.7759/cureus.7386.
3. Fan Y, Zhao K, Shi ZL, et al. Bat Coronaviruses in China. Viruses. 2019;11(3):11. doi:10.3390/v11030210.
4. Yin Y, Wunderink RG. MERS, SARS and other coronaviruses as causes of pneumonia. Respirology. 2018;23(2):130–137. doi:10.1111/resp.13196.
5. Wu F, Zhao S, Yu B, et al. A new coronavirus associated with human respiratory disease in China. Nature. 2020;579(7798):265–269. doi:10.1038/s41586-020-2008-3.
6. Zhou P, Yang X-L, Wang X-G, et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature. 2020;579(7798):270–273. doi:10.1038/s41586-020-2012-7.
7. Chan JF-W, To KK-W, Tse H, et al. Interspecies transmission and emergence of novel viruses: lessons from bats and birds. Trends Microbiol. 2013;21:544–555. doi:10.1016/j.tim.2013.05.005.
8. Peng X, Xu X, Li Y, et al. Transmission routes of 2019-nCoV and controls in dental practice. Int J Oral Sci. 2020;12(1):9. doi:10.1038/s41368-020-0075-9.
9. Xu H, Zhong L, Deng J, et al. High expression of ACE2 receptor of 2019-nCoV on the epithelial cells of oral mucosa. Int J Oral Sci. 2020;12(1):8. doi:10.1038/s41368-020-0074-x.
10. Hu B, Guo H, Zhou P, Shi ZL. Characteristics of SARS-CoV-2 and COVID-19. Nat Rev Microbiol. 2020;6:1–14. doi:10.1038/s41579-020-00459-7
11. Atkinson J, Chartier Y, Pessoa-Silva C, et al. Natural Ventilation for Infection Control in Health-Care Settings WHO Guidelines Approved by the Guidelines Review Committee. Geneva: World Health Organization; 2009.
12. Li Q, Guan X, Wu P, et al. Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus-Infected Pneumonia. N Engl J Med. 2020;382:1199–1207. doi:10.1056/NEJMoa2001316.
13. Lo Giudice R. The Severe Acute Respiratory Syndrome Coronavirus-2 (SARS CoV-2) in Dentistry. Management of Biological Risk in Dental Practice. Int J Environ Res Public Health. 2020;17(9):3067. doi:10.3390/ijerph17093067.
14. Meng L, Hua F, Bian Z. Coronavirus Disease 2019 (COVID-19): emerging and Future Challenges for Dental and Oral Medicine. J Dent Res. 2020;99:481–487. doi:10.1177/0022034520914246.
15. Backer JA, Klinkenberg D, Wallinga J. Incubation Period of 2019 Novel Coronavirus (2019-NCoV) Infections among Travellers from Wuhan, China, 20–28 January 2020. Euro Surveill. 2020;25(5):5. doi:10.2807/1560-7917.ES.2020.25.5.2000062
16. Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020;395(10223):497–506. doi:10.1016/S0140-6736(20)30183-5.
17. Wang D, Hu B, Hu C, et al. Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus–Infected Pneumonia in Wuhan, China. JAMA. 2020;323(11):1061–1069. doi:10.1001/jama.2020.1585.
18. Moher D, Liberati A, Tetzlaff J, et al. PRISMA Group Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7):e1000097. doi:10.1371/journal.pmed.1000097.
19. Herron JBT, Agc H-D, Gilliam AD, et al. Personal protective equipment and Covid 19- a risk to healthcare staff? Br J Oral Maxillofacial Surg. 2020;58(5):500–502. doi:10.1016/j.bjoms.2020.04.015.
20. Azarpazhooh A, Diogenes AR, Fouad AF, et al. Insights into the May 2020 Issue of the Journal of Endodontics. J Endod. 2020;46(5):561–562. doi:10.1016/j.joen.2020.03.023.
21. ADA develops guidance on dental emergency, nonemergency care Available online: https://www.ada.org/en/publications/ada-news/2020-archive/march/ada-develops-guidance-on-dental-emergency-nonemergency-care.
22. Tahamtan A, Tavakoli-Yaraki M, Mokhtari-Azad T, et al. Opioids and Viral Infections: A Double-Edged Sword. Front Microbiol. 2016;7. doi:10.3389/fmicb.2016.00970.
23. Skoglund LA, Vigen EC, Coulthard P. Coronavirus and analgesics. Br Dent J. 2020;228(7):487. doi:10.1038/s41415-020-1485-y.
24. Ather A, Patel B, Ruparel NB, et al. Hargreaves, K.M. Coronavirus Disease 19 (COVID-19): implications for Clinical Dental Care. J Endod. 2020;46(5):584–595. doi:10.1016/j.joen.2020.03.008.
25. Alharbi A, Alharbi S, Alqaidi S. Guidelines for dental care provision during the COVID-19 pandemic. Saudi Dental J. 2020;32(4):181–186. doi:10.1016/j.sdentj.2020.04.001.
26. Coulthard P. Dentistry and coronavirus (COVID-19) - moral decision-making. Br Dent J. 2020;228(7):503–505. doi:10.1038/s41415-020-1482-1.
27. Spagnuolo G, De Vito D, Rengo S, et al. COVID-19 Outbreak: an Overview on Dentistry. IJERPH. 2020;17:2094. doi:10.3390/ijerph17062094.
28. Ge Z, Yang L, Xia J, et al. Possible aerosol transmission of COVID-19 and special precautions in dentistry. J Zhejiang Univ Sci B. 2020;21:361–368. doi:10.1631/jzus.B2010010.
29. Sabino-Silva R, Jardim ACG, Siqueira WL. Coronavirus COVID-19 impacts to dentistry and potential salivary diagnosis. Clin Oral Invest. 2020;24:1619–1621. doi:10.1007/s00784-020-03248-x.
30. Chen L, Zhao J, Peng J, et al. Detection of 2019-Ncov in Saliva and Characterization of Oral Symptoms in COVID-19 Patients. Rochester, NY: Social Science Research Network; 2020.
31. Lamy E, Capela-Silva F, Tvarijonaviciute A. Research on Saliva Secretion and Composition. Biomed Res Int. 2018;2018:1–2. doi:10.1155/2018/7406312.
32. Dominiak M, Różyło-Kalinowska I, Gedrange T, et al. COVID-19 and professional dental practice. The Polish Dental Association Working Group recommendations for procedures in dental office during an increased epidemiological risk. jos. 2020;73:1–10. doi:10.5114/jos.2020.94168.
33. van Doremalen N, Bushmaker T, Morris DH, et al. Aerosol and Surface Stability of SARS-CoV-2 as Compared with SARS-CoV-1. N Engl J Med. 2020;382:1564–1567. doi:10.1056/NEJMc2004973.
34. Herrera D, Serrano J, Roldán S, Sanz M. Is the oral cavity relevant in SARS-CoV-2 pandemic? Clin Oral Investig. 2020;8:2925–2930. doi:10.1007/s00784-020-03413-2.
35. Carrouel F, Conte MP, Fisher J, et al. COVID-19: A Recommendation to Examine the Effect of Mouthrinses with β-Cyclodextrin Combined with Citrox in Preventing Infection and Progression. J Clin Med. 2020;9(4):1126. doi:10.3390/jcm9041126.
36. Antiseptic Mouthwash/Pre-Procedural Rinse on SARS-CoV-2 Load (COVID-19) (AMPoL). Available from: ClinicalTrials.gov.
37. Clinical A Trial of Gargling Agents in Reducing Intraoral Viral Load Among COVID-19 Patients (GARGLES). ClinicalTrials.gov.
38. To KK-W, Tsang OT-Y, Yip CC-Y, et al. Consistent Detection of 2019 Novel Coronavirus in Saliva. Clin Infect Dis. 2020;71(15):841–843. doi:10.1093/cid/ciaa149.
39. Gurzawska-Comis K, Becker K, Brunello G, Gurzawska A, Schwarz F. Recommendations for Dental Care during COVID-19 Pandemic. J Clin Med. 2020;9(6):1833. doi:10.3390/jcm9061833
40. Ren YF, Rasubala L, Malmstrom H. Dental Care and Oral Health under the Clouds of COVID-19. JDR Clin Trans Res. 2020;5(3):202–210. doi:10.1177/2380084420924385.
41. Volgenant CMC, Persoon IF, Rag DR, de Soet JJH. Infection control in dental health care during and after the SARS-CoV-2 outbreak. Oral Dis. 2020;11.
42. Mallinen SK, Innes NP, Raggio DP, et al. Coronavirus disease (COVID‐19): characteristics in children and considerations for dentists providing their care. Int J Paediatr Dent. 2020;30:245–250. doi:10.1111/ipd.12653.
43. Bordea IR, Lucaciu PO, Crișan B, et al. The Influence Of Chromophore Presence In An Experimental Bleaching Gel On Laser Assisted Tooth Whitening Efficiency. Studia Univ Babes Bolyai. 2016;61.
44. Bordea IR, Hanna R, Chiniforush N, et al. Evaluation of the outcome of various laser therapy applications in root canal disinfection: A systematic review. Photodiagnosis Photodyn Ther. 2020;29:101611. doi:10.1016/j.pdpdt.2019.101611.
45. Matys J, Grzech-Leśniak K. Dental Aerosol as a Hazard Risk for Dental Workers. Materials. 2020;13(22):5109. doi:10.3390/ma13225109
46. Addy M. Toothbrushing against coronavirus. Br Dent J. 2020;228(7):487. doi:10.1038/s41415-020-1450-9.
47. Kampf G, Todt D, Pfaender S, et al. Persistence of coronaviruses on inanimate surfaces and their inactivation with biocidal agents. J Hospital Infect. 2020;104(3):246–251. doi:10.1016/j.jhin.2020.01.022.
48. Holohan T, Ghebreyesus TA. COVID-19 and dental practice in Ireland; 2020. Available from: https://www.dentist.ie/_fileupload/Covid%2019/IDA%20Paper%20re%20Covid19%20to%20send%20to%20HPSC%2018_03_2020.pdf.
49. Samaranayake LP, Reid J, Evans D. The Efficacy of Rubber Dam Isolation in Reducing Atmospheric Bacterial Contamination. ASDC J Dent Child. 1989;56(6):442–444.
50. Harrel SK, Molinari J. Aerosols and Splatter in Dentistry. J Am Dental Assoc. 2004;135(4):429–437. doi:10.14219/jada.archive.2004.0207.
51. Yang Y, Soh HY, Cai ZG, et al. Experience of Diagnosing and Managing Patients in Oral Maxillofacial Surgery during the Prevention and Control Period of the New Coronavirus Pneumonia. Chin J Dent Res. 2020;23(1):57–62. doi:10.3290/j.cjdr.a44339.
52. Martelli-Júnior H, Machado RA, Martelli DRB, et al. Dental journals and coronavirus disease (COVID-19): A current view. Oral Oncol. 2020;106:104664. doi:10.1016/j.oraloncology.2020.104664.
53. Khader Y, Al Nsour M, Al-Batayneh OB. Dentists’ Awareness, Perception, and Attitude Regarding COVID-19 and Infection Control: cross-Sectional Study Among Jordanian Dentists. JMIR Public Health Surveill. 2020;6:e18798. doi:10.2196/18798.
54. Ing E, Xu AQ, Salimi A, et al. Physician Deaths from Corona Virus Disease (COVID-19). medRxiv. 2020:20054494. doi:10.1101/2020.04.05.20054494
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.