Back to Journals » Cancer Management and Research » Volume 12
Efficacy and Safety of Anlotinib for Patients with Advanced NSCLC Who Progressed After Standard Regimens and the Preliminary Analysis of an Efficacy Predictor
Authors Cheng JD, Chai LX, Zhao ZP, Hao YY, Li S
Received 10 March 2020
Accepted for publication 12 June 2020
Published 12 July 2020 Volume 2020:12 Pages 5641—5650
DOI https://doi.org/10.2147/CMAR.S253366
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Eileen O'Reilly
Jian-De Cheng,1,* Li-Xun Chai,2,* Zhi-Ping Zhao,1 Yan-Yan Hao,1 Shuo Li3
1Department of Respiratory and Critical Care Medicine, The Shanxi Bethune Hospital, Taiyuan 030032, Shanxi, People’s Republic of China; 2Department of Thoracic Surgery, The Shanxi Bethune Hospital, Taiyuan 030032, Shanxi, People’s Republic of China; 3Department of Respiratory and Critical Medicine, Tianjin Medical University General Hospital, Tianjin 300052, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Shuo Li
Department of Respiratory and Critical Medicine, Tianjin Medical University General Hospital, Tianjin 300052, People’s Republic of China
Tel +86 13512279233
Email [email protected]
Background: The aim of this study was to investigate the efficacy and safety of anlotinib for patients with advanced non-small cell lung cancer (NSCLC) who progressed after standard regimens in real world situations and the preliminary analysis of an efficacy predictor.
Methods: A total of 118 patients with advanced NSCLC who progressed after standard regimens were included in this retrospective study. Efficacy was evaluated and toxicity profile was recorded. Progression-free survival (PFS) and overall survival (OS) were assessed using Kaplan–Meier survival curve and multivariate analysis was adjusted using Cox regression analysis.
Results: All of the 118 patients with NSCLC were available for evaluation of efficacy. Complete response (CR, 0 case), partial response (PR, 10 cases), stable disease (SD, 79 cases) and progressive disease (PD, 29 cases) were evaluated according to RECIST version 1.1. In consequence, objective response rate (ORR) was 8.47% and disease control rate (DCR) was 75.42%. The median PFS of the 118 patients with NSCLC was 4.3 months and the median OS was 10.3 months. The results of Cox regression analysis suggested that ECOG score was an independent factor for PFS. The toxicity profile indicated that hypertension and hand-foot syndrome were the most common adverse reactions. Additionally, the preliminary analysis of an efficacy predictor suggested that the PFS of patients with hypertension was superior to those without hypertension.
Conclusion: Anlotinib is effective and safe for patients with advanced NSCLC who progressed after standard regimens in real world situations. Hypertension may be a biomarker for efficacy prediction.
Keywords: non-small cell lung cancer, anlotinib, efficacy, safety, biomarker
Introduction
Lung cancer is the most common malignancy and the leading cause of cancer-related deaths worldwide, which accounts for approximately 2.1 million new cases and 1.77 million new deaths around the world annually.1 Currently, there are approximately 0.733 million new cases and 0.61 million new deaths in the People's Republic of China each year.2 Non-small cell lung cancer (NSCLC) accounts for 80~85% of lung cancer cases.3 Recent years have witnessed great progress in the treatment for advanced NSCLC with regard to molecular and targeted therapy, which rendered advanced NSCLC the most successful cancer in precision medicine.4 Targeted drugs were developed in EGFR, ALK, ROS1, BRAF and provided significant survival benefits for the patients.5 However, approximately 50% of patients with NSCLC in the People's Republic of China did not have a driver gene mutation with clinical significance and could only receive platinum-containing double drug chemotherapy regimen as the first-line treatment.6 The efficacy of chemotherapy was limited with an objective response rate (ORR) of 20%~30% and the median progression-free survival (PFS) of 4~5 months.7 When the patients progressed after first-line therapy, docetaxel, pemetrexed, gemcitabine and immunotherapy was available as second-line treatment.8 However, the advantages of traditional second-line single-agent chemotherapy were dismal. Fortunately, immune checkpoint inhibitor (ICI) had shown remarkable benefit in the treatment of patients with NSCLC and emerged as an effective treatment option as first- and second-line therapy. The anti-PD-1 agent pembrolizumab is approval for use as first- and second-line treatment. Nivolumab and atezolizumab were both indicated for use as second-line therapy regardless of PD-L1 expression.9 However, the first ICI drug nivolumab was licensed in mainland People's Republic of China in June 2018 with a high price after anlotinib was approved. In consequence, the application of ICIs as further-line treatment of patients with NSCLC was relatively limited. Therefore, patients with NSCLC were in need of effective drugs urgently when progressing after standard regimens.
Angiogenesis plays an important role in proliferation and metastasis of tumor.10 Antiangiogenic drugs have demonstrated potential anticancer activity in the treatment of advanced NSCLC recently. Bevacizumab was the first antiangiogenic humanized monoclonal antibody with the prevention for the bonding of the VEGF ligand-receptor. It was proved to significantly improve PFS and OS as first-line treatment for patients with NSCLC in ECOG4599 and Beyond clinical trials.11,12 Furthermore, ramucirumab showed additional survival benefits for patients with NSCLC as second-line treatment in the REVEL clinical trial.13
Regarding the anti-angiogenesis small molecule tyrosine kinase inhibitor (TKI), sorafenib, sunitinib, pazopanib and fruquintinib were proved to prolong PFS for patients with NSCLC in third-line therapy.14,15 Fortunately, anlotinib prolonged PFS and OS in a phase III clinical trial for patients with advanced NSCLC as a novel oral multi-target TKI with the inhibition of VEGFR1~3, FGFR1~4, PDGFRα~β, c-Kit and Ret.16,17 In consequence, anlotinib was licensed as the standard third-line regimen for patients with advanced NSCLC by the China State Food and Drug Administration (cFDA) in 2018.
To the best of our knowledge, the ORR in the clinical application of anti-angiogenic drugs was generally low. In the treatment of advanced NSCLC, the ORR of sorafenib, anlotinib, fruquintinib and apatinib monotherapy were 4.9%, 9.2%, 16.4% and 4.0%, respectively.18 Therefore, it seemed that there was great individual difference regarding the efficacy of anti-angiogenic drugs clinically. Consequently, the investigation of biomarkers for patients who received vascular targeted drugs was a research hotspot in the field of anti-angiogenesis therapy.19
Therefore, the aim of the present study was to investigate the efficacy and safety of anlotinib for patients with advanced NSCLC who progressed after standard regimens in real world situations and the preliminary analysis of an efficacy predictor.
Patients and Methods
Study Design
This study was a retrospective analysis. Patients with advanced NSCLC who progressed after standard therapy in the Department of Respiratory and Critical Care Medicine of the Shanxi Bethune Hospital from June 2018 to December 2019 were included in this study. The eligibility criteria included: 1) diagnosis of NSCLC with pathological stage IIIb or IV; 2) age ≥18 years; 3) an Eastern Cooperative Oncology Group (ECOG) performance status of 0~2; 4) anlotinib was administered for patients who progressed after standard regimens; and 5) at least a measurable target lesion. The exclusion criteria included: 1) brain metastasis symptoms or controlled symptoms for <2 months; 2) concomitant with another cancer or serious disease; 3) hemoptysis >50 mL/day; 4) efficacy evaluation or follow-up data of the patients was not available. The flow chart of this retrospective study is illustrated in Figure 1. Finally, a total of 118 patients with advanced NSCLC was enrolled. The present study was approved by the ethics committee of the Shanxi Bethune Hospital. Informed consent was signed by each enrolled patient in accordance with the recommendations of the Declaration of Helsinki.
 |
Figure 1 The flow chart of the retrospective study of anlotinib for patients with advanced NSCLC who progressed after standard regimens. |
Administration of Anlotinib
Anlotinib was orally administered at an initial dosage of 12 mg per day, half an hour after meals with warm water for 14 days and discontinued for 7 days, repeated every 21 days. Patients continued anlotinib until disease progression or intolerable as a result of adverse reactions. Additionally, 10 mg and 8 mg were alternative dosages for the adjustment of anlotinib according to the toxicity during the treatment. And the treatment was discontinued following the occurrence of a potentially life-threatening toxic reaction.
Evaluation of Efficacy and Safety and the Protocol of Follow-Up
The efficacy of treatment with anlotinib was assessed according to RECIST 1.1 criteria.20 The change in target lesions was evaluated using computed tomography (CT) scans every two cycles or depending on the actual situations when clinical symptoms of the patients were getting worse. Adverse reactions during treatment were evaluated using Common Terminology Criteria for Adverse Events (CTCAE) 4.03 to record toxicity profile that might be drug-related.21 From the objective view, the adverse reactions with the incidence >5% were documented and analyzed. Hypertension was mainly performed and included in the preliminary analysis of efficacy predictor. The hypertension included in the analysis of efficacy predictor was the acquired hypertension resulting from the treatment of anlotinib.
The initial follow-up was performed in the hospital where baseline characteristics and adverse reactions and the date of disease progression could be obtained using the electronic medical record system clearly. The subsequent follow-up was performed by telephone. Patients were followed up every 3 months and status of death was mainly inquired. When a patient had progressed or died, it had to be confirmed by at least two research colleagues before it could be confirmed as an event of progression or death.
Statistical Analysis
All of the variables in this study were statistically processed using SPSS version 25.0 (IBM Corporation, Armonk, NY, USA). The significance of observed differences in proportion variables and continuous variables according to hypertension status was tested using the chi-square test and the Mann–Whitney U nonparametric test, respectively. The primary analysis was performed on PFS. Kaplan–Meier survival curves were created using Stata 14.0. Survival differences in PFS and OS according to the hypertension status of the patients were compared using Log rank test. PFS was defined as the period from the time of treatment with anlotinib to disease progression or death of the patient from any cause, whichever occurred first. OS was defined as the period from the time of treatment with anlotinib to patients’ death from any cause. For those without disease progression or death by the end of the study follow-up, survival end points were censored at the date of last follow-up.22 Cox regression analysis was constructed for PFS for multivariable analysis and the backward-selection procedure was used to adjust for potential confounding covariates. Statistical significance was accepted when P<0.05.
Results
Baseline Characteristics
The baseline characteristics of the 118 patients with NSCLC is shown in Table 1. The median age of the patients was 61 years (range: 22~77 years). A total of 77 patients were male (65.25%). Pathological stage IV was observed in 111 patients (94.07%). ECOG 0 score was noted in 25 patients (21.19%). A total of 82 patients were Nonsmoker/former smokers (69.49%). The most common histology was adenocarcinoma (85 cases, 72.03%). Number of metastases sites of ≤3 and >3 were 73 and 45 cases, respectively. Positive driver gene mutation was noted in 44 patients (37.29%). History of previous treatment of second line and further line was observed in 38 and 80 cases, respectively. A total of 73 patients (61.86%) had received targeted drug therapy previously. And 8 patients (6.78%) previously received the treatment of anti-vascular TKI.
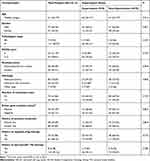 |
Table 1 Baseline Characteristics of the 118 Patients with NSCLC According to Hypertension Status of the Patients |
Efficacy of the 118 Patients with Advanced NSCLC Who Received Anlotinib Therapy
All of the 118 patients were available for efficacy evaluation. The best overall response among the 118 patients was recorded during anlotinib treatment. Complete response (CR, 0 case), partial response (PR, 10 cases), stable disease (SD, 79 cases) and progressive disease (PD, 29 cases) were assessed according to RECIST version 1.1. Therefore, the ORR was 8.47%, disease control rate (DCR) was 75.42%. The waterfall plot of the best percentage change in target lesion is shown in Figure 2.
 |
Figure 2 The waterfall plot of best change (reductions in sum of target lesion diameters) from baseline in the 118 patients with NSCLC who received anlotinib treatment. |
The data cutoff date was February 2020. The median follow-up of all patients from the time of enrollment to the last follow-up was 10.1 months (follow-up range: 1~19 months). As shown in Figure 3, the median PFS of the 118 patients with NSCLC was 4.3 months (Lower confidence interval [LCI]~Upper confidence interval [UCI]: 3.68~4.92).
 |
Figure 3 The progression-free survival and overall survival of the 118 patients with NSCLC who received anlotinib treatment. |
Additionally, the PFS according to different baseline characteristic subgroups were analyzed. As shown in Figure 4, the results of univariate analysis suggested that ECOG score was significantly associated with PFS. The median PFS of the patients with ECOG 0 score was longer than those with ECOG 1~2 score (5.60 vs 3.70, P=0.015). Also, patients with the number of metastases sites >3 demonstrated a trend for worse PFS, even though the difference was not statistically significant (P=0.075).
 |
Figure 4 The forest plot of median progression-free survival of the 118 patients with NSCLC who received anlotinib treatment according to different baseline characteristics subgroups. |
Furthermore, given that the follow-up period was long enough, OS was also assessed in this study. The median OS of the 118 patients with NSCLC was 10.3 months (LCI~UCI: 8.62~11.98).
Safety Profile of 118 Patients with NSCLC Who Received Anlotinib Treatment
To the best of our knowledge, adverse reaction was an important aspect to evaluate the clinical application of anlotinib at an initial dosage of 12 mg. No grade 5 adverse reactions were observed in this study. As shown in Table 2, the common drug-related adverse reactions with an incidence >5% during anlotinib monotherapy were hypertension, hand-foot syndrome, fatigue, anorexia symptoms, hypertriglyceridemia, oral mucositis, diarrhea, proteinuria, weight loss, and hoarseness. And the incidence was 33.05%, 29.66%, 23.73%, 22.04%, 18.64%, 13.56%, 10.17%, 7.63%, 5.93%, and 5.08%, respectively. Most of the adverse reactions were moderate of grade 1~2. The grade ≥3 adverse reactions were hypertension (7.63%), hand-foot syndrome (5.93%), fatigue (2.54%), hypertriglyceridemia (0.85%), oral mucositis (0.85%) and diarrhea (0.85%), respectively. Interestingly, patients with hemoptysis was observed in 2 cases (1.69%).
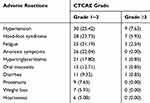 |
Table 2 The Safety Profile of the 118 Patients with NSCLC Who Received Anlotinib Monotherapy |
Preliminary Analysis of an Efficacy Predictor
The preliminary analysis of an efficacy predictor was mainly focused on hypertension. As shown in Table 2, a total of 39 patients experienced hypertension during anlotinib treatment. In consequence, the PFS of the patients with NSCLC according to hypertension status was analyzed. The baseline characteristics of the 118 patients with NSCLC according to hypertension status were well balanced. The PFS of 118 patients with NSCLC according to hypertension status is illustrated in Figure 5, the median PFS of patients with hypertension was longer than that of patients with non-hypertension (5.0 vs 3.3 months, χ2=5.13, P=0.02). Furthermore, Cox regression analysis was constructed including the baseline characteristics which were significant in the univariate analysis to adjust for the confounding factors. Results of multivariate analysis are shown in Table 3, a statistically significant difference was observed for the influence of hypertension status on PFS after the multivariate adjustment, which suggested that hypertension status was an independent factor for PFS (hazard ratio [HR]=1.51, P=0.031). Additionally, ECOG score was also an independent factor for PFS (HR=1.65, P=0.018).
 |
Table 3 Multivariate Cox Regression Analysis for PFS According to Baseline Characteristics and Hypertension Status |
 |
Figure 5 The progression-free survival of the 118 patients with NSCLC who received anlotinib treatment according to hypertension status. |
Discussion
This retrospective study provided real-world evidence regarding the efficacy and safety of anlotinib for patients with advanced NSCLC who progressed after standard regimens. The preliminary analysis of an efficacy predictor indicated that hypertension predicted superior prognosis. Anlotinib was effective and safe in patients with advanced NSCLC who progressed after standard regimens.
Recent years have witnessed great progress in the treatment for advanced NSCLC regarding first-line and second-line of molecular and targeted therapy, which gives more opportunities for patients to receive third-line and further-line treatment.23 As a multi-target tyrosine kinase inhibitor, anlotinib suppressed tumor angiogenesis via inhibition of VEGFR, PDGFR and FGFR.24 Besides, tumor cell proliferation was inhibited by anlotinib through the target of c-Kit, Ret and c-FMS. And these were newly identified kinase targets involving tumor progression.25 Consequently, anlotinib demonstrated promising anticancer activity and safety in NSCLC,17 SCLC,26 soft tissue sarcoma,22 renal carcinoma,27 and esophageal squamous cell carcinoma.28
With regard to the clinical outcomes of the patients with advanced NSCLC included in our study, the ORR was 8.47% and DCR was 75.42%. And the median PFS was 4.3 months. The efficacy of anlotinib in our study was slightly lower and worse than that of the phase III clinical trial of anlotinib for advanced NSCLC initiated by Han et al17 in ALTER0303 study (ORR=9.2%, DCR=81.0%, mPFS=5.4 months of anlotinib group). We hypothesized that the reason might be attributed to the retrospective design of our study, the management of the patients was not sufficient and normative compared with the phase III clinical trial, as shown in the other previous retrospective study.29 On the other hand, patients with ECOG score 2 were also included in our study. To the best of our knowledge, the influence of ECOG score on the prognosis of patients was confirmed in numerous studies. And the conclusion indicated that the higher the score, the worse the prognosis.30 Additionally, the results of Cox regression analysis in our study suggested that patients with 1~2 ECOG score were associated with worse PFS. And the result was in concert with that of a previous study.31 Interestingly, a retrospective analysis initiated by Wu et al32 included 81 patients with advanced NSCLC who received anlotinib treatment. The ORR, DCR and median PFS in their study was 7%, 84% and 5 months, respectively. And the results were consistent with that of our study. Furthermore, another retrospective analysis of anlotinib in the treatment for advanced lung cancer initiated by Shao et al33 included 58 patients with advanced lung cancer. The median PFS was similar with that of our study. Unfortunately, both of these two retrospective studies failed to assess the OS owing to the relatively insufficient period of follow-up. Given that the period of follow-up in our study was long, OS was carried out eventually. Amazingly, the median OS of the 118 patients who received anlotinib therapy was 10.3 months, which was slightly longer than that reported in ALTER0303 study (median OS=9.6 months). We speculated that the reason might be attributed to the continued approval of immunotherapy drugs and targeted drugs in the People's Republic of China since the license of anlotinib in 2018. Patients with advanced NSCLC had sufficient opportunity to use immunotherapy and targeted drugs in the subsequent-line treatment, which were proved to be effective and offered survival benefit to the patients.34
With regard to safety profile, our study indicated that hypertension was the most common adverse reaction, which is consistent with the results of the previous studies in patients with NSCLC and other tumors who received anlotinib treatment.35 The other adverse reactions were hand-foot syndrome, fatigue, anorexia symptoms, hypertriglyceridemia, oral mucositis, diarrhea, proteinuria, weight loss, and hoarseness. And these were the common adverse reactions found in the ALTER0303 trial. No new adverse events were observed and the results were consistent with the previous retrospective studies.32 Interestingly, the incidence of the adverse reactions in the retrospective studies were lower than that in the ALTER0303 trial. We speculated that the difference might be attributed to the retrospective design. The adverse reactions of retrospective studies were documented poorly and insufficiently compared to the phase III clinical trial, which was in line with the other retrospective study.36
To our knowledge, our study was the first report regarding the association between prognosis and adverse reaction of anlotinib. The preliminary analysis of an efficacy predictor in our study suggested that hypertension could be used as a biomarker to predict the efficacy, which was consistent with the results of the previous study of apatinib.31,37 Additionally, a retrospective analysis regarding the relationship between hypertension and clinical outcomes among patients with advanced NSCLC who were treated with bevacizumab demonstrated a similar result.38 Hypertension is a common adverse reaction which is associated with treatment of angiogenesis inhibitors that target the VEGF/VEGFR pathway. However, the mechanisms have not been thoroughly elucidated. Several studies found that inhibition of VEGFR in vascular endothelial cells decreased the production of nitric oxide and prostacyclins, thus contributing to increased blood pressure.39 Therefore, hypertension induced by angiogenesis inhibitors could partly reflect the inherent host biology which resulted in the difference in VEGF/VEGFR blockade and served as a biomarker for the efficacy of anlotinib. Furthermore, the conclusion that patients with hypertension conferred a superior PFS should be validated in large-scale prospective trials. Additionally, medical control should be used to control hypertension rather than interruption of anlotinib. However, this approach should be differentiated and the prompt discontinuation of anlotinib administration was necessary when life-threatening adverse reactions occurred.
From the objective view, a number of limitations existed in our study. Firstly, the sample size was small as a real-world study. Efficacy of anlotinib in patients with NSCLC and the prognostic significance of hypertension needed to be validated in clinical trials. Secondly, our study was designed as a retrospective analysis and some bias might have been unavoidable. However, the prognosis significance of the hypertension was fully evaluated and interpreted. We thought our study was of clinical significance for the evaluation of prognosis in patients with advanced NSCLC who were treated with anlotinib.
Conclusion
This retrospective study provides real-world evidence regarding the efficacy and safety of anlotinib for patients with advanced NSCLC who progressed after standard regimens. Hypertension may be a biomarker for efficacy prediction. Medical control should be used to control hypertension rather than interruption of anlotinib. However, this approach should be differentiated and the prompt discontinuation of anlotinib administration was necessary when life-threatening adverse reactions occurred.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Bray F, Ferlay J, Soerjomataram I, et al. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68(6):394–424. doi:10.3322/caac.21492
2. Chen W, Zheng R, Baade PD, et al. Cancer statistics in China, 2015. CA Cancer J Clin. 2016;66(2):115–132. doi:10.3322/caac.21338
3. Zhi XY, Zou XN, Hu M, et al. Increased lung cancer mortality rates in the Chinese population from 1973–1975 to 2004–2005: an adverse health effect from exposure to smoking. Cancer. 2015;121(Suppl 17):3107–3112. doi:10.1002/cncr.29603
4. Ruiz-Cordero R, Devine WP. Targeted therapy and checkpoint immunotherapy in lung cancer. Surg Pathol Clin. 2020;13(1):17–33. doi:10.1016/j.path.2019.11.002
5. Dong J, Li B, Lin D, et al. Advances in targeted therapy and immunotherapy for non-small cell lung cancer based on accurate molecular typing. Front Pharmacol. 2019;10:230. doi:10.3389/fphar.2019.00230
6. Arbour KC, Riely GJ. Systemic therapy for locally advanced and metastatic non-small cell lung cancer: a review. JAMA. 2019;322(8):764–774. doi:10.1001/jama.2019.11058
7. Ghadyalpatil NS, Pandey A, Krishnamani I, et al. First-line management of metastatic non-small cell lung cancer: an Indian perspective. South Asian J Cancer. 2019;8(2):73–79. doi:10.4103/sajc.sajc_294_18
8. Gridelli C, Baas P, Barlesi F, et al. Second-line treatment options in non-small-cell lung cancer: report from an international experts panel meeting of the Italian Association of Thoracic Oncology. Clin Lung Cancer. 2018;19(4):301–314. doi:10.1016/j.cllc.2017.12.010
9. Lim SM, Hong MH, Kim HR. Immunotherapy for non-small cell lung cancer: current landscape and future perspectives. Immune Netw. 2020;20(1):e10. doi:10.4110/in.2020.20.e10
10. Cantelmo AR, Dejos C, Kocher F, et al. Angiogenesis inhibition in non-small cell lung cancer: a critical appraisal, basic concepts and updates from American Society for Clinical Oncology 2019. Curr Opin Oncol. 2020;32(1):44–53. doi:10.1097/cco.0000000000000591
11. Sandler A, Gray R, Perry MC, et al. Paclitaxel-carboplatin alone or with bevacizumab for non-small-cell lung cancer. N Engl J Med. 2006;355(24):2542–2550. doi:10.1056/NEJMoa061884
12. Zhou C, Wu YL, Chen G, et al. BEYOND: a randomized, double-blind, placebo-controlled, multicenter, phase III study of first-line carboplatin/paclitaxel plus bevacizumab or placebo in Chinese patients with advanced or recurrent nonsquamous non-small-cell lung cancer. J Clin Oncol. 2015;33(19):2197–2204. doi:10.1200/jco.2014.59.4424
13. Garon EB, Ciuleanu TE, Arrieta O, et al. Ramucirumab plus docetaxel versus placebo plus docetaxel for second-line treatment of stage IV non-small-cell lung cancer after disease progression on platinum-based therapy (REVEL): a multicentre, double-blind, randomised phase 3 trial. Lancet. 2014;384(9944):665–673. doi:10.1016/s0140-6736(14)60845-x
14. Qiang H, Chang Q, Xu J, et al. New advances in antiangiogenic combination therapeutic strategies for advanced non-small cell lung cancer. J Cancer Res Clin Oncol. 2020;146(3):631–645. doi:10.1007/s00432-020-03129-6
15. Spagnuolo A, Palazzolo G, Sementa C, et al. Vascular endothelial growth factor receptor tyrosine kinase inhibitors for the treatment of advanced non-small cell lung cancer. Expert Opin Pharmacother. 2020;1–16. doi:10.1080/14656566.2020.1713092.
16. Xie C, Wan X, Quan H, et al. Preclinical characterization of anlotinib, a highly potent and selective vascular endothelial growth factor receptor-2 inhibitor. Cancer Sci. 2018;109(4):1207–1219. doi:10.1111/cas.13536
17. Han B, Li K, Wang Q, et al. Effect of anlotinib as a third-line or further treatment on overall survival of patients with advanced non-small cell lung cancer: the ALTER 0303 phase 3 randomized clinical trial. JAMA Oncol. 2018;4(11):1569–1575. doi:10.1001/jamaoncol.2018.3039
18. Villaruz LC, Socinski MA. The role of anti-angiogenesis in non-small-cell lung cancer: an update. Curr Oncol Rep. 2015;17(6):26. doi:10.1007/s11912-015-0448-y
19. Liu X, Qin S, Wang Z, et al. Correction to: early presence of anti-angiogenesis-related adverse events as a potential biomarker of antitumor efficacy in metastatic gastric cancer patients treated with apatinib: a cohort study. J Hematol Oncol. 2018;11(1):5. doi:10.1186/s13045-017-0545-5
20. Eisenhauer EA, Therasse P, Bogaerts J, et al. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer. 2009;45(2):228–247. doi:10.1016/j.ejca.2008.10.026
21. Miller TP, Fisher BT, Getz KD, et al. Unintended consequences of evolution of the common terminology criteria for adverse events. Pediatr Blood Cancer. 2019;66(7):e27747. doi:10.1002/pbc.27747
22. Chi Y, Fang Z, Hong X, et al. Safety and efficacy of anlotinib, a multikinase angiogenesis inhibitor, in patients with refractory metastatic soft-tissue sarcoma. Clin Cancer Res. 2018;24(21):5233–5238. doi:10.1158/1078-0432.ccr-17-3766
23. Hu Z, Li M, Chen Z, et al. Advances in clinical trials of targeted therapy and immunotherapy of lung cancer in 2018. Transl Lung Cancer Res. 2019;8(6):1091–1106. doi:10.21037/tlcr.2019.10.17
24. Lin B, Song X, Yang D, et al. Anlotinib inhibits angiogenesis via suppressing the activation of VEGFR2, PDGFRbeta and FGFR1. Gene. 2018;654:77–86. doi:10.1016/j.gene.2018.02.026
25. Sun Y, Niu W, Du F, et al. Safety, pharmacokinetics, and antitumor properties of anlotinib, an oral multi-target tyrosine kinase inhibitor, in patients with advanced refractory solid tumors. J Hematol Oncol. 2016;9(1):105. doi:10.1186/s13045-016-0332-8
26. Chen D, Xu J, Zhao Y, et al. Prognostic value of tumor cavitation in extensive-stage small-cell lung cancer patients treated with anlotinib. J Cancer Res Clin Oncol. 2020;146(2):401–406. doi:10.1007/s00432-019-03064-1
27. Zhou AP, Bai Y, Song Y, et al. Anlotinib versus sunitinib as first-line treatment for metastatic renal cell carcinoma: a randomized phase II clinical trial. Oncologist. 2019;24(8):e702–e708. doi:10.1634/theoncologist.2018-0839
28. Zhang PL, Liu ZJ. Esophago-tracheobronchial fistula following treatment of anlotinib in advanced squamous cell lung cancer: two case reports. Medicine (Baltimore). 2019;98(44):e17700. doi:10.1097/md.0000000000017700
29. Song ZZ, Zhao LF, Zuo J, et al. Clinical outcomes and safety of apatinib mesylate in the treatment of advanced non-squamous non-small cell lung cancer in patients who progressed after standard therapy and analysis of the KDR gene polymorphism. Onco Targets Ther. 2020;13:603–613. doi:10.2147/ott.s222985
30. Friedlaender A, Banna GL, Buffoni L, et al. Poor-performance status assessment of patients with non-small cell lung cancer remains vague and blurred in the immunotherapy era. Curr Oncol Rep. 2019;21(12):107. doi:10.1007/s11912-019-0852-9
31. Fang SC, Huang W, Zhang YM, et al. Hypertension as a predictive biomarker in patients with advanced non-small-cell lung cancer treated with apatinib. Onco Targets Ther. 2019;12:985–992. doi:10.2147/ott.s189984
32. Wu D, Nie J, Dai L, et al. Salvage treatment with anlotinib for advanced non-small cell lung cancer. Thorac Cancer. 2019;10(7):1590–1596. doi:10.1111/1759-7714.13120
33. Shao L, Wang W, Song Z, et al. The efficacy and safety of anlotinib treatment for advanced lung cancer. Onco Targets Ther. 2019;12:6549–6554. doi:10.2147/ott.s205674
34. Nadal E, Massuti B, Domine M, et al. Immunotherapy with checkpoint inhibitors in non-small cell lung cancer: insights from long-term survivors. Cancer Immunol Immunother. 2019;68(3):341–352. doi:10.1007/s00262-019-02310-2
35. Tian Z, Liu H, Zhang F, et al. Retrospective review of the activity and safety of apatinib and anlotinib in patients with advanced osteosarcoma and soft tissue sarcoma. Invest New Drugs. 2020. doi:10.1007/s10637-020-00912-7
36. Liu Z, Ou W, Li N, et al. Apatinib monotherapy for advanced non-small cell lung cancer after the failure of chemotherapy or other targeted therapy. Thorac Cancer. 2018;9(10):1285–1290. doi:10.1111/1759-7714.12836
37. Fan M, Zhang J, Wang Z, et al. Phosphorylated VEGFR2 and hypertension: potential biomarkers to indicate VEGF-dependency of advanced breast cancer in anti-angiogenic therapy. Breast Cancer Res Treat. 2014;143(1):141–151. doi:10.1007/s10549-013-2793-6
38. Dahlberg SE, Sandler AB, Brahmer JR, et al. Clinical course of advanced non-small-cell lung cancer patients experiencing hypertension during treatment with bevacizumab in combination with carboplatin and paclitaxel on ECOG 4599. J Clin Oncol. 2010;28(6):949–954. doi:10.1200/jco.2009.25.4482
39. Tang JR, Markham NE, Lin YJ, et al. Inhaled nitric oxide attenuates pulmonary hypertension and improves lung growth in infant rats after neonatal treatment with a VEGF receptor inhibitor. Am J Physiol Lung Cell Mol Physiol. 2004;287(2):L344–351. doi:10.1152/ajplung.00291.2003
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
