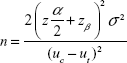Back to Journals » Clinical Interventions in Aging » Volume 11
Efficacy and safety of tamsulosin hydrochloride 0.2 mg and combination of tamsulosin hydrochloride 0.2 mg plus solifenacin succinate 5 mg after transurethral resection of the prostate: a prospective, randomized controlled trial
Authors Shin YS , Zhang LT, You JH, Choi IS, Zhao C, Park J
Received 15 June 2016
Accepted for publication 15 July 2016
Published 19 September 2016 Volume 2016:11 Pages 1301—1307
DOI https://doi.org/10.2147/CIA.S115042
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Richard Walker
Yu Seob Shin,1,* Li Tao Zhang,1,* Jae Hyung You,1 In Sung Choi,1 Chen Zhao,2 Jong Kwan Park1
1Department of Urology, Chonbuk National University and Research Institute of Clinical Medicine of Chonbuk National University-Biomedical Research Institute and Medical Device Clinical Trial Center of Chonbuk National University, Jeonju, Republic of Korea; 2Department of Urology, Renji Hospital, Shanghai Jiao Tong University School of Medicine, and Shanghai Institute of Andrology, Shanghai, People’s Republic of China
*These authors contributed equally to this work
Objective: The objective of this study was to evaluate the safety and efficacy of tamsulosin hydrochloride 0.2 mg (TAM) and its combination with solifenacin succinate 5 mg (SOL) after transurethral resection of the prostate (TURP).
Patients and methods: The patients were randomized into three groups: TURP (group 1), TURP plus TAM (group 2), and TURP plus TAM + SOL (group 3). Patients in group 2 and group 3 received medication for 4 weeks. The primary efficacy end points were the mean change in total International Prostate Symptom Score (IPSS) and IPSS subscores. The secondary end points included quality-of-life score, Overactive Bladder Symptom Score, and short-form voiding and storage score of International Continence Society.
Results: In total, 37 men (31.8%) in group 1, 37 men (31.8%) in group 2, and 42 men (36.2%) in group 3 completed the study. In total IPSS, no significant improvement was seen from baseline to the end of treatment in groups 2 and 3 compared with group 1. However, in group 2, the decrement in the IPSS storage score was smaller than group 1 (P=0.02), and in group 3, the decrement in the IPSS voiding score was smaller than group 1 (P=0.05). In groups 2 and 3 compared with group 1, improvements in the quality of life score, total score of Overactive Bladder Symptom Score, and short-form voiding score and storage score of International Continence Society were not statistically significant.
Conclusion: Treatment with TAM and combination of TAM and SOL did not have significant additional benefits for lower urinary tract symptoms during the early recovery period after TURP.
Keywords: benign prostate hyperplasia, tamsulosin, solifenacin, combination, transurethral resection of the prostate
Introduction
Benign prostatic hyperplasia (BPH) is a common condition generally associated with aging. It is estimated that the prevalence of BPH already reaches 43% between 50 years and 59 years of age, 70% at 61–70 years of age, and as high as 82% in men >71 years of age.1 Lower urinary tract symptoms (LUTS) are commonly observed in BPH-associated bladder outlet obstruction and overactive bladder. Bladder outlet obstruction resulting from BPH can directly lead to voiding and postvoiding LUTS.2 Additionally, LUTS have adverse effects on health-related quality of life (QoL), including interference with daily activities and decreased psychological well-being, which worsens with symptom severity.3
Current treatment options for BPH include medication and surgery, and transurethral resection of the prostate (TURP) is known to be the most effective among the traditional surgical methods. Within this context, TURP has become the standard treatment option, and it is regarded as an effective tool for the removal of obstructive prostatic tissue.4 However, not all patients demonstrate successful resolution of these symptoms after the prostate intervention. The morbidity of TURP is more or less inevitable in the clinical setting, and most patients complain of voiding and storage symptoms, hematuria, painful urination, and incontinence, leading to a negative impact on health-related QoL within the first 4–6 weeks after TURP.5
Some patients with persistent urinary symptoms may benefit from medical therapy even after TURP. However, there has been little research as to whether antimuscarinics and α-blockers can alleviate voiding and storage symptoms and other symptoms in the patients during the early postoperative period after TURP. Therefore, we conducted an open-label, controlled, randomized clinical trial to evaluate the efficacy and safety of tamsulosin hydrochloride 0.2 mg (TAM) and combination of TAM plus solifenacin succinate 5 mg (SOL) in men who underwent TURP due to LUTS/BPH.
Patients and methods
Study design and patients
This was a randomized, open-label, controlled study in men who underwent TURP due to BPH/LUTS with moderate-to-severe voiding and storage symptoms. All study materials were reviewed and approved by the Institutional Review Board of Chonbuk National University Hospital. All patients provided written informed consent before screening. Patients with more than 3 months of prior treatment with TAM or administration of antimuscarinics or 5-alpha-reductase inhibitors were eligible for inclusion in this study.
The inclusion criteria at baseline were total International Prostate Symptom Score (IPSS) ≥8, maximum urinary flow rate (Qmax) ≤15 mL/s, voided volume ≥125 mL, and prostate volume ≥30 mL and <100 mL.
The sample size was estimated by the following formula:
|
|
According to this formula, 43 patients were taken for each group. In consideration of 20% of dropout rates, 55 patients were taken in each group to obtain a significant value. Thus, 165 patients were taken in our study for three groups.
All the patients underwent a general and urological standard evaluation prior to surgery, including urine analysis and digital rectal and transrectal ultrasound (B&K 2102; Brüel & Kjær, Nærum, Denmark) evaluation of prostate size, and they were tested for prostate-specific antigen levels and performed self-assessments using the total IPSS and IPSS subscores, QoL score, Overactive Bladder Symptom Score (OABSS) questionnaire, and short-form voiding and storage score of International Continence Society (ICS). Additionally, all patients were older than 55 years, candidates for TURP, and lacked any evidence of symptomatic urinary tract infections and urinary stones.
The patients were excluded if they had a postvoid residual volume (PVR) >150 mL, evidence of suspected prostate cancer, a diagnosis of urinary retention, any previous surgery of the bladder neck or prostate, and any other relevant disease history, as determined by the investigator.
Surgical procedure
TURP was performed using a standard technique: bipolar resectoscope (Richard Wolf, Knittlingen, Germany) and standard bipolar wire loop. A 20 Fr Foley catheter was inserted at the end of the procedure. The catheter was removed when gross hematuria had resolved, 2–5 days post operation. After the patients were able to urinate, they underwent uroflowmetry, PVR, and transrectal ultrasonography. The patients were discharged from the hospital after the Foley catheter was removed.
Medications
After removal of the Foley catheter, all the patients were randomized into three groups: TURP (group 1), TURP plus TAM (group 2), and TURP plus TAM + SOL (group 3). Patients in group 2 and group 3 received treatment once daily for 4 weeks as open-label treatments. The usual dose of TAM is 0.4 mg once daily; however, in our study, we used 0.2 mg of TAM once daily.
Efficacy assessments
The primary end point was the change in total IPSS and IPSS storage and voiding subscores. The secondary end points were QoL score, total OABSS questionnaire, and short-form voiding and storage score of ICS. Additionally, mean changes in measures were evaluated at baseline and the end point of therapy after TURP and also at 4 weeks and 8 weeks after removal of the Foley catheter. Micturition diary variables included volume voided (Vvoid) per micturition. Safety parameters included patient-reported adverse events, PVR, and Qmax.
Statistical analysis
Statistical analyses were performed on an intention-to-treat basis for all patients who were randomized and who completed the open-label study. Mean and proportion values for patient demographics and baseline characteristics were compared using one-way analysis of variance followed by Tukey’s post hoc test.
In each step, comparisons were made by variance analysis by using the treatment group as a fixed factor to analyze each of the secondary efficacy end points. We assessed the mean change in total IPSS and IPSS subscores, QoL score, OABSS total score, short-form voiding and storage score of ICS, Qmax, Vvoid, and PVR from baseline to end point (8 weeks) for medication treatment groups compared with group 1. Unless otherwise stated, efficacy data are expressed as mean ± standard error. Statistical calculations were performed using the SPSS software (Version 21.0; IBM Corporation, Armonk, NY, USA). P-values <0.05 were considered to indicate statistical significance.
Results
Patients and baseline characteristics
Of the 169 men with LUTS who were screened, 151 were randomized to treatment (group 1, n=52; group 2, n=48; and group 3, n=51). In total, 37 men (31.8%) in group 1, 37 men (31.8%) in group 2, and 42 men (36.2%) in group 3 completed the study (Figure 1).
There were no significant differences in baseline characteristics among the three groups (Table 1). The majority of men were older than 65 years. In all treatment groups, at baseline, the range of the total IPSS was 16.35–17.58 and the range of the Vvoid per micturition was 152.14–162.17 mL (Table 1).
Efficacy
Primary efficacy end point
All groups showed significant decrement in total IPSS and IPSS storage and voiding subscores at all points after TURP. However, there was no statistical significance between the groups in total IPSS and IPSS storage and voiding subscores from baseline to discharge day, week 1, and week 4. Also, with respect to total IPSS, no significant improvement was achieved from baseline to the end of treatment in group 2 compared with group 1 (P=0.73; Table 2). Decrement in total IPSS from baseline to the end of treatment was smaller in group 3, with no significant difference between groups 3 and 1 (P=0.69; Table 2). However, in group 2, decrement in the IPSS storage score from baseline to the end of treatment was smaller than group 1 (P=0.02; Table 2). Also, in group 3, decrement in the IPSS voiding score from baseline to the end of treatment was smaller than group 1 (P=0.05; Table 2). TURP plus TAM and TURP plus the combination of TAM and SOL did not have significant additional benefits for LUTS during the early recovery period after TURP.
Secondary efficacy end points
In group 2 compared with group 1, improvements as assessed by mean changes from baseline to the end of treatment in QoL score (P=0.08), OABSS total score (P=0.36), short-form voiding score of ICS (P=0.42), and storage score of ICS (P=0.99) were not statistically significant. Also, in group 3 compared with group 1, improvements as assessed by mean changes from baseline to the end of treatment in QoL score (P=0.67), OABSS total score (P=0.51), short-form voiding score of ICS (P=0.47), and storage score of ICS (P=0.36) were not statistically significant. Numerical improvements were observed in Vvoid per micturition in group 3 at all time points compared with group 1; however, the improvements were not statistically significant (P=0.44; Table 2 and Figure 2A).
Safety
In groups 2 and 3 compared with group 1, the mean changes in PVR from baseline to the end of treatment were significantly higher (P=0.03 and P=0.03, respectively; Table 2 and Figure 2B). At the end of the treatment, the adjusted mean change in PVR was 19.46 mL in group 3, 18.67 mL in group 2, and −1.50 mL in group 1 (Table 2 and Figure 2B). Treatment-emergent adverse events were mild to moderate, and they occurred in 14.2%, 8.1%, and 8.1% of patients in groups 3, 2, and 1, respectively. The most common adverse events in the treatment group that received SOL were dry mouth and constipation. Treatment-related dry mouth was reported in five (11.9%) patients in the combination-therapy group versus one (2.7%) patient in the TAM group and in none of the patients who underwent TURP alone. Urinary retention was only seen in one patient of group 2.
Discussion
For decades, TURP has been the gold standard therapy for elderly men (>60 years old) with LUTS caused by benign prostatic enlargement and benign prostatic obstruction.6,7 During the past 20 years, various technical improvements, such as video TURP, continuous-flow instruments, and bipolar TURP, have substantially decreased the morbidity associated with TURP.6 However, some postoperative complications of TURP occur in the patients, although minimally invasive procedures may be an alternative.5 Dissatisfaction may be attributable to an increase in the sensitivity of muscarinic receptors to acetylcholine in the smooth muscle of the bladder as opposed to a prostatic pathology that leads to overactive bladder after TURP surgery.2,8
Various drugs are available for men with LUTS suggestive of BPH. In 1994, Chapple and Smith9 referred to the possibility of combination treatment with antimuscarinics and α-blockers for LUTS. Since then, both antimuscarinics and α-blockers have been evaluated for the treatment of voiding and storage symptoms.9–11 More recent meta-analyses and systematic reviews have demonstrated that combination of antimuscarinics and α-blockers improved voiding and storage symptoms in patients compared to those treated with α-blocker monotherapy.12–16 Also, these medications are needed in post-TURP patients who have persistent or even worse urinary symptoms after TURP. Han et al reported ~205 (55.1%) patients who continued their LUTS/BPH medications for >3 months after TURP. Among the patients who continued their medications after TURP, 13.7% received α-blocker monotherapy and 12.2% received antimuscarinics.17 A theoretical basis exists for using α-blockers to treat irritative symptoms in the absence of bladder outlet obstruction, although antimuscarinics apparently remain the mainstay of treatment for overactive bladder.
The present study was performed to evaluate the efficacy and safety of combination therapy with the antimuscarinic SOL and the α-blocker TAM in the treatment of men with both voiding and storage symptoms of LUTS/BPH and bothersome symptoms, such as painful urination, incontinence, and urgency, during the early period after TURP surgery. Combination therapy did not show significant additional benefits in total IPSS, IPSS voiding and storage subscore, QoL score, Qmax, OABSS total score, or Vvoid per micturition when we compared group 1 vs groups 2 and 3. Furthermore, treatment with TAM and combination of TAM and SOL had a potential side effect of an increase in PVR.
In our study, many patients suffered from LUTS immediately after TURP. These bothersome symptoms may have been induced by inflammation of the prostatic urethra or edema that occurred during TURP. The major finding of the present study was that early initiation of LUTS medication did not have any benefit in patients who suffered from LUTS during the early recovery period after TURP.
One of the limitations of the study could be that it is a single-center study. We sought to determine the efficacy of the α-blockers or α-blockers plus anticholinergic in decreasing the LUTS that occurred within a short time period after TURP, which could be another limitation of the study. Further multicenter studies are needed in patients. Despite these limitations, to the best of our knowledge, the present study is the first reported prospective, randomized trial that analyzed the safety and efficacy of TAM and its combination with SOL during the early period after TURP.
Conclusion
In the present study, treatment with TAM and combination of TAM and SOL did not have significant additional benefits for LUTS during the early recovery period after TURP. Moreover, treatment with TAM and combination of TAM and SOL had a potential side effect of an increase in PVR.
Acknowledgments
Jong Kwan Park received a grant from Astellas Pharma Korea, Inc. However, the funder had no involvement in study design, data collection, data analysis, manuscript preparation, and/or publication decisions. Jong Kwan Park also received an honorarium for a presentation and served as a consultant to Astellas Pharma Korea, Inc. during the study.
Author contributions
All authors contributed toward data analysis, drafting and critically revising the paper and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
Roberts RO, Jacobsen SJ, Jacobson DJ, Reilly WT, Talley NJ, Lieber MM. Natural history of prostatism: high American urological association symptom scores among community-dwelling men and women with urinary incontinence. Urology. 1998;51(2):213–219. | ||
Athanasopoulos A, Chapple C, Fowler C, et al. The role of antimuscarinics in the management of men with symptoms of overactive bladder associated with concomitant bladder outlet obstruction: an update. Eur Urol. 2011;60(1):94–105. | ||
Wasson JH, Reda DJ, Bruskewitz RC, Elinson J, Keller AM, Henderson WG. A comparison of transurethral surgery with watchful waiting for moderate symptoms of benign prostatic hyperplasia. The Veterans Affairs Cooperative Study Group on transurethral resection of the prostate. N Engl J Med. 1995;332(2):75–79. | ||
Ho HS, Yip SK, Lim KB, Fook S, Foo KT, Cheng CW. A prospective randomized study comparing monopolar and bipolar transurethral resection of prostate using transurethral resection in saline (TURIS) system. Eur Urol. 2007;52(2):517–522. | ||
Rassweiler J, Teber D, Kuntz R, Hofmann R. Complications of transurethral resection of the prostate (TURP) – incidence, management, and prevention. Eur Urol. 2006;50(5):969–980. | ||
Marszalek M, Ponholzer A, Pusman M, et al. Transurethral resection of the prostate. Eur Urol. 2009;Suppl 8:504–512. | ||
Min DS, Cho HJ, Kang JY, Yoo TK, Cho JM. Effect of transurethral resection of the prostate based on the degree of obstruction seen in urodynamic study. Korean J Urol. 2013;54(12):840–845. | ||
Kang YJ, Kim KH, Seo Y, Lee KS. Effect of transurethral resection of the prostate on storage symptoms in patients with benign prostatic hyperplasia of less than 30 ml. World J Mens Health. 2013;31(1):64–69. | ||
Chapple CR, Smith D. The pathophysiological changes in the bladder obstructed by benign prostatic hyperplasia. Br J Urol. 1994;73(2):117–123. | ||
Yamaguchi O, Kakizaki H, Homma Y, et al. Solifenacin as add-on therapy for overactive bladder symptoms in men treated for lower urinary tract symptoms – ASSIST, randomized controlled study. Urology. 2011;78(1):126–133. | ||
Oelke M, Bachmann A, Descazeaud A, et al. EAU guidelines on the treatment and follow-up of non-neurogenic male lower urinary tract symptoms including benign prostatic obstruction. Eur Urol. 2013;64(1):118–140. | ||
Li MC, Wang ZY, Yang J, et al. Efficacy and safety of solifenacin plus tamsulosin oral controlled absorption system in men with lower urinary tract symptoms: a meta-analysis. Asian J Androl. 2015;17(1):124–134. | ||
Hao N, Tian Y, Liu W, et al. Antimuscarinics and alpha-blockers or alpha-blockers monotherapy on lower urinary tract symptoms – a meta-analysis. Urology. 2014;83:556–562. | ||
Johnson TM 2nd, Markland AD, Goode PS, et al. Efficacy of adding behavioural treatment or antimuscarinic drug therapy to alpha-blocker therapy in men with nocturia. BJU Int. 2013;112:100–108. | ||
Kaplan SA, Roehrborn CG, Abrams P, Chapple CR, Bavendam T, Guan Z. Antimuscarinics for treatment of storage lower urinary tract symptoms in men: a systematic review. Int J Clin Pract. 2011;65(4):487–507. | ||
Xin Z, Huang Y, Lu J, Zhang Q, Chen C. Addition of antimuscarinics to alpha-blockers for treatment of lower urinary tract symptoms in men: a meta-analysis. Urology. 2013;82(2):270–277. | ||
Han HH, Ko WJ, Yoo TK, et al. Factors associated with continuing medical therapy after transurethral resection of prostate. Urology. 2014;84(3):675–680. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.