Back to Journals » Neuropsychiatric Disease and Treatment » Volume 14
Clinical characteristics and course of oral somatic delusions: a retrospective chart review of 606 cases in 5 years
Authors Umezaki Y , Miura A , Shinohara Y , Mikuzuki L , Sugawara S , Kawasaki K , Tu TTH , Watanabe T , Suga T , Watanabe M, Takenoshita M, Yoshikawa T, Uezato A , Nishikawa T, Hoshiko K, Naito T, Motomura H, Toyofuku A
Received 7 March 2018
Accepted for publication 27 April 2018
Published 13 August 2018 Volume 2018:14 Pages 2057—2065
DOI https://doi.org/10.2147/NDT.S167527
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Taro Kishi
Yojiro Umezaki,1 Anna Miura,2 Yukiko Shinohara,2 Lou Mikuzuki,2 Shiori Sugawara,2 Kaoru Kawasaki,2 Trang TH Tu,2 Takeshi Watanabe,2 Takayuki Suga,2 Motoko Watanabe,3 Miho Takenoshita,2 Tatsuya Yoshikawa,2 Akihito Uezato,4 Toru Nishikawa,4 Ken Hoshiko,5 Toru Naito,1 Haruhiko Motomura,2 Akira Toyofuku2
1Section of Geriatric Dentistry, Department of General Dentistry, Fukuoka Dental College, Fukuoka, Japan; 2Department of Psychosomatic Dentistry, Graduate School of Medical and Dental Sciences, Tokyo Medical and Dental University, Tokyo, Japan; 3Department of Oral and Maxillofacial Radiology, Tokyo Dental College, Tokyo, Japan; 4Department of Psychiatry and Behavioral Sciences, Graduate School of Medical and Dental Sciences, Tokyo Medical and Dental University, Tokyo, Japan; 5Department of Pharmacy, Dental Hospital, Tokyo Medical and Dental University, Tokyo, Japan
Objective: Oral cenesthopathy is characterized by foreign body sensations without medical and dental evidence for them. It is thought to be a rare disease in psychiatry, but many patients are visiting dental clinics seeking treatment to remove a foreign body. Even though the features of oral cenesthopathy might be different between a psychiatric clinic and a dental clinic, there has been no clinico-statistical study from dentists. In this study, we report a clinico-statistical study of patients with oral cenesthopathy in dentistry.
Methods: This is a retrospective chart review of 606 outpatients with oral cenesthopathy in Tokyo Medical and Dental University from April 2010 through to March 2015.
Results: A total of 159 male and 447 female patients were included in this study. The mean age was 62.08 years, and female patients were older than male patients. The trigger of the dental treatment and the acute phase of depression at the onset were significantly related (p=0.037). Only 128 patients (36%) had clinically significant improvement after 6 months of pharmacotherapy. No history of psychiatric disorders (odds ratio [OR] 0.479 [95% confidence interval {CI}: 0.262–0.875], p=0.017) and longer duration of illness (>18 months) (OR 2.626 [95% CI: 1.437–4.799], p=0.002) were significant factors for clinical outcomes.
Conclusion: Patients with oral cenesthopathy in our clinic were predominantly elderly female patients. Dental treatment in the acute phase of depression might be a risk factor for oral cenesthopathy. Therefore, comprehending the situation of psychiatric disorder and obtaining adequate informed consent might be required to prevent the trouble concerning oral cenesthopathy.
Keywords: oral cenesthopathy, delusional disorder somatic type, DDST, chart review, dentistry
Introduction
Cenesthopathy is characterized by foreign body sensations despite the lack of any medical evidence for them.1,2 Oral cavity is the most affected region of cenesthopathy, and it is called “oral cenesthopathy,”3–5 “oral somatic delusions,” or “oral dysesthesia.”6 There are various complaints of oral cenesthopathy. Some patients complain of unusual oral sensations, such as excessive mucus secretion or a slimy sensation, and others complain of a bizarre oral sensation, such as a feeling of coils or wires being present within the oral region. Patients commonly have an unshakable conviction that some foreign body is existing in their mouths. They often spend hours each day examining their mouth and sometimes try to catch the foreign body. To prove the abnormal sensations to be real, they sometimes show “the specimen sign:”7 taking specimens such as saliva or dental plaque and collecting them in a bottle or plastic case (Figure 1). Sometimes the patients with oral cenesthopathy had other comorbid psychosomatic oral symptoms including burning mouth syndrome (BMS). Normally oral cenesthopathy does not induce pain symptom, which is different from BMS.
The patients tend to avoid seeing psychiatrists even if the dentists suggest to visit them, because they have a firm conviction that the foreign body is real. When the complaints are obviously a delusion or hallucination developed by psychotic diseases, it is not difficult for dentists to consult the patients to psychiatrists. However, many patients without obvious psychotic diseases exist in dental clinics seeking treatment to remove the foreign body.6
In such situations, it is said that oral cenesthopathy is a rare disorder, and most of the cases are a secondary symptom of depression or schizophrenia; however, such studies were reported by psychiatrists.8–10 From the viewpoint of psychiatry, the oral symptoms were sometimes suspected as a side effect of prescription drugs. Even though the clinical features of oral cenesthopathy might be different between a psychiatric clinic and a dental clinic, to the best of our knowledge, there has been no clinico-statistical study from dentists. To delineate the clinical features of oral cenesthopathy in dentistry, we herein report a clinico-statistical study on the patients with oral cenesthopathy in our clinic.
Patients and methods
Data collection and ethical approval
Data for individual patients diagnosed as having oral cenesthopathy in our clinic between April 2010 and March 2015 were retrospectively and consecutively collected. Oral cenesthopathy was diagnosed by a specialist in psychosomatic dentistry who had examined the patients over 25 years and certified by Japanese society of psychosomatic dentistry (AT). The inclusion criteria were as follows: 1) an outpatient of our clinic, 2) complaining of a bizarre or strange sensation in the mouth, and 3) absence of corresponding abnormal findings from a dental panoramic radiograph and intra- and-extra-oral examination. Patients who did not give us the written consent for this study were excluded.
Epidemiological profiles, features of symptoms, original referrer, comorbid oral psychosomatic disorders, and psychiatric history were documented. In the features of symptoms, we checked the trigger, the reason which the patients think to develop the symptom of oral cenesthopathy. State of depression at the onset of oral cenesthopathy was checked if the patients had a history of depression. The diagnosis of psychiatric disorders and state of depression were investigated by obtaining referral letters from the psychiatrists. The outcomes of our treatments were also documented if the patients continued to visit our clinic.
This study is approved by the institutional review boards of Tokyo Medical and Dental University dental hospital (approval number: 356). Written informed consent was provided by all patients before the study.
Treatment protocol and assessment
Psychotherapy and pharmacotherapy are the mainstream treatments for oral cenesthopathy. Antidepressants and antipsychotic drugs were prescribed in our clinic depending on the patients’ symptoms, medical complications, former reports,11–16 personality features, and background such as lifestyle, habits, income, opportunity, and family relationships. If dental treatment was needed during our treatment, their family dentists or attending dentists in our clinic (YU, AM, YS, LM, SS, KK, TT, TW, TS, MW, MT, and TY) treated them while confirming their symptoms. In cases where the patients had primary psychiatric disorders, we contacted their psychiatrist and observed their symptoms every 1–3 months, as possible. When severe psychiatric disorders were developed during our treatment, we consulted the psychiatrists who cooperated.
The relationship between oral cenesthopathy and depression was classified into three types: 1) “onset after depression,” the onset of oral cenesthopathy was during depression treatment; 2) “simultaneous,” the onsets of oral cenesthopathy and depression were simultaneous; and 3) “onset before depression,” the depression developed after the onset of oral cenesthopathy. In addition, the “onset after depression” group was divided into two subgroups if the onset of oral cenesthopathy was during the “acute phase” or “recovery phase” of depression, which were assessed by referral letters from attending psychiatrists.
We defined “acute phase” in this study as the period when the symptoms of depression were aggravated or not stable and with repeated fluctuation. The prescriptions were not fixed as well. Likewise, “recovery phase” was defined as the period when no or mild residual symptoms of depression were observed due to the effective treatment.
The outcomes were assessed by each attending dentist by using the clinical global impression improvement scale (CGI-I)17 after 6 months of treatment. CGI-I scores range from 0 to 7 (0, not assessed; 1, very much improved; 2, much improved; 3 minimally improved; 4, no change; 5, minimally worse; 6, much worse; and 7, very much worse). CGI-I scores were calibrated before evaluation among the raters. CGI-I scores of 1 and 2 were thought to be a clinically significant improvement.
Statistical analysis
Mann–Whitney U test and chi-square test were used for comparing each variable. A chi-square test was used for the association between the trigger of oral cenesthopathy and the phase of depression. Logistic regression analysis was performed to detect the clinical factors for a good outcome. Sex, age at the time of onset, duration of illness, expression of the symptom, psychiatric history, and trigger of the symptom were selected for inclusion in the binomial logistic regression analysis. All analyses were performed with PASW 17.0 software (IBM Corporation, Armonk, NY, USA). p-values of <0.05 were considered as statistically significant.
Results
Demographic data
Table 1 shows the demographic and clinical characteristics of the patients. In total, 606 patients were included in this study of which 159 were male and 447 female patients. The mean ages were 62.08 years in total, 58.69 years in the male patients, and 63.28 years in the female patients. The distributions of the male and female patients are shown in Figure 2. The mean duration of illness at the time of first examination was 40.12 months. As to the comorbidity of other psychosomatic dental symptoms, BMS, atypical odontalgia, phantom bite syndrome, and halitophobia were seen in 159 patients (26%), 35 patients (6%), 27 patients (4%), and 4 patients (1%), respectively, including multiple diagnosis. There were various original referrers. Family physicians were the most common (n=253), followed by psychiatry (n=245), otorhinolaryngology (n=35), surgery (n=28), neurology (n=19), ophthalmology (n=11), gynecology (n=8), other departments (n=7), and nothing (n=22) including multiple referrers.
  | Table 1 Demographic and clinical characteristics of patients |
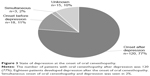
As to the psychiatric comorbidity, which was described in the referral letter, patients with no history of psychiatric disorder were the most common (38%). Psychotic disorders including schizophrenia and bipolar disorder were only 6%. Although depression was seen in 26%, almost all of them were in recovery phase. With regard to the trigger of the symptom, “spontaneous” was seen in 379 patients (63%), “dental treatment” was 181 patients (30%), and “the others” were 46 patients (8%). “The others” included drug change and intra-oral change such as stomatitis, traffic accident, and surgical treatment outside of the oral region. With regard to the “dental treatment,” various treatments including tooth extraction (n=38), dental implants (n=21), prosthodontic treatment (n=49), restoration (n=21), endodontics (n=14), periodontics (n=18), bite adjustment (n=8), and other treatments (n=12) were described (Table 2).
  | Table 2 Details of the dental treatments that are considered to trigger the symptoms |
There were various symptoms. Some foreign body sensation was seen in 208 patients (34.3%). A sticky sensation, rough sensation, and sucking sensation were seen in 221 (36.5%), 54 (8.9%), and 64 patients (10.6%), respectively. Taste disturbance and dry mouth which were self-reported were seen in 204 (33.7%) and 120 patients (19.8%), respectively.
Male–female comparison
To assess the differences between male and female patients, each variable, which is mentioned above, was analyzed (Table 3). Mean age, mean duration of illness, number of other comorbid psychosomatic oral symptoms with oral cenesthopathy, number of comorbid psychiatric disorders, and number of onsets with dental treatment were compared between male and female patients. A Mann–Whitney U test revealed that the female patients were significantly older than male patients (p=0.001), and a Pearson’s chi-square test showed that the frequency of other comorbid psychosomatic oral symptoms was significantly higher in the female patients (p=0.0005).
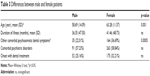  | Table 3 Differences between male and female patients |
Young–old comparison
In addition, to assess the differences between young and old patients, each variable was analyzed, using age =60 years as the cutoff value. Sex, mean duration of illness, number of onsets with dental treatment, number of comorbid psychiatric disorders, and symptoms were compared. A Pearson’s chi-square test revealed that being female (p=0.017) and a sticky sensation were significantly dominated in elderly patients (p=0.003). Also, the differences between the patients of early onset and the other patients were scrutinized. The patients whose onset of the symptom were at an age of <30 years were male dominant (p<0.001) and complaining sucking sensation (p<0.001) but neither sticky sensation (p=0.003) nor taste disturbance (p=0.033), compared to the other patients.
Obviously bizarre complaints and relatively understandable complaints
Another interesting point is differences in the themes of delusions of cenesthopathy. The contents of delusions vary from patient to patient. Some patients have obviously bizarre delusional complaints such as “a moving coil in the oral cavity,” so any doctor or dentist can easily notice their strange contents. On the other hand, other patients complain that saliva or bubbles, normally existing in the oral cavity, are extraordinary in some ways, so some doctors or dentists may not notice their delusions. Then, we divided the patients into two groups (patients with obviously bizarre complaints and others) with respect to the content of complaints and compared them. Of the 606 cases, 211 patients had obviously bizarre delusional complaints. As to clinical factors such as age (p=0.188, non significant [ns]), sex (p=0.792, ns), duration of illness (p=0.352, ns), comorbid psychiatric disorders (p=0.898, ns), and onset of the symptom (p=0.271, ns), no significant differences were detected between the two groups. Furthermore, the treatment outcomes of both the groups were compared. In patients with obviously bizarre complaints, 41 patients were improved and 78 were unimproved, whereas in other patients, 87 patients were improved and 146 were unimproved. A Pearson’s chi-square test revealed no significant difference between the two groups (p=0.64, ns).
Relationship between the trigger of oral cenesthopathy and depression phase at onset
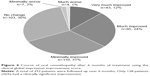
Because depression is the most common disease among comorbid psychiatric disorders, we next focused on the relationship between the onset of oral cenesthopathy and the state of depression. Referring to the referral letter, patients who were comorbid with depression were classified into four types: “onset after depression,” “simultaneous,” “onset before depression,” and “unknown.” More than three quarters of cenesthopathic patients with depression developed the oral symptoms during depression treatment (n=120, 77%). “Onset before depression,” “simultaneous” onset, and “unknown” were seen in 11%, 2%, and 10%, respectively (Figure 3). In the “onset after depression” group, 80 patients were in “recovery phase,” and 40 patients were in “acute phase” at the time of onset of oral cenesthopathy.
A Pearson’s chi-square test between the trigger of the symptom (spontaneous and dental treatment) and the history of depression (depression and no psychiatric history) showed no significant difference (p=0.49, ns). On the other hand, a Pearson’s chi-square test between the trigger of the symptom (spontaneous and dental treatment) and the phase of depression at the onset (recovery and acute phase) detected a significant difference (p=0.037) (Table 4).
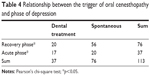  | Table 4 Relationship between the trigger of oral cenesthopathy and phase of depression |
Logistic regression analysis of treatment outcomes
Next, the clinical outcomes after 6 months of treatment were analyzed using the CGI-I score (Figure 4). A total of 352 patients could be followed up over 6 months. Only 128 patients (36%) had clinically significant improvements. In line with former studies, the overall outcomes were not satisfactory. Logistic regression analysis revealed that no history of psychiatric disorder (odds ratio [OR] 0.479 [95% confidence interval {CI}: 0.262–0.875], p=0.017) and longer duration of illness (>18 months) (OR 2.626 [95% CI: 1.437–4.799], p=0.002) were significant factors for clinical outcomes (Table 5). Therefore, any history of psychiatric disorder and longer duration of illness over 18 months are significant risk factors for a poor prognosis. The reliability of this binomial logistic regression analysis was checked with the Hosmer and Lemeshow test (p=0.306).
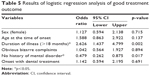  | Table 5 Results of logistic regression analysis of good treatment outcome |
Effective drugs for oral cenesthopathy
Of the aggregate data from improved patients whose CGI-I score were 1 or 2, 94 patients were prescribed in our department and the rest of them (n=34) were prescribed by their attending psychiatrist. The most prescribed medicine was aripiprazole (n=56) including monotherapy and combination therapy. The mean dosage of aripiprazole was 1.52 mg/day. In some cases, mirtazapine (n=15), amitriptyline (n=9), perospirone (n=1), tetracyclic antidepressants (n=9), SNRI (n=5), and SSRI (n=6) were effective.
Discussion
In this retrospective study, we described the epidemiological and clinical features of oral cenesthopathy, the risk factors for the onset of oral cenesthopathy, the outcomes, and the risk factors for a poor prognosis. It is the first retrospective chart review for oral cenesthopathy in dentistry. The patients in this study maintained enough social skills to come to our clinic regularly as scheduled, though some of them had comorbid psychiatric disorders.
Patients with oral cenesthopathy in our clinic were predominantly elderly female patients. The mean age was 62 years, and the male patients were significantly younger than female patients. In a study4 for oral cenesthopathy consisting of three men and 25 women, the mean age was 55.1 years. A review18 collecting several studies of cenesthopathy, including that outside of the oral region, reported that oral symptoms are more frequent in patients aged >40 years and are more common in female patients in this age group. The gross distribution of the present study was similar to former studies. Compared to other clinical entities similar to oral cenesthopathy, such as delusional infestation or delusional parasitosis, which was reported to be observed in elderly patients who were aged >50 years, male patients were younger than female patients. In addition, other comorbid psychosomatic dental symptoms were more common in female patients. This seemed to be due in part to the biological characteristics of psychosomatic oral symptoms, which were originally female dominant.19
There are various symptoms: some patients complained that a real object such as a wire, metal, or finger was existing, and others complained of the feeling of something about to spout out or a spontaneous taste. From the viewpoint of psychiatry, only obviously delusional complaints tend to be regarded as oral cenesthopathy, so such a large number of oral cenesthopathy patients in this study might be difficult to believe. In our clinic, however, not just delusional but bizarre complaints such as “excessive saliva secretion” and “a sticky sensation in the mouth” were included in oral cenesthopathy. These complaints are commonly understandable, so psychiatrists do not have the chance to see such patients. Assuming psychiatrists see such patients, the two types of complaints (obviously delusional/relatively understandable) might be classified under different diagnosis (somatic delusion/somatic symptom disorder). But they are bizarre enough to be diagnosed as oral cenesthopathy based on our clinical experience. In fact, no significant differences were detected between the delusional complaints and other factors including sex, age, and history of depression. Moreover, the complaints did not reflect the treatment outcome at all. Therefore, the expression of complaints might not indicate the category in oral cenesthopathy. The obviously bizarre complaints did not necessarily anticipate a worse clinical course. Thus, although patients with oral cenesthopathy complain of various clinical symptoms, from an apparently abnormal experience that no one can believe, seemingly to a usual malfunction such as excessive mucus secretion or a slimy sensation, they essentially seem to be categorized into the same disease. Originally, it is difficult to categorize oral cenesthopathy using the Diagnostic and Statistical Manual of Mental Disorders, Fifth edition (DSM5).20 Delusional disorder, somatic type (DDST) is the best category for oral cenesthopathy so far, but it does not fit this disorder satisfactorily. DDST is the only one that was not included in Kraepelin’s original description of paranoia,21 and no discussion was made about whether oral cenesthopathy should be described as delusion or not. In Europe, delusional parasitosis is generally believed to represent a primary hallucination with an accompanying secondary delusion that explains the sensory perception, whereas in the United States, the sensory phenomena associated with delusional parasitosis are viewed as components of a systematized and encapsulated delusion.21 Most of our patients seem to be polite and have no problem in their social skills or interpersonal relationships. They usually complain about their strange symptoms plangently or in a detached tone and ask us to remove their troublesome sensations. Also, they occasionally notice that their complaints are very strange and unacceptable to others.
Intuitively, they try to express their strange perception in the oral cavity as precisely as possible, sometimes resulting in showing “the specimen sign” in order to explain. Thus, some patients with oral cenesthopathy in our clinic might have a perceptual dysfunction (illusion or hallucination) rather than delusion. In fact, our study, which revealed the asymmetrical regional cerebral blood flow (rCBF) between the right and left side,22 might suggest a micro disorder in a sensory pathway. Therefore, some patients with oral cenesthopathy, at least in our clinic, might be appropriate to be categorized into “organic hallucinosis (F06.0 in ICD-10)” rather than “delusional disorder, somatic type (DDST).”
Around 40% of patients in this study had no psychiatric histories. Moreover, while some patients had a history of depression, they were mostly in remission at the time of onset of oral cenesthopathy. Therefore, oral cenesthopathy might not be merely a partial symptom of psychotic disorder that presents delusional symptoms, as we previously mentioned in a case report.11 Hozaki23 reported that cenesthopathy without psychiatric disorders is rare. In the present study, oral cenesthopathy without psychiatric disorder was not rare, which might be because of the difference of clinical setting between dentistry and psychiatry. Accordingly, our data are likely to reflect the patients’ characteristics, which actually distress the dentists. Interestingly, as to delusional infestation, which is experienced mainly by a dermatologist, it is consistent with our data that ~40% of patients are pure cases that are not the secondary symptoms of psychiatric diseases.24,25
One of the most important findings of dentists in the present study is that dental treatments in the acute phase of depression might be a risk factor for oral cenesthopathy, as suggested in Table 3. Oral cenesthopathy is known to be so intractable that we have only a 36% treatment efficacy. Other psychosomatic oral symptoms such as BMS and atypical odontalgia are still treatable, but some refractory cases still exist. Therefore, to prevent the trouble concerning psychosomatic oral symptoms, comprehending the situation of the psychiatric disorder and obtaining adequate informed consent are required.
Under the clinical entity of DDST, some case reports and reviews suggested that antidepressants, antipsychotic drugs, and electroconvulsive therapy (ECT) are effective. When only the oral symptoms are present, paroxetine,12 fluvoxamine,13 amitriptyline,13,14 sulpiride,14 risperidone,13,15 olanzapine,13 perospirone,11 aripiprazole,16 and ECT11,26 were reported to be effective. In this study, aripiprazole was the most effective medicine, especially in low doses. At the same time, various drugs including amitriptyline, mirtazapine, and other antidepressants were also effective in some cases. The disproportionality of the drug response may suggest the heterogeneity of a clinical entity of DDST. Any history of mental disorder and a duration of illness over 18 months, which were detected as significant risk factors for clinical course using binomial logistic regression analysis, and onset age might be factors for classifying oral cenesthopathy or DDST into clinically meaningful disease units.
We recently found the asymmetrical rCBF pattern between the right and left hemispheres with right side dominance using single-photon emission computed tomography.22 The asymmetrical rCBF pattern was common regardless of the comorbidity of depression.27 However, as discussed in the studies, heterogeneity may again have existed in this clinical entity, because the asymmetrical rCBF pattern was also not homogeneous in the research. More studies that combine clinical data and brain imaging are needed to understand oral cenesthopathy better.
This study has several limitations. Because the psychiatric history was collected by referral letter and our examination, some psychiatric disorders may have remained undiagnosed. However, as shown in the “Results” section, almost all patients brought the referral letter, and we consulted with a psychiatrist about suspicious patients. Hence, the hidden psychiatric disorders may be few. Another limitation of this study is the duration of illness which was 40.12 months. This long duration might increase the number of the patients with histories of depression. But the number of patients whose depression was developed after the onset of oral cenesthopathy is not frequent.
Conclusion
Patients with oral cenesthopathy in our clinic were predominantly elderly female patients, and there were various complaints. Considering the psychiatric history, oral cenesthopathy might not be merely a partial symptom of psychotic disorders that present delusional symptoms. Dental treatment in the acute phase of depression might be a risk factor of oral cenesthopathy. Therefore, comprehending the situation of psychiatric disorder and obtaining adequate informed consent might be required to prevent the trouble concerning oral cenesthopathy. Not only dentists but also the psychiatrists should be aware of this. Further research studies using brain imaging and reliable assessment tools are warranted.
Acknowledgment
This work was supported by JSPS KAKENHI Grant Number JP18K17306.
Disclosure
The authors report no conflicts of interest in this work.
References
Dupré E, Camus P. Les cénesthopathies. [The Cenesthopathies]. Encéphale. 1907;2:616–631. French. | ||
Graux J, Lemoine M, Gaillard P, Camus V. Les cénesthopathies: un trouble des émotions d’arrière plan. Regards croisés des sciences cognitives et de la phénoménologie [Cenesthopathies: a disorder of background emotions at the crossroads of the cognitive sciences and phenomenology]. Encephale. 2011;37(5):361–370. French. | ||
Umezaki Y, Miura A, Watanabe M, et al. Oral cenesthopathy. Biopsychosoc Med. 2016;10:20. | ||
Honma F, Kimura M, Endo S, Ohtsu M, Okada T, Satoh T. Oral cenesthopathy examined by Rorschach test. Psychiatry Clin Neurosci. 2006;60(2):154–159. | ||
Uezato A, Toyofuku A, Umezaki Y, et al. Oral dysesthesia rating scale: a tool for assessing psychosomatic symptoms in oral regions. BMC Psychiatry. 2014;14(1):1696. | ||
Spencer CJ, Klasser GD. Oral dysesthesia: a perplexing problem for practitioners. J Am Dent Assoc. 2017;148(12):941–945. | ||
Freudenmann RW, Lepping P, Huber M, et al. Delusional infestation and the specimen sign: a European multicentre study in 148 consecutive cases. Br J Dermatol. 2012;167(2):247–251. | ||
Wake Y, Fujiwara Y, Aoki S, Kuroda S. Clinical character of cenesthopathy located in oral cavity. Seishin Igaku (in Japanese). 1998;40(4):437–440. | ||
Miyachi H, Wake H, Mitsuhashi A, Tamaki K, Yoshida Y, Miyaoka H. Oral cenesthopathy in the elderly. Rounenseisinigakuzasshi (in Japanese). 2009;20(2):160–164. | ||
Yoshimatsu K. The psychopathology of cenesthopathia. Seishinshinkeigaku zasshi (in Japanese). 1966;68:872–890. | ||
Uezato A, Yamamoto N, Kurumaji A, et al. Improvement of asymmetrical temporal blood flow in refractory oral somatic delusion after successful electroconvulsive therapy. J ECT. 2012;28(1):50–51. | ||
Hayashi H, Oshino S, Ishikawa J, Kawakatsu S, Otani K. Paroxetine treatment of delusional disorder, somatic type. Hum Psychopharmacol. 2004;19(5):351–352. | ||
Nemoto K, Mizukami K, Hori T, et al. Hyperperfusion in primary somatosensory region related to somatic hallucination in the elderly. Psychiatry Clin Neurosci. 2010;64(4):421–425. | ||
Hanihara T, Takahashi T, Washizuka S, Ogihara T, Kobayashi M. Delusion of oral parasitosis and thalamic pain syndrome. Psychosomatics. 2009;50(5):534–537. | ||
Akahane T, Hayashi H, Suzuki H, Kawakatsu S, Otani K. Extremely grotesque somatic delusions in a patient of delusional disorder and its response to risperidone treatment. Gen Hosp Psychiatry. 2009;31(2):185–186. | ||
Umezaki Y, Uezato A, Toriihara A, Nishikawa T, Toyofuku A. Two cases of oral somatic delusions ameliorated with brain perfusion asymmetry. Clin Neuropharmacol. 2017;40(2):97–99. | ||
Guy W, editor. ECDEU Assessment Manual for Psychopharmacology. Rockville, MD: US Department of Heath, Education, and Welfare Public Health Service Alcohol, Drug Abuse, and Mental Health Administration; 1976. | ||
Takahashi T, Fuke T, Washizuka S, Hanihara T, Amano N. A review of recent case reports of cenesthopathy in Japan. Psychogeriatrics. 2013;13(3):196–198. | ||
Watanabe M, Katagiri A, Umezaki Y, et al. Clinico-statistical Study on 1210 outpatients examined at the department of Psychosomatic Dentistry (2009–2011). Jpn J Psychosom Dent (in Japanese). 2012;27(1,2):37–43. | ||
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Washington, DC: American Psychiatric Association; 2013. | ||
Fennig S, Forchtmann LJ, Bromet EJ. Kaplan & Sadock’s Comprehensive Textbook of Psychiatry. 8th ed. Sadock BJ, Sadock VA, editors. Philadelphia, PA, USA: Lippincott Williams & Wilkins; 2005. | ||
Umezaki Y, Katagiri A, Watanabe M, et al. Brain perfusion asymmetry in patients with oral somatic delusions. Eur Arch Psychiatry Clin Neurosci. 2013;263(4):315–323. | ||
Hozaki H. Cenestopathia and related condition. Seishin Igaku (in Japanese). 1960;2:325–332. | ||
Trabert W. 100 years of delusional parasitosis. Meta-analysis of 1,223 case reports. Psychopathology. 1995;28(5):238–246. | ||
Lepping P, Huber M, Freudenmann RW. How to approach delusional infestation. BMJ. 2015;350:h1328. | ||
Ota M, Mizukami K, Katano T, Sato S, Takeda T, Asada T. A case of delusional disorder, somatic type with remarkable improvement of clinical symptoms and single photon emission computed tomograpy findings following modified electroconvulsive therapy. Prog Neuropsychopharmacol Biol Psychiatry. 2003;27(5):881–884. | ||
Watanabe M, Umezaki Y, Miura A, et al. Comparison of cerebral blood flow in oral somatic delusion in patients with and without a history of depression: a comparative case series. BMC Psychiatry. 2015;15:42. |
 © 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.