Back to Journals » Open Access Journal of Contraception » Volume 12
Assessment of Male Involvement in Long-Acting and Permanent Contraceptive Use of Their Partner in West Badewacho, Southern Ethiopia
Authors Abose A, Adhena G , Dessie Y
Received 14 December 2020
Accepted for publication 11 February 2021
Published 26 February 2021 Volume 2021:12 Pages 63—72
DOI https://doi.org/10.2147/OAJC.S297267
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Igal Wolman
Abera Abose,1 Girmay Adhena,2 Yadeta Dessie3
1Department of Reproductive Health, West Badewacho, Ethiopia; 2Department of Reproductive Health, Tigray Regional Health Bureau, Tigray, Ethiopia; 3School of Public Health, College of Health and Medical Science, Haramaya University, Harar, Ethiopia
Correspondence: Girmay Adhena Email [email protected]
Background: Male involvement in family planning use particularly in long-acting and permanent contraceptive methods (LAPCM) is a key strategy to reduce fertility, and promote maternal and child health. Despite this, little is known about male involvement in LAPCM use of their partners in Africa, particularly in Ethiopia. This study aimed to assess male involvement in long-acting and permanent contraceptive method use in west Badewacho district, Southern Ethiopia.
Methods: A community-based cross-sectional study was conducted among 564 participants from April 1 to 30/2019. A multi-stage sampling technique was used to select eligible participants. A pre-tested, structured, and interviewer-administered questionnaire was used. Binary and multivariable logistic regression analysis was done to identify associated factors. The adjusted odds ratio with 95% CI was estimated to show the direction and strength of the association. Variables with p< 0.05 were considered statistically significant.
Results: About 108 (19.9%, 95% CI: (16.8, 23.2)) participants were involved in LAPCM use. Being urban dweller [AOR=3.13; 95% CI: (1.58, 6.19)], discussion with wives about LAPCM [AOR=2.81; 95% CI: (1.64, 4.8)], having good knowledge about LAPCM [AOR=2.55; 95% CI: (1.42, 4.57)], and positive attitude towards LAPCM [AOR=2.16; 95% CI: (1.16, 4.02)] were significantly associated factors.
Conclusion: Overall, the male involvement in LAPCM use was low. Enhancing male involvement in family planning use through creating community awareness, encouraging inter-spousal communication to enhance decision making, and increasing positive attitude towards LAPCM in the community is crucial to decrease the problem.
Keywords: male involvement, long-acting contraceptive, permanent contraceptive, Ethiopia
Background
Male involvement in family planning refers to when the men accept, discuss, and support their partner’s needs, choices, and rights in fertility regulation methods and sexual behaviors.1 Male involvement in family planning use particularly in long-acting and permanent contraceptive methods is key strategies to reduce fertility and promote maternal and child health.2 It is crucial to the success of family planning programs and women’s empowerment and associated with better outcomes in reproductive health such as contraceptive acceptance, continuation, and safer sexual behaviors.3
Contraceptives are used by the majority of married women, and evidence showed that 63% of married women worldwide used some form of contraceptive, and 58% of them used modern contraception methods.2–4 Even though the involvement of the male partner in the globe is low, long-acting and permanent contraceptive methods (LAPCM) are more effective, save costs, and enable women to control their reproductive lives better.4 This method accounted for about 56% of contraceptive use globally. Nineteen percent of married or in-union women relied on female sterilization, and about 14% used an intrauterine device (IUD). Yet most contraceptive users in Africa depend on short term methods.5 Evidence showed that short-acting contraceptives using women were 21 times more likely to have an unintended pregnancy than women using long-acting reversible and permanent methods.6
The unmet need for modern contraceptives was much higher in less developed regions, about 15% in Oceania, and 22% were in Africa.7,8 In the developing world, 74 million women each year have an unintended pregnancy.9 A projection in sub-Saharan African (SSA) countries indicated that more than 1.8 million unintended pregnancies would have been averted if 20% of women using oral contraceptives and injectable shifts to the implant.10 If the unmet need for family planning is fulfilled, it would prevent about 52 million unintended pregnancies, 500,000 newborn deaths, and 70,000 maternal deaths per year.11 Countries in sub-Saharan Africa have documented fertility rates of over 5 children per woman and the fastest average growth rate of 2.5% per year.12 The world’s largest regional percentage increase in population will be in Africa, which expects about 2.3 billion, from this sub-Saharan Africa (SSA) expected to be 1.96 billion by the year 2050.13,14
Ethiopia has made several important international commitments to improve sexual and reproductive health but the service has been amongst the lowest in Africa.15 It is the fast-growing, second most popular nation in Africa.16 The total fertility rate of the country is 4.6, with the highest in a rural region, and least-educated families. Despite contraceptive utilization increase internationally, Ethiopia’s current contraceptive prevalence rate (CPR) remains 36%, from which LAPCM accounts for only 10.4%, of which 0.4% female sterilization, 2% IUCD, and 8% implants which are lowest compared to globally, and unmet need for contraceptives remains high 22%.15 This unmatched expansion of human numbers creates a range of social, economic, and environmental challenges which is associated with high maternal, infant, and child morbidity, mortality rates, and other related problems.17
Due to a lack of open discussion between the couple about reproductive health issues, many women do not know what their partners think about family planning use.18,19 Lack of knowledge, myths, misconceptions, lack of access, desire to have more children, fear of social disapproval, worries of side effects, husband’s opposition and religious prohibition, and negative attitude are among the main barriers in the male involvement of long-acting and permanent contraceptive method (LAPCM) use in Ethiopia.20–22
For many years most family planning programs including research have focused attention primarily on women and offered their services exclusively to women. This has reinforced the belief that family planning is largely a woman’s business and gave little attention to the role of men concerning women’s reproductive health decision-making and behavior.23 In Ethiopia, studies were conducted at a male involvement point of understanding for their contribution to short-acting family planning use. However, little is known about male involvement in LAPCM use of their partners. Thus, this study was aimed to assess male involvement in LAPCM use in West Badewacho, Southern Ethiopia.
Methods
Study Area and Period
The study was conducted in the west Badewacho district, Southern Ethiopia. It is located 353 kilometers away from Addis Ababa, the capital city of Ethiopia. The district has a total of 22 kebeles, 20 rural and 2 urban kebeles. Based on the 2007 census population projection, the total population of the district was 110,702 of which about 56,458 (51%) were female and 54,244 (49%) were male. The contraceptive prevalence rate in the district was 51% and the prevalence of long-acting and permanent contraceptive methods was 9%.24 The study was conducted from April 1–30/2019.
Study Design
A community-based cross-sectional study design was conducted.
Population
All husbands whose wives in the age group of 15–49 years old living in West Badewacho district were the source population. All husbands whose wives in reproductive age (15–49) of the selected kebeles constituted the study population. Currently, married men whose wives age 15–49 years and who were regularly living in the study area for at least six months and men living together with their wives were included. Men who were critically ill during the study period were excluded.
Sample Size Determination and Sampling Procedures
The sample size was calculated for the first objective by using the single population proportion formula (n= (zα/2)2 p (1-p)/d2) where n is the desired sample size, P (11.5%) is the prevalence of male involvement in LAPM, from the previous study done in Mizan-Aman Town,25 Z is the critical value at 95% confidence level of certainty (1.96), d is the margin of error (5%). Then based on the formula n= (1.96)2*0.115*0.885/(0.05)2 =157, assuming 10% non-response rate, 157+157*10% = 173 and considering 2 for design effect 173*2= 346. The sample size was also calculated for the second objective (factor) using Epi-info software version 7, power 80%, and 95% level of confidence and it gives 564. Finally, sample sizes calculated for the second objective (564) were greater than the sample size calculated for the first objective (346). Thus, the final sample size used for this study was 564.
For the sampling procedure, there were 24 kebeles in the district. First kebeles were clustered us urban and rural kebeles then 6 kebeles from rural and one kebele from urban were selected using a simple random (lottery) method. The number of the household for each kebele was seen from the registration book of the health office, kebele as well as the health extension workers. Allocation of proportion to the sample size was done to identify the required number of households for each selected kebele. A systematic sampling method was employed to select the household from each kebele. After that, the first household was selected from the house of respective kebele using the lottery method, and the next household was identified using a systematic sampling technique. When more than one eligible respondent was found in the selected household, only one respondent was chosen by the lottery method. In cases where eligible was not found in the selected household, a revisit has been arranged a minimum of three times, and finally if they were not present considered as non-respondent.
Data Collection Tools and Procedures
The data were collected using pretested, structured and interviewer-administered questionnaires which were adapted and developed with modification from similar previous studies.15,25 It includes socio-demographic characteristics, economic status, reproductive characteristics, knowledge, attitude, and practices towards long-acting and permanent contraceptive use. It was first prepared in English and then translated into Hadiya (local language) by the language expert (person) to check its consistency, the questionnaire was translated back to English by another language expert. Data were collected by seven high school graduate male students who were residing in the study area and supervised by two-degree holder health professionals who were fluent speakers in the local language Hadiya. House to house data collection and a revisit has been arranged a minimum of three times. Intensive supervision was done by the principal investigators and supervisors throughout the data collection period.
Operational Definition
Knowledge
This was measured by 10 knowledge of LAPCM items, and those who scored above 67% had high knowledge. Those who scored 33–67% had moderate knowledge, and those who scored below 33% were categorized as they have low knowledge about LAPCM.25
Attitude
Measured by 7 attitude items and those who scored above 67% of attitude questions of LAPCM had a positive attitude, those who scored from 33–67% had an indifferent way, and those who scored below 33% grouped as they had a negative attitude.25
Male Involvement
Measured by four-questions that had a yes or no response. Respondents were categorized as involved for those who had participated in at least one, and not involved for those who did not participate in the for items.25,26
Data Quality Assurance
To assure the quality of the data, a structured and pretested questionnaire was used. The pretest was done among 28 (5%) currently married men at Jarso kebele which is out of the study area. Based on the pre-test of the questionnaire, the necessary modifications and corrections took place to ensure its validity. The final version of the questionnaire was made from the English language to the local language Hadiya and back-translated to the English language by language experts to ensure its consistency. Two days of training was given for data collectors and supervisor and regular follow-up was done to check the collected data for completeness, accuracy, and consistency throughout the data collection period.
Data Processing and Analysis
The data were coded, checked, entered, and cleaned using Epi-Data 3.1 version software and exported into SPSS version 22 for analysis. The wealth index was constructed using principal component analysis (PCA) by considering locally available household assets to assess economic status. The outcome variable was recoded to dichotomous outcomes either they are involved or not. The male involved was coded as 1 and not involved were coded as ‘0ʹ. Univariate analysis such as simple frequency, a measure of central tendency, and a measure of variability was used to describe the characteristics of participants, and information was presented using tables, narratives, and figures. Bivariate analysis was done to see the association between the independent variable and the outcome variable. Independent variables with a p-value of <0.25 were the candidate for the multi-variable analysis to control confounding factors. Multi-collinearity was checked to see the linear correlation among the independent variables. Hosmer-Lemeshow test was found to be insignificant at (p-value = 0.79) and omnibus tests were significant (p-value≤0.001) which indicated the model was fitted. The adjusted odds ratio along 95% CI was estimated to show the strength and direction and the level of statistical significance was considered at a p-value <0.05.
Ethical Consideration
Ethical clearance was secured from the Haramaya University College of Health and Medical Science Institutional Health Research Ethics Review Committee (IHRERC). The official letter was sent to the West Badewacho district, and the data collection was begun after a permission letter was written to all selected kebeles. The study purpose, procedure, possible risks, and benefits of the study were explained for each participant. Informed, volunteer, signed, and written consent was obtained from each participant. The respondents were assured of confidentiality by excluding their names during the period of data collection. They were informed well that they have the full right to refuse to participate and/or withdraw from the interview at any time if they have any difficulty.
Results
Socio-Demographic Characteristics of Study Participant
From a total of 564 expected participants, 543 were interviewed making a response rate of 96.3%. The mean age of the participants was 34.5 (SD±7) years old. Near half of the respondents, 256 (47.1%) were in the age group of 31 to 40. About three-fourth, 412 (75.9%) of respondents were Hadiya in their ethnicity. The majority, 418 (77.0%) of respondents were protestant followers in their religion and 475 (87.5%) were rural dwellers. Regarding their educational status, about 84 (15.5%) never attended formal education, 128 (23.6%) were able to read and write, 148 (27.3%) attended primary education and 183 (33.7%) attended secondary and above education. More than half, 287 (52.9%) were farmers, more than one fourth, 141 (25.9%) were merchants, and the majority, 444 (81.7%) of participants had lower quartile economic status (Table 1).
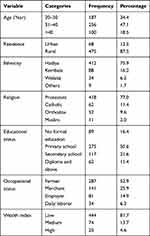 |
Table 1 Sociodemographic Characteristics of Respondents in West Badewacho District, Hadiya Zone, Southern Ethiopia, 2019 (N=543) |
Reproductive Characteristics of Respondents
Among study participants, the average number of total and currently living children was 4.86, and 4.22 per man respectively, while the average desired number of children was 5.46 per man. The majority of respondents, 486 (89.5%) wished to have more children, out of this number, about 42.38% of them want by the preference of the male child. Thirty percent of the respondents preferred to have the next child within 2 years gap, while, 42.5% and 27.5% of the respondents wished to have their next child between 2 and 3 years and after 3 years old gaps respectively (Table 2).
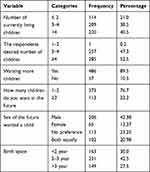 |
Table 2 Reproductive Characteristics of the Study Subjects, West Badewacho District, Hadiya Zone, Southern Ethiopia, 2019 |
Male Involvement in LAPCM Use
Among 543 participants, 108 (19.9%, 95% CI: (16.8, 23.2)) were involved in the LAPCM use of their partner (Figure 1). About 98 (18.0%) of respondents’ wife were utilized LAPCM, 99 (18.2%) participants support their partner, and others use LAPCM, and 87 (16%) of participants gone to the health facility with their wife to discuss LAPCM use with the health care provider.
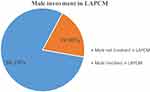 |
Figure 1 Male involvement in long-acting and permanent contraceptive methods use in West Badewacho, Southern Ethiopia, 2019. |
Awareness to LAPCM-Related Characteristics of Respondents
About 486 (89.5%) respondents reported that they heard about LAPCM. The most commonly known LAPCM reported by study participants was Implant 483 (99.4%), followed by IUCD 428 (88.06%). But female sterilization 247 (50.8%) and male sterilization 232 (47.7%) was the least known reported methods. Among those who had ever heard about LAPMs, the majority 367 (75.5%) of them had heard messages of LAPCMs in the last 12 months through the mass media, 63.3% got from health institutions, 60.3% got information from friends and 58.2% got from a family member. Participants were also asked about the advantage of LAPCMs, and about 443 (91.2%) said for the spacing of childbirth, 351 (72.2%) for preventing unwanted pregnancy, 319 (65.6%) for limiting the number of children, and 201 (41.3%) of respondents said it is used to reduce maternal and child death. This study asked about the LAPCM participants currently used method, the most commonly used method by the respondent’s wives was implant 50 (51.01%), and IUCD 42 (42.8%), but no one underwent male sterilization in the study area. Forty percent of study participants discussed LAPCM use with their partner in the last twelve months. Regarding the decision on the current use of LAPCMs, 72 (76.5%) of respondents made the decision jointly, while 20 (20.7%) of the respondents decided by themselves, and 66.4% of current users of LAPCM were using for birth spacing (Table 3).
 |
Table 3 Awareness-Related Characteristics of Respondents in the West Badewacho District, Southern Ethiopia, 2019 (n=543) |
Knowledge and Attitude to LAPCM of Respondents
Nearly half 251 (46.2%) and 233 (42.9%) of married men aware there is an operation to prevent further pregnancy for both women and men respectively. More than half 298 (54.9%) of respondents were aware that IUCD can prevent pregnancy for more than 10 years. One fourth 139 (25.9%) of respondents were aware that IUCD cannot cause cancer. About 105 (19.5%) of participants were aware that IUCD has no influence on sexual intercourse, and 292 (53.8%) were aware of immediate pregnancy after removal of the contraceptive method (Table 4).
 |
Table 4 Knowledge-Related Characteristics of Respondents in West Badewacho District, Hadiya Zone, Southern Ethiopia, 2019 (n=543) |
The attitude of participants on the LAPCM was assessed in this study and about 329 (60.6) participants agreed that the availability of family planning information and service for men is necessary. The majority of married men (70%) believed that the sterilization of both men and women was no acceptable Above four-fifths (83.5%) of married men beliefs that male sterilization cause impotence. About 71.4% of respondents’ beliefs using IUCD restrict routine activity and 77.8% of them beliefs using an implant and IUCD cause infertility for future life (Table 5).
 |
Table 5 Attitude-Related Characteristics of Respondents in West Badewacho District, Hadiya Zone, Southern Ethiopia, 2019 (N=543) |
Factors Associated with Male Involvement in LAPCM Use
In a bivariate analysis, residence, educational status, age of husbands, number of the living child, number of the child wanted in the future, birth spacing, ever heard information, history of using LAPCM, knowledge, and attitude was significantly associated with male involvement in LAPCM use. In the final model (multivariable analysis), discussion with wives, residence, high knowledge, and positive attitude towards LAPCM use were found significantly associated factors with male involvement in LAPCM use (Table 6).
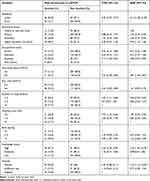 |
Table 6 Factors Independently Associated with Male Involvement in LAPCM Use of Their Partner in West Badewacho District, SNNPR, Ethiopia, 2019 (N=543) |
Discussion
Overall, about 19.9% (95% CI: (16.8, 23.2)) of participants were involved in LAPCM use. Being an urban resident, discussion with wives about LAPCM, having high knowledge, and a positive attitude towards LAPCM use were significantly associated factors.
The finding in this study (19.9%) is higher than the study conducted in Bodit town (13%), and Debre Markos town (8.4%).20,27 But it is lower than from a study conducted in Gedeo town (36%),28 and Afar (42.2%).29 The variation may be due to demographic, socio-cultural variation of the study subjects. For example, participants in the study in Bodit were urban residents which may know the family planning use whereas this study includes both rural and urban residents. The discrepancy could also be due to the definition, and time difference of the study. Some of the studies include male involvement in all family planning methods where this study focused only LAPCM this might decrease the magnitude of male involvement in LAPCM.
This study also assessed factors associated with male involvement in LAPCM use. Participants who have high knowledge of LAPCM were 2.55 times more likely involved in LAPCM than men who had low knowledge about LAPCM. This is consistent with a study done in Tigray, Bodit, Debre Markos, Gedio, and Afar.20,26,28,29 Men who have good knowledge about family planning may more likely have know-how about how to use contraceptives and play roles in couple contraceptive use and continuation, due to this reason husband’s background knowledge of family planning affects their involvement in LAPCM use.
Men who have a positive attitude towards family planning services were 2.16 times more likely to be involved in LAPCM utilization as compared to those who have a negative attitude. This finding is consistent with a study conducted in Debre Markos and Gedio.20,28 The possible reason could be due to those who have a positive attitude towards LAPCM may like the service and they might be interested to involve in their partners’ family planning service. Whereas those who have a negative attitude to LAPCM may even refuse and violet their partner not only to involve but also they may also stop the family planning method used by their partner.
In this study men who had discussed with their wives about LAPCM use were 2.81 times more likely to involve in LAPMs use than those who did not discuss. This finding is consistent with studies done in Bodit, Mizan-Aman, Wolaita Soddo, Kenya, and Nigeria.25,27,30–32 This may be due to through discussion a couple can come to a mutual decision on whether or not to use contraception to plan when to have children and how many to have. Partners may know how to express their desires and feelings without any fears, and easily make out his/her spouse’s attitudes and beliefs regarding LAPM which increases the involvement of the male partner.
Husbands who live in urban were 3.13 times more likely involved in LAPCM utilization compared to those who live in rural areas. This finding is consistent with a study conducted in Bangladesh and Southeast Nigeria.33,34 The possible reason could be due to urban residents tend to have higher literacy and socioeconomic status, enjoy better access to healthcare service, and receives greater media exposure, all of which are likely to improve knowledge of family planning, in general, this may increase the involvement of the partner in LAPCM.
Limitation
Since this study included only men, the practice of their spouses might be different from what is measured by this study, and there might be social-desirability of responses rather than actual knowledge or practices could be response biases.
Conclusion
Male involvement in long-acting and permanent contraceptive method use was low. Being an urban resident, discussion with wives about LAPCM, having a high knowledge of LAPCM, and a positive attitude towards LAPCM use were significantly associated factors. Enhancing male involvement in family planning use through creating community awareness, encouraging inter-spousal communication to enhance decision making, and increasing positive attitude towards LAPCM in the community is crucial to decrease the problem.
Abbreviations
CPR, contraceptive prevalence rate; IUCD, intrauterine contraceptive method; LAPCM, long-acting and permanent contraceptive method; SSA, sub-Saharan Africa.
Data Sharing Statement
The data used for the findings of this study are available from the corresponding author upon reasonable request.
Ethical Approval
The study was conducted following the declaration of Helsinki on human subjects. After the purpose, benefit and risk were briefed, informed consent was obtained from the study participants. Ethical clearance was secured by Haramaya University Institutional Health Research Ethics Review Committee (IHRERC) and official permission was obtained from West Badewacho district health office and municipal.
Acknowledgments
We would like to appreciate Haramaya University. Our heartfelt thanks also extend to the staff of east Badichiwa, supervisors, data collectors, and the study participants for their willingness and cooperation in the data collection process.
Author Contributions
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Disclosure
The authors declare that they have no conflicts of interest in this work.
References
1. Abdel A, Amira O, Busby J, Gilbert R, Cahill DJ, Hollingworth W. Factors affecting unmet need for family planning in Eastern Sudan. BMC Public Health. 2013;13(1):112–165. doi:10.1186/1471-2458-13-112
2. Blumenthal P, Voedisch A, Gemzell-Danielsson K. Strategies to prevent unintended pregnancy: increasing use of long-acting reversible contraception. Hum Reprod Update. 2010;17(1):121–137. doi:10.1093/humupd/dmq026
3. Joshi R, Khadilkar S, Patel M. Global trends in the use of long-acting reversible and permanent methods of contraception: seeking a balance. Int J Gynecol Obstet. 2015;131:S60–S3. doi:10.1016/j.ijgo.2015.04.024
4. Winner B, Peipert J, Zhao Q, Buckel C, Madden T, Allsworth J. Effectiveness of long-acting reversible contraception. N Engl J Med. 2012;366(21):1998–2007. doi:10.1056/NEJMoa1110855
5. UN. United Nations Department of economic and social affairs population division. Trends in contraceptive use worldwide in 2015 2015.
6. Lotke P. Increasing use of long-acting reversible contraception to decrease unplanned pregnancy. Obstet Gynecol Clin N Am. 2015;42(4):557–567. doi:10.1016/j.ogc.2015.07.008
7. United Nations. World family planning. 2017.
8. WHO. Global summit on family planning world health organization. 2017.
9. UNFPA. Choices do not chance UNFPA family planning strategy. 2017.
10. Hubacher D, Mavranezouli I, McGinn E. Unintended pregnancy in sub-Saharan Africa: the magnitude of the problem and potential role of contraceptive implants to alleviate it. Contraception. 2008;78(1):73–78. doi:10.1016/j.contraception.2008.03.002
11. WHO. Family planning, and the post-2015 development agenda. 2015.
12. World Bank 2012. World Development Indicators. World Bank; 2012.
13. Hartmann M, Gilles K, Shattuck D, Kerner B, Guest G. Changes in couple’s communication as a result of a male-involvement family planning intervention. J Health Commun. 2012;17:7. doi:10.1080/10810730.2011.650825
14. Ader A, Belete T, Gebru A, Hagos A, Gebregziabher W. Assessment of the role of men in family planning utilization at edaga-Hamuse Town, Tigray, North Ethiopia. Am J Nurs Sci. 2015;4:4.
15. EDHS. Ethiopia Demographic and Health Survey. Addis Ababa, Ethiopia, and Rockville, Maryland, USA: CSA and ICF; 2016.
16. Population Reference Bureau. World Population Data. 2018.
17. John BJC. Fertility transition: is Sub-Saharan Africa different? Popul Dev Rev. 2012;38(SuPPlement):153–168.
18. Kamal I, Islam MA. Interspousal communication on family planning and its effect on contraceptive adoption in Bangladesh. Asia Pac J Public Health. 2012;24:3. doi:10.1177/1010539511399118
19. FMOH. The National Policy Guidelines and Service Standard for Reproductive Health Services. 2011.
20. Kassa A, Abajobir AA, Gedefaw M. Level of male involvement and associated factors in family planning services utilization among married men in Debremarkos town, Northwest Ethiopia. BMC Int Health Hum Rights. 2014;14:33. doi:10.1186/s12914-014-0033-8
21. Omar J, Roble S. Constructive men’s engagement in reproductive health and HIV in Ethiopia, facilitating policy dialogue. Health Policy Initiative. 2011.
22. Gebremariam A, Addissie A. Knowledge and perception on long acting and permanent contraceptive methods in Adigrat town, Tigray, northern Ethiopia: a qualitative study. Int J Family Med. 2014;2014:1–6. doi:10.1155/2014/878639
23. Girum T, Shegaze M, Tariku Y. The role of currently married men in family planning and its associated factors in Agaro town, South West Ethiopia. Ann Med Health Sci Res. 2017;7.
24. CSA: Population and Housing Census of Ethiopia. The administrative report, Addis Ababa. 2007.
25. Mulatu K, Mekonnen W. Men’s involvement in long-acting and permanent contraceptive use in Mizan-Aman District Southwestern Ethiopia: a community based cross-sectional study. Health Sci J. 2016;10(2):2.
26. Bayray A. Assessment of male involvement in family planning use among men in the south eastern zone of Tigray, Ethiopia. J Med. 2012;2:1–10.
27. Tadesse M, Meskele M, Dana T. The role of male partner on current utilization of long-acting and permanent contraceptive methods in Bodit Town, Southern Ethiopia. J Health Med Nurs. 2016;33.
28. Dereje A, Abainew A, AbdoKurke K. Male involvement in family planning and associated factors among married male in Gedo Town West Shoa Zone, Oromia, Ethiopia. J Culture Soc Dev. 2016;15.
29. Chekole K, Medhanyie G, Medhanyie AA, Gebreslassie MA, Bezabh AM. Husbands’ involvement in family planning use and its associated factors in pastoralist communities of Afar, Ethiopia. BMC J Reprod Health. 2019;16:33. doi:10.1186/s12978-019-0697-6
30. Abraham W, Adamu A, Deresse D. The involvement of men in family planning an application of transtheoretical model in Wolaita SoddoTown South Ethiopia. Asian J Med Sci. 2010;2.
31. Irani L, Speizer SI, Jean- FC. Couple characteristics and contraceptive use among women and their partners in Urban Kenya. Int Perspect Sex Reprod Health. 2014;40:11–20. doi:10.1363/4001114
32. Oyediran KA. Husband-wife communication and couple’s fertility desires among the Yoruba of Nigeria. Afr Popul Stud. 2014;17.
33. Ghos B, Shangfeng T, Sanni Y, Ide S. Factors associated with male involvement in reproductive care in Bangladesh. BMC Public Health. 2017.
34. Ezeanolu E, Lwelunmor J, Asaolu J, Obiefune M, Ezeanolu C, Osuiji A. Impact of male partner’s awareness and support for contraceptives on females intent to use contraceptives in Southeast Nigeria. BMC Public Health. 2015;15:859.
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
