Back to Journals » International Medical Case Reports Journal » Volume 8
Acute orbital apex syndrome and rhino-orbito-cerebral mucormycosis
Authors Anders U , Taylor E, Martel J, Martel J
Received 17 February 2015
Accepted for publication 2 March 2015
Published 17 April 2015 Volume 2015:8 Pages 93—96
DOI https://doi.org/10.2147/IMCRJ.S83036
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Ursula M Anders,1 Elise J Taylor,1 Joseph R Martel,1–3 James B Martel1–3
1Research Center, Martel Eye Medical Group, Rancho Cordova, 2Graduate Medical Education, California Northstate University College of Medicine, Elk Grove, 3Department of Ophthalmology, Dignity Health, Carmichael, CA, USA
Purpose: To demonstrate the successful clinical identification and management of rhino-orbital mucormycosis, a fungal infection with a high mortality rate.
Patients and methods: A diabetic male patient with a headache and orbital apex syndrome in the right eye was examined using computed tomography (CT) and magnetic resonance imaging (MRI) for a possible fungal infection. Endoscopic surgical resection was performed and a pathology sample was taken. Specimens were prepared with Gömöri methenamine silver and hematoxylin and eosin staining. The patient was treated with liposomal amphotericin B 400 mg daily, followed by posaconazole 400 mg twice daily.
Results: CT and MRI revealed a mass of the right sphenoid spreading into the orbit, indicative of a fungal infection. The biopsy confirmed the diagnosis of mucormycosis. Complete recovery of eyelid and oculomotor function was achieved after 10 months of treatment, although the patient continues to suffer from irreversible blindness in the right eye due to optic nerve atrophy. He has been without signs or symptoms of recurrence.
Conclusion: Patients with rhino-orbito-cerebral mucormycosis need extensive surgical and medical treatment to maximize outcomes. Success requires multidisciplinary management.
Keywords: ophthalmoplegia, sixth nerve palsy, diabetes mellitus, nephrotoxicity, amphotericin B, posaconazole
Introduction
Orbital apex syndrome (OAS) is an uncommon clinical presentation consisting of complete ophthalmoplegia with vision loss, involving cranial nerves II, III, IV, V1, and VI.1 OAS may result from trauma, malignancy, infection, inflammation, or vascular origins. Some of these conditions, particularly among the infectious causes, can be life-threatening with delayed diagnosis and treatment. Rhino-orbito-cerebral mucormycosis (ROCM) is an invasive and often fatal fungal infection. The incidence of mucormycosis is increasing,2,3 with a current estimate of 1.7/1,000,000 cases in the US annually.4 In the emergent setting, any patient with OAS who is either immune compromised or diabetic should be evaluated for the presence of mucormycosis. We present a case of a successfully treated diabetic patient with OAS resulting from rhino-orbital mucormycosis who presented to the emergency department for treatment of headache symptoms.
Case report
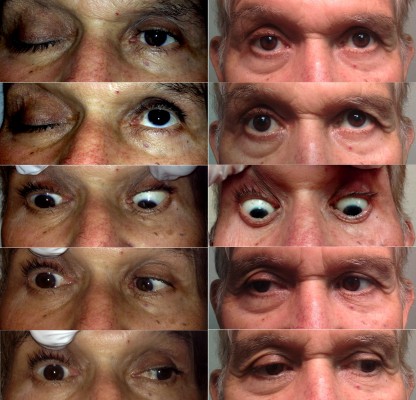
A 68-year-old Hispanic male presented to the Emergency Department for severe headache, dizziness, and nausea. He had a past history of prostate cancer with 48 days of ongoing radiotherapy, and an acoustic neuroma that was treated with gamma knife surgery 3 years prior to this presentation. Current medical history revealed poorly diet-controlled type 2 diabetes. He was noted to have significantly decreased ocular motility and loss of vision in his right eye. Ophthalmologic examination revealed no light perception and ophthalmoplegia in the right eye (Figure 1) with impairment of cranial nerves II, III, IV, V1, and VI, culminating in a diagnosis of OAS. Funduscopic examination showed no significant abnormalities.
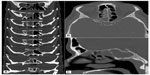
A computed tomography (CT) scan of the brain showed bilateral opacification of the ethmoids, near complete opacification of the right sphenoid, and mild mucosal thickening in the left sphenoid and maxillary sinuses (Figure 2). Hyperintense T2 signals of the right sphenoid sinus shown on MRI suggested the presence of fungal involvement. ENT evaluated the patient and concurred with the possible diagnosis of mucormycosis.
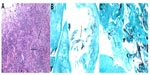
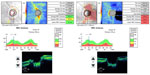
Endoscopic surgical resection was performed by ENT, and a pathology sample was taken. Histopathology of tissue stains showed positivity for mucormycosis (Figure 3). The patient subsequently underwent aggressive endoscopic removal of the involved tissue. The patient was treated with liposomal amphotericin B 400 mg, IV, postsurgery. After 3 weeks, he experienced some minor nephrotoxicity as a side effect of the liposomal amphotericin B, and was switched to posaconazole 400 mg twice daily for 2 months. After 10 months, there was complete resolution of ophthalmoplegia, although there was evidence of presynaptic atrophy of the right optic nerve (Figure 4).
Written informed consent was obtained from the patient to allow the publication of photographs for educational purposes. This study adhered to the tenets of the Declaration of Helsinki and was Health Insurance Portability and Accountability Act (HIPAA) compliant. Dignity Health Institutional Review Committee ruled that approval was not required for this study.
Discussion
OAS is a common presentation of ROCM, but unfortunately blindness is permanent and the risk of mortality is increased at this stage of progression. Mucormycosis is the third most frequent fungal disease after candidiasis and aspergillosis,3 and is more likely to cause OAS.5 Prime susceptibility factors for ROCM include diabetes mellitus, ketoacidosis, immunosuppression, and elevated levels of serum iron.5,6 Elevated blood glucose levels and change in acidity levels nourish fungal colonies, and increased availability of unbound serum iron in acidotic conditions aids in the growth of fungus and development of vascular invasion.7 Angioinvasion with thrombus and further tissue necrosis is the most likely mechanism of the sinus disease spreading into the orbit and brain.
Mucormycosis can be difficult to identify if indicators such as thrombosis and necrotic tissue are absent or are late in presentation. Thurtell et al5 reported 14 patients with biopsy proven ROCM and OAS, with only one patient being correctly diagnosed at presentation. In diabetics, OAS secondary to ROCM may initially present as a sixth nerve palsy or partial ophthalmoplegia and is felt to represent microvascular disease, particularly when there is minimal disease sinus findings by CT.8 When any sinus disease with OAS is observed in a diabetic or immunocompromised patient by CT or MRI, a fungal etiology should be suspected. MRI is an effective technique in diagnosing OAS, with biopsy being the most reliable.
Mucormycosis is a highly aggressive infection known to have a high mortality rate when not treated. Survival rates depend on the interval period from appearance of symptoms to onset of treatment or surgery, extent and location of the infection, type of treatment, and amount of immunosuppression. Roden et al2 published a review of infectious patterns and outcomes of 929 patients with zygomycosis between 1885 and 2005. The most common sites of infection were sinus (39%), pulmonary (24%), and cutaneous (19%). Of the sinus infections, 21% of patients had rhinocerebral involvement, 8% had sino-orbital involvement, and 8% had sinusitis. Of these, the mortality rates were 62%, 24%, and 16%, respectively. Orbital involvement is unilateral,9 and the survival rate decreases dramatically with bilateral sinus involvement.6
Amphotericin B has been the antifungal of choice since the first successful treatment of this disease by Gass in 1961.6,10 Liposomal amphotericin B has similar or better survival rates than amphotericin B with less nephrotoxicity.4,6,9 However, in this case the patient still developed mild nephrotoxicity and was switched to posaconazole. Posaconazole is useful as a secondary treatment when kidney function is affected, and is more effective against Mucorales in vitro than other triazoles.4,9 Optimal therapy requires a multidisciplinary approach between internists and ENT, ophthalmology, and infectious disease specialists.
Disclosure
The authors report no conflicts of interest in this work.
References
Anders UM, Taylor EJ, Martel JR, Martel JB. Pseudo-orbital apex syndrome in the acute trauma setting due to ipsilateral dissection of internal carotid artery. Ophthal Plast Reconstr Surg. Epub September 11, 2014. | |
Roden MM, Zaoutis TE, Buchanan WL, et al. Epidemiology and outcome of zygomycosis: a review of 929 reported cases. Clin Infect Dis. 2005; 41(5):634–653. | |
Di Carlo P, Pirrello R, Guadagnino G, et al. Multimodal surgical and medical treatment for extensive rhinocerebral mucormycosis in an elderly diabetic patient: a case report and literature review. Case Rep Med. 2014;2014:527062. | |
Gamaletsou MN, Sipsas NV, Roilides E, Walsh TJ. Rhino-orbital-cerebral mucormycosis. Curr Infect Dis Rep. 2012;14(4):423–434. | |
Thurtell MJ, Chiu AL, Goold LA, et al. Neuro-ophthalmology of invasive fungal sinusitis: 14 consecutive patients and a review of the literature. Clin Exp Ophthalmol. 2013;41(6):567–576. | |
Yohai RA, Bullock JD, Aziz AA, Markert RJ. Survival factors in rhino-orbital-cerebral mucormycosis. Surv Ophthalmol. 1994;39(1):3–22. | |
Sravani T, Uppin SG, Uppin MS, Sundaram C. Rhinocerebral mucormycosis: pathology revisited with emphasis on perineural spread. Neurol India. 2014;62(4):383–386. | |
Balch K, Philips HP, Newman NJ. Painless orbital apex syndrome from mucormycosis. J Neuroophthalmol. 1997;17(3):178–182. | |
Toumi A, Larbi Ammari F, Loussaief C, et al. Rhino-orbito-cerebral mucormycosis: five cases. Med Mal Infect. 2012;42(12):591–598. | |
Sponsler TA, Sassani JW, Johnson LN, Towfighi J. Ocular invasion in mucormycosis. Surv Ophthalmol. 1992;36(5):345–350. |
 © 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.