Back to Journals » Neuropsychiatric Disease and Treatment » Volume 13
Effect of aripiprazole on non-24-hour sleep–wake rhythm disorder comorbid with major depressive disorder: a case report
Authors Matsui K, Takaesu Y, Inoue T , Inada K , Nishimura K
Received 9 March 2017
Accepted for publication 10 April 2017
Published 19 May 2017 Volume 2017:13 Pages 1367—1371
DOI https://doi.org/10.2147/NDT.S136628
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Taro Kishi
Kentaro Matsui,1,2 Yoshikazu Takaesu,2,3 Takeshi Inoue,3 Ken Inada,1 Katsuji Nishimura1
1Department of Psychiatry, Tokyo Women’s Medical University, 2Japan Somnology Center, Neuropsychiatric Research Institute, 3Department of Psychiatry, Tokyo Medical University, Tokyo, Japan
Background: Patients with non-24-hour sleep–wake rhythm disorder (N24SWD) exhibit a sleep pattern that is asynchronous with the external light–dark cycle, typically involving a cycling, relapsing–remitting pattern of sleep disturbances, including nighttime insomnia and daytime sleepiness. Here, we report the case of a patient with N24SWD comorbid with major depressive disorder, who was successfully treated with a low dose of aripiprazole.
Case presentation: A 47-year-old female presented with an 8-year complaint of difficulty falling asleep and waking up in the morning. The patient was diagnosed with major depressive disorder at the age of 35 years and was treated with various antidepressants since that time. At the age of 40 years, the patient’s sleep–wake cycle began to extend without exacerbation of depressive symptoms. The patient was diagnosed with N24SWD at the age of 43 years. Ramelteon 8 mg/d and then melatonin 1 mg/d were administered, but these did not provide effective treatment. In January 2016, after treatment with aripiprazole 3 mg/d in the morning for 4 weeks, the patient’s sleep–wake cycle became markedly synchronized to the environmental light–dark cycle. Her sleep–wake cycle remained synchronized when the same dose of aripiprazole was administered for at least 6 months.
Conclusion: Treatment-refractory asynchrony of the sleep–wake cycle in an N24SWD patient with depression was successfully treated with aripiprazole. Although the detailed mechanism of action is unclear, aripiprazole may be an appropriate treatment for patients with circadian rhythm sleep–wake disorders.
Keywords: circadian rhythm sleep–wake disorder, non-24-hour sleep–wake rhythm disorder, melatonin, long sleep duration, antipsychotic
Introduction
Non-24-hour sleep–wake rhythm disorder (N24SWD) is a circadian rhythm sleep–wake disorder (CRSWD) characterized by an inability of the endogenous circadian rhythm to be entrained to the external light–dark cycle. N24SWD patients typically exhibit an intrinsic rhythm longer than 24 h, and a cycling, relapsing–remitting pattern of sleep disturbances, including nighttime insomnia and daytime sleepiness, arising from internal desynchronization.1,2 Interestingly, previous studies reported that mood disorders, including major depressive disorder (MDD) and bipolar disorder, are highly comorbid in reported N24SWD patients.2,3 These findings suggest that certain pathophysiological relationships may exist between mood disorders and N24SWD.4 However, no reports have described effective treatment strategies for mood disorders with CRSWDs.
Aripiprazole is a second-generation antipsychotic (SGA) with the unique profile of a dopamine partial agonist. Regarding the efficacy of aripiprazole for CRSWD comorbid with mood disorder, only one delayed sleep–wake phase disorder (DSWPD) case with MDD5 and one complex CRSWD case with bipolar disorder6 have been reported, with both reports suggesting a phase-modulating effect of aripiprazole. DSWPD is another CRSWD, defined by an abnormally late sleep period compared with conventional or socially desirable times. DSWPD has an onset mechanism similar to that of N24SWD, and some patients progress from DSWPD to N24SWD.2 In the current study, we report a case of a sighted N24SWD patient with MDD whose sleep–wake cycle was markedly improved with aripiprazole.
Case
Written informed consent was obtained from the patient for the publication of this case and accompanying images.
A 47-year-old female presented with an 8-year complaint of difficulty falling asleep and waking up in the morning. The patient was consequently unable to maintain stable entrainment to a 24-h sleep–wake pattern. She visited our hospital (Tokyo Women’s Medical University Hospital) for the first time in August 2004 and was diagnosed with MDD according to Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (DSM-IV-TR) criteria,7 exhibiting depressed mood, markedly diminished interest, and loss of energy. The patient had no history of problems with the use of alcohol and other substances. Pharmacological treatment with antidepressants, including paroxetine, milnacipran, fluvoxamine, and duloxetine, was administered alternately. However, her depressive symptoms showed repeated exacerbation, and she was unable to work regularly. After a 3-month period of hospitalization for depression in 2007, the patient stopped working and exhibited social withdrawal. The patient exhibited depression with moderate severity, as indicated by a Clinical Global Impression-Severity scale (CGI-S)8 score of 4.0. The moderate depressive state continued from that time.
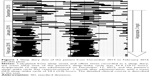
At the age of 40 years (in 2009), the patient’s sleep–wake cycle began to extend, independently of changes in depressive symptoms. In December 2014, she was diagnosed with N24SWD using the International Classification of Sleep Disorders, Third Edition (ICSD-3).9 At that time, she was taking 40 mg/d of duloxetine (in the morning), but no other antidepressants or sedatives/hypnotics. Ramelteon 8 mg/d (at 7 PM) was administered, and sleep hygiene education was provided, but these treatments did not positively affect circadian dysregulation. In June 2015, the patient began taking melatonin 1 mg/d (at 7 PM), but this treatment also had no effect. Calculated from sleep onset and offset time using sleep diary data between September 2014 and November 2015, the mean (standard deviation [SD]) time of the patient’s sleep, awake, and sleep–wake cycle were 12.9 (5.2), 20.5 (7.3), and 33.4 (10.2) h, respectively. In December 2015, aripiprazole 3 mg/d (after morning meal) was administered, primarily to improve the loss of energy. After treatment for 4 weeks (in the middle of January 2016), the patient’s sleep–wake cycle had become markedly synchronized to the environmental light–dark cycle. Subsequently, the patient fell asleep between 12 midnight and 3 AM and awoke between 8 AM and 11 AM (Figure 1), similar to her sleep–wake pattern before she was diagnosed with N24SWD. Although the patient’s depressive symptoms, including loss of energy, were not improved by treatment with aripiprazole (a CGI-S score of 4.0), her sleep–wake cycle remained synchronized on the same dose of aripiprazole for at least 6 months, and the mean (SD) time of the patient’s sleep, awake and sleep–wake cycle were 9.9 (2.1), 14.3 (2.7) and 24.2 (3.0) h, respectively (calculated using sleep diary data between February 2016 and July 2016).
Discussion
To our knowledge, this is the first case report showing an effect of aripiprazole on N24SWD comorbid with MDD. In this case, depression preceded the onset of N24SWD. Thus, the patient’s social withdrawal as a result of depressive symptoms may have affected the development of N24SWD. In addition, the use of antidepressants may also have altered sleep architecture and/or phase shift. However, the patient’s prolonged sleep–wake cycle lasted for >6 years, independently of the severity of depressive symptoms or differences in antidepressants used. Moreover, the patient’s social withdrawal did not improve after the administration of aripiprazole. Additionally, it should be noted that the patient’s depressive symptoms did not show any significant improvement, in contrast to the drastic change in sleep–wake cycle. Therefore, it is unlikely that an augmentation effect of aripiprazole on depression indirectly improved N24SWD. Rather, our findings suggest that aripiprazole may have directly affected the internal circadian rhythm.
Therapeutic interventions for N24SWD should be targeted at entraining the patient’s circadian pacemaker at an appropriate phase relative to the environmental light–dark cycle. Morning light therapy has been used in a number of cases with N24SWD.10–13 As a pharmacological treatment, melatonin, which can induce phase shifts of the human circadian pacemaker, has been used in patients with N24SWD. Melatonin therapy has been reported to be efficacious for patients with N24SWD in open-label studies.13–15 The melatonin receptor agonist ramelteon is an alternative treatment option. Regarding the efficacy of ramelteon for N24SWD, a small case series with two patients has been previously reported.16 It is unclear why melatonin and its synthetic agonist did not improve the sleep–wake cycle in the current case. One possibility is that melatonin and ramelteon may not have been administered at the most appropriate time of day. In the current study, we did not measure melatonin to evaluate dim-light melatonin onset, or deep body temperature, which could have indicated more appropriate timing for taking melatonin or ramelteon. However, unlike idiopathic CRSWD, CRSWD comorbid with mood disorders may require a specialized treatment approach that includes the use of lithium17 or aripiprazole.
Understanding the mechanisms underlying the effect of aripiprazole on the modulation of the sleep–wake rhythm is a clinically important issue. In recent years, as a circadian rhythm adjustment factor other than melatonin, several studies have suggested that dopamine and serotonin regulate the circadian rhythm by coordinating with melatonin secretion.18–23 Aripiprazole, a partial agonist of dopamine and serotonin, can modulate both dopamine and serotonin through D2 and 5-hydroxytryptamine (5-HT)-1A receptors when used at low doses.24,25 In addition, aripiprazole can secondarily increase hypothalamic histamine release, which can promote wakefulness.26 Furthermore, treatment with aripiprazole has been reported to increase the level of GSK-3β phosphorylation.27 Through the inhibition of GSK-3β, aripiprazole can promote proteasome-mediated degradation of Rev-erbα and inhibit the transcription of the clock gene Bmal1, which has the potential to shorten the sleep–wake cycle.28 It remains unclear whether aripiprazole contributes to a decrease in sleep duration. It would be useful to ascertain whether aripiprazole is effective for non-CRSWD patients exhibiting difficulty waking up, long sleep duration, or excessive daytime sleepiness. Further research with a larger number of cases will be needed to clarify the effects of aripiprazole on N24SWD.
Conclusion
Treatment-refractory asynchrony of the sleep–wake cycle in a N24SWD patient with depression was successfully treated with aripiprazole. Severe CRSWD is relatively common, particularly among patients with mood disorders in clinical situations. Therefore, early detection and appropriate intervention should be encouraged. The current study suggests that aripiprazole may be an appropriate treatment choice for patients with CRSWDs. However, further research will be needed to confirm these preliminary findings.
Disclosure
Kentaro Matsui has received speaker’s honoraria from Merck Sharp & Dohme (MSD), Otsuka Pharmaceutical, Meiji Seika Pharma, Eisai, and Yoshitomi Pharmaceutical and has received research funding from Eisai. Yoshikazu Takaesu has received speaker’s honoraria from Otsuka Pharmaceutical, Meiji Seika Pharma, Eli Lilly, Eisai, Mitsubishi Tanabe Pharma, and Yoshitomi Pharmaceutical, as well as research funding from Otsuka Pharmaceutical, Meiji Seika Pharma, and Eisai. Takeshi Inoue has received speaker’s honoraria from GlaxoSmithKline, Pfizer, Eli Lilly, Mitsubishi Tanabe Pharma, Mochida Pharmaceutical, Otsuka Pharmaceutical, Meiji Seika Pharma, Asahi Kasei Pharma, Shionogi, Dainippon Sumitomo Pharma, Takeda Pharmaceutical, MSD, Eisai, AbbVie GK, and Yoshitomi Pharmaceutical; he has received research/grant support from Otsuka Pharmaceutical, Eli Lilly, Eisai, Mitsubishi Tanabe Pharma, Yoshitomi Pharmaceutical AbbVie GK, Pfizer, Astellas, MSD, and Meiji Seika Pharma; he is a member of the advisory boards of GlaxoSmithKline, Pfizer, Eli Lilly, Mochida Pharmaceutical, and Mitsubishi Tanabe Pharma. Ken Inada has received speaker’s honoraria from Dainippon Sumitomo Pharma, Eisai, Eli Lilly, GlaxoSmithKline, Janssen Pharmaceutical, Meiji Seika Pharma, Mitsubishi Tanabe Pharma, Mochida Pharmaceutical, MSD, Novartis, Otsuka Pharmaceutical, Pfizer, Shionogi, Takeda Pharmaceutical, and Yoshitomi Pharmaceutical. Katsuji Nishimura has received speaker’s honoraria from Meiji Seika Pharma, Mochida Pharmaceutical, Takeda Pharmaceutical, Eli Lilly, MSD, Shionogi, Janssen Pharmaceutical, Eisai, Otsuka Pharmaceutical, Novartis, Mitsubishi Tanabe Pharma, and Chugai Pharmaceutical; he has received research/grant support from Mochida Pharmaceutical, Takeda Pharmaceutical, Otsuka Pharmaceutical, Novartis, Mitsubishi Tanabe Pharma, Dainippon Sumitomo Pharma, MSD, Eisai, Tsumura, and Mebix. The authors report no other conflicts of interest in this work.
References
Uchiyama M, Lockley SW. Non–24-hour sleep–wake syndrome in sighted and blind patients. Sleep Med Clin. 2009;4(2):195–211. | ||
Hayakawa T, Uchiyama M, Kamei Y, et al. Clinical analyses of sighted patients with non-24-hour sleep-wake syndrome: a study of 57 consecutively diagnosed cases. Sleep. 2005;28(8):945–952. | ||
Takaesu Y, Inoue Y, Murakoshi A, et al. Prevalence of circadian rhythm sleep-wake disorders and associated factors in euthymic patients with bipolar disorder. PLoS One. 2016;11(7):e0159578. | ||
Pinho M, Sehmbi M, Cudney LE, et al. The association between biological rhythms, depression, and functioning in bipolar disorder: a large multi-center study. Acta Psychiatr Scand. Epub 2015 May 22. | ||
Takaki M, Ujike H. Aripiprazole is effective for treatment of delayed sleep phase syndrome. Clin Neuropharmacol. 2014;37(4):123–124. | ||
Tashiro T. Improvement of a patient’s circadian rhythm sleep disorders by aripiprazole was associated with stabilization of his bipolar illness. J Sleep Res. 2017;26(2):247–250. | ||
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (DSM-IV-TR). Washington: American Psychiatric Association; 2000. | ||
Guy W. ECDEU Assessment Manual for Psychopharmacology. Vol. 76. Kensington: US Department of Health, Education, and Welfare, Public Health Service, Alcohol, Drug Abuse, and Mental Health Administration, National Institute of Mental Health, Psychopharmacology Research Branch, Division of Extramural Research Programs; 1976. | ||
American Academy of Sleep Medicine. International Classification of Sleep Disorders – Third Edition (ICSD-3). Darien, IL: American Academy of Sleep Medicine; 2014. | ||
Wollman M, Lavie P. Hypernychthemeral sleep-wake cycle: some hidden regularities. Sleep. 1986;9(2):324–334. | ||
Sugita Y, Ishikawa H, Mikami A. Successful treatment for a patient with hypernychthemeral syndrome. Sleep Res. 1987;16:642. | ||
Watanabe T, Kajimura N, Kato M, Sekimoto M, Hori T, Takahashi K. Case of a non-24 h sleep–wake syndrome patient improved by phototherapy. Psychiatry Clin Neurosci. 2000;54(3):369–370. | ||
Hayakawa T, Kamei Y, Urata J, et al. Trials of bright light exposure and melatonin administration in a patient with non-24 hour sleep-wake syndrome. Psychiatry Clin Neurosci. 1998;52(2):261–262. | ||
McArthur AJ, Lewy AJ, Sack RL. Non-24-hour sleep-wake syndrome in a sighted man: circadian rhythm studies and efficacy of melatonin treatment. Sleep. 1996;19(7):544–553. | ||
Kamei Y, Hayakawa T, Urata J, et al. Melatonin treatment for circadian rhythm sleep disorders. Psychiatry Clin Neurosci. 2000;54(3):381–382. | ||
Yanagihara M, Nakamura M, Usui A, et al. The melatonin receptor agonist is effective for free-running type circadian rhythm sleep disorder: case report on two sighted patients. Tohoku J Exp Med. 2014;234(2):123–128. | ||
Yin L, Joshi S, Wu N, Tong X, Lazar MA. E3 ligases Arf-bp1 and Pam mediate lithium-stimulated degradation of the circadian heme receptor Rev-erbα. Proc Natl Acad Sci U S A. 2010;107(25):11614–11619. | ||
Fifel K, Cooper HM. Loss of dopamine disrupts circadian rhythms in a mouse model of Parkinson’s disease. Neurobiol Dis. 2014;71:359–369. | ||
Garmabi B, Vousooghi N, Vosough M, Yoonessi A, Bakhtazad A, Zarrindast MR. Effect of circadian rhythm disturbance on morphine preference and addiction in male rats: involvement of period genes and dopamine D1 receptor. Neuroscience. 2016;322:104–114. | ||
Gallardo CM, Darvas M, Oviatt M, et al. Dopamine receptor 1 neurons in the dorsal striatum regulate food anticipatory circadian activity rhythms in mice. Elife. 2014;3:e03781. | ||
Domínguez-López S, Howell RD, López-Canúl MG, Leyton M, Gobbi G. Electrophysiological characterization of dopamine neuronal activity in the ventral tegmental area across the light–dark cycle. Synapse. 2014;68(10):454–467. | ||
Nakamaru-Ogiso E, Miyamoto H, Hamada K, Tsukada K, Takai K. Novel biochemical manipulation of brain serotonin reveals a role of serotonin in the circadian rhythm of sleep–wake cycles. Eur J Neurosci. 2012;35(11):1762–1770. | ||
Sprouse J, Li X, Stock J, McNeish J, Reynolds L. Circadian rhythm phenotype of 5-HT7 receptor knockout mice: 5-HT and 8-OH-DPAT-induced phase advances of SCN neuronal firing. J Biol Rhythms. 2005;20(2):122–131. | ||
Burris KD, Molski TF, Xu C, et al. Aripiprazole, a novel antipsychotic, is a high-affinity partial agonist at human dopamine D2 receptors. J Pharmacol Exp Ther. 2002;302(1):381–389. | ||
Jordan S, Koprivica V, Chen R, Tottori K, Kikuchi T, Altar CA. The antipsychotic aripiprazole is a potent, partial agonist at the human 5-HT 1A receptor. Eur J Pharmacol. 2002;441(3):137–140. | ||
Murotani T, Ishizuka T, Isogawa Y, Karashima M, Yamatodani A. Possible involvement of serotonin 5-HT2 receptor in the regulation of feeding behavior through the histaminergic system. Neuropharmacology. 2011;61(1):228–233. | ||
Park SW, Lee JG, Ha EK, et al. Differential effects of aripiprazole and haloperidol on BDNF-mediated signal changes in SH-SY5Y cells. Eur Neuropsychopharmacol. 2009;19(5):356–362. | ||
Hirota T, Lewis WG, Liu AC, Lee JW, Schultz PG, Kay SA. A chemical biology approach reveals period shortening of the mammalian circadian clock by specific inhibition of GSK-3beta. Proc Natl Acad Sci U S A. 2008;105(52):20746–20751. |
 © 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.