Back to Journals » Cancer Management and Research » Volume 12
Current Therapeutic Progress of CDK4/6 Inhibitors in Breast Cancer
Authors Wu Y, Zhang Y, Pi H, Sheng Y
Received 20 February 2020
Accepted for publication 16 April 2020
Published 15 May 2020 Volume 2020:12 Pages 3477—3487
DOI https://doi.org/10.2147/CMAR.S250632
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Chien-Feng Li
Yanmei Wu,1 Yu Zhang,2 Hao Pi,1 Yuan Sheng1
1Department of Breast and Thyroid Surgery, Changhai Hospital, Navy Medical University, Shanghai 200433, People’s Republic of China; 2Medical Affairs, Pfizer Biopharmaceutical Group, Shanghai 200041, People’s Republic of China
Correspondence: Yuan Sheng
Department of Breast and Thyroid Surgery, Changhai Hospital, Navy Medical University, Shanghai 200433, People’s Republic of China
Email [email protected]
Abstract: The clinical use of selective cyclin-dependent kinase (CDK) 4/6 inhibitors has significantly improved the prognosis of patients with hormone receptor (HR)-positive human epidermal growth factor receptor 2 (HER2)-negative advanced or metastatic breast cancer (ABC/mBC), which almost achieved the double progression-free survival (PFS) in combination with endocrine therapy (ET) compared with ET alone. To date, there are 3 CDK4/6 inhibitors (palbociclib, ribocilcib and abemaciclib) approved by the US Food and Drug Administration (FDA) and European Medicines Agency (EMA) to treat patients with HR+/HER2-ABC/mBC in the first and later lines. The aim of this review is to summarize the current clinical use and ongoing clinical trials of CDK4/6 inhibitors, the published overall survival data, and the potential biomarkers and resistance to CDK4/6 inhibitors.
Keywords: CDK4/6 inhibitor, breast cancer, mechanism, clinical efficacy, resistance
Introduction
Breast cancer (BC) is a worldwide health problem for women with almost 2.1 million new cases diagnosed and an estimated 0.6 million deaths every year.1 Although the overall 5-year survival has reached to 90%, the 5-year survival rate was only 25% in metastatic or advanced BC (mBC/ABC).2 Of all BC cases, ~ 70% of women were diagnosed as hormone receptor-positive (HR+), human epidermal growth factor receptor two-negative (HER2-) BC.3 Recent innovative therapeutic regimens have revealed that endocrine therapy (ET) plus targeted therapy such as everolimus, has improved the prognosis of ER+/HER2- mBC/ABC.4 Moreover, the combination of ET and cyclin-dependent kinase (CDK) 4/6 inhibitors has also shown significantly clinical benefit.5
In this review, we summarized the recent therapeutic progress of 3 CDK4/6 inhibitors, palbociclib, ribociclib and abemaciclib, which have been approved by US Food and Drug Administration (FDA) and European Medicines Agency (EMA) to treat patients with HR+/HER2- mBC/ABC, including their mechanism of action, approved indications, the published overall survival data, ongoing clinical trials and potential clinical use in future.
Mechanism of Action of CDK4/6 Inhibitors
Cell division is a common cell process under strict control in normal cells in case of unexpected proliferation, which is usually the cause of cancer. There are many pathways involved in regulating cell cycle and CDK family is one of the most important protein families in cell division regulation (Figure 1).6 In G1 phase of cell cycle, CDK4/6 interacts with cyclin D to form the cyclin D-CDK4/6 complex, which phosphorylates retinoblastoma (Rb).7,8 Inactivated Rb is tightly binding to E2F, the transcription factor, and phosphorylation of Rb releases E2F from Rb-E2F complex, followed by inducing upregulation of E2F target genes and initiating DNA synthesis, resulting in cell cycle entry into S phase.8–10 There are several instinct negative regulators of cyclin D-CDK4/6-Rb signaling pathway, which prevent cells from unchecked proliferation, such as the INK4 family of proteins (p16, p15, p18, and p19), cyclin inhibitory proteins (CIPs) and kinase inhibitory proteins (KIPs, p21 and p27).11–13
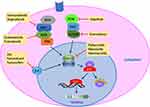 |
Figure 1 Mechanism of CDK4/6 inhibitors and possible combined therapy with CDK4/6 inhibitors. Activation of upstream signaling pathways, such as MAPK, PI3K and ER, promotes the formation of cyclin D-CDK4/6 complex, which phosphorylates Rb protein. With phosphorylation of Rb, E2F is dissociated from Rb-E2F complex.84 As a transcription factor, released E2F initiates DNA synthesis, resulting in cell cycle progressed into S phase from G1 phase. CDK4/6 inhibitors (palbociclib, ribociclib and abemaciclib) prevent the activation of CDK4/6 to cause cell cycle arrest at G1 phase. Combination therapeutic strategies mainly focus on blockade of upstream of cyclin D-CDK4/6 signaling, including blockade of ER by AIs, fulvestrant and tamoxifen, blockade MAPK by BRAF89 inhibitors (vemurafenib and dabrafenib) and MEK inhibitors (cobimetinib and trametinib),90 and blockade of PI3K pathway by alpelisib91 and everolimus.92 Abbreviations: CDK, cyclin-dependent kinase; MAPK, mitogen-activated protein kinase; PI3K, phosphoinositide 3-kinase; ER, estrogen receptor; AI, aromatase inhibitor. |
In breast cancer and other malignancies, dysregulation of cyclin D1-CDK4/6-Rb signaling cascade was observed and promoted unchecked cell proliferation.14,15 Nearly 15% of breast cancers have been detected amplification of the cyclin D2 gene, CCND1, and expression of cyclin D1 at mRNA and protein has been determined to upregulated in up to 50% of primary ER+ breast cancers, and well-differentiated tumors.16,17 In breast cancer cell lines, induction of cyclin D initiate cell cycle process and increase the number of cell processing from G1 to S phase,18 and in vivo study showed that overexpression of cyclin D promoted abnormal mammary cell proliferation and promoting the development of mammary carcinomas in transgenic mice.19 Overexpression of Cyclin D1 is associated with poor prognosis in many cancers and is often associated with increased metastasis.16,20,21 Similarly, overexpression of CDK4 is positively correlated with high proliferative ability of tumor cells in sporadic breast carcinomas.22 Elevated activity of CDK6 was detected in five squamous cell carcinoma lines23 and inhibition of cyclin D3-CDK6 led to tumor cell apoptosis.24 All these evidences indicate that CDK4/6 and cyclin D could be the potential therapeutic targets in cancer.
Current Indications and Dosage of CDK4/6 Inhibitors
So far, three CDK4/6 inhibitors have been approved by both FDA and EMA: palbociclib (Ibrance, Pfizer, USA), ribociclib (Kisqali, Novartis, Switzerland) and abemaciclib (Verzenio, Lilly, USA).
The prescribing information between palbociclib and ribociclib is similar: in combination with an aromatase inhibitor (AI) for the treatment of patients with HR+/HER2-locally ABC/mBC as initial therapy in postmenopausal women or in combination with fulvestrant in women who have previously treated with ET.25,26 In women who have not yet reached menopause, luteinising hormone-releasing hormone agonists should also be given according to EMA approval.27,28 In addition, the indication of palbociclib has been expanded to male patients with HR+/HER2-mBC on the basis of real-world data from electronic health records and insurance claims on April 4, 2019, by FDA.29
The indication of abemaciclib from FDA is different from palbociclib and ribociclib: in combination with fulvestrant to treat women with HR+/HER2- mBC/ABC who have previously treated with ET; As monotherapy for the treatment of adult patients with HR+/HER2- mBC/ABC who have previously treated with ET and prior chemotherapy in the metastatic setting.30 Abemaciclib is the only CDK4/6 inhibitor that can be used as a monotherapeutic drug.
Palbociclib is started with 125 mg/day on a 3/1 schedule (21-day on, 7-day off); If patients were not resistant, the dose should be reduced to 100 mg/day and further reduced to the final dose of 75 mg.25 Ribociclib is also administrated on a 3/1 schedule (21-day on, 7-day off) at a dose of 600 mg/day; Dose reduction is allowed if patients were not resistant with the first dose reduction to 400 mg/day, and the final reduction to 200 mg/day.26 Abemaciclib is primarily prescribed with 200 mg twice daily continuously as a monotherapy. If combined with endocrine treatment, the start dose is 150 mg twice daily continuously. The first dose reduction is 100 mg twice daily, and the final dose is 50 mg twice daily.30 Palbociclib should be taken orally with food because the drug exposure is decreased with an empty stomach, which may reduce effectiveness.31 On the contrary, the absorption and exposure of ribociclib or abemaciclib are not affected by food intake.26,30
Treatment of HR+/HER2- ABC/mBC with CDK4/6 Inhibitors Plus ET
CDK4/6 Inhibitors and AIs in Treatment-Naïve HR+/HER2- ABC/mBC
There are 3 Phase III randomized clinical trials (RCTs) to prove the efficacy and safety of the CDK4/6 inhibitors combined with AIs as the first-line treatment of postmenopausal HR+/HER2- ABC/mBC (Table 1).32 The results are consistent among the 3 CDK4/6 inhibitors.
Palbociclib was granted accelerated approval by FDA33 based just on the Phase II trial PALOMA-1/TRIO-18 results, which demonstrated that a remarkable prolongation in the median progression-free survival (PFS) from 10.2 months with letrozole alone to 20.2 months with palbociclib plus letrozole (hazard ratio [HR], 0.49, p = 0.0004),34 and the median overall survival (OS) was prolonged by 3 months (37.5 months versus [vs] 34.5 months HR = 0.897, p = 0.281).35 Since this accelerated approval is conditional, a phase III RCT termed PALOMA-2 (n = 666) was conducted to validate these promising results.36,37 The final PFS in addition of palbociclib to letrozole was 27.6 months compared to 14.5 months with letrozole alone (HR, 0.563; p < 0.001). The objective response rate (ORR) was 42.1% vs 34.7% (p = 0.06) and the clinical benefit rate (CBR) was significantly improved from 70.3% to 84.9% (p < 0.001).
Similarly, the efficacy of ribociclib and abemaciclib plus AI was confirmed by MONALEESA-2 and MONARCH 3, respectively. MONALEESA-2 is a phase III RCT enrolled 668 postmenopausal women with HR+/HER2-ABC as first-line treatment38,39 with a median follow-up of 26.4 months. The final PFS was 25.3 months with combination of ribociclib with letrozole and 16.0 months with letrozole alone (HR, 0.568; p = 9.63 × 10–8). The ORR (ribociclib plus letrozole vs letrozole alone) was 40.7% vs 27.5 % (p = 9.18 × 10–5) and the CBR is 79.6% vs 72.8 %. The aim of MONARCH 3 is to validate the clinical effectiveness and safety of abemaciclib plus a nonsteroidal AI in 493 postmenopausal women with previously untreated HR+/HER2-ABC.40,41 Both ORR (48.2% vs 34.5%. p = 0.02) and PFS (28.2 vs 14.8 months; HR 0.54; p = 0.000002) were significantly improved in the combination arm compared with placebo control.
In summary, as the initial treatment of postmenopausal BC patients, the efficacy was similar among the 3 CDK4/6 inhibitors, and the prolonged PFS was more than one year in palbociclib/abemaciclib + AIs while there was only 9-month prolongation of PFS with ribociclib + letrozole. The OS data were highly expected to achieve the significant benefit in combination treatment group.
CDK4/6 Inhibitors Plus Fulvestrant in Previously ET Treated mBC/ABC
PALOMA-3 was a phase III RCT study to investigate palbociclib plus fulvestrant in pre- or postmenopausal patients with disease progression during previous endocrine therapy. The combination of palbociclib and fulvestrant significantly prolonged PFS to 9.5 months compared with 4.6 months in fulvestrant alone (HR: 0.46, 0.36–0.59; p < 0.001). ORR was increased from 9% to 19% in the intent-to-treat (ITT) patients.42 The OS did not show any statistical difference although 6.9-month absolute improvement was achieved in combination group compared with fulvestrant group (34.9 vs 28.0 months, HR, 0.81; p = 0.09).43 Further subgroup analysis demonstrated that, the OS was extended from 29.7 to 39.7 (HR, 0.72; 95% CI, 0.55 to 0.94; absolute improvement, 10.0 months) in patients who were sensitive to previous ET.43
MONALEESA-3 is a phase III RCT study to test the clinical efficacy of ribociclib + fulvestrant as first- or second-line treatment in postmenopausal HR+/HER2- mBC patients. Unlike the PALOMA-3, MONALEESA-3 included ET treatment-naïve patients (about 50% of population) or relapsed >12 months from completion of adjuvant ET. PFS was improved by the addition of ribocilib from 12.8 to 20.5 months (HR: 0.593, 0.415–0.802; p < 0.001). The ORR was also improved from 21.5 % to 32.4% (p < 0.001).44 The OS data was not reached in the ribociclib plus fulvestrant arm while the OS was 40 months in the fulvestrant alone arm (HR: 0.724, p = 0.00455) and the relative risk of death was reduced by 28%.45
MONARCH 2 aimed to study abemaciclib plus fulvestrant in HR+/HER2-mBC patients who had progressed with prior endocrine therapy. The results manifested that PFS was significantly prolonged to 16.4 months in the abemaciclib + fulvestrant arm compared with 9.3 months in the fulvestrant arm (HR: 0.553, p < 0.001). The ORR was again increased from 16.1% to 35.2% (p < 0.001) in ITT population. Further subgroup analysis demonstrated that the benefit was consistent across all subgroups.46 The significant OS data was achieved with 46.7 months in combination of abemaciclib and fulvestrant arm and 37.3 months in fulvestrant arm (HR: 0.757; 95% CI: 0.606–0.945; p = 0.01). The absolute prolongation of OS is 9.4 months and the improvement in OS was consistent across all stratification factors. Moreover, the median time to second disease progression (23.1 vs 20.6 months), chemotherapy (50.2 vs 22.1months), and chemotherapy-free survival (25.5 vs 18.2 months) was also significantly extended in the abemaciclib + fulvestrant arm.47
Taken together, all these 3 RCTs have demonstrated that CDK4/6 inhibitors plus fulvestrant prolonged the PFS in HR+/HER2- ABC/mBC patients who had progressed on endocrine therapy (Table 1). The meaningful prolongation of OS was observed in MONALEESA-3 and MONARCH 2 but not in PALOMA-3. Ribociclib and abemaciclib in MONALEESA-3 and MONARCH 2 were used only as first- and second-line treatment of ABC/mBC.44,46 Palbociclib in PALOMA-3 was used to treatment ABC/mBC in any line, including first line (25%), second line (39%) and later lines.42 In addition, the phase III trial MONALEESA-7, which investigated ribociclib + ET + goserelin in pre-menopausal women, has proved that ribociclib + ET + goserelin significantly prolonged both PFS and OS in patients with HR+/HER2-ABC.48,49 The inclusive patients were allowed to receive up to only one previous line of chemotherapy and no previous ET for ABC in MONALEESA-7. With a comparison of the inclusion criteria and OS data, the results indicated that earlier intervention with CDK4/6 inhibitor might be positively associated with more benefits achieved, especially in OS benefits.
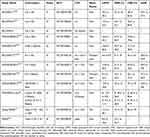 |
Table 1 Combination of CDK4/6 Inhibitors and ET in Patients with HR+/HER2- ABC/mBC |
CDK4/6 Inhibitors in Neoadjuvant Therapy of HR+/HER2-BC
The major objective of neoadjuvant therapy is to historically shrink inoperable lesions to make them operable and facilitate breast conservation without significant increase in local recurrence. The clinical efficacy of CDK4/6 inhibitors plus ET was also explored in neoadjuvant therapy of HR+/HER2-BC patients (Table 2).
 |
Table 2 The (Neo)adjuvant Therapy of CDK4/6 Inhibitor in HR+/HER2-BC |
The phase II NeoPalAna trial50 is a single-arm study to test the antiproliferative activity of anastrozole plus palbociclib in clinical stage II/III ER+ BC. Primary endpoint is the rate of complete cell cycle arrest (CCCA, defined as Ki-67 < 2.7% after 15 days of combination therapy). The results of this trial demonstrated that the rate of CCCA was significantly higher than that on Day 1 (87% vs 26%; p < 0.001), suggesting that palbociclib is an effective anti-proliferative medication for early-stage BC. However, the pathological complete response (pCR) was not evaluated in this study. Another phase II randomized trial PALLET51 demonstrated that adding palbociclib to letrozole significantly suppressed malignant HR+ BC cell proliferation (Ki-67) but did not increase the clinical response rate and pCR rate.
CORALLEEN is an open-label, multicenter, randomized, Phase 2 trial to evaluate the proportion of patients with PAM50 low-risk-of-relapse (ROR) disease at surgery after neoadjuvant treatment with ribociclib plus letrozole versus chemotherapy.52 This study has enrolled 106 women with the luminal B subtype of BC at the stage I-IIIA. The low-ROR was 46.9% (95% CI 32.5–61.7) in ribociclib plus letrozole group and 46.1% (95% CI 32.9–61.5) in chemotherapy group, and the pCR rate (2.0% vs 5.8%) and ORR (57.2% vs 78.8%) did not show any significant difference. The neoMONARCH53 is a phase II study to evaluate the clinical efficacy of abemaciclib plus anastrozole in the neoadjuvant setting. This study enrolled 223 postmenopausal women with HR+/HER2− primary breast tumor (≥1 cm) and the primary endpoint is the change in Ki67 from baseline to 2 weeks after treatment (CCCA). More patients in the combination arm versus anastrozole alone achieved CCCA (68% vs 14%, p < 0.001), and pCR was 4% in ITT patients. Taken together, all the 3 CDK4/6 inhibitors have manifested their advantage in CCCA, but these clinical trials have not observed any advantages on pCR compared with ET alone or chemotherapy. Phase III head-to-head clinical trials are still needed to confirm the biological and clinical activity of CDK4/6 inhibitors in the neoadjuvant setting. In the adjuvant setting, there are several ongoing phase III trials (https://clinicaltrials.gov/): PALLAS (NCT02513394), PENELOPE-B (NCT01864746), EarLEE-2 (NCT03081234), NATALEE (NCT03701334) and monarchE (NCT03155997), etc. (Table 2). The promising results are expected to benefit more patients with early BC.
CDK4/6 Inhibitors in HER2-Positive BC
HER2-positive (HER2+) tumors account for 15–20% of all BC. HER2+ BC is associated with biological aggressiveness and poor outcomes.54 Cell cycle is also alternated in HER2+ BC.55 Studies have demonstrated that both cyclin D1 and CDK4 are essential for HER2+ murine mammary tumor development.56–58 Combination of palbociclib and trastuzumab demonstrates a synergistic effects on 3 HER2-amplified BC cell lines.59 On a basis of these preclinical data, clinical trials are conducted to explore the clinical activity of CDK4/6 inhibitors in HER2+ BC.
A multicohort, open-label, single-arm, phase II study NA-PHER2 aimed to investigate the combination of palbociclib, fulvestrant and trastuzumab in patients with HR+/HER2+ BC in the neoadjuvant setting.60 Ki67 expression was reduced from 31.9% to 4.3% at Week 2 (n = 25, p < 0.001) and 12.1% in the triple combination group at time of surgery (n = 22, p = 0.013). The clinical objective response was 29 of 30 patients (97%, 95% CI 83–100) immediately before surgery and 8 (27%; 95% CI 12–46) patients had a pathological complete response in the arm of palbociclib + fulvestrant + trastuzumab.
PATRICIA II study (NCT02448420) is a prospective, multicenter, open-label phase II trial. The objective of this study is to test the role of palbociclib and trastuzumab plus or minus letrozole in HER2+ mBC. The primary endpoint of this study is PFS at 6 months and secondary endpoint is the safety profile, including the cardiac safety, the overall tumor ORR and the OS. PATINA (NCT02947685) is an open-label, randomized phase III trial that aimed to assess the prolongation of PFS with the addition of palbociclib to HER2-directed therapy and ET compared with HER2-directed therapy and ET in HR+/HER2+ ABC/mBC. The inclusive patients are those who have completed standard first-line treatment with dual HER2-directed therapy and a taxane. Results of this study are expected in 2021.
monarcHER is a multicenter, randomized, three-arm, open-label, phase II trial evaluating the clinical efficacy of abemaciclib plus trastuzumab ± fulvestrant compared with standard chemotherapy plus trastuzumab in women with HR+/HER2+ ABC/mBC (NCT02675231). The primary endpoint is PFS and secondary endpoints include OS, ORR, CBR, quality of life, pain control and pharmacokinetics. The initial results are expected in 2021.
An ongoing phase II trial aims to evaluate the effects of palbociclib and trastuzumab on HER2+ patients with brain metastasis (NCT02774681). The primary endpoint of this single-arm study is to measure the radiographic response rate in the central nervous system (CNS). The secondary endpoints are PFS, OS, ORR, time to CNS progression and toxicity.
There is another ongoing phase I/II trial investigating ribociclib plus trastuzumab or T-DM1 for HER2+ ABC/mBC (NCT02657343). This study includes three cohorts: ribociclib + trastuzumab + fulvestrant for HR+/HER2+ BC, ribociclib plus T-DM1 and ribociclib plus trastuzumab. The primary outcomes are the maximum tolerated dose or recommended phase II dose. The secondary outcomes are the plasma concentration of ribociclib, ORR, PFS, OS, frequency of biomarkers and frequency of adverse events.
The role of CDK4/6 inhibitors in patients with HER2+ BC is still under exploration. To date, most ongoing trials are phase II studies and NA-PHER2 is the only one that has been reported its results. Therefore, more phase III RCTs are warranted to figure out the effectiveness of CDK4/6 inhibitors in patients with HER2+ BC in future.
Biomarkers and Resistance of CDK4/6 Inhibitors
As mentioned above, the discovery of CDK4/6 inhibitors has improved the prognosis of HR+ BC and may also benefit HER2+ BC and other solid tumors. However, not all patients respond to the CDK4/6 inhibitors and even patient sensitive to CDK4/6 inhibitors might develop the acquired resistance.61 Mechanism of resistance to CDK4/6 inhibitors is still unclear and predicting biomarkers have not been identified. This review summarized the potential mechanisms and biomarkers in both preclinical and clinical data.
Loss of Rb
Rb, as the target of CDK4/6, is considered as one of the most important biomarkers of sensitivity to CDK4/6 target therapy.62 Preclinical studies have proved that loss of Rb function was detected in palbociclib resistance cell lines.63 In mBC patients who had received the treatment with palbociclib or ribociclib, somatic Rb1 mutations were detected when disease was progressed,64 suggesting that Rb mutation might be associated with acquired resistance to CDK4/6 inhibitors. However, only three patients reported in this publication. A large study is warranted to confirm this conclusion.
Overexpression of Cyclin E1
In addition to cyclin D-CDK4/6 complex, cyclin E-CDK2 complex could also release E2E via phosphorylating Rb.65 Expression of Cyclin E1 was upregulated in CDK4/6 inhibitor resistance cell lines66 and overexpression of Cyclin E1attenuated the inhibitory effects of CDK4/6 on cell cycle progress.67 Biomarker analysis of PALOMA-3 manifested that high expression of CCNE1 mRNA demonstrated a shorter PFS in patients received palbociclib plus fulvestrant treatment68 while this was not found in PALOMA-2 study,69 indicating that mRNA level of cyclinE1 was an effective biomarker in previously treated HR+/HER2-mBC.
p16 Amplification
p16INK4A is an intrinsic tumor-suppressor which can bind to CDK4/6 to disrupt the formation of cyclin D-CDK4/6 complex.70–72 Overexpression of p16 is observed during oncogenic stress. When p16 overexpression is concurrent with loss of Rb, resistance to CDK4/6 inhibitor was gained as a result of Rb dysfunction.73 In the presence of Rb, overexpression of p16 showed resistance to CDK4/6 inhibitor due to diminished CDK4.61,74 However, the results of PALOMA-1 did not show any significant difference in PFS in the loss of p16/CCND1 amplification cohort compared with the unselected cohort.75 Similar results were also obtained from the biomarker analysis of PALOMA-2 and PALOMA-3.68,69 Therefore, it is controversial to use p16 amplification as a biomarker.
TK1
Thymidine kinase-1 (TK1) is a key regulator of cell cycle and highly expresses in S/G2 phase to catalyze DNA precursor synthesis.76 Serum TK1 level and activity were increased in solid tumors, including lung, colorectal and breast cancer.77 In primary BC patients, high TK1 levels and activity are associated with large tumor size and poor prognosis.78,79 In patients with HR+/HER2-mBC, lower baseline TK1 activity was correlated with a longer PFS and decrease of TK1 activity after one month of treatment was also linked to a significantly better PFS,80 indicating that TK1 is a meaningful biomarker and a potential therapeutic target in HR+/HER2-mBC. ECLIPS is a prospective, pharmacogenetic study to identify the predictive biomarkers which are responsive/resistant to palbociclib plus ET (letrozole or fulvestrant).81 The results showed that the number of copies/mL of TK1 was significantly increased before treatment compared to that after 3 months of treatment (1200 vs 3350 copies/mL, p = 0.01) in patients with disease progression, suggesting that TK1 mRNA copies/mL is correlated to acquired resistance to CDK4/6 inhibitors.
Loss of FAT1
FAT1 is a tumor-suppressor belonging to the cadherin superfamily and interacts with the β-catenin and Hippo signaling pathways.75 Loss of FAT1 has been reported to promote cancer progression.82 With gene sequencing of 1501 HR+/HER2-BC patients, FAT1 mutation accounted for ~ 2% in primary and ~ 6% in metastatic tumors.83 Preclinical data demonstrated that FAT1 loss-induced upregulation of CDK6 expression through Hippo pathway, resulting in resistance to CDK4/6 inhibitors.66 Gene analysis results from 348 ER+/HER2-BC patients, who have previously treated with CDK4/6 inhibitors, showed that loss of FAT1 was linked to poor prognosis of CDK4/6 inhibitor therapy and shorter PFS (2.4 months) compared with FAT1 wild type arm (PFS: 10.1 months; p = 2.2 × 10−11.66 Therefore, loss of FAT1 might be an effective predictor of CDK4/6 inhibitor resistance.
Besides the potential biomarkers mentioned above, results from ECLIPS demonstrated that the number of copies/mL of CDK9 was significantly increased before treatment compared to that after 3 months of treatment (3800 vs 7500 copies/mL, p = 0.03) in HR+/HER2-mBC patients with disease progression.81 Interestingly, biomarker analysis of PALOMA-2 found that high level of PD-1 showed less benefit from the combination of palbociclib and letrozole compared to low PD-1expression.69 Results from PALOMA studies have demonstrated that CCND1, CDK4 and CDK6 did not indicate any predictive effects on resistance to CDK4/6 inhibitors.1,34,68 Therefore, future studies should focus on identification of the effective biomarkers of sensitivity/resistance to CDK4/6 inhibitors.
Conclusion and Future Prospection
With the introduction of CDK4/6 inhibitor, a longer PFS and better CBR and ORR were achieved in patients with HR+/HER2- ABC/mBC, and the benefit of OS was also observed in the patient previously treated with ET. Ongoing clinical trials focus on treatment with CDK4/6 inhibitors in the early stage of HR+/HER2- and HER2+ BC. Since cell cycle regulation of CDK4/6 was not only observed in breast cancer, but also in the other cancers,84 several phase I/II trials have been reported the preliminary clinical efficacy of CDK4/6 inhibitors in non-BC such as head and neck squamous cell carcinoma,85 mantle cell lymphoma,86 glioblastoma,87 germ cell tumor.88 Therefore, CDK4/6 inhibitor is hopeful to expand to treat patients with other tumors in addition to breast cancer and more and more cancer patient will gain benefit from CDK4/6 inhibitor therapy in future.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Funding
No funding was received.
Disclosure
Yu Zhang was employed by Pfizer, Inc. at the time of the study. The authors declare that they have no other conflict of interest.
References
1. Globocan. Breast cancer fact sheet. 2018. Available from: http://gco.iarc.fr/today/data/factsheets/cancers/20-Breast-fact-sheet.pdf.
2. Institute NC. Cancer Stat facts: female breast cancer. 2019. Available from: https://seer.cancer.gov/statfacts/html/breast.html.
3. Serra F, Lapidari P, Quaquarini E, Tagliaferri B, Sottotetti F, Palumbo R. Palbociclib in metastatic breast cancer: current evidence and real-life data. Drugs Context. 2019;8:212579. doi:10.7573/dic.212579
4. Baselga J, Campone M, Piccart M, et al. Everolimus in postmenopausal hormone-receptor-positive advanced breast cancer. N Engl J Med. 2012;366(6):520–529. doi:10.1056/NEJMoa1109653
5. Messina C, Cattrini C, Buzzatti G, et al. CDK4/6 inhibitors in advanced hormone receptor-positive/HER2-negative breast cancer: a systematic review and meta-analysis of randomized trials. Breast Cancer Res Treat. 2018;172(1):9–21. doi:10.1007/s10549-018-4901-0
6. Diaz-Moralli S, Tarrado-Castellarnau M, Miranda A, Cascante M. Targeting cell cycle regulation in cancer therapy. Pharmacol Ther. 2013;138(2):255–271. doi:10.1016/j.pharmthera.2013.01.011
7. Narasimha AM, Kaulich M, Shapiro GS, Choi YJ, Sicinski P, Dowdy SF. Cyclin D activates the Rb tumor suppressor by mono-phosphorylation. Elife. 2014;3:e02872. doi:10.7554/eLife.02872
8. Harbour JW, Luo RX, Santi AD, Postigo AA, Dean DC. Cdk phosphorylation triggers sequential intramolecular interactions that progressively block Rb functions as cells move through G1. Cell. 1999;98(6):859–869. doi:10.1016/S0092-8674(00)81519-6
9. Hiebert SW, Chellappan SP, Horowitz JM, Nevins JR. The interaction of RB with E2F coincides with an inhibition of the transcriptional activity of E2F. Genes Devel. 1992;6(2):177–185.
10. Weintraub SJ, Chow KNB, Luo RX, Zhang SH, He S, Dean DC. Mechanism of active transcriptional repression by the retinoblastoma protein. Nature. 1995;375(6534):812–816.
11. Wade Harper J, Adami GR, Wei N, Keyomarsi K, Elledge SJ. The p21 Cdk-interacting protein Cip1 is a potent inhibitor of G1 cyclin-dependent kinases. Cell. 1993;75(4):805–816. doi:10.1016/0092-8674(93)90499-G
12. Blain SW, Montalvo E, Massagué J. Differential interaction of the cyclin-dependent kinase (Cdk) inhibitor p27Kip1 with cyclin A-Cdk2 and cyclin D2-Cdk4. J Biol Chem. 1997;272(41):25863–25872.
13. LaBaer J, Garrett MD, Stevenson LF, et al. New functional activities for the p21 family of CDK inhibitors. Genes Develop. 1997;11(7):847–862.
14. Mayer EL. Targeting breast cancer with CDK inhibitors. Curr Oncol Rep. 2015;17(5):20. doi:10.1007/s11912-015-0443-3
15. Malumbres M, Barbacid M. Cell cycle, CDKs and cancer: a changing paradigm. Nat Rev Cancer. 2009;9(3):153–166. doi:10.1038/nrc2602
16. Taneja P, Maglic D, Kai F, et al. Classical and novel prognostic markers for breast cancer and their clinical significance. Clin Med Insights Oncol. 2010;4:
17. Musgrove EA, Caldon CE, Barraclough J, Stone A, Sutherland RL. Cyclin D as a therapeutic target in cancer. Nat Rev Cancer. 2011;11(8):558–572. doi:10.1038/nrc3090
18. Musgrove EA, Lee CS, Buckley MF, Sutherland RL. Cyclin D1 induction in breast cancer cells shortens G1 and is sufficient for cells arrested in G1 to complete the cell cycle. Proc Natl Acad Sci. 1994;91(17):8022–8026.
19. Wang TC, Cardiff RD, Zukerberg L, Lees E, Arnold A, Schmidt EV. Mammary hyperplasia and carcinoma in MMTV-cyclin D1 transgenic mice. Nature. 1994;369(6482):669–671. doi:10.1038/369669a0
20. Jares P, Colomer D, Campo E. Genetic and molecular pathogenesis of mantle cell lymphoma: perspectives for new targeted therapeutics. Nat Rev Cancer. 2007;7(10):750–762. doi:10.1038/nrc2230
21. Roy PG, Thompson AM. Cyclin D1 and breast cancer. The Breast. 2006;15(6):718–727. doi:10.1016/j.breast.2006.02.005
22. An H-X, Beckmann MW, Reifenberger G, Bender HG, Niederacher D. Gene amplification and overexpression of CDK4 in sporadic breast carcinomas is associated with high tumor cell proliferation. Am J Pathol. 1999;154(1):113–118. doi:10.1016/S0002-9440(10)65257-1
23. Timmermann S, Hinds P, Munger K. Elevated activity of cyclin-dependent kinase 6 in human squamous cell carcinoma lines. Cell Growth Diff Publ Am Assoc Cancer Res. 1997;8(4):361–370.
24. Wang H, Nicolay BN, Chick JM, et al. The metabolic function of cyclin D3-CDK6 kinase in cancer cell survival. Nature. 2017;546(7658):426–430. doi:10.1038/nature22797
25. FDA. Ibrance Prescribing Infomation. 2019. Available from: https://www.accessdata.fda.gov/drugsatfda_docs/label/2019/207103s008lbl.pdf.
26. FDA. Kisqali Prescribing Information. 2017. Available from: https://www.accessdata.fda.gov/drugsatfda_docs/label/2017/209092s000lbl.pdf.
27. EMA. Ibrance authorisation details. 2019. Available from: https://www.ema.europa.eu/en/medicines/human/EPAR/ibrance.
28. EMA. Verzenio authorisation details. 2019. Available from: https://www.ema.europa.eu/en/medicines/human/EPAR/verzenios.
29. Wedam S, Fashoyin-Aje L, Bloomquist E, et al. FDA approval summary: palbociclib for male patients with metastatic breast cancer. Clin Cancer Res. 2019. doi:10.1158/1078-0432.CCR-1119-2580
30. FDA. Verzenio prescribing information. 2017. Available from: https://www.accessdata.fda.gov/drugsatfda_docs/label/2017/208716s000lbl.pdf.
31. Sun W, Klamerus KJ, Yuhas LM, et al. Impact of acid-reducing agents on the pharmacokinetics of palbociclib, a weak base with pH-dependent solubility, with different food intake conditions. Clin Pharmacol Drug Develop. 2017;6(6):614–626.
32. Messina C, Messina M, Zanardi E. Risks and benefits from CDK inhibitors for advanced HR+ Her 2- breast cancer. Ann Oncol. 2017;28(12):3099–3100. doi:10.1093/annonc/mdx530
33. Garber K. The cancer drug that almost wasn’t. 2014;345(6199):865–867.
34. Finn RS, Crown JP, Lang I, et al. The cyclin-dependent kinase 4/6 inhibitor palbociclib in combination with letrozole versus letrozole alone as first-line treatment of oestrogen receptor-positive, HER2-negative, advanced breast cancer (PALOMA-1/TRIO-18): a randomised phase 2 study. Lancet Oncol. 2015;16(1):25–35. doi:10.1016/S1470-2045(14)71159-3
35. Finn RS, Crown J, Lang I, et al. Overall survival results from the randomized phase II study of palbociclib (P) in combination with letrozole (L) vs letrozole alone for frontline treatment of ER+/HER2– advanced breast cancer (PALOMA-1; TRIO-18). J Clin Oncol. 2017;35(15_suppl):1001. doi:10.1200/JCO.2017.35.15_suppl.1001
36. Finn RS, Martin M, Rugo HS, et al. Palbociclib and letrozole in advanced breast cancer. N Engl J Med. 2016;375(20):1925–1936. doi:10.1056/NEJMoa1607303
37. Rugo HS, Finn RS, Diéras V, et al. Palbociclib plus letrozole as first-line therapy in estrogen receptor-positive/human epidermal growth factor receptor 2-negative advanced breast cancer with extended follow-up. Breast Cancer Res Treat. 2019;174(3):719–729. doi:10.1007/s10549-018-05125-4
38. Hortobagyi GN, Stemmer SM, Burris HA, et al. Ribociclib as first-line therapy for HR-positive, advanced breast cancer. N Eng J Med. 2016;375(18):1738–1748.
39. Hortobagyi GN, Stemmer SM, Burris HA, et al. Updated results from MONALEESA-2, a phase III trial of first-line ribociclib plus letrozole versus placebo plus letrozole in hormone receptor-positive, HER2-negative advanced breast cancer. Ann Oncol. 2018;29(7):1541–1547. doi:10.1093/annonc/mdy155
40. Goetz MP, Toi M, Campone M, et al. MONARCH 3: abemaciclib as initial therapy for advanced breast cancer. 2017;35(32):3638–3646.
41. Johnston S, Martin M, Di Leo A, et al. MONARCH 3 final PFS: a randomized study of abemaciclib as initial therapy for advanced breast cancer. NPJ Breast Cancer. 2019;5:5. doi:10.1038/s41523-018-0097-z
42. Cristofanilli M, Turner NC, Bondarenko I, et al. Fulvestrant plus palbociclib versus fulvestrant plus placebo for treatment of hormone-receptor-positive, HER2-negative metastatic breast cancer that progressed on previous endocrine therapy (PALOMA-3): final analysis of the multicentre, double-blind, Phase 3 randomised controlled trial. Lancet Oncol. 2016;17(4):425–439. doi:10.1016/S1470-2045(15)00613-0
43. Turner NC, Slamon DJ, Ro J, et al. Overall survival with palbociclib and fulvestrant in advanced breast cancer. N Engl J Med. 2018;379(20):1926–1936. doi:10.1056/NEJMoa1810527
44. Slamon DJ, Neven P, Chia S, et al. Phase III randomized study of ribociclib and fulvestrant in hormone receptor–positive, human epidermal growth factor receptor 2–negative advanced breast cancer: MONALEESA-3. J Clin Oncol. 2018;36(24):2465–2472.
45. Slamon DJ, Neven P, Chia S, et al. Overall survival with ribociclib plus fulvestrant in advanced breast cancer. N Engl J Med. 2019;382(6):514–524. doi:10.1056/NEJMoa1911149
46. Sledge GW, Toi M, Neven P, et al. MONARCH 2: abemaciclib in combination with fulvestrant in women with HR+/HER2− advanced breast cancer who had progressed while receiving endocrine therapy. J Clin Oncol. 2017;35(25):2875–2884. doi:10.1200/JCO.2017.73.7585
47. Sledge GW
48. Tripathy D, Im S-A, Colleoni M, et al. Ribociclib plus endocrine therapy for premenopausal women with hormone-receptor-positive, advanced breast cancer (MONALEESA-7): a randomised phase 3 trial. Lancet Oncol. 2018;19(7):904–915. doi:10.1016/S1470-2045(18)30292-4
49. Im S-A, Lu Y-S, Bardia A, et al. Overall survival with ribociclib plus endocrine therapy in breast cancer. N Engl J Med. 2019;381(4):307–316. doi:10.1056/NEJMoa1903765
50. Ma CX, Gao F, Luo J, et al. NeoPalAna: neoadjuvant palbociclib, a cyclin-dependent kinase 4/6 inhibitor, and anastrozole for clinical stage 2 or 3 estrogen receptor–positive breast cancer. Clin Cancer Res. 2017;23(15):4055–4065. doi:10.1158/1078-0432.CCR-16-3206
51. Johnston S, Puhalla S, Wheatley D, et al. Randomized Phase II study evaluating palbociclib in addition to letrozole as neoadjuvant therapy in estrogen receptor-positive early breast cancer: PALLET Trial. J Clin Oncol. 2019;37(3):178–189. doi:10.1200/JCO.18.01624
52. Prat A, Saura C, Pascual T, et al. Ribociclib plus letrozole versus chemotherapy for postmenopausal women with hormone receptor-positive, HER2-negative, luminal B breast cancer (CORALLEEN): an open-label, multicentre, randomised, phase 2 trial. Lancet Oncol. 2019.
53. Hurvitz SA, Martin M, Press MF, et al. Potent cell-cycle inhibition and upregulation of immune response with abemaciclib and anastrozole in neoMONARCH, Phase II neoadjuvant study in HR(+)/HER2(-) breast cancer. Clin Cancer Res. 2019. doi:10.1158/1078-0432.CCR-1119-1425
54. English DP, Roque DM, Santin AD. HER2 expression beyond breast cancer: therapeutic implications for gynecologic malignancies. Mol Diagn Ther. 2013;17(2):85–99. doi:10.1007/s40291-013-0024-9
55. Cancer Genome Atlas N. Comprehensive molecular portraits of human breast tumours. Nature. 2012;490(7418):61–70.
56. Yu Q, Geng Y, Sicinski P. Specific protection against breast cancers by cyclin D1 ablation. Nature. 2001;411(6841):1017–1021. doi:10.1038/35082500
57. Landis MW, Pawlyk BS, Li T, Sicinski P, Hinds PW. Cyclin D1-dependent kinase activity in murine development and mammary tumorigenesis. Cancer Cell. 2006;9(1):13–22. doi:10.1016/j.ccr.2005.12.019
58. Corona SP, Ravelli A, Cretella D, et al. CDK4/6 inhibitors in HER2-positive breast cancer. Crit Rev Oncol Hematol. 2017;112:208–214. doi:10.1016/j.critrevonc.2017.02.022
59. Finn RS, Dering J, Conklin D, et al. PD 0332991, a selective cyclin D kinase 4/6 inhibitor, preferentially inhibits proliferation of luminal estrogen receptor-positive human breast cancer cell lines in vitro. Breast Cancer Res. 2009;11(5):R77. doi:10.1186/bcr2419
60. Gianni L, Bisagni G, Colleoni M, et al. Neoadjuvant treatment with trastuzumab and pertuzumab plus palbociclib and fulvestrant in HER2-positive, ER-positive breast cancer (NA-PHER2): an exploratory, open-label, phase 2 study. Lancet Oncol. 2018;19(2):249–256. doi:10.1016/S1470-2045(18)30001-9
61. Pandey K, An H-J, Kim SK, et al. Molecular mechanisms of resistance to CDK4/6 inhibitors in breast cancer: A review. Int J Cancer. 2019;145(5):1179–1188. doi:10.1002/ijc.32020
62. Wiedemeyer WR, Dunn IF, Quayle SN, et al. Pattern of retinoblastoma pathway inactivation dictates response to CDK4/6 inhibition in GBM. Proc Natl Acad Sci U S A. 2010;107(25):11501–11506. doi:10.1073/pnas.1001613107
63. Malorni L, Piazza S, Ciani Y, et al. A gene expression signature of retinoblastoma loss-of-function is a predictive biomarker of resistance to palbociclib in breast cancer cell lines and is prognostic in patients with ER positive early breast cancer. Oncotarget. 2016;7(42):68012–68022. doi:10.18632/oncotarget.12010
64. Condorelli R, Spring L, O’Shaughnessy J, et al. Polyclonal RB1 mutations and acquired resistance to CDK 4/6 inhibitors in patients with metastatic breast cancer. Ann Oncol. 2018;29(3):640–645. doi:10.1093/annonc/mdx784
65. Obeyesekere MN, Herbert JR, Zimmerman SO. A model of the G1 phase of the cell cycle incorporating cyclin E/cdk2 complex and retinoblastoma protein. Oncogene. 1995;11(6):1199–1205.
66. Li Z, Razavi P, Li Q, et al. Loss of the FAT1 tumor suppressor promotes resistance to CDK4/6 inhibitors via the hippo pathway. Cancer Cell. 2018;34(6):893–905.e898. doi:10.1016/j.ccell.2018.11.006
67. Taylor-Harding B, Aspuria P-J, Agadjanian H, et al. Cyclin E1 and RTK/RAS signaling drive CDK inhibitor resistance via activation of E2F and ETS. Oncotarget. 2015;6(2):696–714. doi:10.18632/oncotarget.2673
68. Turner NC, Liu Y, Zhu Z, et al. Cyclin E1 expression and palbociclib efficacy in previously treated hormone receptor–positive metastatic breast cancer. J Clin Oncol. 2019;37(14):1169–1178. doi:10.1200/JCO.18.00925
69. Finn RS, Liu Y, Zhu Z, et al. biomarker analyses of response to cyclin dependent kinase 4/6 inhibition and endocrine therapy in women with treatment-naïve metastatic breast cancer. Clin Cancer Res. 2019;(clincanres.0751.2019).
70. Siebert R, Willers CP, Opalka B. Role of the cyclin-dependent kinase 4 and 6 inhibitor gene family p15, p16, p18 and p19 in leukemia and lymphoma. Leuk Lymphoma. 1996;23(5–6):505–520. doi:10.3109/10428199609054859
71. Serrano M, Hannon GJ, Beach D. A new regulatory motif in cell-cycle control causing specific inhibition of cyclin D/CDK4. Nature. 1993;366(6456):704–707. doi:10.1038/366704a0
72. Russo AA, Tong L, Lee JO, Jeffrey PD, Pavletich NP. Structural basis for inhibition of the cyclin-dependent kinase Cdk6 by the tumour suppressor p16INK4a. Nature. 1998;395(6699):237–243. doi:10.1038/26155
73. Liu Y, Zhong X, Wan S, et al. p16(INK4a) expression in retinoblastoma: a marker of differentiation grade. Diagn Pathol. 2014;9:180. doi:10.1186/s13000-014-0180-1
74. Dean JL, McClendon AK, Hickey TE, et al. Therapeutic response to CDK4/6 inhibition in breast cancer defined by ex vivo analyses of human tumors. Cell Cycle. 2012;11(14):2756–2761. doi:10.4161/cc.21195
75. Finn RS, Crown JP, Ettl J, et al. Efficacy and safety of palbociclib in combination with letrozole as first-line treatment of ER-positive, HER2-negative, advanced breast cancer: expanded analyses of subgroups from the randomized pivotal trial PALOMA-1/TRIO-18. Breast Cancer Res. 2016;18(1):67. doi:10.1186/s13058-016-0721-5
76. Jagarlamudi KK, Shaw M. Thymidine kinase 1 as a tumor biomarker: technical advances offer new potential to an old biomarker. Biomark Med. 2018;12(9):1035–1048. doi:10.2217/bmm-2018-0157
77. Topolcan O, Holubec L. The role of thymidine kinase in cancer diseases. Expert Opin Med Diagn. 2008;2(2):129–141. doi:10.1517/17530059.2.2.129
78. Broët P, Romain S, Daver A, et al. Thymidine kinase as a proliferative marker: clinical relevance in 1692 primary breast cancer patients. J Clin Oncol. 2001;19(11):2778–2787. doi:10.1200/JCO.2001.19.11.2778
79. Romain S, Spyratos F, Descotes F, et al. Prognostic of DNA-synthesizing enzyme activities (thymidine kinase and thymidylate synthase) in 908 T1–T2, N0–N1, M0 breast cancers: a retrospective multicenter study. Int J Cancer. 2000;87(6):860–868. doi:10.1002/1097-0215(20000915)87:6<860::AID-IJC16>3.0.CO;2-Y
80. Bonechi M, Galardi F, Biagioni C, et al. Plasma thymidine kinase-1 activity predicts outcome in patients with hormone receptor positive and HER2 negative metastatic breast cancer treated with endocrine therapy. Oncotarget. 2018;9(23):16389–16399. doi:10.18632/oncotarget.24700
81. Del Re M, Bertolini I, Crucitta S, et al. Overexpression of TK1 and CDK9 in plasma-derived exosomes is associated with clinical resistance to CDK4/6 inhibitors in metastatic breast cancer patients. Breast Cancer Res Treat. 2019;178(1):57–62. doi:10.1007/s10549-019-05365-y
82. Morris LGT, Kaufman AM, Gong Y, et al. Recurrent somatic mutation of FAT1 in multiple human cancers leads to aberrant Wnt activation. Nat Genet. 2013;45(3):253–261. doi:10.1038/ng.2538
83. Schoninger SF, Blain SW. The ongoing search for biomarkers of CDK4/6 inhibitor responsiveness in breast cancer. Mol Cancer Ther. 2020;19(1):3–12. doi:10.1158/1535-7163.MCT-19-0253
84. O’Leary B, Finn RS, Turner NC. Treating cancer with selective CDK4/6 inhibitors. Nat Rev Clin Oncol. 2016;13(7):417–430. doi:10.1038/nrclinonc.2016.26
85. Swiecicki PL, Durm G, Bellile E, Bhangale A, Brenner JC, Worden FP. A multi-center phase II trial evaluating the efficacy of palbociclib in combination with carboplatin for the treatment of unresectable recurrent or metastatic head and neck squamous cell carcinoma. Invest New Drugs. 2020. doi:10.1007/s10637-020-00898-2
86. Leonard JP, LaCasce AS, Smith MR, et al. Selective CDK4/6 inhibition with tumor responses by PD0332991 in patients with mantle cell lymphoma. Blood. 2012;119(20):4597–4607. doi:10.1182/blood-2011-10-388298
87. Taylor JW, Parikh M, Phillips JJ, et al. Phase-2 trial of palbociclib in adult patients with recurrent RB1-positive glioblastoma. J Neurooncol. 2018;140(2):477–483. doi:10.1007/s11060-018-2977-3
88. Vaughn DJ, Hwang W-T, Lal P, Rosen MA, Gallagher M, O’Dwyer PJ. Phase 2 trial of the cyclin-dependent kinase 4/6 inhibitor palbociclib in patients with retinoblastoma protein-expressing germ cell tumors. Cancer. 2015;121(9):1463–1468. doi:10.1002/cncr.29213
89. Eschbach RS, Kazmierczak PM, Heimer MM, et al. (18)F-FDG-PET/CT and diffusion-weighted MRI for monitoring a BRAF and CDK 4/6 inhibitor combination therapy in a murine model of human melanoma. Cancer Imaging. 2018;18(1):2. doi:10.1186/s40644-018-0135-y
90. Lee MS, Helms TL, Feng N, et al. Efficacy of the combination of MEK and CDK4/6 inhibitors in vitro and in vivo in KRAS mutant colorectal cancer models. Oncotarget. 2016;7(26):39595–39608. doi:10.18632/oncotarget.9153
91. André F, Ciruelos E, Rubovszky G, et al. Alpelisib for PIK3CA-mutated, hormone receptor–positive advanced breast cancer. N Engl J Med. 2019;380(20):1929–1940. doi:10.1056/NEJMoa1813904
92. Olmez I, Brenneman B, Xiao A, et al. Combined CDK4/6 and mTOR inhibition is synergistic against glioblastoma via multiple mechanisms. Clin Cancer Res. 2017;23(22):6958–6968. doi:10.1158/1078-0432.CCR-17-0803
93. Hortobagyi GN. Ribociclib for the first-line treatment of advanced hormone receptor-positive breast cancer: a review of subgroup analyses from the MONALEESA-2 trial. Breast Cancer Res. 2018;20(1):123. doi:10.1186/s13058-018-1050-7
94. Turner NC, Jungsil R, André F, et al. Palbociclib in hormone-receptor–positive advanced breast cancer. N Engl J Med. 2015;373(17):1672–1673. doi:10.1056/NEJMoa1505270
95. George W, Sledge J, Toi M, et al. MONARCH 2: abemaciclib in combination with fulvestrant in women with HR+/HER2− advanced breast cancer who had progressed while receiving endocrine therapy. 2017;35(25):2875–2884.
96. Jiang Z, Hu X, Zhang Q, et al. MONARCHplus: a phase III trial of abemaciclib plus nonsteroidal aromatase inhibitor (NSAI) or fulvestrant (F) for women with HR+/HER2- advanced breast cancer (ABC). Ann Oncol. 2019;30:v863. doi:10.1093/annonc/mdz394.014
97. Park YH, Kim T-Y, Kim GM, et al. Palbociclib plus exemestane with gonadotropin-releasing hormone agonist versus capecitabine in premenopausal women with hormone receptor-positive, HER2-negative metastatic breast cancer (KCSG-BR15-10): a multicentre, open-label, randomised, phase 2 trial. Lancet Oncol. 2019;20(12):1750–1759. doi:10.1016/S1470-2045(19)30565-0
98. Martín M, Zielinski C, Ruíz-Borrego M, et al. Results from PEARL study (GEICAM/2013-02_CECOG/BC.1.3.006): a phase 3 trial of Palbociclib (PAL) in combination with endocrine therapy (ET) versus Capecitabine (CAPE) in hormonal receptor (HR)-positive/human epidermal growth factor receptor (HER) 2-negative metastatic breast cancer (MBC) patients (pts) whose disease progressed on aromatase inhibitors (AIs).
99. Cottu P, D’Hondt V, Dureau S, et al. Letrozole and palbociclib versus chemotherapy as neoadjuvant therapy of high-risk luminal breast cancer. Ann Oncol. 2018;29(12):2334–2340. doi:10.1093/annonc/mdy448
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
