Back to Journals » International Journal of Nanomedicine » Volume 14
Analysis of toxicity and anticancer activity of micelles of sodium alginate-curcumin
Authors Karabasz A, Lachowicz D , Karewicz A , Mezyk-Kopec R , Stalińska K , Werner E , Cierniak A , Dyduch G, Bereta J , Bzowska M
Received 30 April 2019
Accepted for publication 29 July 2019
Published 6 September 2019 Volume 2019:14 Pages 7249—7262
DOI https://doi.org/10.2147/IJN.S213942
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Anderson Oliveira Lobo
Alicja Karabasz1, Dorota Lachowicz2, Anna Karewicz3, Renata Mezyk-Kopec1, Krystyna Stalińska1, Ewa Werner4,5, Agnieszka Cierniak6, Grzegorz Dyduch7, Joanna Bereta1, Monika Bzowska1
1Department of Cell Biochemistry, Faculty of Biochemistry, Biophysics and Biotechnology, Jagiellonian University, Kraków, Poland; 2Academic Centre for Materials and Nanotechnology, AGH University of Science and Technology, Kraków, Poland; 3Faculty of Chemistry, Jagiellonian University, Kraków, Poland; 4Department of Medical Biotechnology, Faculty of Biochemistry, Biophysics and Biotechnology, Jagiellonian University, Kraków, Poland; 5Department of Animal Reproduction and Anatomy, Faculty of Animal Science, University of Agriculture, Krakow, Poland; 6Department of General Biochemistry, Faculty of Biochemistry, Biophysics and Biotechnology, Jagiellonian University, Kraków, Poland; 7Department of Pathomorphology, Jagiellonian University Medical College, Kraków, Poland
Correspondence: Monika Bzowska
Jagiellonian University in Kraków, Faculty of Biochemistry, Biophysics and Biotechnology, Department of Cell Biochemistry, 7 Gronostajowa St., Kraków 30-387, Poland
Tel +48 12 664 6388
Fax +48 12 664 6388
Email [email protected]
Background: Curcumin is a natural polyphenol with anti-inflammatory, chemopreventive and anticancer activity. However, its high hydrophobicity and poor bioavailability limit its medical application. The development of nanocarriers for curcumin delivery is an attractive approach to overcome its low bioavailability and fast metabolism in the liver. We synthesized a blood compatible alginate-curcumin conjugate, AA-Cur, which formed colloidally stable micelles of approximately 200 nm and, as previously shown, exerted strong cytotoxicity against mouse cancer cell lines. Here we analyze in vivo toxicity and antitumor activity of AA-Cur in two different mouse tumor models.
Method: Potential toxicity of intravenously injected AA-Cur was evaluated by: i) analyses of blood parameters (morphology and biochemistry), ii) histology, iii) DNA integrity (comet assay), and iv) cytokine profiling (flow cytometry). Antitumor activity of AA-Cur was evaluated by measuring the growth of subcutaneously inoculated colon MC38-CEA- or orthotopically injected breast 4T1 tumor cells in control mice vs mice treated with AA-Cur.
Results: Injections of four doses of AA-Cur did not reveal any toxicity of the conjugate, thus indicating the safety of its use. AA-Cur elicited moderate anti-tumor activity toward colon MC38-CEA or breast 4T1 carcinomas.
Conclusion: The tested conjugate of alginate and curcumin, AA-Cur, is non-toxic and safe, but exhibits limited anticancer activity.
Keywords: curcumin, alginate conjugates, in vivo toxicity, antitumor activity
Introduction
Curcumin (diferuloylmethane) is a natural polyphenol from Curcuma longa and has been used in Asian cuisine for more than 5000 years. It has also been employed for centuries in the traditional medicine of the Far East as a painkiller and for the treatment of infections, as well as skin and digestive diseases. The last 50 years of research, both in vitro and in animal models, have confirmed that curcumin has strong anti-inflammatory, antioxidant, antimutagenic, and bactericidal properties, hence it is regarded as a good candidate for the treatment of diabetes, psoriasis, rheumatoid arthritis, chronic enteritis, cardiovascular diseases, Alzheimer’s disease, and cancer.1 The difficulty of this approach, recognized already by Wahlstrom in 1978, lies in the very low bioavailability of curcumin caused by its high hydrophobicity. After oral administration of a very high dose of curcumin to animals (1 g per 1 kg of body mass), over 70% of this compound was excreted in the feces. The rest, absorbed from the gut to the circulation, underwent rapid transformation in the liver into inactive metabolites.2 These observations have been confirmed by numerous clinical studies which showed very low plasma levels of curcumin after its oral administration.
Recently, highly water-soluble complexes of curcumin and Eudragit polymers have been generated for the treatment of inflammatory bowel disease after oral administration.3,4
The problem of poor absorption and immediate curcumin degradation in the liver could be, at least partially resolved by its intravenous application.
However, as the compound dissolves only in organic solvents such as dimethyl sulfoxide (DMSO), ethanol or acetone, a suitable formulation compatible with needs to be developed to enable this route of administration. Two approaches are currently being tested: i) developing a nanomaterial-based curcumin delivery system and ii) introducing chemical modifications into a curcumin molecule to generate its derivative with preserved biological activity but significantly enhanced bioavailability and resistance against liver-mediated degradation. The ideal delivery system should allow an effective and selective transport of curcumin to the diseased tissue, preferably with the omission of the liver to avoid or at least limit curcumin conversion to inactive derivatives. Various nanocarriers have already been proposed for curcumin, including liposomes, poly(lactic-co-glycolic acid) (PLGA) nanocapsules, polysaccharide micro- and nanoparticles, and gold- and silver nanoparticles.5–9 The second approach, the chemical modification of curcumin, often involves its conjugation with hydrophilic polymers such as polyethylene glycol, PLGA, dextran, carboxymethyl chitosan, hyaluronic acid, or alginate.10–17
We have previously described the synthesis of alginate-curcumin conjugate (AA-Cur) forming colloidally stable micelles of approximately 200 nm in diameter. We confirmed that AA-Cur was taken up by cancer cells, was not toxic for cells isolated from human blood or for mouse endothelial cells, and exerted strong cytotoxic activity against different mouse cancer cell lines.16 The promising results of those experiments encouraged us to continue our studies in order to test the in vivo toxicity and anticancer activity of the intravenously administered AA-Cur conjugate.
Materials and methods
Preparation of bioconjugate of alginate and curcumin (AA-Cur)
The bioconjugate of alginate and curcumin (AA-Cur) was synthesized and characterized according to the procedures described by us previously.16 Briefly, 75 mg of N,Nʹ-dicyclohexylcarbodiimide 8 and 30 mg of 4-(dimethyl)aminopyridine was added to 600 mg of alginic acid sodium salt from brown algae (AA) dissolved in 150 mL of DMSO. Next, 25 mL of 0.152 mM curcumin solution in DMSO was added and the mixture was stirred for 6 hrs at 63°C in the atmosphere of argon. Directly after synthesis, the reaction mixture was cooled down and dialyzed in a dialysis tubing (molecular weight cut-off 12 kDa) in room temperature (RT) for the first 24 hrs against DMSO and for the following 7 days against water (pH = 7). The resulting solution was centrifuged (20 mins, 10,000xg at 4°C) to remove solid traces of unbound curcumin and lyophilized.
The successful synthesis was confirmed by 1H Nuclear Magnetic Resonance (1H NMR), Fourier Transform Infrared (FTIR) and UV-Vis absorption spectroscopies.
Apparatus
Dynamic light scattering (DLS) measurements were performed using NANOSIZER-ZS (Malvern Instruments, Malvern, UK). The sample was illuminated with a 633-nm laser, and the intensity of light scattered at 173º was measured by an avalanche photodiode. The measurements were performed at 25°C.
Transmission electron microscopy (TEM) images were obtained using Tecnai TF 20 X-TWIN (FEI) microscope (FEI, Hillsboro, OR, USA). Cross-linked micelles were deposited onto an ultrathin carbon film on a holey carbon. The mean size and the size distribution were obtained by fitting circles around the lattice fringes of the micelles and measuring their diameters.
Cell lines
MC38-CEA is a murine colon adenocarcinoma with stable expression of human carcinoembryonic antigen (CEA). MC38 was a gift from Professor Schabel FM and was stably transfected with DNA coding for CEA by Dr. Michał Bereta (Jagiellonian University, Kraków).18 The Animal Welfare Committee at the Faculty of Biochemistry, Biophysics and Biotechnology, Jagiellonian University has approved the usage of this cell line.
4T1 cell line (murine mammary carcinoma that stably expresses a firefly luciferase) was purchased from Dr Gary Sahagian’s lab (Tufts University, Boston).
Animals
Six-week-old C57BL/6 female mice were obtained from the Animal Facility of the Faculty of Biochemistry, Biophysics and Biotechnology, Jagiellonian University, Kraków, Poland. Six-week-old BALB/c female mice were purchased from the Centre of Experimental Medicine of the Medical University of Białystok, Poland. Animals were housed under controlled conditions and provided with food and water ad libitum. All animal procedures were performed pursuant to Polish law, and specifically to the Act on the Protection of Animals used for Scientific or Educational Purposes (D20150266L), which implements the Directive of the European Parliament and the Council (2010/63/EU). All experimental procedures were in agreement with the guidelines of the Institutional Animal Care and Use Committee (IACUC) and were approved by the 2nd Local IACUC in Kraków.
Analysis of in vivo toxicity of AA-Cur
Intravenous administration of AA-Cur conjugate
C57BL/6 mice were weighted and randomly divided into two experimental groups (n=9). On day 0 of the experiment, the animals were injected in the tail vein with 200 µL of 0.9% NaCl (group 1) or 200 µL of 0.9% NaCl containing AA-Cur in a dose of 70 mg/kg of body mass (bm) (group 2).
Collection of blood, organs, and bone marrow-derived cells for toxicity analysis
Three days after first injection and 1 day before euthanasia blood was taken from the facial vein for hematological analysis. On 30th day of the experiment, the animals were euthanized using an intraperitoneal injection of ketamine (50 mg/kg bm) and xylazine (5 mg/kg bm). Blood was drawn postmortem by cardiac puncture and was allowed to clot and centrifuged (800xg, 10 mins, RT). Serum, isolated by centrifugation (800×g, 10 mins, RT) was used for biochemical analysis and cytokine profiling. Major organs: the liver, spleen, and kidneys were isolated, weighted and transferred to 4% formaldehyde for histological analysis. Additionally, bone marrow-derived cells were isolated by flushing femurs with PBS in order to analyze DNA damage (comet assay). The organ-to-body mass indexes were calculated according to the following equation: organ/body mass index = organ mass/body mass.
Hematological and serum biochemical analyses
The blood collected from facial vein was analyzed for hematological parameters: counts of white blood cells, red blood cells, platelets, granulocytes, lymphocytes, monocytes, hematocrit, mean corpuscular volume, hemoglobin concentration , and red cell distribution width using a fully automated veterinary analyzer ABC Vet (HORIBA®, UK). The samples of sera separated from blood (collected by cardiac puncture) were analyzed using Spotchem EZ Chemistry Analyzer (Woodley; Lancashire, UK) and multiparameter strips: Spotchem II Panel V, according to the manufacturer’s instructions. The following biochemical parameters were measured: activities of ALP and alanine transaminase (ALT), concentrations of total protein (T-Pro), creatinine (Cre) and blood urea nitrogen (BUN).
Quantification of cytokines
Serum concentrations of cytokines: IL-1α, IL-1β, IL-6, IL-10, IL-12p70, IL-17α, IL-23, IL-27, MCP-1, interferon-β (IFN-β), IFN-γ, tumor necrosis factor-α (TNF-α), and GM-CSF were measured using LEGENDplex Mouse Inflammation Panel (13-plex) immunoassay (Biolegend; San Diego, CA, USA) and BD LSRFortessa flow cytometer and analyzed using LEGENDplex software (Biolegend).
Histological analysis
Histological evaluation of 3 µm-thin slices of formalin-fixed, paraffin-embedded organs (liver, kidney, spleen) was performed after staining with hematoxylin/eosin (H&E).
Comet assay
DNA damage in bone marrow-derived cells (1×105 cells/100 µL of PBS) was assessed by comet assay, according to the previously described procedure.19 Fifty cells were randomly selected from two slides per sample and percentage of DNA in the comet tail (% DNA damage) was determined for each cell using epifluorescence microscope (Olympus IX-50, Olympus Corporation, Tokyo, Japan) with CCD camera and COMET ASSAY 2.9 software (Comet Plus, Theta System GmbH, Germany).
Analysis of antitumor activity of AA-Cur in two tumor models: MC38-CEA colon carcinoma and 4T1 breast carcinoma
Mice were weighted and randomly divided into two experimental groups (control and AA-Cur-treated). Tumor cells MC38-CEA or 4T1 were cultured in 10-cm dishes in DMEM medium (Lonza; Basel, Switzerland) supplemented with 10% FBS (Gibco, Waltham, MA, USA). The cells were trypsinized (0.05% trypsin, 0.53 mM EDTA, Lonza) and centrifuged (450×g for 5 mins at RT). After discarding the supernatant, the cells were washed with 10 mL PBS (Lonza), centrifuged and resuspended in PBS to a final density of 5×105 cells/0.1 mL. MC38-CEA cells (5×105) were injected subcutaneously (s.c.) into the left flank of C57BL/6 mice (n=9) and 4T1 cells (5×105) orthotopically into the fourth mammary fat pad of BALB/c mice (n=12). Seven days later, mice were injected intravenously with 0.9% NaCl or AA-Cur (70 mg/kg bm). The animals continued to receive four doses of AA-Cur (in 2- or 3 days intervals). The values of body mass and tumor size were recorded in 3-day intervals. Mice were euthanized 2 or 3 days after the last dose of AA-Cur (on 15th or 21st day of the experiment for C57BL/6 and BALB/c, respectively). Blood and tumors were isolated for further analyses.
Statistical analysis
Statistical significance was analyzed by the multiple t-test with the use of GraphPad Prism 6 (GraphPad Software, Inc., La Jolla, CA, USA), with P<0.05 being considered significant.
Results
Synthesis of AA-Cur
The successful synthesis of AA-Cur conjugate was confirmed by FTIR, 1H NMR and UV-Vis absorption spectroscopies. The detailed synthesis procedure and the obtained AA-Cur spectra were presented and discussed in the Supplementary Materials section of our previous paper.16 Based on the spectrophotometric analysis the curcumin content in 1 g of AA-Cur conjugate was estimated as 45 mg (4.5 wt%). AA-Cur exhibits high solubility in water (7 mg/mL), as can be observed in Figure 1. Due to the amphiphilic character of the conjugate, it aggregates in aqueous solutions forming micelles. The critical micelle concentration (cmc) for AA-Cur was established based on conductometric titration to be 0.654 mg/mL. DLS measurements presented in our previous paper allowed to estimate the average diameter of the micelles formed as 205 nm.16 The average zeta potential value measured for the micelles was −53 mV, which is a value high enough to ensure good colloidal stability of the AA-Cur micelles.
The model studies have shown that at 37 ºC curcumin is released from the conjugate dissolved in phosphate buffer (pH = 7.4) to the oleic acid phase gradually, without burst effect, over a period of 5 hrs.16 When pH of the aqueous phase was decreased to mimic the environment of cancer tissue the release was much faster – almost all curcumin was released within 1 hr. Further studies of the AA-Cur micelles showed that, based on TEM measurements, the diameter of the cross-linked micelle in the dry state is in the range of 160 nm (Figure 2) and is smaller than that obtained from DLS. This is expected, as the hydrodynamic diameter of the micelle includes the solvation shell, which is not present in the TEM images of the dried material. Additional DLS studies performed at various pH values revealed that with increasing pH the AA-Cur micelles tend to swell, but in the physiologically relevant pH range (6.5–7.4) the observed effect is relatively small (<50%). The obtained results are presented in Table 1.
 |
Table 1 Hydrodynamic diameter (dz) for AA-Cur conjugate solutions (0.6 mg/mL) at different pH. The presented results are the average of three measurements |
 |
Figure 2 TEM image of the AA-Cur micelle cross-linked with calcium ions. Abbreviations: AA-Cur, alginate-curcumin conjugate; TEM, transmission electron microscopy. |
Analysis of in vivo biocompatibility of AA-Cur
The analysis of AA-Cur conjugate biocompatibility was performed after repeated intravenous injections of C57BL/6 mice with micellar solution of AA-Cur (70 mg/kg bm, once a week for 4 weeks). The animals were sacrificed on the 30th day of the experiment. This experimental approach allowed to analyze the potential short- and long-term toxicity of the tested micelles.
AA-Cur does not cause any alterations in hematological parameters
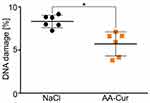
The animals injected with 4 doses of AA-Cur within a month did not present any weight alteration or changes in the size of main internal organs (data not shown) indicating the lack of acute toxicity of the tested micelles. Analysis of the main hematological parameters performed 3 days after first injection of AA-Cur and 1 day before euthanasia (after injections of four doses of the conjugate) also revealed no toxic effects of AA-Cur toward blood cells (Figure 3). Additionally, we did not observe any increase in DNA damage in bone marrow-derived cells of AA-Cur-treated animals, quite contrary, the percentage of damaged DNA was slightly higher in the cells of control- vs AA-Cur-injected mice and may indicate protective activity of AA-Cur (Figure 4).
AA-Cur does not cause liver, kidney, and spleen injury
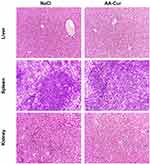
The analysis of organ to body mass indexes did not reveal any alteration in size of major organs such as the liver, kidney, and spleen (data not shown). The potential AA-Cur-induced injury of the liver or kidneys was also analyzed by biochemical analysis of main markers of hepatotoxicity or nephrotoxicity in sera isolated from blood taken postmortem by cardiac puncture (on the 30th day of the experiment). Measurements of serum activities of the main liver enzymes (ALP, ALT) and concentrations of non-enzymatic markers of liver injury (glucose and T-Pro) or renal failure (Cre and BUN) indicated no hepatotoxicity and nephrotoxicity of tested micelles (Figure 5). These results were confirmed by histological assessment, which did not demonstrate any liver or kidney abnormalities (Figure 6).
AA-Cur leads to decrease in basal concentration of several cytokines in healthy animals
We performed the analysis of cytokine levels in sera obtained from C57BL/6 mice exposed to four doses of AA-Cur. We observed decreased concentration of IL-23 and IL-1α in sera of mice injected with AA-Cur micelles in comparison to those of control animals (Figure 7). The concentrations of IFN-γ, IL-12p70, IL-1β were also lower in sera of AA-Cur-treated animals, however, the observed differences did not reach statistical significance. The concentrations of TNF-α, GM-CSF, IL-27, IL17α, IFN-β, IL-6, IL-10, and MCP-1 were similar to those obtained in control animals. Histological analysis also excluded alteration of spleen morphology (Figure 6).
Antitumor activity of AA-Cur
To evaluate the potential anti-tumor activity of AA-Cur, two different mouse tumor models were used. In the first one, C57BL/6 mice were inoculated subcutaneously with colon carcinoma MC38-CEA cells. In the second one, breast cancer 4T1 cells were injected orthotopically, i.e., into the mammary fat pad of BALB/c mice. In both models, 7 days after injection of tumor cells, animals were given the first of four iv doses of AA-Cur. As presented in Figure 8, AA-Cur had moderate effect on the size of MC38-CEA and 4T1 tumors. The mean tumor weight of the mice from control groups was 0.79 g and 0.16 g (for MC38-CEA or 4T1 tumors, respectively) versus 0.45 g and 0.11 g for groups treated with AA-Cur (for MC38-CEA or 4T1 tumors, respectively). Thus, although the changes in the size of tumors did not reach statistical significance, in both models the average tumor masses in mice treated with AA-Cur were more than 30% lower than those in control mice.
Additionally, we evaluated serum cytokine profiles in tumor-bearing mice untreated and treated with AA-Cur. Similarly to the results of cytokine measurements in healthy animals, we observed slightly decreased concentrations of IL-23 and IL-1α in the serum of mice bearing MC38-CEA tumors injected with AA-Cur than in those injected with vehicle, however, the changes did not reach statistical significance (Figure 9). Animals with 4T1 tumors exposed to AA-Cur had lower levels of several cytokines including IL-6, IL-1β, IL-27, IL-17α, IFN-β, however, statistically significant changes were observed only for IFN-γ and IL-10 (Figure 10).
Discussion
Numerous studies have indicated that various delivery systems used for encapsulation of curcumin including liposomes, polymeric nanoparticles, or polymeric micelles might be a promising carriers for poorly aqueous soluble curcumin.20 Another approach to overcoming the problem of low bioavailability of curcumin is its conjugation with hydrophilic polymers. Recently, many different curcumin bioconjugates have been synthesized, however, most of them have only been tested in vitro.12,21–25 Therefore, little is known not only about the systemic toxicity of curcumin-polymer conjugates but also about their biological activity in vivo. Moreover, the toxicity of curcumin either free or encapsulated in nanoparticles has been studied primarily after oral administration, hence little is known about its possible toxic effects after intravenous injection.26–28
The aim of this study was to investigate the toxicity and anti-tumor activity of intravenously administered micelles of AA-Cur, the alginate-curcumin conjugate. We evaluated the toxicity of AA-Cur after administration of four doses of the conjugate. In this study, we did not use free curcumin as a reference because our previous in vitro analyses demonstrated that curcumin dissolved in DMSO (at the final concentration of 5.95 μg/mL, comparable to this in alginate-based micelles) exerted very weak cytotoxicity against the tested tumor cells.16 Alginates are biocompatible, nonimmunogenic and nontoxic polysaccharides approved by US Food and Drug Administration (FDA) for the use in food and pharmaceutical industry.29,30 Therefore, in the experiments concerning toxicity and activity of AA-Cur we used saline (AA-Cur solvent) as a control. The dose of AA-Cur (70 mg/kg of body mass) used in the experiments corresponds to 3.15 mg of intravenously administered pure curcumin per kg bm. The results proved the lack of in vivo toxicity of repeatedly injected AA-Cur in healthy animals. First of all, we did not observe changes in the general hematological parameters. This is in line with the already published results of our in vitro studies, which showed that AA-Cur is not toxic to cells isolated from human blood.16 In contrast, Storka et al demonstrated that intravenous administration of liposomes loaded with curcumin may result in transient changes in red blood cell morphology and increased mean cellular volume of red cells in healthy human subjects. This probably results from interaction between erythrocytes and DPMC (1,2-dimyristoyl-sn-glycero-3-phosphocholine) used for the synthesis of liposomes.31 The serum biochemical analyses demonstrated that AA-Cur-treated animals had no liver or kidney injury. These results are consistent with previously published data, which ruled out the idea of possible hepatotoxicity and nephrotoxicity of curcumin.32–35
Curcumin exerts cancer chemopreventive effects via, among others, protection of cells from DNA damage, however, high doses of curcumin may induce DNA damage by increasing level of ROS (reactive oxygen species) or by influencing activity of various proteins including DNA topoisomerases or tumor suppressor p53.26,36–38 Analysis of DNA damage in bone marrow-derived cells did not show any negative effects of AA-Cur conjugates. Quite the contrary, we observed that the basic level of DNA damage was slightly lower in cells isolated from mice treated with AA-Cur suggesting protective activity of AA-Cur.
Numerous studies have demonstrated anti-inflammatory activity of curcumin manifesting in reduced serum levels of many cytokines such as TNF, IFN-γ, IL-1α, IL-1β, MCP-1, IL-6.39 The majority of this type of research has been carried out using experimental animal models of inflammatory diseases, for example, arthritis, inflammatory bowel disease, multiple sclerosis, colitis or psoriasis.40–44 To exclude any detrimental effect of AA-Cur on the immune system we compared the basal levels of chosen cytokines in sera of control- vs AA-Cur-treated mice. The strongest decrease in cytokine levels in response to AA-Cur was observed for IL-23 and IL-1α. IL-23 is the cytokine essential for inducing differentiation of CD4+ T cells into T helper cells that secrete IL-17 (Th17), which is a key proinflammatory cytokine involved, among others, in the pathogenesis of T-cell-mediated autoimmune diseases.45,46 Our results are in agreement with the studies by Brück et al and Dolati et al, who recently elucidated the mechanism of anti-inflammatory activity of curcumin in IL-23/Th17-mediated autoimmune diseases. They demonstrated that suppression of IL-23 expression in response to curcumin results from activation of STAT3, which negatively regulates transcription of IL-23.47,48 Our observation that in response to AA-Cur the serum levels of several cytokines are slightly decreased suggests that curcumin in this complex has an ability to keep immune system activity at a low basal level.
Our previous in vitro observations demonstrated high cytotoxicity of AA-Cur against various cancer cell lines including murine colon adenocarcinoma MC38-CEA and mammary carcinoma 4T1 cells.16 However, the results of in vivo studies performed using these two tumor models are less spectacular. The regimen of four doses of AA-Cur given at 1-week intervals led to average 44% and 31% inhibition of MC38CEA and 4T1 tumor growth, respectively. However, big variations in the final tumor sizes within experimental groups caused a lack of statistical significance of the tumor size differences between control- and AA-Cur-treated animals.
Similar level of curcumin-mediated tumor growth inhibition was observed by Wang et al, who demonstrated statistically significant ca. 34% reduced size of human breast MDA-MB-231 tumors growing in nude mice injected iv with micelles of hyaluronian-curcumin conjugates as compared to saline-injected animals. However, in this case, mice obtained much higher total doses of curcumin (10 doses of 25 mg curcumin per 1 kg of body mass) than in our studies (4 doses of 3.15 mg curcumin per 1 kg of body mass).49 Similarly, a conjugate of curcumin with albumin (BSA-Cur) administered intraperitoneally, reduced cancer cells growth by 30% in Dalton’s lymphoma ascites mouse model. However, in this case, unlike in solid tumors, all cancer cells were exposed to curcumin immediately after the conjugate administration.50
Detailed pharmacokinetic studies may help to design the optimal therapeutic dosing regimen. It is also possible that AA-Cur will be more effective against hematologic malignancies than solid tumors. Because curcumin is often considered as a drug in combined therapy rather than a monotherapeutic agent, various curcumin formulations might be compatible with other proposed components of therapy.51,52
Many anti-tumor approaches aim at boosting the anti-cancer response of the immune system. There is a growing need for new drugs with potent immunomodulatory activity. Downregulation of IFN-γ synthesis by curcumin has been reported by other groups and was considered as negative effect of this compound on anti-tumor immune response.53,54 On the other hand, studies by Bhattacharyya et al demonstrated that curcumin may prevent Tregs suppressor activity in tumor-bearing animals by downregulating synthesis of IL-10.55
The results of our study indicate that AA-Cur does not have strong immunoregulatory impact on the immune cells of tumor-bearing mice. Whether these small changes in serum cytokine levels reflect changes in anti-tumor activity of immune cells in curcumin-treated mice requires further studies.
Conclusion
We examined toxicity and anticancer activity of alginate-curcumin conjugate (AA-Cur), which forms colloidally stable micelles. Our results indicate that AA-Cur administered iv four times at one-week intervals in a dose of 3.15 mg curcumin per 1 kg bm does not have any toxic effects toward blood- and bone marrow cells as well as the liver, kidney and spleen, and leads to slightly lower serum levels of certain cytokines. The same dosing regimen of AA-Cur results in only moderate reduction of size of two types of tumors. Thus, the design of the best scheme of medical application of this safe curcumin derivative for the therapy of cancer or inflammatory diseases requires further studies.
Acknowledgments
This work was supported by the Grant for employees over 35 – “Program 35+” no. 35p/4/2016 to MB and The Grant for Young Researchers no. BMN 9/2018 to AK funded by the Faculty of Biochemistry, Biophysics and Biotechnology of the Jagiellonian University in Kraków. The Faculty of Biochemistry, Biophysics and Biotechnology of the Jagiellonian University in Kraków was partner of the Leading National Research Center (KNOW) supported by the Polish Ministry of Science and Higher Education. Agnieszka Cierniak’s present affiliation is now the Department of Biochemistry, Faculty of Medicine and Health Sciences, Andrzej Frycz Modrzewski Krakow University, Kraków, Poland.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Salehi B, Stojanović-Radić Z, Matejić J, et al. The therapeutic potential of curcumin: a review of clinical trials. Eur J Med Chem. 2019;163:527–545. doi:10.1016/J.EJMECH.2018.12.016
2. Wahlström B, Blennow G. A study on the fate of curcumin in the rat. Acta Pharmacol Toxicol (Copenh). 2009;43(2):86–92. doi:10.1111/j.1600-0773.1978.tb02240.x
3. Kumar S, Kesharwani SS, Mathur H, Tyagi M, Bhat GJ, Tummala H. Molecular complexation of curcumin with pH sensitive cationic copolymer enhances the aqueous solubility, stability and bioavailability of curcumin. Eur J Pharm Sci. 2016;82:86–96. doi:10.1016/J.EJPS.2015.11.010
4. Kesharwani SS, Ahmad R, Bakkari MA, et al. Site-directed non-covalent polymer-drug complexes for inflammatory bowel disease (IBD): formulation development, characterization and pharmacological evaluation. J Control Release. 2018;290:165–179. doi:10.1016/j.jconrel.2018.08.004
5. Karewicz A, Bielska D, Loboda A, et al. Curcumin-containing liposomes stabilized by thin layers of chitosan derivatives. Colloids Surf B Biointerfaces. 2013;109:307–316. doi:10.1016/j.colsurfb.2013.03.059
6. Klippstein R, Wang JT-W, El-Gogary RI, et al. Passively targeted curcumin-loaded PEGylated PLGA nanocapsules for colon cancer therapy in vivo. Small. 2015;11(36):4704–4722. doi:10.1002/smll.201403799
7. Saranya TS, Rajan VK, Biswas R, Jayakumar R, Sathianarayanan S. Synthesis, characterisation and biomedical applications of curcumin conjugated chitosan microspheres. Int J Biol Macromol. 2018;110:227–233. doi:10.1016/j.ijbiomac.2017.12.044
8. Rojewska A, Karewicz A, Boczkaja K, et al. Modified bionanocellulose for bioactive wound-healing dressing. Eur Polym J. 2017;96:200–209. doi:10.1016/J.EURPOLYMJ.2017.09.010
9. Jaiswal S, Mishra P. Antimicrobial and antibiofilm activity of curcumin-silver nanoparticles with improved stability and selective toxicity to bacteria over mammalian cells. Med Microbiol Immunol. 2018;207(1):39–53. doi:10.1007/s00430-017-0525-y
10. Novelli F, De Santis S, Diociaiuti M, et al. Curcumin loaded nanocarriers obtained by self-assembly of a linear d,l-octapeptide-poly(ethylene glycol) conjugate. Eur Polym J. 2018;98:28–38. doi:10.1016/J.EURPOLYMJ.2017.11.010
11. Waghela BN, Sharma A, Dhumale S, Pandey SM, Pathak C. Curcumin conjugated with PLGA potentiates sustainability, anti-proliferative activity and apoptosis in human colon carcinoma cells. Anto RJ, ed. PLoS One. 2015;10(2):e0117526. doi:10.1371/journal.pone.0117526.
12. Raveendran R, Bhuvaneshwar GS, Sharma CP. Hemocompatible curcumin–dextran micelles as pH sensitive pro-drugs for enhanced therapeutic efficacy in cancer cells. Carbohydr Polym. 2016;137:497–507. doi:10.1016/J.CARBPOL.2015.11.017
13. Ni J, Tian F, Dahmani FZ, et al. Curcumin-carboxymethyl chitosan (CNC) conjugate and CNC/LHR mixed polymeric micelles as new approaches to improve the oral absorption of P-gp substrate drugs. Drug Deliv. 2016;23(9):3424–3435. doi:10.1080/10717544.2016.1189625
14. Jiang Z, Dong X, Liu H, Wang Y, Zhang L, Sun Y. Multifunctionality of self-assembled nanogels of curcumin-hyaluronic acid conjugates on inhibiting amyloid β-protein fibrillation and cytotoxicity. React Funct Polym. 2016;104:22–29. doi:10.1016/J.REACTFUNCTPOLYM.2016.04.019
15. Sarika PR, James NR, Kumar PRA, Raj DK. Galactosylated alginate-curcumin micelles for enhanced delivery of curcumin to hepatocytes. Int J Biol Macromol. 2016;86:1–9. doi:10.1016/J.IJBIOMAC.2016.01.037
16. Lachowicz D, Karabasz A, Bzowska M, Szuwarzyński M, Karewicz A, Nowakowska M. Blood-compatible, stable micelles of sodium alginate – curcumin bioconjugate for anti-cancer applications. Eur Polym J. 2019;113:208–219. doi:10.1016/J.EURPOLYMJ.2019.01.058
17. Kesharwani SS, Kaur S, Tummala H, Sangamwar AT. Multifunctional approaches utilizing polymeric micelles to circumvent multidrug resistant tumors. Colloids Surf B Biointerfaces. 2019;173:581–590. doi:10.1016/J.COLSURFB.2018.10.022
18. Corbett TH, Griswold DP, Roberts BJ, Peckham JC, Schabel FM. Tumor induction relationships in development of transplantable cancers of the colon in mice for chemotherapy assays, with a note on carcinogen structure. Cancer Res. 1975;35(9):2434–2439.
19. Karabasz A, Szczepanowicz K, Cierniak A, Bereta J, Bzowska M. In vitro toxicity studies of biodegradable, polyelectrolyte nanocapsules. Int J Nanomedicine. 2018;13:5159–5172. doi:10.2147/IJN.S169120
20. Naksuriya O, Okonogi S, Schiffelers RM, Hennink WE. Curcumin nanoformulations: a review of pharmaceutical properties and preclinical studies and clinical data related to cancer treatment. Biomaterials. 2014;35(10):3365–3383. doi:10.1016/J.BIOMATERIALS.2013.12.090
21. Zhao G, Dong X, Sun Y. Self-assembled curcumin–poly(carboxybetaine methacrylate) conjugates: potent nano-inhibitors against amyloid β-protein fibrillogenesis and cytotoxicity. Langmuir. 2019;35(5):1846–1857. doi:10.1021/acs.langmuir.8b01921
22. Tian C, Asghar S, Xu Y, et al. The effect of the molecular weight of hyaluronic acid on the physicochemical characterization of hyaluronic acid-curcumin conjugates and in vitro evaluation in glioma cells. Colloids Surf B Biointerfaces. 2018;165:45–55. doi:10.1016/j.colsurfb.2018.02.016
23. Bai F, Diao J, Wang Y, et al. A new water-soluble nanomicelle formed through self-assembly of pectin–curcumin conjugates: preparation, characterization, and anticancer activity evaluation. J Agric Food Chem. 2017;65(32):6840–6847. doi:10.1021/acs.jafc.7b02250
24. Gelderblom H, Verweij J, Nooter K, Sparreboom A. Cremophor EL: the drawbacks and advantages of vehicle selection for drug formulation. Eur J Cancer. 2001;37(13):1590–1598. doi:10.1016/S0959-8049(01)00171-X
25. Chaharband F, Kamalinia G, Atyabi F, Mortazavi SA, Mirzaie ZH, Dinarvand R. Formulation and in vitro evaluation of curcumin-lactoferrin conjugated nanostructures for cancerous cells. Artif Cells Nanomed Biotechnol. 2018;46(3):626–636. doi:10.1080/21691401.2017.1337020
26. López-Lázaro M. Anticancer and carcinogenic properties of curcumin: considerations for its clinical development as a cancer chemopreventive and chemotherapeutic agent. Mol Nutr Food Res. 2008;52(S1):S103–S127. doi:10.1002/mnfr.200700238
27. Choi YH, Han DH, Kim S, et al. A randomized, double‐blind, placebo‐controlled trial to evaluate the role of curcumin in prostate cancer patients with intermittent androgen deprivation. Prostate. 2019;79(6):614–621. doi:10.1002/pros.23766
28. Lv K-J, Chen T-C, Wang G-H, Yao Y-N, Yao H. Clinical safety and efficacy of curcumin use for oral lichen planus: a systematic review. J Dermatolog Treat. 2018;1–7. doi:10.1080/09546634.2018.1543849
29. Szekalska M, Puciłowska A, Szymańska E, Ciosek P, Winnicka K. Alginate: current use and future perspectives in pharmaceutical and biomedical applications. Int J Polym Sci. 2016;2016:1–17. doi:10.1155/2016/7697031
30. Sachan NK, Pushkar S, Jha A, Bhattcharya A. Sodium alginate: the wonder polymer for controlled drug delivery. J Pharm Res. 2009;2(8):1191–1199.
31. Storka A, Vcelar B, Klickovic U, et al. Safety, tolerability and pharmacokinetics of liposomal curcumin in healthy humans. Int J Clin Pharmacol Ther. 2015;53(1):54–65. doi:10.5414/CP202076
32. Dattani JJ, Rajput DK, Moid N, Highland HN, George LB, Desai KR. Ameliorative effect of curcumin on hepatotoxicity induced by chloroquine phosphate. Environ Toxicol Pharmacol. 2010;30(2):103–109. doi:10.1016/j.etap.2010.04.001
33. Serairi Beji R, Ben Mansour R, Bettaieb Rebey I, et al. Does Curcuma longa root powder have an effect against CCl4-induced hepatotoxicity in rats: a protective and curative approach. Food Sci Biotechnol. 2019;28(1):181–189. doi:10.1007/s10068-018-0449-3
34. Alharbi B, Fadda L, Ali HM. Evaluation of the renoprotective effect of nano turmeric against toxic dose of copper sulfate: role of vascular cell adhesion molecule-1, kidney injury molecule-1, and signal transducer and activator of transcription 3 protein expressions. J Biochem Mol Toxicol. 2019;33(2):e22243. doi:10.1002/jbt.22243
35. Edrees NE, Galal AAA, Abdel Monaem AR, Beheiry RR, Metwally MMM. Curcumin alleviates colistin-induced nephrotoxicity and neurotoxicity in rats via attenuation of oxidative stress, inflammation and apoptosis. Chem Biol Interact. 2018;294:56–64. doi:10.1016/j.cbi.2018.08.012
36. Ahsan H, Hadi SM. Strand scission in DNA induced by curcumin in the presence of Cu(II). Cancer Lett. 1998;124(1):23–30. doi:10.1016/s0304-3835(97)00442-4
37. Blasiak J, Trzeciak A, Kowalik J. Curcumin damages DNA in human gastric mucosa cells and lymphocytes. J Environ Pathol Toxicol Oncol. 1999;18(4):271–276.
38. Martín-Cordero C, López-Lázaro M, Gálvez M, Jesús Ayuso M. Curcumin as a DNA topoisomerase II poison. J Enzyme Inhib Med Chem. 2003;18(6):505–509. doi:10.1080/14756360310001613085
39. Aggarwal BB, Harikumar KB. Potential therapeutic effects of curcumin, the anti-inflammatory agent, against neurodegenerative, cardiovascular, pulmonary, metabolic, autoimmune and neoplastic diseases. Int J Biochem Cell Biol. 2009;41(1):40–59. doi:10.1016/j.biocel.2008.06.010
40. Holt PR, Katz S, Kirshoff R. Curcumin therapy in inflammatory bowel disease: a pilot study. Dig Dis Sci. 2005;50(11):2191–2193. doi:10.1007/s10620-005-3032-8
41. Jian Y-T, Mai G-F, Wang J-D, Zhang Y-L, Luo R-C, Fang Y-X. Preventive and therapeutic effects of NF-kappaB inhibitor curcumin in rats colitis induced by trinitrobenzene sulfonic acid. World J Gastroenterol. 2005;11(12):1747–1752. doi:10.3748/wjg.v11.i12.1747
42. Billerey-Larmonier C, Uno JK, Larmonier N, et al. Protective effects of dietary curcumin in mouse model of chemically induced colitis are strain dependent. Inflamm Bowel Dis. 2008;14(6):780–793. doi:10.1002/ibd.20348
43. Deguchi Y, Andoh A, Inatomi O, et al. Curcumin prevents the development of dextran sulfate Sodium (DSS)-induced experimental colitis. Dig Dis Sci. 2007;52(11):2993–2998. doi:10.1007/s10620-006-9138-9
44. Funk JL, Oyarzo JN, Frye JB, et al. Turmeric extracts containing curcuminoids prevent experimental rheumatoid arthritis. J Nat Prod. 2006;69(3):351–355. doi:10.1021/np050327j
45. Geisel J, Bruck J, Glocova I, et al. Sulforaphane protects from T cell-mediated autoimmune disease by inhibition of IL-23 and IL-12 in dendritic cells. J Immunol. 2014;192(8):3530–3539. doi:10.4049/jimmunol.1300556
46. Xie L, Li X-K, Funeshima-Fuji N, et al. Amelioration of experimental autoimmune encephalomyelitis by curcumin treatment through inhibition of IL-17 production. Int Immunopharmacol. 2009;9(5):575–581. doi:10.1016/j.intimp.2009.01.025
47. Brück J, Holstein J, Glocova I, et al. Nutritional control of IL-23/Th17-mediated autoimmune disease through HO-1/STAT3 activation. Sci Rep. 2017;7(1):44482. doi:10.1038/srep44482
48. Dolati S, Ahmadi M, Rikhtegar R, et al. Changes in Th17 cells function after nanocurcumin use to treat multiple sclerosis. Int Immunopharmacol. 2018;61:74–81. doi:10.1016/j.intimp.2018.05.018
49. Wang K, Guo C, Dong X, et al. In vivo evaluation of reduction-responsive alendronate-hyaluronan-curcumin polymer-drug conjugates for targeted therapy of bone metastatic breast cancer. Mol Pharm. 2018;15(7):2764–2769. doi:10.1021/acs.molpharmaceut.8b00266
50. Aravind SR, Krishnan LK. Curcumin-albumin conjugates as an effective anti-cancer agent with immunomodulatory properties. Int Immunopharmacol. 2016;34:78–85. doi:10.1016/J.INTIMP.2016.02.010
51. Hong Y, Che S, Hui B, et al. Lung cancer therapy using doxorubicin and curcumin combination: targeted prodrug based, pH sensitive nanomedicine. Biomed Pharmacother. 2019;112:108614. doi:10.1016/J.BIOPHA.2019.108614
52. Kesharwani SS, Kaur S, Tummala H, Sangamwar AT. Overcoming multiple drug resistance in cancer using polymeric micelles. Expert Opin Drug Deliv. 2018;15(11):1127–1142. doi:10.1080/17425247.2018.1537261
53. Halder RC, Almasi A, Sagong B, Leung J, Jewett A, Fiala M. Curcuminoids and ω-3 fatty acids with anti-oxidants potentiate cytotoxicity of natural killer cells against pancreatic ductal adenocarcinoma cells and inhibit interferon γ production. Front Physiol. 2015;6. doi:10.3389/fphys.2015.00129.
54. Fiala M. Curcumin and omega-3 fatty acids enhance NK cell-induced apoptosis of pancreatic cancer cells but curcumin inhibits interferon-γ production: benefits of omega-3 with curcumin against cancer. Molecules. 2015;20(2):3020–3026. doi:10.3390/molecules20023020
55. Bhattacharyya S, Md Sakib Hossain D, Mohanty S, et al. Curcumin reverses T cell-mediated adaptive immune dysfunctions in tumor-bearing hosts. Cell Mol Immunol. 2010;7(4):306–315. doi:10.1038/cmi.2010.11
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.