Back to Journals » International Journal of Nanomedicine » Volume 11
Folate-conjugated boron nitride nanospheres for targeted delivery of anticancer drugs
Authors Feng S, Zhang H , Yan T, Huang D, Zhi C, Nakanishi H, Gao X
Received 16 April 2016
Accepted for publication 21 July 2016
Published 12 September 2016 Volume 2016:11 Pages 4573—4582
DOI https://doi.org/10.2147/IJN.S110689
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Linlin Sun
Shini Feng,1 Huijie Zhang,1 Ting Yan,1 Dandi Huang,1 Chunyi Zhi,2 Hideki Nakanishi,1 Xiao-Dong Gao1
1Key Laboratory of Carbohydrate Chemistry and Biotechnology, Ministry of Education, School of Biotechnology, Jiangnan University, Wuxi, People’s Republic of China; 2Department of Physics and Materials Science, City University of Hong Kong, Hong Kong SAR, People’s Republic of China
Abstract: With its unique physical and chemical properties and structural similarity to carbon, boron nitride (BN) has attracted considerable attention and found many applications. Biomedical applications of BN have recently started to emerge, raising great hopes in drug and gene delivery. Here, we developed a targeted anticancer drug delivery system based on folate-conjugated BN nanospheres (BNNS) with receptor-mediated targeting. Folic acid (FA) was successfully grafted onto BNNS via esterification reaction. In vitro cytotoxicity assay showed that BNNS-FA complexes were non-toxic to HeLa cells up to a concentration of 100 µg/mL. Then, doxorubicin hydrochloride (DOX), a commonly used anticancer drug, was loaded onto BNNS-FA complexes. BNNS-FA/DOX complexes were stable at pH 7.4 but effectively released DOX at pH 5.0, which exhibited a pH sensitive and sustained release pattern. BNNS-FA/DOX complexes could be recognized and specifically internalized by HeLa cells via FA receptor-mediated endocytosis. BNNS-FA/DOX complexes exhibited greater cytotoxicity to HeLa cells than free DOX and BNNS/DOX complexes due to the increased cellular uptake of DOX mediated by the FA receptor. Therefore, BNNS-FA complexes had strong potential for targeted cancer therapy.
Keywords: boron nitride nanospheres, folic acid, doxorubicin, targeted delivery, cancer therapy
Introduction
Cancer is among the top devastating diseases in the world.1 A variety of therapies including surgery, radiation, chemotherapy, and their combinations have been developed to treat cancer.2 Unfortunately, these therapies often result in severe side effects and cause toxicity to the patient.3 Especially, the applications of anticancer drugs for chemotherapy have some shortcomings, such as nonspecific cell and tissue distribution, short blood circulation times and multiple-drug resistance, which significantly limit the therapeutic efficacy.4,5 Recently, nanocarrier-based drug delivery systems have been rapidly developed to improve cancer therapy.3,6 Compared with the traditional administration of free drugs, nanocarrier-based drug delivery has unique advantages such as increased preferential tumor accumulation due to enhanced permeability and retention effect. A number of nanomaterial-mediated effects, such as improved chemical stability, controlled release, and protection of the drug from the immune system, may increase therapeutic efficacy.7 Meanwhile, incorporation of drugs into nano-sized delivery vehicles may reduce the adverse effects of chemotherapeutic drugs.8–10
With its structural similarity to carbon and novel properties such as excellent mechanical properties and superb thermal conductivity, boron nitride (BN) has attracted remarkable attention and found many applications.11–14 BN nanomaterials’ applications have recently been expanded in biomedical fields. BN nanomaterials can deliver a higher concentration of boron atoms into cancer cells than in blood and other organs, which makes them promising nanovehicles for boron neutron capture cancer therapy.15 Therefore, this advantageous property of BN nanospheres (BNNS) allows the combination of chemotherapy with boron neutron capture cancer therapy which will achieve a synergistic effect in cancer therapy. This is indeed an advantage over other nanocarriers for cancer therapy.
Many studies have shown that BN nanotubes possess better biocompatibility and lower cytotoxicity than carbon nanotubes.16–22 The use of BN nanotubes as carriers for the delivery of anticancer drugs has recently been reported.15,23,24 However, BNNS are considered to be more suitable for biomedical applications since spheres possess lower structure induced toxicity and easier cell uptake etc.25,26 Zhi et al reported that BNNS were non-toxic and easily taken up by cells without affecting cell proliferation.27 We previously used BNNS as carriers for intracellular delivery of immunostimulatory CpG oligodeoxynucleotides. Functionalized BNNS enhanced the loading capacity and cellular uptake of CpG oligodeoxynucleotides and significantly enhanced their immunostimulatory activity.28–30 However, biomedical applications of BNNS remain largely unexplored. To the best of our knowledge, no report on application of BNNS for targeted anticancer drug delivery can be found. Therefore, it is of tremendous interest to explore the application of BNNS in targeted cancer therapy.
One of the major challenges in cancer chemotherapy is selectively targeting tumor sites. The efficacy of chemotherapy is greatly limited by non-specific accumulation of anticancer drugs to healthy tissues, caused by the lack of specificity for cancer cells.31 One strategy is to utilize antibodies or targeting moieties since these molecules can selectively bind to cancer cells and induce receptor-mediated endocytosis.32 Among them, folic acid (FA) is a promising candidate for tumor targeting. Folate receptors (FR) are expressed at low levels in normal tissues, while they are overexpressed on the surfaces of most human tumor cells, including brain, kidney, ovarian, and breast cancer cells.33 Parker et al reported that HeLa cells also express high levels of FR compared with normal cell lines.34 Given that FA has high binding affinity to the FR,35 its conjugation to anticancer drug delivery vectors could lead to specific targeting of cancer cells.23,36–40 Therefore, folate-conjugated BNNS with receptor-mediated targeting ability would improve the cellular uptake and therapeutic efficacy of anticancer drugs.
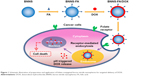
In the present work, we developed a novel targeted anticancer drug delivery system based on FA conjugated BNNS (BNNS-FA) (Figure 1). FA was used as a targeting ligand against tumor cells. BNNS-FA complexes were fabricated by covalent functionalization of FA onto BNNS via esterification reaction. The BNNS-FA complexes were fully characterized. Meanwhile, doxorubicin hydrochloride (DOX), a model of anticancer drug, was loaded onto BNNS-FA complexes and its pH-dependent releasing behavior was studied. Then, the cellular uptake of the BNNS-FA/DOX complexes was investigated to confirm the enhanced internalization of DOX by FR-mediated endocytosis. Finally, the cytotoxicity of BNNS-FA/DOX complexes against HeLa cells was studied to validate the potential of BNNS-FA complexes as carriers in cancer therapy.
Materials and methods
Materials
FA, N-(3-dimethylaminopropyl)-N′-ethylcarbodiimide hydrochloride (EDC), N-hydroxysuccinimide, and 4-(dimethylamino) pyridine (DMAP) were purchased from Shanghai Sangon Biological Engineering Technology and Services Co., Ltd (Shanghai, People’s Republic of China). Dulbecco’s Modified Eagle’s Medium (DMEM) and fetal bovine serum (FBS) were obtained from Gibco (Thermo Fisher Scientific, Waltham, MA, USA). Cell Counting Kit-8 (CCK-8) and Annexin V-fluorescein isothiocyanate Apoptosis Detection Kit were purchased from Dojindo (Kumamoto, Japan).
Preparation of BNNS-FA
BNNS were prepared through a chemical vapor deposition method.41 FA was covalently grafted on the surface of BNNS through esterification reaction according to a previously reported method.40 Briefly, 10 mg of BNNS was first treated with HNO3 (65%) and ultrasound for 1 hour, then subjected to stirring overnight at 70°C. Thus, hydroxyl groups were introduced on the surface of BNNS. Thereafter, BNNS-OH was purified and dried. Secondly 10 mg of FA, 10 mg of EDC, and 6.7 mg of DMAP were simultaneously dispersed in 20 mL of N,N-dimethylacetamide (99.8%). After stirring for 30 minutes, 10 mg of dried BNNS-OH was added and stirred overnight. Then the BNNS-FA conjugates were obtained by centrifugation, washed with water several times, and redispersed in phosphate-buffered saline (PBS).
Characterizations
Transmission electron microscopy images were obtained using a JEM-2100 transmission electron microscope operating at an acceleration voltage of 200 kV (JEOL, Tokyo, Japan). Fourier transform infrared (FTIR) spectra were measured on a Nexus spectrophotometer (Nicolet, Madison, WI, USA) at 4 cm−1 resolution with 32 scans. Zeta potential, particle size and particle polydispersity index were measured using a Zetasizer Nano ZS system (Malvern Instruments, Malvern, UK). Ultraviolet–visible absorption spectra was measured using a Nanodrop 2000 spectrophotometer (Thermo Fisher Scientific).
Cell culture
HeLa cells were purchased from the Cell Bank of Chinese Academy of Sciences (Shanghai, People’s Republic of China). Cells were cultured in DMEM with 10% FBS, 100 units/mL penicillin and 100 mg/mL streptomycin. Cells were maintained at 37°C in a humidified atmosphere with 5% CO2.
Cell viability assay
The cytotoxicity of BNNS and BNNS-FA complexes to HeLa cells was evaluated using CCK-8 assay. HeLa cells were seeded at 104 cells per well in a 96-well plate for 24 hours to allow the cells to attach. Then, BNNS and BNNS-FA complexes at a series of concentrations were added to the medium. After 24 hours’ incubation, 10 μL of CCK-8 solution was added to each well and incubated for another 3 hours. Finally, the absorbance at 450 nm was recorded using a microplate reader (Bio-Rad Laboratories Inc., Hercules, CA, USA) to determine the relative cell viability.
DOX loading and releasing
An amount of 2 mL of BNNS and BNNS-FA complexes (0.5 mg/mL in PBS) was mixed with 100 μL of DOX solution (1 mg/mL). Then, the mixture was shaken in the dark for 24 hours at room temperature, followed by centrifugation and washing to remove the free DOX. DOX loading capacity on BNNS and BNNS-FA complexes was calculated from the concentration of DOX in the supernatant determined by the Nanodrop 2000 spectrophotometer. In the DOX release experiments, 1 mg of BNNS/DOX and BNNS-FA/DOX complexes were suspended in 2 mL PBS at respective pH values of 7.4 and 5.0 and shaken at room temperature. At fixed time intervals, 0.5 mL of PBS was withdrawn by centrifugation and the same volume of fresh PBS was added to the original suspension. The concentration of released DOX was measured by the Nanodrop 2000 spectrophotometer.
Cellular uptake
For confocal laser scanning microscope observations, HeLa cells (5×104) were seeded in a 35 mm petri dish with a glass bottom and incubated for 24 hours at 37°C with 5% CO2. BNNS/DOX and BNNS-FA/DOX complexes were then added to the dish; free DOX was used as control. After incubation for 24 hours, the cells were washed twice with cold PBS to terminate the uptake and then fixed with 4% (v/v) paraformaldehyde. Fluorescence in the fixed cells was visualized using a C2Si confocal laser scanning microscope (Nikon Corporation, Tokyo, Japan). To further determine whether the cellular uptake of BNNS-FA/DOX complexes was mediated by FR, a competition experiment was conducted. HeLa cells (5×104) were pre-treated with free FA at final concentrations of 0, 5, and 20 μM for 1 hour to block the FR on the cell surface. Then, the BNNS-FA/DOX complexes were added to the medium with a final DOX concentration of 4 μg/mL, and the cells were incubated for another 2 hours. After incubation, cells were washed three times with PBS before being subjected to fluorescence microscopy imaging.
For flow cytometry assay, the quantitative evaluation of cellular uptake was performed by BD Accuri C6 flow cytometer (BD Biosciences, San Jose, CA, USA). HeLa cells were seeded in 6-well plates (5×105) and cultured in DMEM containing 10% FBS for 24 hours. Then, DOX-loaded nanoparticles were added with the same DOX concentration of 5 μg/mL, and the cells were further incubated for another 4 hours. Then the medium was removed and the cells were washed twice with cold PBS. The cells were detached by 100 μL of trypsin and washed twice with PBS, and then resuspended in 0.5 mL PBS. The amount of internalized nanoparticles was analyzed at Fluorescein isothiocyanate-A channel by a flow cytometer. Cells without any treatment were used as negative control. The fluorescence scan was performed with 2×104 cells.
In vitro cytotoxicity of BNNS/DOX and BNNS-FA/DOX complexes
HeLa cells were seeded at 104 cells per well in a 96-well plate at 37°C with 5% CO2 for 24 hours. Then, free DOX, BNNS/DOX complexes and BNNS-FA/DOX complexes were added to the medium with the same DOX concentration of 2.5 μg/mL. After incubation for 12 hours, 24 hours and 72 hours, respectively, 10 μL of the CCK-8 solution was added and incubated for another 3 hours. The absorbance at 450 nm was measured using the microplate reader to determine the cell viability.
Statistical analysis
Statistical analysis was performed using Student’s t-test. Data are presented as mean ± standard deviation. Differences were considered to be statistically significant (P<0.05).
Results and discussion
Preparation and characterization of BNNS-FA complexes
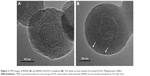
BNNS were synthesized by a chemical vapor deposition method.41 BNNS had uniform spherical shape, as visualized by transmission electron microscopy images, which showed an average diameter of approximately 150 nm (Figure 2). FA was grafted to BNNS by esterification reaction between hydroxyl groups of BNNS and carboxyl groups of FA. Figure 3A shows the FTIR spectra of BNNS and BNNS-FA complexes. BNNS had a strong asymmetric band at around 1,540 cm−1, corresponding to the B-N stretching vibration, along with a less intense band at 780 cm−1, which is ascribed to the B-N-B bending vibration.29,30,42 The distinct peaks at 1,700 cm−1 assigned to the C=O amide stretching of FA molecule appeared in the spectrum of BNNS-FA complexes.40 This result suggested that FA was grafted onto BNNS. UV-vis spectra of FA, BNNS, and BNNS-FA complexes are shown in Figure 3B. FA had an absorption peak at 290 nm, which was also observed in BNNS-FA complexes, indicating that FA was successfully conjugated to BNNS. Zeta potential measurements further confirmed the successful grafting of FA on BNNS. As shown in Figure 3C, the grafting of FA decreased the zeta potential of BNNS from −10 mV to −21.7 mV.
In vitro cytotoxicity of BNNS-FA complexes
Cytotoxicity of vehicles is a crucial issue that needs to be addressed before utilization in drug delivery systems. Although BNNS and FA were reported to be biocompatible, it is necessary to validate the cytotoxicity of BNNS-FA complexes, which were fabricated under organic solution conditions. HeLa cells were cultured with BNNS and BNNS-FA complexes with a series of concentrations, then their cytotoxicities were determined by CCK-8 assay. As shown in Figure 4, both BNNS and BNNS-FA complexes showed little cytotoxicity up to the highest testing concentration of 100 μg/mL. Therefore, the synthesized BNNS-FA could be used as drug delivery vehicles.
DOX loading and pH-dependent release
To investigate the drug delivery of BNNS-FA complexes, DOX was used as a model drug to load onto BNNS and BNNS-FA complexes. Figure 5 shows the loading of DOX onto BNNS-FA complexes. After incubation of DOX with BNNS-FA complexes, UV-vis spectra of DOX in the supernatant presented a decreased intensity compared to that before incubation, indicating the loading of DOX onto BNNS (Figure 5A). DOX loading capacity of BNNS and BNNS-FA complexes was calculated to be 6.9 and 20.7 μg per 1 mg of carriers, respectively (Figure 5B). The higher loading capacity of BNNS-FA complexes was possibly due to the enhanced negative surface charge and dispersity of BNNS by modification of FA, which facilitated the electrostatic interaction between DOX molecules and BNNS in solution. Compared with the clean surface of the pristine BNNS and BNNS-FA complexes, black dots are visible on the surface of BNNS-FA after loading of DOX, indicating the loaded DOX (Figure 2B). Furthermore, we investigated the stability of BNNS-FA/DOX complexes by measuring the hydrodynamic size of BNNS-FA/DOX complexes in PBS using dynamic laser scattering. As shown in Figure 6, no remarkable change in particle size and polydispersity index of BNNS-FA/DOX complexes was observed within 5 days, indicating the good stability of the BNNS-FA/DOX complexes.
The releasing profiles of DOX from BNNS-FA/DOX complexes in PBS at different pH values (5.0 and 7.4) are shown in Figure 7. DOX release from both BNNS/DOX and BNNS-FA/DOX complexes was pH-dependent and increased at lower pH condition. A fast release happened within 7 hours, followed by a relatively slow release rate until the end of the assay. This result was due to the increased hydrophilicity of DOX at lower pH caused by the protonation of the amino group in the DOX molecule, which weakened the interaction between DOX and hydrophobic BNNS surface and triggered DOX release. For BNNS-FA/DOX complexes, 72% of the DOX released at pH 5.0 while only 22% of DOX released at pH 7.4 after 60 hours. However, the release rate of BNNS-FA complexes was a little slower than that of BNNS complexes, which might be due to the increased electrostatic interaction between BNNS-FA complexes and DOX.
  | Figure 7 pH-dependent DOX release from BNNS/DOX and BNNS-FA/DOX complexes versus time. |
Intracellular uptake of DOX
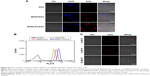
FA was conjugated to BNNS since it could target cancer cells and induce the receptor-mediated endocytosis. Herein, the cellular uptake of BNNS-FA/DOX complexes was investigated in HeLa cells, which are known to express high levels of FR.34 Confocal laser scanning microscopy images of HeLa cells after incubation with BNNS/DOX and BNNS-FA/DOX complexes for 4 hours are shown in Figure 8A. Weak fluorescence was detected within HeLa cells treated with free DOX and BNNS/DOX complexes, while strong DOX fluorescence appeared in the nuclei of the cells treated with BNNS-FA/DOX complexes. Then, a flow cytometry experiment was carried out to further quantitatively evaluate the cellular uptake of these complexes by measuring the mean fluorescence intensity from HeLa cells. As shown in Figure 8B, a dramatic enhancement of mean fluorescence intensity values was observed from HeLa cells treated with BNNS-FA/DOX complexes compared with DOX and BNNS/DOX complexes, which was consistent with the confocal laser scanning microscopy images in Figure 8A. This result was due to the significantly improved specific targeting of the BNNS-FA/DOX complexes toward FR overexpressing HeLa cells, which facilitated the cell uptake through receptor mediated endocytosis.
To further confirm the FR-mediated cell uptake of BNNS-FA/DOX complexes, free FA with concentrations of 0, 5, and 20 μM was added into the HeLa cell medium to block the FR. As shown in Figure 8C, the fluorescence from BNNS-FA/DOX complexes in the FA-free medium was significantly decreased when incubated with free FA, which showed a concentration-dependent manner. This result suggested that endocytosis of the BNNS-FA/DOX complexes in HeLa cells was mediated by FR. Free DOX molecules were transported into the cytoplasm of the cells in a passive diffusion manner, some of them were actively flushed out by P-gp, and only a small amount of DOX could enter the nucleus and bind to DNA.43 In contrast, BNNS-FA/DOX complexes were internalized by the FR-mediated endocytosis pathway, resulting in increased internalization of DOX.44 These results confirmed that FA grafting facilitates cellular uptake of BNNS-FA/DOX complexes by HeLa cells, and could enhance drug delivery efficacy.
In vitro antitumor effect of BNNS-FA/DOX complexes
To investigate DOX delivery efficacy of BNNS-FA complexes, the in vitro cytotoxic effect of BNNS-FA/DOX complexes on HeLa cells was evaluated by CCK-8 assay. Figure 9 shows cell viabilities against free DOX, BNNS/DOX complexes and BNNS-FA/DOX complexes at equivalent DOX concentration. Cell proliferation was markedly decreased in the presence of either DOX or DOX-loaded nanospheres, indicating the cytotoxicity of DOX to HeLa cells. BNNS-FA/DOX complexes exhibited the highest cytotoxicity. This result was due to the enhanced internalization of BNNS-FA/DOX complexes by FR-mediated endocytosis. Internalized DOX was triggered and released from BNNS under the acidic environment in endosomes and accumulated in nuclei, thus inducing more cell death. Free DOX showed less cytotoxicity against HeLa cells, which was caused by reduced cellular uptake and fast efflux of free DOX. Our results demonstrated that BNNS-FA complexes as drug delivery vehicles significantly enhanced antitumor efficacy in vitro. However, animal experiments are still needed to further confirm their antitumor effect in vivo.
Conclusion
In summary, we have developed a targeted anticancer drug delivery system based on folate-conjugated BNNS. FA was successfully grafted onto BNNS via esterification reaction. BNNS-FA complexes were nontoxic to HeLa cells up to a high concentration of 100 μg/mL. DOX released from BNNS-FA complexes showed a sustained release pattern, and the release rate could be triggered and increased at acidic pH condition. Most importantly, BNNS-FA/DOX complexes exhibited greater cytotoxicity compared with free DOX and BNNS/DOX complexes, which was mainly due to the increased cell uptake of DOX mediated by the FR. Therefore, BNNS-FA complexes have strong potential for targeted cancer therapy.
Acknowledgments
This work was supported by the Scientific Research Foundation for the Returned Overseas Chinese Scholars, State Education Ministry, National Natural Science Foundation of China (21406087, 31400693, 21576118), Natural Science Foundation of Jiangsu Province (BK20140141), Agriculture Science Technology Achievement Transformation Fund (2014GB2A000268) and 111 Project (No 111-2-06).
Disclosure
The authors have no conflict of interest to disclose.
References
Bardhan R, Lal S, Joshi A, Halas NJ. Theranostic nanoshells: from probe design to imaging and treatment of cancer. Acc Chem Res. 2011;44(10):936–946. | ||
Mizuno Y, Naoi T, Nishikawa M, et al. Simultaneous delivery of doxorubicin and immunostimulatory CpG motif to tumors using a plasmid DNA/doxorubicin complex in mice. J Control Release. 2010;141(2):252–259. | ||
Peer D, Karp JM, Hong S, FaroKhzad OC, Margalit R, Langer R. Nanocarriers as an emerging platform for cancer therapy. Nat Nanotechnol. 2007;2(12):751–760. | ||
Mura S, Nicolas J, Couvreur P. Stimuli-responsive nanocarriers for drug delivery. Nat Mater. 2013;12(11):991–1003. | ||
Mitscher LA, Pillai SP, Gentry EJ, Shankel DM. Multiple drug resistance. Med Res Rev. 1999;19(6):477–496. | ||
Brigger I, Dubernet C, Couvreur P. Nanoparticles in cancer therapy and diagnosis. Adv Drug Delivery Rev. 2002;54(5):631–651. | ||
Ma X, Zhao Y, Liang XJ. Theranostic nanoparticles engineered for clinic and pharmaceutics. Acc Chem Res. 2011;44(10):1114–1122. | ||
Ali-Boucetta H, Al-Jamal KT, McCarthy D, Prato M, Bianco A, Kostarelos K. Multiwalled carbon nanotube-doxorubicin supramolecular complexes for cancer therapeutics. Chem Commun (Camb). 2008;(4):459–461. | ||
Liu Z, Fan AC, Rakhra K, et al. Supramolecular stacking of doxorubicin on carbon nanotubes for in vivo cancer therapy. Angew Chem Int Ed Engl. 2009;48(41):7668–7672. | ||
Ciofani G, Danti S, D’Alessandro D, Moscato S, Petrini M, Menciassi A. Barium titanate nanoparticles: highly cytocompatible dispersions in glycol-chitosan and doxorubicin complexes for cancer therapy. Nanoscale Res Lett. 2010;5(7):1093–1101. | ||
Chopra NG, Luyken RJ, Cherrey K, et al. Boron nitride nanotubes. Science. 1995;269(5226):966–967. | ||
Golberg D, Bando Y, Huang Y, et al. Boron nitride nanotubes and nanosheets. ACS Nano. 2010;4(6):2979–2993. | ||
Golberg D, Bando Y, Tang CC, Zhi CY. Boron nitride nanotubes. Adv Mater. 2007;19(18):2413–2432. | ||
Zhi CY, Bando Y, Tang CC, Golberg D. Boron nitride nanotubes. Mater Sci Eng R. 2010;70(3–6):92–111. | ||
Li X, Zhi C, Hanagata N, Yamaguchi M, Bando Y, Golberg D. Boron nitride nanotubes functionalized with mesoporous silica for intracellular delivery of chemotherapy drugs. Chem Commun (Camb). 2013;49(66):7337–7339. | ||
Chen X, Wu P, Rousseas M, et al. Boron nitride nanotubes are noncytotoxic and can be functionalized for interaction with proteins and cells. J Am Chem Soc. 2009;131(3):890–891. | ||
Ciofani G, Danti S, Genchi GG, et al. Pilot in vivo toxicological investigation of boron nitride nanotubes. Int J Nanomedicine. 2012;7:19–24. | ||
Ciofani G, Danti S, Genchi GG, Mazzolai B, Mattoli V. Boron nitride nanotubes: biocompatibility and potential spill-over in nanomedicine. Small. 2013;9(9–10):1672–1685. | ||
Ciofani G, Danti S, Nitti S, Mazzolai B, Mattoli V, Giorgi M. Biocompatibility of boron nitride nanotubes: an up-date of in vivo toxicological investigation. Int J Pharm. 2013;444(1–2):85–88. | ||
Ciofani G, Raffa V, Menciassi A, Cuschieri A. Cytocompatibility, interactions, and uptake of polyethyleneimine-coated boron nitride nanotubes by living cells: confirmation of their potential for biomedical applications. Biotechnol Bioeng. 2008;101(4):850–858. | ||
Salvetti A, Rossi L, Iacopetti P, et al. In vivo biocompatibility of boron nitride nanotubes: effects on stem cell biology and tissue regeneration in planarians. Nanomedicine (Lond). 2015;10(12):1911–1922. | ||
Horvath L, Magrez A, Golberg D, et al. In vitro investigation of the cellular toxicity of boron nitride nanotubes. ACS Nano. 2011;5(5):3800–3810. | ||
Li X, Hanagata N, Wang X, et al. Multimodal luminescent-magnetic boron nitride nanotubes@NaGdF4:Eu structures for cancer therapy. Chem Commun (Camb). 2014;50(33):4371–4374. | ||
Weng Q, Wang B, Wang X, et al. Highly water-soluble, porous, and biocompatible boron nitrides for anticancer drug delivery. ACS Nano. 2014;8(6):6123–6130. | ||
Jonsson E, Simonsen L, Karlsson M, Larsson R. The hollow fiber model: A new method for in vivo-evaluation of antitumor effect, toxicity and pharmacokinetics of new anticancer drugs. Ann Oncol. 1998;9:44–44. | ||
Waritz RS, Ballantyne B, Clary JJ. Subchronic inhalation toxicity of 3.5–mu m diameter carbon fibers in rats. J Appl Toxicol. 1998;18(3):215–223. | ||
Zhi C, Meng W, Yamazaki T, et al. BN nanospheres as CpG ODN carriers for activation of toll-like receptor 9. J Mater Chem. 2011;21(14):5219–5222. | ||
Zhang H, Yamazaki T, Zhi C, Hanagata N. Identification of a boron nitride nanosphere-binding peptide for the intracellular delivery of CpG oligodeoxynucleotides. Nanoscale. 2012;4(20):6343–6350. | ||
Zhang H, Chen S, Zhi C, Yamazaki T, Hanagata N. Chitosan-coated boron nitride nanospheres enhance delivery of CpG oligodeoxynucleotides and induction of cytokines. Int J Nanomedicine. 2013;8:1783–1793. | ||
Zhang H, Feng S, Yan T, Zhi C, Gao XD, Hanagata N. Polyethyleneimine-functionalized boron nitride nanospheres as efficient carriers for enhancing the immunostimulatory effect of CpG oligodeoxynucleotides. Int J Nanomedicine. 2015;10:5343–5353. | ||
Jaracz S, Chen J, Kuznetsova LV, Ojima L. Recent advances in tumor-targeting anticancer drug conjugates. Bioorg Med Chem. 2005;13(17):5043–5054. | ||
Rosenholm JM, Meinander A, Peuhu E, et al. Targeting of porous hybrid silica nanoparticles to cancer cells. ACS Nano. 2009;3(1):197–206. | ||
Leamon CP, Low PS. Folate-mediated targeting: from diagnostics to drug and gene delivery. Drug Discov Today. 2001;6(1):44–51. | ||
Parker N, Turk MJ, Westrick E, Lewis JD, Low PS, Leamon CP. Folate receptor expression in carcinomas and normal tissues determined by a quantitative radioligand binding assay. Anal Biochem. 2005;338(2):284–293. | ||
Ciofani G, Raffa V, Menciassi A, Cuschieri A. Folate functionalized boron nitridenanotubes and their selective uptake by glioblastoma multiforme cells: implications for their use as boron carriers in clinical boron neutron capture therapy. Nanoscale Res Lett. 2008;4(2):113–121. | ||
Atluri R, Iqbal MN, Bacsik Z, Hedin N, Villaescusa LA, Garcia-Bennett AE. Self-assembly mechanism of folate-templated mesoporous silica. Langmuir. 2013;29(38):12003–12012. | ||
Du C, Deng D, Shan L, et al. A pH-sensitive doxorubicin prodrug based on folate-conjugated BSA for tumor-targeted drug delivery. Biomaterials. 2013;34(12):3087–3097. | ||
Lu YJ, Wei KC, Ma CCM, Yang SY, Chen JP. Dual targeted delivery of doxorubicin to cancer cells using folate-conjugated magnetic multi-walled carbon nanotubes. Colloids Surf B Biointerfaces. 2012;89:1–9. | ||
Du JZ, Du XJ, Mao CQ, Wang J. Tailor-made dual pH-sensitive polymer-doxorubicin nanoparticles for efficient anticancer drug delivery. J Am Chem Soc. 2011;133(44):17560–17563. | ||
Ferreira TH, Marino A, Rocca A, et al. Folate-grafted boron nitride nanotubes: possible exploitation in cancer therapy. Int J Pharm. 2015;481(1–2):56–63. | ||
Tang CC, Bando Y, Huang Y, Zhi CY, Golberg D. Synthetic routes and formation mechanisms of spherical boron nitride nanoparticles. Adv Funct Mater. 2008;18(22):3653–3661. | ||
Sukhorukova IV, Zhitnyak IY, Koyalslkii AM, et al. Boron nitride nanoparticles with a petal-like surface as anticancer drug-delivery systems. ACS Appl Mater Interfaces. 2015;7(31):17217–17225. | ||
Speelmans G, Staffhorst R, Dekruijff B, Dewolf FA. Transport studies of doxorubicin in model membranes indicate a difference in passive diffusion across and binding at the outer and inner leaflets of the plasma membrane. Biochemistry. 1994;33(46):13761–13768. | ||
Bildstein L, Dubernet C, Couvreur P. Prodrug-based intracellular delivery of anticancer agents. Adv Drug Deliv Rev. 2011;63(1–2):3–23. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.