Back to Journals » Journal of Pain Research » Volume 13
Effectiveness of Kinesio Taping on the Management of Knee Osteoarthritis: A Systematic Review of Randomized Controlled Trials
Authors Melese H , Alamer A , Hailu Temesgen M , Nigussie F
Received 15 February 2020
Accepted for publication 8 April 2020
Published 28 May 2020 Volume 2020:13 Pages 1267—1276
DOI https://doi.org/10.2147/JPR.S249567
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Professor Robert B. Raffa
Haimanot Melese,1 Abayneh Alamer,1 Melaku Hailu Temesgen,1 Fetene Nigussie2
1Department of Physiotherapy, School of Medicine, College of Health Sciences and Ayder Comprehensive Specialized Hospital, Mekelle University, Mekelle, Ethiopia; 2Department of Nursing Institute of Medicine, College of Health Sciences, Debre Berhan University, Debre Berhan, Ethiopia
Correspondence: Abayneh Alamer Tel +251 922276256
Fax +251 344416681/91
Email [email protected]
Abstract: The purpose of this review was to summarize the current best evidence for the effectiveness of Kinesio Taping in reducing pain and increasing knee function for patients with knee osteoarthritis. A comprehensive search of literature published between 2014 and 2019 was conducted using the following electronic databases: PubMed, Google Scholar, Physiotherapy Evidence Database (PEDro), Science Direct, and Scopus. Only randomized controlled trials evaluating the effect of Kinesio Taping on knee osteoarthritis were included. PEDro was used to assess the risk of bias of included trials. This study was reported according to the guideline of the PRISMA statement. The methodological quality of the studies was done using the PEDro scale and GRADE approach. The overall quality of evidence was rated from moderate to high. Eighteen randomized trials involving 876 patients were included. The present systematic review demonstrated that there were significant differences between Kinesio Taping groups and control groups in terms of visual analog scale (VAS), Western Ontario and MacMaster Universities Osteoarthritis Index (WOMAC) scale and flexion range of motion. Kinesio Taping is effective in improving pain and joint function in patients with knee OA.
Keywords: Kinesio Taping, osteoarthritis, knee joint, systematic review
Introduction
Osteoarthritis (OA) is a long-term chronic degenerative disease characterized by the deterioration of cartilage in joints and creating stiffness, pain, and impaired movement.1 According to the World Health Organization (WHO), OA is one of the major disabling conditions among musculoskeletal disorders and forecasted that it will become the fourth primary cause of disability by the year 2020.2,3 It had increasing physical, psychological, and socioeconomic burden globally.3,4 Osteoarthritis of the knee is a major leading cause of mobility impairment.5,6 Knee pain, decreased knee flexibility, and functional inability are common clinical manifestations during daily activities among patients with knee OA.7,8 Previous studies have reported that pain and significant physical functional limitations have been associated with reduced muscle strength, poor proprioception, and impaired self-reported knee status anticipated that worsening of knee instability over time.9–12
Clinically, conservative nonpharmacological treatments such as resistance strengthening exercises, low-impact aerobic exercises, whole-body vibration, neuromuscular education, and KT were used to relieve pain, to delay complications, and to prevent disease progression for knee OA.13,14 Among those different treatments used to treat knee OA, the application of Kinesio Taping (KT) had gained popularity.15–17 Current evidence18–20 showed that KT is becoming the latest and routine treatment option among other forms of intervention for pain relief and to improve functional performance on subjects with knee OA.
KT was originally developed by Kase et al21 and has been used in clinics for Various therapeutic benefits such as; inhibiting pain, increasing muscle strength, facilitating motor skills and reducing muscle fatigue to patients with sport injuries or musculoskeletal disorders.22,23 The physiological effects of KT have been assumed lifting the skin to increases the inter-tissue space and improves blood and lymph circulation,20 “Gate-control of pain”, and through “Neurofacilitation” on a human body system.24 However, the current evidence regarding its effectiveness appear to be unclear and debatable in reducing pain, improving range of motion and preventing functional disability when compared to other forms of intervention in individuals with musculoskeletal disorders.23,25–28
Given the lack of consistency and resulted uncertainty regarding the clinical worthiness of KT in parameters of pain, range of motion, functional disability among subjects with knee OA, there is still a need for current evidence with high-quality trials in a systematic way. Therefore, this review was aimed to call into question about the effectiveness of KT on subjects with Knee osteoarthritis based on recent trials.
Methods
Design and Protocol Registration
This systematic review was conducted and reported in compliance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines.29
Search Strategy
A literature search was performed to identify all eligible randomized controlled trials. An electronic search of the literature was conducted to identify relevant studies from Google Scholar, PEDro, Science direct, Scopus, and PubMed. The following terms were used as key words: “Kinesio Taping”, “Elastic Taping, “knee osteoarthritis” and “randomized controlled trial”. As subject headings varied between the databases, various combinations of the key words were used; “Kinesio Taping /Elastic Taping/sham taping/patellar taping/Kinesiology Taping” AND “osteoarthritis/knee joint pain/Arthritis/degenerative knee arthritis” AND “randomized controlled trial”. The retrieving of the studies was set from 2014 to 2019 for the articles.
Eligibility Criteria
Studies searched were considered eligible if they met the following criteria: 1) population: patients with knee OA; 2) intervention: intervention groups received KT for the treatment of knee OA; 3) comparisons: control group received sham taping/placebo KT; 4) outcomes: visual analog scale (VAS), McMaster Universities Arthritis Index (WOMAC) scale, range of motion, TUG test. All randomized control trials (RCT) conducted to determine the effectiveness of KT rehabilitation on knee osteoarthritis patients were included in this review. Studies in which the addition of KT over other interventions (experimental group) compared with other interventions only (control group) were also included. Only full-length articles reported in English were included. Observational studies, quasi-experimental studies and conference abstracts were excluded from this review.
Study Selection
Three reviewers (H.M, M.H and A.A) retrieved papers from the identified lists on the basis of title/abstract, based on the established criteria for inclusion. The studies were retrieved in detail through methodological quality and data extraction. The fourth reviewer (F.N) solved the discordance among the reviewers.
Data Extraction
A data extraction tool was prepared by the reviewers and reviewers extracted the data independently. The following data were extracted from each trial using PICOS: authors’ name and year of publication, OA definition (severity measure, type and duration), number of participants in treatment and control group, mean follow-up time, type of treatment, mean age of the participants, primary outcome measures, study design, study results and study conclusions.
Risk of Bias
Three reviewers assess the quality of included studies based on the Physiotherapy Evidence Database (PEDro) Scale scored using 10 items with the first item (external validity of the article) quality assessments of controlled interventional studies tool.30,31 The PEDro scale assesses the methodological quality of a study based on important criteria, such as concealed allocation, intention-to-treat analysis, and adequacy of follow-up. These characteristics make the PEDro scale a useful tool to assess the methodological quality of physical therapy and rehabilitation trials. The overall quality of the evidence and the strength of recommendations were also evaluated using the GRADE approach.32 The GRADE approach specifies four levels of quality (high, moderate, low and very low). The overall evidence was downgraded depending on the presence of five factors: limitations (due to risk of bias); consistency of results; directness (e.g. whether participants are similar to those about whom conclusions are drawn); precision (ie, sufficient data to produce narrow confidence intervals); and other (e.g., publication bias).
Results
Study Selection
A total of 2443 articles were identified by the searching strategy. After adjusting for duplicates, 1740 remained. After title and abstract screening among 703studies, 635studies were excluded. After full-text screening out of 68 articles, 18 randomized controlled trials were included in this review (Figure 1).
 |
Figure 1 Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) diagram. Notes: Adapted from Moher et al.53 |
Study Characteristics
The details of 18 included trials that were conducted between 2014 and 2019 are presented in Table 1. Among these trials three of the studies were conducted in Republic of Korea33,34 and three studies were from Iran,35–37 whereas the other studies were conducted in different countries like Turkey,38 Lithuania,39 two studies were conducted in India,40,41 Italy,42 Germany43 Egypt,44 Myanmar45 Brazil.46
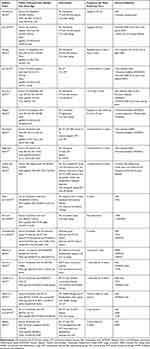 |
Table 1 Summary of Included Randomized Controlled Trials |
A total of 876 patients with knee OA aged from 50 to 77 years old were included in the selected trails. The mean age ranges of the participants were between 51.73 ± (5.1) and 74.76 ± (6.85) in the experimental group34,47 and 50.24 ± (8.63) to 77.2 ± (5.49) in the control group.34,48 The follow-up duration of the intervention ranged from 3 days to 3 months for both experimental and control groups with outcome measures of VAS, WOMAC, and ROM.
Risk of Bias Within Individual Studies
The risk of bias within individual studies and the decisions of each item for the included trials are shown in Table 2. Among the included trials, PEDro score ranges from 5 to 9; with a mean score of 7, which is indicating high quality. Only two trials have blind therapist38,48 and baseline similarity, intention-to-treat analysis, between-group control, point measures of the participants were not stated in two trials.5,34 The sample size of the included trails varied from 30 to 187 participants. Based on the quality of the evidence and the strength of recommendations GRADE approach and PEDro score, the overall quality of the trails was ranged from moderate to high (Table 2).
 |
Table 2 Quality Assessment of Controlled Intervention Studies |
Interventions
Trials comparing the effectiveness of KT and comparison/control group: sham/placebo taping, mobilization with movement, phonophoresis, and/or conventional physiotherapy and/or sham taping with NSAID therapy intervention were included. The conventional interventions/physiotherapy in the studies ranged from other formal taping methods, exercise, manual techniques, analgesics, heat/cold packs, and phonophoresis. The application procedure and the regimen of taping applications (duration, frequency of re-taping) were used to characterize the interventions.
Outcome Measures
Data were extracted for the following outcomes: pain intensity, disability, physical function, and range of motion. All 10 trials used the Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) to measure the Functional Disability status of subjects with knee OA. Only one trial used Knee injury and Osteoarthritis Outcome Scores (KOOS) to measure the physical function of the participants.39 Pain intensity was measured using the visual Analogue Scale (VAS) in 13 trials (Table 1).
Effectiveness of KT on Pain Reduction
Information extracted from the articles were summarized and presented in Table 1. Out of 18 trails, 16 of them (n= 798) reported that the number of participants with knee OA who claimed; knee pain was significantly improved in the KT groups compared to the control group.33–36,39,40,42,43,45,47,48 However, only two studies (n=81) reported the KT group had no improvement of knee pain compared to that of the control groups.38,44 A total of 13 studies (n=136) assessed knee pain intensity by using VAS33,35,36,40,42,45,48 and four studies assessed pain intensity by using the Numeric Pain Rating Scale (NPRS).34,39,41,47
Effectiveness of KT on Knee Joint ROM
Out of the included trails, seven of them (n=422) had assed ROM. From these, five studies (n= 306) reported that KT has beneficial effects on joint mobility for OA patients compared to the control groups.35,36,41,43,45 From those, two of the studies (n=69 knee joint mobility was assessed by pain-free passive ROM using an electronic digital goniometer,41,43 and two studies (n=177) were assessed by pain-free active ROM.33,43 However, there were two studies (n=116) the KT group had no improvement of knee ROM compared to that of the other intervention groups.44,46
Effectiveness KT on Functional Status
From the total included trails, 10 studies (n=685) had assessed functional status. Nine of them (n=609) had reported that KT has beneficial effects on functional activities in OA patients compared to the control groups.34,35,39,41–43,45,47 Only one study (n=76) showed that KT had no significant effect on knee-related physical function in patients with knee osteoarthritis.46
Discussion
This systematic review synthesized the effectiveness of KT in subjects with knee OA. To the extent of the author’s knowledge, there was lack of a systematic review of recently published trials on the efficacy of KT in subjects with knee OA. In this systematic review, large numbers of recent trials were included. Most of the included trials with moderate to high quality of evidence reported that KT was effective for knee osteoarthritis. The overall effect of KT on knee OA was evaluated for different durations of intervention with heterogonous outcome measures.
Even though KT was effective for the management of knee OA from most included trials, but there were few studies that did not report its beneficial effect for Knee OA.44,46 For instance, the study done by Wageck et al46 reported that KT had no beneficial effects for subjects with knee osteoarthritis on any of the assessed outcomes. The reason for that could possibly be explained by the short time that participants had the KT on (4 days), which may not have been long enough to induce any real benefits in knee osteoarthritis. In contrast, trials done by Rahlf et al43 have already noted an inconsistency with Wageck’s claim that reported KT had beneficial effects on pain relief, reducing joint stiffness and increasing knee function within short time (three consecutive days).
This difference might be due to; Wageck’s study reported that the large dropout rate during the follow-up time, taping technique (using of sham application of KT without tension for the control group) and for participants with bilateral knee osteoarthritis, the most affected side was used. Besides the direct method of measuring pain, two questionnaires that include questions related to pain (Lysholm and WOMAC) were also used, and the score was isolated and analyzed from the pain domain from the WOMAC questionnaire. Kocyigit et al's38 study reported that inconclusive evidence of a beneficial effect of KT over sham taping in knee osteoarthritis. This might be because Lequesne index could not be sensitive enough and responsive measures to document the changes within a short time period and the absence of a control group with no treatment.
Anandkumarr et al40 reported that therapeutic KT is effective in improving isokinetic quadriceps torque, and reducing pain in knee osteoarthritis. However, it is unclear whether the measurements were done with or without the KT on, making it difficult to understand how blinding of assessors was performed and possible benefits of KT might only be supposed while the tape is on. Likewise, Cho et al33 investigated that pain decreased significantly immediately after taping in KT group compared to the sham taping. However, Cho et al performed a single KT application in this study; thus, the long-term effects of KT application are unclear. Similarly, the study done by Dhanakotti et al47 showed that KT improving quadriceps strength and knee functional ability in knee OA participants (p<0.05).
On the contrary, the study done by Sedhom et al44 reported that phonophoresis, using of aescin, diethylamine salicylate gel is more effective than KT application in relieving knee pain in knee osteoarthritis patients. This might be due to drug capillary resistance that inhibits inflammatory phenomena and improves microcirculatory conditions besides; regulating capillary permeability.49 In contradiction to this, the study done by Hayati et al48 suggested that KT as a treatment option for early OA that can be used for pain reduction and reduce demands or at least delay non-steroidal anti-inflammatory drug prescriptions in patients with early OA. This improvement may be related to the pain relief effect of KT and regulation of muscle tone by KT. Besides, Nwe et al’s45 study also showed more significant reduction of pain, ROM, improving function and reduction in analgesics consumption was found in intervention group than control group in patients with OA knee. This inconsistent finding may also contribute from various severity levels of knee OA, although we failed to find the available evidence.
Tripathi and Hande41 found that KT plus conventional exercise group studied in geriatric population showed more significant improvement of pain than conventional exercise group after 3 weeks intervention. The possible mechanism for pain relief by KT may be the stabilizing effect (structural support) of KT is believed to relief pain. In addition, the lifting effect of KT creates additional space between the dermis and the muscle. This additional space is supposed to relieve pressure on the pain receptors located under the skin resulting in pain relief.50 Taken together, these findings suggest that KT is effective in improving pain and joint function in patients with knee OA compared with other forms of treatments.
Limitations
This review had the following limitations: this review was included in only English language articles. Hence, there might be a chance of missing articles published in non-English languages. The heterogeneity across the studies for the entire reported outcomes in post intervention and beyond the intervention periods was not estimated by pooled analysis. Studies with short treatment duration were included because longer treatment could likely result in a significant intergroup difference. Sham taping design of the included studies is somewhat inadequate. Taping in the same way as therapeutic banding but with a non-therapeutic material would fit better with the definition of ideal sham taping.
Clinical Implication
This review suggests that KT appears to result in improved outcomes for pain, and functional disability. Clinical decision-making shall be based on the accessibility of KT, especially in a resource-limited setting.
Conclusion
KT was found to improve pain and physical functioning of subjects with knee osteoarthritis. Although this systematic review found that KT is effective in improving muscular strength compared to other interventions, the psychological benefit and supporting effects of stability to knee joint, which were not considered in this review, may constitute further benefits of taping. Moreover, great attention is needed when we use KT for knee osteoarthritis subjects as the course of disease duration and severity.
Ethical Approval
Ethical approval or patient consent was not required since the present study was a review of previously published literature.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Ofluoglu D, Ofluoglu O. Assessment of disease activity and progression of osteoarthritis with using molecular markers of cartilage and synovium turnover. Curr Rheumatol Rev. 2005;1(1):29–32. doi:10.2174/1573397052954181
2. Johnson VL, Hunter DJ. The epidemiology of osteoarthritis. Best Pract Res Clin Rheumatol. 2014;28(1):5–15. doi:10.1016/j.berh.2014.01.004
3. Litwic A, Edwards MH, Dennison EM, Cooper C. Epidemiology and burden of osteoarthritis. Br Med Bull. 2013;105(1):185–199. doi:10.1093/bmb/lds038
4. Woolf AD, Pfleger B. Burden of major musculoskeletal conditions. Bull World Health Organ. 2003;81:646–656.
5. Mathers DSC, Pfleger B. Global Burden of Osteoarthritis in the Year 2000. World Health Organization; 2003. Available from: www. who. int/healthinfo/statistics/bod osteoarthritis. pdf. Accessed April 13, 2020.
6. Eastmond C, Hudson A, Wright V. A radiological survey of the hips and knees in female specialist teachers of physical education. Scand J Rheumatol. 1979;8(4):264–268. doi:10.3109/03009747909114633
7. Marks R. knee osteoarthritis and its psychological complications: consequences, and intervention.
8. Dieppe P. Osteoarthritis: clinical and research perspective. Br J Rheumatol. 1991;30:1.
9. Skou ST, Wrigley TV, Metcalf BR, et al. Association of knee confidence with pain, knee instability, muscle strength, and dynamic varus–valgus joint motion in knee osteoarthritis. Arthritis Care Res (Hoboken). 2014;66(5):695–701. doi:10.1002/acr.22208
10. Colbert CJ, Song J, Dunlop D, et al. Knee confidence as it relates to physical function outcome in persons with or at high risk of knee osteoarthritis in the osteoarthritis initiative. Arthritis Rheum. 2012;64(5):1437–1446. doi:10.1002/art.33505
11. Sharma L, Chmiel JS, Almagor O, et al. Knee instability and basic and advanced function decline in knee osteoarthritis. Arthritis Care Res (Hoboken). 2015;67(8):1095–1102. doi:10.1002/acr.22572
12. Knoop J, van der Leeden M, van der Esch M, et al. Association of lower muscle strength with self‐reported knee instability in osteoarthritis of the knee: results from the amsterdam osteoarthritis cohort. Arthritis Care Res (Hoboken). 2012;64(1):38–45. doi:10.1002/acr.20597
13. Zhang W, Moskowitz RW, Nuki G, et al. OARSI recommendations for the management of hip and knee osteoarthritis, part II: OARSI evidence-based, expert consensus guidelines. Osteoarthr Cartil. 2008;16(2):137–162. doi:10.1016/j.joca.2007.12.013
14. Zhang W, Nuki G, Moskowitz RW, et al. OARSI recommendations for the management of hip and knee osteoarthritis: part III: changes in evidence following systematic cumulative update of research published through January 2009. Osteoarthr Cartil. 2010;18(4):476–499. doi:10.1016/j.joca.2010.01.013
15. Brown GA. AAOS clinical practice guideline: treatment of osteoarthritis of the knee: evidence-based guideline. J Am Acad Orthop Surg Glob Res Rev. 2013;21(9):577–579.
16. Bannuru RR, Schmid CH, Kent DM, et al. Comparative effectiveness of pharmacologic interventions for knee osteoarthritis: a systematic review and network meta-analysis. Ann Intern Med. 2015;162(1):46–54. doi:10.7326/M14-1231
17. Hochberg M, Altman RD, April KT, et al. American college of rheumatology. American College of Rheumatology 2012 recommendations for the use of nonpharmacologic and pharmacologic therapies in osteoarthritis of the hand, hip, and knee. Arthritis Care Res (Hoboken). 2012;64(4):465–474. doi:10.1002/acr.21596
18. Kalron A, Bar-Sela S. A systematic review of the effectiveness of kinesio taping–fact or fashion. Eur J Phys Rehabil Med. 2013;49(5):699–709.
19. Mostafavifar M, Wertz J, Borchers J. A systematic review of the effectiveness of kinesio taping for musculoskeletal injury. Phys Sportsmed. 2012;40(4):33–40. doi:10.3810/psm.2012.11.1986
20. Campolo M, Babu J, Dmochowska K, Scariah S, Varughese J. A comparison of two taping techniques (kinesio and mcconnell) and their effect on anterior knee pain during functional activities. Int J Sports Phys Ther. 2013;8(2):105.
21. Kase K, Wallis J, Kase T, editors. Clinical Therapeutic Applications of the Kinesio Taping Method.3rd edition. Tokyo: Ken Clin Co., Ltd; 2003.
22. Thelen MD, Dauber JA, Stoneman PD. The clinical efficacy of kinesio tape for shoulder pain: a randomized, double-blinded, clinical trial. J Orthop Sports Phys Ther. 2008;38(7):389–395. doi:10.2519/jospt.2008.2791
23. Morris D, Jones D, Ryan H, et al. The clinical effects of Kinesio® Tex taping: a systematic review. Physiother Theory Pract. 2013;29(4):259–270. doi:10.3109/09593985.2012.731675
24. Abolhasani M, Halabchi F, Afsharnia E, et al. Effects of kinesiotaping on knee osteoarthritis: a literature review. J Exercise Rehabil. 2019;15(4):498. doi:10.12965/jer.1938364.182
25. Parreira PDCS, Costa LDCM, Hespanhol Junior LC, et al. Current evidence does not support the use of Kinesio Taping in clinical practice: a systematic review. J Physiother. 2014;60(1):31–39. doi:10.1016/j.jphys.2013.12.008
26. Lim ECW, Tay MGX. Kinesio taping in musculoskeletal pain and disability that lasts for more than 4 weeks: is it time to peel off the tape and throw it out with the sweat? A systematic review with meta-analysis focused on pain and also methods of tape application. Br J Sports Med. 2015;49(24):1558–1566. doi:10.1136/bjsports-2014-094151
27. Ellis RF. The use and treatment efficacy of kinaesthetic taping for musculoskeletal conditions: a systematic review. NZ J Physiother. 2010;38(2):56.
28. Montalvo AM, Cara EL, Myer GD. Effect of kinesiology taping on pain in individuals with musculoskeletal injuries: systematic review and meta-analysis. Phys Sportsmed. 2014;42(2):48–57. doi:10.3810/psm.2014.05.2057
29. Moher D, Shamseer L, Clarke M, et al. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev. 2015;4(1):1. doi:10.1186/2046-4053-4-1
30. de Morton NA. The PEDro scale is a valid measure of the methodological quality of clinical trials: a demographic study. Aust J Physiother. 2009;55(2):129–133. doi:10.1016/S0004-9514(09)70043-1
31. Maher CG, Sherrington C, Herbert RD, et al. Reliability of the PEDro scale for rating quality of randomized controlled trials. Phys Ther. 2003;83(8):713–721. doi:10.1093/ptj/83.8.713
32. Guyatt GH, Oxman AD, Kunz R, et al. GRADE guidelines: 7. Rating the quality of evidence—inconsistency. J Clin Epidemiol. 2011;64(12):1294–1302. doi:10.1016/j.jclinepi.2011.03.017
33. Cho H, Kim EH, Kim J, et al. Kinesio taping improves pain, range of motion, and proprioception in older patients with knee osteoarthritis: a randomized controlled trial. Am J Phy Med Rehabil. 2015;94(3):192–200. doi:10.1097/PHM.0000000000000148
34. Park KN, Kim SH. Effects of knee taping during functional activities in older people with knee osteoarthritis: a randomized controlled clinical trial. Geriatr Gerontol Int. 2018;18(8):1206–1210. doi:10.1111/ggi.13448
35. Lee K, Yi C-W, Lee S. The effects of kinesiology taping therapy on degenerative knee arthritis patients’ pain, function, and joint range of motion. J Phys Ther Sci. 2016;28(1):63–66. doi:10.1589/jpts.28.63
36. Taheri P, Vahdatpour B, Asl MM, Ramezanian H. Effects of taping on pain and functional outcome of patients with knee osteoarthritis: a pilot randomized single-blind clinical trial. Adv Biomed Res. 2017;6.
37. Abolhasani M, Halabchi F, Honarpishe R, et al. Effects of kinesiotape on pain, range of motion, and functional status in patients with osteoarthritis: a randomized controlled trial. J Exercise Rehabil. 2019;15(4):603. doi:10.12965/jer.1938290.145
38. Kocyigit F, Turkmen MB, Acar M, et al. Kinesio taping or sham taping in knee osteoarthritis? A randomized, double-blind, sham-controlled trial. Complement Ther Clin Pract. 2015;21(4):262–267. doi:10.1016/j.ctcp.2015.10.001
39. Donec V, Kubilius R. The effectiveness of Kinesio Taping® for pain management in knee osteoarthritis: a randomized, double-blind, controlled clinical trial. Ther Adv Musculoskelet Dis. 2019;11:1759720X19869135. doi:10.1177/1759720X19869135
40. Anandkumar S, Sudarshan S, Nagpal P. Efficacy of kinesio taping on isokinetic quadriceps torque in knee osteoarthritis: a double blinded randomized controlled study. Physiother Theory Pract. 2014;30(6):375–383. doi:10.3109/09593985.2014.896963
41. Tripathi B, Hande D. Effects of kinesiotaping on osteoarthritis of knee in geriatric population. IJAR. 2017;3(2):301–305.
42. Castrogiovanni P, Di Giunta A, Guglielmino C, et al. The effects of exercise and kinesio tape on physical limitations in patients with knee osteoarthritis. J Funct Morphol Kinesiol. 2016;1(4):355–368. doi:10.3390/jfmk1040355
43. Rahlf AL, Braumann K-M, Zech A. Kinesio taping improves perceptions of pain and function of patients with knee osteoarthritis: a randomized, controlled trial. J Sport Rehabil. 2018;1–7.
44. Sedhom MG. Efficacy of kinesio-taping versus phonophoresis on knee osteoarthritis: an experimental study. Int j Physiother. 2016;3(4):494–499. doi:10.15621/ijphy/2016/v3i4/111062
45. Nwe AA, Tun MT, Aung ST, et al. Effectiveness of Kinesio taping in the management of knee osteoarthritis. J Adv Med Med Res;2019. 1–10. doi:10.9734/jammr/2019/v29i230063
46. Wageck B, Nunes GS, Bohlen NB, et al. Kinesio Taping does not improve the symptoms or function of older people with knee osteoarthritis: a randomised trial. J Physiother. 2016;62(3):153–158. doi:10.1016/j.jphys.2016.05.012
47. Dhanakotti S, Samuel RK, Thakar M, Doshi S, Vadsola K. Effects of additional kinesiotaping over the conventional physiotherapy exercise on pain, quadriceps strength and knee functional disability in knee osteoarthritis participants: a randomized controlled study. IJHSR. 2016;6(1):221–229.
48. Hayati M, Yazdi Z, Abbasi M. Comparison of non-steroidal anti-inflammatory drugs and knee kinesio taping in early osteoarthritis pain: a randomized controlled trial. J Bodyw Mov Ther. 2019;23(3):666–670. doi:10.1016/j.jbmt.2018.06.011
49. Kaya ME, Mustafaoglu R, Birinci T, Razak OA. Does Kinesio taping of the knee improve pain and functionality in patients with knee osteoarthritis?: a randomized controlled clinical trial. Am J Phys Med Rehabil. 2016;96(1):25–33.
50. Anandkumar S, Sudarshan S, Nagpal P. Efficacy of kinesio taping on isokinetic quadriceps torque in knee osteoarthritis: a double blinded randomized controlled study. Physiother Theor Pr. 2014;30(6):375–83.
51. Zhang, L.-M., et al, et al. Escin may exert a synergistic anti-inflammatory effect with glucocorticoids. Health. 2010;2(2):79. doi:10.4236/health.2010.220137
52. Gramatikova, M., E. Nikolova, and S. Mitova, Nature, application and effect of kinesio-taping. Activities in Physical Education and Sport. 2014;4(2):115–119.
53. Moher D, liberati A., tetzlaff J., et al. prefered prisma reporting item for systematic review and metaanalysis :the PRISMA statement. plos mea.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
