Back to Journals » OncoTargets and Therapy » Volume 13
Efficacy of Pyrotinib in a Heavily Pretreated Patient with Lung Adenocarcinoma Harboring HER2 Amplification and Exon 20 Insertions: A Case Report
Authors Shan J, Ruan J, Tan Y, Yan L, Chen S, Du M, Wang L
Received 14 July 2020
Accepted for publication 5 September 2020
Published 2 October 2020 Volume 2020:13 Pages 9849—9856
DOI https://doi.org/10.2147/OTT.S271999
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Federico Perche
Jianzhen Shan,1,* Jian Ruan,1,* Yanbin Tan,2 Li Yan,3 Songan Chen,3 Miaoyan Du,1 Lingjie Wang1
1Department of Medical Oncology, The First Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, People’s Republic of China; 2Department of Radiology, The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, People’s Republic of China; 3Department of Medicine, Burning Rock Biotech, Guangzhou, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Jianzhen Shan
The First Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou 310003, People’s Republic of China
Tel +86 571-87235409
Email [email protected]
Abstract: The clinical benefits of HER2 inhibitors in patients with non-small cell lung cancer (NSCLC) have been limited. There is a paucity of effective therapies in NSCLC after developing resistance to initial anti-HER2 therapy. Herein, we presented the clinical benefit of pyrotinib in a 53-year-old patient with advanced lung adenocarcinoma whose circulating tumor DNA (ctDNA) analysis of pleural effusion revealed the coexistence of HER2 exon 20 p.Y772_A775dup (mutation ratio: 38.86%) and HER2 amplification (copy number: 4.5) following failures of multiple therapies including afatinib and ado-trastuzumab emtansine (T-DM1). Notably, pyrotinib treatment induced rapid and marked improvement of clinical symptoms, and partial response was observed after 8 weeks. CtDNA monitoring during the treatment showed that the mutation ratio of HER2 decreased to 7.99%, and the amplification disappeared. The patient achieved a progression-free survival of 7.5 months after treatment with pyrotinib. Thus, pyrotinib may be a new treatment strategy for the subgroup of lung adenocarcinoma patients, with coexistence of HER2 exon 20 p.Y772_A775dup and HER2 amplification even after failures of multiple anti-HER2 therapies. It also indicated the value of capture-based next-generation sequencing to monitor and guide therapy.
Keywords: pyrotinib, HER2 mutation, HER2 amplification, non-small cell lung cancer, next-generation sequencing
Introduction
Human epidermal growth factor receptor 2 (HER2) has been identified as a key oncogenic driver gene in non-small cell lung cancer (NSCLC).1 The incidence of HER2 mutation and amplification in NSCLC is approximately 2–3% and 2–5%, respectively.2 As shown in previous studies, typically, these modifications are not associated with each other and act as distinct molecular targets.3,4 For over a decade, many clinical trials have investigated HER2-targeted drugs for the treatment of NSCLC with HER2 variations. Trastuzumab and afatinib were previously recommended (category 2B) by National Comprehensive Cancer Network Guidelines for NSCLC with HER2 mutations, however, due to the merge of ado-trastuzumab emtansine (T-DM1), which showed superior response rates and efficacy in this patient group, the recommendation was then switched to T-DM1 (category 2A).5,6 In a Phase II basket trial, T-DM1 produced a 44% confirmed partial response rate and a median progression-free survival (PFS) of 5 months in HER2 mutated NSCLC.7 However, thus far, there is no targeted therapy specifically approved for this patient population. In China, pyrotinib (an oral irreversible tyrosine kinase inhibitor targeting HER1, HER2, and HER4 receptors) has been approved for the treatment of HER2-positive advanced breast cancer. A preclinical study of pyrotinib displayed excellent in vitro potency and selectivity, as well as robust in vivo efficacy in HER2-dependent mouse xenograft models. Metabolic pathway data indicated that pyrotinib was primarily metabolized by CYP3A4. In addition, the study also demonstrated the desirable pharmacokinetic properties and safety profile of this agent.8 A Phase I study of pyrotinib assessed the safety, tolerability, pharmacokinetics, antitumor activity, and predictive biomarkers in patients with HER2-positive metastatic breast cancer.9 Preliminary data showed its promising antitumor activity and acceptable tolerability, with an overall objective response rate of 50.0% (18 of 36 patients) and median PFS of 35.4 weeks. The only grade 3 adverse event reported was diarrhea. Moreover, circulating tumor DNA (ctDNA) dynamics was discovered as a novel indicator of resistance in patients with metastatic breast cancer receiving anti-HER2 therapy.10 A randomized phase II study assessed the efficacy and tolerability of pyrotinib versus lapatinib, both in combination with capecitabine, in women with HER2-positive metastatic breast cancer who received taxanes, anthracyclines, and/or trastuzumab. The results showed that pyrotinib plus capecitabine yielded statistically significant better overall response rate (78.5% vs 57.1%, respectively) and median PFS (18.1 vs 7.0 months, respectively) than lapatinib plus capecitabine.11 In addition, pyrotinib showed a superior antitumor effect than afatinib and T-DM1 in the patient-derived xenograft model and mice model. In a phase II clinical trial designed to evaluate the efficacy and safety of pyrotinib in the treatment of advanced NSCLC with HER2 exon 20 insertions showed promising results.12 In another published phase II study, pyrotinib also showed a favorable objective response rate and an acceptable safety profile in chemotherapy-treated patients with HER2-mutant NSCLC.13
In this study, we report a case with HER2-mutant advanced NSCLC, who had previously been treated with multiple lines of therapy, including anti-HER2 therapies (ie, afatinib and T-DM1), benefiting from pyrotinib as salvage therapy with coexistence of HER2 mutation and amplification. During the treatment, we also detected ctDNA at various milestones by capture-based next-generation sequencing (NGS) to monitor and guide therapy.
Case Report
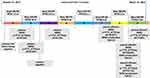
A 53-year-old male detected a space-occupying lesion in the left lung through physical examination 1 month prior to admission. He was admitted to our hospital on October 18, 2015. Imaging examinations showed a nodule measuring 17 × 15 × 15 mm in the upper lobe of the left lung inferior lingular segment. Moreover, the left supraclavicular lymph node was swollen (1.1 × 0.5 mm), with no evidence of brain or bone metastasis. The levels of tumor biomarker carcinoembryonic antigen were 12.2 ng/mL. Computed tomography (CT)-guided biopsy of the left lung and left supraclavicular lymph node revealed the presence of adenocarcinoma. The pathological stage of the disease was T1bN3M0 (stage IIIB). NGS analysis of blood ctDNA and tumor tissue using a targeted panel (Burning Rock Biotech, Guangzhou, China) revealed no known mutations. We summarized the therapeutic regimens received and major mutations detected in Figure 1.
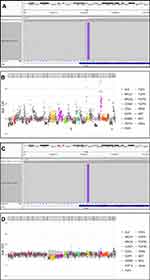
In brief, our patient received multiple lines of therapy. On November 8, 2015, the patient was administered 4 cycles of chemotherapy with pemetrexed plus carboplatin. Then, combined with radiotherapy after the first cycle. After that, pemetrexed maintenance treatment for a total of 10 cycles. There was a progressive increase in blood carcinoembryonic antigen (CEA) (42.6ng/mL), the chest CT showed that the left lung lesion had increased in size. Results of a positron emission tomography-computed tomography (PET-CT) scan demonstrated mediastinal lymph nodes, right supraclavicular lymph nodes, the right scapula and vertebra bone metastasis. Capture-based targeted sequencing of plasma ctDNA revealed a HER2 exon 20 p.Y772_A775dup (mutation ratio: 5.52%). The patient was treated with afatinib (40 mg once a day) for 3 months. The levels of CEA were declined. On May 18, 2017, the PET-CT showed a slight reduction in mediastinal lymph nodes, and it was considered to be a stable disease (SD). However, due to 3-degree adverse events (diarrhea and rash), the patient stopped taking afatinib, the levels of CEA were elevated again 2 months after stopping taking afatinib. On May 10, 2017, NGS of plasma ctDNA revealed lower HER2 mutation abundance than before (0.25%). On May 18, the PET-CT scan revealed multiple lymphadenopathies in the right clavicle area and mediastinum, increasing in size and number compared with the previous PET-CT scan, as well as metastasis of the right scapula and chest bone. On June 8, the patient received radiotherapy: 4500 cGy/15 F of the right scapula, 5600 cGy/28 F of the mediastinal metastasis tumor area and chest tumor area. After radiotherapy, a reexamination of CT showed that mediastinal lymph nodes were smaller than before, the peripheral blood NGS test was negative. The Eastern Cooperative Oncology Group (ECOG) score was 1 point. No significant progress was found in head magnetic resonance imaging (MRI), chest and abdomen CT. On June 19, 2018, an MRI of thoracic vertebrae revealed thoracic appendages, thoracic vertebrae and bone metastasis. From July 4, 2018, to August 21, 2018, the patient was administered with pembrolizumab (keytruda) at a dose of 200 mg once every three weeks for 3 cycles. The patient experienced progressive disease (PD) shortly after pembrolizumab treatment, with a progressive increase of blood CEA. Results of a PET-CT scan showed an enlarged lesion in the left upper lobe, new metastasis in hepatogastric space, retroperitoneal lymph nodes and vertebral bone. The ECOG score was 1 point. Back pain and other symptoms were the same as before. On October 10, the patient was treated with chemotherapy (paclitaxel plus carboplatin) combined with an anti-vascular drug (bevacizumab) for 2 cycles. The enhanced chest CT on November 24, 2018 (after 2 cycles) showed a larger lesion in the left upper lobe than before with left pleural effusion. NGS of plasma ctDNA revealed a HER2 exon 20 p.Y772_A775dup (0.18%). Based on the NGS results, the patient started T-DM1 (320mg, once every four weeks) for 2cycles. The blood CEA level increased to 192 ng/mL, the ECOG score was 2 points. The patient showed fatigue, 2-degree thrombocytopenia and elevated blood pressure (considered as adverse reactions related to T-DM1). The MRI scan demonstrated cervical vertebrae and thoracic vertebrae metastases. In the six-line therapy, the patient was administered with afatinib at a dose of 30 mg once a day for rechallenge, which resulted in stable disease. After the failure of afatinib rechallenge, the patient was switched to chemotherapy with gemcitabine alone for two cycles along with intracavitary administration of recombinant human endostatin injection (ENDOSTAR) for the treatment of pleural effusion. A PET-CT scan performed on August 28, 2019, revealed progression of the lung, bone, and lymph node lesions with bulk pleural effusion (Figure 2). At the same time, the patient showed hypoproteinemia, cough, chest distress, and shortness of breath after activity. NGS analysis (Burning Rock Biotech, Guangzhou, China) of pleural effusion ctDNA showed HER2 exon 20 p.Y772_A775dup (38.86%) and HER2 amplification (copy number: 4.5) (Figure 3). Subsequently, he was treated with pyrotinib 400 mg once daily. The symptoms were markedly relieved after 2 weeks and were evaluated after 8 weeks of treatment using PET-CT. He achieved partial response according to the Response Evaluation Criteria in Solid Tumors 1.1 (Figure 2). Dynamic monitoring of the pleural effusion ctDNA (Burning Rock Biotech, Guangzhou, China) showed that the HER2 mutation ratio had decreased significantly (7.99%) and the amplification had disappeared (Figure 3). The levels of tumor CEA showed dynamic changes with different treatments (Figure 4). However, PET-CT performed on March 16, 2020, showed an increase in the size of the left lung lesion, indicating progressive disease. The PFS after treatment with pyrotinib was 7.5 months.
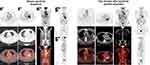 |
Figure 2 Image scans revealed the clinical response to the treatment of pyrotinib. |
 |
Figure 4 Fluctuation of CEA level in the blood. CEA, carcinoembryonic antigen. |
Discussion
Compared with epidermal growth factor receptor mutations, HER2 alterations are rare in patients with NSCLC. Previous reports on the clinicopathological characteristics of HER2-mutant NSCLC have demonstrated that these alterations are more common in females, non-smokers, and patients with adenocarcinomas (median age: 62 years).14 Furthermore, the prognosis is poor with a median overall survival of 1.6–1.9 years.15 The most frequent metastatic sites are the lungs, brain, and liver, while some patients had more than two metastatic lesions.16 Our patient is a younger male with lymph node, bone, and pleural metastases, as well as slow progression of disease.
Pyrotinib is a novel irreversible tyrosine kinase inhibitor with activity against HER1, HER2, and HER4. Preclinical studies suggested that pyrotinib can significantly inhibit the growth of HER2 factor-driven tumor cells both in vivo and in vitro.17 This is achieved by blocking the cell cycle in the G1 phase through inhibition of the HER2 downstream signaling pathway. In a phase II study of 15 pretreated NSCLC patients with HER2 mutations, the administration of pyrotinib 400 mg resulted in an overall response rate of 53.3% and a median PFS of 6.4 months.12 Notably, there was no occurrence of grade 3 or 4 adverse events. This cohort included 10 patients with Y772_A775dup in exon 20 of HER2, but not coupled with HER2 amplification. To the best of our knowledge, this is the first report of the efficacy of pyrotinib in patients with co-existence of HER2 mutation and amplification. In our case, after treatment with pyrotinib 400 mg, the patient achieved partial response accompanied by rapid relief of clinical symptoms, and pyrotinib showed better tolerability compared with afatinib and T-DM1. In this patient’s anti-HER2 therapy, afatinib has demonstrated certain clinical effect, no matter it was used for the first time or challenged again. However, full dose afatinib yielded 3-degree diarrhea and rash, causing discontinuation of afatinib. Pembrolizumab monotherapy was ineffective in this patient at all. It was suggested that HER2 variations similar as EGFR or ALK alterations might influence the effect of PD-1/PD-L1 inhibitor monotherapy.18 Although T-DM1 was recommended at higher level by the guidelines, our patient did not respond to it and he experienced 2-degree thrombocytopenia and elevated blood pressure. But in the treatment of pyrotinib, he did not require dose reduction or treatment termination.
In the present case, the co-existence of HER2 exon 20 p.Y772_A775dup and HER2 amplification was firstly detected after failure of afatinib rechallenge with no HER2 amplification detected previously. A previous report of a 36-year-old Asian woman diagnosed with stage IV lung adenocarcinoma with a HER2 exon 20 insertion suggested that HER2 copy number gain may be a potential resistance mechanism to afatinib.19 It was reported that HER2 mutations with in-frame insertions in exon 20 and amplification resulted in constitutive activation of the downstream signaling pathways. All three anti-HER2 drugs, afatinib, T-DM1 and pyrotinib can block HER2 downstream signaling pathways, but among them, pyrotinib was the most potent at inhibiting tumor growth in vitro and in vivo using clinically relevant concentration.12 According to findings from early phase clinical trials, pyrotinib demonstrated encouraging antitumor activity and a manageable toxicity profile in patients with heavily pretreated HER2-mutant NSCLC, as well as other advanced solid tumors harboring activating HER2 alterations including amplification.12,13,20 These positive findings showed the potential of pyrotinib in targeting HER2 amplification and exon 20 insertions. Further studies are warranted to prove the efficacy of pyrotinib in HER2-altered NSCLC and other solid tumors. Moreover, many other HER2-targeted agents in NSCLC are in clinical trials, including neratinib, poziotinib, TAK788, DS-8201a and so on. With the continuous supplement of clinical evidence, NSCLC with HER2 alterations may soon enter the era of targeted therapy.
Conclusion
Our case showed pyrotinib could be a potential treatment option for the subgroup of lung adenocarcinoma patients with coexistence of HER2 exon 20 p.Y772_A775dup and HER2 amplification who have developed progress after multi-line anti-HER2 therapy. It also indicated the value of capture-based NGS to monitor and guide therapy, even if the result of the initial test is negative.
Abbreviations
NSCLC, non-small cell lung cancer; NGS, next-generation sequencing; PFS, progression-free survival; HER1, human epidermal growth factor receptor 1; HER2, human epidermal growth factor receptor 2; HER4, human epidermal growth factor receptor 4; CT, computed tomography; PET-CT, positron emission tomography-computed tomography; T-DM1, ado-trastuzumab emtansine; CEA, carcinoembryonic antigen.
Ethics Approval and Consent to Participate
The study was approved by the ethical committee of the First Affiliated Hospital of Zhejiang University School of Medicine and the patient signed an informed consent to participate in the study. The First Affiliated Hospital of Zhejiang University School of Medicine approved to publish the case details.
Consent for Publication
Publication of the case was consent by the patient. Informed consent was obtained from the patient for use of his samples, imagings and the publication of this report.
Acknowledgments
The authors sincerely thank the patient and his family. This work was supported by the Public Welfare Technology Research Project of Zhejiang Province (grant number LGJ18H160001) and the Medical and Health Science and Technology Project of Zhejiang Province (grant number 2017205840, grant number 2018274816).
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Disclosure
Li Yan is an employee of Burning Rock Biotech. The authors report no other potential conflicts of interest in this work.
References
1. Hyman DM, Piha-Paul SA, Won H, et al. HER kinase inhibition in patients with HER2- and HER3-mutant cancers. Nature. 2018;554(7691):189–194. doi:10.1038/nature25475
2. Li BT, Ross DS, Aisner DL, et al. HER2 amplification and HER2 mutation are distinct molecular targets in lung cancers. J Thorac Oncol. 2016;11(3):414–419. doi:10.1016/j.jtho.2015.10.025
3. Kris MG, Camidge DR, Giaccone G, et al. Targeting HER2 aberrations as actionable drivers in lung cancers: phase II trial of the pan-HER tyrosine kinase inhibitor dacomitinib in patients with HER2-mutant or amplified tumors. Ann Oncol. 2015;26(7):1421–1427. doi:10.1093/annonc/mdv186
4. Liu S, Li S, Hai J, et al. Targeting HER2 aberrations in non–small cell lung cancer with osimertinib. Clin Cancer Res. 2018;24(11):2594–2604. doi:10.1158/1078-0432.CCR-17-1875
5. Mazieres J, Peters S, Lepage B, et al. Lung cancer that harbors an HER2 mutation: epidemiologic characteristics and therapeutic perspectives. J Clin Oncol. 2013;31(16):1997–2003. doi:10.1200/JCO.2012.45.6095
6. Shigematsu H, Takahashi T, Nomura M, et al. Somatic mutations of the HER2 kinase domain in lung adenocarcinomas. Cancer Res. 2005;65(5):1642–1646. doi:10.1158/0008-5472.CAN-04-4235
7. Li BT, Shen R, Buonocore D, et al. Ado-trastuzumab emtansine for patients with HER2-mutant lung cancers: results from a phase II basket trial. J Clin Oncol. 2018;36(24):2532–2537. doi:10.1200/JCO.2018.77.9777
8. Li X, Yang C, Wan H, et al. Discovery and development of pyrotinib: a novel irreversible EGFR/HER2 dual tyrosine kinase inhibitor with favorable safety profiles for the treatment of breast cancer. Eur J Pharm Sci. 2017;110:51–61. doi:10.1016/j.ejps.2017.01.021
9. Ma F, Li Q, Chen S, et al. Phase I study and biomarker analysis of pyrotinib, a novel irreversible pan-erbB receptor tyrosine kinase inhibitor, in patients with human epidermal growth factor receptor 2-positive metastatic breast cancer. J Clin Oncol. 2017;35:3105–3112.
10. Ma F, Zhu W, Guan Y, et al. ctDNA dynamics: a novel indicator to track resistance in metastatic breast cancer treated with anti-HER2 therapy. Oncotarget. 2016;7(40):66020–66031. doi:10.18632/oncotarget.11791
11. Ma F, Ouyang Q, Li W, et al. Pyrotinib or lapatinib combined with capecitabine in HER2-positive metastatic breast cancer with prior taxanes, anthracyclines, and/or trastuzumab: a randomized, phase II study. J Clin Oncol. 2019;37(29):2610–2619. doi:10.1200/JCO.19.00108
12. Wang Y, Jiang T, Qin Z, et al. HER2 exon 20 insertions in non-small-cell lung cancer are sensitive to the irreversible pan-HER receptor tyrosine kinase inhibitor pyrotinib. Ann Oncol. 2019;30(3):447–455. doi:10.1093/annonc/mdy542
13. Zhou C, Li X, Wang Q, et al. Pyrotinib in HER2-mutant advanced lung adenocarcinoma after platinum-based chemotherapy: a multicenter, open-label, single-arm, phase II study. J Clin Oncol. 2020;O2000297.
14. Eng J, Hsu M, Chaft JE, Kris MG, Arcila ME, Li BT. Outcomes of chemotherapies and HER2 directed therapies in advanced HER2-mutant lung cancers. Lung Cancer. 2016;99:53–56. doi:10.1016/j.lungcan.2016.05.030
15. Kris MG, Johnson BE, Berry LD, et al. Using multiplexed assays of oncogenic drivers in lung cancers to select targeted drugs. JAMA. 2014;311(19):1998–2006. doi:10.1001/jama.2014.3741
16. Auliac JB, Do P, Bayle S, et al. Non-small cell lung cancer patients harboring HER2 mutations: clinical characteristics and management in a real-life setting. Cohort HER2 EXPLORE GFPC 02-14. Adv Ther. 2019;36(8):2161–2166. doi:10.1007/s12325-019-01001-9
17. Li Q, Guan X, Chen S, et al. Safety, efficacy, and biomarker analysis of pyrotinib in combination with capecitabine in HER2-positive metastatic breast cancer patients: a phase I trial. Clin Cancer Res. 2019;25(17):5212–5220. doi:10.1158/1078-0432.CCR-18-4173
18. Mazieres J, Drilon A, Lusque A, et al. Immune checkpoint inhibitors for patients with advanced lung cancer and oncogenic driver alterations: results from the immunotarget registry. Ann Oncol. 2019;30(8):1321–1328. doi:10.1093/annonc/mdz167
19. Chuang JC, Stehr H, Liang Y, et al. ERBB2-mutated metastatic non-small cell lung cancer: response and resistance to targeted therapies. J Thorac Oncol. 2017;12(5):833–842. doi:10.1016/j.jtho.2017.01.023
20. Li BT, Li T, Johnson ML, et al. Safety and efficacy of pyrotinib in patients with NSCLC and other advanced solid tumors with activating HER2 alterations: A phase I basket trial. J Clin Oncol. 2020;38(15_suppl):3510. doi:10.1200/JCO.2020.38.15_suppl.3510
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.