Back to Journals » Cancer Management and Research » Volume 11
Frequency of germline mutations in BRCA1 and BRCA2 in ovarian cancer patients and their effect on treatment outcome
Authors Ashour M , Ezzat Shafik H
Received 26 February 2019
Accepted for publication 17 May 2019
Published 8 July 2019 Volume 2019:11 Pages 6275—6284
DOI https://doi.org/10.2147/CMAR.S206817
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Chien-Feng Li
Mohamed Ashour1,2, Hanan Ezzat Shafik3
1Clinical Oncology, Faculty of Medicine, Al Azhar University, Kuwait, Egypt; 2Department of Medical Oncology, Kuwait Cancer Control Centre, Farwanyia, Ragai, Kuwait, Egypt; 3Medical Oncology Department, National Cancer Institute, Cairo University, Giza, Cairo, Egypt
Aim of work: Reporting the incidence and the variants of BRCA1/2 mutations in ovarian cancer patients exploring their effects on the treatment outcomes.
Patients and methods: In total, 104 patients with epithelial ovarian cancer were prospectively recruited to the study. Analysis consisted of the sequencing of all the translated exons and immediately adjacent intronic regions of the BRCA1/2 genes. Responses to multiple lines of chemotherapy were assessed, as well as the effect of BRCA gene mutations on progression-free survival (PFS) and overall survival (OS).
Results: Pathogenic BRCA1/2 mutations were found in 21.15% of the patients. BRCA1 mutations represented 68.2% of the total mutations. Two novel BRCA1 mutations were identified. Age at diagnosis was a strong predictor of the presence of a pathogenic BRCA1/2 mutation. Patients with a family history of cancer had a higher incidence of BRCA mutations (P=0.005). As high as 72% of the patients with BRCA mutations were diagnosed at advanced stage. High-grade serous tumors have a higher incidence of pathogenic mutation (P=0.07). Response to neoadjuvant chemotherapy was high (93.9%). All patients underwent surgery which was optimal in 73.1% of the patients. As high as 85.6% of the patients received adjuvant chemotherapy. Relapse rate was 45.2%. Visceral metastasis was more often in BRCA carriers (P=0.01). Patients carrying pathogenic BRCA1/2 mutations had a longer median PFS of 42.43 months (95% CI 32.04–52.83) compared to 22.24 months (95% CI 14.83–29.58) for non-carriers (P=0.08). OS was 64.32 months (95% CI 38.09–90.06) for BRCA mutation patients versus 56.63 months (95% CI 50.05–63.21) (P=0.04) for non-carriers. In multivariate analysis, early stage at diagnosis and optimal debulking were the only independent predictors of better PFS and OS.
Conclusion: We documented a number of pathogenic BRCA1 and 2 mutations in this patients cohort; two novel mutations were detected. BRCA status seemed to affect survival in ovarian cancer patients.
Keywords: hereditary, ovarian, cancer, mutation, platinum, sensitive
Introduction
Ovarian cancer (OC) is the seventh leading cancer diagnosis and the fifth leading cause of cancer-related mortality.1 The American Cancer Society estimated that in 2018, 22,240 new cases will be diagnosed, with 14,070 deaths.2 OC represents the 8th most common cancer in Kuwait among Kuwaitis and non-Kuwaitis.3 Epithelial ovarian cancer (EOC) is the most common type of OC; serous tumors are the most common subtype.4
BRCA1/2 are important tumor suppressor genes implicated in DNA double-strand break repair by homologous recombination (HR), which is also involved in cellular proliferation and chromosomal stability.5
The association between germline mutations in BRCA1 and BRCA2 and the risk of developing OC is well established. The lifetime prevalence rates of OC are estimated to be 28–66% for individuals with BRCA1 mutations and 16–27% for those with BRCA2 mutations.6
Variation in the worldwide prevalence of BRCA1 and BRCA2 mutations is well recognized. The prevalence of germline BRCA1 and BRCA2 mutations in individuals with EOC varies from 5% to 20%, and somatic mutations occur less frequently (2% and 8%, respectively).7–9
BRCA mutations are associated with longer survival rates after OC diagnosis and a favorable response to platinum-based therapy, with an overall improved prognosis.10
In our region, there is a paucity of data about the proportion of OC patients carrying these mutations; these data would improve genetic screening and counseling for women with OC. In Kuwait, this is the 1st study discussing the prevalence of BRCA1/2 mutation in ovarian cancer patients.
In the current study, we recruited prospectively women diagnosed with OC were prospectively studied to assess the BRCA1 and BRCA2 mutation frequencies, with a focus on the clinical characteristics of mutation carriers compared to non-carriers and an exploration of the outcomes of treatment.
Patients and methods
Women aged 18 to 75 years who were diagnosed with EOC were eligible for the study. A total of 104 patients were recruited; 64 (61.54%) were of Arab origin, 34 (32.69%) were Asian, 4 (3.85%) were European, and 2 (1.92%) were African. The study was approved by the ethical committee of the Ministry of Health (Kuwait) with the number 295/2015 on 18/10/2015. All patients received an explanation of the nature of the study and signed a detailed informed consent form. At the time of their entry into the study, a complete personal and family history, including a detailed history of relatives diagnosed with cancer (age at diagnosis, site of cancer), was taken and recorded. All patients were subjected to full clinical examinations; laboratory tests (complete blood work, liver function tests, kidney function tests, and CA125 level assessment); baseline CT scans of the chest, abdomen, and pelvis; and pathological examinations by an expert gynecological pathologist.
Eligible patients provided a 20-mL blood sample. Samples were sent within 72 hrs to Myriad Genetics.
The genetic analysis consisted of sequencing all the translated exons and immediately adjacent intronic regions of the BRCA1 and BRCA2 genes, as well as large rearrangement analysis (MLPA) of all the BRCA1 (OMIM 113705/GenBank entry U14680) and BRCA2 (OMIM 600185/GenBank entry U43746) exons.
The mutations reported were checked in linked Database of Single Nucleotide Polymorphisms (dbSNP), ClinVar databases, BRCA Exchange, LOVD, and Associated regional and university pathologists (ARUP).11–15
The variants were classified based on the American Society of Medical Genetics and Genomics (ACMG) into 1) Class 5 (pathogenic), Class 4 (likely pathogenic), Class 3 (variant of uncertain significance), class2 (likely benign), and Class 1(benign).16
Details regarding the chemotherapy treatments (neoadjuvant, adjuvant, first line, and subsequent lines of chemotherapy) were recorded. Details of the surgeries were also recorded. Assessment included measurement of the level of CA125 and CT scans of the chest, abdomen, and pelvis. The date of first progression was determined based on the CA125 level and confirmed by imaging according to the response evaluation criteria in solid tumor guidelines (RECIST criteria). The median duration of follow-up was 39.75 months (95% CI 25.18–54.33).
Statistical methods
The statistical analyses were performed with SPSS version 22. Categorical data were summarized using percentages; numerical data were summarized as the means and standard deviations or medians and ranges. Chi-square tests and Fisher’s exact tests were used to examine the relationships between qualitative variables. The survival analysis was performed using the Kaplan–Meier method. A log-rank test was used to compare the survival curves. All tests of hypotheses were conducted at an alpha level of 0.05, with a 95% confidence interval.
The median duration of follow-up was estimated using the reverse Kaplan–Meier method. PFS was defined as the interval from histological diagnosis to the date of first progression or last follow-up. OS was defined as the interval from histological diagnosis to the date of death or last follow-up.
Results
Pathogenic BRCA1 and 2 mutations were detected in 22 patients (21.15%). BRCA1 in 15 patients (17.05%) and BRCA 2 in 7 patients (7.95%). On analyzing the frequency of BRCA mutation based on ancestry, we found that out of the 64 Arab patients, 14 (21.9%) were carriers for a pathogenic BRCA mutation, and out of the 34 patients of Asian origin, 8 (23.5%) were BRCA carriers, none of the patients from European or African origin carried the mutation. Only one mutation occurred twice. Among the 21 detected mutations, 19 were pathogenic, 1 was of uncertain significance, and 1 was benign. Fifteen mutations were Frameshifts, two were missense, two nonsense, and 2 were splice-site. Two Novel BRCA 1 mutations were detected; c.4658del which is predicted to result in the premature truncation of the BRCA 1 protein at position 1558 (p.Leu1553Cysfs*6) and c.3919del which is predicted to result in the premature truncation of the BRCA1 protein at amino acid position 1317 (p.Thr1307Leufs*11).
The age at diagnosis was a strong predictor of the presence of a pathogenic BRCA1/2 mutation; out of the 22 patients carrying the mutation, 19 were younger than 50 years (86.4%). Compared with patients with no family history of cancer, patients with a family history of cancer had a significantly higher incidence of BRCA mutations (P=0.005). Approximately 72% of the patients with pathogenic BRCA mutations were diagnosed with tumors at an advanced stage. Compared with women diagnosed with other histologies, those diagnosed with high-grade serous tumors had a higher incidence of pathogenic mutations (P=0.07). The relationships between patient characteristics and BRCA 1/2 carrier status are listed in Table 1. The locations of the BRCA gene mutations are listed in Table 2.
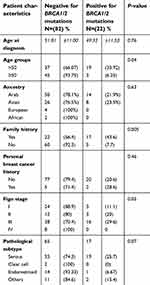 |
Table 1 Patient characteristics |
 |
Table 2 Location of BRCA gene mutations |
The details of the primary treatments received by all patients are listed in Table 3. The response to neoadjuvant chemotherapy was high (93.9%). All patients underwent surgery, which was optimal in approximately three-fourths of the patients. In total, 85.6% of the patients received adjuvant chemotherapy.
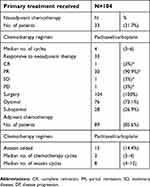 |
Table 3 Primary treatment received |
After primary treatment, 47 patients (45.2%) relapsed. Thirty-seven patients (78.7%) relapsed locally and 10 (21.3%) developed visceral metastases. (Table 4) Compared with non-carriers, BRCA mutation carriers experienced visceral metastasis more often (P=0.01) (Table 5).
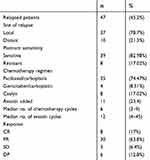 |
Table 4 Pattern of relapse and treatment received at relapse |
 |
Table 5 Association of relapse pattern with BRCA1/2 mutation status |
Patients with relapse-free intervals greater than 6 months were considered platinum sensitive. In this cohort, 39 (82.98%) relapsed patients were platinum sensitive. The BRCA mutation status did not appear to affect the pattern of platinum sensitivity at the time of relapse (P=0.59). Details of the treatments received at the time of relapse are shown in Table 4.
Patients carrying pathogenic BRCA1/2 mutations had a median PFS of 42.43 months (95% CI 32.04–52.83), which was longer than the median PFS of 22.24 months (95% CI 14.83–29.58) in non-carriers; this difference approached significance (P=0.08) (Figure 1).
 |
Figure 1 Relationship of overall survival with BRCA1/2 mutation status. |
BRCA1/2 mutations were predictors of longer OS times; patients with mutations had a median OS of 64.32 months (95% CI 38.09–90.06), while non-carriers had a median OS of 56.63 months (95% CI 50.05–63.21) (P=0.04) (Figure 2).
 |
Figure 2 Relationship of relapse free survival with BRCA1/2 mutation status. |
The results of the univariate analysis showing the association of tumor characteristics with PFS and OS are shown in Tables 6 and 7.
 |
Table 6 Univariate analysis for the association of tumor characteristics with progression-free survival |
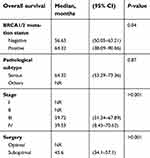 |
Table 7 Univariate analysis for the association of tumor characteristics with overall survival |
In the multivariate analysis, only an early stage at diagnosis and optimal debulking were predictors of longer PFS and OS.
Discussion
This prospective observational cohort study was performed on all patients with non-mucinous OC, either newly presenting to a medical oncology outpatient clinic or old under follow-up. The aim of this study was to determine the prevalence of germline BRCA mutations in OC patients and their correlation with clinical outcomes.
Pathogenic BRCA1/2 mutations were found in 22 patients (21.15%). BRCA1 mutations were detected in 15 patients (68.2%), and BRCA 2 mutations were found in 7 (31.8%). This was consistent with the overall incidence rate of 22.5% reported by Safra T et al, with 16.8% carrying BRCA1 mutations and 5.8% carrying BRCA2 mutations.17 Alsop K found pathogenic BRCA1/2 mutations in 14.1% of the patients enrolled in his trial, and more than half of the mutations were in BRCA1.18 Other studies found lower incidence rates of BRCA 1/2 mutations, ranging from 8% to 13%.19,20 In a study performed by Alhuqail A et al in the King Faisal Specialist Hospital and Research Centre, 19 of 65 OC patients (29.2%) had BRCA 1/2 mutations. Sixteen of the 65 OC patients (24.6%) had BRCA1 mutations, while the remaining 3 patients (4.6%) had BRCA2 mutations.21 This prevalence of BRCA mutations in patients with OC is higher than that identified in this study.
If we exclude the high prevalence of BRCA 1/2 mutations in one study of Ashkenazi Jews (AJs), most of the studies found comparable prevalence rates of BRCA 1/2 mutations of approximately 13–15% in OC patients in African, Asian, white, and Hispanic populations.22 In the Arab population, the available data are not conclusive. The slightly higher prevalence of BRCA 1/2 mutations observed in this region compared to other regions may be attributed to the tradition of consanguineous marriages, which increase the rate of genetic and congenital abnormalities.
In this series, the age of the patients at presentation was a strong predictor of the presence of a pathogenic BRCA1/2 mutation; 86.4% of the patients carrying mutations were diagnosed before the age of 50. Helpman L reported a mean age of 44±5 years for patients carrying BRCA1/2 mutations in his cohort, Jaya M found that most of the patients carrying BRCA1/2 mutations were younger than 50 years, and SoonKhoo U et al reported an average age of 53 years among patients with BRCA1/2 mutations. Safara T et al reported a higher median age of 58 years among patients with S mutations.23–26
In a study by Safra T that explored the prevalence of BRCA mutations in ethnically diverse groups, more than half of the BRCA carriers (59.1%) were of AJ descent. Other BRCA1/2 mutation carriers were non-AJ, non-Jewish Caucasian, African American, Hispanic, and unknown.17 The mutation prevalence among African–Americans with strong histories of breast cancer and OC was 16.3% in BRCA1 and 11.3–14.4% in BRCA2.26 Hispanic patients with strong family histories of cancer had mutation prevalence rates of 15.7–22.7% in BRCA1 and 6–8% in BRCA2.27
In this series, the incidence rates of BRCA1/2 mutations were 21.9% in patients from the Middle East and 23.5% in patients from Asia. The prevalence of BRCA mutations in this cohort was close to that found in Hispanic populations, lower than that identified in African American populations, and substantially lower than that observed in AJ populations.17
In this study, 43.6% of the patients with a family history of cancer carried a BRCA mutation, while patients with no family history of cancer had an incidence rate of BRCA1/2 mutations of 7.7%; the difference was significant (P=0.005). This finding was consistent with those reported by Helpman L et al, Alsop K et al, and Menkiszk J et al, who found that 63%, 43.5%, and 38.7% of the patients with BRCA mutations, respectively, had a family history of breast or OC.18,23,28 Many factors may contribute to this finding, including the accuracy of the history collected, patient ethnicity, and patient selection.18,29,30 In most of the published data, family history has an important impact on an individual’s risk of cancer. This may emphasize the importance of testing for BRCA1/2 mutations based on family history.
Approximately three-fourths of the patients with BRCA1/2 mutations in this study presented with an advanced stage of OC; a similar finding was reported by J. Liu et al, with 75% of the BRCA1 mutation carriers and 67.3% of the BRCA2 mutation carriers diagnosed at stage 3 or 4. Alsop K et al also found that women with pathogenic mutations were diagnosed with tumors at an advanced stage.18,31 In a study performed by Alhuqail A et al in the King Faisal Specialist Hospital and Research Centre, 90% of the OC patients harboring pathogenic BRCA mutations were diagnosed with advanced-stage serous carcinomas.21
In this series, pathogenic BRCA1/2 mutations were detected in 86.3% of the patients with high-grade serous carcinoma (HGSC). This finding was consistent with the results of other reports by Alsop K, Malander S, and Fong PC.18,32,33 These results support the routine testing for BRCA1/2 mutations in all patients with non-mucinous OC, especially HGSC.
Compared with non-carriers, BRCA1/2 mutation carriers experience a better response to platinum-based chemotherapy and a longer PFS;18,34–36 however, this conclusion is not consistent across all studies, as some other trials reported no effect of BRCA mutation status on response to chemotherapy, PFS, or OS.31,37 This heterogeneity in terms of the outcome can be explained by the effect of other prognostic factors, such as optimal surgery and age.38
The mechanism by which BRCA mutations sensitize tumor cells to chemotherapy is well known. However, it is not clear how this sensitization translates into a survival.39 Data on survival (PFS and OS) were found to be inconsistent in a recent meta-analysis.
Zhong et al reported longer OS and PFS in patients carrying BRCA1/2 mutations than in non-carriers.40
Xu et al reported the same findings, and another meta-analysis analyzing the results of 34 studies showed a favorable effect of BRCA mutation on OS (HR 0.69; 95% CI 0.6–0.79, P>0.002). Eighteen of those studies reported a longer PFS in patients with BRCA1/2 mutations (HR 0.69; 95% CI 0.63–0.67, P=0.118).41 In this study, patients with pathogenic BRCA1/2 mutations had median PFS of 42.43 months, which was longer than the PFS of 22.24 months observed in non-carriers; the difference approached significance (P=0.08). Additionally, compared with non-carriers, BRCA1/2 mutation carriers had longer OS times (64.32 months and 56.63 months, respectively) (P=0.04).
In multivariate analysis, stage at diagnosis and optimal cytoreductive surgery were the only independent predictors of both PFS and OS. These findings were consistent with those in previous reports by Kathryn Alsop et al, Limor Helpman, and others.5,18,23
In conclusion, this study reveals that the overall frequency of BRCA germline mutations (both pathogenic and likely pathogenic mutations) in OC patients is high. We believe that these results have significant implications for the development of preventive strategies and the use of effective targeted treatments, such as PARP inhibitors, in women affected by OC.
Conclusion
We documented a number of pathogenic BRCA1 and 2 mutations in this patients cohort, two novel mutations were detected.
The importance of BRCA mutations in the assessment of prognosis and prediction of survival in OC patients is clear; therefore, it is important to include the BRCA1/2 mutation status in the stratification of patients and the design of future clinical trials.
Acknowledgment
We would like to thank and express great appreciation to our colleagues in the Gynecology Oncology Unit and Kuwait Cancer Control Center (KCCC) in managing and facilitating the release of this work. In addition, we would like to thank our leader in the Medical Oncology Department for encouraging and improving the work atmosphere.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Coburn SB, Bray F, Sherman ME, Trabert B. International patterns and trends in ovarian cancer incidence, overall and by histologic subtype. Int J Cancer. 2017;140(11):2451–2460. doi:10.1002/ijc.30676
2. Torre LA, Trabert B, DeSantis CE, et al. Ovarian cancer statistics, 2018. CA: Cancer J Clin. 2018;68:284–296. doi:10.3322/caac.21456
3. El-Basmy A. Kuwait Cancer Registry. Kuwait Cancer Control Center; 2012.
4. Kaku T, Ogawa S, Kawano Y. Histological classification of ovarian cancer. Med Electron Microsc. 2003;36:9–17. doi:10.1007/s007950300002
5. Tutt A, Ashworth A. The relationship between the roles of BRCA genes in DNA repair and cancer predisposition. Trends Mol Med. 2002;8(12):571–576.
6. Whittemore AS, Gong G, Itnyre J. Prevalence and contribution of BRCA1 mutations in breast cancer and ovarian cancer: results from three U. S. population-based case-control studies of ovarian cancer. Am J Hum Genet. 1997;60:496–504.
7. Ramus SJ, Gayther SA. The contribution of BRCA1 and BRCA2 to ovarian cancer. Mol Oncol. 2009;3:138–150. doi:10.1016/j.molonc.2009.02.001
8. Berchuck A, Heron KA, Carney ME, et al. Frequency of germline and somatic BRCA1 mutations in ovarian cancer. Clin Cancer Res. 1998;4:2433–2437.
9. John EM, Miron A, Gong G, et al. Prevalence of pathogenic BRCA1 mutation carriers in 5 US racial/ethnic groups. Jama. 2007;298(24):2869–2876. doi:10.1001/jama.298.24.2869
10. Biglia N, Sgandurra P, Bounous VE, et al. Ovarian cancer in BRCA1 and BRCA2 gene mutation carriers: analysis of prognostic factors and survival published online May 3, 2016]. E Cancer Med Sci. 2016;10:639.
11. Database of Single Nucleotide Polymorphisms (Dbsnp) [Homepage on the Internet]. Bethesda, MD: National Center for Biotechnology Information, National Library of Medicine; 2001. Available from: http://www.ncbi.nlm.nih.gov/SNP/. Accessed September 9, 2018.
12. Landrum MJ, Lee JM, Riley GR, et al. ClinVar: public archive of relationships among sequence variation and human phenotype. Nucleic Acids Res. 2014;42(Database issue):D980–D985. doi:10.1093/nar/gkt1113
13. BRCA Exchange [database online]. UC Santa Cruz; 2017. Available from: http://www.brcaexchange.org/.
14. Fokkema IF, Taschner PE, Schaafsma GC, Celli J, Laros JF, Den Dunnen JT. LOVD v.2.0: the next generation in gene variant databases. Hum Mutat. 2011;32(5):557–563. doi:10.1002/humu.21331
15. Associated Regional and University Pathologists (ARUP). The University of UTAH. Available from: http://arup.utah.edu/database/BRCA. Accessed June 17, 2019.
16. Richards S, Aziz N, Bale S, et al. Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med. 2015;17(5):405–423. doi:10.1038/gim.2015.30
17. Safra T, Waissengrin B, Borgato L, et al. Outcome in epithelial ovarian cancer experience in ethnically diverse group. Ajho. 2016;12(9):21–25.
18. Alsop K, Fereday S, Meldrum C, et al. BRCA mutation frequency and patterns of treatment response in BRCA mutation-positive women with ovarian cancer: a report from the Australian Ovarian Cancer Study Group. J Clin Oncol. 2012;30:2654–2663. doi:10.1200/JCO.2011.39.8545
19. Risch HA, McLaughlin JR, Cole DE, et al. Prevalence and penetrance of germline BRCA1 and BRCA2 mutations in a population series of 649 women with ovarian cancer. Am J Hum Genet. 2001;68(3):700–710. doi:10.1086/318787
20. Pal T, Permuth-Wey J, Betts JA, et al. BRCA1 and BRCA2 mutations account for a large proportion of ovarian carcinoma cases. Cancer. 2005;104(12):2807–2816. doi:10.1002/cncr.21400
21. Alhuqail A, Alzahrani A, Almubarak H, et al. High prevalence of deleterious BRCA1 and BRCA2 germline mutations in arab breast and ovarian cancer patients. Breast Cancer Res Treat. 2018;168(3):695–702. doi:10.1007/s10549-017-4635-4
22. Kurian AW. BRCA1 and BRCA2 mutations across race and ethnicity: distribution and clinical implications. Curr Opin Obstet Gynecol. 2009;22:72–78. doi:10.1097/GCO.0b013e328332dca3
23. Helpman L, Perri T, Zidan O, et al. Young Israeli women with epithelial ovarian cancer: prevalence of BRCA mutations and clinical correlates. J Gynecol Oncol. 2017;28(5):e61. doi:10.3802/jgo.2017.28.e61
24. Satagopan JM, Jeff Boyd ND, Kauff MR, Scheuer L, Narod S, Offi KE. Ovarian cancer risk in Ashkenazi Jewish carriers of BRCA1 and BRC2 mutations. Clin Cancer Res. 2002;8(12):3776–3781.
25. Khoo US, Ngan HY, Cheung AN, et al. Mutational analysis of BRCA1 and BRCA2 genes in chinese ovarian cancer identifies 6 novel germline mutations. Hum Mutat. 2000;16:88–89. doi:10.1002/1098-1004(200007)16:1<88::AID-HUMU16>3.0.CO;2-G
26. Nanda R, Schumm LP, Cummings S, et al. Genetic testing in an ethnically diverse cohort of high-risk women: a comparative analysis of BRCA1 and BRCA2 mutations in American families of European and African ancestry. Jama. 2005;294:1925–1933. doi:10.1001/jama.294.15.1925
27. Vogel KJ, Atchley DP, Erlichman J, et al. BRCA1 and BRCA2 genetic testing in Hispanic patients: mutation prevalence and evaluation of the BRCAPRO risk assessment model. J Clin Oncol. 2007;25:4635–4641. doi:10.1200/JCO.2006.10.4703
28. Menkiszak J, Gronwald J, Go Rski B, et al. Hereditary ovarian cancer in poland. Int J Cancer. 2003;106:942–945. doi:10.1002/ijc.11338
29. Jacobi CE, van Ierland Y, van Asperen CJ, et al.Prediction of BRCA1/2 mutation status in patients with ovarian cancer from a hospital-based cohort. Genet Med. 2007;(9):173–179. doi:10.1097/GIM.0b013e318032e4ab
30. Hodgson SV, Heap E, Cameron J, et al. Risk factors for detecting germline BRCA1 and BRCA2 founder mutations in Ashkenazi Jewish women with breast or ovarian cancer. J Med Genet. 1999;36:369373.
31. Liu J, Cristea MC, Frankel P, et al. Clinical characteristics and outcomes of BRCA-associated ovarian cancer (OC): genotype and survival. Cancer Genet. 2012;205(1–2):34–41. doi:10.1016/j.cancergen.2012.01.008
32. Malander S, Ridderheim M. Måsba¨ck A., et al. One in 10 ovarian cancer patients carry germ line BRCA1 or BRCA2 mutations: results of a prospective study in Southern Sweden. Eur J Cancer. 2004;40:422–428.
33. Fong PC, Boss DS, Yap TA, et al. Inhibition of poly(ADP-ribose) polymerase in tumors from BRCA mutation carriers. N Engl J Med. 2009;361:123134. doi:10.1056/NEJMoa0900212
34. Vencken PM, Kriege M, Hoogwerf D, et al. Chemosensitivity and outcome of BRCA1- and BRCA2-associated ovarian cancer patients after first-line chemotherapy compared with sporadic ovarian cancer patients. Ann Oncol. 2011;22:1346–1352. doi:10.1093/annonc/mdq731
35. Rudaitis V, Zvirblis T, Kanopiene D, et al. BRCA1/2 mutation status is an independent factor of improved survival for advanced (stage III-IV) ovarian cancer. Int J Gynecol Cancer. 2014;24:1395–1400. doi:10.1097/IGC.0000000000000247
36. Gallagher DJ, Konner JA, Bell-McGuinn KM, et al. Survival in epithelial ovarian cancer: a multivariate analysis incorporating BRCA mutation status and platinum sensitivity. Ann Oncol. 2011;22:1127–1132. doi:10.1093/annonc/mdq731
37. Kotsopoulos J, Rosen B, Fan I, et al. Ten-year survival after epithelial ovarian cancer is not associated with BRCA mutation status. Gynecol Oncol. 2016;140:42–47. doi:10.1016/j.ygyno.2015.11.009
38. Muggia F, Safra T. ‘BRCAness’ and its implications for platinum action in gynecologic cancer. Anticancer Res. 2014;34:551–556.
39. Huang Y-W. Association of BRCA1/2 mutations with ovarian cancer prognosis. Medicine. 2018;97(2):e9380. doi:10.1097/MD.0000000000009380
40. Zhong Q, Peng HL, Zhao X, et al. Effects of BRCA1- and BRCA2 related mutations on ovarian and breast cancer survival: a meta-analysis. Clin Cancer Res. 2015;21:211–220. doi:10.1158/1078-0432.CCR-14-1816
41. Xu K, Yang S, Zhao Y. Prognostic significance of BRCA mutations in ovarian cancer: an updated systematic review with meta-analysis. Oncotarget. 2017;8:285–302.
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
