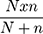Back to Journals » Patient Related Outcome Measures » Volume 11
Antiepileptic Drug Treatment Outcomes and Seizure-Related Injuries Among Adult Patients with Epilepsy in a Tertiary Care Hospital in Ethiopia
Authors Nasir BB, Yifru YM, Engidawork E , Gebrewold MA , Woldu MA , Berha AB
Received 27 December 2019
Accepted for publication 31 March 2020
Published 21 April 2020 Volume 2020:11 Pages 119—127
DOI https://doi.org/10.2147/PROM.S243867
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Robert Howland
Beshir Bedru Nasir,1 Yared Mamushet Yifru,2 Ephrem Engidawork,1 Meron Awraris Gebrewold,2 Minyahil Alebachew Woldu,1 Alemseged Beyene Berha1
1Department of Pharmacology and Clinical Pharmacy, School of Pharmacy, College of Health Sciences, Addis Ababa University (AAU), Addis Ababa, Ethiopia; 2Department of Neurology, School of Medicine, College of Health Sciences, AAU, Addis Ababa, Ethiopia
Correspondence: Beshir Bedru Nasir
Department of Pharmacology and Clinical Pharmacy, School of Pharmacy, AAU, Churchill Avenue, P.O. Box 1176, Addis Ababa, Ethiopia
Email [email protected]
Objective: Anti-epileptic drugs (AEDs) are the primary therapeutic modalities for epilepsy management. However, one-third of epileptic patients continue to experience seizure even with appropriate AED use. Patients with epilepsy are at increased risk for seizure-related injury and they have higher incidences of home, street and work accidents. There is a paucity of data on AED use pattern and treatment outcomes among patients with epilepsy in the tertiary hospitals of Ethiopia. Therefore, the aim of this study was to assess AED use pattern, treatment outcome, and prevalence of seizure-related injury among patients with epilepsy in Tikur Anbessa specialized Hospital (TASH), Ethiopia.
Patients and Methods: An institution-based cross-sectional study was carried out on 291 patients with epilepsy attending the neurology clinic of TASH. A semi-structured questionnaire and data abstraction format were used to collect data through patient interview and medical chart review. Binary logistic regression was utilized to identify the associated factors of treatment outcome.
Results: About 172 (59%) of the patients were taking a single AED, in which phenobarbital, 195 (67%), and phenytoin, 97 (33.3%), were the most frequently prescribed AEDs as monotherapy and combination therapy. Headache, depressed mood and epigastric pain were frequently reported as adverse drug reactions. Seizure-related injury was reported among 78 (26.8%) patients and head injury 15 (5.2%), desntal injury 15 (5.2%), soft tissue injury 14 (4.8%) and burns 10 (3.4%) were the commonest. About two-thirds (191, 65.6%) of the study participants had uncontrolled seizure. Medication adherence and multiple AEDs were significantly associated with treatment outcome.
Conclusion: All the study participants were put on old generation AEDs with phenobarbital being the most frequently used. About two-thirds of the patients had uncontrolled seizure and seizure-related injury is still a serious concern among patients with epilepsy.
Keywords: epilepsy, treatment outcome, seizure-related injuries, Ethiopia
Introduction
Epilepsy is a neurologic disorder characterized by an enduring predisposition to generate epileptic seizures.1 It is a common neurological illness affecting more than 50 million people worldwide and approximately 85% of people afflicted with epilepsy live in developing countries including Ethiopia.2 The ultimate goal of epilepsy management is freedom from seizure and no side effects while having an optimal quality of life.3 Even though the currently available antiepileptic drugs (AEDs) could successfully treat a great proportion of newly diagnosed patients, inappropriate drug therapy in combination with non-adherence is leading to suboptimal seizure control.4 Furthermore, the treatment of epilepsy in developing countries remains far from satisfactory, mainly because of the inaccessibility of medications and suboptimal/lack of information and/or education on epilepsy for both patients and health-care providers.5 Uncontrolled seizures may be associated with adverse effects, psychiatric co-morbidities and cognitive impairments resulting in employment restriction, physical injuries and finally to death.6 Physical injuries are common among people with epilepsy compared to the general population and the occurrences of physical injury has a negative impact on the quality of life among patients with epilepsy and a higher mortality rate compared to the general population.7
Treatment outcome is affected by several factors including drug-related factors, disease-related factors and patient-related factors. Drug-related factors include pharmacokinetics of the drugs, drug-drug interactions and toxicity among others. Similarly, irrational prescribing with respect to drug selection and inappropriate dose will result in poor treatment outcome. Thus, previous studies revealed that only 70% of children and 60% of adults achieved a complete seizure control with AEDs.8–10
Though studies have been conducted in different parts of the world, there is a paucity of established studies regarding treatment outcomes among ambulatory patients with epilepsy and seizure-related injury in Ethiopia. Therefore, the aim of this study was to assess AEDs use pattern, treatment outcomes, and seizure-related injuries among ambulatory patients with epilepsy attending the neurology clinic of Tikur Anbessa Specialized Hospital (TASH) in Ethiopia.
Patients and Methods
Study Design
An institution-based cross-sectional study was conducted among ambulatory patients with epilepsy at the neurology clinic of TASH, which is the largest tertiary referral and teaching hospital in Ethiopia. Data collection was done from 5 June to 28 August 2017.
Sampling and Sample Size Calculations
The sample size was computed based on a single population proportion formula with a proportion of 50% of seizure-related injury and confidence level of 95%, with a z-value of 1.96 (assuming the statistical significance at P=0.05).
Since the total number of patients with epilepsy who had follow-up at TASH were around 1,100, a correction formula was used, with an addition of 5% contingency, and 299 patients were enrolled, but eight patients were excluded due to incomplete data on their medical charts and 291 were used in the study.
N= 1,100 (total patients with epilepsy at (TASH)
n= 384 (sample size by considering the prevalence to be 50%)
A systematic random sampling method was used to recruit the study participants on each day of the data collection process. The sampling fraction (k) varied on different days of data collection as the total number of the study population varied on different days of data collection. It was calculated through dividing the number of the study population available each day by the maximum possible number of patients that could be interviewed on that day. Then every kth (k= 2 or 3 depending on the number of patients available on each day) patient was interviewed with simultaneous medical chart review.
Inclusion Criteria
We included patients who had follow-up at adult neurology clinics of TASH and were diagnosed as cases of seizure disorder or epilepsy, who had been on AEDs therapy for at least 1 year, patients who had complete medical records and were willing to participate in the study.
Study Variables
The dependent variables were treatment outcome (seizure free period) and seizure-related injuries which included any physical injuries that happened due to the seizure. Demographic variables (age, gender, marital status, education, and residential area) and patient clinical characteristics (type of seizure, duration of therapy, presence of ADRs, presence of major drug-drug interactions, number of medications, and presence of comorbid conditions) were the independent variables.
Recruitment of Data Collectors and Data Quality Assurance
Trained clinical pharmacists and nurses were involved in the data collection process. One full day training was given to the data collectors. Pre-test was done on 5% of the sample size to ensure appropriateness of the data collection instruments and the tool was re-prepared with some modifications after inputs were obtained from deep review during the pre-test.
Data Collection Instrument and Collection Process
The relevant information about each patient (demographic data and patients’ clinical characteristics including seizure-related injury) was collected using an interviewer administered questionnaire. The episodes of seizure-related injury was assessed since the diagnosis of epilepsy. Laboratory results, current medications, co-morbidities, relevant previous medical and medication histories were collected using data abstraction format from medical chart review. Micromedex® (Micromedex 2.0.Truven Health Analytics Inc.) drug interaction checker was used to identify significant drug-drug interactions. Adherence was measured using the Morisky Medication Adherence test (Morisky Green Levine test) that consists of four items (MMA4). In the present study, medium and high adherence were considered as adherent and low adherence was considered as non-adherent. Thus, patients having a score of two or more out of four were considered as adherent for their medications. In the present study, definition of epilepsy syndrome and seizure classification was used based on the International League Against Epilepsy (ILAE/2014).11
Treatment outcome was solely assessed by measuring the length of the seizure-free period.
Data Analysis
The data was entered by using Epi Info version 7.2.1 and analyzed using the Statistical Package for Social Science (SPSS) version 21. Univariable binary logistic regression analysis was performed to relate each independent variable with seizure control. Among the univariable analysis, those variables with p<0.25 were selected for multi-variable binary logistic regression analysis. Multivariable binary logistic regression analysis was used to assess the predictability of the independent variables to treatment outcomes and seizure-related injuries. P values < 0.05 were used to declare statistical significance.
Ethics Approval
A letter of ethical clearance was obtained from Addis Ababa University, College of Health Sciences, Institutional Review Board (AAU, CHS, IRB, protocol number = 002/17/SPharma).
Results
Socio Demographic Characteristics
Among 291 study participants, the mean age was 30.2 ±11.4 years and half of them (146, 50.2%) were young adults with a median age of 28 years (range 15–73 years). The majority (185, 63.6%) of the study participants were single and were from urban area 236 (81.1%). Among the study participants, 112 (38.5%) were unemployed and 50 (17.2%) were students (Table 1).
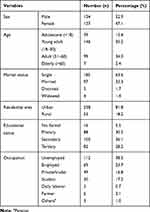 |
Table 1 Socio Demographic Characteristics of Patients with Epilepsy Attending the Neurology Clinic of Tikur Anbessa Specialized Hospital, 2017 |
Clinical Characteristics
The commonest (193, 66.3%) seizure type was GTCS (Generalized tonic-colonic seizure) followed by focal with secondary generalization. The majority of the study participants (244, 83.8%) had follow up for more than 2 years. A total of 68 (23.4%) of them had chronic comorbid conditions (Table 2).
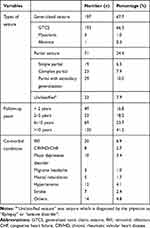 |
Table 2 Clinical Characteristics of Patients with Epilepsy Attending the Neurology Clinic of Tikur Anbessa Specialized Hospital, 2017 |
Pattern of Antiepileptic Drug Use Among the Study Participants
The majority (171, 58.8%) of them were on monotherapy regimen followed by dual (97, 33.3%) and triple therapy (21, 7.2%) (Figure1).
 |
Figure 1 Number of Antiepileptic drugs used among patients with epilepsy attending the Neurology Clinic of Tikur Anbessa Specialized Hospital, 2017. |
Phenobarbital (PHB; 67.0%) was the most frequently prescribed AEDs among the study participants both as monotherapy and combination therapy followed by phenytoin (PHT; 33.3%), carbamazepine (CBZ; 27.1%) and valproic acid (VPA; 18.9%). PHB + PHT was the most frequently used dual therapy regimen regarding AEDs use based on seizure type, while PHB followed by PHT were frequently used for generalized seizure, and CBZ followed by PHB were the most frequently prescribed AEDs for partial seizure. PHB was the most frequently used AED for unclassified seizure and the use of VPA was low for all seizure type (Table 3).
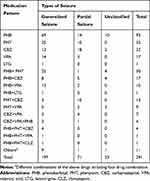 |
Table 3 Types of Antiepileptic Drugs Prescribed with Corresponding Seizure Type Among Patients with Epilepsy Attending the Neurology Clinic of Tikur Anbessa Specialized Hospital, 2017 |
About half (49.5%) of the participants experienced ADRs (adverse drug reactions) that could possibly be associated with AEDs. Headache, depressed mood, and epigastric pain were the top three ADRs encountered (Table 4).
 |
Table 4 Types and Prevalence of ADRs Identified from Patients with Epilepsy Attending the Neurology Clinic of Tikur Anbessa Specialized Hospital, 2017 |
About half (162, 55.7%) of the study participants were adherent to their AEDs and the rest (129, 44.3%) were non-adherent.
Prevalence and Types of Seizure-Related Physical Injuries
The prevalence of seizure-related physical injury among the study participants was found to be 78 (26.8%). Of the 26.8% of seizure-related physical injuries, 15 (5.2%) were head injuries, 15 (5.2%) were dental injuries, 14 (4.8%) were soft tissue injuries including moderate to severe tongue bite, 10 (3.4%) were burns, 8 (2.7%) were abrasions, 7 (2.4%) were fractures, 5 (1.7%) were dislocation of limb joints, and 4 (1.4%) were other injuries including to the eyes. This study also revealed that poor seizure control was significantly associated with risk of having seizure-related physical injuries. Accordingly, patients with uncontrolled seizure were at greater risk by 1.96 times (AOR=1.964, 95% CI=1.05–3.66) of havinge seizure-related injuries as compared to patients with controlled seizure.
Seizure Free Period and Seizure Frequency
The majority (191, 65.6%) of the study participants had uncontrolled seizure (seizure-free period less than 1 year) (Figure 2). Regarding seizure frequency, 37 (12.7%) had more than ten seizure episodes per year, 32 (11.0%) had 6–10 seizure episodes and the rest (76.3%) had 0–5 episodes per year (in the previous 1 year).
 |
Figure 2 Seizure-free period of participants among patients with epilepsy attending the Neurology Clinic of Tikur Anbessa Specialized Hospital, 2017. |
Factors Associated with Poor Treatment Outcomes
In this study, medication adherence and number of AEDs used by the study participants were the only statistically significant factors to affect the treatment outcomes, whereas the association with presence of ADRs and drug-drug interaction were not statistically significant (Table 5).
 |
Table 5 Factors Associated with Treatment Outcomes Among Patients with Epilepsy Attending the Neurology Clinic of Tikur Anbessa Specialized Hospital, 2017 |
Discussion
In this study GTCS was the commonest seizure type encountered, which is in line with studies conducted in Saudi Arabia and Bangladesh.12,13 But it is lower as compared to a study conducted in Jimma.8 Accessibility of diagnostic tools for seizure classification and qualification of expertise might be the reason for the discrepancies. Peoples having focal seizure usually have less serve symptoms as compared to GTCS and they did not seek medical attention in developing countries like Ethiopia that will underestimate the prevalence of focal seizure. Choice of the most appropriate AEDs depends on the proper classification of seizure type. Lack of proper classification of seizure type affects the selection of AEDs and the treatment outcomes.8,14 In this study 7.9% of the patients were not categorized to a specific seizure type which could possibly have contributed to inappropriate drug selection and poor treatment outcomes.
The present study revealed that monotherapy (58.8%) was the preferred treatment regimen. This finding is in line with the findings of Jimma referral hospital (54.5%),8 India (62%)15 and Singapore (63%).16 But it was lower than the findings in Bishoftu hospital (88%),17 in Gondar referral hospital (80.35%)18 and in findings from five European countries (87%).19 The discrepancy might be due to the study settings. This study was conducted in a tertiary care hospital, where complicated and uncontrolled seizures could be referred, which might need combination therapy.
In this study, PHB was the most frequently prescribed drug both as monotherapy and combination therapy. PHB appears to be the most commonly used drug in Ethiopia, as various local studies produced a proportion ranging from 55 to 92.8%.8,17,20 Even though the best AED therapy depends on the extent of optimal seizure control and absence of unacceptable side-effects,21 recent evidence-based treatment recommendation for newly diagnosed patients with epilepsy in developed countries considered PHB a second/third line option. Contrary to this finding, the most frequently prescribed AED was VPA in Saudi Arabia,12 CBZ in Bangladesh,13 PHT in India15 and levetiracetam in London, UK.22 In general, newer AEDs (gabapentin, pregabalin, lamotrigine, levetiracetam, and topiramate) are extensively used in most western countries.19 This might be due to cost of the drugs and their accessibility in resource limited settings. In this study, headache, depressed mood, epigastric pain, hypersomnia, and gingival hyperplasia due to PHT were the most common adverse effects reported by the study participants. Similar findings were obtained in Jimma hospital8 and Bishoftu hospital.17 The use of old generation antiepileptic drugs like PHB might increase the risk of having ADRs.
The prevalence of seizure-related physical injury was 26.8% and head injury, dental injury, soft tissue injury, and burn were the commonest. In the present study only patients who had significant physical damage were considered. Due to lack of complete patient data we could not assess mortality secondary to seizure-related physical injuries. However, we expect that numerous patients will die due to severe injuries and its complication in their home or after they arrived to health institutions. The prevalence and type of injury were in line with a study carried out in Gondar hospital (27.9%) where abrasion, burn and head injury were the commonest,7 in the UK (27%) burn and head injuries were the commonest.23 However, the prevalence in this study was lower than the studies conducted in Thailand (38.6%)24 and Nigeria (45.6%).25 These differences may be due to seizure severity, duration of the seizure, and type of seizure. In contrast, the prevalence of seizure-related injury in a Canadian study was 11%, of which 6.4% were lacerations 5% fractures and 3.2% broken teeth.26 A study in Germany also revealed a lower prevalence of seizure-related injuries (14.0%) in which lacerations (6.2%), abrasions and bruises (3.1%) and fractures (2.2%) were the commonest.27 The lower rate of seizure-related injuries in western studies might be due to the shorter study period, and the fact that the majority of the patients had focal seizure that ha s a low risk of seizure-related injuries and better seizure control due to better treatment options.
In this study, poor seizure control was shown to be a risk factor for seizure-related injury. Similarly, a study conducted in London reported that presence of seizure was significantly associated with physical injuries. The study also showed that the use of multiple AEDs, having depression and having the ADRs of restlessness were significantly associated with seizure-related injuries.22 In addition, a study conducted in Germany revealed that patients with active epilepsy and a refractory course of disease were predictors of seizure-related physical injury.27 Therefore, appropriate treatment should be commenced to improve seizure control and prevent seizure-related injuries.
According to this study only about one-third of the study participants had controlled seizure (seizure-free period of 1 year and above). Our seizure control rate looks lower than the findings in Jima specialized hospital where 56.7%8 and Ambo hospital where 54.3%28 had controlled seizure.
Though different studies have revealed that 60–70% of seizures could be completely controlled with appropriate AEDs,8–10 seizure control in our setup is still suboptimal. The reasons for poor seizure control in the present study may include the study setting, which was conducted in tertiary care specialized hospital, in which most patients with epilepsy who were refractory to AEDs were referred. In addition, inappropriate drug selection with poor medication adherence may contribute for poor treatment outcomes. The remaining two-thirds of patients in this study did not achieve optimal seizure control. In this study, medication adherence and number of AEDs were significantly associated with poor treatment outcomes. The treatment outcome was higher by 72% for patients with high adherence than for patients with low adherence (AOR= 0.28, 95% CI: 0.13–0.64). Furthermore, treatment outcome was higher by 80% and 78% for patients taking single AEDs as compared to two and three AEDs respectively. Poor medication adherence was reported as a significant factor for seizure control.28,29 According to this study those taking multiple AEDs had poor seizure control. The reason might be physicians usually use multiple AEDs for patients having refractory seizure despite the the fact that treatment might not improve the seizure-free period. The other reason might be that use of multiple AEDs increases the potential for drug-drug interactions, can increase the risk of chronic toxicity and compromise medication adherence.30 Therefore, adequate support should be given through reconsideration of choice of AEDs based on seizure type, optimization of dose, improving medication adherence, considering additional non-pharmacologic modalities may be beneficial for patients who are refractory to AEDs. Patient education regarding prevention of seizure-related injuries in relation to their occupation and rehabilitation after the injury is vital for the patients.
Limitations of the Study
Treatment outcome was assessed solely by measuring the length of the seizure-free period without considering seizure severity and frequency. Recall and response biases might have occurred since we relied on the respondents’ retrospective recall of their past medical history. Several factors could affect seizure-related injuries, and treatment outcomes which are not included in this study. Severity of seizure-related injuries and related mortality were not addressed.
Conclusion
The majority of patients were on monotherapy with old generation AEDs (PHB and PHT). Only one-third of the study participants had controlled seizure and the number of AEDs and medication adherence were contributing factors for suboptimal treatment outcome. Furthermore, uncontrolled seizure was shown to increase the risk of seizure-related physical injury. More than a quarter of the study participants (26.8%) had seizure-related physical injury in which, head, dental, soft tissue and burn were the commonest. Therefore, all possible efforts including non-pharmacologic treatment modalities should be implemented to improve the treatment outcomes. Additionally optimal patient education regarding medication adherence should be considered.
Abbreviations
ADR, adverse drug reaction; AEDs, anti-epileptic drugs; AOR, adjusted odds ratio; CBZ, carbamazepine; CLZ, clonazepam; COR, crude odds ratio; GTCS, generalized tonic clonic seizure; ILAE, international league against epilepsy; LTG, lamotrigine; PHB, phenobarbital; PHT, phenytoin; TASH, Tikur Anbessa Specialized Hospital, VPA, valproic acid.
Data Sharing Statement
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Ethics and Consent Statement
The study complied with the Declaration of Helsinki. A letter of ethical clearance was obtained from Addis Ababa University, College of Health Sciences, Institutional Review Board (AAU, CHS, IRB, protocol number = 002/17/SPharma). Written informed consent was obtained from each patient or parents/guardians for patients who were under 18 years to participate in the interview and to extract data from their medical charts. Privacy and confidentiality were ensured during patient interview and medical chart review.
Acknowledgments
The authors would like to thank all the study participants for their time and willingness to participate in the study. We would also like to extend our sincere gratitude to the data collectors, physicians, pharmacists and nurses working in the neurology department of TASH for their support throughout the study period.
Author Contributions
All authors made substantial contributions to conception and design, analysis and interpretation of data, took part in revising the article critically for important intellectual content, gave final approval of the version to be published and agree to be accountable for all aspects of the work.
Funding
The authors received no specific funding for this work.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Fisher RS, WvE B, Blume W, et al. Epileptic seizures and epilepsy: definitions proposed by the International League Against Epilepsy (ILAE) and the International Bureau for Epilepsy (IBE). Epilepsia. 2005;46(4):470–472. doi:10.1111/j.0013-9580.2005.66104.x
2. World Health Organization. Global Burden of Epilepsy and the Need for Coordinated Action at the Country Level to Address its Health, Social and Public Knowledge Implications. Vol. 20. Resolution WHA68. 2015:26.
3. Kerr M, Scheepers M, Arvio M, et al. Consensus guidelines into the management of epilepsy in adults with an intellectual disability. J Intellectual Disabil Res. 2009;53(8):687–694. doi:10.1111/j.1365-2788.2009.01182.x
4. Jones R, Butler J, Thomas V, Peveler R, Prevett M. Adherence to treatment in patients with epilepsy: associations with seizure control and illness beliefs. Seizure. 2006;15(7):504–508. doi:10.1016/j.seizure.2006.06.003
5. Wilby J, Kainth A, Hawkins N, et al. Clinical effectiveness, tolerability and cost-effectiveness of newer drugs for epilepsy in adults: a systematic review and economic evaluation. Health Technol Assess (Rockv). 2005;9. doi:10.3310/hta9150
6. Gilliam F. Optimizing Epilepsy Management: Seizure Control, Reduction, Tolerability, and Co-Morbidities. AAN Enterprises; 2002.
7. Bifftu BB, Tadesse Tiruneh B, Mekonnen Kelkay M, et al. Seizure-related injuries among people with epilepsy at the outpatient department of the University of Gondar Hospital, Northwest Ethiopia: cross-sectional institutional-based study. Neurol Res Inte. 2017;2017.
8. Gurshaw M, Agalu A, Chanie T. Anti-epileptic drug utilization and treatment outcome among epileptic patients on follow-up in a resource poor setting. J Young Pharm. 2014;6(3):47. doi:10.5530/jyp.2014.3.8
9. Garrard J, Cloyd J, Gross C, et al. Factors associated with antiepileptic drug use among elderly nursing home residents. J Gerontol a Biol Sci Med Sci. 2000;55(7):M384–M392. doi:10.1093/gerona/55.7.M384
10. Brodie MJ, Barry SJ, Bamagous GA, Norrie JD, Kwan P. Patterns of treatment response in newly diagnosed epilepsy. Neurology. 2012;78(20):1548–1554. doi:10.1212/WNL.0b013e3182563b19
11. Fisher RS, Acevedo C, Arzimanoglou A, et al. A practical clinical definition of epilepsy. Epilepsia. 2014;55(4):475–482. doi:10.1111/epi.12550
12. Gabr WM, Shams ME. Adherence to medication among outpatient adolescents with epilepsy. Saudi Pharm J. 2015;23(1):33–40. doi:10.1016/j.jsps.2014.05.003
13. Habib M, Khan SU, Hoque MA, et al. Antiepileptic drug utilization in Bangladesh: experience from Dhaka Medical College Hospital. BMC Res Notes. 2013;6(1):1.
14. Azar NJ, Abou-Khalil BW. Considerations in the choice of an antiepileptic drug in the treatment of epilepsy.
15. Sebastian J, Adepu R, Keshava B, Harsha S. Assessment of antiepileptic drugs usage in a South Indian tertiary care teaching hospital. Neurol Asia. 2013;18:2.
16. Hsieh L-P, Huang C-Y. Antiepileptic drug utilization in Taiwan: analysis of prescription using National Health Insurance database. Epilepsy Res. 2009;84(1):21–27. doi:10.1016/j.eplepsyres.2008.11.018
17. Rishe W, Seifu MF, Gelaw BK, Gunasekaran T, Tadesse E, Gebremariam MAM. Drug use evaluation of antiepileptic drugs in outpatient epilepsy clinic of bishoft general hospital, East Shoa, Ethiopia. Indo Am J Pharm Res. 2015;5.
18. Birru EM, Shafi M, Geta M. Drug therapy of epileptic seizures among adult epileptic outpatients of University of Gondar Referral and Teaching Hospital, Gondar, North West Ethiopia. Neuropsychiatr Dis Treat. 2016;12:3213. doi:10.2147/NDT.S119030
19. Groot MC, Schuerch M, de Vries F, et al. Antiepileptic drug use in seven electronic health record databases in Europe: a methodologic comparison. Epilepsia. 2014;55(5):666–673. doi:10.1111/epi.12557
20. Hailu W, Tamiru W, Berhane A, Tsega B, Ergetie Z, Admassie E. Prescription pattern of psychotropic, narcotic and anticonvulsant drugs in Gondar University Hospital, North West Ethiopia. Int J Pharm Sci Rev Res. 2012;2(04):424–428.
21. Christopher C. Pattern of anti-epileptic drug usage in a tertiary referral hospital in Singapore. Neurol Southesas Asia. 1997;2:77–85.
22. Gur-Ozmen S, Mula M, Agrawal N, Cock HR, Lozsadi D, von Oertzen TJ. The effect of depression and side effects of antiepileptic drugs on injuries in patients with epilepsy. Eur J Neurol. 2017;24(9).
23. Téllez‐Zenteno JF, Hunter G, Wiebe S. Injuries in people with self‐reported epilepsy: a population‐based study. Epilepsia. 2008;49(6):954–961. doi:10.1111/j.1528-1167.2007.01499.x
24. Tiamkao S, Kaewkiow N, Pranbul S, Sawanyawisuth K, Group IER. Validation of a seizure-related injury model. J Neurol Sci. 2014;336(1–2):113–115. doi:10.1016/j.jns.2013.10.019
25. Lagunju IA, Oyinlade AO, Babatunde OD. Seizure-related injuries in children and adolescents with epilepsy. Epilepsy Behav. 2016;54:131–134. doi:10.1016/j.yebeh.2015.11.019
26. Camfield C, Camfield P. Injuries from seizures are a serious, persistent problem in childhood onset epilepsy: a population based study. Seizure. 2015;27:80–83. doi:10.1016/j.seizure.2015.02.031
27. Willems LM, Watermann N, Richter S, et al. Incidence, risk factors and consequences of epilepsy-related injuries and accidents: a retrospective, single center study. Front Neurol. 2018;9:414. doi:10.3389/fneur.2018.00414
28. Tefera GM, Woldehaimanot TE, Angamo MT. Poor treatment outcomes and associated factors among epileptic patients at Ambo Hospital, Ethiopia. Gaziantep Med J. 2015;21(1):9–16. doi:10.5455/GMJ-30-163442
29. Obiako O, Sheikh T, Kehinde J, et al. Factors affecting epilepsy treatment outcomes in Nigeria. Acta Neurol Scand. 2014;130(6):360–367. doi:10.1111/ane.12275
30. Arulkumaran K, Palanisamy S, Rajasekaran A. A study on drug use evaluation of anti-epileptics at a multispecialty tertiary care teaching hospital. Int J Pharm Tech Res. 2009;1(4):1541–1547.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.