Back to Journals » Clinical Ophthalmology » Volume 14
Evaluation of Visual and Subjective Outcomes with Mix-and-Match of Three One-Piece Tecnis Multifocal IOLs of Varying Add Powers
Authors Dell SJ
Received 23 June 2020
Accepted for publication 28 August 2020
Published 29 September 2020 Volume 2020:14 Pages 2903—2911
DOI https://doi.org/10.2147/OPTH.S266120
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Steven J Dell
Dell Laser Consultants, Austin, TX, USA
Correspondence: Steven J Dell
Dell Laser Consultants, Austin, TX, USA
Tel +1 512-347-0255
Email [email protected]
Purpose: To evaluate visual and subjective outcomes after bilateral mix-and-match implantation of one-piece diffractive multifocal IOLs in different near add powers (+2.75 D, +3.25 D, +4.0 D).
Setting: Four US clinics.
Design: Prospective, multi-center, parallel comparison clinical study design.
Patients and Methods: Two treatment groups received implantation with either the +3.25 D (ZLB00) or the +4.00 D (ZMB00) Tecnis® Multifocal 1-piece IOL in their non-dominant eye, and the +2.75 D (ZKB00) Tecnis Multifocal 1-piece IOL in their dominant eye (Abbott Medical Optics, Inc., Santa Ana, CA). Each study patient underwent the same routine cataract extraction procedures for each eye, with the second eye scheduled to undergo cataract extraction within 7 to 30 days after the 1st eye surgery. Visual and subjective outcomes were evaluated at 90 days after 2nd eye surgery for the two groups: +3.25D/+2.75D (n=41) and +4.00D/+2.75D (n=36).
Results: Mean binocular uncorrected distance visual acuities at 90 days postop were 0.02 ± 0.082 (+3.25D/+2.75D) vs 0.07 ± 0.128 (+4.00D/+2.75D) (p=0.025). Mean binocular uncorrected intermediate visual acuities at 90 days postop were 0.14 ± 0.185 (+3.25D/+2.75D) vs 0.26 ± 0.261 (+4.00D/+2.75D) (p=0.024). Mean binocular uncorrected near visual acuities at 90 days postop were 0.06 ± 0.098 (+3.25D/+2.75D) vs 0.19 ± 0.286 (+4.00D/+2.75D) (p=0.018). Over 88% of patients reported “none” for visual symptoms of glare, halos, starburst, or other. Freedom from glasses or contacts was reported by groups +3.25D/+2.75D and +4.00D/+2.75D as follows: distance (95.1% vs 97.1%), intermediate (92.7% vs 94.1%), and near activities (82.9% vs 64.7%).
Conclusion: At 90 days postoperatively, both groups demonstrated good visual and subjective outcomes; however, differences in near and intermediate outcomes favored the +3.25/+2.75 IOL combination.
Clinicaltrials.gov Registration: NCT02863159 (08/11/2016).
Keywords: extended range of vision, TECNIS multifocal IOL, ZKB00, ZLB00, ZMB00, cataract, blended vision, contralateral, mix-and-match
Introduction
The landscape of IOL technology continues to change rapidly with the evolution of new IOLs that provide increased range of vision with fewer visual symptoms. The usage trend of multifocals (MIOLs) has shifted toward low power add MIOLs owing to good visual performance, particularly in the intermediate range, and patient satisfaction.1–4 Mixing different power MIOLs is an emerging trend that has shown promising outcomes.4,5 Previous research has shown that MIOLs or monovision techniques can provide patients with good visual acuity at various distances and spectacle freedom.7–10 Mix-and-match of IOLs with different add powers is an approach that has been used to individualize visual correction.11–13 Combinations of near add MIOLs and low add MIOLs, such as +4.0 D add and +2.75 D IOLs have shown good visual acuities for near and distance performance, however less has been reported about the combination of +2.75 D with a +3.25 D IOL.14,15
Patients with unique lifestyle needs can now choose to combine IOL options to best suit their visual needs. Johnson and Johnson Vision has developed three multifocal 1-Piece IOLs for quality vision at one of three focal points to address lifestyle needs for near-to-intermediate distance vision. As new IOLs emerge, it is important to understand how they can be used to effectively meet lifestyle demands. Some patients may spend more time on near or intermediate activities, whereas others may be more interested in distance activities.
The objective of the study was to evaluate uncorrected binocular distance, intermediate and near visual acuities, and assess spectacle independence and satisfaction after bilateral mix-and-match implantation of one-piece diffractive multifocal IOLs in different near add powers (+3.5 D or +4.0 D) in the non-dominant eye and a low add IOL (+2.75 D) in the dominant eye.
Patients and Methods
This study was a prospective, multi-center, parallel comparison clinical study with two treatment groups. Based upon the investigator’s discussion with each patient on their lifestyle visual requirement, the investigator determined if the patient received the +3.25 D (ZLB00) or the +4.00 D (ZMB00) Tecnis® Multifocal 1-piece IOL in their non-dominant eye and all patients received the +2.75 D (ZKB00) Tecnis Multifocal 1-piece IOL in their dominant eye. Each qualified study patient was sequentially assigned a patient ID number upon enrollment.
Each study patient underwent standard routine cataract extraction procedures for each eye, consisting of small clear corneal incision, phacoemulsification extraction surgical technique, with IOL implantation in the capsular bag. The second eye underwent cataract surgery within 7 to 30 days after the first eye. In addition, as was customary for the surgeon (SD, FT, KW, or JW), each study patient received the same open-label pre-operative, operative and post-operative medications over the course of the study period. Intraoperative management of corneal astigmatism was permitted using either arcuate incision(s) or LRI(s).Patients participated in study visits from the preoperative visit through Day 90 after the 2nd eye surgery.
The study was approved by Alpha IRB, San Clemente, CA, and was conducted in accordance with principles outlined in the Declaration of Helsinki and GCP. All patients provided written informed consent. The study was registered with clinicaltrials.gov (NCT02863159).
Study Criteria
Inclusion criteria were as follows: adults ≥21 years of age, male or female, bilateral cataracts with planned phacoemulsification extraction and a posterior multifocal IOL implantation, willing to have surgery on their 2nd eye within 7 to 30 days of their 1st eye, postoperative visual potential of 20/32 or better in each eye, preoperative corneal astigmatism of <1.5 D in each eye and post-operative astigmatism target of <0.5 D in each eye, clear ocular media other than cataract in each eye, normal OCT of the macula in each eye, naturally dilated mesopic pupil sizes of >3.5 mm, and able to read, comprehend and willing give HIPAA & informed consent and complete study visits.
Enrollment was excluded based on the following criteria: known pathology that could affect visual acuity, pupil abnormalities, retinal changes that affect vision (macular degeneration, cystoid macular edema, proliferative diabetic retinopathy, etc.) in either eye, amblyopia or strabismus, capsular or zonular abnormalities affecting IOL position, evidence of Epithelial Basement Membrane Dystrophy, keratoconus or significant irregular astigmatism, history of ocular trauma or prior ocular or refractive surgery, anticipated surgical intervention and/or ocular laser treatment prior to or during the study period, PMMA lens wear within 6 months, gas permeable lenses within 1 month, extended-wear or daily soft contact lens within 7 days of surgery, systemic or ocular medications that could affect vision, uncontrolled acute or chronic or systemic disease or illness that could confound study results, current or recent participation (within 30 days) in a drug or other investigational research study.
Study Endpoints
Study endpoints included visual acuities, safety outcomes, and subjective outcomes. Visual acuities (VA) were measured in logMar and Snellen Equivalent. The ETDRS Chart was used to measure Distance VA (at 4 meters), and the ETDRS Near Chart was used to measure Intermediate VA (at 66.7 cm) and Near VA (at 40 cm). Photopic (85 cd/m2) and mesopic (3 cd/m2) illumination (for mesopic testing, patients given a minimum of 5 minutes to adapt to mesopic lighting prior to testing). Patient questionnaires were administered preoperatively at baseline, and postoperatively at 90 days and included queries about spectacle wear, satisfaction, and function (Figure 1). Visual symptoms were reported by the patient with possible responses of none, mild, moderate, or severe. Safety outcomes were collected over the course of the study including the type, severity, duration and frequency of reported adverse events for each treatment group.
 |
Figure 1 Patient questionnaires administered preoperatively at baseline and postoperatively at 90 days included queries about spectacle wear, satisfaction, and function. |
Study Lenses
All three study lenses evaluated in this study shared the Tecnis Multifocal 1-piece IOL design, but each have a different add power: +2.75 D (ZKB00), +3.25 D (ZLB00), +4.00 D (ZMB00). The +2.75 D IOL favors long intermediate vision activities at distance of ~50 cm, the +3.25 D favors intermediate vision activities at ~42 cm and the +4.00 D IOL favors near vision activities at distance of ~33 cm (Package Insert Tecnis Multifocal 1-piece IOLs). All of the IOLs are made of UV-blocking hydrophobic acrylic and have a 6.0 mm optic designed with a biconvex, anterior aspheric surface, and a posterior diffractive surface.
Statistical Analysis
Statistical analyses were performed using JMP 10 (SAS Institute, Inc; Cary, NC). Differences between mean visual acuities were calculated using paired t-test and were considered significant at the 5% level. Descriptive statistics (ie, mean, standard deviation, etc.) were calculated for all continuous variables, and frequency distributions provided for all categorical variables.
Results
Demographics
Patient demographics and baseline characteristics are presented in Table 1. The study population was predominantly female (64.6%), Caucasian (93.9%), and averaged 65 years of age. Of the 82 patients who underwent bilateral cataract surgery at baseline, five patients discontinued the study due to personal reasons (2) or were lost to follow-up (3). A total of 77 patients completed the 90-day visit, with IOL distribution as follows: 41 patients received a +2.75 D in their dominant eye and a +3.25 D IOL in their non-dominant eye, and 36 patients received a +2.75 D in their dominant eye and a +4.00 D IOL in their non-dominant eye.
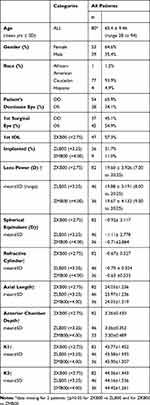 |
Table 1 Baseline Patient Characteristics |
Visual Acuities
Binocular visual acuities under photopic and mesopic conditions are presented in Table 2. Visual acuities under photopic and mesopic lighting conditions were similar. Differences between groups favored the +3.25 group (p=<0.05) across all distances and lighting conditions and were greater at near and intermediate distances. Overall mean logMAR UDVA for all patients (n=77) was 0.04 ± 0.109 (photopic). Overall mean logMAR UIVA for all patients (n=77) was 0.19 ± 0.230 (photopic). Overall mean logMAR UNVA for all patients (n=77) was 0.12 ± 0.216 (photopic). Binocular best-corrected VA for distance, intermediate, and near are presented in Table 3. Likewise, differences between groups favored the +3.25 group (p=<0.05) across all distances. Cumulative Snellen VA of 20/40 or better was achieved by the majority of patients, for distance, intermediate, and near. (Figure 2) Cumulative Snellen VA of 20/20 or better for distance, intermediate, and near are shown in Figure 3.
 |
Table 2 Binocular Mean logMAR Uncorrected Visual Acuity, 90 Days Postoperative, Photopic and Mesopic |
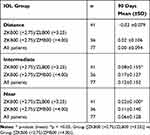 |
Table 3 Binocular Best-Corrected Visual Acuity, 90 Days Postop, Photopic |
 |
Figure 2 Uncorrected Visual Acuity 20/40 or better for distance, intermediate, and near at 90 days postoperatively. |
 |
Figure 3 Uncorrected Visual Acuity of 20/20 or better for distance, intermediate, and near at 90 days postoperatively. |
Refraction
Refractive outcomes for spherical equivalent and cylinder improved from baseline to 90 days Refraction remained stable from preoperative visit to 90 days postoperative (after 2nd eye surgery). (Figure 4) Mean postoperative spherical equivalent at Day 90 was 0.18 ± 0.445 (+2.75 D IOL), 0.20 ± 0.555 (+3.25 D IOL), and 0.08 ± 0.486 (+4.00 D IOL). Mean postoperative refractive cylinder at Day 90 was: −0.36±0.368 (+2.75 D IOL), −0.40 ±0.316 (+3.25 D IOL), and −0.43 ±0.331 (+4.00 D IOL).
 |
Figure 4 Spherical Equivalent at baseline and after 2nd eye surgery on Day 30 and Day 90. |
Safety
Postoperative examinations by slit lamp, fundoscopic exam, and corneal topography were within normal limits with the exception of the following observations that were considered clinically significant: 7 mm dilated pupil (1), irregular fovea (1), and posterior capsular opacification (6). Adverse events occurred in two eyes (+2.75 D IOL and a +4.00D IOL) treated for Toxic Anterior Segment Syndrome which resolved without sequelae. The majority of patients reported no visual symptoms for glare, halos, starbursts, or other at the 90-day visit, and none of the patients reported severe symptoms. (Figure 5)
 |
Figure 5 Visual symptoms reported by patients postoperatively at 90 days after 2nd eye surgery. |
Patient Questionnaire (+3.25 D vs +4.00 D @ 90 Day Visit)
The majority of patients with +3.25 D or +4.00 D IOLs indicated they did not require glasses or contacts for distance, intermediate, or near activities (Figure 6). Most patients with +3.25 D or +4.00 D IOLs reported being able to function without prescription glasses/contacts “With NO Difficulty” for distance (95.1%/85.7%), intermediate (92.7%/88.6%), near activities (68.3%/54.3%), and overall (near to distant) (78.0%/74.3%). Nearly all patients with +3.25 D or +4.00 D IOL implantations indicated they would recommend the procedure (100%/91.2%, respectively). Regarding satisfaction with overall vision without prescription glasses/contacts, most patients with +3.25 D or +4.00 D reported being either extremely satisfied (65.9%/71.4%) or satisfied (22.0%/11.4%).
 |
Figure 6 Percent of patients that did not require prescription glasses or contacts Spectacle Wear at 90 days after 2nd eye surgery. |
Discussion
The development of MIOLs with different add powers has made it possible to combine IOLs to meet individual vision needs. In this study, we placed a lower add IOL in the dominant eye and a higher add power lens in the non-dominant eye. The combination was determined after reviewing the visual needs of the patient. We found that visual acuities favored the +3.25 group for near and intermediate (p<0.05) and distance (p<0.05). These IOL combinations showed good and comparable results under both photopic and mesopic lighting conditions. Postoperative refraction improved and remained stable at 90 days. Patient responses to the combined IOL approach was also promising, as patients reported high rates of spectacle freedom and functionality, especially for distance and intermediate activities. Only 1 safety event occurred over the course of the study, and photic phenomena were comparable between groups, typically subsiding by the 90-day visit. Ultimately, nearly all study patients would recommend the procedure to others.
Results from our study are consistent with another prospective, contralateral study conducted by Yang et al, in which 20 patients underwent bilateral implantation with a+ 2.75 D IOL (ZKB00) in the dominant eye, and +3.25 D IOL (ZLB00) in the non-dominant eye.6 Mean binocular UDVA (−0.08 ± 0.10), UIVA (0.09 ± 0.09), and UNVA (0.14 ± 0.09), with the +3.25 and +2.75 D IOLs at 3-month postoperatively were similar to our study, although it should be noted that measurements were made at slightly difference differences for near (43 cm) and distance (5 m). Relative to subjective outcomes, their study also found high rates of satisfaction, freedom from corrective wear and minimal visual symptoms at 3 months. In addition, they found improvements in contrast sensitivity from preop to postop. Although our study did not measure contrast sensitivity, visual acuities under photopic and mesopic conditions were comparable and similar between groups.
Another recent study evaluated blended vision in 30 patients with implantation of the Symfony IOL (ZXR00) in the dominant eye and a +3.25 D (ZLB00) in the non-dominant eye.5 At 3 months, binocular results showed excellent uncorrected VA across distances, and very low incidence of visual symptoms such as glare, halo, and starbursts. The primary dysphotopsia seen with this study was halos, and by the 90-day mark, this symptom was tolerable for an overwhelming majority of study patients. In our study, the +3.25 D combination provided better visual acuity at near and intermediate distances compared with the +4.00 D IOL. This was an interesting finding for near distance, as better near VA might be expected with the higher add power IOL. One possible explanation for this phenomenon is the testing distance used in the study for intermediate (at 66.7 cm) and near (at 40 cm) corresponded more closely to the near points of focus of the +3.25/2.75 D group (~50 cm/~42cm), as compared with the +4.00/2.75 group (~33 cm/~42cm). As a result, patients in the +4.00/2.75 group might have performed better for near if the testing distance were closer. The patient questionnaire also reflected increased spectacle freedom and functionality with the +3.25/2.75 D group vs the +4.00/2.75 group for intermediate and near activities. Further study is needed to understand whether this was possibly due to neuroadaptation, preferred near working distance, or other patient factors.
A study evaluating IOL implantations with +2.75 D, +3.25 D, or +4.00 D MIOLs found that patients with lower add power MIOLs had greater satisfaction, more spectacle independence, and fewer visual symptoms than those with +4.00 D add.4 Results from the present study showed good subjective results for both the +3.25 and +4.00 D groups; however, for some outcomes such as halos, the higher add power IOL performed similarly or better. Conversely, patients with the +3.25/2.75 combo reported better functionality and less spectacle wear, as noted above. These findings are relevant for understanding patient needs and the corresponding IOL selection.
This study provided results from a prospective, clinic setting in which a custom approach was taken based on patient’s visual needs. There are few published outcomes combining the specific IOLs evaluated in this study. Some limitations that should be mentioned include the modest sample size, non-randomization, and lack of a true control. One option might have been to include a group with bilateral implant of the same add IOL. Statistically significant differences were found between the two groups at far, intermediate, and near distances; however, the modest sample sizes should be taken into account as study power was not determined at the start of the study. In terms of generalizability, the enrollment criteria limited some chronic or systemic conditions typically seen in everyday clinical practice, such as diabetes. Future studies in these populations may be beneficial as these populations may also desire this type of visual correction.16
The present study queried patients about visual symptoms and compared frequency outcomes, but future studies could evaluate symptoms and functionality with a validated questionnaire and additional statistical analyses to measure differences between the groups. Additionally, binocular defocus curves could be included to characterize the range of focus with this mix-and-match approach. Findings from this study may be of interest for patients desiring an individualized approach to meet lifestyles needs. Future studies should continue to match evolving technologies with patient needs.
In conclusion, at 90 days postoperatively, both groups demonstrated good visual and subjective outcomes, however, differences in near and intermediate outcomes favored the +3.25/+2.75 D combination over the +4.00/+2.75 D. A mix of varying add power IOLs can be a good approach for meeting near and intermediate range of vision needs.
Acknowledgments
Funding for the study was provided by J&J Vision through an unrestricted grant. Farrell Tyson, MD; Kevin Waltz, OD, MD; and Jeffrey Whitsett, MD were co-investigators in the study. Medical writing assistance was provided by Suzie Webster (ConsignMed, Inc.) and was funded by J&J Vision. Final clinical study reports (deidentified data) for visual and subjective outcomes may be made available upon email request to the corresponding author for 6 months after online publication. Previously presented in part at the American Society of Cataract and Refractive Surgery. April 2018, Washington, DC.
Disclosure
Dr Steven J Dell reports grants from Johnson and Johnson vision, during the conduct of the study and served as a consultant for Johnson and Johnson Vision, outside the submitted work. The author reports no other conflicts of interest in this work.
References
1. Cardona G, Vega F, Gil MA, Varón C, Buil JA, Millán MS. Visual acuity and image quality in 5 diffractive intraocular lenses. Eur J Ophthalmol. 2018;28(1):36–41. doi:10.5301/ejo.5000994.
2. Boujan A, Tandogan T, Pinelli G, et al. [Clinical results after implantation of a new diffractive, multifokal intraocular lens with a reduced near add power (+ 2.75 D)]. Klin Monbl Augenheilkd. 2016;233(5):633–638. doi:10.1055/s-0042-104587. German.
3. Kretz FT, Gerl M, Gerl R, Müller M, Auffarth GU, ZKB00 Study Group. Clinical evaluation of a new pupil independent diffractive multifocal intraocular lens with a +2.75 D near addition: a European multicentre study. Br J Ophthalmol. 2015;99(12):1655–1659. doi:10.1136/bjophthalmol-2015-306811.
4. Kim JS, Jung JW, Lee JM, Seo KY, Kim EK, Kim TI. Clinical outcomes following implantation of diffractive multifocal intraocular lenses with varying add powers. Am J Ophthalmol. 2015;160(4):702–9.e1. doi:10.1016/j.ajo.2015.07.021.
5. Black S. A clinical assessment of visual performance of combining the TECNIS® Symfony Extended Range of Vision IOL (ZXR00) with the +3.25 D TECNIS Multifocal 1-piece IOL (ZLB00) in subjects undergoing bilateral cataract extraction. Clin Ophthalmol. 2018;12:2129–2136. doi:10.2147/OPTH.S175901
6. Yang CM, Lim DH, Hwang S, Hyun J, Chung TY. Prospective study of bilateral mix-and-match implantation of diffractive multifocal intraocular lenses in Koreans. BMC Ophthalmol. 2018;18(1):73. doi:10.1186/s12886-018-0735-0.
7. Greenstein S, Pineda R. The quest for spectacle independence: a comparison of multifocal intraocular lens implants and pseudophakic monovision for patients with presbyopia. Semin Ophthalmol. 2017;32(1):111–115. doi:10.1080/08820538.2016.1228400
8. Labiris G, Giarmoukakis A, Patsiamanidi M, Papadopoulos Z, Kozobolis VP. Mini-monovision versus multifocal intraocular lens implantation. J Cataract Refract Surg. 2015;41(1):53–57. doi:10.1016/j.jcrs.2014.06.015
9. Goldberg DG, Goldberg MH, Shah R, Meagher JN, Ailani H. Pseudophakic mini-monovision: high patient satisfaction, reduced spectacle dependence, and low cost. BMC Ophthalmol. 2018;18(1):293. doi:10.1186/s12886-018-0963-3
10. Mu J, Li YZ, Wu Q, Yan L, Chen H. [Clinical observation on monovision of cataract surgery with different near addition]. Zhonghua Yan Ke Za Zhi. 2017;53(6):451–454. doi:10.3760/cma.j.issn.0412-4081.2017.06.011.
11. Yoon SY, Song IS, Kim JY, et al. Bilateral mix-and-match versus unilateral multifocal intraocular lens implantation: long-term comparison. J Cataract Refract Surg. 2013;39:1682–1690. doi:10.1016/j.jcrs.2013.04.043
12. Jiang Y, Bu S, Tian F, et al. Long-term clinical outcomes after mix and match implantation of two multifocal intraocular lenses with different adds. J Ophthalmol. 2019;14(2019):6789263.
13. Tarib I, Kasier I, Herbers C, et al. Comparison of visual outcomes and patient satisfaction after bilateral implantation of an EDOF IOL and a mix-and-match approach. J Refract Surg. 2019;35(7):408–416. doi:doi:10.3928/1081597X-20190417-02
14. Bissen-Miyajima H. Binocular visual function with staged implantation of diffractive multifocal intraocular lenses with three add powers. Am J Ophthalmol. 2019;199:223–229. doi:10.1016/j.ajo.2018.11.020
15. Lee JH, Lee H, Lee JA, et al. Clinical outcomes after mix-and-match implantation of diffractive multifocal intraocular lenses with + 2.75 and + 4.00 diopter add powers. BMC Ophthalmol. 2020;20(193). doi:10.1186/s12886-020-01460-7
16. Ouchi M, Kinoshita S. Implantation of refractive multifocal intraocular lens with a surface-embedded near section for cataract eyes complicated with a coexisting ocular pathology. Eye (Lond). 2015;29(5):649–655. doi:10.1038/eye.2015.12
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
