Back to Journals » Journal of Pain Research » Volume 10
Age differences in salivary markers of inflammation in response to experimental pain: does venipuncture matter?
Authors Cruz-Almeida Y , Aguirre M, Sorenson H, Tighe P, Wallet SM, Riley JL III
Received 31 March 2017
Accepted for publication 9 August 2017
Published 3 October 2017 Volume 2017:10 Pages 2365—2372
DOI https://doi.org/10.2147/JPR.S138460
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Katherine Hanlon
Yenisel Cruz-Almeida,1–3 Maria Aguirre,1,4 Heather Sorenson,4,5 Patrick Tighe,1,6 Shannon M Wallet,4,5 Joseph L Riley III1,4
1Pain Research and Intervention Center of Excellence, 2Institute on Aging, 3Department of Aging and Geriatric Research, 4Department of Community Dentistry & Behavioral Science, 5Department of Oral Biology, 6Department of Anesthesiology, University of Florida, Gainesville, FL, USA
Abstract: An important consideration in mechanistic research using biomarkers should include the use of saliva as an alternative to blood. The use of saliva would allow the study of susceptible populations such as older adults where venipuncture may not be feasible. Although saliva has been most commonly used to measure cortisol and tumor necrosis factor-α (TNFα), there is limited evidence that other cytokines found in saliva significantly change in response to laboratory-induced pain. Therefore, the aim of the current preliminary study was to characterize the time course, duration and magnitude of changes of commonly measured pro- (interleukin [IL]-6, IL-8) and anti-inflammatory (IL-10, IL-4) cytokines in saliva samples and to test for age-related differences in separate experimental painful and non-painful control sessions. In addition, we also tested whether venipuncture results in significant cytokine alterations similar to a painful stimulus in a non-painful, non-venipuncture control session. All cytokines were significantly induced by the cold pressor task compared to a warm control session (p < 0.001). Specifically, healthy older adults experienced greater salivary changes in all cytokines during the cold pressor session compared to younger adults in the non-painful sessions (p < 0.001). There were no significant differences between the venipuncture and non-venipuncture sessions across all cytokines (p > 0.05). Our findings support the use of saliva as a substitute for blood in both young and older healthy individuals to measure changes after experimental pain stimulation. In addition, venipuncture alone is not sufficient to induce IL-6, IL-8, IL-10 and IL-4. Future studies in the community are urgently needed to validate and further move translational mechanistic pain research to those populations most underrepresented in clinical research.
Keywords: salivary markers, experimental pain, age, venipuncture
Introduction
The Institute of Medicine report highlights the significant burden of pain to our nation and the need to enhance the understanding of pain mechanisms through increased levels of pain research.1 Translational pain research relies on the administration of standardized stimuli using validated experimental protocols in the laboratory and measuring targeted biomarker responses. These biomarkers can provide the insight needed to address specific questions of interest. Specifically, results of mechanistic human laboratory studies may potentially offer a link between basic animal research and studies in people with or at risk for chronic pain. One area of inquiry that is appropriate for these study designs is the associations between expression of immune biomarkers and experimental pain.2–5 These studies typically examine plasma levels of various cytokines following administration of painful stimuli. In addition, other studies have examined immune biomarkers in chronic pain samples.6–8
The study of biomarkers in susceptible individuals including older and pediatric populations where venipuncture may become a medical complication may benefit from the use of saliva as an alternative to blood. The use of saliva as a diagnostic sample provides a noninvasive, cost-efficient method of sample collection without the need for highly trained professionals. Saliva collection is far more practical and safe compared to invasive methods of sample collection, because of the infection risk from contaminated needles during, for example, blood sampling. Furthermore, the use of saliva could increase the availability of research to remote and impoverished regions.
Although saliva has been commonly used to reliably measure cortisol in studies related to psychological and social stress,9–11 there is limited evidence that immune biomarkers found in saliva significantly change in response to laboratory-induced pain.2–5 Along those lines, we have previously reported age-related differences in blood cytokines after experimental pain,4 but it is not currently known whether these differences can be equally measured in saliva samples. The use of saliva as a reliable substitute for blood would provide an avenue for biomarker measurement in large community-based pain studies that would otherwise not be feasible (i.e., putting a central line in community-dwelling older adults for repeated biomarker measurements). Therefore, the aim of the current study was to characterize the time course, duration and magnitude of changes of cytokines in saliva samples and to test for age-related differences in separate experimental painful and non-painful control sessions. Given that venipuncture alone may lead to increases in circulating biomarkers, we also tested whether venipuncture results in significant alterations to the immune markers similar to a painful stimulus as evidenced by measurable changes in saliva biomarkers in a non-painful, non-venipuncture control session. We hypothesized that participants will show increased saliva biomarker concentrations in response to painful cold compared to a non-painful control stimulus tested on separate experimental sessions; 2) older participants will show greater saliva biomarker concentrations over time and across sessions compared to younger adults and 3) participants will show greater saliva biomarker concentrations following a non-painful session with venipuncture compared to a non-painful session without venipuncture on separate days. We hypothesized greater immune response in older adults consistent with the inflammation theory of aging, also called “inflamm-aging” (inflammation + aging), which links between immune changes and the increased incidence of age-related diseases.12,13
Materials and methods
The University of Florida Institutional Review Board approved the study, and all participants provided written informed consent for their data to be used in the study. We have previously reported results of the blood sample in a separate publication.4 The current report focuses on the saliva collection with and without venipuncture, although we reference the blood samples for comparison purposes only and detailed plasma data have been previously published.4
Participants
Healthy study participants were free of chronic and/or systemic diseases. Potential study participants were screened over the phone and again in person during their first visit. As previously explained,4 the exclusion criteria included: serious mental health conditions (e.g., schizophrenia, bipolar disorder and severe depression), systemic diseases (e.g., uncontrolled hypertension, diabetes and thyroid problems), neurological problems with aberrations in somatosensory and pain perception, currently receiving pain treatment for chronic pain (e.g., low back pain and postherpetic neuralgia) or any other ongoing pain problems (e.g., headaches, arthritis and injury-related pain) and the current use of analgesics, narcotics or any other tobacco products. Females who were pregnant or trying to get pregnant were also excluded from the study. The day preceding their session, participants were instructed to go to sleep at their normal bedtime and to avoid any vigorous exercise past 12 a.m. Regarding their intake, they were also instructed to have breakfast no later than 1 hour before their scheduled visit, avoid foods high in sugar, fat or acidity and to avoid dairy products and beverages with any caffeine or alcohol content. Each participant had their visits scheduled after 11 a.m. and at the same time for each of their respective sessions. Before each experimental session, participants were assessed by a dentist at the Dental Clinical Research Center (CRC) to assess oral health, and the presence of oral inflammatory conditions as oral local inflammation (e.g., gingivitis and periodontal disease) may confound measures of salivary inflammation.
The study subjects were eight younger healthy adults (four males, four females) with a mean age of 21.4 years (SD = 5.8) and eight older healthy adults (four males, four females) with a mean age of 68.3 years (SD = 6.3). There were no differences in body mass index between the younger sample (24.6, SD = 3.0) and older sample (24.8, SD = 2.5).
Experimental sessions
All sessions were carried out at the University of Florida Clinical and Translational Science Institute (CTSI) CRC in a quiet, standardized clinic environment. We conducted three experimental sessions on 3 separate days with the order of experimental sessions counterbalanced across subjects and at least 2 days between sessions. For all female participants, nurses were available on staff to supervise the urine collection for pregnancy testing. For the collection of vitals, participants sat in a reclining chair and rested for 5 minutes before the collection of their first blood pressure reading. A second blood pressure measurement was taken 5 minutes later. If the two readings differed by more than 5%, participants were instructed to rest for an additional 5 minutes and a third blood pressure measurement was taken.
Cold pressor task (CPT): painful experimental session with venipuncture
The CPT methodology for this study is identical to that which has been previously published.4 Staff nurses inserted an indwelling catheter in subjects’ left forearm. After a resting period of 15 minutes, participants’ baseline salivary samples were collected. Participants then immersed a foot in cold water for their exposure to painful stimuli (i.e., CPT). Water temperatures were sex specific, as our previous work has shown men and women to experience equivalent levels of pain at different temperatures (8°C and 10°C, respectively).14 The water level was set at a height of 7 cm and was constantly recirculated to keep the stimulated area consistent and prevent the local warming/cooling of water. The cold stimulus was administered in four 60-second trials with a 60-second rest/withdrawal period between trials. Subjects provided ratings of cold pain during each of four 60-second trials at 15, 30 and 45 seconds for a total of 12 pain ratings. Water temperatures were adjusted as needed to ensure participant pain ratings remained between 40 and 50 (Visual Analog Scale [VAS]: 0 = no pain and 100 = intolerable pain). For example, if a participant indicated a VAS pain rating of below 40 during a CPT trial, the temperature was decreased for the subsequent trial. Additional samples of saliva were collected at 3, 15, 30, 45, 60, 90 and 120 minutes later (Figure 1).
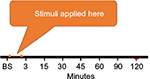  | Figure 1 Saliva samplings across all experimental sessions. Abbreviation: BS, baseline. |
Thermal warm: non-painful experimental session with venipuncture
Exactly as mentioned earlier, staff nurses inserted an indwelling catheter in the left forearm and subjects rested for an additional 15 minutes. Testing began with collection of a baseline salivary sample followed by exposure to the non-painful stimuli (i.e., warm control). The warm stimulus was similarly administered in four trials of about 60 seconds each with a 60-second rest/withdrawal period between trials. Subjects were asked to rate the warm stimulus using a VAS (0 = no warm sensation and 100 = maximal warm sensation). Testing temperatures during this session were kept between 32° and 35° with an increasing ramp of 1°/second. Additional saliva samples were collected at 3, 15, 30, 45, 60, 90 and 120 minutes later (Figure 1).
Thermal warm: non-painful experimental session without venipuncture
During this session, the subjects rested for an additional 15 minutes with no catheter placement (i.e., no venipuncture procedure). Testing began with collection of a baseline salivary sample followed by exposure to the warm control exactly as mentioned earlier. Additional saliva samples were collected at 3, 15, 30, 45, 60, 90 and 120 minutes later (Figure 1).
Sample collection and analysis
CTSI nurses followed established protocols for saliva collection using Salivettes, where a sponge is gently chewed and rolled around the mouth for 2 minutes. This method of collection is commonly used for obtaining total salivary cortisol concentrations.15 Subjects were asked not to brush their teeth as well as to avoid acidic and milk-containing drinks at least 30 minutes before arriving at the laboratory. Subjects were also asked to drink plenty of fluids before the sessions, and after each salivary collection we provided eight ounces of water for rehydration. All samples were immediately placed on ice and transported to the CRC laboratory where they were centrifuged at 12,000 rpm for 15 minutes. Samples were immediately stored at −80°C at time of collection and remained frozen until the time of measurement.
Multiplex soluble mediator analysis
Saliva soluble mediators were qualitatively and quantitatively evaluated, utilizing the MILLIPLEX XMAP human cytokine/chemokine-premixed 13-Plex assay (EMD Millipore, Billerica, MA, USA). The soluble mediators were probed according to the manufacturer’s protocols. Briefly, saliva and antibody-coated beads were added to 96-well primed filter plate and allowed to incubate overnight at 4°C. Following three washes, biotinylated detection antibodies were allowed to incubate for 1 hour at room temperature, after which streptavidin (SAV)–phycoerythrin was allowed to incubate for 30 minutes. Following three washes, beads were resuspended in sheath fluid and reactivity acquired using a Luminex 200 IS system (Luminex, Austin, TX, USA). Concentrations in picogram per milliliter were determined using a standard curve, five-parameter logistics and Milliplex analyst (Viagene, Tampa, FL, USA).
Statistical analysis
The dependent variables for this study were circulating pro-inflammatory (interleukin [IL]-6, IL-8) and anti-inflammatory (IL-10, IL-4) cytokine concentrations expressed in picogram per milliliter, adjusted for baseline levels calculated as poststimulation – baseline. This study tested the following hypotheses: 1) participants will show increased saliva biomarker concentrations in response to painful cold compared to a non-painful control stimulus tested on separate experimental sessions; 2) older participants will show greater saliva biomarker concentrations across sessions compared to younger adults and 3) participants will show greater saliva biomarker concentrations following a non-painful session with venipuncture compared to a non-painful session without venipuncture on separate days.
To test our proposed hypotheses, we employed a repeated-measures ANOVA examining differences in saliva concentrations at baseline, 3, 15, 30, 45, 60, 90 and 120 minutes for the three sessions of interest (i.e., cold pressor with venipuncture, non-painful venipuncture and non-painful/non-venipuncture) across age groups with sex as a covariate. To test hypotheses 1 and 3, the primary independent variable of interest was “session,” which tested the magnitude of the overall biomarker response across the sessions. After a significant main effect, post hoc analyses were undertaken to examine differences between the painful versus non-painful sessions (hypothesis 1) and between the non-painful/venipuncture and non-painful/non-venipuncture sessions (hypothesis 3). For hypothesis 2, we examined the “time X age X session” interaction effect to test whether age differences in saliva biomarker expression were dependent on type of session as well as over time. Mauchly’s test of sphericity assessed whether the assumption of sphericity had been violated, and if so, we applied the Greenhouse–Geisser correction. Data analysis was performed using IBM SPSS v23 (IBM Corporation, Armonk, NY, USA).
Results
Detailed health and demographic data for these participants have been previously reported.4 Half of the participants were nonpregnant females of Caucasian origin, and the younger individuals were undergraduate students at the University of Florida. In summary, on the day of testing, these individuals were queried about present or recent illness and/or infections including cold/flu symptoms. Participants were also instructed the previous day to avoid alcoholic beverages, to go to sleep and wake up the next morning approximately at the same time they usually did and not to exercise vigorously up to 2 hours before the experimental testing session was scheduled including to come with plenty of time as not to feel rushed or stressed. We queried each participant, and if any of the abovementioned scenarios were endorsed the participants were rescheduled. We had to reschedule one participant because an oral lesion was found right before an experimental session, and another participant’s data were not included because he/she had participated in vigorous physical activity before arriving for a session. Across the two sessions that participants experienced venipuncture, there was not a statistically significant difference between how the older (16.3 ± 11.8) versus the younger (11.5 ± 9.0, p = 0.383) participants rated how painful was the venipuncture procedure. Finally, we also found that the time course of the peak levels of cytokines in the CPT session was nearly identical in saliva and plasma (Table 1). Similarly, peak values of saliva and plasma highly correlated in the total sample (Table 2) with effect sizes for changes from baseline to peak also similar, only smaller in saliva compared to plasma (Table 3).
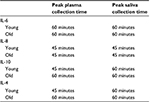  | Table 1 Time of peak levels of cytokines in the CPT session in saliva and plasma Note: Young: 18–25 years old, old: >65 years old. Abbreviations: CPT, cold pressor task; IL, interleukin. |
  | Table 2 Correlations between peak values of saliva and plasma in the total sample Abbreviation: IL, interleukin. |
  | Table 3 Effect sizes for changes from baseline to peak in plasma and saliva Abbreviation: IL, interleukin. |
IL-6
The repeated-measures ANOVA revealed a significant effect of “session” (F[2,13] = 19.2, p < 0.001) with post hoc comparisons indicating that saliva IL-6 concentrations were significantly higher in the CPT (i.e., painful) compared to the warm control (i.e., non-painful) sessions (Bonferroni adjusted p < 0.001). However, there were no significant differences between the non-painful/venipuncture and non-painful/non-venipuncture sessions (p > 0.05). The “time X age X session” interaction was statistically significant (F[14,1] = 5.1, p < 0.05) with post hoc tests indicating that older adults had a greater IL-6 saliva response after the CPT at the 60-minute time point (p < 0.05, Figure 2A).
IL-8
The doubly repeated-measures ANOVA revealed a significant effect of “session” (F[2,13] = 36.8, p < 0.001) with post hoc comparisons indicating that saliva IL-8 concentrations were significantly higher in the CPT (i.e., painful) compared to the warm control (i.e., non-painful) sessions (Bonferroni adjusted p < 0.001). However, there were no significant differences between the non-painful/venipuncture and non-painful/non-venipuncture sessions (p > 0.05). The “time X age X session” interaction term (F[14,1] = 9.4, p < 0.05) was statistically significant indicating that older adults had greater IL-8 saliva responses after the CPT at the 45- and 60-minute time points (p < 0.05, Figure 2B).
IL-10
The doubly repeated-measures ANOVA revealed a significant effect of “session” (F[2,13] = 12.8, p < 0.001) with post hoc comparisons indicating that saliva IL-10 concentrations were significantly higher in the CPT (i.e., painful) compared to the warm control (i.e., non-painful) sessions (Bonferroni adjusted p < 0.001). However, there were no significant differences between the non-painful/venipuncture and non-painful/non-venipuncture sessions (p > 0.05). The “time X age X session” interaction term (F[14,1] = 7.8, p < 0.05) was statistically significant indicating that older adults had greater IL-10 saliva responses at the 60-minute time point (p < 0.05, Figure 2C).
IL-4
The doubly repeated-measures ANOVA revealed a significant effect of “session” (F[2,13] = 14.9, p < 0.001) with post hoc comparisons indicating that saliva IL-4 concentrations were significantly higher in the CPT (i.e., painful) compared to the warm control (i.e., non-painful) sessions (Bonferroni adjusted p < 0.001). However, there were no significant differences between the non-painful/venipuncture and non-painful/non-venipuncture sessions (p > 0.05). The “time X age X session” interaction term (F[14,1] = 7.9, p < 0.05) was statistically significant indicating that older adults had greater IL-4 saliva responses after the CPT at the 60-minute time point (p < 0.05, Figure 2D).
Discussion
The aim of the current study was to characterize the time course, duration and magnitude of changes of pro-inflammatory and anti-inflammatory cytokines in “saliva” samples following experimental pain stimulation. In addition, we tested for age-related differences as well as the effects of venipuncture in these salivary immune markers. To our knowledge, this is the first experimental study using saliva that has been designed to investigate these associations in several pro- and anti-inflammatory cytokines simultaneously over a period of 120 minutes in response to a commonly used experimental pain manipulation (i.e., cold pressor pain).
A major study finding was the reliable detection of all four cytokines in saliva after laboratory-induced pain using a simple, inexpensive, reliable collection system. We have previously reported the induction of these same cytokines after experimental pain in blood samples.4 However, only a few studies have previously reported salivary cortisol and soluble tumor necrosis factor-α receptor II (sTNFαRII) responses provoked by various experimental pain modalities.3,16 Our study findings add salivary measures of IL-6, IL-8, IL-10 and IL-4 to the biomarker repertoire available for mechanistic pain research. Furthermore, our findings that older adults have an increased concentration of salivary cytokines after experimental pain are consistent with our previous findings using blood samples with similar effect sizes. Previous research studies have reported low to moderate associations between salivary and plasma cytokine concentrations,17 likely due to the cytokine’s restrictive pathway of entry into the salivary glands. However, exposure to stress may change this dynamic process, given that salivary production is regulated by the autonomic nervous system. The finding that salivary cytokines provide equally useful information in older individuals allows researchers to move translational research to the community as the more vulnerable, frail older adults do not usually come to our research settings.
In addition, we postulated that venipuncture would be a stressful event that would increase circulating cytokines with our older participants experiencing greater induction of salivary cytokines. However, we found that venipuncture did not significantly increase the salivary cytokines in our participants including the older ones. Our original hypothesis was based on the observation that the venipuncture procedure required insertion of an indwelling catheter that remained in the participant around 2 hours. However, our findings suggest that venipuncture alone was not sufficient to contaminate the salivary biomarkers of interest. It is possible that the setting was partially responsible for this result. Experiments were conducted in quiet rooms where friendly, highly skilled and experienced CTSI nurses performed the venipuncture procedures. Nonetheless, a 15-minute wait between catheter insertion and baseline sample collection was adequate to avoid any potential carryover effects.
Finally, the finding that peak saliva concentrations were almost always at similar time points as the peak plasma concentrations across all participants following cold pain suggests that salivary cytokine concentrations likely mirror cellular processes from their plasma counterpart, at least in healthy individuals. This finding is consistent with a study reporting stable salivary gland flow rates over 2 hours in healthy adults with no differences between young versus older individuals.18 However, this needs further study since chronic health conditions associated with aging may negatively impact salivary gland function.19
Despite a small sample size, our study had a strong methodological design, which likely accounted for decreasing the significant variability usually found in biomarker studies. Our results provide the first evidence that acute experimental pain in humans indeed can activate an immune response that can be measured in saliva. However, our findings were under very controlled experimental conditions, including the selection of healthy subjects, limiting the study generalizability. In addition, biomarker samples including saliva collection require stringent storage requirements (i.e., refrigeration) which may not be easily available in all settings. In the future, larger studies in the community are urgently needed to validate and finally move translational mechanistic research to those populations most underrepresented in clinical research including geriatric and pediatric individuals.
Acknowledgments
This research was supported by NIH–NIA Grant R01AG039659 (JLR). This publication was also made possible by the UF Clinical and Translational Science Institute (UL1TR000064) and NIH–NIA Grant K01AG048259 (YCA). Its contents are solely the responsibility of the authors and do not necessarily represent the official views of the NIH.
Disclosure
The authors report no conflicts of interest in this work.
References
Institute of Medicine, IOM. Relieving Pain in America: A Blueprint for Transforming Prevention, Care, Education, and Research. Washington, DC: National Academies Press; 2011. | ||
Edwards RR. Catastrophizing and interleukin-6 reactivity to pain. J Pain. 2008;9:55. | ||
Goodin BR, Quinn NB, King CD, et al. Salivary cortisol and soluble tumor necrosis factor-alpha receptor II responses to multiple experimental modalities of acute pain. Psychophysiology. 2012;49(1):118–127. | ||
Cruz-Almeida Y, Aguirre M, Sorenson HL, Tighe P, Wallet SM, Riley JL 3rd. Age differences in cytokine expression under conditions of health using experimental pain models. Exp Gerontol. 2015;72:150–156. | ||
Cruz-Almeida Y, King CD, Wallet SM, Riley JL 3rd. Immune biomarker response depends on choice of experimental pain stimulus in healthy adults: a preliminary study. Pain Res Treat. 2012;2012:538739. | ||
Bäckryd E, Tanum L, Lind AL, Larsson A, Gordh T. Evidence of both systemic inflammation and neuroinflammation in fibromyalgia patients, as assessed by a multiplex protein panel applied to the cerebrospinal fluid and to plasma. J Pain Res. 2017;10:515–525. | ||
Kosek E, Altawil R, Kadetoff D, et al. Evidence of different mediators of central inflammation in dysfunctional and inflammatory pain – interleukin-8 in fibromyalgia and interleukin-1 β in rheumatoid arthritis. J Neuroimmunol. 2015;280:49–55. | ||
Kadetoff D, Lampa J, Westman M, Andersson M, Kosek E. Evidence of central inflammation in fibromyalgia-increased cerebrospinal fluid interleukin-8 levels. J Neuroimmunol. 2012;242(1–2):33–38. | ||
Chiang JJ, Eisenberger NI, Seeman TE, Taylor SE. Negative and competitive social interactions are related to heightened proinflammatory cytokine activity. Proc Natl Acad Sci U S A. 2012;109(6):1878–1882. | ||
Izawa S, Sugaya N, Kimura K, et al. An increase in salivary interleukin-6 level following acute psychosocial stress and its biological correlates in healthy young adults. Biol Psychol. 2013;94(2):249–254. | ||
Slavich GM, Way BM, Eisenberger NI, Taylor SE. Neural sensitivity to social rejection is associated with inflammatory responses to social stress. Proc Natl Acad Sci U S A. 2010;107(33):14817–14822. | ||
Franceschi C, Bonafè M, Valensin S, et al. Inflamm-aging. An evolutionary perspective on immunosenescence. Ann N Y Acad Sci. 2000;908:244–254. | ||
Pizza V, Agresta A, D’Acunto CW, Festa M, Capasso A. Neuroinflammation and ageing: current theories and an overview of the data. Rev Recent Clin Trials. 2011;6(3):189–203. | ||
Riley JL 3rd, King CD, Wong F, Fillingim RB, Mauderli AP. Lack of endogenous modulation and reduced decay of prolonged heat pain in older adults. Pain. 2010;150(1):153–160. | ||
Poll EM, Kreitschmann-Andermahr I, Langejuergen Y, et al. Saliva collection method affects predictability of serum cortisol. Clin Chim Acta. 2007;382(1–2):15–19. | ||
Goodin BR, Quinn NB, Kronfli T, et al. Experimental pain ratings and reactivity of cortisol and soluble tumor necrosis factor-alpha receptor II following a trial of hypnosis: results of a randomized controlled pilot study. Pain Med. 2012;13(1):29–44. | ||
Soto-Méndez MJ, Romero-Abal ME, Aguilera CM, et al. Associations among inflammatory biomarkers in the circulating, plasmatic, salivary and intraluminal anatomical compartments in apparently healthy preschool children from the western highlands of Guatemala. PLoS One. 2015;10(6):e0129158. | ||
Fischer D, Ship JA. Effect of age on variability of parotid salivary gland flow rates over time. Age Ageing. 1999;28(6):557–561. | ||
Yeh CK, Johnson DA, Dodds MW. Impact of aging on human salivary gland function: a community-based study. Aging (Milano). 1998;10(5):421–428. |
 © 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

