Back to Journals » Clinical, Cosmetic and Investigational Dentistry » Volume 11
Evaluating Fracture Resistance And Failure Modes Of Root Filled Teeth Restored With CAD/CAM-Fabricated Post And Core
Authors Alkhatri R , Saleh ARM , Kheder W
Received 17 June 2019
Accepted for publication 26 September 2019
Published 14 November 2019 Volume 2019:11 Pages 349—355
DOI https://doi.org/10.2147/CCIDE.S219712
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Christopher E. Okunseri

Reem Alkhatri,1 Abdul Rahman Mohammed Saleh,1 Waad Kheder2
1Department of Restorative Dentistry, Ajman University, Ajman, United Arab Emirates; 2College of Dental Medicine, University of Sharjah, Sharjah, United Arab Emirates
Correspondence: Abdul Rahman Mohammed Saleh
Ajman University, PO Box 346, Ajman University Street, Aljurf, Ajman, United Arab Emirates
Tel +971 4 50228 3188
Fax +971 4 670 56874
Email [email protected]
Objective: The aim of this study was to measure the fracture resistance and failure modes of root-filled teeth restored with three different computer-aided design/computer-aided manufacturing (CAD/CAM)-fabricated post and core assemblies.
Methods: Thirty extracted intact maxillary central incisors were used in the study, and the teeth were endodontically treated and sectioned to a root length of 16 mm. The samples were divided into three groups (n = 10) according to the mean of the dimensions at the cervical portion of the root. The posts and cores were fabricated with CAD/CAM technology using metal, zirconia, and polymer-infiltrated ceramic network (PICN) material. The posts were luted using resin cement, and then, metal crowns were fabricated, cemented, and then subjected to a compression to determine the fracture resistance force. Fracture of the post and core or fracture of the root above the level of the acrylic resin was considered as a favorable fracture, while nonfavorable fractures were those where the root fracture occurred below the level of the acrylic resin. Statistical analysis was carried out using SPSS software, and one-way analysis of variance was used to analyze root fracture resistance in Newton. The number of failure modes, post–core fractures and/or root fractures was calculated. The differences between study groups were revealed using the chi-square test.
Results: The results of ANOVA revealed a nonsignificant difference in the resistance to fracture among the study groups (P = 0.114). The failure modes were nonfavorable for all metal and zirconia samples and seven PICN samples. However, three PICN samples exhibited a favorable represented by core fracture without root fracture.
Conclusion: There was no significant difference between metal and zirconia samples in terms of nonfavorable fracture, while few PICN samples exhibited a favorable fracture. PICN material can be used in the fabrication of post and core assemblies using CAD/CAM.
Keywords: CAD/CAM, cast post, PICN, failure mode
Introduction
For the final restoration of endodontically treated teeth (ETT) with varying degrees of remaining tooth structure, the teeth must be able to withstand masticatory forces.1,2 To obtain a restoration with the most optimal results, the material used for postfabrication should have physical properties similar to those of dentin, should be bonded to the tooth structure, and must be biocompatible in the oral environment.3–6 Moreover, a good clinical outcome should be achieved if post materials are chosen that possess satisfactory modulus of elasticity, compressive strength, thermal expansion, and esthetics similar to those of dentin.4 Accordingly, the type of materials that may be used to fabricate the post and core would influence the fracture resistance of crowned ETT.7
The post must exclusively resist occlusal forces so that the load will not concentrate at the connection of the post to the core, with possibility for post breakage;8,9 In some cases, a vertical root fracture may occur when there is no ferrule or due to the transmission of occlusal forces to intraradicular parts of the root.10
Customized metal post–cores have been successfully used to restore ETT due to their excellent physical properties. However, because of the high elastic modulus, there is a high concentration of stress in the surrounding radicular dentin, leading to root fracture.11 In addition, a metal post–core has some disadvantages such as microleakage, corrosion, and an esthetic drawback as a result of metal color reflection on all-ceramic restorations.9
A zirconia post and core fabricated by using computer-aided design/computer-aided manufacturing (CAD/CAM) technology has been used to restore anterior ETT.12 However, the high modulus of elasticity (200 MPa)13 of zirconia posts leads to the transfer of stress to the less rigid dentin and causes fracture of the root.14 The polymer-infiltrated ceramic network (PICN) Vita Enamic (Vident, Brea, CA, USA) is currently available to be milled as a post and core using CAD/CAM technology. This material has high flexural strength, elasticity, and physical properties similar to those of natural teeth to overcome the brittleness of ceramic that causes wearing on antagonist natural teeth.15,16 This material combines the positive characteristics of ceramic materials with those of composite and can be used with CAD/CAM technology.16
The advantage of using CAD/CAM technology to fabricate the post and core is that there is improved adaptation with minimum tooth structure reduction17 and the ability to overcome the errors of conventional fabrication methods such as impression, waxing, and casting errors.18–20 The aim of this study was to measure the fracture resistance and failure modes of endodontically treated teeth restored with three different CAD/CAM-fabricated post and core materials.
Materials And Methods
The study was conducted after getting the approval of the Ethics and Research Committee of Ajman University (RD-2014/15-20) and a written informed consent from the patients. Thirty extracted intact maxillary central incisors were collected from periodontally compromised patients, during a period of time of approximately 6 months, and were immediately stored in normal saline inside an incubator at 100% humidity and 37°C temperature until the time of conducting the research. The teeth included in the study were radiographically examined and inspected under a stereomicroscope (Leica EZ4, Wetzlar, Germany) to ensure that they were free of restorations, caries, or visible defects and to confirm the presence of a straight, single canal with completely formed apex, as well as to rule out the presence of previous endodontic therapy or calcifications. Any teeth with flared canals, internal resorption, defects, or cracks were excluded from the study. The study samples were endodontically treated by using hand ProTaper files (Dentsply, Maillefer, Ballaigues, Switzerland) with F4 as the final master apical file and were obturated using the cold lateral technique. Then, each sample was horizontally sectioned, using a precision SAW machine (IsoMet 1000, Buehler, Lake Bluff, IL, USA), leaving a root of 16 mm in length with a flat surface area. Each sample was then measured using a digital caliper in the buccopalatal and mesiodistal directions at the flat sectioned area (cervical area).
The experimental samples were divided into three groups (n = 10) based on the mean root diameter (33.4 ± 3.2 mm2) at the cervical area, and then the mean values were subjected to statistical analysis with the analysis of variance (ANOVA) test to ensure an even distribution of samples within the groups. Group A was restored with metal post and core, group B was restored with zirconia post and core, and group C was restored with PICN post and core.
A customized round metal cap and cylinder-shaped tube were fabricated to simplify the reproduction of an acrylic block for each sample, and a notch was drilled on the block to indicate the buccal side of the tooth. Molten wax (Renfert GmbH, Hilzingen, Germany) was used to cover the root up to 2.0 mm apical to the coronal surface, to obtain 0.2–0.3 mm wax thickness. Then, the tooth was embedded in self-polymerized acrylic resin to 2.0 mm below the coronal level. Thereafter, the root was removed from the acrylic block, and the wax was replaced with polyvinyl silicon impression material (Honigum Light, DMG, Hamburg, Germany), which represents the periodontal ligament.21,22
The coronal portion of gutta percha was removed with a heated hand plugger, and the post space was prepared using a tapered Peeso reamer with a black unimetric 1.0 kit to match the preparation of the root canal (Dentsply Maillefer, Ballaigues, Switzerland). Accordingly, the length of the post space was 11 mm, and the diameter was 1 mm apically and 1.7 mm coronally. The width and length of the post space preparation were standardized for all groups by using the same post space preparation protocol and AF360 milling machine (Amann Girrbach AG, Koblach, Austria).
The post pattern was fabricated by using a prefabricated polycarbonate post that was relined with acrylic resin until passive retention was achieved. The core was fabricated using the same material, and the measurements were standardized: buccal height (5 mm), cingulum height (2 mm), buccopalatal width cervically (5.5 mm) and incisally (1 mm), mesiodistal width cervically (5 mm) and (4.5 mm) incisally (Figure 1).
The resulting standard post and core pattern was scanned using a 3D Ceramill Map 300 scanner (Amann Girrbach AG) to obtain a digital 3D model, and the data were transformed into a standard template library (STL) (Figure 2). The mill command was given to a CAD/CAM Ceramill Motion 2 milling machine (Amann Girrbach AG) to begin the milling of the zirconia (Ceramil ZI, Amann Girrbach AG) post and core. The STL design data were used to fabricate 10 PICN (Vident, Brea, CA, USA) post and core assemblies using a different milling unit (Galaxy BioMill, Biolase, USA) (Figure 1).
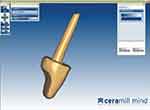 |
Figure 2 Image of scanned three-dimensional post and core tooth using CAD/CAM Ceramill Mind software. Image courtesy of Amann Girrbach GMBH, Pforzheim, Germany. |
To fabricate 10 metal (nickel–chrome alloy) (Argeloy N.P. Special, Argen, Hannover, Germany) post and core assemblies, 10 pieces of standard post and core wax patterns were prepared with a CAD/CAM milling machine and Ceramil wax blocks (Amann Girrbach AG).
The fitness of the post in the canal space preparation was confirmed and the cast posts and cores were sandblasted with aluminum oxide particles (50 μm) under 2 bar pressure for 10 s and then were cleaned under ultrasonic vibration with distilled water. The post space was cleaned with 1.0% sodium hypochlorite solution, rinsed with normal saline, and dried using paper points.23 Then, all posts were cemented with dual-cure resin cement (Panavia F 2.0, Kuraray Company, Osaka, Japan). The cementation process was standardized in all samples by applying a 500 g load to each specimen for 5 mins.24 The samples then remained undisturbed for 15 mins, prior to storage in a 100% humidity environment at 37°C for 1 week, to ensure full polymerization of the resin cement.
Before sectioning the crown from the root, an impression of each crown sample was taken using silicon impression material. This impression was used as a wax mold for the central incisor. Another impression was obtained for each core sample, and after the cementation of the post and core, type IV extremely hard stone Marmorock® 20 (Siladent, Goslar, Germany) was poured into the impression. Molten wax (Renfert, Germany) was placed inside the mold of the crown, and the die stone of the core was inserted into the molten wax. After the wax cooled, the core and wax separated from the crown mold, and the cervical margins of the wax were adjusted. To create a standard loading point on the crown, a notch (0.5 mm deep × 2 mm long, and 3 mm under the incisal edge) was carved into the palatal surface of the wax buildup. Then, the wax pattern crown was cast with the Co–Cr alloy Argeloy N.P. Special (ARGEN, Hannover, Germany). The same protocol for post and core cementation was followed for crown cementation.
Each specimen (post and core covered with crown) was mounted with a metal cylindrical mold on a steel custom-made block with an inclination of 45°. Then, the specimen was subjected to fracture resistance test using a universal testing machine (Testometric, UK). The force was loaded with a custom chisel head (size 1.2 mm) at a crosshead speed of 1 mm/min. The force was applied at an angle of 135° to the long axis of the crown on the palatal side (Figure 3). The point of fracture was defined by an abrupt drop in the strain–stress diagram, and the fracture was recorded as the point at which the loading force reached a maximum value.7 The test was continued until there was split or fracture of the root, which was examined under a stereomicroscope (Pyser-SGI Limited, Edenbridge, UK) to determine the failure mode. The failure was considered favorable and potentially repairable when it was represented by a fracture of the post only or root fracture above the level of the acrylic resin. On the other hand, a nonfavorable fracture was a root fracture below the level of the acrylic resin, including a vertical fracture.25–27
 |
Figure 3 The image shows custom-made assemblies, starting from the superior part; the chisel head is pointed at 135° on the palatal surface of the tested tooth. |
Statistical Analysis
Statistical analysis was carried out using SPSS software (IBM SPSS statistics version 22, Chicago, IL, USA). One-way analysis of variance (ANOVA) was used to analyze the differences in fracture resistance force (in Newtons) between post and core samples fabricated of metal, zirconia, and PICN. The Chi-square test was used to calculate failure modes and the number of samples with favorable or nonfavorable fractures.
Results
The ANOVA results revealed no significant difference in fracture resistance force among metal, zirconia, and PICN post and core samples (P = 0.114). The mean and SD of the fracture resistance of the metal, zirconia, and PICN post and core samples were (324.05 N ± 71.47), (328.06 N ± 54.37), and (271.06 N ± 69.57), respectively.
According to the Chi-square test, there were no significant differences in favorable or non-favorable fractures between study groups. All samples in the metal and zirconia groups exhibited a nonfavorable fracture (Figures 4 and 5), whereas in the PICN group, there were seven samples with a nonfavorable fracture, and three samples showed a favorable fracture represented by a core fracture only (Figure 6). Furthermore, there was a highly significant difference in the post–core fractures between the study groups. Metal post–cores showed no fracture, while all PICN and zirconia post–cores demonstrated post–core fractures. Moreover, two samples exhibited longitudinal root fracture, one in the metal group and another in the zirconia group.
 |
Figure 4 Stereomicroscopic images show a nonfavorable fracture in the metal group; notice the bending of the metal post. |
 |
Figure 5 Stereomicroscopic images show a nonfavorable root fracture and post–core fracture in the zirconia group. |
 |
Figure 6 Stereomicroscopic images show a favorable root fracture and post–core fracture in the PICN group. |
Discussion
This study examined the use of different post and core materials to restore endodontically treated maxillary anterior teeth; the maxillary central incisor was used because it is an acceptable model for these types of in vitro studies.28 Although the use of artificial teeth may produce a large variation in the results of the study, the variations in the root canal morphology of tooth samples may also cause variations in the results. Accordingly, the mean of the cervical area diameter was calculated using the ellipse area equation (area = π r1r2) to ensure even distribution of samples in the study groups, where r1 = semi-major axis or ½ of the major axis (buccopalatal width), r2 = semi-minor axis or ½ the minor axis (mesiodistal width), and π = 3.14159. Nevertheless, the mechanical test results may still be affected by differences in biochemical composition and canal morphology.29,30
The angle between the tooth sample and the testing machine was 135° to mimic a normal clinical situation consisting of the angle formed between the long axis of the mandibular central incisor and maxillary central incisor.31 The findings of this study revealed that the force of resistance to fracture was nonsignificant between study groups (metal, zirconia, and PINC), which indicates that PICN could be a suitable option for restoration of incisors requiring a custom post–core. Although PICN was the material with the least fracture resistance, it remains the material of choice because it has a fracture resistance force higher than the reported maximal occluding force (146 ± 44 N) exerted by a maxillary incisor.32
The similarity in fracture resistance force between metal samples with a mean load value of 324.05 N and zirconia samples of 328.06 N may be due to the fact that zirconia possesses chemical stability, elastic modulus, good mechanical strength, and toughness.33 This is in agreement with the findings of Abduljabbar et al, who showed that CAD/CAM zirconia posts had the highest modulus of elasticity among different tested posts.34
All samples in the metal and zirconia groups exhibited nonfavorable fractures, which could be related to a mismatch in the modulus of elasticity between the root dentin and post material. Another explanation is that there was a difference in the stress distribution of the load on the restoration system, which contained different rigidity components. The component with high rigidity is able to resist forces without distortion, and the stress transfer to the component with less rigidity causes fracture.9 The distribution of the occlusal forces along the root length is affected by the rigidity of the post, which should be close or equal to the rigidity of the root itself.35
The similarity in the mode of failure between the metal and zirconia groups has been proved in a study by Abduljabbar et al,34 who stated that “The failure modes between milled zirconia posts and cast metal posts were similar and classified as a non-restorable fracture.”
In the present study, the posts and cores in the metal group exhibited no fracture due to the superior bending characteristic and high elastic modulus of the metal in comparison to that of the tooth structure, while the samples in the zirconia group exhibited a combined post-root fracture. This is supported by the study by Soundar et al,36 who noted that all samples with cast metal post–cores exhibited tooth fracture, while all-ceramic post–core samples revealed fracture of the post.
For the PICN group, seven samples exhibited a nonfavorable fracture, and three samples showed a favorable fracture represented by postfracture only. The presence of both modes of failure in the PICN group is related to the differences in the elastic modulus between PICN and the root dentin of the study samples. When the elastic modulus of PICN (30 GPa) is close to that of dentin with a range of 10–30 GPa,5 this will lead to the creation of a mechanically homogenous unit,37 and favorable fracture will occur. This finding is in agreement with studies by Bitter and Kielbassa, and Cagidiaco et al,38,39 who found that materials with a low elastic modulus will bend early under load, leading to failure before root fracture occurs. This may be considered as a protective mechanism for the tooth structure.
It was observed that one sample in each group (metal and zirconia) exhibited a buccal vertical (longitudinal) crack along the root. This is explained by the force applied to the palatal aspect of the teeth restored with cast post and core, with the stresses then becoming concentrated on the coronal labial third and apical palatal aspects of the root.40 This observation was in agreement with the research findings of Abduljabbar et al34 who found that there were multiple cracks in the root body that could be restored with a zirconia post in comparison to those restored with fiber posts.
Conclusions
There was no significant difference in the fracture resistance force between metal, zirconia, and PINC post and core samples. PICN could be an alternative to metal and zirconia that can be used in the fabrication of a CAD/CAM post and core. There was no significant difference between metal and zirconia samples in terms of nonfavorable fracture, while a few of the PICN samples exhibited a favorable fracture represented by core fracture only without root fracture.
Disclosure
The authors report no conflicts of interest in this study.
References
1. Vire DE. Failure of endodontically treated teeth: classification and evaluation. J Endod. 1991;17(7):338–342. doi:10.1016/S0099-2399(06)81702-4
2. Naumann M, Preuss A, Rosentritt M. Effect of incomplete crown ferrules on load capacity of endodontically treated maxillary incisors restored with fiber posts, composite buildups, and all-ceramic crowns: an in vitro evaluation after chewing simulation. Acta Odontol Scand. 2006;64(1):31–36. doi:10.1080/00016350500331120
3. Deutsch AS, Musikant BL, Cavallari J, Lepley JB. Prefabricated dowels: a literature review. J Prosthet Dent. 1983;49(4):498–503. doi:10.1016/0022-3913(83)90310-4
4. Cheung W. A review of the management of endodontically treated teeth. Post, core and the final restoration. J Am Dent Assoc. 2005;136(5):611–619. doi:10.14219/jada.archive.2005.0232
5. Plotino G, Grande NM, Bedini R, Pameijer CH, Somma F. Flexural properties of endodontic posts and human root dentin. Dent Mater. 2007;23(9):1129–1135. doi:10.1016/j.dental.2006.06.047
6. Ma J, Miura H, Okada D, Yusa K. Photoelastic stress analysis of endodontically treated teeth restored with different post systems: normal and alveolar bone resorption cases. Dent Mater J. 2011;30(6):806–813. doi:10.4012/dmj.2011-070
7. Fragou T, Tortopidis D, Kontonasaki E, et al. The effect of ferrule on the fracture mode of endodontically treated canines restored with fiber posts and metal-ceramic or all-ceramic crowns. J Dent. 2012;40(4):276–285. doi:10.1016/j.jdent.2012.01.002
8. Akkayan B. An in vitro study evaluating the effect of ferrule length on fracture resistance of endodontically treated teeth restored with fiber-reinforced and zirconia dowel systems. J Prosthet Dent. 2004;92(2):155–162. doi:10.1016/j.prosdent.2004.04.027
9. Salameh Z, Sorrentino R, Ounsi HF, Sadig W, Atiyeh F, Ferrari M. The effect of different full-coverage crown systems on fracture resistance and failure pattern of endodontically treated maxillary incisors restored with and without glass fiber posts. J Endod. 2008;34(7):842–846. doi:10.1016/j.joen.2008.03.025
10. Zhi-Yue L, Yu-Xing Z. Effect of post-core design and ferrule on fracture resistance of endodontically treated maxillary central incisors. J Prosthet Dent. 2003;89(4):368–373. doi:10.1067/mpr.2003.73
11. Özkurt Z, Işeri U, Kazazoğlu E. Zirconia ceramic post systems: a literature review and a case report. Dent Mater J. 2010;29(3):233–245.
12. Streacker AB, Geissberger M. The milled ceramic post and core: a functional and esthetic alternative. J Prosthet Dent. 2007;98(6):486–487. doi:10.1016/S0022-3913(07)60151-6
13. Guazzato M, Albakry M, Ringer SP, Swain MV. Strength, fracture toughness and microstructure of a selection of all-ceramic materials. Part II. Zirconia-based dental ceramics. Dent Mater. 2004;20(5):449–456. doi:10.1016/j.dental.2003.05.002
14. Bateman G, Ricketts DN, Saunders WP. Fibre-based post systems: a review. Br Dent J. 2003;195(1):43–48. doi:10.1038/sj.bdj.4810278
15. He LH, Swain M. A novel polymer infiltrated ceramic dental material. Dent Mater. 2011;27(6):527–534. doi:10.1016/j.dental.2011.02.002
16. Coldea A, Swain MV, Thiel N. Mechanical properties of polymer-infiltrated-ceramic-network materials. Dent Mater. 2013;29(4):419–426. doi:10.1016/j.dental.2013.01.002
17. Smith CT, Schuman NJ, Wasson W. Biomechanical criteria for evaluating prefabricated post-and-core systems: a guide for the restorative dentist. Quintessence Int. 1998;29(5):305–312.
18. Beuer F, Schweiger J, Edelhoff D. Digital dentistry: an overview of recent developments for CAD/CAM generated restorations. Br Dent J. 2008;204(9):505–511. doi:10.1038/sj.bdj.2008.350
19. Miyazaki T, Hotta Y. CAD/CAM systems available for the fabrication of crown and bridge restorations. Aust Dent J. 2011;56(Suppl1):97–106. doi:10.1111/j.1834-7819.2010.01300.x
20. Abduo J, Lyons K. Rationale for the use of CAD/CAM technology in implant prosthodontics. Int J Dent. 2013;2013:768121.
21. Soares CJ, Pizi EC, Fonseca RB, Martins LR. Influence of root embedment material and periodontal ligament simulation on fracture resistance tests. Braz Oral Res. 2005;19(1):11–16.
22. Rathi A, Chowdhry P, Kaushik M, Reddy P, Roshni R, Mehra N. Effect of different periodontal ligament simulating materials on the incidence of dentinal cracks during root canal preparation. J Dent Res Dent Clin Dent Prospects. 2018 Summer;12(3):196–200. doi:10.15171/joddd.2018.030
23. Da Silva NR, Raposo LH, Versluis A, Fernandes-Neto AJ, Soares CJ. The effect of post, core, crown type, and ferrule presence on the biomechanical behavior of endodontically treated bovine anterior teeth. J Prosthet Dent. 2010;104(5):306–317. doi:10.1016/S0022-3913(10)60146-1
24. Santos-Filho PC, Castro CG, Silva GR, Campos RE, Soares CJ. Effects of post system and length on the strain and fracture resistance of root filled bovine teeth. Int Endod J. 2008;41(6):493–501. doi:10.1111/j.1365-2591.2008.01383.x
25. Akkayan B, Gulmez T. Resistance to fracture of endodontically treated teeth restored with different post systems. J Prosthet Dent. 2002;87(4):431–437. doi:10.1067/mpr.2002.123227
26. Pontius O, Hutter JW. Survival rate and fracture strength of incisors restored with different post and core systems and endodontically treated incisors without coronoraducular reinforcement. J Endodont. 2002;28(10):710–715. doi:10.1097/00004770-200210000-00008
27. Alharbi F, Nathanson D, Morgano SM, Baba NZ. Fracture resistance and failure mode of fatigued endodontically treated teeth restored with fiber-reinforced resin posts and metallic posts in vitro. Dent Traumatol. 2014;30(4):317–325. doi:10.1111/edt.12095
28. Al-Wahadni A, Hamdan S, Al-Omiri M, Hammad MM, Hatamleh MM. Fracture resistance of teeth restored with different post systems: in vitro study. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008;106(2):77–83. doi:10.1016/j.tripleo.2008.03.038
29. Fokkinga WA, Kreulen CM, Le Bell-Rönnlöf AM, Lassila LV, Vallittu PK, Creugers NH. In vitro fracture behavior of maxillary premolars with metal crowns and several post-and-core systems. Eur J Oral Sci. 2006;114(3):250–256. doi:10.1111/j.1600-0722.2006.00357.x
30. Qing H, Zhu Z, Chao Y, Zhang W. In vitro evaluation of the fracture resistance of anterior endodontically treated teeth restored with glass fiber and zircon posts. J Prosthet Dent. 2007;97(2):93–98.
31. Clavijo VG, Reis JM, Kabbach W, Silva AL, Oliveira Junior OB, Andrade MF. Fracture strength of flared bovine roots restored with different intraradicular posts. J Appl Oral Sci. 2009;17(6):574–578.
32. Goodacre CJ, Bernal G, Rungcharassaeng K, Kan JY. Clinical complications in fixed prosthodontics. J Prosthet Dent. 2003;90(1):31–41.
33. Piconi C, Maccauro G. Zirconia as a ceramic biomaterial. Biomaterials. 1999;20(1):1–25.
34. Abduljabbar T, Sherfudhin H, AlSaleh SA, Al-Helal AA, Al-Orini SS, Al-Aql NA. Fracture resistance of three post and core systems in endodontically treated teeth restored with all-ceramic crowns. King Saud Univ J Dent Sci. 2012;3(1):33–38.
35. Lassila LV, Tanner J, Le Bell AM, Narva K, Vallittu PK. Flexural properties of fiber reinforced root canal posts. Dent Mater. 2004;20(1):29–36.
36. Soundar SI, Suneetha TJ, Angelo MC, Kovoor LC. Analysis of fracture resistance of endodontically treated teeth restored with different post and core system of variable diameters: an in vitro study. J Indian Prosthodont Soc. 2014;14(2):144–150.
37. Bijelic J, Garoushi S, Vallittu PK, Lassila LV. Fracture load of tooth restored with fiber post and experimental short fiber composite. Open Dent J. 2011;29(5):58–65.
38. Bitter K, Kielbassa AM. Post-endodontic restorations with adhesively luted fiber reinforced composite post systems: a review. Am J Dent. 2007;20(6):353–360.
39. Cagidiaco MC, Goracci C, Garcia-Godoy F, Ferrari M. Clinical studies of fiber posts: a literature review. Int J Prosthodont. 2008;21(4):328–336.
40. Holmes DC, Diaz-Arnold AM, Leary JM. Influence of post dimension on stress distribution in dentin. J Prosthet Dent. 1996;75(2):140–147.
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

