Back to Journals » OncoTargets and Therapy » Volume 13
A Novel ROS1-FBXL17 Fusion Co-Existing with CD74-ROS1 Fusion May Improve Sensitivity to Crizotinib and Prolong Progression-Free Survival of Patients with Lung Adenocarcinoma
Authors Lan S, Li H, Liu Y, Xu J, Huang Z, Yan S, Zhang Q, Cheng Y
Received 26 August 2020
Accepted for publication 21 October 2020
Published 10 November 2020 Volume 2020:13 Pages 11499—11504
DOI https://doi.org/10.2147/OTT.S278907
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Arseniy Yuzhalin
Shaowei Lan,1,2,* Hui Li,1,2,* Ying Liu,3 Jinhua Xu,3 Zhicheng Huang,4 Shi Yan,1,2 Qiang Zhang,5 Ying Cheng1– 3
1Translational Oncology Research Lab, Jilin Provincial Cancer Hospital, Changchun 130012, People’s Republic of China; 2Jilin Provincial Key Laboratory of Molecular Diagnostics for Lung Cancer, Jilin Provincial Cancer Hospital, Changchun 130012, People’s Republic of China; 3Department of Medical Thoracic Oncology, Jilin Provincial Cancer Hospital, Changchun 130012, People’s Republic of China; 4Department of Radiology, Jilin Provincial Cancer Hospital, Changchun 130012, People’s Republic of China; 5Burning Rock Biotech, Guangzhou 510000, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Ying Cheng
Jilin Provincial Cancer Hospital, 1066 Jinhu Road, Changchun, Jilin, People’s Republic of China
Tel +86-431-80596051
Email [email protected]
Purpose: The rearrangement of ROS1 (C-ros oncogene 1) is an important driver of non-small cell lung cancer (NSCLC). Currently, only approximately 24 ROS1 fusion partners have been shown to be sensitive to crizotinib. Although fusion partner determination is not required to treat patients with tyrosine kinase inhibitor, the correlation between ROS1 phenotypes and efficacies still needs more researches. Furthermore, non-reciprocal/reciprocal ROS1 translocations are rare and have not yet been reported. Thus, more novel ROS1 fusion partners and non-reciprocal/reciprocal fusions need to be provided and supplemented to guide targeted therapy and prognosis for patients.
Case Presentation: Targeted next-generation sequencing panel was used to identify ROS1 rearrangements in a Chinese patient with advanced lung adenocarcinoma. We identified a non-reciprocal/reciprocal ROS1 translocation which contained a novel ROS1-FBXL17 (F-box and leucine-rich repeat protein 17) fusion co-existing with the CD74-ROS1 fusion and the patient was sensitive to crizotinib. The ROS1 rearrangement was then validated using RT-qPCR. The progression-free survival (PFS) was 15.7 months which exceeded the highest PFS level (14.2 months) in the Chinese population reported recently. Thus, this non-reciprocal/reciprocal ROS1 translocation patient had an excellent efficacy to crizotinib which was different from that in ALK. And it may be possible that the ROS1-FBXL17 fusion in this patient synergistically promotes the sensitivity of the CD74-RSO1 fusion to crizotinib.
Conclusion: The ROS1-FBXL17 fusion may be a novel driver of NSCLC and we provide a non-reciprocal/reciprocal ROS1 translocation mode very sensitive to crizotinib. Our study adds new data to the ROS1 fusion database and provides a reference strategy for the clinical treatment of patients with double ROS1 fusions or non-reciprocal/reciprocal ROS1 translocation.
Keywords: ROS1-FBXL17 fusion, CD74-ROS1 fusion, non-reciprocal/reciprocal ROS1 translocation, next-generation sequencing, intratumor heterogeneity, non-small cell lung cancer
Background
ROS1 (C-ros oncogene 1) rearrangement is a proven driver of non-small cell lung cancer (NSCLC) and occurs in approximately 1‒3% of the patients with NSCLC worldwide.1–4 Crizotinib, an oral tyrosine kinase inhibitor (TKI) that targets the ROS1, ALK, and Met receptor tyrosine kinases, is sensitive to the rearrangement of ROS1.5–8 Many genes can fuse with ROS1, and currently, at least 24 partner genes of ROS1 have been identified in patients with NSCLC.9–13 The application of next-generation sequencing (NGS) is reliable and helpful in the discovery of novel variants, including ROS1 partners.13–15 It is widely known that the EML4-ALK variants (V1-V7) or EGFR mutations (L858R/T790M/C797S/19 del.) have different TKIs efficacies between subtypes.16–19 Furthermore, it had recently been confirmed that crizotinib-treated patients with non-reciprocal/reciprocal ALK translocation had a poor efficacy compared with patients carrying 3ʹ-ALK fusion alone or with EML4-ALK fusion alone.20 Therefore, it may also have different drug sensitivities and resistances between ROS1 fusion subtypes. More important, the crizotinib efficacy in patients with non-reciprocal/reciprocal ROS1 translocation has not been reported. Here, we identified a novel ROS1-FBXL17 (F-box and leucine-rich repeat protein 17) fusion that co-existed with the CD74-ROS1 fusion in one patient who was sensitive to crizotinib and was with a stable disease (SD) for more than 15 months, thus identifying a rare sensitive double fusion mode (a non-reciprocal/reciprocal translocation) for ROS1.
Case Report
In June 2018, a 51-year-old Chinese female showing symptoms such as productive cough (whitish sputum), chest pain, and dyspnea, was diagnosed with adenocarcinoma in the superior lobe of the right lung through systematic examination. The clinical stage of the cancer was determined as T3N2M0 (stage IIIb). Surgical resection of the superior lobe of the right lung was performed in Shanghai. However, a reexamination in our hospital for the patient in the 28th day after surgery found that the patient had pleural invasion, bilateral mediastinal and hilar lymph node metastasis, right supraclavicular lymph node metastasis, and right cervical lymph node metastasis (pT4N3M1c IVb). NGS was performed for an DNA sequence based 8 gene panel, including EGFR, ALK, ROS1, MET, RET, BRAF, ERBB2, and KRAS, using postoperative tissue samples, and no genetic alterations were found in any genes. The patient was administered one course of pemetrexed, combined with cisplatin chemotherapy, and achieved the SD state, according to the Response Evaluation Criteria in Solid Tumors version 1.1 (RECIST v1.1); however, the patient could not tolerate the side effects.
To determine whether the patient was suitable for treatment with immune checkpoint inhibitors, the immunotherapy biomarker programmed death ligand 1 (PD-L1, immunohistochemistry) and the tumor mutational burden (TMB, NGS) were detected using surgical specimens that were sliced consecutively. TMB was detected through a DNA sequence based 520 gene panel (520 genes closely associated to solid tumors) using the Illumina Novaseq 6000 Sequencing Platform and a Dx Oncoscreen plus TM kit (Burning Rock, China). This panel includes the driver genes involved in 8 gene panel. The results showed 5‒10% PD-L1 positive cells and a TMB value of 5.6 mutations per megabase. Interestingly, NGS identified a ROS1-FBXL17 fusion (R33: Fintergenic; mutation frequency: because FBXL17 was not included in the panel, the accurate mutation frequency of the ROS1-FBXL17 fusion could not be obtained.) coexisting with the CD74-ROS1 fusion (C6: R33; mutation frequency: 27.70%), and TP53, APC, MGA, and ZNF217 mutations. The novel ROS1-FBXL17 rearrangement (2476 amino acids) was generated through the fusion of ROS1 exons 1–32 on chr6: q22.1 (5ʹ-3ʹ, 1–1776 amino acids) to FBXL17 exons 1–9 on chr5: q21.2 (5ʹ-3ʹ, 1–700 amino acid) (Figure 1A and C), while the CD74-ROS1 rearrangement (778 amino acids) was generated through the fusion of CD74 exons 1‒6 on chr5: q33.1 (5ʹ-3ʹ, 1–207 amino acids) to ROS1 exons 33‒43 on chr6: q22.1 (5ʹ-3ʹ, 1786–2356 amino acids) (Figure 1B and C). In addition, RNA isolation and reverse transcription were performed in postoperative tissue samples, and real-time PCR (amplification refractory mutation system, ARMS) result confirmed the presence of the CD74-ROS1 fusion for clinical requirement (Figure 1D). However, due to the shortage of tumor tissue, RNA sequencing could not be performed.
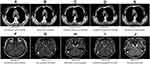
Before undergoing molecular targeting treatments, the patient underwent a computed tomography (CT) examination, which showed that the mediastinal lymph nodes were 1.35 cm (Figure 2A). The patient was then orally treated with crizotinib for more than 17 months (data cut-off: March 2, 2020). The mediastinal lymph nodes continued to shrink (from 0.65 cm to unmeasurable) without any other observable metastasis (Figure 2B–D). The efficacy evaluation in the lung indicated SD. However, magnetic resonance imaging (MRI) on January 10, 2020 showed a new lesion in the cerebellum (0.69 cm) compared with before (Figure 2F–H), and the patient received continued oral treatment with crizotinib. At the time of the assessment on March 3, 2020, the lesion was still growing in size (1.0 cm), confirming disease progression (Figure 2I). The patient presented with mild myelosuppression and there was no head discomfort or movement disorder. The progression-free survival (PFS) was 15.7 months. Then the patient received radiotherapy (30Gy/10 times/12 days) on head and the cerebellar lesion began to shrink. Thus far, the disease remains stable and the patient is still under crizotinib treatment. On October 13, 2020 the MRI showed a 0.64 cm lesion in the cerebellum (Figure 2J) and CT showed the mediastinal lymph nodes remained stable (Figure 2E).
Discussion
To our knowledge, double genes fused with ROS1 are rare and FBXL17 is a novel partner for ROS1, making the right regimen for this mutation unclear. Although fusion variant determination was not required for patients treated with TKIs, the efficacies were different between fusion modes.20 As compared with the CD74-ROS1 fusion, the non-CD74-ROS1 fusion might have a significantly longer PFS.21 Therefore, identification of the mutant subtypes or non-reciprocal/reciprocal translocations are beneficial for both treatment and prognosis.
There is little information regarding the efficacy of crizotinib for patients harboring double genes fused with ROS1. A Chinese study in 2018 identified a patient who harbored a CD74-ROS1 fusion that coexisted with the SDC4-ROS1 fusion, and another patient who harbored a SDC4-ROS1 fusion that coexisted with the EZR-ROS1 fusion.21 Crizotinib showed different efficacies in the two patients, which indicated that crizotinib may have different efficacies in double fusions of ROS1. The translocations in the two patients were both 3ʹ-ROS1. But nothing was known about the efficacy of non-reciprocal/reciprocal ROS1 translocation patients treated with crizotinib. Presence of non-reciprocal/reciprocal ALK translocation was predictive for worse survival and greater likelihood of baseline brain metastases in first-line crizotinib treated NSCLC patients.20 In this case, we confirmed a patient with non-reciprocal/reciprocal ROS1 translocation (ROS1-FBXL17 fusion that coexisted with the CD74-ROS1 fusion) had an excellent response to crizotinib. The PFS reached 15.7 months and exceeded the highest level (14.2 months) of the ROS1 fusion reported in a recent study in Chinese population.22 It is also higher than the median level (12.6 months) in Chinese patients with 3ʹ-ROS1 fusion or with CD74-ROS1 fusion alone.21 These suggested that the crizotinib efficacy in patients with non-reciprocal/reciprocal translocation in ROS1 might be superior to that in ALK. The speculated reason may be that the biological effect of ROS1 translocation is different from that of ALK, and the mechanism in ROS1 may be more complex, or there may be some unknown mechanisms of concomitant mutation with ROS1 that has not yet been discovered and revealed. However, further observations and more cases are needed to confirm these points. In addition, brain metastasis occurred after crizotinib treated over 15 months in this case. In the future, more studies are needed to explore whether patients with 5ʹ-ROS1 are also greater likelihood of baseline brain metastases, such as 5ʹ-ALK.
It was not clear whether the ROS1-FBXL17 fusion was functional and sensitive to crizotinib. Xu et al12 have reported a ROS1-ADGRG6 rearrangement alone that is generated by the fusion of the exons 1–33 of ROS1 on chr6: q22.1 to exons 2–26 of ADGRG6 on chr6: q24.2 and is clearly sensitive to crizotinib. The main structural framework and the junction point on the ROS1 of the ROS1-FBXL17 fusion were similar to those of the ROS1-ADGRG6 fusion; thus, we speculated that the ROS1-FBXL17 fusion may have biological functions similar to those of ROS1-ADGRG6. Therefore, ROS1-FBXL17 may be a novel driver mutation, or confer a positive and synergistic effect on the sensitivity of the CD74-ROS1 fusion to crizotinib.
Furthermore, in this case, serial sectioning of a single postoperative tissue specimen was performed for targeted detection, using an 8 genes panel and a 520 genes panel successively. Interestingly, different results were obtained from the two experimental runs, each of which used different sections from the same paraffin block. The possible reasons for the difference included heterogeneity between slices,23–25 formalin-fixed paraffin-embedded samples,26 or differences in panels, or others. Thus, multi-point sampling and multiple detections may be important steps for determining the ROS1 fusions, and for molecular subtyping, which can dictate the clinical treatment strategies for patients. Moreover, cytological samples or liquid biopsy is also a feasible strategy for patients with tissue sampling difficulties.
Conclusion
In summary, we identified a novel ROS1-FBXL17 fusion that coexisted with the CD74-ROS1 fusion in an advanced NSCLC patient sensitive to crizotinib. We provided a non-reciprocal/reciprocal ROS1 translocation pattern very sensitive to crizotinib. The ROS1-FBXL17 fusion may be functional and may promote the sensitivity of the CD74 fusion to crizotinib but this needs further validation. Although fusion partners determination is not required for patients treated with crizotinib, due to the presence of intratumor heterogeneity and non-reciprocal/reciprocal translocations, molecular subtyping of ROS1 fusions should be accurately and timely identified.
Ethics Statement
The study was approved by the Ethics Committee of Jilin Provincial Cancer Hospital. The patient provided written informed consent for the publication of any associated data.
Consent for Publication
All authors agreed to the publication of these data.
Acknowledgments
The authors would like to thank the patient for her positive attitude during clinical treatment. We also thank the doctors from the auxiliary departments who were involved in the accurate diagnosis of the patient’s condition.
Funding
This research was supported in part by the Department of Science and Technology of Jilin Province (20190303157SF, 202002062JC and 202002063JC) and Scientific Research Funds of Jilin Province of Health and Family Planning Commission (2018J021 and 2018J023).
Disclosure
Qiang Zhang is an employee of Burning Rock Biotech. The authors report no other conflicts of interest in this work.
References
1. Bergethon K, Shaw AT, Ou SH, et al. ROS1 rearrangements define a unique molecular class of lung cancers. J Clin Oncol. 2012;30(8):863–870. doi:10.1200/JCO.2011.35.6345
2. Cai W, Li X, Su C, et al. ROS1 fusions in Chinese patients with non-small-cell lung cancer. Ann Oncol. 2013;24(7):1822–1827. doi:10.1093/annonc/mdt071
3. Zhang Q, Wu C, Ding W, et al. Prevalence of ROS1 fusion in Chinese patients with non-small cell lung cancer. Thorac Cancer. 2019;10(1):47–53. doi:10.1111/1759-7714.12899
4. Shaw AT, Solomon BJ, Chiari R, et al. Lorlatinib in advanced ROS1-positive non-small-cell lung cancer: a multicentre, open-label, single-arm, Phase 1–2 trial. Lancet Oncol. 2019;20(12):1691–1701. doi:10.1016/S1470-2045(19)30655-2
5. Wiesweg M, Schuler M, Schildhaus HU. Crizotinib in ROS1 and MET deregulated NSCLC-letter. Clin Cancer Res. 2020;26(7):1774. doi:10.1158/1078-0432.CCR-19-3740
6. Lee A, Howell VM, Itchins M, Wheeler HR, Pavlakis N. ROS1-rearranged non-small-cell lung cancer, factor v leiden, and recurrent venous thromboses. Clin Lung Cancer. 2018;19(5):457–459. doi:10.1016/j.cllc.2018.05.015
7. Davies KD, Le AT, Theodoro MF, et al. Identifying and targeting ROS1 gene fusions in non-small cell lung cancer. Clin Cancer Res. 2012;18(17):4570–4579. doi:10.1158/1078-0432.CCR-12-0550
8. Ou SH. Crizotinib: a novel and first-in-class multitargeted tyrosine kinase inhibitor for the treatment of anaplastic lymphoma kinase rearranged non-small cell lung cancer and beyond. Drug Des Devel Ther. 2011;5:471–485. doi:10.2147/DDDT.S19045
9. Zhu YC, Zhou YF, Wang WX, et al. CEP72-ROS1: a novel ROS1 oncogenic fusion variant in lung adenocarcinoma identified by next-generation sequencing. Thorac Cancer. 2018;9(5):652–655. doi:10.1111/1759-7714.12617
10. Hicks JK, Boyle T, Albacker LA, Madison R, Frampton G, Creelan BC. Clinical activity of crizotinib in lung adenocarcinoma harboring a rare ZCCHC8-ROS1 fusion. J Thorac Oncol. 2018;13(8):e148–e150. doi:10.1016/j.jtho.2018.03.028
11. He Y, Sheng W, Hu W, et al. Different types of ROS1 fusion partners yield comparable efficacy to crizotinib. Oncol Res. 2019;27(8):901–910. doi:10.3727/096504019X15509372008132
12. Xu S, Wang W, Xu C, et al. ROS1-ADGRG6: a case report of a novel ROS1 oncogenic fusion variant in lung adenocarcinoma and the response to crizotinib. BMC Cancer. 2019;19(1):769. doi:10.1186/s12885-019-5948-y
13. Liu Y, Liu T, Li N, Wang T, Pu Y, Lin R. Identification of a novel WNK1-ROS1 fusion in a lung adenocarcinoma sensitive to crizotinib. Lung Cancer. 2019;129:92–94. doi:10.1016/j.lungcan.2018.12.011
14. Tsoulos N, Papadopoulou E, Metaxa-Mariatou V, et al. Tumor molecular profiling of NSCLC patients using next generation sequencing. Oncol Rep. 2017;38(6):3419–3429.
15. Shulskaya MV, Alieva AK, Vlasov IN, et al. Whole-exome sequencing in searching for new variants associated with the development of parkinson’s disease. Front Aging Neurosci. 2018;10:136. doi:10.3389/fnagi.2018.00136
16. Lin JJ, Zhu VW, Yoda S, et al. Impact of EML4-ALK variant on resistance mechanisms and clinical outcomes in ALK-positive lung cancer. J Clin Oncol. 2018;36(12):1199–1206. doi:10.1200/JCO.2017.76.2294
17. Woo CG, Seo S, Kim SW, et al. Differential protein stability and clinical responses of EML4-ALK fusion variants to various ALK inhibitors in advanced ALK-rearranged non-small cell lung cancer. Ann Oncol. 2017;28(4):791–797. doi:10.1093/annonc/mdw693
18. Li Y, Zhang T, Zhang J, et al. Response to crizotinib in advanced ALK-rearranged non-small cell lung cancers with different ALK-fusion variants. Lung Cancer. 2018;118:128–133. doi:10.1016/j.lungcan.2018.01.026
19. Castellanos E, Feld E, Horn L. Driven by mutations: the predictive value of mutation subtype in EGFR-mutated non-small cell lung cancer. J Thorac Oncol. 2017;12(4):612–623. doi:10.1016/j.jtho.2016.12.014
20. Zhang Y, Zeng L, Zhou C, et al. Detection of nonreciprocal/reciprocal ALK translocation as poor predictive marker in patients with first-line crizotinib-treated ALK-rearranged NSCLC. J Thorac Oncol. 2020;15(6):1027–1036. doi:10.1016/j.jtho.2020.02.007
21. Li Z, Shen L, Ding D, et al. Efficacy of crizotinib among different types of ROS1 fusion partners in patients with ros1-rearranged non-small cell lung cancer. J Thorac Oncol. 2018;13(7):987–995. doi:10.1016/j.jtho.2018.04.016
22. Liu C, Yu H, Chang J, et al. Crizotinib in Chinese patients with ROS1-rearranged advanced nonsmall-cell lung cancer in routine clinical practice. Target Oncol. 2019;14(3):315–323. doi:10.1007/s11523-019-00636-6
23. Lai GGY, Lim TH, Lim J, et al. Clonal MET amplification as a determinant of tyrosine kinase inhibitor resistance in epidermal growth factor receptor-mutant non-small-cell lung cancer. J Clin Oncol. 2019;37(11):876–884.
24. McLaughlin J, Han G, Schalper KA, et al. Quantitative assessment of the heterogeneity of PD-L1 expression in non-small-cell lung cancer. JAMA Oncol. 2016;2(1):46–54. doi:10.1001/jamaoncol.2015.3638
25. Vukovic V, Nicklee T, Hedley DW. Microregional heterogeneity of non-protein thiols in cervical carcinomas assessed by combined use of HPLC and fluorescence image analysis. Clin Cancer Res. 2000;6(5):1826–1832.
26. Haile S, Corbett RD, Bilobram S, et al. Sources of erroneous sequences and artifact chimeric reads in next generation sequencing of genomic DNA from formalin-fixed paraffin-embedded samples. Nucleic Acids Res. 2019;47(2):e12. doi:10.1093/nar/gky1142
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.