Back to Journals » International Journal of Women's Health » Volume 6
Burden of menstrual symptoms in Japanese women – an analysis of medical care-seeking behavior from a survey-based study
Authors Tanaka E, Momoeda M , Osuga Y, Rossi B , Nomoto K, Hayakawa M, Kokubo K, CY Wang E
Received 3 August 2013
Accepted for publication 26 September 2013
Published 17 December 2013 Volume 2014:6 Pages 11—23
DOI https://doi.org/10.2147/IJWH.S52429
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Erika Tanaka,1 Mikio Momoeda,2 Yutaka Osuga,3 Bruno Rossi,4 Ken Nomoto,5 Masakane Hayakawa,5 Kinya Kokubo,6 Edward CY Wang1
1Health Economics and Outcomes Research, Bayer Yakuhin Ltd, Tokyo, Japan; 2Department of Integrated Women's Health, St Luke's International Hospital, Tokyo, Japan; 3Department of Obstetrics and Gynecology, Faculty of Medicine, The University of Tokyo, Tokyo, Japan; 4Market Access, Bayer Yakuhin Ltd, Osaka, Japan; 5Medical Affairs Women's Health and Dermatology, Bayer Yakuhin Ltd, Osaka, Japan; 6Consumer Goods/Service and Healthcare Industry Consulting Department, Nomura Research Institute, Tokyo, Japan
Background: Menstrual symptoms are associated with various health problems in women of reproductive age, and this may impact their quality of life. Despite this, Japanese women are likely to hesitate seeking a specialist's medical help for their menstrual symptoms.
Purpose: To study subject parameters including symptom severity, gynecological disorders, and treatments in medical care-seeking women (outpatient) and women opting for self-care (nonvisit), to identify reasons why Japanese women do not see a gynecologist, and to document the benefit of gynecologist visits by assessing the impact on women's daily lives.
Methods: Two online surveys were conducted among women aged 15–49 years. Sampling was structured to approximate the age and geographic distribution in Japan. Results of the first survey and part of the second survey on the overall current burden of menstrual symptoms are reported in a separate publication. Further outcomes from the second survey reported in this paper included data from the outpatient (n=274) and nonvisit (n=500) groups on symptom severity, gynecological disorders, medical treatment use, reasons for not seeking medical care, and the improvement of daily life.
Results: The outpatient group tended to have greater symptom severity compared to the nonvisit group. Uterine fibroids, dysmenorrhea, endometriosis, and premenstrual syndrome were the most commonly self-reported diagnoses, and oral contraceptives were frequently prescribed at gynecologist visits. Nonvisit group subjects felt that gynecologist consultations were unnecessary or felt resistant to them. Daily life was significantly improved after medical treatment from a gynecologist visit with associated economic savings, whilst the nonvisit group had no change after taking over-the-counter drugs to relieve their menstrual symptoms.
Conclusion: The present study results indicate that Japanese women who were suffering from menstrual symptoms could benefit from visiting a gynecologist for easing their symptoms, hence improving their daily life.
Keywords: menstrual symptoms, burden, outpatient, care-seeking, MDQ score, patient reported outcome
Introduction
For women of reproductive age, menstrual symptoms present a burden that is often underestimated and not extensively researched.1–3 Many women experience menses-associated health problems, such as menstrual pain (dysmenorrhea), heavy menstrual bleeding, and premenstrual syndrome (PMS), during reproductive age.4 The prevalence of menstrual pain, a major symptom of dysmenorrhea, can range from 25% (among all women) to as high as 90% (among adolescents).5 Menstrual pain is the most common gynecological complaint in women who have menstruation.5 Heavy menstrual bleeding is also a common complaint; it may be defined as excessive menstrual blood loss. Prevalence rates of heavy menstrual bleeding range between 4%–52%, depending on whether an objective or subjective assessment is performed;1 yet, when measured objectively (a menstrual blood loss of greater than 80 mL), it has been found to be 10%.6
Among adolescent girls with dysmenorrhea, less than 15% seek medical help, even though their symptoms interfere with their daily lives. More than one-third do nothing about their condition.7,8 A similar ratio of women from other age groups seek medical help. In a large survey-based research study in 2001 of more than 4,000 Japanese women of reproductive age by Taketani, 12% of the surveyed women sought a clinician’s help for their menstrual pain.9 Most women (67%) indicated that their symptoms did not impact their social life, because they felt it was natural to experience pain.9 This perception may play a part in the low consultation rate for menstrual problems in Japan.
In the current study, two surveys were conducted to assess the burden of menstrual symptoms in Japanese women of reproductive age. In the first publication, we reported results from the first survey of 19,254 Japanese women focusing on the current burden, including impact on daily life and work productivity as well as from the second survey to estimate the economic burden.10 Results showed that, despite the large proportion of women (74%) suffering from menstrual symptoms including pain and heavy bleeding that interfered with their daily lives, only 20% visited a gynecologist. The greater severity of menstrual symptoms was directly related to more visits to a gynecologist and greater work productivity loss, which led to a significant economic burden to society. Results clarified that most of the over-the-counter (OTC) drugs used by all menstruating women were analgesics, indicating that relieving menstrual pain was the most common reason for the use of OTC drugs.10 However, menstrual symptoms are associated with other health problems beyond pain, such as heavy menstrual bleeding. Some symptoms may also be indicative of more serious conditions, such as endometriosis or uterine fibroids, which require medical attention. Thus, it is important for women who are experiencing menstrual problems to consult a gynecologist as this can improve their patient outcomes and, hence, their quality of life.
Subsequent to our first publication, the current paper reports on the additional outcomes of the second survey. Specifically, it provides: 1) a detailed account of the subject parameters, such as symptom severity, gynecological disorders, and treatments, for two subgroups – the group seeking medical care (outpatient) and the group opting for self-care (nonvisit); 2) an assessment of the women’s perceptions of gynecologist visits; and 3) documentation of the benefit of gynecologist visits for women who suffer from menstrual symptoms by assessing the impact on their daily lives.
Methods
Surveys
Two online surveys were conducted from May 2011–June 2011 (Figure 1). In the first survey (N=21,477) conducted in May 2011 and reported elsewhere, we assessed the current overall burden.10 Japanese women aged 15–49 years who were registered in TrueNavi, an online panel fielded by Nomura Research Institute Ltd. (Tokyo, Japan), were sampled according to the age and geographic distribution of the female population in Japan.11 TrueNavi was selected for its large number of potential respondents and its frequent use in the health care field, with an average of approximately ten surveys conducted each year. The relevance of direct-to-patient health surveys using an online panel to collect medical record data and patient-reported outcomes has been previously reported.12
  | Figure 1 Methodology of the first and second surveys. |
Methodology of the first and second surveys
The first survey, reported in a separate publication,10 collected the following information: characteristics of menstruation; treatments in outpatient visits; OTC product use including analgesics, sleeping pills, minor tranquilizers for reducing irritability and tension, Traditional Chinese Medicine (TCM), supplements and vitamins; and impact of menstrual symptoms on work (Figure 1). Menstrual symptoms were defined by the six domains of the Japanese modified Menstrual Distress Questionnaire (mMDQ) and one question on self-reported menstrual bleeding.10
The second survey, reported in both the first publication and this paper, was conducted in June 2011. Subjects were categorized into two groups – the outpatient group and the nonvisit group – based on their first survey responses for visiting a gynecologist. Data were analyzed regarding the severity of menstrual symptoms, gynecological disorders, medical treatments used, reasons for not seeking medical care, and the improvement of daily life by the treatment of menstrual symptoms. In addition, willingness-to-pay to eliminate menstrual symptoms and their interference with daily life, as well as cervical cancer screening, were assessed.
Assessment by the mMDQ
A 35-item Japanese mMDQ was used to assess symptom severity. The questionnaire includes six domains: Pain (six items), Concentration (eight items), Behavioral Change (five items), Autonomic Reactions (four items), Water Retention (four items), and Negative Affect (eight items).
The original MDQ was developed to assess menstrual symptomatology during menstrual flow, the week before menstrual flow, and the remainder of the cycle. Response options consist of a six-point scale ranging from no experience of the symptom to an acute or partially disabling experience of the symptom, where higher scores indicate greater distress.13,14 It was reported that two domains, Arousal and Control, were less relevant for the Japanese population in previous research15,16 and, therefore, were excluded in the modified version of the questionnaire for this study.
To maintain consistency of the recall period across the surveys administered in this research, subjects were asked to complete the mMDQ based on their menstrual and premenstrual experience in the prior 3 months, where the premenstrual period was defined as 3–10 days before menstruation. The severity of menstrual symptoms was defined by four severity groups, based on a total score distribution of the summed premenstrual and menstrual cycle mMDQ scores: “very strong” (top 10th percentile of the summed score distribution, where the actual range of the summed score was 215 and above), “strong” (top 10th–25th percentile of the score distribution, where the actual range of the summed score was 148–214), “slightly strong” (top 25th–50th percentile of the score distribution, where the actual range of the summed score was 103–147), and “moderate and below” (lower 50th percentile of the score distribution, where the actual range of the summed score was 102 points and less).
Subject categories
Subjects were resampled and categorized into two groups as described below. The study initially targeted 500 subjects per group.
Outpatient group
Of the 19,254 subjects who reported having menses at the time of the first survey (reported in a separate publication10), 677 subjects met the following inclusion criteria for the outpatient group and were asked to complete the second survey:
- responded to the first survey that they visited a gynecologist within the prior 3 months; and
- received drug treatment for menstrual symptoms from a gynecologist within the prior 3 months.
Of those 677 subjects, survey responses were collected from 510 subjects among whom 236 subjects were disqualified from further analyses for the following reasons:
- subjects did not have menses;
- subjects visited a gynecologist for reasons other than for menstrual symptoms;
- subjects reported drug treatments for menstrual symptoms used in the prior 4 months or longer, and no drug treatments for menstrual symptoms were used within the prior 3 months; or
- there were discrepancies in the municipality category that the subjects belonged to, between the first and second survey responses.
As a result, the remaining 274 subjects were included in the analyses for the outpatient group.
Nonvisit group
Of the 19,254 subjects with menses, 741 subjects met the following inclusion criteria for the nonvisit group and were asked to complete the second survey:
- took OTC analgesics for menstrual symptoms within 3 months of the survey or had heavy menstrual bleeding that interfered with or limited daily activities;
- had not visited a gynecologist within the prior 3 months despite having menstrual symptoms; and
- missed at least one day of work due to menstrual symptoms within the prior 3 months.
Of those 741 subjects, survey responses were collected from 602 subjects among whom 92 subjects were excluded from further analyses because of discrepancies between the first and second survey responses in:
- the type of OTC drug used within the prior 3 months (ie, analgesic, sleeping pill, minor tranquilizer or TCM); or
- the municipality category that subjects belonged to.
In addition, 500 of the remaining 510 subjects were randomly sampled and included in the analyses for the nonvisit group as originally planned.
Subject characteristics
The age, employment status, annual income, individual expenditure excluding living expenses, and cervical cancer screening rates were reported.
Clinical outcomes and treatment use
The severity of menstrual symptoms based on the mMDQ was reported in both groups. Subjects in the outpatient group were asked to report diagnoses of menstrual-related conditions and prescribed drug treatments, using a multiple-choice method. OTC analgesic use for menstrual pain was reported in both groups.
Reasons for not seeking medical care: nonvisit group
Reasons why nonvisit subjects did not consult a gynecologist for their menstrual symptoms were assessed using a multiple-choice method.
Improvement of daily life by the treatment of menstrual symptoms
The impact of menstrual symptoms on the inhibition and limitation of the subjects’ daily lives was assessed by asking the following questions:
- Outpatient group: Before visiting your gynecologist (taking medication), to what extent did your menstrual symptoms interfere with or limit your daily life?
- Nonvisit group: Before taking OTC drugs or supplements, to what extent did your menstrual symptoms interfere with or limit your daily life?
- Outpatient and nonvisit groups: Now, to what extent do your menstrual symptoms interfere with or limit your daily life?
Each of these three questions had five response options, including “not at all,” “minimally,” “uncertain,” “quite a bit,” and “a great deal.” Responses to the above mentioned third question asking the impact on daily life “now” were assumed to reflect the interference with daily life after visiting a gynecologist (outpatient group) or self-medicating with OTC drugs (nonvisit group), as a comparison to the preceding questions. A hypothetical calculation was performed to estimate women’s economic savings that were associated with gynecologist visits, using the percentage of improvement in daily life (Supplementary materials).
Willingness-to-pay
Willingness-to-pay was assessed by asking the following questions, where subjects were allowed free-text responses to indicate the amounts they would pay:
- If a medicine exists that would improve all your menstrual symptoms and their interference with daily life, then how much is the maximum amount per month you would pay for it?
- If a medicine exists that would eliminate all menstrual symptoms, then how much is the maximum amount per month you would pay for it?
Statistical analyses
Data were descriptive in nature. The online survey was not designed to match between the outpatient and nonvisit groups. There were differences in demographic and clinical characteristics between them; therefore, statistical significance between the groups was not assessed. However, within-group statistical testing was conducted for the subjects reporting impact on daily life (defined to be the sum of subjects reporting “a great deal” and “quite a bit” of interference with daily life). The impact on daily life was compared before and after the subjects received drugs at gynecologist visits (outpatient group) and separately for the self-medicating group using OTC drugs (nonvisit group), using McNemar’s test.
Results
Subject characteristics
Mean ages were 35.1 (standard deviation [SD] 7.8) years for the outpatient group (n=274) and 33.0 (SD 8.5) years for the nonvisit (n=500) group (Table 1). The proportion of full-time workers in the outpatient group tended to be higher than in the nonvisit group. On the other hand, the proportion of students in the outpatient group tended to be lower than in the nonvisit group. The distribution of annual income levels and individual expenditure excluding living expenses were confirmed to be similar between the two groups. A large difference was observed between the two groups on the cervical screening experience, with 43.4% in the outpatient group reporting regular screening compared to 18.4% in the nonvisit group.
Clinical outcomes and treatment use
Comparing the mMDQ scores between the two subject groups, more outpatient group subjects had a tendency of experiencing “very strong,” “strong,” and “slightly strong” symptoms and a relatively higher mean total mMDQ score (Table 1). In the outpatient group, uterine fibroids, dysmenorrhea, endometriosis, and PMS were most frequently self-reported diagnoses of gynecological disorders (Figure 2).
  | Figure 2 Percentages for self-reported diagnoses of menstrual disorders in the outpatient group (n=274) who visited a gynecologist in the prior 3 months, using a multiple-choice response method. |
In all outpatient group subjects, oral contraceptives (OCs), including low-dose hormonal combinations, low-dose oral contraceptives, and high-dose hormonal combinations, were most frequently prescribed, followed by analgesics and TCM (Figure 3). Upon further analysis of the use of these medications for the four major diagnoses of gynecological disorders, OCs followed by analgesics were most frequently prescribed for dysmenorrhea, uterine fibroids, and endometriosis. Subjects who had dysmenorrhea reported the highest prescription OCs use. Subjects with PMS were most frequently prescribed with OCs followed by TCM (Figure 4). Of the nonvisit group subjects, 94.8% reported using OTC analgesics for their menstrual pain (Table 1).
Reasons for not seeking medical care: nonvisit group
The most commonly reported reasons for not visiting a gynecologist were: 1) not feeling the need to see a gynecologist for their menstrual symptoms (46.8%); and 2) feeling resistance or aversion toward gynecologists and hospitals (17.8%) (Table 2).
  | Table 2 Reasons for not visiting a gynecologist for menstrual symptoms |
Improvement of daily life by treatment of menstrual symptoms
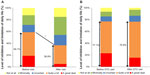
More nonvisit group subjects (77.1%) tended to report an impact on daily life due to their menstrual symptoms (ie, the sum of responses to “a great deal” and “quite a bit” of interference with daily life) than did outpatient group subjects (59.1%) before using OTC drugs and visiting a gynecologist, respectively (Figure 5). In the outpatient group, a significantly lower percentage of subjects (36.9%) reported an impact due to menstrual symptoms after compared to before their visits receiving medical treatment from their gynecologist visits (P<0.01). This led to an average reduction of 22.2% (ie, 59.1% minus 36.9%) in the impact on daily life due to menstrual symptoms among outpatient group subjects, which is later used for the hypothetical calculation of the women’s economic savings (see also the Supplementary materials). The nonvisit group, on the other hand, showed no clear differences before and after self-treating with OTC drugs.
Willingness-to-pay
Average costs that outpatient and nonvisit group subjects were willing to pay for a drug that would eliminate all menstrual symptoms were 4,834 (SD 7,341) and 2,450 (SD 2,902) Japanese yen (JPY), respectively. The outpatient group and nonvisit group subjects’ willingness-to-pay to eliminate interference with daily life due to menstrual symptoms were 3,304 (SD 4,833) JPY and 1,712 (SD 1,865) JPY, respectively (Table 1).
Hypothetical calculation of days saved by gynecologist treatment and their estimated economic savings
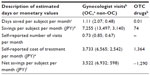
A hypothetical calculation was performed to address the following two questions (Table 3):
- what are the implications of gynecologist visits and OC treatment?
- what are the associated economic savings for women? The methodology including the equation used is explained in the Supplementary materials.
The monthly savings per subject for avoided work loss from medical care through gynecologist visits was 7,255 JPY, compared to a savings of 74 JPY from OTC drug use. The net monthly economic savings for subjects who visited were 3,522 JPY, compared to a loss of 1,290 JPY for subjects using OTC drugs. Further analyses of gynecologist visits showed that the subjects receiving OC treatment had net monthly savings of 6,932 JPY, compared to net monthly savings of 598 JPY for subjects receiving non-OC treatments.
Discussion
The present study was conducted to evaluate the clinical and economic burden of menstrual symptoms in a large population and reflects the actual current situation of Japanese women with menstruation. Findings on the overall current burden in Japanese women with menses are reported in a separate publication,10 while this paper provides further details of the severity of menstrual symptoms, diagnoses of menstrual disorders, currently used treatments for menstrual symptoms, reasons why women did not visit a gynecologist, and the improvement of daily life after gynecologist visits.
The four major gynecological disorders in this study, which were the diagnoses that were most commonly self-reported by subjects in the outpatient group, were uterine fibroids in 26%, dysmenorrhea in 22%, endometriosis in 21%, and PMS in 19% of the women. A similar order of prevalence has been previously reported in a study of more than 40,000 Japanese women aged 30–59 years, in which uterine myoma (10.1%) and endometriosis (5.3%) were two of the most frequently reported past diagnoses, in addition to hypercholesterolemia (8.2%).17 Furthermore, results from an online survey-based study in women aged 15–49 years (N=21,746) indicated that the prevalence of endometriosis18 and uterine fibroids19 across eight countries (Brazil, Canada, France, Germany, Italy, South Korea, and the UK) ranged from 9.3%–24.0% and from 4.5%–9.8%, respectively. While these findings were comparable to the self-reported diagnosis rate of endometriosis (19.3%) in Japan in the present study, uterine fibroids was reported more frequently in the present study (23.4%) compared to other countries.
Uterine fibroids and endometriosis have both been associated with pain symptoms and a negative impact on quality of life, especially on women’s sexual life, relationship and family, as well as work, school, and housekeeping.18,19 Findings from previous studies on the prevalence and negative impact of endometriosis and uterine fibroids, in conjunction with the present study results, altogether suggest that menstrual symptoms and associated gynecological disorders pose a significant burden upon women’s lives. Therefore, it highlights the importance of a specialist’s appropriate treatment for menstrual symptoms.
In the present study, a seemingly high 21% self-reported “no abnormality” in the diagnosis from a gynecologist visit. However, it is possible that some subjects had normal results by clinical testing although they had heavy menstrual pain (ie, a major symptom of dysmenorrhea); hence, underreporting the actual prevalence rate of dysmenorrhea needing medical intervention, which has been reported to be one-third in Japanese women of reproductive age.20
In terms of the treatment of menstrual symptoms in the present study, OCs, including low-dose hormonal combinations, low-dose oral contraceptives, and high-dose hormonal combinations, were prescribed most frequently to women who had been diagnosed with the major gynecological disorders (uterine fibroids, dysmenorrhea, endometriosis, and PMS). In Japan, different from other countries, the most recently approved OCs have a labeled indication for dysmenorrhea and not for contraception. This may explain why OCs are the most commonly prescribed drug treatments for dysmenorrhea in Japan, as well as for endometriosis and for PMS, for which dysmenorrhea is a major symptom. As such, OCs have been widely recognized for their benefits in the treatment and risk reduction of medical disorders in women.21
In Japan, this is also evident through the publication of the Guidelines for Office Gynecology in Japan 2011 Edition,22 which lists OCs as the first treatment option for dysmenorrhea along with nonsteroidal anti-inflammatory drugs. The noncontraceptive benefits of OCs have been recognized overseas as well.21
Results from the first survey in the present research, published elsewhere, reported approximately 20% of women suffering from menstrual symptoms visited a gynecologist; hence, the majority did not seek medical help.10 In the present survey, the most commonly reported reasons why women did not visit a gynecologist were that they felt it was unnecessary since their symptoms were not severe enough or because menstruation was a natural condition and thus did not warrant treatment. Women also felt reluctant toward consultation and pelvic exams.
Women’s behavior in seeking medical help through outpatient visits would be indicative of their level of interest toward their personal health. In this study, subjects were asked how frequently they underwent cervical cancer screening to assess their interest in caring for their own personal health. Twice the proportion of outpatient group subjects underwent cervical cancer screening at least once a year than did the nonvisit group subjects, and the willingness-to-pay for a drug that would eliminate all menstrual symptoms or their impact on daily life tended to be higher in the outpatient group subjects. These findings suggest that women who consulted a gynecologist had a higher level of interest in caring for their personal health than did women who did not visit.
OTC analgesics were frequently used by women who opted for self-treatment (nonvisit group). However, it should be noted that, due to the selection criteria, the use of OTC analgesics in the nonvisit group was likely overestimated. Specifically, the selection criteria for the nonvisit group subjects included: 1) taking OTC analgesics within the previous 3 months; or 2) having heavy menstrual bleeding that interfered or limited their daily life.
Subjects who self-treated with OTC drugs other than analgesics were not included in this group to focus on those who suffered from pain. Nonetheless, a larger proportion (35%) of the 19,254 women who had menses took OTC analgesics to self-treat their menstrual symptoms than those who sought medical care by visiting a gynecologist (20%). The data on the gynecologist visiting rate are published in a separate paper.10
Although more women seemingly choose to self-medicate than to consult a gynecologist, the present survey findings showed that OTC drug use did not make a difference in the overall impact on daily life (ie, including “a great deal” and “quite a bit” of interference with daily life). This suggests that OTC analgesics did not help with improving the daily lives of women suffering from menstrual symptoms beyond pain. On the other hand, medical treatment from gynecologist visits led to a significant decrease in the overall impact of menstrual symptoms on daily life. A hypothetical calculation of the economic savings for women that were associated with this improvement in daily life showed that gynecologist visits produced a net saving of 3,522 JPY per month, whereas OTC drug use resulted in a loss of 1,290 JPY per month. These findings altogether point to the benefit of medical care from a gynecologist in terms of improving menstrual problems beyond pain and, thus, daily life. Increasing the awareness of the benefits associated with consultation and appropriate treatment may also tie in to lowering the hurdle toward visiting a gynecologist and encouraging women to engage more in self-care activities, such as regular cervical cancer screening.
Key findings from the present research:
- The most commonly self-reported diagnoses of gynecological disorders in the outpatient group were uterine fibroids, dysmenorrhea, endometriosis, and PMS – in that order.
- OCs were frequently prescribed at a gynecologist visit in general, and for major gynecological disorders.
- Of the nonvisit group subjects, 46.8% felt that visiting a gynecologist was unnecessary, and 17.8% felt resistance or aversion toward gynecologists and hospitals.
- Medical treatment from a gynecologist visit led to a decrease in the interference with daily life due to menstrual symptoms. Improvement in daily life from visits and OC treatments coupled with visits resulted in estimated monthly savings of 3,522 JPY and 6,932 JPY, respectively.
- No differences in the impact on daily life were observed when comparing results before and after OTC use in the nonvisit group subjects, who also had an estimated monthly loss of 1,290 JPY.
- Overall, it is necessary to help more women to consult a gynecologist for their menstrual symptoms by increasing public awareness of the benefits associated with gynecologist consultation and by lowering their feeling of resistance toward consultation; thus, increasing women’s motivation and lowering the hurdle toward seeking medical help.
Conclusion
The present survey results indicate that Japanese women suffering from menstrual symptoms could benefit from visiting a gynecologist and receiving appropriate treatment to ease their symptoms, hence improving their daily life. OCs were most commonly prescribed to women presenting to a gynecologist with menstrual symptoms. Economic savings associated with gynecologist visits and treatment for women further support the benefit of appropriate patient management. Overall, there is a need to increase awareness of the above benefits and, hence, to encourage women to consult a gynecologist. The current findings were reported for the general population; therefore, a further investigation could be conducted to clarify the burden of menstrual symptoms associated with specific clinical diagnoses, such as dysmenorrhea or endometriosis, as well as with matched control subjects.
Acknowledgments
The authors would like to thank Professor Yasuki Kobayashi and Professor Kenji Shibuya from The University of Tokyo for providing their insights on the interpretation of results from the public health perspective. The authors would also like to thank Ms Etsuyo Ogawa from Bayer Yakuhin Ltd, for her support during the conduct of the study, and Ms Kuri Kobayashi and Mr Kenji Adachi, also from Bayer Yakuhin Ltd, for their review of the manuscript drafts.
Author contributions
All authors contributed important intellectual content, including important discussions on the interpretation of study results, and critical revision of the manuscript. All authors approved the final draft for submission and take full and final responsibility for the contents of the article.
Disclosure
This study was sponsored by Bayer Yakuhin Ltd, Osaka, Japan. The TrueNavi Internet research service is fielded by Nomura Research Institute. All survey data were collected and provided by Nomura Research Institute. Bayer Yakuhin Ltd developed the study concept and design in collaboration with Nomura Research Institute, contributed to the interpretation of study results, and drafted and edited the manuscript.
Bayer Yakuhin Ltd provided funding to Nomura Research Institute to conduct the study. Authors E Tanaka, B Rossi, K Nomoto, M Hayakawa and ECY Wang are salaried employees of Bayer. Author K Kokubo is a salaried employee of Nomura Research Institute. Authors M Momoeda and Y Osuga have received fees for consulting from Bayer Yakuhin Ltd.
References
Wasiak R, Filonenko A, Vanness DJ, et al. Impact of estradiol-valerate/dienogest on work productivity and activities of daily living in European and Australian women with heavy menstrual bleeding. Int J Women’s Health. 2012;4:271–278. | |
Fraser IS, Langham S, Uhl-Hochgraeber K. Health-related quality of life and economic burden of abnormal uterine bleeding. Expert Review of Obstetrics and Gynecology. 2009;4(2):179–189. | |
Liu Z, Doan QV, Blumenthal P, Dubois RW. A systematic review evaluating health-related quality of life, work impairment, and health-care costs and utilization in abnormal uterine bleeding. Value Health. 2007;10(3):183–194. | |
Yamamoto K, Okazaki A, Sakamoto Y, Funatsu M. The relationship between premenstrual symptoms, menstrual pain, irregular menstrual cycles, and psychosocial stress among Japanese college students. J Physiol Anthropol. 2009;28(3):129–136. | |
Daley AJ. Exercise and primary dysmenorrhea: a comprehensive and critical review of the literature. Sports Med. 2008;38(8):659–670. | |
Hallberg L, Högdahl AM, Nilsson L, Rybo G. Menstrual blood loss – a population study. Variation at different ages and attempts to define normality. Acta Obstet Gynecol Scand. 1966;45(3):320–351. | |
Wong LP. Attitudes towards dysmenorrhea, impact and treatment seeking among adolescent girls: a rural school-based survey. Aust J Rural Health. 2011;19(4):218–223. | |
Wong LP, Khoo EM. Dysmenorrhea in a multiethnic population of adolescent Asian girls. Int J Gynaecol Obstet. 2010;108(2):139–142. | |
Taketani Y. Investigating the prevention, diagnosis and treatment of conditions including endometriosis from the perspective of reproductive health (health related to sex and reproduction). Ministry of Health, Labor and Welfare Research report for the 2000 fiscal year. 2001:503–550. Report in Japanese. | |
Tanaka E, Momoeda M, Osuga Y, et al. Burden of menstrual symptoms in Japanese women: results from a survey-based study. J Med Econ. Epub September 10, 2013. | |
[Population by geographic location (prefecture) and gender – total population, Japanese population (as of October 1st each year)] Statistics Bureau, Director-General for Policy Planning (Statistical Standards) and Statistical Research and Training Institute, the Ministry of Internal Affairs and Communications of Japan. Available from: http://www.stat.go.jp. Accessed October 1, 2009. [Japanese] | |
Cascade E, Marr P, Winslow M, Burgess A, Nixon M. Conducting research on the Internet: medical record data integration with patient-reported outcomes. J Med Internet Res. 2012;14(5):e137. | |
Moos, RH. The development of a menstrual distress questionnaire. Psychosom Med. 1968;30(6):853–867. | |
PROQOLID database Menstrual Distress Questionnaire (MDQ). [webpage on the Internet]. Lyon, France: MAPI Research Trust; 2012. Available from: http://www.proqolid.org/instruments/menstrual_distress_questionnaire_mdq. Accessed August 7, 2012. | |
Takamatsu K, Fujii E. Series: General malaise in women’s life cycles – 3. Menstruation at reproductive age. Stress and Clinical Practice. 2003;16:14–19. Japanese. | |
Hattori R, Nin K. General malaise and depression during menstruation in nursing school students. Adolescentology. 1998;16:524–530. Japanese. | |
Fujita T, Hayashi K, Katanoda K, et al. Prevalence of diseases and statistical power of the Japan Nurses’ Health Study. Ind Health. 2007;45(5):687–694. | |
Bernuit D, Ebert AD, Halis G, et al. Female perspectives on endometriosis: findings from the uterine bleeding and pain women’s research study. Journal of Endometriosis. 2011;3(2):73–85. | |
Zimmermann A, Bernuit D, Gerlinger C, Schaefers M, Geppert K. Prevalence, symptoms and management of uterine fibroids: an international internet-based survey of 21,746 women. BMC Womens Health. 2012;12:6. | |
Osuga Y, Hayashi K, Kobayashi Y, et al. Dysmenorrhea in Japanese women. Int J Gynaecol Obstet. 2005;88(1):82–83. | |
Schindler AE. Non-contraceptive benefits of oral hormonal contraceptives. Int J Endocrinol Metab. 2013;11(1):41–47. | |
Japan Society of Obstetrics and Gynecology, Japan Association of Obstetricians and Gynecologists. Guidelines for Office Gynecology in Japan. 2011 ed. Tokyo: The Society; 2011. Japanese. |
Supplementary materials
Research questions and groups compared
A hypothetical calculation in the “Results” section assessed the following research questions:
- What are the implications of gynecologist visits and OC treatment?
- What are the associated economic savings for women?
The results for subjects receiving treatment from gynecologist visits including prescription drugs (outpatient group) was compared with those self-treating with OTC drugs (nonvisit group). A further analysis compared OC treatment with non-OC treatment from gynecologist visits. OC treatment included low-dose hormonal combinations and high-dose hormonal combinations, which are reimbursed in Japan, and low-dose oral contraceptives, which are not reimbursed in Japan.
Estimation of work days lost per month
First, the average number of work days lost in a month due to absence from work, decreased work volume or time, and decreased efficiency at work, were assessed. Subjects were asked to self-report the total number of days that they lost in the previous 3 months because they were absent from or had decreased volume or time of their work, school, or household chores, due to menstrual symptoms. Subjects were also asked to self-report the number of days that they had decreased efficiency in the previous 3 months, as well as the percentage of efficiency on those days compared to a normal day (ie, 100% efficiency). To estimate the number of work days lost from decreased efficiency, the number of self-reported days with decreased efficiency was multiplied by the percentage of inefficiency (ie, 100% minus the self-reported percentage of efficiency on the affected days). The estimated average number of work days lost in the previous 3 months due to absence, decreased work volume or time, and decreased efficiency were each divided by 3 to estimate the work days lost per month.
Estimation of days saved and the equation used for the hypothetical cost calculation
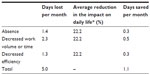
Second, the average number of days avoided from being lost due to absence, decreased work volume or time, and decreased efficiency, was estimated (ie, “days saved per month” in Table S1).
To compare the days saved from gynecologist visits with days saved from OTC drug use, the estimated work days lost per month were multiplied by the average reduction in the percentage of the self-reported impact on daily life after visits and OTC use. Percentages of impact on daily life were based on the proportions of subjects reporting “a great deal” and “quite a bit” of interference with daily life before and after visits and OTC drug use. A further analysis of the days saved from OC and non-OC treatments was also conducted.
Third, to estimate the economic savings, the average numbers of days saved each month from being lost to absence, decreased work volume or time, and decreased efficiency, were multiplied by the working cost per day. The working cost per day (6,536 JPY) was calculated by taking the average between mean daily salaries of the Japanese population aged 30–34 years and those aged 35–39 years, weighted by employment rates obtained from the present survey. The above age ranges were selected to include the average ages of the outpatient and nonvisit groups in the present survey.
To summarize, the equation used to estimate the monthly savings associated with the days saved from improvement in daily life is shown below:
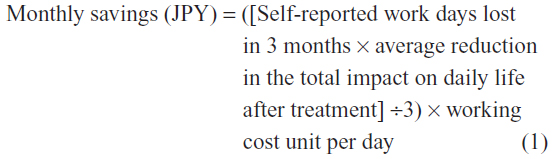
The monthly savings from avoidance of absence, decreased work volume or time, and decreased efficiency are summed.
Estimation of net monthly economic savings
Finally, the net monthly economic savings after subtracting treatment costs (ie, gynecologist visit or purchasing OTC drugs) were estimated. For gynecologist visits, OC treatment and non-OC treatment, the average of the subjects’ self-reported treatment costs in the prior 3 months were divided by the average of self-reported number of visits in the prior 3 months. The resulting average treatment costs and costs spent on purchasing OTC drugs (ie, analgesics, sleeping pills, minor tranquilizers, TCM, supplements, and vitamins) per month were each subtracted from the total monthly savings.
 © 2013 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2013 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.