Back to Journals » Journal of Pain Research » Volume 13
Pulsed Radiofrequency of C2 Dorsal Root Ganglion Under Ultrasound-Guidance and CT Confirmed for Chronic Headache: Follow-Up of 20 Cases and Literature Review
Authors Li J, Yin Y, Ye L , Zuo Y
Received 5 September 2019
Accepted for publication 24 December 2019
Published 13 January 2020 Volume 2020:13 Pages 87—94
DOI https://doi.org/10.2147/JPR.S229973
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Michael A Ueberall
Jun Li, 1, 2 Yan Yin, 2 Ling Ye, 2 Yunxia Zuo 3
1National Clinical Research Center for Geriatrics and Department of Pain Management, West China Hospital, Sichuan University, Chengdu, Sichuan Province 610041, People’s Republic of China; 2Department of Pain Management, West China Hospital, Sichuan University, Chengdu, Sichuan Province 610041, People’s Republic of China; 3Department of Anesthesiology, West China Hospital, Sichuan University, Chengdu, Sichuan Province 610041, People’s Republic of China
Correspondence: Ling Ye
Department of Pain Management, West China Hospital, Sichuan University, Chengdu, Sichuan Province 610041, People’s Republic of China
Tel +86-28-85423593
Email [email protected]
Background: Chronic headache is common but difficult to treat. Most patients respond poorly to drugs. Nerve block is an effective treatment but has no continuous effect. The pulsed radiofrequency (PRF) technique has been shown to be effective in relieving head pain and extending the effect of nerve block.
Objective: The purpose of this study is to evaluate the long-term efficacy of C2 dorsal root ganglion after pulsed radiofrequency (PRF) guided by ultrasound for chronic headache.
Setting: The Department of Pain Management, West China Hospital.
Methods: Twenty patients who did not respond to medications and peripheral nerve blocks underwent ultrasound-guided PRF of the C2 dorsal root ganglion. The patients were followed up for 6 months. Visual analog scale (VAS) score was evaluated at 1 week, 1 month, 3 months, and 6 months. The quality of life (QOL) was assessed by Brief Pain Inventory (BPI) scores which were rated at pre-procedure and 1 month, 3 months, and 6 months after the procedure. The occurrence of complications was evaluated and reported.
Results: Mean VAS scores were significantly decreased at 1 week, 1 month, 3 months and 6 months compared to the pre-procedure mean VAS score. Mean BPI scores decreased significantly at each postoperative time point compared to the preoperative baseline and low scores remained throughout the follow-up period: 45.05± 3.44 at pre-procedure, 10.60 ± 2.37 at 1 weeks, 12.50 ± 2.46 at 1 month, 12.90 ± 2.62 at 3 months, and 11.63 ± 2.98 at 6 months. Mild complications occurred, including 1 case (4.7%) of transient cervicalgia (lasting for 24 hrs) and 3 cases (14.2%) of transient dizziness (lasting for 30 mins).
Limitations: Firstly, it included a small sample of patients. Another is the short duration of the follow-up.
Conclusion: C2 PRF may be considered as an alternative treatment for chronic headache.
Keywords: ultrasound guidance, pulsed radiofrequency, dorsal root ganglion, chronic intractable headache, translateral approach
Introduction
Headache is the third leading cause of disability in the world. Nearly 95% of people suffer from headaches during their lifetime.1 Headache was classified into three major categories by the International Headache Society: primary headache, secondary headache, and cranial neuropathies. Primary headache, also known as functional headache, chronic headache, including migraine, tension-type headache, cluster headache, is a common clinical headache type. Secondary headache, is always due to local organic damage or systemic disease caused by a symptom, such as cervical spondylosis, intracranial tumors, infections, and so on.2 Chronic headache is more likely associated with insomnia, bad mood (such as anxiety and depression). It can also reduce immune function, and even worsen other chronic diseases related such as high blood pressure, coronary heart disease, ulcers, and so on.3 Some of them causes severe burden and quality-of-life impairment.4 Most patients respond poorly to drugs and suffered from high recurrence rates. Reasons for the treatment failure included wrong diagnosis, inadequate analgesia, intolerable side effects, and the development of drug tolerance.5 Thus, an innovative treatment with fewer adverse effects and long-term relief was necessary for Chronic headache.
Although much efforts are being made to improve the outcome of chronic headache. The management of headache is still challenging to clinicians. Nerve block is a commonly used method that can relieve pain attacks, prolong the remission period and reduce the use of medications, but often without continuous effect6. In recent years, as an alternative treatment method, neuromodulation has been developed more and more widely. Neuromodulation procedures can target central or peripheral nerves or dorsal root ganglion (DRG).7 Pulsed radiofrequency (PRF) is a neuromodulation technique that has been proved to be effective in regulating nerve function. Occipital nerve regulation is considered to be useful in the treatment of various types of chronic headache, such as migraine, tension headache, cluster headache, and cervical headache.8 Cervical 2 dorsal root ganglion is the best site for occipital nerve regulation, which is often carried on under the guidance of C-arm or CT.9 In recent years, ultrasound guided has been widely used for the treatment of chronic pain. This article intended to observe the accuracy, safety, and efficacy of ultrasound-guided Pulsed Radiofrequency of C2 dorsal root ganglion.
Methods
Participants
This prospective trial received approval from the Clinical trial and Biomedical Ethics Committee, West China Hospital, Sichuan University, Chengdu, China. It was conducted in accordance with the Declaration of Helsinki. Written informed consent was provided by these patients. From January 2017 to September 2018, 20 patients underwent Ultrasound-guided PRF of the C2 dorsal root ganglion (DRG) in our department for the treatment of chronic headache. These patients did not respond to the anti-inflammatory analgesics, antidepressants, antiepileptic drugs, triptans, and other medications guidelines recommended. Stellate ganglion block (SGB) also could not relieve it. The patients all presented with headache of at least 5 years, nearly 3 months each year more than 15 days. All patients had visited neurologists and the neurologists referred them to the pain department. They were admitted to complete routine examinations, cervical and cranial MRI. The exclusion criteria were as following: hypersensitivity to any of the constituents of the drugs injected, local or general infection, anti-coagulation therapy, those who with severe organ dysfunction, psychiatric disorders, drug and/or alcohol abuse histories, patients with puncture contraindications and refusal to perform invasive treatment. PRF was conducted on the DRG of the C2 level in cases of which conventional blocks achieved only temporary pain reduction. The informed consent must be completed before the procedure.
Clinical characteristics of the patients including age, gender, and clinical presentation were recorded. Patients were followed by pain physicians.
Procedure
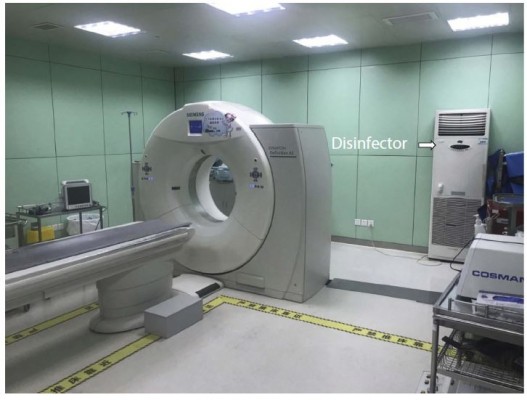
For PRF procedure, the patient was under local anesthesia and placed in prone position with the head slightly flexion facing the puncture site in the especial CT operation room for interventional procedures with sterilization of the room (Figure 1). As we have described before,10 under US-guidance (Philips CX50 ultrasound system), a probe with a frequency of 12 Mhz was used. The target site was defined as being the space in the medial of the atlantoaxial joint (AA joint). After local skin sterilization and a sterile packaging of the probe, the optimal target site was spotted. The spinous process of C2 was located in a short-axis view, then the probe shifted laterally towards the space between C1 and C2, approximately 1 cm in axial slice, showing an irregular hypoechoic image in the medial of atlantoaxial joint (Figure 2). Doppler was used to avoid inadvertent vascular structure puncture. A step-by-step progression of the 22 G needle was performed under US-guidance, tangentially to the probe, until the needle tip was accurately situated at the target site (Figure 3).
 |
Figure 1 CT operation room for interventional procedures with sterilization of the room. |
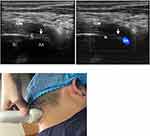 |
Figure 2 Short-axis sonogram at the level of AA joint (top left and top right). The white arrows show the atlantoaxial joint (top left and top right). Technique of how to do the US on the patient (bottom). Reproduced from Li J, Yin Y, Ye L, Zuo Y. Pulsed radiofrequency of C2 dorsal root ganglion under ultrasound guidance for chronic migraine: a case report. Journal of Pain Research. 2018;11:1915–1919. Copyright © 2018 Li et al.10 Abbreviations: VA, vertebral artery; N, C2 nerve root and dorsal root ganglion; AA, atlantoaxial joint; SC, spinal cord; IOM, inferior oblique muscle. |
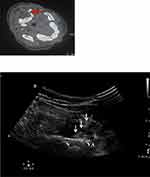 |
Figure 3 Needle was placed under US-guidance and confirmed by CT-slice. Red arrow: C2 in the CT scan. White arrow: puncture needle in the US fig. Reproduced from Li J, Yin Y, Ye L, Zuo Y. Pulsed radiofrequency of C2 dorsal root ganglion under ultrasound guidance for chronic migraine: a case report. Journal of Pain Research. 2018;11:1915–1919. Copyright © 2018 Li et al.10 Abbreviations: VA, vertebral artery; N, C2 nerve root and dorsal root ganglion. |
In order to control the technical accuracy of this new guided technique, the procedures were confirmed on a low dose CT scan (Siemens Somatom Sensation CT 64-channel) in order to allow accurate needle location. Stimulation with 50 Hz of current was applied to determine the correct needle electrode position. If a tingling sensation was perceived in the nerve distribution area at less than 0.5 V, the needle electrode was considered to be in the appropriate position. After confirming the needle position, PRF was conducted for 900 s at 42°C with 20-ms current, 2 Hz, 65 V. Diluted iodinated contrast (0.5 mL) material (Iohexol) was added to the mixture of fast and slow acting anesthetic (1 mL lidocaine 0.5% and 1 mL ropivacaine 2 mg/mL) injected in order to control accurate position and diffusion of the medicines after PRF procedure. Then, 1 mL of betamethasone (2.5 mg) was injected before the needle was removed. The patient was supervised for 10 mins to observe any early complication.10
Technical success was defined as the ability to inject anesthetics and contrast media in the space in the medial of atlantoaxial joint, confirmed by CT scan, and then to do PRF and inject corticosteroids in the accurate anatomical space (Figure 3).
Assessment Indices and Pain Evaluation
All patients rated their pain status on a visual analog scale (VAS) of pain of headache before and after the procedure. A score of 0 indicated no pain and a score of 10 represented maximal pain. Pain follow-up was at 1 week, 1 month, 3 months, and 6 month. Nerve Block efficacy was defined by a decrease of at least 50% of VAS of headache at 24 hrs following the procedure. The quality of life (QOL) was assessed by brief pain inventory (BPI) scores which was rated pre-procedure and 1 month, 3 months, 6 months after the procedure. The occurrence of complications was evaluated and reported.
Statistical Analysis
Results of continuous variables were expressed as mean ± standard deviation. All block test efficacy were studied. The results at all of the study time points were analyzed using ANOVA test with PRISM statistical software, version 22.0. P value < 0.05 was considered significant for the statistical analysis.
Results
Patients
A total of 20 consecutive patients were included and all of them completed the trial with a mean age of 46.5 ± 8.5 (27–66) years old. Patients suffered from chronic headache in 16 cases, cervicogenic headache in 2 cases, tension-type headache in 1 case, and cluster headache in 1 case.
Technical Success
Ultrasound-guided C2 PRF via a translateral approach was successfully performed in 20 patients. Technical success, as defined, was 100%. The rate in (18/20) with single puncture was 90%. All procedures were completed within 30–40 mins.
Pain Evaluation
The mean VAS decreased from 7.1 to 1.75 from one week to 6 months after the procedures. The VAS scores remained low throughout the follow-up period: 2.75 ± 0.27 at 1 week, 2.25 ± 0.45 at 1 month, 1.95 ± 0.47 at 3 months, 1.75 ± 0.48 at 6 months. Mean VAS was significantly decreased at 1 week, 1 month, 3 months, and 6 months compared to the VAS of pre-procedure. All P values were < 0.05 (Figure 4).
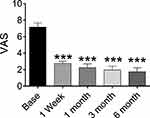 |
Figure 4 VAS of patients at pre-procedure and each post-procedure time of the follow-up period. ***P < 0.05. |
Block test efficacy, as defined, was obtained in 93.4% cases (P < 0.0009). In one case of clinical failure after infiltration, the pain was not relieved after the injection. No headache occurred in 19 patients within 2 hrs and less than 24 hrs after puncture. VAS score was 0/10 point. In the following 1 week, 5 patients had 1–2 short episodes. The VAS was below 3 points. A month later, 2 patients had recurrent pain with a VAS score greater than 7 and they were admitted to hospital again.
Mean BPI scores decreased significantly at each postoperative time point compared to the preoperative baseline (45.05 ± 3.437) at each post-procedure time point which remained low throughout the follow-up period: 10.06 ± 2.37 at 1 week, 12.50 ± 2.46 at 1 month, 12.90 ± 2.62 at 3 months, 11.63 ± 2.98 at 6 months. All P values were <0.05 (Figure 5).
No major complications occurred, such as local anesthetic poisoning, total spinal anesthesia, infection, and so on. In 4 procedures, minor Grade I side effects occurred as follows: One case of transient cervicalgia (lasting for 24 hrs) and 3 cases of transient dizziness (lasting for 30 mins).
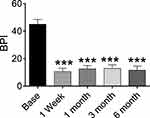 |
Figure 5 BPI scores of patients at pre- procedure and each post- procedure time of follow-up. ***P < 0.05. |
Discussion
Chronic headache is a more challenging and troublesome clinical condition. There are few therapeutic options for the treatment. Peripheral nerve blocks have been performed in headache treatment for a long time.11 The occipital nerve block, sphenoidal ganglion (SPG) block, and SGB are most widely used. Occipital nerve block showed the relief of chronic headache in 70–80% of occipital headache patients.12 According to the anatomical location, occipital nerve block can be divided into C2 dorsal root ganglion block, great occipital nerve block, lesser occipital nerve block, and sometimes also the greater auricular nerve block.13 Among them, cervical 2 DRG block can affect primary sensory neurons located in dorsal root ganglion. Some drugs may also enter the higher spinal cord through the root sheath (including some trigeminal nuclei) and play a role in regulating the head sensory conduction (14). Based on the above principles, it can be used to alleviate the symptoms of painful attack, prevent epileptic seizures (abnormal discharge of nerves), prolong the intermission period and reduce the use of drugs, but the effect often can not be sustained. The recent studies have shown that PRF regulation of C2 dorsal root ganglion is an effective treatment.15 Unlike radio frequency (RF) nerve thermocoagulation, PRF is a non-neurodestructive regulation procedure with temperature not higher than 42°C. Recent experimental studies have shown that pulsed radiofrequency may increase c-fos expression16,17 and synaptic changes in transmission, as well as minimize the neuritis and lessen the neural damage.18,19 C2 PRF will be more effective on occipital migraine involving sensitive neurons of the posterior fossa while SPG PRF will be more effective in migraine involving the anterior two-thirds of the head. In our study, the patients suffered from occipital headache involving sensitive pain. However, the exact mechanism of analgesia is yet to be known. PRF has been shown to get long-term pain relief in various chronic pain conditions.20 Appropriate guidance can improve the accuracy and safety of radiofrequency therapy. The PRF procedures were usually performed under the guidance of C-arm or CT. In recent years, ultrasound-guided therapy has been widely used in the treatment of chronic pain without radiation.
Due to the anatomic characteristics of the cervical dorsal root ganglion, ultrasound may be suitable for this interventional treatment. Unlike other dorsal root ganglions, C2 DRG locates on coverage of bones. It passes through the middle part of the atlantoaxial joint, and then it travels between obliquus capitis inferior muscle and semispinalis capitis muscle, continuing as the Great occipital nerve. Through ultrasound, the target nerve can be visualized, so the needle electrode can be introduced directly onto the nerve in real-time, the clinician can also avoid the damage to important structures and tissues. Therefore, multiple puncture can be reduced, and related complications can be minimized, such as bleeding, tissue injury, and infections. Compared to other traditional methods, ultrasound-guidance can greatly compensate the shortcomings, and improve the safety and effectiveness of neuro-interventional therapy. Study has shown that ultrasound can be used for the posterior branch of the cervical 2 spinal nerve block and electrode implantation,21–23 but there are no reports on ultrasound-guided C2 DRG radiofrequency. Under the guidance of X-ray or CT, the target is the atlantoaxial joint. Ultrasound guidance can not only see the C2 dorsal root nerve and atlantoaxial joints but also can identify the blood vessels accompanying the nerve and the vertebral artery that runs along the lateral side of the atlantoaxial joint by color Doppler.24 This new method can avoid vascular injury, especially vertebral artery injury. In addition, the intervertebral space between the C1 and C2 is wider and there is no skeletal protection in the spinal cord. Ultrasound can identify the dural sac to avoid the puncture injury.
This present study is the first to assess C2 DRG PRF with US-guidance. Results show a high technical success rate of 100% (20/20) with a high block efficacy rate of 93.4%, and with a good efficacy rate of 80%. Indeed, the predefined target site (in the medial of atlantoaxial joint) was accurately visualized in all cases. This procedure appears to be safe, as no major complication occurred and only four minor side effects were noted, which does not appear to be higher than other techniques. Theoretical risk of injury to the vertebral artery is known, but it may be avoided by the use of color Doppler, allowing detecting surrounding vascular structures present near the atlantoaxial joint.
We observed a gradual decrease up in the VAS scores throughout the follow-up period. The decrease in pain on the injected side was statistically significant (P < 0.05). Similarly, the BPI score also showed a significant decrease after C2 DRG PRF.
This is a new report to describe ultrasound-guided PRF regulation of the C2 DRG with chronic headache. The study shows a significant pain relief without serious adverse events in a 6 months follow-up period.
This trial has some limitations. First, it included a small sample of patients. Another is the short duration of the follow-up. The patients were followed for only 6 months after the injection. We hope further studies with larger samples of patients and a more extended observation period should be performed.
Conclusion
Our report demonstrated a new method of PRF on C2 dorsal root ganglion under ultrasound guidance for chronic intractable headache, which might be considered as an alternative method. More studies may be carried out to confirm the new method.
Acknowledgments
We thank Dr Pingliang Yang for his help with the analysis of the study. Pingliang Yang came from Department of Anesthesiology, The First Affiliated Hospital of Chengdu Medical College, Xindu, Sichuan, 610500, P. R. China. This study was supported by the National Clinical Research Center for Geriatrics, West China Hospital, Sichuan University (Z2018A03), the grant 2018JY0105 from Science & Technology Department of Sichuan Province, and 18ZA0158 from the Education Department of Sichuan.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Jensen R, Stovner LJ. Epidemiology and comorbidity of headache. Lancet Neurol. 2008;7(4):354–361. doi:10.1016/S1474-4422(08)70062-0
2. Headache Classification Committee of the International Headache S. The international classification of headache disorders, 3rd edition (beta version). Cephalalgia. 2013;33:629–808. doi:10.1177/0333102413485658
3. Voigt AW1, Gould HJ
4. Linde M1, Gustavsson A, Stovner LJ, et al. The cost of headache disorders in Europe: the Eurolight project. Eur J Neurol. 2012;19(5):703–711. doi:10.1111/ene.2012.19.issue-5
5. Blumenfeld AM, Bloudek LM, Becker WJ, Buse DC, Varon SF, Maglinte GA. Patterns of use and reasons for discontinuation of prophylactic medications for episodic migraine and chronic migraine: results from the second international burden of migraine study (IBMS-II). Headache. 2013;53:644–655. doi:10.1111/head.2013.53.issue-4
6. Reed KL, Will KR, Conidi F, Bulger R. Concordant occipital and supraorbital neurostimulation therapy for hemiplegic migraine; initial experience; a case series. Neuromodulation. 2015;18(4):297–303. doi:10.1111/ner.2015.18.issue-4
7. Lee PB, Horazeck C, Francis S, Billy K. Peripheral nerve stimulation for the treatment of chronic intractable headaches: long-term efficacy and safety study. Pain Physician. 2015;18:505–516.
8. Palamar D, Uludu D, Saip S, Erden G, Unalan H, Akarirmak U. Ultrasound-guided greater occipital nerve block: an efficient technique in chronic refractory migraine without aura? Pain Physician. 2015;18:153–162.
9. Kim ED, Kim YH, Park CM, Kwak JA, Moon DE. Ultrasound-guided pulsed radiofrequency of the third occipital nerve. Korean J Pain. 2013;26(2):186–190. doi:10.3344/kjp.2013.26.2.186
10. Li J, Yin Y, Ye L, Zuo Y. Pulsed radiofrequency of C2 dorsal root ganglion under ultrasound guidance for chronic migraine: a case report. J Pain Res. 2018;11:1915–1919. doi:10.2147/JPR.S172017
11. Cho SJ, Song TJ, Chu MK. Treatment update of chronic migraine. Curr Pain Headache Rep. 2017;21(6):26. doi:10.1007/s11916-017-0628-6
12. Zipfel J, Kastle A, Tatu L, Behr J, Kechidi R, Kastler B. Ultrasound-guided intermediate site greater occipital nerve infiltration: a technical feasibility study. Pain Physician. 2016;19:E1027–E1034.
13. Cesmebasi A, MA M, Hulsberg P, et al. Occipital neuralgia: anatomic considerations. Clin Anat. 2015;28(1):101–108. doi:10.1002/ca.22468
14. DM. Cervico headache: mechanism, evaluation,and treatment strategies. Am Osteopath Assoc. 2000;100(9 Supply):S7–S14.
15. Hamer J, Purath T. Response of cervicogenic headaches and occipital neuralgia to radiofrequency ablation of the dorsal root ganglion and/or third occipital nerve. Headache. 2014;335:500–510. doi:10.1111/head.12295
16. Podhajsky RJ, Sekiguchi Y, Kikuchi S, Myers RR. The histologic effects of pulsed and continuous radiofrequency lesions at 42 °C to rat dorsal root ganglion and sciatic nerve. Spine. 2005;30(9):1008–1013. doi:10.1097/01.brs.0000161005.31398.58
17. Nagar VR, Birthi P, Grider JS, Asopa A. Systematic review of radiofre- quency ablation and pulse radiofrequency for management of cervicogenic headache. Pain Physician. 2015;18(2):109–130.
18. Fang L, Tao W, Jingjing L, Nan J. Comparison of high-voltage-with standard-voltage pulsed radiofrequency of Gasserian ganglion in the treatment of idiopathic trigeminal neuralgia. Pain Pract. 2015;15(7):595–603. doi:10.1111/papr.12227
19. Rohof OJ. Caudal epidural of pulsed radiofrequency in Post Herpetic Neuralgia (PHN); report of three cases. Anesth Pain Med. 2014;4(3):e16369.
20. Zhang X, Xu Y, Zhou J, et al. Ultrasound-guided alcohol neurolysis and radiofrequency ablation of painful stump neuroma: effective treatments for post-amputation pain. J Pain Res. 2017;10:295–302. doi:10.2147/JPR
21. Hamer JF, Purath TA. Repeat RF ablation of C2 and third occipital nerves for recurrent occipital neuralgia and cervicogenic headaches. World J Neurosci. 2016;6:236–242. doi:10.4236/wjns.2016.64029
22. Zipfel J, Kastler A, Tatu L, Behr J, Kechidi R, Kastler B. Ultrasound-guided intermediate site greater occipital nerve infiltration: a technical feasibility study. Pain Physician. 2016;19(7):1027–1034.
23. Eldrige JS, Obray JB, Pingree MJ, Hoelzer BC. Occipital neuromodulation: ultrasound guidance for peripheral nerve stimulator implantation. Pain Pract. 2010;10(6):580–585. doi:10.1111/j.1533-2500.2010.00381.x
24. Narouze SN. Atlas of Ultrasound-Guided Procedures in Interventional Pain Management. Vol. 29. Springer; 2011:353–356.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
