Back to Journals » International Journal of Nanomedicine » Volume 9 » Issue 1
Enhanced regenerative healing efficacy of a highly skin-permeable growth factor nanocomplex in a full-thickness excisional mouse wound model
Authors Bae I, Park JW , Kim D
Received 25 May 2014
Accepted for publication 19 July 2014
Published 25 September 2014 Volume 2014:9(1) Pages 4551—4567
DOI https://doi.org/10.2147/IJN.S68399
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 5
Il-Hong Bae,1 Jin Woo Park,2 Dae-Yong Kim1
1College of Veterinary Medicine, Seoul National University, Seoul, Republic of Korea; 2College of Pharmacy and Natural Medicine Research Institute, Mokpo National University, Muan-gun, Jeonnam, Republic of Korea
Abstract: Exogenous administration of growth factors has potential benefits in wound healing; however, limited percutaneous absorption, inconsistent efficacy, and the need for high doses have hampered successful clinical use. To overcome these restrictions, we focused on the development of a topical formulation composed of highly skin-permeable multimeric nanocomplex of growth factors. In the present study, we fused low-molecular-weight protamine (LMWP) with epidermal growth factor (EGF), insulin-like growth factor 1 (IGF-I), and platelet-derived growth factor A ligand (PDGF-A) (producing recombinant [r]LMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A, respectively) via genetic modification. Then, we used in vitro cell proliferation studies to assess the biological activity and the benefits of the combination. The LMWP-conjugated growth factors were complexed with low-molecular-weight heparin (LMWH) and formulated with Poloxamer 188 as a delivery vehicle. After confirming the enhanced skin permeability, in vivo studies were performed to assess whether the LMWP-conjugated growth factor nanocomplex formulations accelerated the healing of full-thickness wounds in mice. The LMWP-conjugated growth factors were biologically equivalent to their native forms, and their combination induced greater fibroblast proliferation. rLMWP-EGF showed significantly enhanced permeability and cumulative permeation, and the rates for rLMWP-IGF-I and rLMWP-PDGF-A, across excised mouse skin, were 124% and 164% higher, respectively, than for the native forms. The LMWP-fused growth factors resulted in formation of nanocomplexes (23.51±1.12 nm in diameter) in combination with LMWH. Topical delivery of growth factors fused with LMWP accelerated wound re-epithelialization significantly, accompanied by the formation of healthy granulation tissue within 9 days compared with a free–growth factor complex or vehicle. Thus, the LMWP-conjugated growth factor nanocomplex can induce rapid, comprehensive healing and may be a candidate wound-healing therapeutic.
Keywords: epidermal growth factor, insulin-like growth factor, platelet-derived growth factor
Introduction
Wound healing is a complex, interactive cellular, and biochemical process involving inflammation, proliferation, and migration of various cell types, leading to tissue regeneration and remodeling. During this dynamic process, tissue repair is accelerated or inhibited by matrix synthesis, collagen deposition that leads to re-epithelialization, neovascularization, the formation of granulation tissue by numerous cells, and the production of growth factors and cytokines.1 Growth factors, such as platelet-derived growth factor (PDGF), epidermal growth factor (EGF), insulin-like growth factor (IGF), vascular endothelial growth factor (VEGF), fibroblast growth factor (FGF), and transforming growth factor (TGF), are key modulators of wound healing and tissue repair that affect chemotaxis and stimulate mitosis of quiescent cells, angiogenesis, and synthesis and degradation of the extracellular matrix (ECM).2
Among the major growth factors related to wound healing, EGF, produced by platelets, macrophages, and monocytes, stimulates epidermal and mesenchymal regeneration and cell motility via interactions with the EGF receptor on epidermal cells and fibroblasts. Thus, endogenous expression of EGF is upregulated markedly in cutaneous wound areas, and exogenously delivered EGF accelerates re-epithelialization.3,4
IGF factor 1 (IGF-I) is widely distributed in various tissues, including skin, and is structurally related to proinsulin. IGF-I is strongly expressed in injured areas, where it plays an important role in epidermal and dermal wound healing. Repeated studies have shown the beneficial effects of exogenously applied IGF-I, alone or in combination with its binding proteins and other growth factors, on wound healing, supporting its use in stimulating collagen synthesis in fibroblasts, the proliferation of fibroblasts and keratinocytes, and angiogenesis.5,6
PDGF family members are expressed by platelets, macrophages, vascular endothelium, fibroblasts, and keratinocytes. PDGF is a strong mitogen for cells of mesenchymal origin, such as fibroblasts and smooth muscle cells. PDGF also regulates the maturation of blood vessels and re-epithelialization, by increasing the production of IGF-I and thrombospondin-1. Since PDGF stimulates the proliferation of fibroblasts, it increases ECM production, narrows the collagen matrix, and induces myofibroblasts.7
Therefore, the exogenous delivery of growth factors is a promising approach for accelerating wound repair and is in the preclinical stages of pharmaceutical development.8 Additionally, the PDGF B homodimer (PDGF-BB), known as becaplermin or Reganex® (Smith and Nephew plc, London, UK), has successfully completed clinical trials and is the only growth factor-based product approved by the US Food and Drug Administration. Recombinant EGF-based products are available worldwide for treatment of chronic diabetic ulcers.
However, major obstacles remain in the application of exogenous growth factors for optimal wound healing efficacy because growth factors are readily degraded by proteinases, removed by exudate before reaching the wound area, or have difficulty permeating through the outermost layer of skin around the wound due to the strong barrier function of the stratum corneum to hydrophilic macromolecular drugs.9,10
To increase the wound-healing efficacies of exogenously applied growth factors, various delivery systems, such as hydrogels, sponges, polymeric micelles, electrospun nanofibers, microspheres, a coacervate delivery system with heparin, and a biomimetic delivery system incorporating growth factors with biocompatible ECM components, such as hyaluronic acid, collagen, and vitronectin, have been used to produce sufficiently high local concentrations of growth factors for sustained periods.11–14 However, these systems have pharmacokinetic limitations, such as poor loading efficacy, loss of bioactivity during preparation and after application, and diffusion through the skin. Additionally, each growth factor is present at different healing stages, has specific functions, and acts at its target site via interactions with its receptor, other growth factors, and ECM components.15,16
However, some single-application growth factors have failed to show sufficient wound repair versus controls, suggesting that a cocktail of growth factors may be a more promising treatment, to accelerate wound healing by promoting the growth of epithelial and connective tissue, as well as the synthesis of total protein and collagen.17,18 Lynch et al applied PDGF-BB and IGF-I to porcine skin wounds of partial thickness and found that the combination acted synergistically to enhance tissue repair by increasing the newly formed connective tissue layer and epidermal thickness.19,20 Greenhalgh et al established the synergy of PDGF and IGF factor 2 (IGF-II) in full-thickness skin wounds of diabetic mice, while Krane et al showed that a combination of EGF with IGF-I or high-dose insulin accelerated the spread and proliferation of keratinocytes compared with each growth factor alone.21,22
Heparin is a highly sulfated glycosaminoglycan composed of alternating-hexuronic acid and D-glucosamine residues that are linked by glycosidic bonds with similar functionalities to heparin sulfate. Clinically, heparin is used as an anticoagulant, and it also modulates several phases of wound healing and specifically interacts with a variety of proteins, including growth factors, via heparin-binding domains.23,24 Therefore, many studies have incorporated heparin with growth factors as a delivery vehicle, maintaining high concentrations around a wound by protecting the growth factors from proteolytic degradation, and increasing their biological activity by promoting binding with their receptors.25,26
Recently, we designed an enhanced percutaneous delivery system for EGF by the genetic conjugation of a highly positively charged low-molecular-weight protamine (LMWP), as a protein transduction domain (PTD) (VSRRRRRRGGRRRR), to the N-terminus of EGF; the conjugated LMWP increased in vitro skin permeability markedly and accelerated wound healing efficacy significantly, in acute and diabetic full-thickness wounds and in a laser-induced burn wound model, due to its rapid and considerable absorption in the wound area.27,28 In the present study, we constructed a topical formulation consisting of highly skin-permeable recombinant growth factors and low-molecular-weight heparin (LMWH) nanocomplexes, for multitargeted wound-healing efficacy. To maintain the native biological properties of the growth factors as well as to increase their skin permeability, we fused the cell-penetrating peptide LMWP with the N-terminus of EGF, IGF-I, and PDGF A ligand (PDGF-A) (producing recombinant [r]LMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A, respectively) via genetic modification. Then, in vitro experiments were performed to characterize the biological activities and skin penetration-enhancing effects of each compound. In addition, the proliferation of fibroblasts in the presence of combinations of native or LMWP-conjugated growth factors was evaluated to assess the synergistic effects of the growth factor combinations. We also prepared nanocomplexes by combining the LMWP-fused growth factors with LMWH, and then formulating them with Poloxamer 188 as a delivery vehicle to enhance their synergistic wound healing activities and resistance to enzymatic degradation. The LMWP-fused growth factors can bind with LMWH via their heparin binding domain, as well as more specific polyionic interactions via the conjugated LMWP, a nontoxic arginine-rich peptide derived from protamine. We further investigated the in vitro characteristics of the native and LMWP-fused growth factor nanocomplexes and conducted in vivo studies to assess whether the novel complexes (versus native complexes) accelerated healing of full-thickness wounds in mice. These in vivo experiments were designed to investigate the coordinated effect of the combination of rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A on the stimulation of re-epithelialization and the regeneration of connective tissue.
Materials and methods
Materials
Recombinant human (rh)EGF, rhIGF-I, and rhPDGF-A were obtained from BIO-FD&C Co., Ltd. (Whasun, Jeonnam, Republic of Korea). LMWH (fraxiparine, 4,500 Da) was from Nanjing King-Friend Biochemical Pharmaceutical (Nanjing, People’s Republic of China). A polyethylene polyoxypropylene block copolymer (Poloxamer 188) for the topical gel formulation was from BASF (Ludwigshafen, Germany). Solvents for high-performance liquid chromatography (HPLC) analyses were from Merck KGaA (Darmstadt, Germany) and Thermo Fisher Scientific Inc. (Waltham, MA, USA).
Preparation of LMWP-conjugated growth factors
EGF carrying LMWP at its N-terminus was prepared as described previously.27,28 rLMWP-IGF-I and rLMWP-PDGF-A were also prepared with an expression plasmid, which overproduced a protein containing rLMWP-IGF-I and LMWP-PDGF-A in Escherichia coli in a similar manner to rLMWP-EGF. Briefly, as the first template, complementary (c)DNAs for rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A were constructed by serial polymerase chain reaction (PCR)-mediated addition of the LMWP codons to the rhEGF, rhIGF-I, and rhPDGF-A genes (GenBank accession numbers P01133, P03143, and NP-008808.3, respectively). Subsequently, the rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A gene fragments were amplified by PCR. To incorporate the cDNA for rLMWP-EGF, rLMWP-IGF-I or rLMWP-PDGF-A between NdeI and XhoI restriction sites, the forward primer for amplifying rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A was 5′-CATATGGTGAGCCGTAGACGTAGACG-3′ and the respective reverse primers for rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A were 5′-CTCGAGTCATTAGCGCAGTTCCCACCACTTCAGGTCTCGGT-3′, 5′-CTCGAGTCATTAAGCTGACTTGGCAGGCTTGAGGGGTGCGC-3′, and 5′-CTCGAGTCATTAGGTGGGTTTTAACCTTTTTCTTTTCCGTT-3′. Then, the resulting PCR products were subcloned into a TOPO vector. After plasmid purification and digestion with NdeI/XhoI, the sequence was confirmed by capillary sequencing and then cloned into the pET-41b(+) expression vector. pET-41b(+)-LMWP-EGF, pET-41b(+)-LMWP-IGF-I, or pET-41b(+)-LMWP-PDGF-A was transformed into competent E. coli cells (BL21-DE3) and cultured at 37°C in potassium-modified Luria broth (LBK) medium supplemented with 100 μg/mL ampicillin until the optical density of the culture at 600 nm was 0.6–0.8. Protein expression was induced by adding 1 M isopropyl-β-D-thiogalactopyranoside (IPTG), and the cells were grown overnight at 25°C with shaking at 100 rpm. The cells were collected by centrifugation (6,000× g for 10 minutes at 4°C), resuspended in cell lysis buffer (sodium phosphate buffer, pH 7.5, containing 10 mM NaCl), and sonicated at 50% amplitude following a 10/10-second sonication/holding cycle. The supernatant, containing rLMWP-EGF, rLMWP-IGF-I, or rLMWP-PDGF-A, was collected by centrifugation (12,000× g, 10 minutes, 4°C) and filtered through a 0.45 μm membrane (EMD Millipore, Billerica, MA, USA) before further analysis. After the expression of rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A, no insoluble aggregates or inactivation was observed. Therefore, no additional protein-refolding process was required.
The expressed rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A were purified using ion-exchange chromatography on a Q-cellulose resin. Briefly, the filtered supernatant was loaded onto a Q-cellulose column and circulated for 30 minutes. After elution of the unbound material, the column was washed twice with 5 mM sodium phosphate buffer, pH 7.5, containing 50 mM NaCl (buffer A) for 10 minutes. Then, the column was washed once with 5 mM sodium phosphate buffer, pH 7.5, containing 100 mM NaCl (buffer B) for 30 minutes and eluted using elution buffer (5 mM sodium phosphate buffer, pH 7.5, containing 500 mM NaCl). The eluate was concentrated 20× by ultrafiltration (Amicon®, cutoff membrane 3,000 Da). The concentrated fractions, containing rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A were next applied to a Sephadex® G-100 column and eluted with running buffer (20 mM sodium phosphate buffer, pH 7.5, containing 500 mM NaCl). The fractions containing purified rLMWP-EGF, rLMWP-IGF-I, or rLMWP-PDGF-A were collected from the column and then diluted with 20 mM sodium phosphate buffer (pH 7.5) to a NaCl concentration of 150 mM.
The purified rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A were quantified using a Micro BCA Protein Assay kit (Pierce, Rockford, IL, USA) with bovine serum albumin as the standard. Purity was analyzed by sodium dodecyl sulfate-polyacrylamide gel electrophoresis (SDS-PAGE) with Coomassie blue staining. The actual molecular weight (MW) was determined by matrix-assisted laser desorption/ionization time-of-flight mass spectroscopy (Applied Biosystems 4800 Plus; Life Technologies Corp., Carlsbad, CA, USA).
To confirm LMWP conjugation, the N-terminal amino acid sequences of the purified rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A were also determined. The samples were separated by SDS-PAGE and transferred to polyvinylidene fluoride (PVDF) membranes presoaked in methanol. The membrane was stained with 0.5% Coomassie Blue R in 50% methanol and rinsed with 50% methanol. The stained bands were excised from the membrane and analyzed by N-terminal sequencing, using an Applied Biosystems Procise 491 protein sequencer (Life Technologies Corp.).
Cell proliferation assay
To evaluate the biological activities of rLMWP-EGF, rLMWP-IGF-I, rLMWP-PDGF-A, and the growth factor complexes, a cell proliferation assay was performed. Mouse NIH 3T3 fibroblasts were seeded at a density of 5×103 cells per well in 100 μL Dulbecco’s Modified Eagle’s Medium (DMEM) (Lonza, Zurich, Switzerland) containing 10% fetal bovine serum (FBS) (Gibco®; Life Technologies Corp.) and 1% penicillin/streptomycin (Gibco®; Life Technologies Corp.) and cultured at 37°C for 24 hours. Then, the serum concentration in the medium was lowered to 0.05%, and the cells were incubated for a further 24 hours. The cells were treated with rhEGF, rhIGF-I, rhPDGF-A, rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A, alone or in combinations. Each growth factor was added at a concentration of 100 ng/mL in low-serum medium (0.5% FBS), and the cells were cultured for an additional 24 hours. To determine cell proliferation activity, the Water-soluble tetrazolium salt-1 (WST-1) assay (F. Hoffman-La Roche Ltd., Basel, Switzerland) was performed following the manufacturer’s protocol. Briefly, a diluted WST-1 solution (5 mg/mL in phosphate-buffered saline [PBS]) was added and incubated for 2 hours. The absorbance was measured with a spectrophotometer (Molecular Devices LLC, Sunnyvale, CA, USA) at 450 nm. The percentage of viable cells was calculated by comparing the values of treated cells with those of untreated cells.
Preparation and characterization of growth factor nanocomplex
Native and LMWP-conjugated growth factor nanocomplexes were prepared by combining each growth factor with LMWH. Briefly, rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A were each dissolved at 300 μg/mL in deionized water and then mixed together under continuous stirring. The weight ratio of rLMWP-EGF to rLMWP-IGF-I to rLMWP-PDGF-A was 1:1:1, and the concentration of each growth factor in the solution was 100 μg/mL. The solution was added dropwise to a 1 mg/mL LMWH aqueous solution with continuous agitation. In the same manner, the native growth factor complex was also prepared with rhEGF, rhIGF-I, rhPDGF-A, and LMWH. After complex formation, the particle size, size distribution, and zeta potential of the prepared growth factor complexes were measured using a dynamic light-scattering analyzer (Zetasizer AS90; Malvern Instruments, Malvern, UK). A morphological evaluation of the growth factor complexes was also performed by transmission electron microscopy (TEM) (JEM-200; JEOL Ltd., Tokyo, Japan). The complex solution was diluted 50-fold with distilled water and then deposited onto a carbon grid. After staining with uranyl acetate solution for 1 minute, the excess solution was removed using filter paper and negatively stained with phosphor tungsten acid solution. Samples were viewed using a TEM.
In vitro artificial skin permeability
The in vitro artificial skin permeability of rhEGF, rhIGF-I, rhPDGF-A, rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A was evaluated using a Skin PAMPA Explorer Test System (Pion Inc., Billerica, MA, USA). Each well of the top (acceptor) compartment of a STIRWELL™ PAMPA sandwich plate, which was precoated with 10 μL skin-mimetic artificial membrane component (ceramide, cholesterol, stearic acid, and silicone oil), was hydrated with 200 μL diluted hydration solution (pH 7.4) overnight. Before forming the sandwich, the bottom (donor) plate was prefilled with 200 μL rhEGF, rhIGF-I, rhPDGF-A, rLMWP-EGF, rLMWP-IGF-I, or rLMWP-PDGF-A dissolved in the Prisma-HT buffer solutions (pH 7.4) with 6% (w/v) Poloxamer 188 at a concentration of 100 μg/mL. The acceptor plate was also filled with 200 μL Prisma-HT buffer solution (pH 7.4), and then the resulting sandwich was incubated at room temperature. After 4, 6, 8, and 24 hours, each PAMPA sandwich was separated, and 150 μL of both the donor and acceptor were collected. The rhEGF, rhIGF-I, and rhPDGF-A concentrations were determined using a solid-phase sandwich enzyme-linked immunosorbent assay (ELISA) at 450 nm (Invitrogen; Life Technologies Corp.). For rLMWP-EGF, 20 μL aliquots from each sample were injected into an HPLC system equipped with a Phenomenex Gemini C18 column (250×4.6 mm, 10 μm), and the samples were chromatographed using an isocratic mobile phase of acetic acid (1→1,000)-acetonitrile (20:80) at a flow rate of 0.8 μL/min. The quantification of rLMWP-EGF was carried out at 210 nm. The permeated rLMWP-IGF-I and rLMWP-PDGF-A were qualified by HPLC, using a ZORBAX 300SB-CN column (150×4.6 mm, 3.5 μm; 20 μL sample injection). The mobile phase consisted of 0.1% (v/v) trifluoroacetic acid (TFA) with a 25%–75% linear gradient of acetonitrile-water (90:10, v/v) containing 0.1% (w/v) TFA for 60 minutes, at a flow rate of 1.0 mL/min. The rLMWP-IGF-I and rLMWP-PDGF-A were detected using an ultraviolet (UV) detector at 214 nm, and the retention times for rLMWP-IGF-I and rLMWP-PDGF-A were ~39.7 and ~11.6 minutes, respectively.
In vitro permeability through the skin of hairless mice
To compare the skin permeability of native growth factors with those of LMWP-conjugated growth factors, excised skin of hairless mice (Han-Lim Experimental Animal Research Center, Hwaseong, Republic of Korea) was mounted with the stratum corneum facing upwards on the receptor phase compartment of a Franz diffusion cell system (Laboratory Glass Apparatus; Fine Science, Seoul, Republic of Korea) filled with 5.5 mL PBS (pH 7.4). The donor compartment was clamped in place, and the diffusion area was 0.785 cm2. Before adding the test formulations to the donor compartment, the cells were allowed to equilibrate for at least 30 minutes to confirm the integrity of the epidermal membranes. After reaching equilibrium, 200 μL native growth factor nanocomplex (10 μg/mL rhEGF, 10 μg/mL rhIGF-I, 10 μg/mL rhPDGF-A, and 100 μg/mL LMWH) or LMWP-conjugated growth factor complex (10 μg/mL rLMWP-EGF, 10 μg/mL rLMWP-IGF-I, 10 μg/mL rLMWP-PDGF-A, and 100 μg/mL LMWH) solution in 6% (w/v) Poloxamer 188 was added to the donor compartment. The receptor compartment was stirred at room temperature with a water-circulating system to maintain a skin surface temperature of 32°C throughout the experiment. Then, 200 μL of the receptor phase were withdrawn after 1, 3, 6, 9, 12, and 24 hours, and each aliquot was replaced with fresh PBS. The withdrawn samples were filtered through a membrane filter (0.45 μm, PVDF) and kept at 4°C until analysis. Samples from the skin-permeation experiments were quantified using a solid-phase sandwich ELISA for rhEGF, rhIGF-I, and rhPDGF-A, and the HPLC system for the permeated rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A. Data were expressed as the fluxes (μg/cm2·h), calculated by linear regression interpolation of the cumulative permeation per unit of skin surface area and hour.
In vivo wound healing efficacy of growth factor complexes
To assess the wound-healing efficacy of LMWP-conjugated growth factor complex, 6- to 7-week-old female hairless mice (Orient, Gyeonggi-do, Republic of Korea) were acclimated for 1 week in an animal facility under controlled temperature (23°C±3°C), relative humidity (55%±10%), and light (12/12-hour light/dark cycle, with no UV exposure) conditions. The animals had free access to a laboratory diet (Purina Co., St Louis, MO, USA) and ion-sterilized tap water. All experiments were performed in accordance with the guidelines of Institutional Animal Care and Use Committee (IACUC) of Seoul National University (Seoul, Republic of Korea).
For in vivo full-thickness wound healing studies, the mice were anesthetized with isoflurane (4%) and two 0.5 mm-thick silicone splits, with a 8 mm diameter hole, were fixed on either side of the dorsal midline, to avoid skin contraction. Two identical, circular, full-thickness wounds were made using a 6 mm round biopsy punch, centered within each split of each mouse, and the wound area was sterilized with a povidone/iodine solution. After 1 day, each wound area was treated topically twice per day for 9 days, with 30 μL vehicle (Poloxamer 188, 6% [w/v]) alone or with vehicle containing one of the following: 10 μg/mL rhEGF; 10 μg/mL rLMWP-EGF; 10 μg/mL rhIGF-I; 10 μg/mL rLMWP-IGF-I; 10 μg/mL rhPDGF-A; 10 μg/mL rLMWP-PDGF-A; native growth factor combination (10 μg/mL each of rhEGF, rhIGF-I, and rhPDGF-A); LMWP-conjugated growth factor combination (10 μg/mL each of rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A); native growth factor nanocomplex (10 μg/mL each of rhEGF, rhIGF-I, and rhPDGF-A, with 100 μg/mL LMWH); or LMWP-conjugated growth factor nanocomplex (10 μg/mL each of rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A, with 100 μg/mL LMWH). The degree of wound healing on the dorsal skin was evaluated by measuring the area of the wound, using a digital camera (PowerShot G9; Canon, Tokyo, Japan) and an image-analysis software package (cellSens Standard; Olympus Corp., Tokyo, Japan). The rate of wound healing was expressed as the percentage of the remaining wound area.
On days 2 and 4, three animals per group were sacrificed, and wounds and surrounding tissues were sampled by a biopsy punch. The remaining animals were sacrificed on day 9. The excised wound tissues were immediately fixed in 10% neutral phosphate-buffered formalin, processed routinely, and embedded in paraffin wax. For standard evaluation, the tissues embedded in paraffin wax were cut to a thickness of 6 μm and stained with hematoxylin and eosin (H&E). Additionally, replicate sections were used for immunohistochemical staining of cytokeratin 6 (CK6), to detect activated keratinocytes in the wound.29 Briefly, tissues were incubated with polyclonal rabbit anti-CK6 antibody (PRB-169P; Covance, Princeton, NJ, USA) as the primary antibody at 4°C overnight and then, with a secondary anti-rabbit HRP conjugated antibody (ab6802; Abcam, Cambridge, UK) for 1 hour. To investigate α-smooth muscle actin (α-SMA) expression in specimens from the wound model, the paraffin block was sectioned to 3 μm thickness, and sections were deparaffinized. For immunostaining, the tissue was incubated with polyclonal rabbit anti-α-SMA antibody (1184-1; Epitomics, Burlingame, CA, USA) as the primary antibody for 1 hour at room temperature and then was subsequently incubated for 10 minutes in a secondary anti-rabbit HRP conjugated antibody (D39-15; Golden Bridge International, New York, NY, USA). All simultaneously stained sections were examined under light microscopy (Olympus Bx-41), and photomicrographs were taken with a DP72 camera (Olympus).
Statistics
All data were expressed as mean ± standard deviation. A P-value of less than 0.05 was considered to indicate statistical significance, using a t-test between two mean values for unpaired data, or one-way analysis of variance (ANOVA) followed by Tukey’s multiple comparison test among more than three mean values for unpaired data.
Results
Expression and purification of rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A
To fuse LMWP with the N-terminus of rhEGF, rhIGF-I, and rhPDGF-A, the amino acid sequence of LMWP was successively encoded and amplified by PCR, using the rhEGF, rhIGF-I, and rhPDGF-A genes as templates. After subcloning into the TOPO vector, we constructed a pET-41b(+) expression vector containing the cDNAs for rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A. The sequence of the insert DNA was confirmed by automated DNA sequencing (data not shown). The rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A cDNAs were expressed in E. coli, purified, and analyzed by SDS-PAGE (Figure 1A). The rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A proteins produced bands with apparent molecular weights of ~8.2, 9.5, and 16.3 kDa, respectively, representing >95% of the total proteins in the densitometric quantification using BandScan software. The actual MWs of rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A determined by mass spectroscopy were 8,047.4, 9,083.8, and 16,119.7 Da, respectively and were consistent with the theoretical and apparent MWs on SDS-PAGE (Figure 1B). The N-terminal amino acid sequences of the purified rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A were determined, with a protein sequencer, to verify the N-terminus-specific conjugation of LMWP with rhEGF, rhIGF-I, and rhPDGF-A. Figure 1C shows representative chromatograms for amino acids 2, 6, 14, and 16 of rLMWP-IGF-I and rLMWP-PDGF-A. The sequences of rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A were consistent with the theoretical sequences: Val-Ser-Arg-Arg-Arg-Arg-Arg-Arg-Gly-Gly-Arg-Arg-Arg-Arg-Asn-Ser for rLMWP-EGF, Val-Ser-Arg-Arg-Arg-Arg-Arg-Arg-Gly-Gly-Arg-Arg-Arg-Arg-Gly-Pro for rLMWP-IGF-I, and Val-Ser-Arg-Arg-Arg-Arg-Arg-Arg-Gly-Gly-Arg-Arg-Arg-Arg-Ser-Ile for rLMWP-PDGF-A.
Biological activity
To determine the biological activity of LMWP-conjugated growth factors, we examined the effects of rhEGF, rhIGF-I, rhPDGF-A, rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A, alone or in combinations, on the proliferation of NIH 3T3 cells. As shown in Figure 2, the conjugation of LMWP showed higher rates of cell proliferation than each unconjugated growth factor, although no statistically significant difference was found. These results suggest that the native biological activity of each growth factor was not altered by the conjugation of LMWP. Subsequently, we investigated the mitogenic effects of combinations of native growth factors or LMWP-conjugated growth factors. The cell viability values for rhEGF + rhIGF-I, rhEGF + rhPDGF-A, rhIGF-I + rhPDGF-A, and rhEGF + rhIGF-I + rhPDGF-A were 133.94%±3.70%, 148.36%±3.28%, 157.85%±5.02%, and 169.70%±3.74% higher than those of the control group, respectively. However, rhEGF, rhIGF-I, and rhPDGF-A alone showed 110.86%±1.15%, 113.27%±1.91%, and 136.90%±2.66% increases in cell proliferation compared with the control group, respectively. After simultaneous addition of rLMWP-PDGF-A to rLMWP-EGF and/or rLMWP-IGF-I, the cell viability values of rLMWP-EGF + rLMWP-PDGF-A, rLMWP-IGF-I + rLMWP-PDGF-A, and rLMWP-EGF + rLMWP-IGF-I + rLMWP-PDGF-A were 1.31-, 1.43-, and 1.43-fold higher than that of rLMWP-EGF; 1.23-, 1.34-, and 1.35-fold higher than that of rLMWP-IGF-I; and 1.14-, 1.24-, and 1.24-fold higher than that of rLMWP-PDGF-A, respectively. Thus, all combinations resulted in a higher proliferative response than each growth factor alone. The combination of rhPDGF-A or rLMWP-PDGF-A with other growth factors exhibited greater synergistic effects on cell proliferation.
Characterization of growth factor nanocomplexes
After combining LMWH with rhEGF, rhIGF-I, and rhPDGF-A, or with rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A, the growth factor combinations formed nanocomplexes. As shown in Figure 3, the native growth factor nanocomplex was 77.16±5.30 nm in size, with a zeta potential of −33.5 to −31.3 mV. The mean diameter of the LMWP-conjugated growth factor nanocomplex was 23.51±1.12 nm, and it displayed negative surface charges, with a zeta potential of −33.9±0.5 mV. TEM images of the LMWP-conjugated growth factor nanocomplex revealed more regular and well-defined spherical nanoparticles than those of the native growth factor nanocomplex.
In vitro skin permeability study
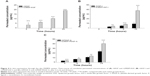
The skin penetration–enhancing effect of LMWP conjugation was evaluated by comparative permeability studies using a Skin PAMPA system. The cumulative penetrated concentrations of rLMWP-EGF were 3.56±2.39, 6.52±0.56, 10.60±0.66, and 19.25±0.07 μg/mL at 4, 6, 8, and 24 hours, respectively. However, rhEGF was not detected in the receptor phase of the skin PAMPA system up to 24 hours (Figure 4A). In the case of rLMWP-IGF-I, its cumulative permeated concentrations were 0.00±0.00, 4.63±0.65, 8.46±0.71, and 38.05±9.14 μg/mL at 4, 6, 8, and 24 hours, respectively (Figure 4B). The penetration of rLMWP-IGF-I through the artificial skin membrane was much faster, and its cumulative permeated concentration after 24 hours was 4.04-fold greater than that of rhIGF-I. The cumulative concentrations of rLMWP-PDGF-A after 4, 6, 8, and 24 hours were 3.77±0.19, 7.35±0.56, 13.59±1.55, and 40.39±5.45 μg/mL, respectively; these values were 1.24-, 1.12-, 1.25-, and 1.73-fold higher than those of rhPDGF-A, respectively (Figure 4C).
Skin penetration of the LMWP-conjugated growth factor nanocomplexes was also examined in hairless mice, and the conjugation of LMWP with rhEGF, rhIGF-I, or rhPDGF-A significantly enhanced skin penetration of these growth factors (Figure 5). After 24 hours incubation, the amounts of rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A that accumulated in the skin chamber were 0.03±0.01, 0.61±0.06, and 1.11±0.07 μg/cm2·h, respectively. In particular, the skin fluxes of rLMWP-IGF-I and rLMWP-PDGF-A were 124% and 164% higher than those of rhIGF-I and rhPDGF-A, respectively. In contrast, rhEGF scarcely permeated the skin after 24 hours.
Effects of growth factor complexes on the full-thickness wound model
The wound healing efficacies of native and LMWP-conjugated growth factors were evaluated in a splinted mouse full-thickness excisional wound model. As shown in Figure 6A and B, rLMWP-EGF and rLMWP-PDGF-A treatment significantly reduced the wound area compared with the rhEGF and rhPDGF-A treatments. At days 4 and 7, the animals treated with rLMWP-EGF showed 123.9% and 106.7% increases in the wound closure rates compared with the animals treated with rhEGF, respectively, and the wound healing rates of rLMWP-PDGF-A were 114.3% and 110.7% higher than those of rhPDGF-A, respectively. The wound area with rLMWP-IGF-I was significantly reduced compared with that of the control at day 4, and the wound healing rate was faster than that of rhIGF-I. However, LMWP conjugation to rhIGF-I did not result in significantly improved wound healing compared with IGF-I. The wound areas of the native growth factor combination treatment group were significantly reduced compared with those of the vehicle, each native growth factor, and LMWP-conjugated EGF or IGF-I group throughout the test period, whereas no significant difference in the wound-healing efficacy was induced by formation of complexes with LMWH. Conversely, the LMWP-conjugated growth factor combination treatment revealed superior wound healing activity to all other native and LMWP-conjugated growth factors; its nanocomplex with LMWH also manifested 105.3% and 106.4% increases in the wound-healing rate at days 7 and 9, respectively. In particular, the accelerated closure of wounds treated with a growth factor nanocomplex composed of rLMWP-EGF, rLMWP-IGF-I, rLMWP-PDGF-A, and LMWH was obvious throughout the test period compared with all other groups. Moreover, treatment with the LMWP-conjugated growth factor nanocomplex resulted in a significantly reduced wound area compared with the vehicle controls or treatment with native growth factor nanocomplex, 2 days after wounding (64.37%±5.05% for the LMWP-conjugated growth factor nanocomplex group, 75.01%±8.00% for the native growth factor nanocomplex group, and 84.91%±6.89% for the controls). In particular, the initial wound closure rate of the LMWP-conjugated treatment was significantly higher than those of the other groups. On days 4 and 7, this group showed enhanced wound-healing activity and a significant difference in wound size. The remaining wound sizes at days 4 and 7 were, respectively, 34.91%±2.39% and 8.62%±2.56% for the LMWP-conjugated growth factor nanocomplex group, 60.88%±6.60% and 29.64%±2.46% in the vehicle, 44.24%±5.31% and 22.01%±3.95% in the native growth factor nanocomplex group, and 36.88%±3.71% and 13.22%±3.34% in the LMWP-conjugated growth factor combination. On day 9 after treatment, all wounds treated with the LMWP-conjugated complex appeared to be closed completely, and no scar formation was observed, whereas 14.49%±1.43% and 9.93%±1.87% of the wounds remained in the vehicle and native growth factor nanocomplex groups, respectively.
Histological analysis of the wound site
To assess the efficacy of the topically administered LMWP-conjugated growth factor complex in vivo, a histological examination was performed to confirm the wound closure rates. Figure 7A represents H&E, CK6, and α-SMA immunostaining of the wound sites 2 days after treatment. The re-epithelialized area of skin treated with LMWP-conjugated complex was thicker and larger than that of the native complex or vehicle. Additionally, the neoepidermis layer around the wound edge of the LMWP-conjugated group migrated further into the wound bed than in the other treatment groups. CK6 immunostaining (brown color) was increased around the wound edge in the LMWP-conjugated group, suggesting that activation of keratinocytes in the suprabasal compartment located near the wound edge was increased versus the other groups.30 Thus, the LMWP-conjugated growth factor complex facilitated quicker epithelium regeneration.
Histological analysis after 9 days showed full coverage of the epithelium in all samples except the vehicle control (Figure 7B). The vehicle-treated wounds exhibited cell migration beyond the proliferating cells at the wound margin, and a loosely arranged and disorganized collagen matrix in the wound bed. Additionally, some infiltrating inflammatory cells remained at the wound site. In contrast, wounds treated with native or LMWP-conjugated complex exhibited thicker and increased cellular granulation tissue with a well-organized epithelial layer. However, the granulation tissue was significantly thinner in the LMWP-conjugated group, indicating a transition from the proliferative phase for tissue regeneration to tissue remodeling, which improved skin functionality because mature collagen fibers were more uniformly distributed throughout the new connective tissue. Immunohistological detection of α-SMA on day 9 was also performed, to investigate the phase of the wound-healing process. This corresponded with the wound-healing stage because fibroblasts that have transformed into myofibroblasts have morphological and biochemical features of contractile cells that are responsible for granulation tissue contraction.31 As shown in Figure 7B, greater and denser expression of α-SMA in myofibroblasts was observed at the wound site treated with the LMWP-conjugated growth factor complex than at that treated with the native complex. Compared with the control and native group, more mature collagen fibers and fewer inflammatory cells were observed with the LMWP group, which also showed thicker re-epithelialization without scabbing, as well as regeneration of hair follicles at the wound site. This morphology indicates that a remodeling phase had occurred in that group after 9 days of treatment, while other samples remained in the tissue regeneration phase, with increased collagen synthesis and retention of infiltrated inflammatory cells.
Discussion
Wound healing is a complex process that includes a sequence of interactions between various cells, ECM components, and signaling molecules. Growth factors play important roles in the regulation and coordination of the processes that are essential for correct epidermal and dermal regeneration. Numerous studies and clinical trials have investigated accelerated healing by supplying exogenous recombinant growth factors. However, due to their short half-life in vivo and limited skin permeability through the wound margin, the necessary multiple high-dose administrations have restricted their clinical use. To overcome these limitations, we used rLMWP-EGF and demonstrated that it showed high skin permeability and enhanced re-epithelialization efficacy in various in vivo wound models. Although it showed a significantly higher rate of healing versus free-EGF treatment, outstanding efficacy was seen only in the early stages of wound healing.27 This may have been caused by the normal progression of matrix synthesis and deposition and remodeling in the dermal layer of the wound bed, which ultimately resulted in no difference in total wound healing time. Thus, no single growth factor can mediate the whole repair process because any one growth factor targets only a specific component or process. To compensate for this, we prepared rhPDGF-A and rhIGF-I fused to LMWP via genetic modification, which produced a trimeric growth factor complex of rLMWP-EGF, rLMWP-IGF-I, and LMWP-PDGF-A, with LMWH.
We successfully added the amino acid sequence for LMWP to the N-terminus of rhPDGF-A and rhIGF-I via serial PCR and cloning, to obtain highly purified and site-specifically modified rhIGF-I and rhPDGF-A, similar to rLMWP-EGF. In vitro cell proliferation assays showed that rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A maintained their bioactivity even after LMWP conjugation. Moreover, in in vitro skin permeability studies, the effective permeability values for LMWP-conjugated rhEGF, rhIGF-I, and rhPDGF-A were significantly increased compared with those of their native forms, illustrating that incorporation of LMWP enhanced the penetration of growth factors through the artificial skin membrane and excised mouse skin. Enhanced skin penetration, mediated by the arginine-rich peptide, LMWP, may involve macropinocytosis, actin rearrangement, and interactions between arginine and lipid phosphates in the intercellular lipid domain of the stratum corneum, leading to disruption of the lipid orientation and formation of a concentration gradient through open channels.32–34 Growth factors are required at the wound margin to stimulate re-epithelialization but are less useful if immobilized elsewhere in the wound.35,36 Moreover, EGF and PDGF are more important at the initial stages of wound healing; thus, rapid and increased absorption through the wound margin is helpful for accelerating the wound-healing process.37 For this reason, the highly skin-permeable LMWP-conjugated growth factors showed better in vivo wound-healing efficacy than the native forms.
In our delivery system, we used LMWH to form nanocomplexes including native or LMWP-conjugated growth factors. The results demonstrated that the LMWP-conjugated growth factor combination generated more compact nanocomplexes by adding them to LMWH than did the native growth factors; this might have been due to further electrostatic interactions between the oppositely charged polyelectrolytes of LMWH and LMWP.38 In addition, the LMWP-conjugated growth factor nanocomplex resulted in significantly accelerated wound closure compared with the LMWP-conjugated growth factor combination – it may be that the LMWP-conjugated growth factors were protected from rapid elimination by proteolytic inactivation, and that binding to their receptors was facilitated.39 Whereas, the native growth factors also formed nanocomplexes after combining with LMWH, the native growth factor complexes failed to exhibit wound-healing efficacy. This might have been caused by the relatively weak interaction between the growth factors and LMWH, and the poor skin permeability of the native growth factors and their complex.
We examined the combinational effects of growth factors on the proliferation of fibroblasts. Complexes composed of LMWP conjugated with rhEGF, rhIGF-I, and rhPDGF-A resulted in a 143%, 135%, and 124% increase in cell proliferation compared with rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A, respectively. These results are consistent with previous studies19–21 that demonstrated the stimulation of epithelial cell regeneration and connective tissue synthesis in wounds in vivo. Neither EGF nor IGF-I alone stimulated significant keratinocyte spread or proliferation, although IGF-I and insulin acted synergistically with EGF because IGF-I or high doses of insulin upregulated the expression of the EGF receptor and keratinocyte responsiveness to EGF. Additionally, IGF-I receptors are localized to the basal proliferative cell compartment, suggesting that the interaction between the IGF-I receptor and EGF receptor pathway may play a role in the regulation of epidermal growth.22 On the other hand, PDGF is a major mitogenic factor for fibroblasts that is known to increase the cell density of the loose subepithelial connective tissue layer, but to cause little or no increase in growth of the epithelial cell layer because keratinocytes lack PDGF receptors and are thus not directly responsive to PDGF.40 Consequently, the growth of connective tissue and epithelial cells may be regulated by different sets of growth factors and intracellular signaling pathways, while PDGF alone appears to have a limited effect on accelerating wound repair. However, PDGF combined with IGF-I resulted in a significant increase in epithelial cell numbers. The form and amount of the new connective tissue layer was greater than those with PDGF or IGF-I alone – the combination stimulated the production of an epithelial cell growth factor and epithelial cell proliferation via proliferation of fibroblasts and regeneration of connective tissue, providing a matrix environment for enhancing epithelial cell proliferation.19,20 PDGF has also been shown to stimulate IGF-binding protein-2 synthesis, which has mitogenic effects on IGF-I.41 These findings demonstrate that growth factors act at specific and sequential steps in the cell cycle to allow continued growth and have synergistic effects in vivo. In particular, EGF and PDGF may serve as compensatory factors to promote cellular responsiveness to IGF-I. Thus, keratinocytes in wounds treated with LMWP-conjugated growth factor complex were found well beyond the wound margin and stained positively for CK6, whereas proliferation was restricted to near the wound margin in the control group. Additionally, the LMWP-conjugated complex led to increased levels and proliferation of dermal fibroblasts, which formed granulation tissue with a high collagen content in the wounds 9 days after acute wound healing. Furthermore, there were dermal appendages within the granulation region, indicating that the wounds treated with this complex were at a later stage of healing than those treated with the other groups. This likely resulted from a direct effect on dermal fibroblasts as well as from indirect effects on signaling by activated epithelial cells.
Conclusion
We prepared skin-permeable and homogeneous rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A by genetic incorporation of a highly positively charged LMWP at the N-terminus of each growth factor. The LMWP-conjugated growth factors were biologically equivalent to their native forms but showed significantly improved skin permeability in vitro. The combination of rLMWP-EGF, rLMWP-IGF-I, and rLMWP-PDGF-A increased fibroblast cell proliferation in vitro compared with individual growth factors, and topically applied LMWP-conjugated growth factor nanocomplexes exhibited considerably accelerated wound healing, with rapid and extensive re-epithelialization, as well as dermal tissue remodeling. Our growth factor–delivery system provided enhanced permeation through the wound margin, as well as synergistic actions for epithelial cell proliferation and granulation tissue formation. Therefore, the LMWP-conjugated growth factor complex might be a candidate wound healing therapy. Additional studies will be carried out to determine the optimum dose and frequency, and to examine the enhanced healing effects on various types of wound, including diabetic ulcers and burns, of formulations applied using a topical delivery system.
Acknowledgments
This research was supported by Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Science, ICT & Future Planning (NRF-2014R1A1A1003122).
Disclosure
The authors report no conflicts of interest in this work.
References
Singer AJ, Clark RA. Cutaneous wound healing. N Engl J Med. 1999;341(10):738–746. | ||
Barrientos S, Stojadinovic O, Golinko MS, Brem H, Tomic-Canic M. Growth factors and cytokines in wound healing. Wound Repair Regen. 2008;16(5):585–601. | ||
Brown GL, Curtsinger L 3rd, Brightwell JR, et al. Enhancement of epidermal regeneration by biosynthetic epidermal growth factor. J Exp Med. 1986;163(5):1319–1324. | ||
Nanney LB. Epidermal and dermal effects of epidermal growth factor during wound repair. J Invest Dermatol. 1990;94(5):624–629. | ||
Gartner MH, Benson JD, Caldwell MD. Insulin-like growth factor I and II expression in the healing wound. J Surg Res. 1992;52(4):389–394. | ||
Todorović V, Pesko P, Micev M, et al. Insulin-like growth factor-I in wound healing of rat skin. Regul Pept. 2008;150(1–3):7–13. | ||
Ross R. Platelet-derived growth factor. Annu Rev Med. 1987;38:71–79. | ||
Goldman R. Growth factors and chronic wound healing: past, present, and future. Adv Skin Wound Care. 2004;17(1):24–35. | ||
Schultz GS, Sibbald RG, Falanga V, et al. Wound bed preparation: a systematic approach to wound management. Wound Repair Regen. 2003;11(Suppl 1):S1–S28. | ||
Jain R, Agarwal A, Kierski PR, et al. The use of native chemical functional groups presented by wound beds for the covalent attachment of polymeric microcarriers of bioactive factors. Biomaterials. 2013;34(2):340–352. | ||
Choi JS, Leong KW, Yoo HS. In vivo wound healing of diabetic ulcers using electrospun nanofibers immobilized with human epidermal growth factor (EGF). Biomaterials. 2008;29(5):587–596. | ||
Gainza G, Aguirre JJ, Pedraz JL, Hernández RM, Igartua M. rhEGF-loaded PLGA-Alginate microspheres enhance the healing of full-thickness excisional wounds in diabetised Wistar rats. Eur J Pharm Sci. 2013;50(3–4):243–252. | ||
Johnson NR, Wang Y. Controlled delivery of heparin-binding EGF-like growth factor yields fast and comprehensive wound healing. J Control Release. 2013;166(2):124–129. | ||
Xie Y, Upton Z, Richards S, Rizzi SC, Leavesley DI. Hyaluronic acid: evaluation as a potential delivery vehicle for vitronectin: growth factor complexes in wound healing applications. J Control Release. 2011;153(3):225–232. | ||
Robson MC, Mustoe TA, Hunt TK. The future of recombinant growth factors in wound healing. Am J Surg. 1998;176(2A Suppl):80S–82S. | ||
Loot MA, Kenter SB, Au FL, et al. Fibroblasts derived from chronic diabetic ulcers differ in their response to stimulation with EGF, IGF-I, bFGF and PDGF-AB compared to controls. Eur J Cell Biol. 2002;81(3):153–160. | ||
Clark RA. Synergistic signaling from extracellular matrix-growth factor complexes. J Invest Dermatol. 2008;128(6):1354–1355. | ||
Xie Z, Paras CB, Weng H, et al. Dual growth factor releasing multi-functional nanofibers for wound healing. Acta Biomater. 2013;9(12):9351–9359. | ||
Lynch SE, Nixon JC, Colvin RB, Antoniades HN. Role of platelet-derived growth factor in wound healing: synergistic effects with other growth factors. Proc Natl Acad Sci USA. 1987;84(21):7696–7700. | ||
Lynch SE, Colvin RB, Antoniades HN. Growth factors in wound healing. Single and synergistic effects on partial thickness porcine skin wounds. J Clin Invest. 1989;84(2):640–646. | ||
Greenhalgh DG, Sprugel KH, Murray MJ, Ross R. PDGF and FGF stimulate wound healing in the genetically diabetic mouse. Am J Pathol. 1990;136(6):1235–1246. | ||
Krane JF, Murphy DP, Carter DM, Krueger JG. Synergistic effects of epidermal growth factor (EGF) and insulin-like growth factor I/somatomedin C (IGF-I) on keratinocyte proliferation may be mediated by IGF-I transmodulation of the EGF receptor. J Invest Dermatol. 1991;96(4):419–424. | ||
McPherson JM, Ledger PW, Ksander G, et al. The influence of heparin on the wound healing response to collagen implants in vivo. Coll Relat Res. 1988;8(1):83–100. | ||
Raman R, Sasisekharan V, Sasisekharan R. Structural insights into biological roles of protein-glycosaminoglycan interactions. Chem Biol. 2005;12(3):267–277. | ||
Saksela O, Moscatelli D, Sommer A, Rifkin DB. Endothelial cell-derived heparan sulfate binds basic fibroblast growth factor and protects it from proteolytic degradation. J Cell Biol. 1988;107(2):743–751. | ||
Chu H, Johnson NR, Mason NS, Wang Y. A [polycation:heparin] complex releases growth factors with enhanced bioactivity. J Control Release. 2011;150(2):157–163. | ||
Choi JK, Jang JH, Jang WH, et al. The effect of epidermal growth factor (EGF) conjugated with low-molecular-weight protamine (LMWP) on wound healing of the skin. Biomaterials. 2012;33(33):8579–8590. | ||
Lee JH, Bae IH, Choi JK, Park JW. Evaluation of a highly skin permeable low-molecular-weight protamine conjugated epidermal growth factor for novel burn wound healing therapy. J Pharm Sci. 2013;102(11):4109–4120. | ||
Jiang CK, Magnaldo T, Ohtsuki M, Freedberg IM, Bernerd F, Blumenberg M. Epidermal growth factor and transforming growth factor alpha specifically induce the activation- and hyperproliferation-associated keratins 6 and 16. Proc Natl Acad Sci USA. 1993;90(14):6786–6790. | ||
Paladini RD, Takahashi K, Bravo NS, Coulombe PA. Onset of re-epithelialization after skin injury correlates with a reorganization of keratin filaments in wound edge keratinocytes: defining a potential role for keratin 16. J Cell Biol. 1996;132(3):381–397. | ||
Darby I, Skalli O, Gabbiani G. Alpha-smooth muscle actin is transiently expressed by myofibroblasts during experimental wound healing. Lab Invest. 1990;63(1):21–29. | ||
Ohtake K, Maeno T, Ueda H, Natsume H, Morimoto Y. Poly-L-arginine predominantly increases the paracellular permeability of hydrophilic macromolecules across rabbit nasal epithelium in vitro. Pharm Res. 2003;20(2):153–160. | ||
Thorén PE, Persson D, Esbjörner EK, Goksör M, Lincoln P, Nordén B. Membrane binding and translocation of cell-penetrating peptides. Biochemistry. 2004;43(12):3471–3489. | ||
Hou YW, Chan MH, Hsu HR, et al. Transdermal delivery of proteins mediated by non-covalently associated arginine-rich intracellular delivery peptides. Exp Dermatol. 2007;16(12):999–1006. | ||
Falanga V, Eaglstein WH. The “trap” hypothesis of venous ulceration. Lancet. 1993;341(8851):1006–1008. | ||
Chen RR, Mooney DJ. Polymeric growth factor delivery strategies for tissue engineering. Pharm Res. 2003;20(8):1103–1112. | ||
Hashimoto K, Higashiyama S, Asada H, et al. Heparin-binding epidermal growth factor-like growth factor is an autocrine growth factor for human keratinocytes. J Biol Chem. 1994;269(31):20060–20066. | ||
Wolzt M, Weltermann A, Nieszpaur-Los M, et al. Studies on the neutralizing effects of protamine on unfractionated and low molecular weight heparin (Fragmin) at the site of activation of the coagulation system in man. Thromb Haemost. 1995;73(3):439–443. | ||
Mori Y, Nakamura S, Kishimoto S, et al. Preparation and characterization of low-molecular-weight heparin/protamine nanoparticles (LMW-H/P NPs) as FGF-2 carrier. Int J Nanomedicine. 2010;5:147–155. | ||
Ansel J, Perry P, Brown J, et al. Cytokine modulation of keratinocyte cytokines. J Invest Dermatol. 1990;94(6 Suppl):101S–107S. | ||
Cohick WS, Gockerman A, Clemmons DR. Regulation of insulin-like growth factor (IGF) binding protein-2 synthesis and degradation by platelet-derived growth factor and the IGFs is enhanced by serum deprivation in vascular smooth muscle cells. J Cell Physiol. 1995;164(1):187–196. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.