Back to Journals » Infection and Drug Resistance » Volume 12
Association of diabetes mellitus with hepatitis B and hepatitis C virus infection: evidence from an epidemiological study
Authors Liu Y, Ye S , Xiao X, Zhou T, Yang S , Wang G, Sun C , Zhang B , Wang G
Received 6 June 2019
Accepted for publication 2 September 2019
Published 12 September 2019 Volume 2019:12 Pages 2875—2883
DOI https://doi.org/10.2147/IDR.S218536
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Joachim Wink
Yujia Liu,1 Shangyuan Ye,2 Xianchao Xiao,1 Tong Zhou,1 Shuo Yang,1 Gang Wang,1 Chenglin Sun,1 Bo Zhang,2 Guixia Wang1
1Department of Endocrinology and Metabolism, The First Hospital of Jilin University, Changchun, Jilin, People’s Republic of China; 2Department of Population and Quantitative Health Sciences, University of Massachusetts Medical School, Worcester, MA, USA
Correspondence: Bo Zhang
Department of Population and Quantitative Health Sciences, University of Massachusetts Medical School, Worcester, MA, USA
Email [email protected]
Guixia Wang
Department of Endocrinology and Metabolism, The First Hospital of Jilin University, Changchun, Jilin, People’s Republic of China
Email [email protected]
Objective: To study the association between glucose metabolism disorders and hepatotropic virus infection.
Methods: A cross-sectional analysis was performed using data from the REACTION study (Risk Evaluation of Cancers in Chinese Diabetic Individuals: A Longitudinal Study). Outcomes of the analysis were test results of kidney function, liver function, lipid metabolism, and the prevalence of hepatitis B virus (HBV) infection and potential hepatitis C virus (HCV) infection (positive hepatitis C virus antibody) among individuals with and without diabetes mellitus (DM) or pre-diabetes mellitus (pre-DM).
Results: Of the 10,080 patients who participated in the study, 7665 eligible subjects were included in the analysis. There was no significant difference in the prevalence of HBV infection between DM and normal subjects, pre-DM and normal subjects, and DM or pre-DM and normal subjects (p-values of 0.9180, 0.8154, and 0.6448, respectively). There was also no significant difference in the prevalence of potential HCV infection between DM and normal subjects, pre-DM and normal subjects, and DM or pre-DM and normal subjects (p-values of 0.1190, 0.0591, and 0.5591, respectively). Lipid metabolism showed a significant difference between DM or pre-DM subjects and normal subjects (p-values were less than 0.0221 in all cases). Multiple logistic regression analysis revealed hypertension as the leading significant variable associated with DM, pre-DM, and both. Other significant factors included gender, body mass index, age, and alanine aminotransferase.
Conclusion: No significant association was detected between DM or pre-DM and HBV or potential HCV infection. Significant association was detected between lipid metabolism disorders and DM, but this association was absent in pre-DM patients when adjusting for other factors.
Keywords: diabetes, pre-diabetes, lipid metabolism disorder, hepatitis B, hepatitis C
Introduction
Diabetes mellitus (DM) and pre-diabetes mellitus (pre-DM) are two common glucose metabolism disorders. DM is defined as a group of metabolic disorders characterized by high blood glucose levels.1 Patients with pre-DM present with disordered glucose metabolism, but their blood glucose levels do not reach the cutoff point for a DM diagnosis. The prevalence of DM continues to increase globally over the past decades.2 Multiple studies3–5 have reported that patients with DM may also suffer from lipid metabolism disorder. It has been established that the composition of lipid particles in diabetic dyslipidemia is more atherogenic than that in other types of dyslipidemia.4,6
Hepatitis B virus (HBV)7 or hepatitis C virus (HCV)8,9 infection is a major risk factor that can result in chronic liver malfunction, liver cirrhosis, and hepatocellular carcinoma. It has been reported that hepatitis B infection is the most predominant among all legally notifiable infectious diseases in China.7,10,11 In addition, it has been estimated that between 130 million and 150 million people (2–3% of the world’s population) are infected by HCV globally.8,9 The prevalence of HCV infection in China is 0.06%; it has become the second most prevalent major liver disease in the nation (surpassed only by HBV infection).12 The association between HBV or HCV infection and DM has been the focus of several studies. These study results were summarized by Desbois and Cacoub13 and El-Serag et al14.
However, the conclusions of these studies were not consistent. Several studies have shown that HCV infection significantly increases the prevalence of DM (eg, Huang et al15 and Sangiorgio et al16). Though the precise biological mechanisms are still unclear, insulin resistance (IR) is believed to play an important role in the development of various complications associated with HCV infection.8,9 Yet, some other studies (eg, Balogun et al17 and da Costa et al18) have shown that no significant association exists between HCV infection and the prevalence of DM. Similar conflicting results have been found among studies of the association between DM and HBV infection.19 Along with the inconsistent results, a major limitation of these studies is that they have only considered the association between hepatotropic virus (HBV or HCV) infection or lipid metabolism disorder and DM, and their associations with pre-DM or both DM and pre-DM have been rarely studied. Here, we report the results from analyzing the data from an epidemiological study to investigate the association between glucose metabolism disorder (DM, pre-DM, or both) and hepatotropic virus infection (HBV or HCV), as well as the association between glucose metabolism disorder and lipid metabolism disorder.
Methods
Study design and data
Between June 2011 and December 2011, an epidemiological study was conducted among individuals aged more than 40 years old from six community health care centers in the city of Changchun, a capital city of Jilin Province that is located in Northeastern China. From the six communities, three housing estates were randomly selected. This study was part of the nationwide survey for the REACTION study (Risk Evaluation of Cancers in Chinese Diabetic Individuals: A Longitudinal Study20). From each housing estate, 560 residents who were older than 40 years participated as the study subjects. Of the 10,080 patients who were included in the study, 9571 subjects completed the survey. Subjects were excluded if they had (1) experienced severe trauma, surgery, myocardial infarction, cerebral infarction, or cardiovascular diseases in the previous 3 months, (2) a history of diabetes mellitus, cancer, or hepatorenal insufficiency, (3) simultaneous infection of both HBV and HCV, or (4) a fasting blood glucose lower than 3.9 mmol/L.
One day before the survey was conducted, a written consent form was obtained from the participants; each participant was then given a serial subject code that was later used to identify the participant and blood collection. On-site health surveys were distributed by trained physicians and medical school students to the participants. The survey questions included general information, medical history, family history, eating habits, and exercise habits of the participants. The participants underwent blood testing after a 12-hr overnight fast to measure liver function (creatinine (CRE), aspartate aminotransferase (AST), glutamyl transpeptidase (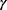 -GT), and alanine aminotransferase (ALT)), blood lipid profile (high-density lipoprotein cholesterol (HDL-C) and low-density lipoprotein cholesterol (LDL-C), triglycerides (TG), total cholesterol (CHOL)), fasting insulin and fasting blood glucose, hepatitis B surface antigen (HBsAg), and hepatitis C virus antibody (HCvAb). Subjects who showed no history of DM were given an oral glucose tolerance test. Fingertip blood samples were collected to test for glycosylated hemoglobin (HbAc). Liver function and lipid profiles were analyzed using an Automated Biochemical Immune Detector (Abbott Laboratories, North Chicago, Illinois, US). HBsAg and HCvAb were analyzed using the enzyme-linked immunosorbent assay (Shanghai Kehua Bio-engineering Co., Ltd. and British Families and New, Xiamen, Fujian, China, respectively). Information on gender, age, history of DM, hepatitis, and other chronic liver diseases and associated treatment were collected using unified questionnaire forms from the participants, and the questions were asked and recorded by trained medical personnel. Body weight and height were also measured. Height was measured in centimeters, and weight was measured in kilograms. Body mass index (BMI) was calculated using height and weight measurements.
-GT), and alanine aminotransferase (ALT)), blood lipid profile (high-density lipoprotein cholesterol (HDL-C) and low-density lipoprotein cholesterol (LDL-C), triglycerides (TG), total cholesterol (CHOL)), fasting insulin and fasting blood glucose, hepatitis B surface antigen (HBsAg), and hepatitis C virus antibody (HCvAb). Subjects who showed no history of DM were given an oral glucose tolerance test. Fingertip blood samples were collected to test for glycosylated hemoglobin (HbAc). Liver function and lipid profiles were analyzed using an Automated Biochemical Immune Detector (Abbott Laboratories, North Chicago, Illinois, US). HBsAg and HCvAb were analyzed using the enzyme-linked immunosorbent assay (Shanghai Kehua Bio-engineering Co., Ltd. and British Families and New, Xiamen, Fujian, China, respectively). Information on gender, age, history of DM, hepatitis, and other chronic liver diseases and associated treatment were collected using unified questionnaire forms from the participants, and the questions were asked and recorded by trained medical personnel. Body weight and height were also measured. Height was measured in centimeters, and weight was measured in kilograms. Body mass index (BMI) was calculated using height and weight measurements.
In our data analysis to investigate the association between glucose metabolism disorder (DM, pre-DM, or both) and HBV or potential HCV infection or lipid metabolism disorder, we included liver function (CRE, AST,  -GT, ALT) and blood lipid profile (HDL-C, LDL-C, TG, CHOL) measures collected from laboratory tests for the subjects. Other four factors (ie, gender, age, hypertension, and BMI) that are commonly associated with DM were also included. We considered the status of DM and pre-DM as the primary outcome, and the status of HBV infection or potential HCV infection was also our primary interest. DM was determined by the fasting plasma glucose (FPG) ≥ 7.0 mmol/L or 2 hr postload plasma glucose (PPG) ≥ 11.1 mmol/L. Pre-DM was determined by the FPG from 6.1 mmol/L to 7.0 mmol/L or 2 hr PPG from 6.1 mmol/L to 7.0 mmol/L. Status of HBV infection was determined by the positive or negative result of HBsAg. Status of potential HCV infection was determined by the positive or negative result of HCvAb (HCV RNA level that can determine HCV infection was not measured in HCvAb positive subjects due to limited study budget). Any subject with missing information in the above measurements were excluded from our analysis. The final data set for analysis consisted of a total of 7665 subjects, of which 2433 were men (31.7%) and 5232 were women (68.3%). The study has been approved by the ethics committee of The First Hospital of Jilin University and was conducted in accordance with the Declaration of Helsinki. The participant consent of the study was written informed consent that was signed by and obtained from the study participants.
-GT, ALT) and blood lipid profile (HDL-C, LDL-C, TG, CHOL) measures collected from laboratory tests for the subjects. Other four factors (ie, gender, age, hypertension, and BMI) that are commonly associated with DM were also included. We considered the status of DM and pre-DM as the primary outcome, and the status of HBV infection or potential HCV infection was also our primary interest. DM was determined by the fasting plasma glucose (FPG) ≥ 7.0 mmol/L or 2 hr postload plasma glucose (PPG) ≥ 11.1 mmol/L. Pre-DM was determined by the FPG from 6.1 mmol/L to 7.0 mmol/L or 2 hr PPG from 6.1 mmol/L to 7.0 mmol/L. Status of HBV infection was determined by the positive or negative result of HBsAg. Status of potential HCV infection was determined by the positive or negative result of HCvAb (HCV RNA level that can determine HCV infection was not measured in HCvAb positive subjects due to limited study budget). Any subject with missing information in the above measurements were excluded from our analysis. The final data set for analysis consisted of a total of 7665 subjects, of which 2433 were men (31.7%) and 5232 were women (68.3%). The study has been approved by the ethics committee of The First Hospital of Jilin University and was conducted in accordance with the Declaration of Helsinki. The participant consent of the study was written informed consent that was signed by and obtained from the study participants.
Statistical analysis
Frequencies were compared between groups using Fisher’s exact test for categorical variables, and Student’s t-test was used to compare means between groups for continuous variables. P-values were calculated for these tests to detect significant differences. Multiple logistic regression analysis was conducted to explore the relationship between DM or pre-DM and HBV or potential HCV infection, adjusting for other factors. The strength of the associations is presented in terms of (OR) with 95% CI and 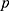 -values. Statistical significance was set at
-values. Statistical significance was set at 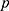 -values of less than 0.05 for all analyses. All statistical analyses were performed in the R statistical environment (R version 3.5.1, 2018 the R Foundation for Statistical Computing Platform).
-values of less than 0.05 for all analyses. All statistical analyses were performed in the R statistical environment (R version 3.5.1, 2018 the R Foundation for Statistical Computing Platform).
Results
Comparison between glucose metabolism disorder patients and normal subjects
The baseline characteristics and group comparison results are summarized in Tables 1–3. Of the 7665 subjects (2433 men and 5232 women) included in our study, 4230 of them had glucose metabolism disorder (2468 with DM and 1762 with pre-DM), and the remaining 3435 subjects were normal. Their mean age was 58.01 years with a SD of 9.82. Comparisons between the two groups, the group with DM or pre-DM, and the group with normal glucose metabolism (see Table 1) revealed that age, hypertension, CRE, HDL-C, LDL-C, CHOL, TG, ALT, AST, 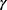 -GT, and BMI were all significantly different between the two groups (
-GT, and BMI were all significantly different between the two groups (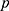 -value less than 0.05; see Table 1). The prevalence of HBV infection among subjects with glucose metabolism disorders and normal subjects was 5.3% (
-value less than 0.05; see Table 1). The prevalence of HBV infection among subjects with glucose metabolism disorders and normal subjects was 5.3% (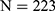 ) and 5.3% (
) and 5.3% (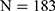 ), respectively (
), respectively (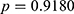 ), and the prevalence of HCV infection in these two groups was 2.0% (
), and the prevalence of HCV infection in these two groups was 2.0% (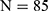 ) and 1.5% (
) and 1.5% (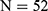 ), respectively (
), respectively (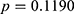 ). Thus, the prevalence of HBV and potential HCV infection was not significantly different between these two groups.
). Thus, the prevalence of HBV and potential HCV infection was not significantly different between these two groups.
 |
Table 1 Comparison of basic characteristics and clinical variables associated with diabetes or pre-diabetes among all 7665 subjects |
 |
Table 2 Comparison of basic characteristics and clinical variables associated with diabetes among 5903 subjects (diabetic and normal subjects) |
 |
Table 3 Basic characteristics and clinical variables associated with pre-diabetes among 5197 subjects (pre-diabetic and normal subjects) |
Comparison between diabetes and normal subjects
If we excluded the pre-DM subjects from the original sample and retained the data from the DM and normal individuals, there were 5903 subjects with a mean age of 57.82 years with a SD of 9.82 years. Comparisons between these two groups, the group with DM, and the group with normal glucose metabolism (see Table 2) showed that the differences between age, hypertension, CRE, HDL-C, LDL-C, CHOL, TG, ALT, 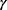 -GT, and BMI remained significant. Contrary to the previous comparison, the mean values for AST were not significantly different between these two groups (
-GT, and BMI remained significant. Contrary to the previous comparison, the mean values for AST were not significantly different between these two groups (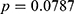 , which is borderline nonsignificant). The prevalence of HBV infection among DM and normal subjects was 5.5% (
, which is borderline nonsignificant). The prevalence of HBV infection among DM and normal subjects was 5.5% (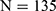 ) and 5.3% (
) and 5.3% (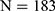 ), respectively (
), respectively (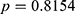 ); the prevalence of potential HCV infection for these two groups was 2.2% (
); the prevalence of potential HCV infection for these two groups was 2.2% (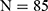 ) and 1.5% (
) and 1.5% (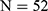 ), with
), with 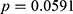 , which is borderline nonsignificant. Thus, the difference in the prevalence of both HBV and potential HCV infection was still not significant between DM and normal subjects after excluding pre-DM subjects.
, which is borderline nonsignificant. Thus, the difference in the prevalence of both HBV and potential HCV infection was still not significant between DM and normal subjects after excluding pre-DM subjects.
Comparison between pre-diabetes and normal subjects
If we excluded the DM subjects from the original sample and retained the data from pre-DM and normal individuals, there were total 5197 subjects, and the mean age was 57.15 years with a SD of 9.98. Comparisons between these two groups, the group with pre-DM and the group with normal glucose metabolism (see Table 3), showed that the differences between age, hypertension, HDL-C, LDL-C, CHOL, TG, ALT, AST, and BMI remained significant. Contrary to the previous two comparisons, the mean values for CRE and 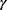 -GT were not significantly different between these two groups (
-GT were not significantly different between these two groups (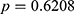 and
and 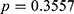 , respectively). The prevalence of HBV infection among pre-DM and normal subjects was 5.0% (
, respectively). The prevalence of HBV infection among pre-DM and normal subjects was 5.0% (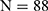 ) and 5.3% (
) and 5.3% (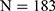 ), respectively (
), respectively (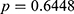 ); the prevalence of potential HCV infection in these two groups was 1.8% (
); the prevalence of potential HCV infection in these two groups was 1.8% (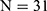 ) and 1.5% (
) and 1.5% (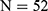 ), respectively (
), respectively (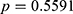 ). Thus, the prevalence of both HBV and potential HCV infection was still not significantly different between the pre-DM and normal groups after excluding the DM subjects.
). Thus, the prevalence of both HBV and potential HCV infection was still not significantly different between the pre-DM and normal groups after excluding the DM subjects.
The prevalence of DM among the subjects with HBV and potential HCV infection was 42.5% (135/318) and 50.9% (54/106), respectively (see Figure 1). The prevalence of pre-DM among subjects with HBV and potential HCV infection was 32.5% (88/271) and 38.3% (31/83), respectively (see Figure 1). The prevalence of DM was significantly different from 50% (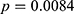 ) among the subjects with HBV infections, but it was not significantly different from 50% (
) among the subjects with HBV infections, but it was not significantly different from 50% (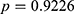 ) among the subjects with potential HCV infection. The prevalence of pre-DM was significantly different from 50% for the subjects with HBV (
) among the subjects with potential HCV infection. The prevalence of pre-DM was significantly different from 50% for the subjects with HBV (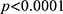 ) and the subjects with potential HCV infection (
) and the subjects with potential HCV infection (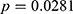 ).
).
 |
Figure 1 Prevalence of diabetes and pre-diabetes among subjects with hepatitis B virus and potential hepatitis C virus infection. |
Multiple logistic regression analysis
Multiple logistic regression analysis was conducted among all 7665 subjects to adjust for the factors that are associated with glucose metabolism disorder (see Table 4). Because of the possible correlation between variables (eg, ALT, AST, and 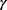 -GT are three measures of liver function, and therefore maybe correlated), we only included sex, age, potential HCV infection, HBV infection, hypertension, BMI, CRE, HDL-C, and ALT. The results showed that hypertension (OR=1.8129) was the most significant independent factor associated with glucose metabolism disorder. Other significant factors were male gender (OR=0.8352), BMI (OR=1.0573), age (OR=1.0305), HDL-C (OR=0.7232), and ALT (OR=1.0146). With an identical set of adjusting factors included, multiple logistic regression analysis was conducted among the 5903 DM and normal subjects (see Table 5). These results showed that hypertension (OR=1.9791) was also the most significant factor associated with DM. Other significant factors were male gender (OR=0.8442), BMI (OR=1.0733), age (OR=1.0362), HDL-C (OR=0.6017), and ALT (OR=1.0114). Multiple logistic regression analysis was also conducted among the 5197 pre-DM and normal subjects (see Table 6). The results showed that hypertension (OR=1.5805) was the most significant independent factor associated with pre-DM. Other significant factors were male gender (OR=0.8366), BMI (OR=1.0361), age (OR=1.0225), and ALT (OR=1.0091). The comparison made through multiple logistic regression showed that neither HBV infection nor potential HCV infection was associated with glucose metabolism disorder.
-GT are three measures of liver function, and therefore maybe correlated), we only included sex, age, potential HCV infection, HBV infection, hypertension, BMI, CRE, HDL-C, and ALT. The results showed that hypertension (OR=1.8129) was the most significant independent factor associated with glucose metabolism disorder. Other significant factors were male gender (OR=0.8352), BMI (OR=1.0573), age (OR=1.0305), HDL-C (OR=0.7232), and ALT (OR=1.0146). With an identical set of adjusting factors included, multiple logistic regression analysis was conducted among the 5903 DM and normal subjects (see Table 5). These results showed that hypertension (OR=1.9791) was also the most significant factor associated with DM. Other significant factors were male gender (OR=0.8442), BMI (OR=1.0733), age (OR=1.0362), HDL-C (OR=0.6017), and ALT (OR=1.0114). Multiple logistic regression analysis was also conducted among the 5197 pre-DM and normal subjects (see Table 6). The results showed that hypertension (OR=1.5805) was the most significant independent factor associated with pre-DM. Other significant factors were male gender (OR=0.8366), BMI (OR=1.0361), age (OR=1.0225), and ALT (OR=1.0091). The comparison made through multiple logistic regression showed that neither HBV infection nor potential HCV infection was associated with glucose metabolism disorder.
 |
Table 4 Multiple logistic regression analysis of variables associated with diabetes or pre-diabetes among all 7665 subjects |
 |
Table 5 Multiple logistic regression analysis of variables associated with diabetes among 5903 subjects |
 |
Table 6 Multiple logistic regression analysis of variables associated with pre-diabetes among 5197 subjects |
Discussion
In this study, we investigated the association between glucose metabolism disorder and hepatotropic virus infection or lipid metabolism disorder. All results (group comparisons and logistic regressions) suggest that glucose metabolism disorder (DM, pre-DM, or both) and hepatotropic virus infection (HBV or potential HCV infection) are not significantly associated. We further determine that hypertension is the leading significant variable associated with DM, pre-DM, or both, followed by the factors including gender, BMI, age, and ALT. HDL-C is a factor that is not significantly associated with pre-DM, but it is associated with DM.
Our results show that there is not a significant association between glucose metabolism disorder and hepatotropic virus infection. Though a few other studies have also reported that no detected association exists between DM and HBV or HCV infection,21 the majority of studies have shown that patients with HBV or HCV infection have an increased risk of DM.22–24 Several studies have proposed that the association can be explained by the cytopathic effects caused by HBV or HCV infection in diseased extrahepatic organs.15,25 Thus, it has been reported that multiple extrahepatic autoimmune diseases (eg, thyroiditis, thrombocytopenia, and arthritis), including DM, can be triggered by these viruses.26,27 Our numerical results appear to contradict previous findings. However, the results of previous studies require further examination. As highlighted by Zhang et al19 and the authors of many other articles, the status of HBV or HCV infection should be clearly defined. After infection, the patients may either develop immunity and clear the disease in the short term (acute infection) or become chronic virus carriers. Chronic carriers, taking HBV infection as an example, can be further classified as asymptomatic chronic HBV carriers or diagnosed with chronic hepatitis B. Other studies have also considered virus holders with different genotypes or other characteristics (eg, viremia vs nonviremia15). The significant associations detected in previous studies have mostly resulted from comparisons between chronic virus carriers or more specific classifications and non-infected controls. Zhang et al19 summarized five different comparisons in previous studies. In our study, because the status of HBV infection and potential HCV infection was determined by HBsAg and HCvAb analyses, respectively, we compared HBV or potential HCV infection in general with a noninfected population. Thus, our results (ie no significant association between glucose metabolism disorder and hepatotropic virus infection) could be significantly different from the results of previous studies, because only 5–10% HBV28 and 75–85% HCV29 infected adults will develop chronic HBV and HCV, respectively. Hence, the association between glucose metabolism disorder and hepatotropic virus infection may only occur for chronic hepatotropic infection, and only long-term HBV or HCV infection in extrahepatic organs can trigger extrahepatic autoimmune diseases such as glucose metabolism disorders. Unfortunately, the current data set cannot be used to confirm this assertion.
Our results show a significant association between glucose metabolism disorder and lipid metabolism disorder. This is a well-represented finding, and these two conditions and their association have been studied frequently because dyslipidemia is an important mediator of the cardiovascular risk associated with diabetes.4 In our data set, HDL-C, LDL-C, CHOL, and TG are measurements of lipid metabolism. All the three group comparisons, ie, DM versus normal subjects, pre-DM versus normal subjects, and DM or pre-DM versus normal subjects, show significant differences in the mean values of these measurements. The logistic regression analysis results reveal that HDL-C is a significant factor associated with glucose metabolism disorder (OR=0.7232 for DM versus normal subjects, OR=0.6017 for pre-DM versus normal subjects). Previous studies confirmed these results and reported that DM patients exhibited low HDL-C, elevated small dense LDL-C, and elevated TG levels.4,30 We further observe that lipid metabolism disorder is not significantly associated with pre-DM (OR=0.9082, p-value =0.3741) when adjusting for other factors. Note that, due to possible associations between adjusting factors, we only present the results from the regression analyses that included HDL-C. The inclusion of other factors (LDL-C, CHOL, or TG) yields similar results, so we do not report these analysis results here.
Our study population has limitations. In the baseline survey of the REACTION study conducted between 2011 and 2012, a total number of 259,657 community-dwelling adults were recruited across mainland China.20 However, our study was conducted from analyzing the data collected in the city of Changchun in Northeastern China. The conclusions drawn from our study may be limited due to the specific region where the participants are located. A nationwide analysis on all participants of the REACTION study may deliver more reliable results.
Conclusion
In conclusion, we studied the association between glucose metabolism disorder and hepatotropic virus infection or lipid metabolism disorder using data collected from the REACTION study. Our results show significant associations exist between lipid metabolism disorder and DM, but no significant associations are detected between lipid metabolism disorder and pre-DM when adjusting for other factors. Furthermore, there is no significant association detected between HBV or potential HCV infection and DM, pre-DM, or both.
Acknowledgment
The present work was one part of the baseline survey from the REACTION study investigating the association of diabetes and cancer, which was conducted among 259,657 adults, aged 40 years and above in 25 communities across mainland China, from 2011 to 2012. This research was supported by the Science and Technology Department of China through grants 20170623092TC-01 and 20180623083TC-01 and by China’s National Development and Reform Commission through grant 2017C019.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Cho N, Shaw JE, Karuranga S, et al. IDF diabetes atlas: global estimates of diabetes prevalence for 2017 and projections for 2045. Diabetes Res Clin Pract. 2018;138:271–281. doi:10.1016/j.diabres.2018.02.023
2. Koye DN, Magliano DJ, Nelson RG, Pavkov ME. The global epidemiology of diabetes and kidney disease. Adv Chronic Kidney Dis. 2018;25(2):121–132. doi:10.1053/j.ackd.2017.10.011
3. Saltiel AR, Kahn CR. Insulin signalling and the regulation of glucose and lipid metabolism. Nature. 2001;414(6865):799. doi:10.1038/414799a
4. Parhofer KG. Interaction between glucose and lipid metabolism: more than diabetic dyslipidemia. Diabetes Metab J. 2015;39(5):353–362. doi:10.4093/dmj.2015.39.5.353
5. Adiels M, Olofsson SO, Taskinen MR, Borén J. Overproduction of very low-density lipoproteins is the hallmark of the dyslipidemia in the metabolic syndrome. Arterioscler Thromb Vasc Biol. 2008;28(7):1225–1236. doi:10.1161/ATVBAHA.107.160192
6. Ozder A. Lipid profile abnormalities seen in T2DM patients in primary healthcare in Turkey: a cross-sectional study. Lipids Health Dis. 2014;13(1):183. doi:10.1186/1476-511X-13-183
7. Yonghao G, Jin X, Jun L, et al. An epidemiological serosurvey of hepatitis B virus shows evidence of declining prevalence due to hepatitis B vaccination in central China. Int J Infect Dis. 2015;1(40):75–80. doi:10.1016/j.ijid.2015.10.002
8. Bose SK, Ray R. Hepatitis C virus infection and insulin resistance. World J Diabetes. 2014;5(1):52. doi:10.4239/wjd.v5.i1.52
9. El-Zayadi AR, Anis M. Hepatitis C virus induced insulin resistance impairs response to anti-viral therapy. World J Gastroenterol. 2012;18(3):212. doi:10.3748/wjg.v18.i3.212
10. Lok AS, McMahon BJ, Brown RS, et al. Antiviral therapy for chronic hepatitis B viral infection in adults: a systematic review and meta-analysis. Hepatology. 2016;63(1):284–306. doi:10.1002/hep.28280
11. Te HS, Jensen DM. Epidemiology of hepatitis B and C viruses: a global overview. Clin Liver Dis. 2010;14(1):1–21. doi:10.1016/j.cld.2009.11.009
12. Zhang Y, Chen LM, He M. Hepatitis C Virus in mainland China with an emphasis on genotype and subtype distribution. Virol J. 2017;14(1):41. doi:10.1186/s12985-017-0710-z
13. Desbois AC, Cacoub P. Diabetes mellitus, insulin resistance and hepatitis C virus infection: A contemporary review. World J Gastroenterol. 2017;23(9):1697. doi:10.3748/wjg.v23.i9.1697
14. El–Serag HB, Hampel H, Javadi F. The association between diabetes and hepatocellular carcinoma: a systematic review of epidemiologic evidence. Clin Gastroenterol Hepatol. 2006;4(3):369–380. doi:10.1016/j.cgh.2005.12.007
15. Huang JF, Dai CY, Hwang SJ, et al. Hepatitis C viremia increases the association with type 2 diabetes mellitus in a hepatitis B and C endemic area: an epidemiological link with virological implication. Am J Gastroenterol. 2007;102(6):1237. doi:10.1111/j.1572-0241.2007.01181.x
16. Sangiorgio L, Attardo T, Gangemi R, Rubino C, Barone M, Lunetta M. Increased frequency of HCV and HBV infection in type 2 diabetic patients. Diabetes Res Clin Pract. 2000;48(2):147–151.
17. Balogun WO, Adeleye JO, Akinlade KS, Kuti M, Otegbayo JA. Low prevalence of hepatitis-C viral seropositivity among patients with type-2 diabetes mellitus in a tertiary hospital. J Natl Med Assoc. 2006;98(11):1805.
18. Costa LM, Mussi AD, Brianeze MR, Souto FJ. Hepatitis C as a risk factor for diabetes type 2: lack of evidence in a hospital in central-west Brazil. Braz J Infect Dis. 2008;12(1):24–26.
19. Zhang J, Shen Y, Cai H, Liu YM, Qin G. Hepatitis B virus infection status and risk of type 2 diabetes mellitus: a meta-analysis. Hepatol Res. 2015;45(11):1100–1109. doi:10.1111/hepr.12481
20. Bi Y, Lu J, Wang W, et al. Cohort profile: risk evaluation of cancers in Chinese diabetic individuals: a longitudinal (REACTION) study. J Diabetes. 2014;6(2):147–157. doi:10.1111/1753-0407.12108
21. Montenegro L, De Michina A, Misciagna G, Guerra V, Di Leo A. Virus C hepatitis and type 2 diabetes: a cohort study in southern Italy. Am J Gastroenterol. 2013;108(7):1108. doi:10.1038/ajg.2013.90
22. Custro N, Carroccio A, Ganci A, et al. Glycemic homeostasis in chronic viral hepatitis and liver cirrhosis. Diabetes Metab. 2001;27(4 Pt 1):476–481.
23. Hammerstad SS, Grock SF, Lee HJ, Hasham A, Sundaram N, Tomer Y. Diabetes and hepatitis C: a two-way association. Front Endocrinol (Lausanne). 2015;14(6):134.
24. White DL, Ratziu V, El-Serag HB. Hepatitis C infection and risk of diabetes: a systematic review and meta-analysis. J Hepatol. 2008;49(5):831–844. doi:10.1016/j.jhep.2008.08.006
25. Strassburg CP, Vogel A, Manns MP. Autoimmunity and hepatitis C. Autoimmun Rev. 2003;2(6):322–331.
26. Cacoub P, Poynard T, Ghillani P, et al. Extrahepatic manifestations of chronic hepatitis C. Arthritis Rheum. 1999;42(10):2204–2212. doi:10.1002/1529-0131(199910)42:10<2204::AID-ANR24>3.0.CO;2-D
27. Mason AL, Lau JY, Hoang N, et al. Association of diabetes mellitus and chronic hepatitis C virus infection. Hepatology. 1999;29(2):328–333. doi:10.1002/hep.510290235
28. Shepard CW, Simard EP, Finelli L, Fiore AE, Bell BP. Hepatitis B virus infection: epidemiology and vaccination. Epidemiol Rev. 2006;28(1):112–125. doi:10.1093/epirev/mxj009
29. Williams I. Epidemiology of hepatitis C in the United States. Am J Med. 1999;107(6):2–9. doi:10.1016/S0002-9343(99)00373-3
30. Wu L, Parhofer KG. Diabetic dyslipidemia. Metabolism. 2014;63(12):1469–1479. doi:10.1016/j.metabol.2014.08.010
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
